COVID-19 in the Eastern Brazilian Amazon: Incidence, Clinical Management, and Mortality by Social Determinants of Health, Symptomatology, and Comorbidities in the Xingu Health Region
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Population and Period
2.3. Inclusion and Exclusion Criteria
2.4. Setting
2.5. Assessments
2.6. Statistical Analysis
2.7. Ethical Issues
3. Results
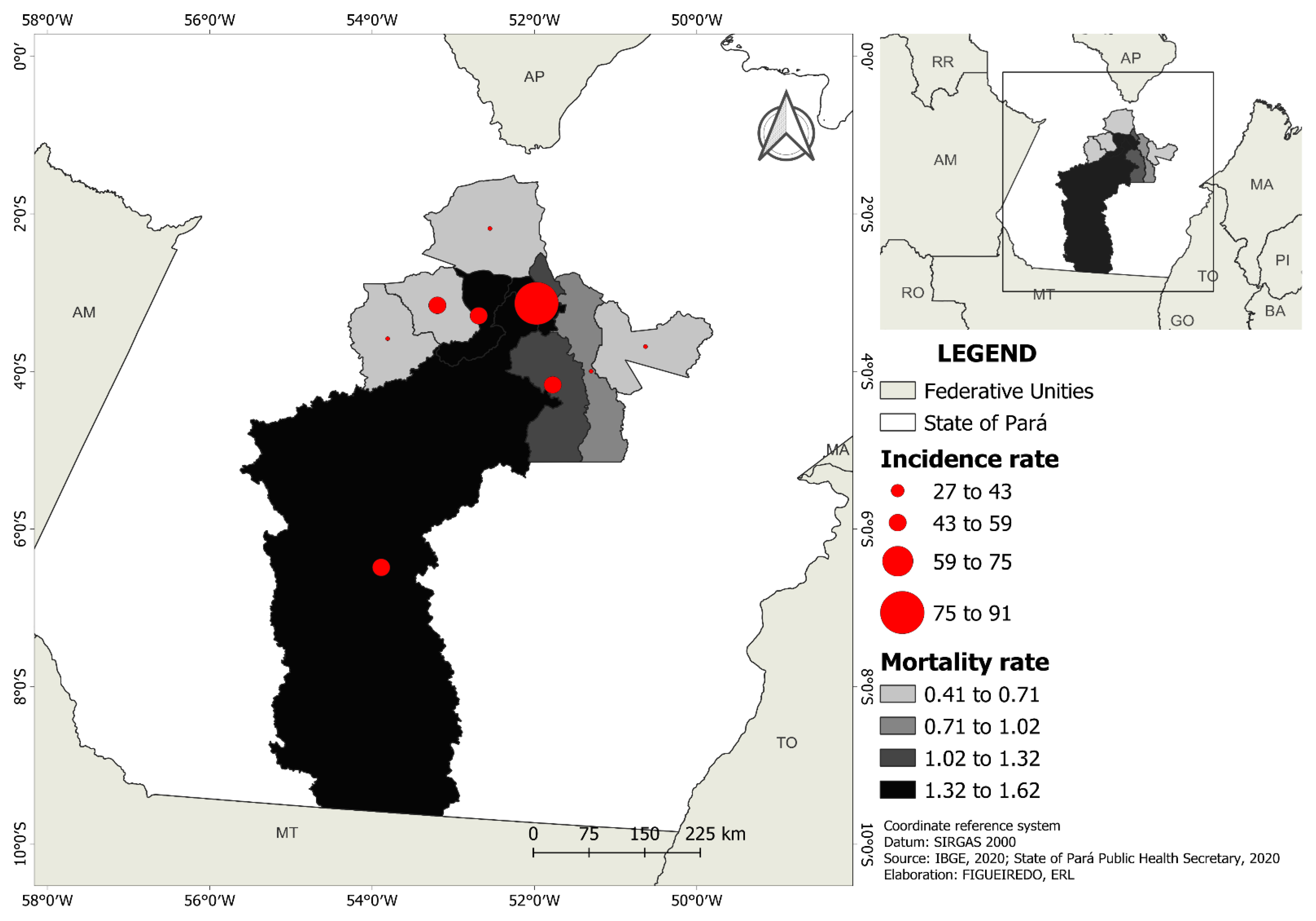
3.1. Relationship among the SDH Indicators, Incidence, and Mortality
3.2. Sociodemographic Factors, Symptoms and Comorbidities as Predictors of Clinical Management
3.3. Sociodemographic Factors, Symptoms and Comorbidities as Predictors of Mortality
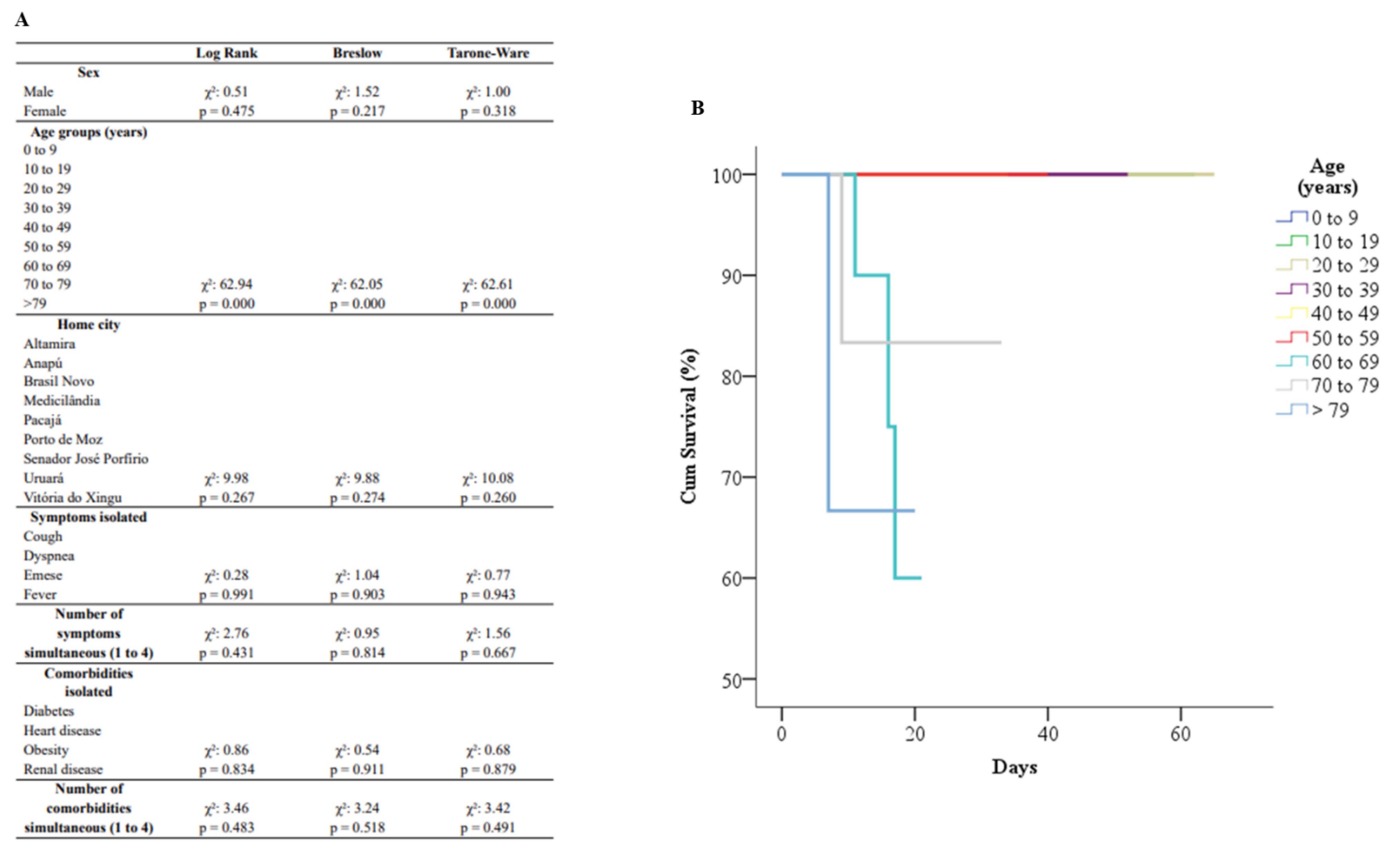
3.4. Survival Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wuhan Municipal Health Commission Report of Clustering Pneumonia of Unknown Etiology in Wuhan City. Available online: http://wjw.wuhan.gov.cn/front/web/showDetail/2019123108989 (accessed on 28 November 2022).
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China. JAMA 2020, 323, 1061–1069. [Google Scholar] [CrossRef] [PubMed]
- New-Type Coronavirus Causes Pneumonia in Wuhan: Expert. Available online: http://www.xinhuanet.com/english/2020-01/09/c_138690570.htm (accessed on 28 November 2022).
