Movement Behavior and Health Outcomes among Sedentary Adults: A Cross-Sectional Study
Abstract
1. Introduction
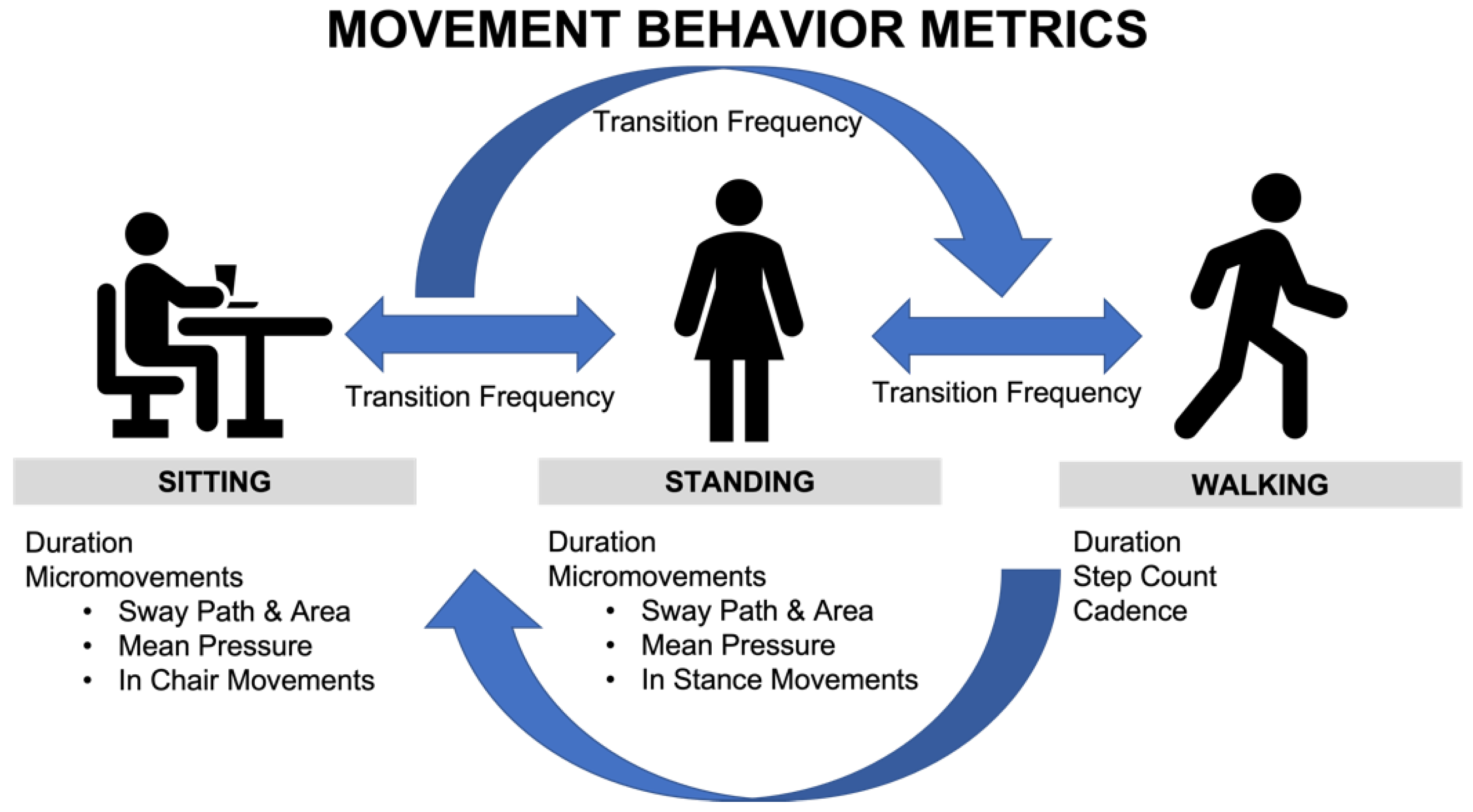
A Comprehensive Movement Behavior Model
2. Methods
2.1. Participants
2.2. Procedure
2.3. Measures
2.4. Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Owen, N.; Healy, G.N.; Dempsey, P.C.; Salmon, J.; Timperio, A.; Clark, B.K.; Goode, A.D.; Koorts, H.; Ridgers, N.D.; Hadgraft, N.T.; et al. Sedentary Behavior and Public Health: Integrating the Evidence and Identifying Potential Solutions. Annu. Rev. Public Health 2020, 41, 265–287. [Google Scholar] [CrossRef] [PubMed]
- Hall, G.; Laddu, D.R.; Phillips, S.A.; Lavie, C.J.; Arena, R. A Tale of Two Pandemics: How Will COVID-19 and Global Trends in Physical Inactivity and Sedentary Behavior Affect One Another? Prog. Cardiovasc. Dis. 2021, 64, 108–110. [Google Scholar] [CrossRef]
- Ding, D.; Lawson, K.D.; Kolbe-Alexander, T.L.; Finkelstein, E.A.; Katzmarzyk, P.T.; van Mechelen, W.; Pratt, M. The Economic Burden of Physical Inactivity: A Global Analysis of Major Non-Communicable Diseases. Lancet 2016, 388, 1311–1324. [Google Scholar] [CrossRef] [PubMed]
- Jans, M.P.; Proper, K.I.; Hildebrandt, V.H. Sedentary Behavior in Dutch Workers: Differences between Occupations and Business Sectors. Am. J. Prev. Med. 2007, 33, 450–454. [Google Scholar] [CrossRef]
- Saidj, M.; Menai, M.; Charreire, H.; Weber, C.; Enaux, C.; Aadahl, M.; Kesse-Guyot, E.; Hercberg, S.; Simon, C.; Oppert, J.-M. Descriptive Study of Sedentary Behaviours in 35,444 French Working Adults: Cross-Sectional Findings from the ACTI-Cités Study. BMC Public Health 2015, 15, 379. [Google Scholar] [CrossRef] [PubMed]
- Hadgraft, N.T.; Lynch, B.M.; Clark, B.K.; Healy, G.N.; Owen, N.; Dunstan, D.W. Excessive Sitting at Work and at Home: Correlates of Occupational Sitting and TV Viewing Time in Working Adults. BMC Public Health 2015, 15, 899. [Google Scholar] [CrossRef]
- Bontrup, C.; Taylor, W.R.; Fliesser, M.; Visscher, R.; Green, T.; Wippert, P.-M.; Zemp, R. Low Back Pain and Its Relationship with Sitting Behaviour among Sedentary Office Workers. Appl. Ergon. 2019, 81, 102894. [Google Scholar] [CrossRef]
- Genin, P.M.; Dessenne, P.; Finaud, J.; Pereira, B.; Dutheil, F.; Thivel, D.; Duclos, M. Effect of Work-Related Sedentary Time on Overall Health Profile in Active vs. Inactive Office Workers. Front. Public Health 2018, 6, 279. [Google Scholar] [CrossRef]
- Mann, S.; Hamid Hamad, A.; Kumbhare, D. The Problem of Sedentary Behaviour in the Office Workspace: A Structured Exercise Program for Primary Prevention. J. Nov. Physiother. 2018, 8, 392. [Google Scholar] [CrossRef]
- Parry, S.; Straker, L. The Contribution of Office Work to Sedentary Behaviour Associated Risk. BMC Public Health 2013, 13, 296. [Google Scholar] [CrossRef]
- Agarwal, S.; Steinmaus, C.; Harris-Adamson, C. Sit-Stand Workstations and Impact on Low Back Discomfort: A Systematic Review and Meta-Analysis. Ergonomics 2018, 61, 538–552. [Google Scholar] [CrossRef] [PubMed]
- Foley, B.; Engelen, L.; Gale, J.; Bauman, A.; Mackey, M. Sedentary Behavior and Musculoskeletal Discomfort Are Reduced When Office Workers Trial an Activity-Based Work Environment. J. Occup. Environ. Med. 2016, 58, 924–931. [Google Scholar] [CrossRef]
