Clinical Features to Predict the Use of a sEMG Wearable Device (REMO®) for Hand Motor Training of Stroke Patients: A Cross-Sectional Cohort Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
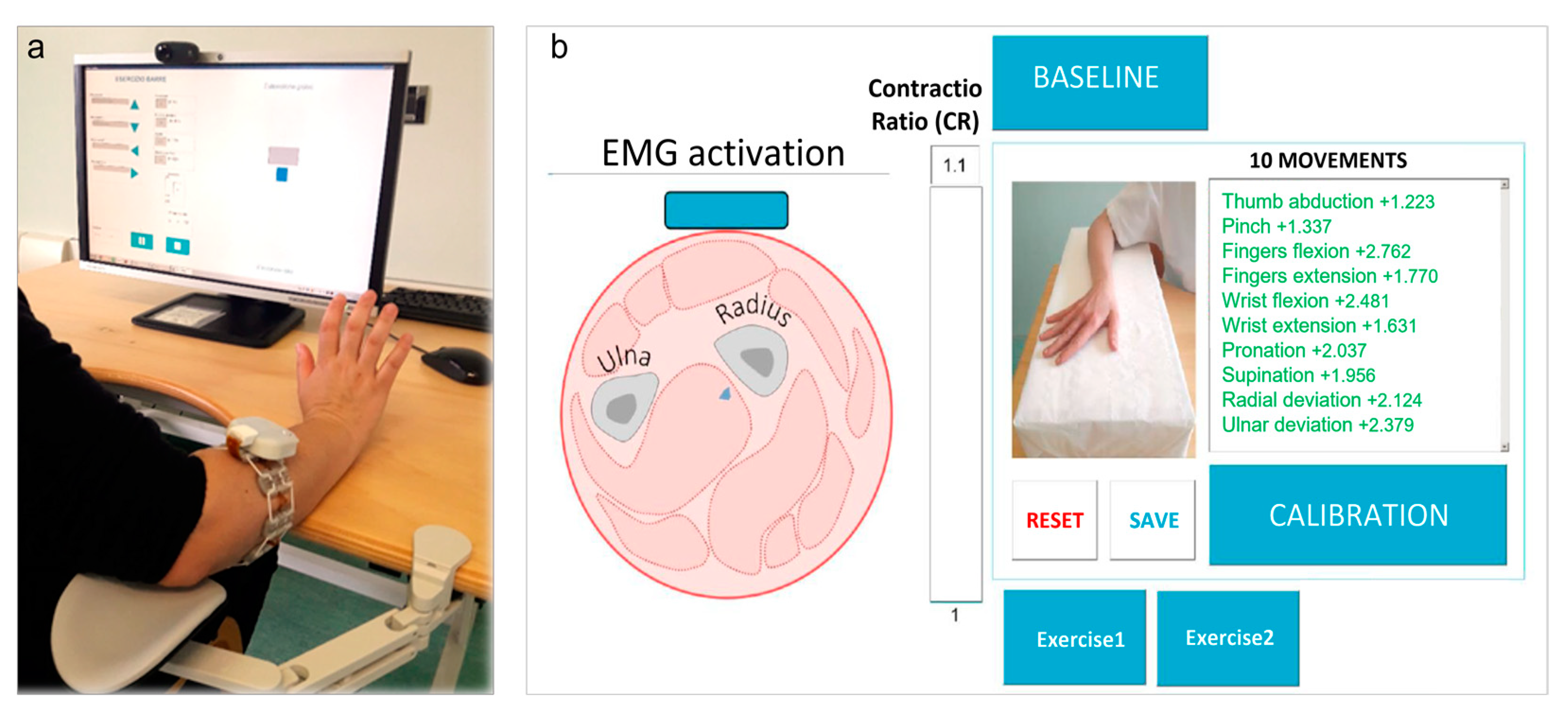
2.2. The Device
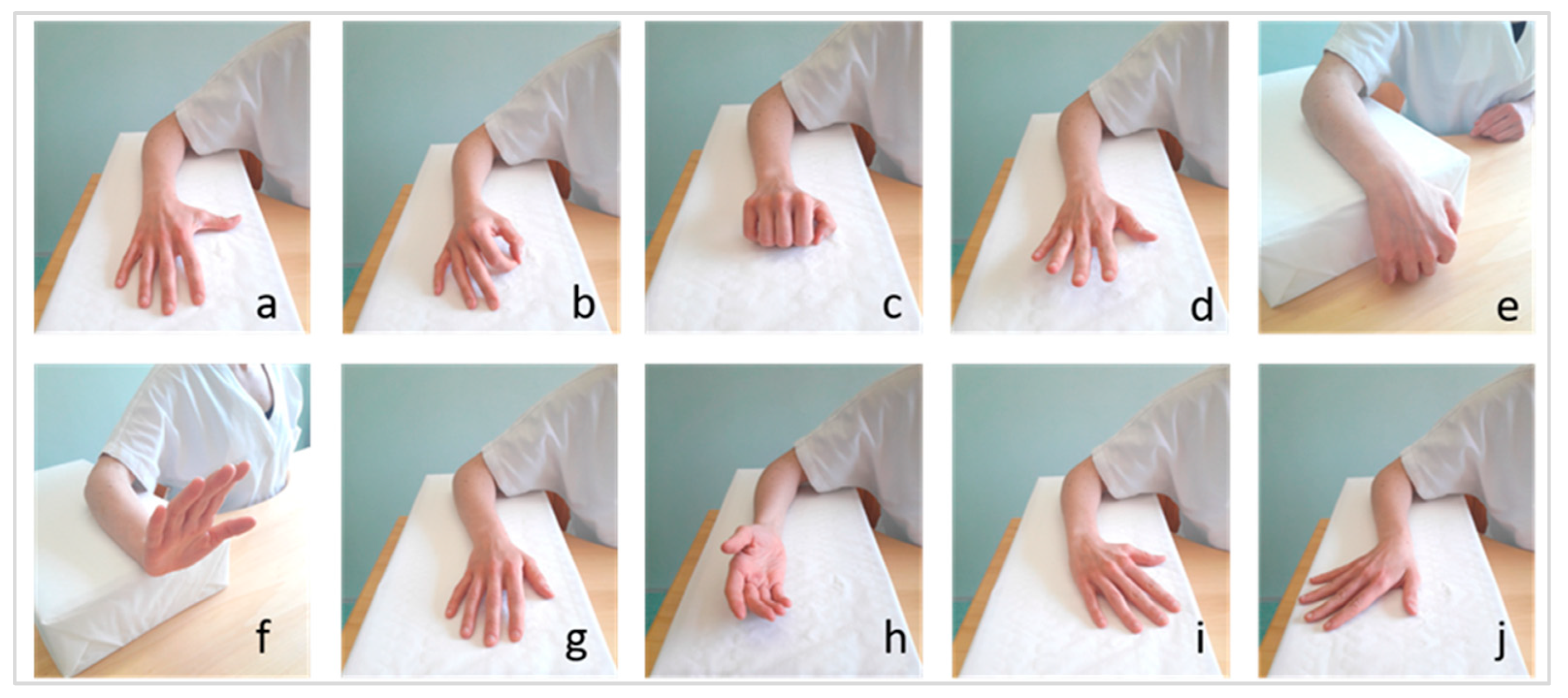
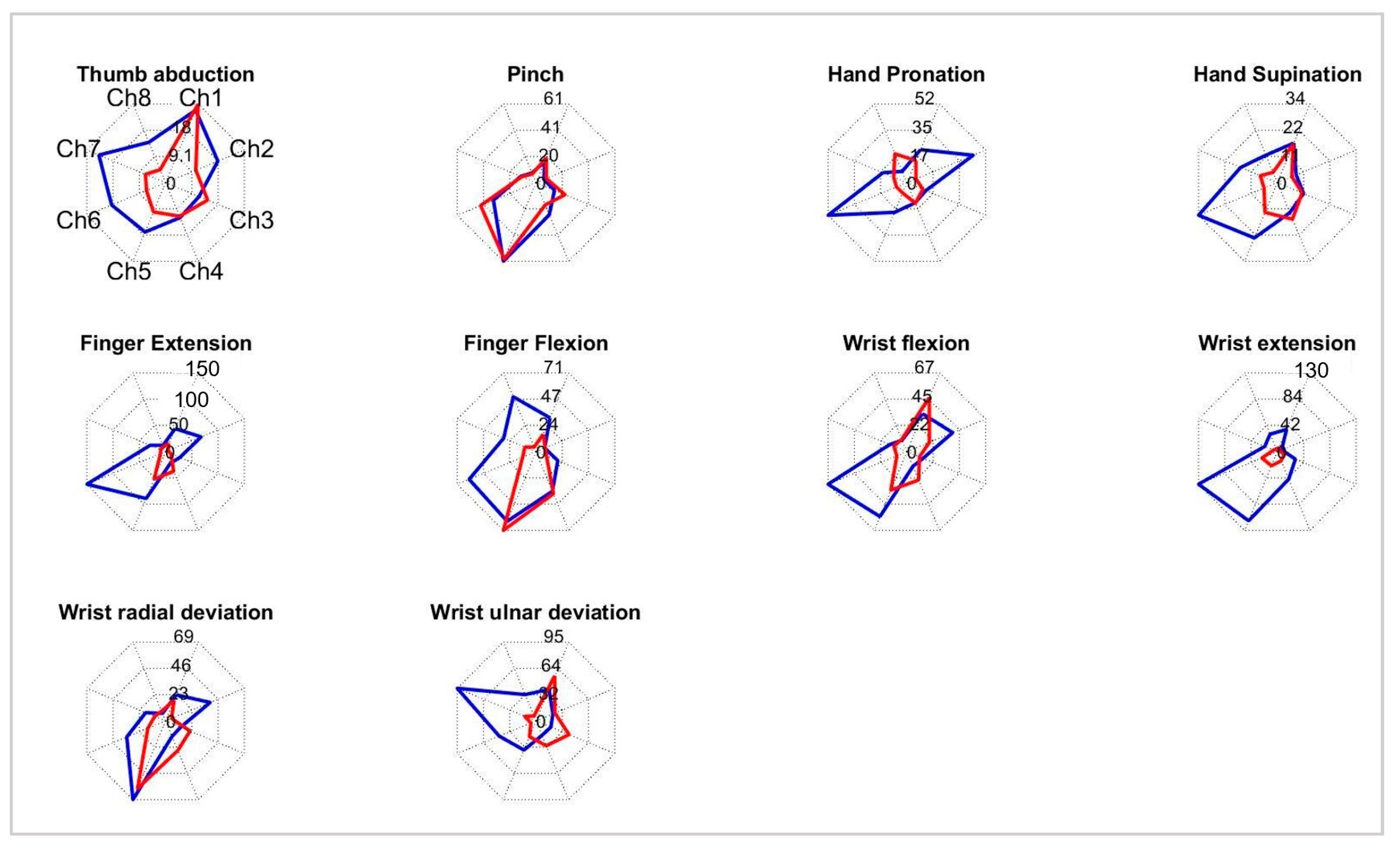
2.3. Test Methods
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| TBR | Technology-Based Rehabilitation |
| sEMG | Surface Electromyography |
| CT | Computed Tomography |
| MRI | Magnetic Resonance Imaging |
| IMU | Inertial Measurement Unit |
| CR | Contraction Ratio |
| MVC | Maximum Voluntary Contraction |
| FMA | Fugl-Meyer Assessment scale |
| FMA-UE | Fugl-Meyer Assessment Upper Extremity |
| FMA-hand | Fugl-Meyer Assessment Upper Extremity, wrist and hand sub-items |
| FMA sensation | Fugl-Meyer Assessment, sensation section |
| FMA pain/ROM | Fugl-Meyer Assessment, range of motion and pain section |
| RPS | Reaching Performance Scale |
| BBT | Box and Blocks Test |
| NHPT | Nine Hole Pegboard Test |
| MAS | Modified Ashworth Scale |
| PecMaj | Pectoralis Major |
| BicBra | Biceps Brachii |
| FlexCarp | Flexor Carpi muscles |
| FlexDigProf | Flexor Digitorum Profundus |
| FlexDigSup | Flexor Digitorum Superficialis |
| FIM | Functional Independence Measure |
| AUC | Area Under the Curve |
| RoC | Receiver Operating Characteristic |
| CI | confidence interval |
| GLM | logistic multivariable regression model |
| GLM0 | logistic multivariable regression model, 0 movement |
| GLM5 | logistic multivariable regression model, 5 movements |
| GLM10 | logistic multivariable regression model, 10 movements |
| GLMk | logistic multivariable regression model, k-means output number |
| DoF | Degree of Freedom |
References
- Feigin, V.L.; Roth, G.A.; Naghavi, M.; Parmar, P.; Krishnamurthi, R.; Chugh, S.; Mensah, G.A.; Norrving, B.; Shiue, I.; Ng, M.; et al. Global burden of stroke and risk factors in 188 countries, during 1990-2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet Neurol. 2016, 15, 913–924. [Google Scholar] [CrossRef]
- Krishnamurthi, R.V.; Feigin, V.L.; Forouzanfar, M.H.; Mensah, G.A.; Connor, M.; Bennett, D.A.; Moran, A.E.; Sacco, R.L.; Anderson, L.M.; Truelsen, T.; et al. Global and regional burden of first-ever ischaemic and haemorrhagic stroke during 1990-2010: Findings from the Global Burden of Disease Study 2010. Lancet Glob. Health 2013, 1, e259–e281. [Google Scholar] [CrossRef]
