Bonding Interface and Repairability of 3D-Printed Intraoral Splints: Shear Bond Strength to Current Polymers, with and without Ageing
Abstract
:1. Introduction
2. Materials and Methods
2.1. Specimen Preparation
2.1.1. Base Material and Ageing
2.1.2. Base Material Surface Conditioning
- AM base + BM (n = 40): The AM base material was blasted with 125µm Al2O3 (Cobra, Renfert GmbH, Hilzingen, Germany) at 3 bar for 10 s. Thereafter the monomer was applied with a microbrush for 30 s and left to air dry for 30 s (Palapress liquid, Heraeus Kulzer GmbH).
- AM base + M (n = 40): The AM base material was conditioned with monomer (Palapress liquid, Heraeus Kulzer GmbH) applied with a microbrush for 30 s and left to air dry for 30 s.
- AM base + B (n = 320): The AM base material was blasted with 125µm Al2O3 (Cobra, Renfert GmbH, Hilzingen, Germany) at 3 bar for 10 s. Eighty out of these 320 were further conditioned with:
- +PS (n = 40): Primostick (PS202; LOT 201202:03/23, Primotec Joachim Mosch e.K, Bad Homburg, Germany) was applied for 30 s with a microbrush and light cured for 2 min (Elipar TriLight, 3M ESPE AG, Seefeld, Germany).
- +FB (n = 40, only “wet storage”): freeform bond liquid (freeform, LOT 200710:07/19; Detax GmbH & Co KG, Ettlingen, Germany) was applied for 30 s with a microbrush and let air dry for 30 s.
- AM base + PS (n = 40): Primostick (PS202; LOT 201202:03/23, Primotec Joachim Mosch e.K, Bad Homburg, Germany) was applied for 30 s with a microbrush and light cured for 2 min (Elipar TriLight, 3M ESPE AG, Seefeld, Germany).
- AM base + FB (n = 40 only “wet storage”): freeform® bond liquid (freeform® bond, LOT 200710:07/19; Detax GmbH & Co KG, Ettlingen, Germany) was applied to untreated AM base specimens for 30 s with a microbrush and left to air dry for 30 s.FB is provided by the manufacturer for adaptations to splints after a period of clinical application, only.
- AM base + NC (n = 200). The AM base material was connected “as printed” to the cylinders without any further surface treatment or conditioning.
2.2. Surface Characterization of the Bonding Interface
2.3. Bonding of the Cylinder Specimens to the Base Materials
- palapress mixing 10 g of powder to 7 mL of liquid (Palapress clear, LOT monomer K010108:05/22, powder K010048:11/21; Heraeus Kulzer GmbH) and polymerized submerged in water within a pressure pot at 2 bar for 20 min and 55 °C.
- primosplint directly applied from the rods (Material primosplint; primotec® Joachim Mosch e.K, Bad Homburg, Germany; LOT# 193138:08/21) to the cylinder with help of a Heidemann specular. Thereafter the material was light-cured for 1 min with direct application within the mold (Elipar TriLight, 3M ESPE AG) and 10 min without molding in a light oven (Speed Labolight, Hager & Werken GmbH & Co KG, Duisburg, Germany).
- freeprint splint was drawn up into a light-protected syringe (5 mL, BD Luer-Lok Tip REF 309649; Becton-Dickinson and Comp, Franklin Lakes, NJ, USA) from the bottle (Material Freeprint splint® 2.0; DETAX GmbH & Co. KG, Ettlingen, Germany; LOT# 220405:04/21) and applied into the cylinder. Thereafter the material was light-cured for 1 min with direct light application within the mold (Elipar TriLight, 3M ESPE AG) and 10 min without molding in a light oven (Speed Labolight, Hager & Werken GmbH & Co KG, Duisburg, Germany).
- freeform fixgel was directly applied from the cartridge with the delivered mixing tip (Material Freeform fixgel®, DETAX GmbH& Co. KG, Ettlingen, Germany; LOT# 210801: 08/20) into the cylinder. Thereafter the material was light-cured for 1 min with direct light application within the mold (Elipar TriLight, 3M ESPE AG) and 10 min without molding in a light oven (Speed Labolight, Hager & Werken GmbH & Co KG, Duisburg, Germany).