- Karakolis, T.; Barrett, J.; Callaghan, J.P. A Comparison of Trunk Biomechanics, Musculoskeletal Discomfort and Productivity during Simulated Sit-Stand Office Work. Ergonomics 2016, 59, 1275–1287. [Google Scholar] [CrossRef]
- Marras, W.S.; Lavender, S.A.; Leurgans, S.E.; Fathallah, F.A.; Ferguson, S.A.; Allread, W.G.; Rajulu, S.L. Biomechanical Risk Factors for Occupationally Related Low Back Disorders. Ergonomics 1995, 38, 377–410. [Google Scholar] [CrossRef]
- Nachemson, A. Intravital Dynamic Pressure Measurements in Lumbar Discs: A Study of Common Movements, Maneuvers and Exercises. Scand. J. Rehabil. Med. 1970, 1, 1–40. [Google Scholar]
- Carson, V.; Wong, S.L.; Winkler, E.; Healy, G.N.; Colley, R.C.; Tremblay, M.S. Patterns of Sedentary Time and Cardiometabolic Risk among Canadian Adults. Prev. Med. 2014, 65, 23–27. [Google Scholar] [CrossRef] [PubMed]
- Carter, S.; Hartman, Y.; Holder, S.; Thijssen, D.H.; Hopkins, N.D. Sedentary Behavior and Cardiovascular Disease Risk: Mediating Mechanisms. Exerc. Sport Sci. Rev. 2017, 45, 80–86. [Google Scholar] [CrossRef]
- Healy, G.N.; Dunstan, D.W.; Salmon, J.; Shaw, J.E.; Zimmet, P.Z.; Owen, N. Television Time and Continuous Metabolic Risk in Physically Active Adults. Med. Sci. Sports Exerc. 2008, 40, 639–645. [Google Scholar] [CrossRef]
- Henson, J.; Yates, T.; Biddle, S.J.H.; Edwardson, C.L.; Khunti, K.; Wilmot, E.G.; Gray, L.J.; Gorely, T.; Nimmo, M.A.; Davies, M.J. Associations of Objectively Measured Sedentary Behaviour and Physical Activity with Markers of Cardiometabolic Health. Diabetologia 2013, 56, 1012–1020. [Google Scholar] [CrossRef]
- Huynh, Q.L.; Blizzard, C.L.; Sharman, J.E.; Magnussen, C.G.; Dwyer, T.; Venn, A.J. The Cross-Sectional Association of Sitting Time with Carotid Artery Stiffness in Young Adults. BMJ Open 2014, 4, e004384. [Google Scholar] [CrossRef]
- Sugiyama, T.; Hadgraft, N.; Clark, B.K.; Dunstan, D.W.; Owen, N. Sitting at Work & Waist Circumference—A Cross-Sectional Study of Australian Workers. Prev. Med. 2020, 141, 106243. [Google Scholar] [CrossRef]
- Morishima, T.; Restaino, R.M.; Walsh, L.K.; Kanaley, J.A.; Fadel, P.J.; Padilla, J. Prolonged Sitting-Induced Leg Endothelial Dysfunction Is Prevented by Fidgeting. Am. J. Physiol.-Heart Circ. Physiol. 2016, 311, H177–H182. [Google Scholar] [CrossRef] [PubMed]
- Padilla, J.; Fadel, P.J. Prolonged Sitting Leg Vasculopathy: Contributing Factors and Clinical Implications. Am. J. Physiol.-Heart Circ. Physiol. 2017, 313, H722–H728. [Google Scholar] [CrossRef] [PubMed]
- Park, H.J.; Park, C.H.; Chang, Y.; Ryu, S. Sitting Time, Physical Activity and the Risk of Lower Urinary Tract Symptoms: A Cohort Study. BJU Int. 2018, 122, 293–299. [Google Scholar] [CrossRef] [PubMed]
- Restaino, R.M.; Walsh, L.K.; Morishima, T.; Vranish, J.R.; Martinez-Lemus, L.A.; Fadel, P.J.; Padilla, J. Endothelial Dysfunction Following Prolonged Sitting Is Mediated by a Reduction in Shear Stress. Am. J. Physiol.-Heart Circ. Physiol. 2016, 310, H648–H653. [Google Scholar] [CrossRef]