- Tsao, C.W.; Aday, A.W.; Almarzooq, Z.I.; Alonso, A.; Beaton, A.Z.; Bittencourt, M.S.; Boehme, A.K.; Buxton, A.E.; Carson, A.P.; Commodore-Mensah, Y.; et al. Heart Disease and Stroke Statistics-2022 Update: A Report From the American Heart Association. Circulation 2022, 145, e153–e639. [Google Scholar] [CrossRef]
- Collaborators, G.B.D.S. Global, regional, and national burden of stroke, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019, 18, 439–458. [Google Scholar] [CrossRef]
- Benjamin, E.J.; Muntner, P.; Alonso, A.; Bittencourt, M.S.; Callaway, C.W.; Carson, A.P.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Das, S.R.; et al. Heart Disease and Stroke Statistics-2019 Update: A Report From the American Heart Association. Circulation 2019, 139, e56–e528. [Google Scholar] [CrossRef]
- Feigin, V.L.; Stark, B.A.; Johnson, C.O.; Roth, G.A.; Bisignano, C.; Abady, G.G.; Abbasifard, M.; Abbasi-Kangevari, M.; Abd-Allah, F.; Abedi, V.; et al. Global, regional, and national burden of stroke and its risk factors, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet Neurol. 2021, 20, 795–820. [Google Scholar] [CrossRef]
- Feigin, V.L.; Norrving, B.; Mensah, G.A. Global Burden of Stroke. Circ. Res. 2017, 120, 439–448. [Google Scholar] [CrossRef]
- Cauraugh, J.H.; Kim, S.B. Chronic stroke motor recovery: Duration of active neuromuscular stimulation. J. Neurol. Sci. 2003, 215, 13–19. [Google Scholar] [CrossRef]
- Sathian, K.; Buxbaum, L.J.; Cohen, L.G.; Krakauer, J.W.; Lang, C.E.; Corbetta, M.; Fitzpatrick, S.M. Neurological principles and rehabilitation of action disorders: Common clinical deficits. Neurorehabil. Neural. Repair 2011, 25, 21S–32S. [Google Scholar] [CrossRef]
- Kwakkel, G.; Kollen, B.J.; van der Grond, J.; Prevo, A.J. Probability of regaining dexterity in the flaccid upper limb: Impact of severity of paresis and time since onset in acute stroke. Stroke 2003, 34, 2181–2186. [Google Scholar] [CrossRef]
- Nichols-Larsen, D.S.; Clark, P.C.; Zeringue, A.; Greenspan, A.; Blanton, S. Factors influencing stroke survivors’ quality of life during subacute recovery. Stroke 2005, 36, 1480–1484. [Google Scholar] [CrossRef]
- Foley, E.L.; Nicholas, M.L.; Baum, C.A.-O.; Connor, L.A.-O. Influence of Environmental Factors on Social Participation Post-Stroke. Behav. Neurol. 2019, 2019, 2606039. [Google Scholar] [CrossRef] [PubMed]