- freeform plast was directly applied from the box (Material Freeform plast®, DETAX GmbH& Co. KG, Ettlingen, Germany; LOT# 210601: 06/20) to the cylinder with help of a Heidemann specular. Thereafter the material was light-cured for 1 min with a direct light application within the mold (Elipar TriLight, 3M ESPE AG) and 10 min without molding in a light oven (Speed Labolight, Hager & Werken GmbH & Co KG, Duisburg, Germany).
2.4. Artificial Ageing and Measurement of the Bonded Specimens
2.5. Shear Bond Test and Fracture Mode Analysis
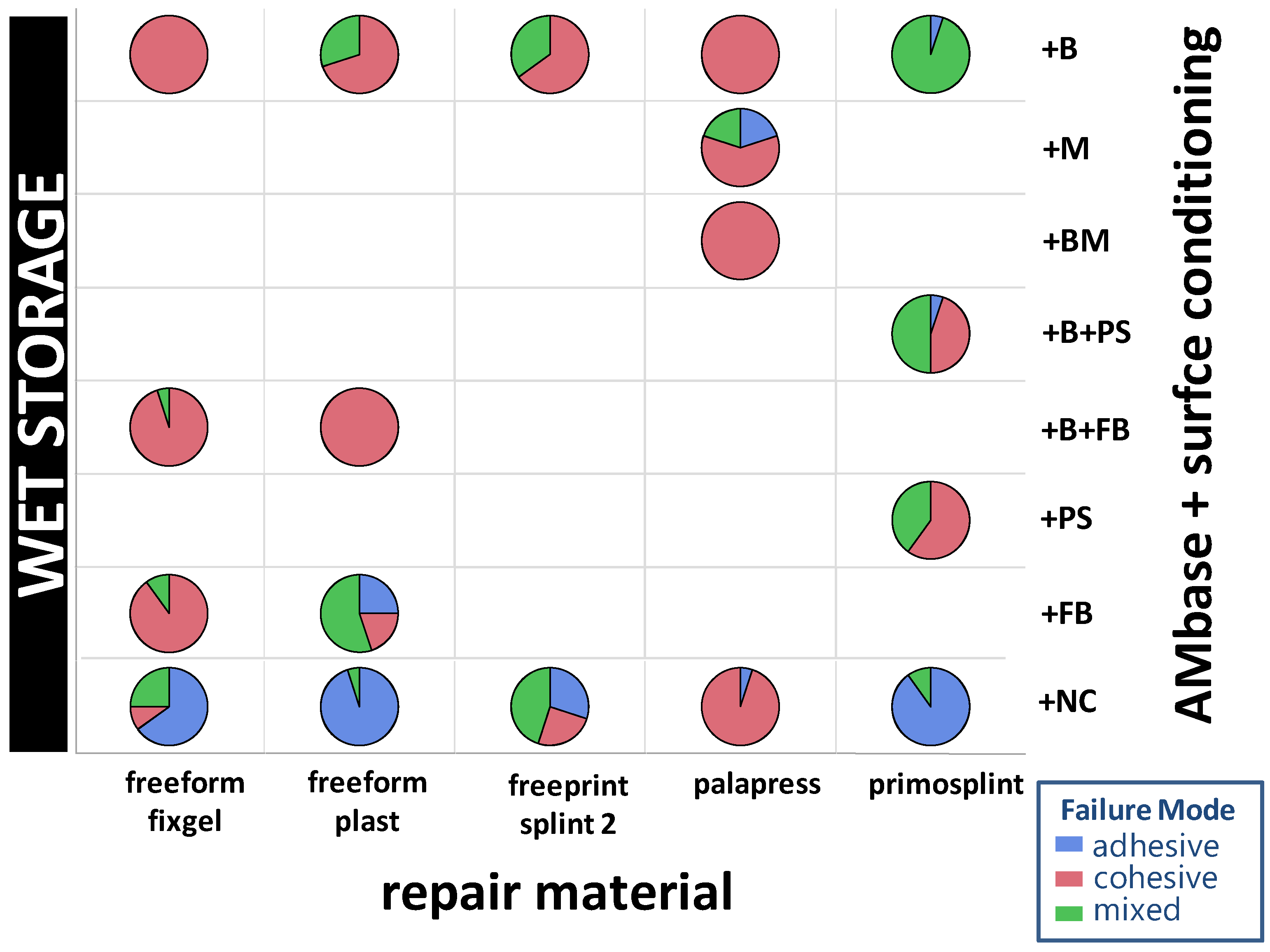
- Cohesive fracture: the fracture ran completely in the resin of the 3D printed base material.