- Callaghan, J.P.; McGill, S.M. Low Back Joint Loading and Kinematics during Standing and Unsupported Sitting. Ergonomics 2001, 44, 280–294. [Google Scholar] [CrossRef]
- Huang, M.; Hajizadeh, K.; Gibson, I.; Lee, T. Analysis of Compressive Load on Intervertebral Joint in Standing and Sitting Postures. Technol. Health Care 2016, 24, 215–223. [Google Scholar] [CrossRef]
- van der Ploeg, H.P.; Chey, T.; Ding, D.; Chau, J.Y.; Stamatakis, E.; Bauman, A.E. Standing Time and All-Cause Mortality in a Large Cohort of Australian Adults. Prev. Med. 2014, 69, 187–191. [Google Scholar] [CrossRef]
- Katzmarzyk, P.T. Standing and Mortality in a Prospective Cohort of Canadian Adults. Med. Sci. Sports Exerc. 2014, 46, 940–946. [Google Scholar] [CrossRef]
- Buckley, J.P.; Hedge, A.; Yates, T.; Copeland, R.J.; Loosemore, M.; Hamer, M.; Bradley, G.; Dunstan, D.W. The Sedentary Office: An Expert Statement on the Growing Case for Change towards Better Health and Productivity. Br. J. Sports Med. 2015, 49, 1357–1362. [Google Scholar] [CrossRef]
- Tüchsen, F.; Krause, N.; Hannerz, H.; Burr, H.; Kristensen, T.S. Standing at Work and Varicose Veins. Scand. J. Work. Environ. Health 2000, 26, 414–420. [Google Scholar] [CrossRef] [PubMed]
- Krause, N.; Lynch, J.W.; Kaplan, G.A.; Cohen, R.D.; Salonen, R.; Salonen, J.T. Standing at Work and Progression of Carotid Atherosclerosis. Scand. J. Work. Environ. Health 2000, 26, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Smith, P.; Ma, H.; Glazier, R.H.; Gilbert-Ouimet, M.; Mustard, C. The Relationship Between Occupational Standing and Sitting and Incident Heart Disease Over a 12-Year Period in Ontario, Canada. Am. J. Epidemiol. 2018, 187, 27–33. [Google Scholar] [CrossRef]
- Waters, T.R.; Dick, R.B. Evidence of Health Risks Associated with Prolonged Standing at Work and Intervention Effectiveness. Rehabil. Nurs. J. 2015, 40, 148–165. [Google Scholar] [CrossRef] [PubMed]
- Chester, M.R.; Rys, M.J.; Konz, S.A. Leg Swelling, Comfort and Fatigue When Sitting, Standing, and Sit/Standing. Int. J. Ind. Ergon. 2002, 29, 289–296. [Google Scholar] [CrossRef]
- Balasubramanian, V.; Adalarasu, K.; Regulapati, R. Comparing Dynamic and Stationary Standing Postures in an Assembly Task. Int. J. Ind. Ergon. 2009, 39, 649–654. [Google Scholar] [CrossRef]
- Andersen, J.H.; Haahr, J.P.; Frost, P. Risk Factors for More Severe Regional Musculoskeletal Symptoms: A Two-Year Prospective Study of a General Working Population. Arthritis Rheum. 2007, 56, 1355–1364. [Google Scholar] [CrossRef]
- Baker, R.; Coenen, P.; Howie, E.; Lee, J.; Williamson, A.; Straker, L. A Detailed Description of the Short-Term Musculoskeletal and Cognitive Effects of Prolonged Standing for Office Computer Work. Ergonomics 2018, 61, 877–890. [Google Scholar] [CrossRef]
- Genaidy, A.M.; Al-Shedi, A.A.; Karwowski, W. Postural Stress Analysis in Industry. Appl. Ergon. 1994, 25, 77–87. [Google Scholar] [CrossRef]
- Liao, M.H.; Drury, C.G. Posture, Discomfort and Performance in a Vdt Task. Ergonomics 2000, 43, 345–359. [Google Scholar] [CrossRef]
- McLean, L.; Tingley, M.; Scott, R.N.; Rickards, J. Computer Terminal Work and the Benefit of Microbreaks. Appl. Ergon. 2001, 32, 225–237. [Google Scholar] [CrossRef] [PubMed]