- Bernhardt, J.; Hayward, K.S.; Kwakkel, G.; Ward, N.S.; Wolf, S.L.; Borschmann, K.; Krakauer, J.W.; Boyd, L.A.; Carmichael, S.T.; Corbett, D.; et al. Agreed definitions and a shared vision for new standards in stroke recovery research: The Stroke Recovery and Rehabilitation Roundtable taskforce. Int. J. Stroke 2017, 12, 444–450. [Google Scholar] [CrossRef] [PubMed]
- Winters, C.; Kwakkel, G.; van Wegen, E.E.H.; Nijland, R.H.M.; Veerbeek, J.M.; Meskers, C.G.M. Moving stroke rehabilitation forward: The need to change research. NeuroRehabilitation 2018, 43, 19–30. [Google Scholar] [CrossRef]
- Kwakkel, G.; Kollen, B.J. Predicting activities after stroke: What is clinically relevant? Int. J. Stroke 2013, 8, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Stinear, C.M.; Lang, C.E.; Zeiler, S.; Byblow, W.D. Advances and challenges in stroke rehabilitation. Lancet Neurol. 2020, 19, 348–360. [Google Scholar] [CrossRef]
- Coupar, F.; Pollock, A.; Rowe, P.; Weir, C.; Langhorne, P. Predictors of upper limb recovery after stroke: A systematic review and meta-analysis. Clin. Rehabil. 2012, 26, 291–313. [Google Scholar] [CrossRef]
- Stinear, C. Prediction of recovery of motor function after stroke. Lancet Neurol. 2010, 9, 1228–1232. [Google Scholar] [CrossRef]
- Meldrum, D.; Pittock, S.J.; Hardiman, O.; Ni Dhuill, C.; O’Regan, M. Recovery of the upper limb post ischaemic stroke and the predictive value of the Orpington Prognostic Score. Clin. Rehabil. 2004, 18, 694–702. [Google Scholar] [CrossRef]
- Hancock, N.J.; Collins, K.; Dorer, C.; Wolf, S.L.; Bayley, M.; Pomeroy, V.M. Evidence-based practice ‘on-the-go’: Using ViaTherapy as a tool to enhance clinical decision making in upper limb rehabilitation after stroke, a quality improvement initiative. BMJ Open Qual. 2019, 8, e000592. [Google Scholar] [CrossRef]
- Wolf, S.L.; Kwakkel, G.; Bayley, M.; McDonnell, M.N.; Upper Extremity Stroke Algorithm Working Group. Best practice for arm recovery post stroke: An international application. Physiotherapy 2016, 102, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Pollock, A.; Farmer, S.E.; Brady, M.C.; Langhorne, P.; Mead, G.E.; Mehrholz, J.; van Wijck, F. Interventions for improving upper limb function after stroke. Cochrane Database Syst. Rev. 2014, 11, CD010820. [Google Scholar] [CrossRef] [PubMed]
- Everard, G.; Declerck, L.; Detrembleur, C.; Leonard, S.; Bower, G.; Dehem, S.; Lejeune, T. New technologies promoting active upper limb rehabilitation after stroke: An overview and network meta-analysis. Eur. J. Phys. Rehabil. Med. 2022, 58, 530–548. [Google Scholar] [CrossRef]