- Martellucci, C.A.; Flacco, M.E.; Cappadona, R.; Bravi, F.; Mantovani, L.; Manzoli, L. SARS-CoV-2 Pandemic: An Overview. Adv. Biol. Regul. 2020, 77, 100736. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Coronavirus Disease 2019 (COVID-19): Situation Report, 191. 2020. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200729-covid-19-sitrep-191.pdf?%20sfvrsn=2c327e9e2 (accessed on 28 November 2022).
- Sheleme, T.; Bekele, F.; Ayela, T. Clinical Presentation of Patients Infected with Coronavirus Disease 19: A Systematic Review. Infect. Dis. 2020, 13, 1178633720952076. [Google Scholar] [CrossRef] [PubMed]
- De Vito, A.; Geremia, N.; Fiore, V.; Princic, E.; Babudieri, S.; Madeddu, G. Clinical Features, Laboratory Findings and Predictors of Death in Hospitalized Patients with COVID-19 in Sardinia, Italy. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 7861–7868. [Google Scholar] [CrossRef]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical Features of Patients Infected with 2019 Novel Coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Vaira, L.A.; Deiana, G.; Fois, A.G.; Pirina, P.; Madeddu, G.; De Vito, A.; Babudieri, S.; Petrocelli, M.; Serra, A.; Bussu, F.; et al. Objective Evaluation of Anosmia and Ageusia in COVID-19 Patients: Single-Center Experience on 72 Cases. Head Neck 2020, 42, 1252–1258. [Google Scholar] [CrossRef]
- Guarneri, C.; Rullo, E.V.; Pavone, P.; Berretta, M.; Ceccarelli, M.; Natale, A.; Nunnari, G. Silent COVID-19: What Your Skin Can Reveal. Lancet Infect. Dis. 2021, 21, 24–25. [Google Scholar] [CrossRef]
- Guarneri, C.; Venanzi Rullo, E.; Gallizzi, R.; Ceccarelli, M.; Cannavò, S.P.; Nunnari, G. Diversity of Clinical Appearance of Cutaneous Manifestations in the Course of COVID-19. J. Eur. Acad. Dermatol. Venereol. 2020, 34, e449–e450. [Google Scholar] [CrossRef]
- Li, L.; Huang, T.; Wang, Y.; Wang, Z.; Liang, Y.; Huang, T.; Zhang, H.; Sun, W.; Wang, Y. COVID-19 Patients’ Clinical Characteristics, Discharge Rate, and Fatality Rate of Meta-analysis. J. Med. Virol. 2020, 92, 577. [Google Scholar] [CrossRef]
- Fiore, V.; De Vito, A.; Bagella, P.; Princic, E.; Mariani, A.A.; Denti, L.; Fois, A.G.; Madeddu, G.; Babudieri, S.; Maida, I. Effectiveness of Vitamin D Supplements among Patients Hospitalized for COVID-19: Results from a Monocentric Matched-Cohort Study. Healthcare 2022, 10, 956. [Google Scholar] [CrossRef]
- Rodriguez-Guerra, M.; Jadhav, P.; Vittorio, T.J. Current Treatment in COVID-19 Disease: A Rapid Review. Drugs Context 2021, 10. [Google Scholar] [CrossRef]
- World Health Organization. Coronavirus Disease (COVID-19) Pandemic. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019?adgroupsurvey={adgroupsurvey}&gclid%20CJWKCAIAJS2BBHACEIWALTBWZVX8ZRICAJ1U0HR6YIFNDW7HNHMCSKU__HKYOUNI79JUDSVMYFBSNROCZVIDOQUEQUENO101S101S10 (accessed on 28 November 2022).
- O’Connor, R.C.; Wetherall, K.; Cleare, S.; McClelland, H.; Melson, A.J.; Niedzwiedz, C.L.; O’Carroll, R.E.; O’Connor, D.B.; Platt, S.; Scowcroft, E.; et al. Mental Health and Well-Being during the COVID-19 Pandemic: Longitudinal Analyses of Adults in the UK COVID-19 Mental Health & Wellbeing Study. Br. J. Psychiatry 2021, 218, 326–333. [Google Scholar] [CrossRef]
- Lekamwasam, R.; Lekamwasam, S. Effects of COVID-19 Pandemic on Health and Wellbeing of Older People: A Comprehensive Review. Ann. Geriatr. Med. Res. 2020, 24, 166–172. [Google Scholar] [CrossRef]
- Wachtler, B.; Hoebel, J. Soziale Ungleichheit und COVID-19: Sozialepidemiologische Perspektiven auf die Pandemie. Gesundheitswesen 2020, 82, 670–675. [Google Scholar] [CrossRef]
- Codeço, C.T.; Dal’Asta, A.P.; Rorato, A.C.; Lana, R.M.; Neves, T.C.; Andreazzi, C.S.; Barbosa, M.; Escada, M.I.S.; Fernandes, D.A.; Rodrigues, D.L.; et al. Epidemiology, Biodiversity, and Technological Trajectories in the Brazilian Amazon: From Malaria to COVID-19. Front. Public Health 2021, 9, 945. [Google Scholar] [CrossRef]
- Rodrigues-Filho, J.L.; Abe, D.S.; Gatti-Junior, P.; Medeiros, G.R.; Degani, R.M.; Blanco, F.P.; Faria, C.R.L.; Campanelli, L.; Soares, F.S.; Sidagis-Galli, C.V.; et al. Spatial Patterns of Water Quality in Xingu River Basin (Amazonia) Prior to the Belo Monte Dam Impoundment. Braz. J. Biol. 2015, 75, 34–46. [Google Scholar] [CrossRef] [Green Version]
- IBGE. Cidades e Estados. 2022. Available online: https://www.ibge.gov.br/cidades-e-estados/ (accessed on 25 July 2022).
- Brasil. Decreto Nº 7508, de 28 de Junho de 2011, Regulamenta a Lei no 8.080, de 19 de Setembro de 1990, Para Dispor Sobre a Organização do Sistema Único de Saúde—SUS, o Planejamento da Saúde, a Assistência à Saúde e a Articulação Interfederativa, e dá Outras Providências. 2011; Diário Oficial da República Federativa do Brasil. Brasília, DF, 29/06/2011; p. 1. Available online: https://planalto.gov.br/ccivil_03/_ato2011-2014/2011/decreto/d7508. (accessed on 25 July 2022).
- Santos, L. Região de saúde e suas redes de atenção: Modelo organizativo-sistêmico do SUS. Ciênc. Saúde Coletiva 2017, 22, 1281–1289. [Google Scholar] [CrossRef] [Green Version]
- da Silva Junior, O.M.; dos Santos, M.A.; Szlafsztein, C.F.; Gomez, J.M.A.; Pereira, J.P. Protected Areas as Strategies for Preserving Vegetation Cover in the Vicinity of Hydroelectric Projects in the Brazilian Amazon. Energ. Sustain. Soc. 2018, 8, 33. [Google Scholar] [CrossRef] [Green Version]
- Lucena, M.D.L.D.; Pereira, T.D.S.; Gonçalves, A.P.; Silva, K.D.; Sousa, L.M.D. Diversity of Loricariidae (Actinopterygii: Siluriformes) Assemblages in Two Conservation Areas of the Middle Xingu River, Brazilian Amazon, and Their Suitability for Sustainable Ornamental Fisheries. Neotrop. Ichthyol. 2021, 19. [Google Scholar] [CrossRef]
- Floss, M.; Franco, C.M.; Malvezzi, C.; Silva, K.V.; Costa, B.D.R.; Silva, V.X.D.L.; Werreria, N.S.; Duarte, D.R. A Pandemia de COVID-19 Em Territórios Rurais e Remotos: Perspectiva de Médicas e Médicos de Família e Comunidade Sobre a Atenção Primária à Saúde. Cad. Saúde Pública 2020, 36, 9–13. [Google Scholar] [CrossRef]
- Bambra, C.; Riordan, R.; Ford, J.; Matthews, F. The COVID-19 Pandemic and Health Inequalities. J. Epidemiol. Community Health 2020, 74, 964–968. [Google Scholar] [CrossRef] [PubMed]
- Caron, R.M.; Adegboye, A.R.A. COVID-19: A Syndemic Requiring an Integrated Approach for Marginalized Populations. Front. Public Health 2021, 9, 515. [Google Scholar] [CrossRef] [PubMed]
- Piroth, L.; Cottenet, J.; Mariet, A.-S.; Bonniaud, P.; Blot, M.; Tubert-Bitter, P.; Quantin, C. Comparison of the Characteristics, Morbidity, and Mortality of COVID-19 and Seasonal Influenza: A Nationwide, Population-Based Retrospective Cohort Study. Lancet Respir. Med. 2021, 9, 251–259. [Google Scholar] [CrossRef] [PubMed]
- Eslava-Castañeda, J.C. Pensando la determinación social del proceso salud-enfermedad. Rev. Salud Pública 2017, 9, 396–403. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mena, G.E.; Martinez, P.P.; Mahmud, A.S.; Marquet, P.A.; Buckee, C.O.; Santillana, M. Socioeconomic Status Determines COVID-19 Incidence and Related Mortality in Santiago, Chile. Science 2021, 372, eabg5298. [Google Scholar] [CrossRef]
- Khanijahani, A.; Iezadi, S.; Gholipour, K.; Azami-Aghdash, S.; Naghibi, D. A Systematic Review of Racial/Ethnic and Socioeconomic Disparities in COVID-19. Int. J. Equity Health 2021, 20, 248. [Google Scholar] [CrossRef]
- Meyerowitz, E.A.; Richterman, A.; Gandhi, R.T.; Sax, P.E. Transmission of SARS-CoV-2: A Review of Viral, Host, and Environmental Factors. Ann. Intern. Med. 2021, 174, 69–79. [Google Scholar] [CrossRef]
- Quesada, J.A.; López-Pineda, A.; Gil-Guillén, V.F.; Arriero-Marín, J.M.; Gutiérrez, F.; Carratala-Munuera, C. Incubation Period of COVID-19: A Systematic Review and Meta-Analysis. Rev. Clínica Española 2021, 221, 109–117. [Google Scholar] [CrossRef]
- Lim, J.; Lee, J. Current Laboratory Diagnosis of Coronavirus Disease 2019. Korean J. Intern. Med. 2020, 35, 741. [Google Scholar] [CrossRef]
- SESPA. Available online: https://www.covid-19.pa.gov.br. (accessed on 31 August 2022).