- Adhesive fracture: the fracture ran between both materials (base material and repair material).
- Mixed fracture: the fracture contained both fracture modes. There were adhesively fractured areas and areas within the same specimen that were cohesively fractured.
2.6. Statistical Methods
2.6.1. Surface Roughness of Base Materials
2.6.2. Shear Bond Strength
2.6.3. Failure Mode
3. Results
3.1. Surface Characteristics of the Base Bonding Interfaces
3.1.1. Surface Roughness of Base Materials
3.1.2. Qualitative Surface Evaluation of Bonding Interface
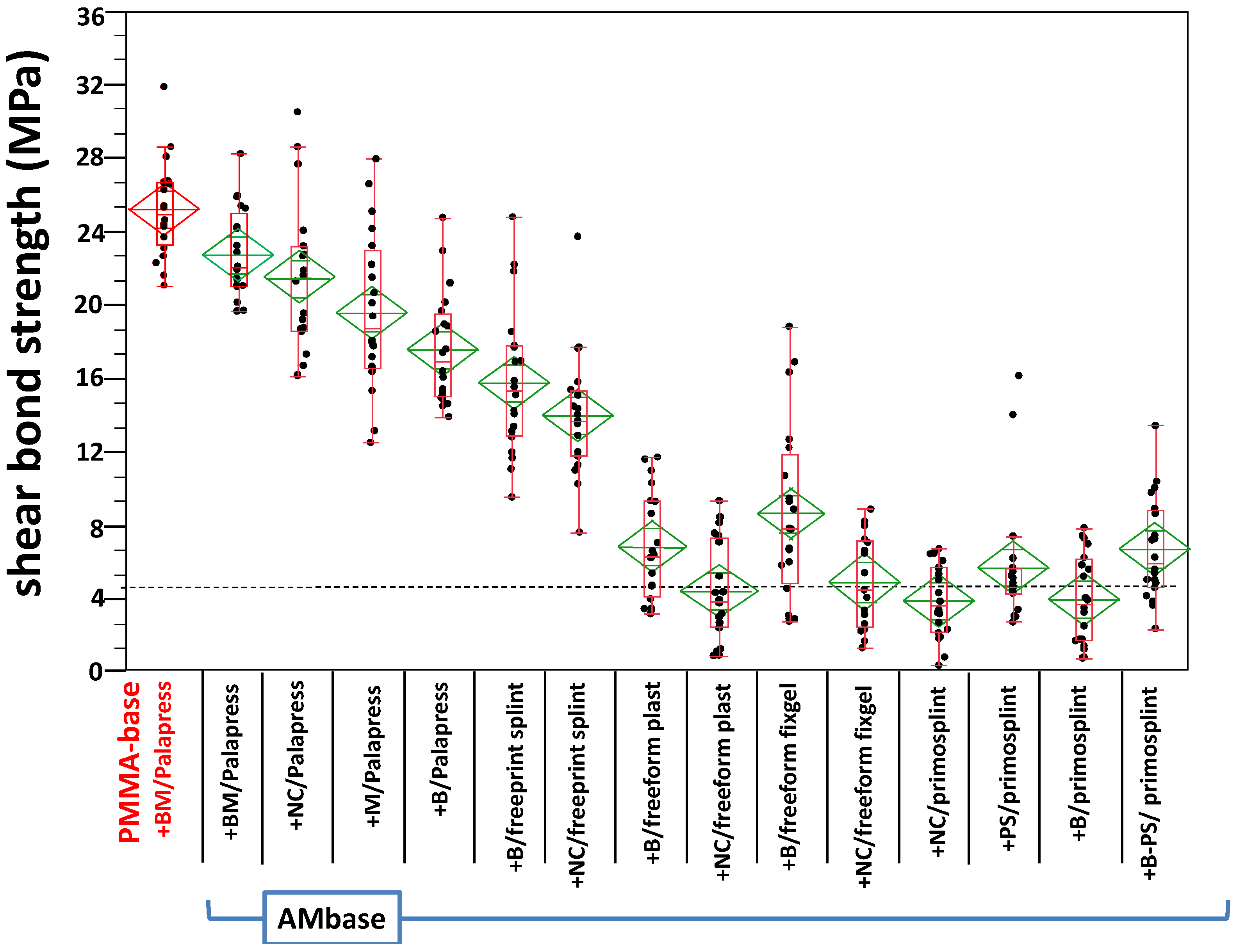
3.2. Shear Bond Strength
3.3. Failure Modes
4. Discussion
4.1. General Observations
4.2. Specifics of Light Curing Material
4.3. Methodical Aspects and Limitations of the Study Design
4.4. Outlook on Clinical Applicability
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Base Material and Conditioning /Repair Material | Dry Storage SBS (n, Mean, SD) | Wet Storage SBS (n, Mean, SD) | SBS Difference Dry and Wet Storage (%) | Lower/Upper 95% –CI Dry Storage | Lower/Upper 95% –CI Wet Storage |
|---|---|---|---|---|---|
| PMMA base + BM/Palapress | 20, 25.18, 2.59 | 20, 23.57, 2 | −6.42 | 23.76/ 26.607 | 22.067/ 25.072 |
| AM base + B/freeform plast | 20, 6.87, 2.89 | 20, 8.85, 1.96 | 28.9 | 5.444/ 8.29 | 7.351/ 10.356 |
| AM base + FB/freeform plast | n.a. | 20, 7.71, 2.24 | n.a. | n.a. | 6.207/ 9.212 |
| AM base + B-FB/freeform plast | n.a. | 20, 15.32, 4.39 | n.a. | n.a. | 13.813/ 16.818 |
| AM base+B/freeprint splint | 20, 15.76, 3.94 | 20, 8.37, 1.43 | −46.9 | 14.334/ 17.181 | 6.871/ 9.876 |
| AM base+FB/freeform fixgel | n.a. | 20, 14.31, 3.6 | n.a. | n.a. | 12.812/ 15.817 |
| AM base+B/freeform fixgel | 20, 8.65, 4.78 | 20, 14.12, 3.21 | +63.3 | 7.222/ 10.068 | 12.615/ 15.62 |
| AM base+B-FB/freeform fixgel | n.a. | 20, 10.93, 3.26 | n.a. | n.a. | 9.425/ 12.43 |
| AM base+PS/primosplint | 20, 5.72, 3.4 | 20, 7.25,1.61 | +26.7 * | 4.3/ 7.147 | 5.747/ 8.752 |
| AM base+B/primosplint | 20, 4.01, 2.42 | 20, 7.22, 1.7 | +80.2 | 2.583/ 5.43 | 5.715/ 8.72 |
| AM base+B-PS/primosplint | 20, 6.73, 2.79 | 20, 6.2, 2.23 | −7.9 * | 5.306/ 8.153 | 4.698/ 7.703 |