- Wu, J.; Zeng, A.; Chen, Z.; Wei, Y.; Huang, K.; Chen, J.; Ren, Z. Effects of Virtual Reality Training on Upper Limb Function and Balance in Stroke Patients: Systematic Review and Meta-Meta-Analysis. J. Med. Internet Res. 2021, 23, e31051. [Google Scholar] [CrossRef] [PubMed]
- Gandolfi, M.; Valè, N.; Posteraro, F.; Morone, G.; Dell’orco, A.; Botticelli, A.; Dimitrova, E.; Gervasoni, E.; Goffredo, M.; Zenzeri, J.; et al. State of the art and challenges for the classification of studies on electromechanical and robotic devices in neurorehabilitation: A scoping review. Eur. J. Phys. Rehabil. Med. 2021, 57, 831–840. [Google Scholar] [CrossRef] [PubMed]
- Veerbeek, J.M.; Langbroek-Amersfoort, A.C.; van Wegen, E.E.; Meskers, C.G.; Kwakkel, G. Effects of Robot-Assisted Therapy for the Upper Limb After Stroke. Neurorehabil. Neural. Repair 2017, 31, 107–121. [Google Scholar] [CrossRef] [PubMed]
- Bell, A.; Grampurohit, N.; Kains, G.; Marino, R.J. Developing guiding principles for technology-based rehabilitation program by engaging people with motor incomplete tetraplegia. J. Neuroeng. Rehabil. 2022, 19, 128. [Google Scholar] [CrossRef]
- Lirio-Romero, C.; Torres-Lacomba, M.; Gómez-Blanco, A.; Acero-Cortés, A.; Retana-Garrido, A.; de la Villa-Polo, P.; Sánchez-Sánchez, B. Electromyographic biofeedback improves upper extremity function: A randomized, single-blinded, controlled trial. Physiotherapy 2021, 110, 54–62. [Google Scholar] [CrossRef] [PubMed]
- Papazian, C.; Baicoianu, N.A.; Peters, K.M.; Feldner, H.A.; Steele, K.M. Electromyography Recordings Detect Muscle Activity Before Observable Contractions in Acute Stroke Care. Arch. Rehabil. Res. Clin. Transl. 2021, 3, 100136. [Google Scholar] [CrossRef]
- Raurale, S.A.; McAllister, J.; Rincon, J.M.d. Real-Time Embedded EMG Signal Analysis for Wrist-Hand Pose Identification. IEEE Trans. Signal Process. 2020, 68, 2713–2723. [Google Scholar] [CrossRef]
- Munoz-Novoa, M.; Kristoffersen, M.B.; Sunnerhagen, K.S.; Naber, A.; Alt Murphy, M.; Ortiz-Catalan, M. Upper Limb Stroke Rehabilitation Using Surface Electromyography: A Systematic Review and Meta-Analysis. Front. Hum. Neurosci. 2022, 16, 897870. [Google Scholar] [CrossRef]
- Mugler, E.M.; Tomic, G.; Singh, A.; Hameed, S.; Lindberg, E.W.; Gaide, J.; Alqadi, M.; Robinson, E.; Dalzotto, K.; Limoli, C.; et al. Myoelectric Computer Interface Training for Reducing Co-Activation and Enhancing Arm Movement in Chronic Stroke Survivors: A Randomized Trial. Neurorehabilit. Neural Repair 2019, 33, 284–295. [Google Scholar] [CrossRef] [PubMed]