- IBGE. Cidades e Estados. 2022. Available online: https://cidades.ibge.gov.br/brasil/pa/ (accessed on 28 July 2022).
- Ministério da Saúde. Cobertura da Atenção Básica (e-Gestor). 2022. Available online: https://egestorab.saude.gov.br/paginas/acessoPublico/relatorios/relHistoricoCoberturaACS.xhtml (accessed on 28 July 2022).
- Ministério da Saúde. Cobertura de Agentes Comunitários de Saúde (e-Gestor). 2022. Available online: https://egestorab.saude.gov.br/paginas/acessoPublico/relatorios/relHistoricoCoberturaACS.xhtml. (accessed on 28 July 2022).
- INPE. Open Data. 2022. Available online: https://www.gov.br/inpe/pt-br/acesso-a-info. (accessed on 31 July 2022).
- Tonin, F.S.; Araujo, A.G.; Fachi, M.M.; Ferreira, V.L.; Pontarolo, R.; Fernandez-Llimos, F. Lag Times in the Publication of Network Meta-Analyses: A Survey. BMJ Open 2021, 11, e048581. [Google Scholar] [CrossRef]
- Whitehead, M.; Dahlgren, G. Concepts and Principles for Tackling Social Inequities in Health: Levelling up Part 1. World Health Organ. Stud. Soc. Econ. Determ. Popul. Health 2006, 2, 460–474. [Google Scholar]
- Conselho Nacional de Saúde. Resolução 510, de 7 de Abril de 2016. Diário Oficial da União. 2016. Available online: https://bvsms.saude.gov.br/bvs/saudelegis/cns/2016/res0510_07_04_2016.html (accessed on 21 July 2022).
- Vallinoto, A.C.R.; da Silva Torres, M.K.; Vallinoto, M.C.; Cayres Vallinoto, I.M.V. The Challenges of COVID-19 in the Brazilian Amazonian Communities and the Importance of Seroepidemiological Surveillance Studies. Int. J. Equity Health 2020, 19, 140. [Google Scholar] [CrossRef]
- Ferrante, L.; Steinmetz, W.A.; Almeida, A.C.L.; Leão, J.; Vassão, R.C.; Tupinambás, U.; Fearnside, P.M.; Duczmal, L.H. Brazil’s Policies Condemn Amazonia to a Second Wave of COVID-19. Nat. Med. 2020, 26, 1315. [Google Scholar] [CrossRef]
- Ortega, F.; Orsini, M. Governing COVID-19 without Government in Brazil: Ignorance, Neoliberal Authoritarianism, and the Collapse of Public Health Leadership. Glob. Public Health 2020, 15, 1257–1277. [Google Scholar] [CrossRef]
- Lima, E.E.C.D.; Gayawan, E.; Baptista, E.A.; Queiroz, B.L. Spatial Pattern of COVID-19 Deaths and Infections in Small Areas of Brazil. PLoS ONE 2021, 16, e0246808. [Google Scholar] [CrossRef]
- Bertolli Filho, C. A Gripe Espanhola em São Paulo, 1918: Epidemia e Sociedade; Paz e Terra, Santa Ifigênia: São Paulo, Brazil, 2003; p. 393. Available online: https://pesquisa.bvsalud.org/portal/resource/pt/lil-384570.
- Pacífico Filho, M.; Borges, T.P.; Iwamoto, H.M.; Cançado, A.C. COVID-19 in the legal Amazon. Mercator 2021, 20. [Google Scholar] [CrossRef]
- Castro, F.d.; Lopes, G.R.; Brondizio, E.S. The Brazilian Amazon in Times of COVID-19: From Crisis to Transformation? Ambient. Soc. 2020, 23, 1–11. [Google Scholar] [CrossRef]
- Figueiredo, A.M.D.; Figueiredo, D.C.M.M.D.; Gomes, L.B.; Massuda, A.; Gil-García, E.; Vianna, R.P.D.T.; Daponte, A. Social Determinants of Health and COVID-19 Infection in Brazil: An Analysis of the Pandemic. Rev. Bras. Enferm. 2020, 73. [Google Scholar] [CrossRef]
- Borges, G.M.; Crespo, C.D. Demographic and Socioeconomic Characteristics of Brazilian Adults and COVID-19: A Risk Group Analysis Based on the Brazilian National Health Survey, 2013. Cad. Saúde Pública 2020, 36. [Google Scholar] [CrossRef]
- Xavier, D.R.; Lima e Silva, E.; Lara, F.A.; e Silva, G.R.R.; Oliveira, M.F.; Gurgel, H.; Barcellos, C. Involvement of Political and Socio-Economic Factors in the Spatial and Temporal Dynamics of COVID-19 Outcomes in Brazil: A Population-Based Study. Lancet Reg. Health Am. 2022, 10, 100221. [Google Scholar] [CrossRef]
- Funcia, F.; Bresciani, L.P.; Benevides, R.; Ocké-Reis, C.O. Análise do financiamento federal do Sistema Único de Saúde para o enfrentamento da Covid-19. Saúde Debate 2022, 46, 263–276. [Google Scholar] [CrossRef]
- Hall, K.S.; Samari, G.; Garbers, S.; Casey, S.E.; Diallo, D.D.; Orcutt, M.; Moresky, R.T.; Martinez, M.E.; McGovern, T. Centring Sexual and Reproductive Health and Justice in the Global COVID-19 Response. Lancet 2020, 395, 1175–1177. [Google Scholar] [CrossRef] [PubMed]
- Galbadage, T.; Peterson, B.M.; Awada, J.; Buck, A.S.; Ramirez, D.A.; Wilson, J.; Gunasekera, R.S. Systematic Review and Meta-Analysis of Sex-Specific COVID-19 Clinical Outcomes. Front. Med. 2020, 7, 348. [Google Scholar] [CrossRef] [PubMed]
- Wehbe, Z.; Hammoud, S.H.; Yassine, H.M.; Fardoun, M.; El-Yazbi, A.F.; Eid, A.H. Molecular and Biological Mechanisms Underlying Gender Differences in COVID-19 Severity and Mortality. Front. Immunol. 2021, 12, 1603. [Google Scholar] [CrossRef] [PubMed]
- Mueller, A.L.; McNamara, M.S.; Sinclair, D.A. Why Does COVID-19 Disproportionately Affect Older People? Aging 2020, 12, 9959. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Ding, M.; Dong, X.; Zhang, J.; Kursat Azkur, A.; Azkur, D.; Gan, H.; Sun, Y.; Fu, W.; Li, W.; et al. Risk Factors for Severe and Critically Ill COVID-19 Patients: A Review. Allergy 2021, 76, 428–455. [Google Scholar] [CrossRef]