| AM base+M/Palapress | 20, 19.56, 4.19 | 18 **, 12.19, 5.51 | −37.7 | 18.138/ 20.985 | 10.609/ 13.776 |
| AM base+B/Palapress | 20, 17.56, 3.02 | 20, 16.08, 6.91 | −8.4 * | 16.134/ 18.98 | 14.582/ 17.587 |
| AM base+BM/Palapress | 20, 22.7, 2.47 | 20, 19.18, 4.72 | −15.5 | 21.275/ 24.122 | 17.674/ 20.679 |
| AM base+NC/freeform fixgel | 17 **, 4.93, 2.49 | 20, 8.11, 2.36 | +64.3 | 3.39/ 6.477 | 6.607/ 9.612 |
| AM base+NC/freeform plast | 20, 4.45, 2.7 | 20, 3.48, 0.82 | −21.8 * | 3.028/ 5.875 | 1.981/ 4.986 |
| AM base+NC/freeprint splint | 20, 13.99, 3.31 | 20, 5.56, 2.83 | −60.2 | 12.562/ 15.409 | 4.059/ 7.064 |
| AM base+NC/Palapress | 20, 21.41, 4.06 | 19 **, 22.97, 5.42 | +7.3 * | 19.989/ 22.836 | 21.43/ 24.513 |
| AM base+NC/primosplint | 20, 3.92, 1.97 | 20, 2.96, 1.46 | −24.4 * | 2.498/ 5.345 | 1.462/ 4.467 |
References
- Türp, J.C.; Komine, F.; Hugger, A. Efficacy of stabilization splints for the management of patients with masticatory muscle pain: A qualitative systematic review. Clin. Oral Investig. 2004, 8, 179–195. [Google Scholar] [CrossRef] [PubMed]
- Nishigawa, K.; Bando, E.; Nakano, M. Quantitative study of bite force during sleep associated bruxism. J. Oral Rehabil. 2001, 28, 485–491. [Google Scholar] [CrossRef] [PubMed]
- List, T.; Axelsson, S. Management of TMD: Evidence from systematic reviews and meta-analyses. J. Oral Rehabil. 2010, 37, 430–451. [Google Scholar] [CrossRef]
- Berntsen, C.; Kleven, M.; Heian, M.; Hjortsjo, C. Clinical comparison of conventional and additive manufactured stabilization splints. Acta Biomater. Odontol. Scand. 2018, 4, 81–89. [Google Scholar] [CrossRef]
- Bell, R.B. A history of orthognathic surgery in north america. J. Oral Maxillofac. Surg. 2018, 76, 2466–2481. [Google Scholar] [CrossRef] [PubMed]
- Rückschloß, T.; Ristow, O.; Müller, M.; Kühle, R.; Zingler, S.; Engel, M.; Hoffmann, J.; Freudlsperger, C. Accuracy of patient-specific implants and additive-manufactured surgical splints in orthognathic surgery—A three-dimensional retrospective study. J. Craniomaxillofac. Surg. 2019, 47, 847–853. [Google Scholar] [CrossRef]