- Parker, J.; Powell, L.; Mawson, S. Effectiveness of Upper Limb Wearable Technology for Improving Activity and Participation in Adult Stroke Survivors: Systematic Review. J. Med. Internet Res. 2020, 22, e15981. [Google Scholar] [CrossRef] [PubMed]
- Meeker, C.; Park, S.; Bishop, L.; Stein, J.; Ciocarlie, M. EMG pattern classification to control a hand orthosis for functional grasp assistance after stroke. IEEE Int. Conf. Rehabil. Robot 2017, 2017, 1203–1210. [Google Scholar] [CrossRef]
- Di Girolamo, M.; Celadon, N.; Appendino, S.; Turolla, A.; Ariano, P. EMG-based biofeedback system for motor rehabilitation: A pilot study. In Proceedings of the 2017 IEEE Biomedical Circuits and Systems Conference (BioCAS), Turin, Italy, 19–21 October 2017; pp. 1–4. [Google Scholar] [CrossRef]
- Rimini, D.; Salvalaggio, S.; Pregnolato, G.; Alhelou, M.; Berlingieri, C.; Mascotto, E.; Turolla, A.; Ariano, P.; Celadon, N.; Ahmed, D. sEMG-biofeedback armband for hand motor rehabilitation in stroke patients: A preliminary pilot longitudinal study. In Proceedings of the 2020 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Bari, Italy, 1 June 2020; pp. 1–5. [Google Scholar] [CrossRef]
- Markovic, M.; Schweisfurth, M.A.; Engels, L.F.; Farina, D.; Dosen, S. Myocontrol is closed-loop control: Incidental feedback is sufficient for scaling the prosthesis force in routine grasping. J. Neuroeng. Rehabil. 2018, 15, 81. [Google Scholar] [CrossRef] [PubMed]
- Hartmann, C.; Dosen, S.; Amsuess, S.; Farina, D. Closed-Loop Control of Myoelectric Prostheses With Electrotactile Feedback: Influence of Stimulation Artifact and Blanking. IEEE Trans. Neural. Syst. Rehabil. Eng. 2015, 23, 807–816. [Google Scholar] [CrossRef]
- Oboe, R.; Tonin, A.; Yu, K.; Ohnishi, K.; Turolla, A. Robotic finger rehabilitation system for stroke patient using surface EMG armband. In Proceedings of the IECON 2016—42nd Annual Conference of the IEEE Industrial Electronics Society, Florence, Italy, 23–26 October 2016; IEEE: Piscataway, NJ, USA, 2016; pp. 785–790. [Google Scholar] [CrossRef]
- Fox, J. The R Commander: A Basic-Statistics Graphical User Interface to R. J. Stat. Softw. 2005, 14, 1–42. [Google Scholar] [CrossRef]
- Milligan, G.W. Clustering Validation: Results and Implications for Applied Analyses. In Clustering and Classification; World Scientific: Singapore, 1996; pp. 341–375. [Google Scholar] [CrossRef]
- Steinley, D. K-means clustering: A half-century synthesis. Br. J. Math. Stat. Psychol. 2006, 59 Pt 1, 1–34. [Google Scholar] [CrossRef] [PubMed]