- Arippa, F.; Leban, B.; Pau, M. Postural Strategies of Bus Drivers during a Regular Work Shift in Urban Area: A Pilot Study. Proc. Hum. Factors Ergon. Soc. Annu. Meet. 2019, 63, 967–971. [Google Scholar] [CrossRef]
- Arippa, F.; Nguyen, A.; Pau, M.; Harris-Adamson, C. Postural Strategies among Office Workers during a Prolonged Sitting Bout. Appl. Ergon. 2022, 102, 103723. [Google Scholar] [CrossRef] [PubMed]
- Sammonds, G.M.; Mansfield, N.J.; Fray, M. Improving Long Term Driving Comfort by Taking Breaks—How Break Activity Affects Effectiveness. Appl. Ergon. 2017, 65, 81–89. [Google Scholar] [CrossRef] [PubMed]
- Bull, F.C.; Al-Ansari, S.S.; Biddle, S.; Borodulin, K.; Buman, M.P.; Cardon, G.; Carty, C.; Chaput, J.-P.; Chastin, S.; Chou, R.; et al. World Health Organization 2020 Guidelines on Physical Activity and Sedentary Behaviour. Br. J. Sports Med. 2020, 54, 1451. [Google Scholar] [CrossRef]
- Sitthipornvorakul, E.; Janwantanakul, P.; Lohsoonthorn, V. The Effect of Daily Walking Steps on Preventing Neck and Low Back Pain in Sedentary Workers: A 1-Year Prospective Cohort Study. Eur. Spine J. 2015, 24, 417–424. [Google Scholar] [CrossRef]
- Sitthipornvorakul, E.; Klinsophon, T.; Sihawong, R.; Janwantanakul, P. The Effects of Walking Intervention in Patients with Chronic Low Back Pain: A Meta-Analysis of Randomized Controlled Trials. Musculoskelet. Sci. Pract. 2018, 34, 38–46. [Google Scholar] [CrossRef]
- Gallagher, K.M.; Payne, M.; Daniels, B.; Caldwell, A.R.; Ganio, M.S. Walking Breaks Can Reduce Prolonged Standing Induced Low Back Pain. Hum. Mov. Sci. 2019, 66, 31–37. [Google Scholar] [CrossRef]
- Levine, J.A.; Schleusner, S.J.; Jensen, M.D. Energy Expenditure of Nonexercise Activity. Am. J. Clin. Nutr. 2000, 72, 1451–1454. [Google Scholar] [CrossRef]
- Healy, G.N.; Dunstan, D.W.; Salmon, J.; Cerin, E.; Shaw, J.E.; Zimmet, P.Z.; Owen, N. Breaks in Sedentary Time: Beneficial Associations with Metabolic Risk. Diabetes Care 2008, 31, 661–666. [Google Scholar] [CrossRef] [PubMed]
- Owen, N.; Healy, G.N.; Matthews, C.E.; Dunstan, D.W. Too Much Sitting: The Population-Health Science of Sedentary Behavior. Exerc. Sport Sci. Rev. 2010, 38, 105–113. [Google Scholar] [CrossRef] [PubMed]
- Bailey, D.P.; Locke, C.D. Breaking up Prolonged Sitting with Light-Intensity Walking Improves Postprandial Glycemia, but Breaking up Sitting with Standing Does Not. J. Sci. Med. Sport 2015, 18, 294–298. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.-P.; Lin, C.-C.; Chen, M.-M.; Lee, K.-C. Short-Term Efficacy of a “Sit Less, Walk More” Workplace Intervention on Improving Cardiometabolic Health and Work Productivity in Office Workers. J. Occup. Environ. Med. 2017, 59, 327–334. [Google Scholar] [CrossRef] [PubMed]
- Kar, G.; Hedge, A. Effects of a Sit-Stand-Walk Intervention on Musculoskeletal Discomfort, Productivity, and Perceived Physical and Mental Fatigue, for Computer-Based Work. Int. J. Ind. Ergon. 2020, 78, 102983. [Google Scholar] [CrossRef]
- Fenety, A.; Putnam, C.; Walker, J.M. In-Chair Movement: Validity, Reliability and Implications for Measuring Sitting Discomfort. Appl. Ergon. 2000, 31, 383–393. [Google Scholar] [CrossRef]