- Li, H.; Burm, S.W.; Hong, S.H.; Ghayda, R.A.; Kronbichler, A.; Smith, L.; Koyanagi, A.; Jacob, L.; Lee, K.H.; Shin, J.I. A Comprehensive Review of Coronavirus Disease 2019: Epidemiology, Transmission, Risk Factors, and International Responses. Yonsei Med. J. 2021, 62, 1–11. [Google Scholar] [CrossRef]
- Jain, V.; Yuan, J.-M. Predictive Symptoms and Comorbidities for Severe COVID-19 and Intensive Care Unit Admission: A Systematic Review and Meta-Analysis. Int. J. Public Health 2020, 65, 533–546. [Google Scholar] [CrossRef]
- Nasir, N.; Habib, K.; Khanum, I.; Khan, N.; Muhammad, Z.A.; Mahmood, S.F. Clinical Characteristics and Outcomes of COVID-19: Experience at a Major Tertiary Care Center in Pakistan. J. Infect. Dev. Ctries. 2021, 15, 480–489. [Google Scholar] [CrossRef]
- Setiati, S.; Harimurti, K.; Safitri, E.D.; Ranakusuma, R.W.; Saldi, S.R.F.; Azwar, M.K.; Marsigit, J.; Pitoyo, Y.; Widyaningsih, W. Risk Factors and Laboratory Test Results Associated with Severe Illness and Mortality in COVID-19 Patients: A Systematic Review. Acta Med. Indones 2020, 52, 227–245. [Google Scholar]
- Yang, J.; Zheng, Y.; Gou, X.; Pu, K.; Chen, Z.; Guo, Q.; Ji, R.; Wang, H.; Wang, Y.; Zhou, Y. Prevalence of Comorbidities and Its Effects in Patients Infected with SARS-CoV-2: A Systematic Review and Meta-Analysis. Int. J. Infect. Dis. 2020, 94, 91–95. [Google Scholar] [CrossRef]
- Kipourou, D.-K.; Leyrat, C.; Alsheridah, N.; Almazeedi, S.; Al-Youha, S.; Jamal, M.H.; Al-Haddad, M.; Al-Sabah, S.; Rachet, B.; Belot, A. Probabilities of ICU Admission and Hospital Discharge According to Patient Characteristics in the Designated COVID-19 Hospital of Kuwait. BMC Public Health 2021, 21, 799. [Google Scholar] [CrossRef]
- Fang, X.; Li, S.; Yu, H.; Wang, P.; Zhang, Y.; Chen, Z.; Li, Y.; Cheng, L.; Li, W.; Jia, H.; et al. Epidemiological, Comorbidity Factors with Severity and Prognosis of COVID-19: A Systematic Review and Meta-Analysis. Aging 2020, 12, 12493. [Google Scholar] [CrossRef]
- Bonow, R.O.; O’Gara, P.T.; Yancy, C.W. Cardiology and COVID-19. JAMA 2020, 324, 1131–1132. [Google Scholar] [CrossRef]
- Li, J.; Huang, D.Q.; Zou, B.; Yang, H.; Hui, W.Z.; Rui, F.; Yee, N.T.S.; Liu, C.; Nerurkar, S.N.; Kai, J.C.Y.; et al. Epidemiology of COVID-19: A Systematic Review and Meta-Analysis of Clinical Characteristics, Risk Factors, and Outcomes. J. Med. Virol. 2021, 93, 1449–1458. [Google Scholar] [CrossRef]
- Liu, L.; Ni, S.-Y.; Yan, W.; Lu, Q.-D.; Zhao, Y.-M.; Xu, Y.-Y.; Mei, H.; Shi, L.; Yuan, K.; Han, Y.; et al. Mental and Neurological Disorders and Risk of COVID-19 Susceptibility, Illness Severity and Mortality: A Systematic Review, Meta-Analysis and Call for Action. EClinicalMedicine 2021, 40, 101111. [Google Scholar] [CrossRef]
- Elimian, K.O.; Ochu, C.L.; Ebhodaghe, B.; Myles, P.; Crawford, E.E.; Igumbor, E.; Ukponu, W.; Olayinka, A.; Aruna, O.; Dan-Nwafor, C.; et al. Patient Characteristics Associated with COVID-19 Positivity and Fatality in Nigeria: Retrospective Cohort Study. BMJ Open 2020, 10, e044079. [Google Scholar] [CrossRef]
- Talic, S.; Shah, S.; Wild, H.; Gasevic, D.; Maharaj, A.; Ademi, Z.; Li, X.; Xu, W.; Mesa-Eguiagaray, I.; Rostron, J.; et al. Effectiveness of Public Health Measures in Reducing the Incidence of Covid-19, SARS-CoV-2 Transmission, and Covid-19 Mortality: Systematic Review and Meta-Analysis. BMJ 2021, 375, e068302. [Google Scholar] [CrossRef]
- Affonso, M.V.D.G.; Souza, I.G.; Rocha, E.S.d.; Goloni-Bertollo, E.M.; Gomes, F.D.C.; Nascimento, L.S.d.; Melo-Neto, J.S.d. Association between Sociodemographic Factors, Coverage and Offer of Health Services with Mortality Due to Oral and Oropharyngeal Cancer in Brazil: A 20-Year Analysis. Int. J. Environ. Res. Public Health 2022, 19, 13208. [Google Scholar] [CrossRef]

| Social Determinants of Health | Xingu Health Region | Altamira | Anapu | Brasil Novo | Medicilândia | Pacajá | Porto de Moz | Senador José Porfírio | Uruará | Vitória do Xingu |
|---|---|---|---|---|---|---|---|---|---|---|
| Sex | ||||||||||
| Incidence in females | 55.42 | 62.09 | 48.40 | 65.43 | 59.97 | 44.14 | 40.31 | 69.88 | 35.31 | 117.77 |
| Incidence in males | 44.37 | 60.43 | 35.45 | 51.55 | 46.79 | 29.98 | 26.43 | 48.38 | 25.65 | 78.61 |
| Mortality in females | 1.38 | 2.10 | 1.17 | 1.22 | 0.54 | 0.45 | 1.00 | 1.66 | 0.78 | 2.59 |
| Mortality in males | 0.71 | 1.13 | 0.64 | 1.23 | 0.48 | 0.32 | 0.51 | 0.97 | 0.23 | 0.73 |
| Sociodemographic and housing | ||||||||||
| Population density (2010) | 2.81 | 0.71 | 2.28 | 2.39 | 3.77 | 3.97 | 2.32 | 0.82 | 4.22 | 4.85 |
| Percentage of elderly in population (2020) | 8.58 | 10.01 | 7.35 | 13.23 | 8.91 | 8.32 | 5.00 | 8.05 | 7.97 | 8.41 |