- Ahn, H. Effect Modeling of Count Data Using Logistic Regression with Qualitative Predictors. Engineering 2014, 6, 758–772. [Google Scholar] [CrossRef][Green Version]
- McFadden, D. Quantitative Methods for Analyzing Travel Behaviour of Individuals: Some Recent Developments; Cowles Foundation for Research in Economics; No 474, Cowles Foundation Discussion Papers, Cowles Foundation for Research in Economics; Yale University: New Haven, CT, USA, 1977. [Google Scholar]
- Brier, G.W. Verification of Forecasts Expressed in terms of Probability. Mon. Weather. Rev. 1950, 78, 1–3. [Google Scholar] [CrossRef]
- Zhang, X.; Chen, X.; Zhao, Z.-Y.; Tu, Y.-Q.; Yang, J.-H.; Lantz, V.; Wang, K.-Q. Research on Gesture Definition and Electrode Placement in Pattern Recognition of Hand Gesture Action SEMG. In Medical Biometrics. ICMB 2008. Lecture Notes in Computer Science; Springer: Berlin/Heidelberg, Germany, 2007; Volume 4901. [Google Scholar] [CrossRef]
- Mesa, I.; Rubio, A.; Tubia, I.; De No, J.; Diaz, J. Channel and feature selection for a surface electromyographic pattern recognition task. Expert Syst. Appl. 2014, 41, 5190–5200. [Google Scholar] [CrossRef]
- Carpinella, I.; Jonsdottir, J.; Ferrarin, M. Multi-finger coordination in healthy subjects and stroke patients: A mathematical modelling approach. J. Neuroeng. Rehabil. 2011, 8, 19. [Google Scholar] [CrossRef]
- van Kordelaar, J.; van Wegen, E.E.; Nijland, R.H.; Daffertshofer, A.; Kwakkel, G. Understanding adaptive motor control of the paretic upper limb early poststroke: The EXPLICIT-stroke program. Neurorehabil. Neural Repair 2013, 27, 854–863. [Google Scholar] [CrossRef]
- Kwakkel, G.; Winters, C.; van Wegen, E.E.; Nijland, R.H.; van Kuijk, A.A.; Visser-Meily, A.; de Groot, J.; de Vlugt, E.; Arendzen, J.H.; Geurts, A.C.; et al. Effects of Unilateral Upper Limb Training in Two Distinct Prognostic Groups Early After Stroke: The EXPLICIT-Stroke Randomized Clinical Trial. Neurorehabil. Neural Repair 2016, 30, 804–816. [Google Scholar] [CrossRef]
- Jarque-Bou, N.J.; Sancho-Bru, J.L.; Vergara, M. A Systematic Review of EMG Applications for the Characterization of Forearm and Hand Muscle Activity during Activities of Daily Living: Results, Challenges, and Open Issues. Sensors 2021, 21, s21093035. [Google Scholar] [CrossRef]
- Cognolato, M.; Atzori, M.; Marchesin, C.; Marangon, S.; Faccio, D.; Tiengo, C.; Bassetto, F.; Gassert, R.; Petrone, N.; Müller, H. Multifunction control and evaluation of a 3D printed hand prosthesis with the Myo armband by hand amputees. bioRxiv 2018, 445460. [Google Scholar] [CrossRef]