- Leban, B.; Fancello, G.; Fadda, P.; Pau, M. Changes in Trunk Sway of Quay Crane Operators during Work Shift: A Possible Marker for Fatigue? Appl. Ergon. 2017, 65, 105–111. [Google Scholar] [CrossRef]
- Sammonds, G.M.; Fray, M.; Mansfield, N.J. Effect of Long Term Driving on Driver Discomfort and Its Relationship with Seat Fidgets and Movements (SFMs). Appl. Ergon. 2017, 58, 119–127. [Google Scholar] [CrossRef] [PubMed]
- Hermann, S.; Bubb, H. Development of an Objective Measure to Quantify Automotive Discomfort over Time; IEEE: New York, NY, USA, 2007; pp. 2824–2830. [Google Scholar]
- Davis, K.G.; Kotowski, S.E. Postural Variability: An Effective Way to Reduce Musculoskeletal Discomfort in Office Work. Hum. Factors 2014, 56, 1249–1261. [Google Scholar] [CrossRef]
- Vergara, M.; Page, Á. Relationship between Comfort and Back Posture and Mobility in Sitting-Posture. Appl. Ergon. 2002, 33, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Aarås, A.; Horgen, G.; Ro, O. Work with the Visual Display Unit: Health Consequences. Int. J. Hum.–Comput. Interact. 2000, 12, 107–134. [Google Scholar] [CrossRef]
- Pynt, J.; Higgs, J.; Mackey, M. Seeking the Optimal Posture of the Seated Lumbar Spine. Physiother. Theory Pract. 2001, 17, 5–21. [Google Scholar] [CrossRef]
- Srinivasan, D.; Mathiassen, S.E. Motor Variability in Occupational Health and Performance. Clin. Biomech. 2012, 27, 979–993. [Google Scholar] [CrossRef]
- Cocate, P.G.; de Oliveira, A.; Hermsdorff, H.H.M.; Alfenas, R.d.C.G.; Amorim, P.R.S.; Longo, G.Z.; Peluzio, M.d.C.G.; Faria, F.R.; Natali, A.J. Benefits and Relationship of Steps Walked per Day to Cardiometabolic Risk Factor in Brazilian Middle-Aged Men. J. Sci. Med. Sport 2014, 17, 283–287. [Google Scholar] [CrossRef]
- Duvivier, B.M.F.M.; Schaper, N.C.; Koster, A.; van Kan, L.; Peters, H.P.F.; Adam, J.J.; Giesbrecht, T.; Kornips, E.; Hulsbosch, M.; Willems, P.; et al. Benefits of Substituting Sitting with Standing and Walking in Free-Living Conditions for Cardiometabolic Risk Markers, Cognition and Mood in Overweight Adults. Front. Physiol. 2017, 8, 353. [Google Scholar] [CrossRef]
- Pulsford, R.M.; Blackwell, J.; Hillsdon, M.; Kos, K. Intermittent Walking, but Not Standing, Improves Postprandial Insulin and Glucose Relative to Sustained Sitting: A Randomised Cross-over Study in Inactive Middle-Aged Men. J. Sci. Med. Sport 2017, 20, 278–283. [Google Scholar] [CrossRef]
- Chastin, S.F.M.; Egerton, T.; Leask, C.; Stamatakis, E. Meta-Analysis of the Relationship between Breaks in Sedentary Behavior and Cardiometabolic Health. Obesity 2015, 23, 1800–1810. [Google Scholar] [CrossRef]
- Callaghan, J.P.; De Carvalho, D.; Gallagher, K.; Karakolis, T.; Nelson-Wong, E. Is Standing the Solution to Sedentary Office Work? Ergon. Des. 2015, 23, 20–24. [Google Scholar] [CrossRef]
- Davis, K.G.; Kotowski, S.E.; Sharma, B.; Herrmann, D.; Krishnan, A.P. Combating the Effects of Sedentary Work: Postural Variability Reduces Musculoskeletal Discomfort. Proc. Hum. Factors Ergon. Soc. Annu. Meet. 2009, 53, 884–886. [Google Scholar] [CrossRef]