| Percentage in vulnerable households with the elderly in the population (2010) | 6.15 | 4.4 | 5.06 | 5.90 | 3.93 | 6.12 | 7.50 | 10.40 | 4.72 | 7.40 |
| Percentage of the population residing in households with walls not made of masonry or wood (2010) | 18.15 | 12.24 | 29.51 | 15.38 | 20.17 | 27.84 | 18.31 | 13.95 | 17.33 | 8.66 |
| Economic and environmental factors | ||||||||||
| Gini index (2010) | 0.6084 | 0.572 | 0.585 | 0.684 | 0.614 | 0.663 | 0.599 | 0.566 | 0.586 | 0.606 |
| Gross Domestic Product in BRL (GDP) (2020) | 43,941.75 | 24,250.13 | 14,926.79 | 18,362.96 | 20,744.58 | 14,223.20 | 7842.34 | 14,017.34 | 13,431.86 | 267,676.58 |
| Human Development Index (HDI) (2010) | 0.569 | 0.665 | 0.548 | 0.613 | 0.582 | 0.515 | 0.503 | 0.514 | 0.589 | 0.596 |
| Percentage urbanization of public roads (2010) | 4.79 | 22.70 | 0.40 | 2.40 | 0.70 | 0.40 | 4.40 | 6.30 | 3.43 | 2.40 |
| Hotspot concentration (2017) | 5.25 | 23.62 | 3.39 | 1.78 | 2.89 | 6.39 | 2.25 | 2.99 | 3.43 | 0.51 |
| Health and resources | ||||||||||
| Primary health care coverage in % (2020) | 66.85 | 63.22 | 74.22 | 100 | 65.51 | 43.39 | 58.71 | 29.59 | 75.86 | 91.19 |
| Percentage of people with health insurance (2017) | 1.21 | 4.72 | 0.9 | 0.84 | 0.47 | 0.24 | 0.25 | 1.3 | 0.64 | 1.58 |
| Number of physicians per 1000 individuals (2021) | 0.41 | 1.22 | 0.28 | 0.26 | 0.22 | 0.18 | 0.19 | 0.42 | 0.30 | 0.66 |
| Public health expenditure in the municipality, in BRL/inhabitant, per capita (2021) | 887.99 | 731.29 | 657.99 | 1120.96 | 597.16 | 602.70 | 549.97 | 841.30 | 624.57 | 2266.03 |
| Education and work | ||||||||||
| Schooling sub-index (2010) | 0.294 | 0.461 | 0.278 | 0.293 | 0.266 | 0.246 | 0.248 | 0.207 | 0.342 | 0.307 |
| Illiteracy rate at age 15 and above (2010) | 18.11 | 12.45 | 19.24 | 16.09 | 18.35 | 21.53 | 21.46 | 22.71 | 15.11 | 16.09 |
| Unemployment rate at 10 years or older (2010) | 5.44 | 6.96 | 3.51 | 4.06 | 2.72 | 4.81 | 6.93 | 5.76 | 6.56 | 7.71 |
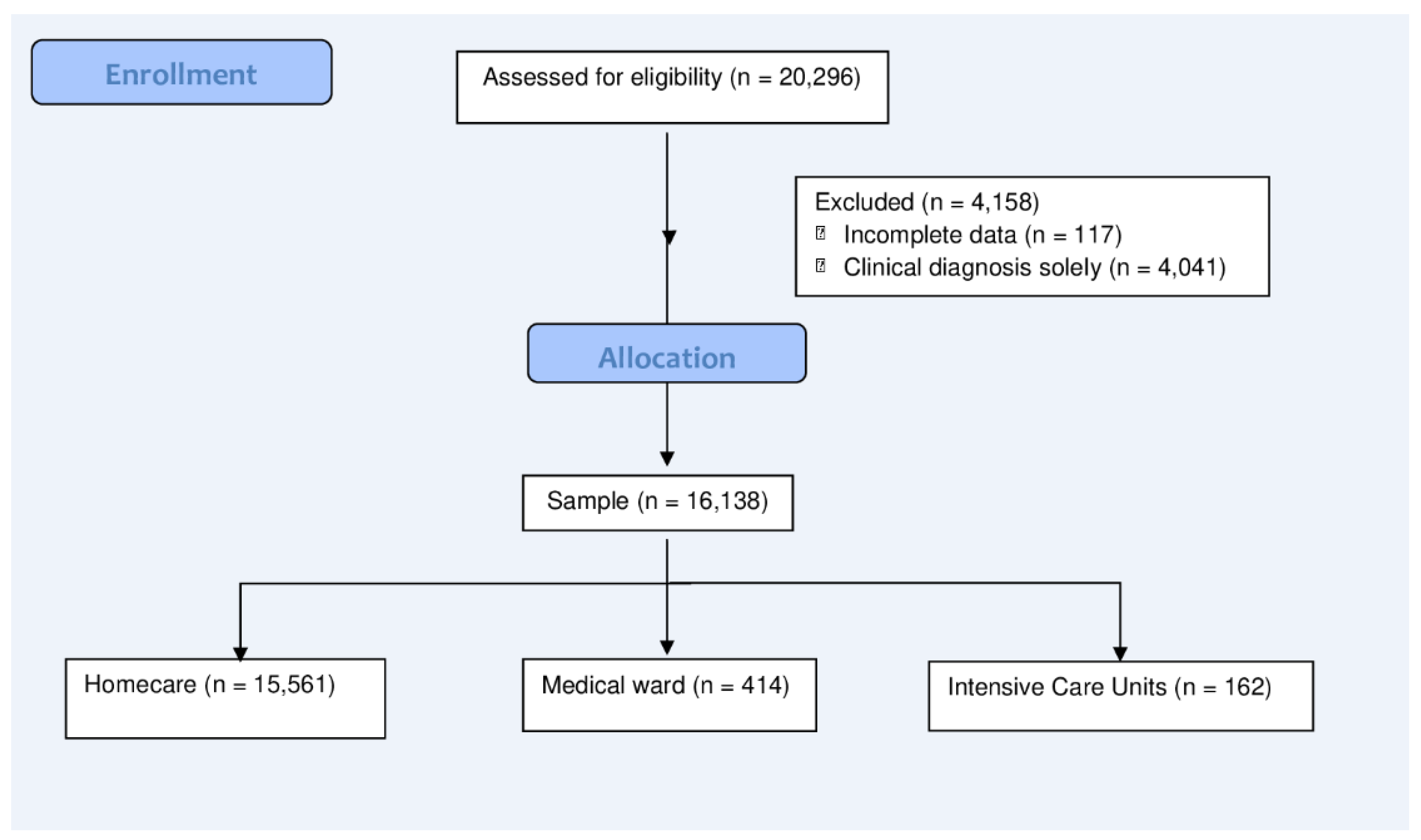
| Characteristic | Home Care N = 15,561 1 | Medical Ward N = 414 1 | N | OR 2 | 95% CI 2 | p-Value | aOR 3 | 95% CI 3 | p-Value |
|---|---|---|---|---|---|---|---|---|---|
| Age | 38 (27, 50) | 64 (46, 77) | 15,975 | 1.06 | 1.06, 1.07 | <0.001 | 1.05 | 1.04, 1.05 | <0.001 |
| Municipality | 15,975 | <0.001 | |||||||
| Altamira | 6297 (40%) | 194 (47%) | — | — | — | — | |||
| Anapu | 1112 (7.1%) | 18 (4.3%) | 0.53 | 0.31, 0.83 | 0.61 | 0.34, 1.02 | 0.072 | ||
| Brasil Novo | 769 (4.9%) | 38 (9.2%) | 1.60 | 1.11, 2.26 | 2.02 | 1.30, 3.07 | 0.001 | ||
| Medicilândia | 1505 (9.7%) | 28 (6.8%) | 0.60 | 0.40, 0.89 | 0.77 | 0.46, 1.23 | 0.29 | ||
| Pacajá | 1551 (10.0%) | 38 (9.2%) | 0.80 | 0.55, 1.12 | 0.70 | 0.45, 1.05 | 0.092 | ||
| Porto de Moz | 1138 (7.3%) | 44 (11%) | 1.25 | 0.89, 1.73 | 1.15 | 0.74, 1.73 | 0.53 | ||
| Senador José Porfírio | 622 (4.0%) | 22 (5.3%) | 1.15 | 0.71, 1.76 | 1.19 | 0.69, 1.96 | 0.51 | ||
| Uruará | 1205 (7.7%) | 11 (2.7%) | 0.30 | 0.15, 0.52 | 0.42 | 0.20, 0.79 | 0.012 | ||
| Vitória do Xingu | 1362 (8.8%) | 21 (5.1%) | 0.50 | 0.31, 0.77 | 0.35 | 0.19, 0.61 | <0.001 | ||
| Sex | 15,975 | ||||||||
| Male | 7208 (46%) | 254 (61%) | — | — | — | — | |||
| Female | 8353 (54%) | 160 (39%) | 0.54 | 0.44, 0.66 | <0.001 | 0.68 | 0.54, 0.86 | 0.001 | |
| Local case | 14,815 (95%) | 377 (91%) | 0.51 | 0.37, 0.74 | <0.001 | 0.41 | 0.25, 0.72 | 0.001 | |
| Imported case | 221 (1.4%) | 21 (5.1%) | 15,975 | 3.71 | 2.28, 5.73 | <0.001 | 1.47 | 0.72, 3.00 | 0.29 |
| Fever | 9532 (61%) | 293 (71%) | 15,975 | 1.53 | 1.24, 1.90 | <0.001 | 1.34 | 1.03, 1.76 | 0.031 |
| Cough | 8724 (56%) | 315 (76%) | 15,975 | 2.49 | 1.99, 3.15 | <0.001 | 1.87 | 1.42, 2.47 | <0.001 |
| Emesis | 463 (3.0%) | 32 (7.7%) | 15,975 | 2.73 | 1.85, 3.90 | <0.001 | 3.55 | 2.17, 5.60 | <0.001 |
| Headache | 5637 (36%) | 50 (12%) | 15,975 | 0.24 | 0.18, 0.32 | <0.001 | 0.48 | 0.34, 0.67 | <0.001 |
| Runny nose | 1548 (9.9%) | 10 (2.4%) | 15,975 | 0.22 | 0.11, 0.40 | <0.001 | 0.54 | 0.25, 1.04 | 0.089 |
| Nasal congestion | 246 (1.6%) | 6 (1.4%) | 15,975 | 0.92 | 0.36, 1.89 | 0.830 | |||
| Sore throat | 6758 (43%) | 112 (27%) | 15,975 | 0.48 | 0.39, 0.60 | <0.001 | 0.38 | 0.29, 0.49 | <0.001 |
| Myalgia and arthralgia | 3642 (23%) | 38 (9.2%) | 15,975 | 0.33 | 0.23, 0.46 | <0.001 | 0.57 | 0.38, 0.82 | 0.003 |
| Diarrhea | 1360 (8.7%) | 38 (9.2%) | 15,975 | 1.06 | 0.74, 1.46 | 0.757 | |||
| Chills | 193 (1.2%) | 1 (0.2%) | 15,975 | 0.19 | 0.01, 0.86 | 0.026 | 0.35 | 0.02, 1.83 | 0.33 |
| Adynamia | 584 (3.8%) | 20 (4.8%) | 15,975 | 1.30 | 0.80, 2.00 | 0.275 | |||
| Odynophagy | 70 (0.4%) | 0 (0%) | 15,975 | 0.00 | 0.00, 0.09 | 0.055 | |||
| Anosmia | 3166 (21%) | 33 (9.1%) | 15,517 | 0.38 | 0.26, 0.53 | <0.001 | 1.00 | 0.54, 1.81 | >0.99 |
| Ageusia | 2950 (19%) | 29 (8.0%) | 15,517 | 0.36 | 0.24, 0.52 | <0.001 | 0.62 | 0.32, 1.16 | 0.14 |