- Farina, D.; Jiang, N.; Rehbaum, H.; Holobar, A.; Graimann, B.; Dietl, H.; Aszmann, O.C. The extraction of neural information from the surface EMG for the control of upper-limb prostheses: Emerging avenues and challenges. IEEE Trans. Neural Syst. Rehabil. Eng. 2014, 22, 797–809. [Google Scholar] [CrossRef]
- Brambilla, C.; Scano, A. The Number and Structure of Muscle Synergies Depend on the Number of Recorded Muscles: A Pilot Simulation Study with OpenSim. Sensors 2022, 22, 8584. [Google Scholar] [CrossRef]
- Paleari, M.; Girolamo, M.D.; Celadon, N.; Favetto, A.; Ariano, P. On optimal electrode configuration to estimate hand movements from forearm surface electromyography. In Proceedings of the 2015 37th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Milan, Italy, 25–29 August 2015; Volume 2015, pp. 6086–6089. [Google Scholar] [CrossRef]
- Celadon, N.; Došen, S.; Binder, I.; Ariano, P.; Farina, D. Proportional estimation of finger movements from high-density surface electromyography. J. Neuroeng. Rehabil. 2016, 13, 73. [Google Scholar] [CrossRef]
- Leone, F.; Gentile, C.; Ciancio, A.L.; Gruppioni, E.; Davalli, A.; Sacchetti, R.; Guglielmelli, E.; Zollo, L. Simultaneous sEMG Classification of Hand/Wrist Gestures and Forces. Front. Neurorobot. 2019, 13, 42. [Google Scholar] [CrossRef]
- Atzori, M.; Gijsberts, A.; Castellini, C.; Caputo, B.; Hager, A.G.; Elsig, S.; Giatsidis, G.; Bassetto, F.; Müller, H. Electromyography data for non-invasive naturally-controlled robotic hand prostheses. Sci. Data 2014, 1, 140053. [Google Scholar] [CrossRef]
- Lyu, M.; Lambelet, C.; Woolley, D.; Zhang, X.; Chen, W.; Ding, X.; Gassert, R.; Wenderoth, N. Training wrist extensor function and detecting unwanted movement strategies in an EMG-controlled visuomotor task. IEEE Int. Conf. Rehabil. Robot 2017, 2017, 1549–1555. [Google Scholar] [CrossRef]


| Age | |
| Mean Years (SD) | 65.09 (12.14) |
| Sex | |
| Female/Male, n (%) | 44/73 (38/62%) |
| Aphasia | |
| Yes/No, n (%) | 37/80 (32/68%) |
| Apraxia | |
| Yes/No, n (%) | 7/110 (6/94%) |
| Lesion Type | |
| Ischemic Stroke, n (%) | 77 (66%) |
| Hemorrhagic Stroke, n (%) | 40 (34%) |
| Affected arm | |
| Right/Left, n (%) | 56/61 (48/52%) |
| Time from stroke | |
| Mean months (SD) | 15.98 (35) |
| FMA, Mean (SD) | |
| FMA-UE | 30.04 (22.66) |
| FMA-hand | 9.94 (9.33) |
| FMA sensation | 16.44 (7.99) |
| FMA Pain/ROM | 42.40 (5.28) |
| RPS | |
| Mean (SD) | 16.62 (14.91) |