- Ferguson, T.; Rowlands, A.V.; Olds, T.; Maher, C. The Validity of Consumer-Level, Activity Monitors in Healthy Adults Worn in Free-Living Conditions: A Cross-Sectional Study. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 42. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Waist Circumference and Waist-Hip Ratio: Report of a WHO Expert Consultation, Geneva, Switzerland, 8–11 December 2008; World Health Organization: Geneva, Switzerland, 2011. [Google Scholar]
- Gelber, R.P.; Gaziano, J.M.; Orav, E.J.; Manson, J.E.; Buring, J.E.; Kurth, T. Measures of Obesity and Cardiovascular Risk Among Men and Women. J. Am. Coll. Cardiol. 2008, 52, 605–615. [Google Scholar] [CrossRef] [PubMed]
- Laukkanen, J.A.; Zaccardi, F.; Khan, H.; Kurl, S.; Jae, S.Y.; Rauramaa, R. Long-Term Change in Cardiorespiratory Fitness and All-Cause Mortality: A Population-Based Follow-up Study. Mayo Clin. Proc. 2016, 91, 1183–1188. [Google Scholar] [CrossRef] [PubMed]
- DeMers, D.; Wachs, D. Physiology, Mean Arterial Pressure. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Zheng, L.; Sun, Z.; Li, J.; Zhang, R.; Zhang, X.; Liu, S.; Li, J.; Xu, C.; Hu, D.; Sun, Y. Pulse Pressure and Mean Arterial Pressure in Relation to Ischemic Stroke Among Patients With Uncontrolled Hypertension in Rural Areas of China. Stroke 2008, 39, 1932–1937. [Google Scholar] [CrossRef] [PubMed]
- Akoglu, H. User’s Guide to Correlation Coefficients. Turk. J. Emerg. Med. 2018, 18, 91–93. [Google Scholar] [CrossRef] [PubMed]
- Chambers, A.J.; Robertson, M.M.; Baker, N.A. The Effect of Sit-Stand Desks on Office Worker Behavioral and Health Outcomes: A Scoping Review. Appl. Ergon. 2019, 78, 37–53. [Google Scholar] [CrossRef]
- Robertson, M.M.; Ciriello, V.M.; Garabet, A.M. Office Ergonomics Training and a Sit-Stand Workstation: Effects on Musculoskeletal and Visual Symptoms and Performance of Office Workers. Appl. Ergon. 2013, 44, 73–85. [Google Scholar] [CrossRef]
- Fewster, K.M.; Gallagher, K.M.; Howarth, S.H.; Callaghan, J.P. Low Back Pain Development Differentially Influences Centre of Pressure Regularity Following Prolonged Standing. Gait Posture 2020, 78, e1–e6. [Google Scholar] [CrossRef]
- Sorensen, C.J.; Norton, B.J.; Callaghan, J.P.; Hwang, C.T.; Van Dillen, L.R. Is Lumbar Lordosis Related to Low Back Pain Development during Prolonged Standing? Man. Ther. 2015, 20, 553–557. [Google Scholar] [CrossRef]
- Gregory, D.E.; Callaghan, J.P. Prolonged Standing as a Precursor for the Development of Low Back Discomfort: An Investigation of Possible Mechanisms. Gait Posture 2008, 28, 86–92. [Google Scholar] [CrossRef]
- Nelson-Wong, E.; Callaghan, J.P. Is Muscle Co-Activation a Predisposing Factor for Low Back Pain Development during Standing? A Multifactorial Approach for Early Identification of at-Risk Individuals. J. Electromyogr. Kinesiol. 2010, 20, 256–263. [Google Scholar] [CrossRef]
- Nelson-Wong, E.; Gregory, D.E.; Winter, D.A.; Callaghan, J.P. Gluteus Medius Muscle Activation Patterns as a Predictor of Low Back Pain during Standing. Clin. Biomech. 2008, 23, 545–553. [Google Scholar] [CrossRef]
- Marshall, P.W.M.; Patel, H.; Callaghan, J.P. Gluteus Medius Strength, Endurance, and Co-Activation in the Development of Low Back Pain during Prolonged Standing. Hum. Mov. Sci. 2011, 30, 63–73. [Google Scholar] [CrossRef]