| Dyspnea | 4097 (26%) | 290 (70%) | 15,975 | 6.54 | 5.30, 8.12 | <0.001 | 4.01 | 3.14, 5.14 | <0.001 |
| Conjunctivitis | 27 (0.2%) | 0 (0%) | 15,975 | 0.00 | 0.00, 13.0 | 0.234 | 0.00 | 0.00, 17.0 | 0.97 |
| Diabetes | 272 (1.7%) | 67 (16%) | 15,975 | 10.9 | 8.09, 14.4 | <0.001 | 3.15 | 2.13, 4.61 | <0.001 |
| Immunodeficiency | 116 (0.7%) | 4 (1.0%) | 15,975 | 1.30 | 0.40, 3.11 | 0.623 | |||
| Heart diseases | 399 (2.6%) | 73 (18%) | 15,975 | 8.13 | 6.16, 10.6 | <0.001 | 2.16 | 1.45, 3.19 | <0.001 |
| Lung diseases | 65 (0.4%) | 1 (0.2%) | 15,975 | 0.58 | 0.03, 2.62 | 0.550 | |||
| Neurological diseases | 1 (<0.1%) | 1 (0.2%) | 15,975 | 37.7 | 1.49, 954 | 0.032 | 168 | 6.14, 4,658 | <0.001 |
| Kidney diseases | 24 (0.2%) | 9 (2.2%) | 15,975 | 14.4 | 6.29, 30.1 | <0.001 | 5.45 | 1.80, 14.9 | 0.002 |
| Obesity | 12 (<0.1%) | 12 (2.9%) | 15,975 | 38.7 | 17.1, 87.5 | <0.001 | 13.9 | 4.60, 42.3 | <0.001 |
| Asthma | 30 (0.2%) | 2 (0.5%) | 15,975 | 2.51 | 0.41, 8.35 | 0.268 | |||
| Blood diseases | 3 (<0.1%) | 2 (0.5%) | 15,975 | 25.2 | 3.31, 152 | 0.005 | 22.6 | 1.01, 515 | 0.059 |
| Liver diseases | 3 (<0.1%) | 2 (0.5%) | 15,975 | 25.2 | 3.31, 152 | 0.005 | 22.6 | 1.01, 515 | 0.059 |
| Characteristic | Home Care N = 15,561 1 | ICU N = 162 1 | N | OR 2 | 95% CI 2 | p-Value | aOR 3 | 95% CI 3 | p-Value |
|---|---|---|---|---|---|---|---|---|---|
| Age | 38 (27, 50) | 66 (50, 75) | 15,723 | 1.07 | 1.06, 1.08 | <0.001 | 1.04 | 1.03, 1.06 | <0.001 |
| Municipality | 15,723 | <0.001 | |||||||
| Altamira | 6297 (40%) | 100 (62%) | — | — | — | — | |||
| Anapu | 1112 (7.1%) | 7 (4.3%) | 0.40 | 0.17, 0.79 | 0.45 | 0.17, 0.99 | 0.069 | ||
| Brasil Novo | 769 (4.9%) | 5 (3.1%) | 0.41 | 0.14, 0.91 | 0.26 | 0.07, 0.73 | 0.021 | ||
| Medicilândia | 1505 (9.7%) | 4 (2.5%) | 0.17 | 0.05, 0.40 | 0.05 | 0.01, 0.17 | <0.001 | ||
| Pacajá | 1551 (10.0%) | 11 (6.8%) | 0.45 | 0.23, 0.80 | 0.36 | 0.15, 0.74 | 0.011 | ||
| Porto de Moz | 1138 (7.3%) | 16 (9.9%) | 0.89 | 0.50, 1.46 | 0.71 | 0.34, 1.37 | 0.33 | ||
| Senador José Porfírio | 622 (4.0%) | 6 (3.7%) | 0.61 | 0.24, 1.28 | 0.29 | 0.06, 0.91 | 0.068 | ||
| Uruará | 1205 (7.7%) | 8 (4.9%) | 0.42 | 0.19, 0.81 | 0.44 | 0.17, 0.98 | 0.060 | ||
| Vitória do Xingu | 1362 (8.8%) | 5 (3.1%) | 0.23 | 0.08, 0.51 | 0.11 | 0.02, 0.34 | <0.001 | ||
| Sex | 15,723 | <0.001 | |||||||
| Male | 7208 (46%) | 110 (68%) | — | — | — | — | |||
| Female | 8353 (54%) | 52 (32%) | 0.41 | 0.29, 0.56 | 0.45 | 0.30, 0.66 | <0.001 | ||
| Local case | 14,815 (95%) | 144 (89%) | 15,723 | 0.40 | 0.25, 0.68 | 0.001 | 1.26 | 0.42, 4.72 | 0.71 |
| Imported case | 221 (1.4%) | 21 (13%) | 15,723 | 10.3 | 6.25, 16.3 | <0.001 | 6.79 | 1.94, 26.0 | 0.004 |
| Fever | 9532 (61%) | 115 (71%) | 15,723 | 1.55 | 1.11, 2.20 | 0.010 | 1.22 | 0.80, 1.90 | 0.37 |
| Cough | 8724 (56%) | 116 (72%) | 15,723 | 1.98 | 1.41, 2.81 | <0.001 | 1.32 | 0.85, 2.07 | 0.23 |
| Emesis | 463 (3.0%) | 16 (9.9%) | 15,723 | 3.57 | 2.04, 5.85 | <0.001 | 6.00 | 2.91, 11.6 | <0.001 |
| Headache | 5637 (36%) | 16 (9.9%) | 15,723 | 0.19 | 0.11, 0.31 | <0.001 | 0.45 | 0.24, 0.81 | 0.011 |
| Runny nose | 1548 (9.9%) | 5 (3.1%) | 15,723 | 0.29 | 0.10, 0.63 | <0.001 | 1.00 | 0.32, 2.59 | >0.99 |
| Nasal congestion | 246 (1.6%) | 2 (1.2%) | 15,723 | 0.78 | 0.13, 2.45 | 0.715 | |||
| Sore throat | 6758 (43%) | 45 (28%) | 15,723 | 0.50 | 0.35, 0.70 | <0.001 | 0.48 | 0.31, 0.74 | 0.001 |
| Myalgia and arthralgia | 3642 (23%) | 15 (9.3%) | 15,723 | 0.33 | 0.19, 0.55 | <0.001 | 0.71 | 0.38, 1.27 | 0.28 |
| Diarrhea | 1360 (8.7%) | 13 (8.0%) | 15,723 | 0.91 | 0.49, 1.55 | 0.745 | |||
| Chills | 193 (1.2%) | 4 (2.5%) | 15,723 | 2.02 | 0.62, 4.83 | 0.216 | 5.14 | 1.14, 16.2 | 0.013 |
| Adynamia | 584 (3.8%) | 6 (3.7%) | 15,723 | 0.99 | 0.39, 2.05 | 0.974 | |||
| Odynophagy | 70 (0.4%) | 0 (0%) | 15,723 | 0.00 | 0.00, 0.23 | 0.228 | 0.00 | 0.00, 0.00 | 0.98 |
| Anosmia | 3166 (21%) | 5 (3.4%) | 15,303 | 0.13 | 0.05, 0.29 | <0.001 | 0.56 | 0.13, 1.90 | 0.39 |
| Ageusia | 2950 (19%) | 5 (3.4%) | 15,303 | 0.14 | 0.05, 0.32 | <0.001 | 0.43 | 0.11, 1.46 | 0.21 |
| Dyspnea | 4097 (26%) | 136 (84%) | 15,723 | 14.6 | 9.78, 22.8 | <0.001 | 10.2 | 6.36, 17.0 | <0.001 |
| Conjunctivitis | 27 (0.2%) | 0 (0%) | 15,723 | 0.00 | 0.00, 33.0 | 0.454 | |||
| Diabetes | 272 (1.7%) | 42 (26%) | 15,723 | 19.7 | 13.4, 28.3 | <0.001 | 4.92 | 2.91, 8.18 | <0.001 |
| Immunodeficiency | 116 (0.7%) | 5 (3.1%) | 15,723 | 4.24 | 1.48, 9.51 | 0.010 | 0.71 | 0.21, 1.96 | 0.55 |
| Heart diseases | 399 (2.6%) | 42 (26%) | 15,723 | 13.3 | 9.14, 19.0 | <0.001 | 3.94 | 2.32, 6.58 | <0.001 |
| Lung diseases | 65 (0.4%) | 3 (1.9%) | 15,723 | 4.50 | 1.09, 12.3 | 0.039 | 2.42 | 0.48, 8.59 | 0.22 |
| Neurological diseases | 1 (<0.1%) | 2 (1.2%) | 15,723 | 194 | 18.5, 4,198 | <0.001 | 22.9 | 0.11, 3,655 | 0.37 |
| Kidney diseases | 24 (0.2%) | 4 (2.5%) | 15,723 | 16.4 | 4.78, 43.0 | <0.001 | 1.32 | 0.14, 7.91 | 0.78 |