| NHPT | |
| Mean (SD) | 0.13 (0.20) |
| BBT | |
| Mean (SD) | 14.82 (18.97) |
| FIM | |
| Mean (SD) | 85.95 (24.37) |
| MAS, Mean (SD) | |
| Total score | 1.92 (2.83) |
| PecMaj | 0.29 (0.68) |
| BicBra | 0.49 (0.75) |
| FlexCarp | 0.56 (0.93) |
| FlexDigProf | 0.24 (0.65) |
| FlexDigSup | 0.35 (0.69) |
| Model | N Movements | Variables | Odds Ratio (CI 95%) | K Value/Total | Se/Sp |
|---|---|---|---|---|---|
| GLM0 | N > 0 | FMA-UE | 1.53 (1.18–1.98) | ≥10/66 | 0.95/0.82 |
| FMA-UE pain/ROM | 1.22 (1.04–1.43) | ≥43/48 | 0.79/0.65 | ||
| GLM5 | N ≥ 5 | FMA-UE | 1.65 (1.22–2.22) | ≥18/66 | 1/0.76 |
| FlexCarp | 0.45 (0.26–0.92) | <0/4 | 1/0 | ||
| GLMk | N ≥ 6 | FMA-UE | 1.52 (1.18–1.97) | ≥18/66 | 1/0.76 |
| FlexCarp | 0.51 (0.26–0.98) | <0/4 | 1/0 | ||
| GLM10 | N = 10 | FMA-UE | 1.11 (1.07–1.15) | ≥18/66 | 0.90/0.86 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pregnolato, G.; Rimini, D.; Baldan, F.; Maistrello, L.; Salvalaggio, S.; Celadon, N.; Ariano, P.; Pirri, C.F.; Turolla, A. Clinical Features to Predict the Use of a sEMG Wearable Device (REMO®) for Hand Motor Training of Stroke Patients: A Cross-Sectional Cohort Study. Int. J. Environ. Res. Public Health 2023, 20, 5082. https://doi.org/10.3390/ijerph20065082
Pregnolato G, Rimini D, Baldan F, Maistrello L, Salvalaggio S, Celadon N, Ariano P, Pirri CF, Turolla A. Clinical Features to Predict the Use of a sEMG Wearable Device (REMO®) for Hand Motor Training of Stroke Patients: A Cross-Sectional Cohort Study. International Journal of Environmental Research and Public Health. 2023; 20(6):5082. https://doi.org/10.3390/ijerph20065082
Chicago/Turabian StylePregnolato, Giorgia, Daniele Rimini, Francesca Baldan, Lorenza Maistrello, Silvia Salvalaggio, Nicolò Celadon, Paolo Ariano, Candido Fabrizio Pirri, and Andrea Turolla. 2023. "Clinical Features to Predict the Use of a sEMG Wearable Device (REMO®) for Hand Motor Training of Stroke Patients: A Cross-Sectional Cohort Study" International Journal of Environmental Research and Public Health 20, no. 6: 5082. https://doi.org/10.3390/ijerph20065082
APA StylePregnolato, G., Rimini, D., Baldan, F., Maistrello, L., Salvalaggio, S., Celadon, N., Ariano, P., Pirri, C. F., & Turolla, A. (2023). Clinical Features to Predict the Use of a sEMG Wearable Device (REMO®) for Hand Motor Training of Stroke Patients: A Cross-Sectional Cohort Study. International Journal of Environmental Research and Public Health, 20(6), 5082. https://doi.org/10.3390/ijerph20065082