- Wolowski, A.; Eger, T.; Braas, R.; Gohr, J.; Weber, N.; Witanski, K.; Wörner, F. Long-term effects of splint therapy in patients with posttraumatic stress disease (PTSD). Clin. Oral Investig. 2020, 24, 1493–1497. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Johansson, A.; Omar, R.; Carlsson, G.E. Bruxism and prosthetic treatment: A critical review. J. Prosthodont. Res. 2011, 55, 127–136. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reyes-Sevilla, M.; Kuijs, R.H.; Werner, A.; Kleverlaan, C.J.; Lobbezoo, F. Comparison of wear between occlusal splint materials and resin composite materials. J. Oral Rehabil. 2018, 45, 539–544. [Google Scholar] [CrossRef] [PubMed]
- Baker, P.S.; Haywood, V.B.; Plummer, K.D. Method for immediate fabrication of an occlusal device. J. Prosthet. Dent. 2007, 98, 411–415. [Google Scholar] [CrossRef]
- Steele, J.G.; Wassell, R.W.; Walls, A.W. A comparative study of the fit and retention of interocclusal splints constructed from heat-cured and autopolymerized polymethylmethacrylate. J. Prosthet. Dent. 1992, 67, 328–330. [Google Scholar] [CrossRef]
- Bohnenkamp, D.M. Dimensional stability of occlusal splints. J. Prosthet. Dent. 1996, 75, 262–268. [Google Scholar] [CrossRef]
- Huettig, F.; Kustermann, A.; Kuscu, E.; Geis-Gerstorfer, J.; Spintzyk, S. Polishability and wear resistance of splint material for oral appliances produced with conventional, subtractive, and additive manufacturing. J. Mech. Behav. Biomed. Mater. 2017, 75, 175–179. [Google Scholar] [CrossRef]
- Marcel, R.; Reinhard, H.; Andreas, K. Accuracy of CAD/CAM-fabricated bite splints: Milling vs. 3D printing. Clin. Oral Investig. 2020. [Google Scholar] [CrossRef]
- Martorelli, M.; Gerbino, S.; Giudice, M.; Ausiello, P. A comparison between customized clear and removable orthodontic appliances manufactured using RP and CNC techniques. Dent. Mater. 2013, 29, e1–e10. [Google Scholar] [CrossRef]
- Salmi, M.; Paloheimo, K.S.; Tuomi, J.; Ingman, T.; Mäkitie, A. A digital process for additive manufacturing of occlusal splints: A clinical pilot study. J. R. Soc. Interface 2013, 10, 20130203. [Google Scholar] [CrossRef]
- Kessler, A.; Reymus, M.; Hickel, R.; Kunzelmann, K.H. Three-body wear of 3D printed temporary materials. Dent. Mater. 2019, 35, 1805–1812. [Google Scholar] [CrossRef] [PubMed]