| Obesity | 12 (<0.1%) | 9 (5.6%) | 15,723 | 76.2 | 30.7, 183 | <0.001 | 48.0 | 14.5, 167 | <0.001 |
| Asthma | 30 (0.2%) | 0 (0%) | 15,723 | 0.00 | 0.00, 9.15 | 0.430 | |||
| Blood diseases | 3 (<0.1%) | 0 (0%) | 15,723 | 0.00 | 0.803 | ||||
| Liver diseases | 3 (<0.1%) | 0 (0%) | 15,723 | 0.00 | 0.803 |
| Characteristic | Medical Ward N = 414 1 | ICU N = 162 1 | N | OR 2 | 95% CI 2 | p-Value | aOR 3 | 95% CI 3 | p-Value |
|---|---|---|---|---|---|---|---|---|---|
| Age | 64 (46, 77) | 66 (50, 75) | 576 | 1.00 | 1.00, 1.01 | 0.378 | |||
| Municipality | 576 | 0.008 | |||||||
| Altamira | 194 (47%) | 100 (62%) | — | — | — | — | |||
| Anapu | 18 (4.3%) | 7 (4.3%) | 0.75 | 0.29, 1.79 | 0.48 | 0.15, 1.32 | 0.18 | ||
| Brasil Novo | 38 (9.2%) | 5 (3.1%) | 0.26 | 0.09, 0.61 | 0.18 | 0.05, 0.50 | 0.002 | ||
| Medicilândia | 28 (6.8%) | 4 (2.5%) | 0.28 | 0.08, 0.73 | 0.13 | 0.03, 0.44 | 0.003 | ||
| Pacajá | 38 (9.2%) | 11 (6.8%) | 0.56 | 0.26, 1.11 | 0.28 | 0.10, 0.67 | 0.007 | ||
| Porto de Moz | 44 (11%) | 16 (9.9%) | 0.71 | 0.37, 1.29 | 0.56 | 0.26, 1.15 | 0.13 | ||
| Senador José Porfírio | 22 (5.3%) | 6 (3.7%) | 0.53 | 0.19, 1.27 | 0.28 | 0.06, 0.91 | 0.056 | ||
| Uruará | 11 (2.7%) | 8 (4.9%) | 1.41 | 0.53, 3.60 | 1.83 | 0.65, 5.03 | 0.24 | ||
| Vitória do Xingu | 21 (5.1%) | 5 (3.1%) | 0.46 | 0.15, 1.17 | 0.24 | 0.05, 0.82 | 0.038 | ||
| Sex | 576 | 0.140 | |||||||
| Male | 254 (61%) | 110 (68%) | — | — | — | — | |||
| Female | 160 (39%) | 52 (32%) | 0.75 | 0.51, 1.10 | 0.59 | 0.37, 0.92 | 0.021 | ||
| Local case | 377 (91%) | 144 (89%) | 576 | 0.79 | 0.44, 1.45 | 0.431 | |||
| Imported case | 21 (5.1%) | 21 (13%) | 576 | 2.79 | 1.47, 5.28 | 0.002 | 3.00 | 1.32, 6.85 | 0.009 |
| Fever | 293 (71%) | 115 (71%) | 576 | 1.01 | 0.68, 1.52 | 0.959 | |||
| Cough | 315 (76%) | 116 (72%) | 576 | 0.79 | 0.53, 1.20 | 0.269 | |||
| Emesis | 32 (7.7%) | 16 (9.9%) | 576 | 1.31 | 0.68, 2.42 | 0.409 | |||
| Headache | 50 (12%) | 16 (9.9%) | 576 | 0.80 | 0.43, 1.42 | 0.450 | |||
| Runny nose | 10 (2.4%) | 5 (3.1%) | 576 | 1.29 | 0.40, 3.68 | 0.655 | |||
| Nasal congestion | 6 (1.4%) | 2 (1.2%) | 576 | 0.85 | 0.12, 3.73 | 0.841 | |||
| Sore throat | 112 (27%) | 45 (28%) | 576 | 1.04 | 0.69, 1.55 | 0.861 | |||
| Myalgia and arthralgia | 38 (9.2%) | 15 (9.3%) | 576 | 1.01 | 0.52, 1.85 | 0.976 | |||
| Diarrhea | 38 (9.2%) | 13 (8.0%) | 576 | 0.86 | 0.43, 1.63 | 0.658 | |||
| Chills | 1 (0.2%) | 4 (2.5%) | 576 | 10.5 | 1.53, 205 | 0.015 | 22.8 | 2.18, 554 | 0.016 |
| Adynamia | 20 (4.8%) | 6 (3.7%) | 576 | 0.76 | 0.27, 1.82 | 0.550 | |||
| Odynophagy | 0 (0%) | 0 (0%) | |||||||
| Anosmia | 33 (9.1%) | 5 (3.4%) | 512 | 0.35 | 0.12, 0.83 | 0.016 | 0.35 | 0.07, 1.53 | 0.19 |
| Ageusia | 29 (8.0%) | 5 (3.4%) | 512 | 0.40 | 0.13, 0.97 | 0.042 | 1.09 | 0.22, 5.27 | 0.92 |
| Dyspnea | 290 (70%) | 136 (84%) | 576 | 2.24 | 1.42, 3.64 | <0.001 | 2.27 | 1.34, 3.98 | 0.003 |
| Conjunctivitis | 0 (0%) | 0 (0%) | |||||||
| Diabetes | 67 (16%) | 42 (26%) | 576 | 1.81 | 1.16, 2.80 | 0.009 | 1.78 | 1.04, 3.04 | 0.034 |
| Immunodeficiency | 4 (1.0%) | 5 (3.1%) | 576 | 3.26 | 0.85, 13.3 | 0.082 | 4.50 | 0.91, 27.3 | 0.074 |
| Heart diseases | 73 (18%) | 42 (26%) | 576 | 1.63 | 1.06, 2.51 | 0.028 | 1.63 | 0.94, 2.81 | 0.079 |
| Lung diseases | 1 (0.2%) | 3 (1.9%) | 576 | 7.79 | 0.99, 158 | 0.051 | 3.50 | 0.42, 72.7 | 0.29 |
| Neurological diseases | 1 (0.2%) | 2 (1.2%) | 576 | 5.16 | 0.49, 112 | 0.165 | 2.12 | 0.16, 50.9 | 0.57 |
| Kidney diseases | 9 (2.2%) | 4 (2.5%) | 576 | 1.14 | 0.31, 3.55 | 0.832 | |||
| Obesity | 12 (2.9%) | 9 (5.6%) | 576 | 1.97 | 0.79, 4.75 | 0.141 | 2.32 | 0.81, 6.79 | 0.12 |
| Asthma | 2 (0.5%) | 0 (0%) | 576 | 0.00 | 0.250 | 0.00 | 0.99 | ||
| Blood diseases | 2 (0.5%) | 0 (0%) | 576 | 0.00 | 0.250 | 0.00 | 0.99 | ||
| Liver diseases | 2 (0.5%) | 0 (0%) | 576 | 0.00 | 0.250 | 0.00 | 0.99 |
| Characteristic | Recovered N = 15,779 1 | Dead N = 359 1 | N | OR 2 | 95% CI 2 | p-Value | aOR 3 | 95% CI 3 | p-Value |
|---|---|---|---|---|---|---|---|---|---|
| Age | 38 (27, 50) | 70 (58, 80) | 16,138 | 1.09 | 1.08, 1.10 | <0.001 | 1.07 | 1.06, 1.08 | <0.001 |
| Municipality | 16,138 | <0.001 | |||||||
| Altamira | 6403 (41%) | 188 (52%) | — | — | 1.24 | 0.63, 2.64 | 0.56 | ||
| Anapu | 1112 (7.0%) | 25 (7.0%) | 0.77 | 0.49, 1.14 | 2.76 | 1.21, 6.56 | 0.018 | ||
| Brasil Novo | 790 (5.0%) | 22 (6.1%) | 0.95 | 0.59, 1.45 | 1.15 | 0.46, 2.93 | 0.77 | ||
| Medicilândia | 1517 (9.6%) | 20 (5.6%) | 0.45 | 0.27, 0.70 | 1.39 | 0.57, 3.49 | 0.48 | ||
| Pacajá | 1581 (10%) | 20 (5.6%) | 0.43 | 0.26, 0.67 | 0.37 | 0.14, 0.99 | 0.045 | ||
| Porto de Moz | 1170 (7.4%) | 28 (7.8%) | 0.82 | 0.53, 1.20 | 0.65 | 0.26, 1.65 | 0.36 | ||
| Senador José Porfírio | 635 (4.0%) | 15 (4.2%) | 0.80 | 0.45, 1.32 | 0.55 | 0.17, 1.72 | 0.31 | ||