- Gallagher, K.M.; Callaghan, J.P. Early Static Standing Is Associated with Prolonged Standing Induced Low Back Pain. Hum. Mov. Sci. 2015, 44, 111–121. [Google Scholar] [CrossRef]
- Viggiani, D.; Callaghan, J.P. A Hip Abduction Exercise Prior to Prolonged Standing Increased Movement While Reducing Cocontraction and Low Back Pain Perception in Those Initially Reporting Low Back Pain. J. Electromyogr. Kinesiol. 2016, 31, 63–71. [Google Scholar] [CrossRef] [PubMed]
- Nelson-Wong, E.; Gallagher, K.; Johnson, E.; Antonioli, C.; Ferguson, A.; Harris, S.; Johnson, H.; Miller, J.B. Increasing Standing Tolerance in Office Workers with Standing-Induced Back Pain. Ergonomics 2020, 63, 804–817. [Google Scholar] [CrossRef]
- Healy, G.N.; Winkler, E.A.H.; Owen, N.; Anuradha, S.; Dunstan, D.W. Replacing Sitting Time with Standing or Stepping: Associations with Cardio-Metabolic Risk Biomarkers. Eur. Heart J. 2015, 36, 2643–2649. [Google Scholar] [CrossRef] [PubMed]
- Hawari, N.S.A.; Al-Shayji, I.; Wilson, J.; Gill, J.M.R. Frequency of Breaks in Sedentary Time and Postprandial Metabolic Responses. Med. Sci. Sports Exerc. 2016, 48, 2495–2502. [Google Scholar] [CrossRef]
- Westgaard, R.H. Work-Related Musculoskeletal Complaints: Some Ergonomics Challenges upon the Start of a New Century. Appl. Ergon. 2000, 31, 569–580. [Google Scholar] [CrossRef]
- Fullick, S.; Grindey, C.; Edwards, B.; Morris, C.; Reilly, T.; Richardson, D.; Waterhouse, J.; Atkinson, G. Relationships between Leisure-Time Energy Expenditure and Individual Coping Strategies for Shift-Work. Ergonomics 2009, 52, 448–455. [Google Scholar] [CrossRef]
- Wang, F.; Boros, S. The Effect of Physical Activity on Sleep Quality: A Systematic Review. Eur. J. Physiother. 2021, 23, 11–18. [Google Scholar] [CrossRef]

| All | MSD | NO-MSD | |
|---|---|---|---|
| N | 26 | 17 | 9 |
| Gender * | |||
| Male | 9 | 8 | 1 |
| Female | 16 | 9 | 7 |
| Other | 1 | - | 1 |
| Age (years) * | 33.2 (9.4) | 32.3 (7.9) | 34.9 (12.1) |
| Children | |||
| No | 20 | 15 | 5 |
| Yes | 6 | 2 | 4 |
| BMI | 24.6 (3.9) | 24.7 (3.5) | 24.5 (4.9) |
| Hip:Waist ratio | 1.2 (0.1) | 1.2 (0.1) | 1.2 (0.1) |
| Cardiometabolic data | |||
| Resting heart rate (HRrest, rpm) | 58.8 (9.7) | 58.7 (9.2) | 58.9 (11.2) |
| Average heart rate (HRaverage, rpm) | 76.5 (10.4) | 78.2 (9.6) | 78.3 (11.7) |
| Average arterial pressure (MAP, mmHg) | 87.4 (8.3) | 86.7 (7.9) | 88.8 (9.5) |
| Average pulse pressure (PP, mmHg) | 42.4 (6.7) | 41.4 (6.7) | 44.1 (6.8) |
| Work hours | 8.1 (0.5) | 8.1 (0.5) | 8.2 (0.4) |
| All | MSD | NO-MSD | |
|---|---|---|---|
| Head/neck/shoulders | 1.5 (1.4) | 2.2 (1.1) | - |
| Upper/lower back | 1.9 (2.1) | 2.9 (1.9) | - |
| Hips/knees/feet/ankle(s) | 1.2 (1.5) | 1.8 (1.5) | - |
| Elbow(s)/hands/wrists | 1.2 (1.1) | 1.7 (1.0) | 0.1 (0.3) |
| Composite MSD | 5.7 (5.0) | 8.7 (3.5) | 0.1 (0.3) |
| MSD (n = 17) | NO-MSD (n = 9) | |||||
|---|---|---|---|---|---|---|
| Daily | Work | Leisure | Daily | Work | Leisure | |
| Steps | 9468.8 (2925.1) | 5153.5 (2086.0) | 4337.8 (1880.7) | 10,055.8 (3556.8) | 5810.3 (3146.0) | 4245.4 (1594.2) |
| Transitions | 52.5 (10.3) | 25.4 (4.3) | 27.1 (8.2) | 49.6 (12.8) | 22.7 (9.0) * | 26.8 (6.6) |
| Hours standing | 5.9 (1.7) | 3.0 (1.1) | 2.9 (1.1) | 7.3 (2.4) | 4.1 (1.6) | 3.2 (1.0) |