| Uruará | 1205 (7.6%) | 19 (5.3%) | 0.54 | 0.32, 0.84 | 1.61 | 0.65, 4.09 | 0.30 | ||
| Vitória do Xingu | 1366 (8.7%) | 22 (6.1%) | 0.55 | 0.34, 0.84 | — | — | |||
| Sex | 16,138 | <0.001 | |||||||
| Male | 7358 (47%) | 215 (60%) | — | — | — | — | |||
| Female | 8421 (53%) | 144 (40%) | 0.59 | 0.47, 0.72 | 1.05 | 0.76, 1.46 | 0.77 | ||
| Local case | 14,998 (95%) | 339 (94%) | 16,138 | 0.88 | 0.57, 1.44 | 0.599 | |||
| Imported case | 242 (1.5%) | 21 (5.8%) | 16,137 | <0.001 | 0.29 | 0.11, 0.75 | 0.013 | ||
| Fever | 9687 (61%) | 254 (71%) | 16,138 | 1.52 | 1.21, 1.92 | <0.001 | 1.54 | 1.07, 2.24 | 0.022 |
| Cough | 8901 (56%) | 255 (71%) | 16,138 | 1.89 | 1.51, 2.39 | <0.001 | 0.95 | 0.66, 1.38 | 0.78 |
| Emese | 489 (3.1%) | 22 (6.1%) | 16,137 | 2.04 | 1.28, 3.10 | 0.004 | 1.34 | 0.62, 2.77 | 0.44 |
| Headache | 5661 (36%) | 43 (12%) | 16,138 | 0.24 | 0.17, 0.33 | <0.001 | 0.81 | 0.51, 1.28 | 0.38 |
| Runny nose | 1550 (9.8%) | 13 (3.6%) | 16,137 | 0.34 | 0.19, 0.58 | <0.001 | 1.44 | 0.67, 2.85 | 0.32 |
| Nasal congestion | 248 (1.6%) | 6 (1.7%) | 16,137 | 1.06 | 0.42, 2.20 | 0.882 | |||
| Sore throat | 6817 (43%) | 98 (27%) | 16,137 | 0.49 | 0.39, 0.62 | <0.001 | 0.57 | 0.39, 0.82 | 0.003 |
| Myalgia and arthralgia | 3662 (23%) | 34 (9.5%) | 16,138 | 0.35 | 0.24, 0.49 | <0.001 | 0.79 | 0.47, 1.30 | 0.36 |
| Diarrhea | 1385 (8.8%) | 26 (7.2%) | 16,137 | 0.81 | 0.53, 1.19 | 0.295 | |||
| Chills | 195 (1.2%) | 3 (0.8%) | 16,137 | 0.67 | 0.17, 1.78 | 0.470 | |||
| Adynamia | 594 (3.8%) | 16 (4.5%) | 16,137 | 1.19 | 0.69, 1.92 | 0.508 | |||
| Odynophagy | 70 (0.4%) | 0 (0%) | 16,137 | 0.00 | 0.00, 0.11 | 0.076 | 0.00 | 0.98 | |
| Anosmia | 3193 (21%) | 11 (3.4%) | 15,666 | 0.13 | 0.07, 0.23 | <0.001 | 0.31 | 0.10, 0.89 | 0.035 |
| Ageusia | 2972 (19%) | 12 (3.7%) | 15,666 | 0.16 | 0.08, 0.27 | <0.001 | 0.86 | 0.28, 2.33 | 0.78 |
| Dyspnea | 4236 (27%) | 287 (80%) | 16,137 | 10.9 | 8.42, 14.2 | <0.001 | 3.66 | 2.57, 5.26 | <0.001 |
| Conjunctivitis | 27 (0.2%) | 0 (0%) | 16,137 | 0.00 | 0.00, 15.2 | 0.270 | |||
| Diabetes | 305 (1.9%) | 76 (21%) | 16,137 | 13.6 | 10.3, 17.9 | <0.001 | 1.01 | 0.60, 1.68 | 0.98 |
| Immunodeficiency | 120 (0.8%) | 5 (1.4%) | 16,137 | 1.84 | 0.65, 4.09 | 0.223 | 0.40 | 0.07, 1.58 | 0.25 |
| Heart diseases | 428 (2.7%) | 86 (24%) | 16,137 | 11.3 | 8.67, 14.6 | <0.001 | 2.05 | 1.26, 3.30 | 0.004 |
| Lung diseases | 66 (0.4%) | 3 (0.8%) | 16,137 | 2.01 | 0.49, 5.43 | 0.288 | |||
| Neurological diseases | 2 (<0.1%) | 2 (0.6%) | 16,137 | 44.2 | 5.29, 369 | 0.002 | 0.91 | 0.01, 110 | 0.98 |
| Kidney diseases | 28 (0.2%) | 9 (2.5%) | 16,137 | 14.5 | 6.40, 29.7 | <0.001 | 3.31 | 0.83, 12.1 | 0.079 |
| Obesity | 17 (0.1%) | 16 (4.5%) | 16,137 | 43.2 | 21.5, 86.7 | <0.001 | 2.76 | 0.86, 9.49 | 0.10 |
| Asthma | 30 (0.2%) | 2 (0.6%) | 16,137 | 2.94 | 0.47, 9.78 | 0.204 | 3.17 | 0.33, 19.0 | 0.26 |
| Blood diseases | 3 (<0.1%) | 2 (0.6%) | 16,137 | 29.5 | 3.87, 178 | 0.003 | 14.3 | 0.23, 883 | 0.36 |
| Liver diseases | 3 (<0.1%) | 2 (0.6%) | 16,137 | 29.5 | 3.87, 178 | 0.003 | |||
| Clinical management | 16,137 | <0.001 | |||||||
| Home care | 15,472 (98%) | 89 (25%) | — | — | — | — | |||
| Medical ward | 274 (1.7%) | 140 (39%) | 88.8 | 66.5, 119 | 21.1 | 14.5, 30.8 | <0.001 | ||
| ICU | 32 (0.2%) | 130 (36%) | 706 | 461, 1112 | 258 | 146, 474 | <0.001 | ||
| Unknown | 1 | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Figueiredo, E.R.L.; Affonso, M.V.d.G.; Jacomel, R.J.; Gomes, F.d.C.; Gonçalves, N.V.; Miranda, C.d.S.C.; Silva, M.C.F.d.; da Silva-Júnior, A.F.; Melo-Neto, J.S.d. COVID-19 in the Eastern Brazilian Amazon: Incidence, Clinical Management, and Mortality by Social Determinants of Health, Symptomatology, and Comorbidities in the Xingu Health Region. Int. J. Environ. Res. Public Health 2023, 20, 4639. https://doi.org/10.3390/ijerph20054639
Figueiredo ERL, Affonso MVdG, Jacomel RJ, Gomes FdC, Gonçalves NV, Miranda CdSC, Silva MCFd, da Silva-Júnior AF, Melo-Neto JSd. COVID-19 in the Eastern Brazilian Amazon: Incidence, Clinical Management, and Mortality by Social Determinants of Health, Symptomatology, and Comorbidities in the Xingu Health Region. International Journal of Environmental Research and Public Health. 2023; 20(5):4639. https://doi.org/10.3390/ijerph20054639
Chicago/Turabian StyleFigueiredo, Eric Renato Lima, Márcio Vinicius de Gouveia Affonso, Rodrigo Januario Jacomel, Fabiana de Campos Gomes, Nelson Veiga Gonçalves, Claudia do Socorro Carvalho Miranda, Márcia Cristina Freitas da Silva, Ademir Ferreira da Silva-Júnior, and João Simão de Melo-Neto. 2023. "COVID-19 in the Eastern Brazilian Amazon: Incidence, Clinical Management, and Mortality by Social Determinants of Health, Symptomatology, and Comorbidities in the Xingu Health Region" International Journal of Environmental Research and Public Health 20, no. 5: 4639. https://doi.org/10.3390/ijerph20054639