| Hours walking | 1.7 (0.5) | 0.9 (0.3) | 0.8 (0.3) | 1.8 (0.6) | 1.0 (0.5) | 0.8 (0.2) |
| Hours sitting | 10.0 (1.8) | 6.0 (1.3) | 4.0 (1.0) | 9.2 (2.1) | 5.1 (1.4) | 4.1 (1.0) |
| Hours sleeping | 8.5 (0.7) | - | - | 8.1 (1.2) | - | - |
| Composite MSD | |||
|---|---|---|---|
| Daily | Work | Leisure | |
| Steps | −0.26 | 0.10 | −0.18 |
| Posture transitions | 0.38 | 0.46 * | 0.20 |
| Hours standing | −0.39 * | −0.27 | −0.30 |
| Hours walking | −0.31 | 0.09 | −0.21 |
| Hours sitting | 0.20 | 0.29 | 0.13 |
| Hours sleeping | 0.21 | - | - |
| Work | ||||||
|---|---|---|---|---|---|---|
| Steps | Transitions | Standing Time | Walking Time | Sitting Time | ||
| Leisure | Steps | 0.04 | −0.05 | 0.01 | 0.00 | −0.07 |
| Transitions | −0.07 | 0.24 | −0.26 | −0.05 | 0.18 | |
| Standing time | 0.03 | −0.29 | 0.21 | −0.02 | −0.31 | |
| Walking time | −0.02 | −0.19 | 0.01 | −0.04 | −0.05 | |
| Sitting time | −0.42 * | −0.20 | −0.64 ** | −0.42 * | 0.36 | |
| Sleeping time | 0.41 * | 0.47 * | 0.07 | 0.40 * | −0.05 | |
| Time | Hip:Waist Ratio | BMI | HRRest | HRAverage | MAPAverage | PPAverage | |
|---|---|---|---|---|---|---|---|
| Steps | Daily | 0.07 | −0.09 | −0.27 | −0.23 | −0.09 | 0.28 |
| Work | 0.04 | 0.02 | −0.17 | −0.16 | −0.11 | −0.05 | |
| Leisure | −0.02 | −0.21 | −0.34 | −0.29 | 0.06 | 0.55 | |
| Transitions | Daily | −0.08 | −0.10 | −0.43 * | −0.58 ** | −0.40 | 0.04 |
| Work | 0.12 | 0.29 | −0.28 | −0.33 | −0.43 | 0.18 | |
| Leisure | −0.22 | −0.39 * | −0.44 * | −0.52 ** | −0.34 | −0.04 | |
| Standing time | Daily | 0.16 | −0.05 | −0.09 | −0.19 | 0.22 | −0.08 |
| Work | 0.18 | 0.03 | −0.14 | −0.14 | 0.10 | −0.33 | |
| Leisure | −0.15 | −0.28 | 0.06 | −0.25 | 0.04 | 0.28 | |
| Walking time | Daily | 0.12 | −0.12 | −0.21 | −0.23 | −0.01 | 0.33 |
| Work | 0.08 | −0.05 | −0.17 | −0.13 | −0.21 | −0.18 | |
| Leisure | 0.05 | −0.25 | −0.20 | −0.20 | 0.25 | 0.58 * | |
| Sitting time | Daily | −0.16 | −0.07 | 0.09 | 0.16 | −0.11 | 0.36 |
| Work | 0.14 | 0.16 | 0.15 | 0.23 | −0.12 | 0.53 | |
| Leisure | −0.38 | −0.19 | −0.08 | 0.06 | −0.29 | −0.04 | |
| Sleeping time | Daily | −0.23 | 0.50 ** | 0.03 | 0.16 | 0.05 | −0.32 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arippa, F.; Nguyen, A.; Pau, M.; Harris-Adamson, C. Movement Behavior and Health Outcomes among Sedentary Adults: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2023, 20, 4668. https://doi.org/10.3390/ijerph20054668
Arippa F, Nguyen A, Pau M, Harris-Adamson C. Movement Behavior and Health Outcomes among Sedentary Adults: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2023; 20(5):4668. https://doi.org/10.3390/ijerph20054668
Chicago/Turabian StyleArippa, Federico, Athena Nguyen, Massimiliano Pau, and Carisa Harris-Adamson. 2023. "Movement Behavior and Health Outcomes among Sedentary Adults: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 20, no. 5: 4668. https://doi.org/10.3390/ijerph20054668
APA StyleArippa, F., Nguyen, A., Pau, M., & Harris-Adamson, C. (2023). Movement Behavior and Health Outcomes among Sedentary Adults: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 20(5), 4668. https://doi.org/10.3390/ijerph20054668