- Kessler, A.; Reichl, F.X.; Folwaczny, M.; Högg, C. Monomer release from surgical guide resins manufactured with different 3D printing devices. Dent. Mater. 2020. [Google Scholar] [CrossRef] [PubMed]
- Quan, H.; Zhang, T.; Xu, H.; Luo, S.; Nie, J.; Zhu, X. Photo-curing 3D printing technique and its challenges. Bioact. Mater. 2020, 5, 110–115. [Google Scholar] [CrossRef]
- Fiedor, P.; Ortyl, J. A new approach to micromachining: High-precision and innovative additive manufacturing solutions based on photopolymerization technology. Materials 2020, 13, 2951. [Google Scholar] [CrossRef] [PubMed]
- Kerr, W.J. Appliance breakages. Br. J. Orthod. 1984, 11, 137–142. [Google Scholar] [CrossRef] [PubMed]
- Mariatos, G.; Frangou, M.; Polyzois, G.; Papadopoulos, T. Evaluation of shear bond strength of microwaveable acrylic resins in denture repair: A comparative study. Acta Odontol. Scand. 2006, 64, 244–248. [Google Scholar] [CrossRef] [PubMed]
- Mahadevan, V.; Krishnan, M.; Krishnan, C.S.; Azhagarasan, N.S.; Sampathkumar, J.; Ramasubramanian, H. Influence of surface modifications of acrylic resin teeth on shear bond strength with denture base resin-an invitro study. J. Clin. Diagn. Res. 2015, 9, ZC16–ZC21. [Google Scholar] [CrossRef] [PubMed]
- Sarac, Y.S.; Sarac, D.; Kulunk, T.; Kulunk, S. The effect of chemical surface treatments of different denture base resins on the shear bond strength of denture repair. J. Prosthet. Dent. 2005, 94, 259–266. [Google Scholar] [CrossRef] [PubMed]
- Dentistry—Polymer-Based Crown and Veneering Materials; International Organization for Standardization: Geneva, Switzerland, 2018; No. DIN EN ISO 10477:2018; p. 19.
- Akin, H.; Kirmali, O.; Tugut, F.; Coskun, M.E. Effects of different surface treatments on the bond strength of acrylic denture teeth to polymethylmethacrylate denture base material. Photomed. Laser Surg. 2014, 32, 512–516. [Google Scholar] [CrossRef] [PubMed]
- Jeong, K.-W.; Kim, S.-H. Influence of surface treatments and repair materials on the shear bond strength of CAD/CAM provisional restorations. J. Adv. Prosthodont. 2019, 11, 95–104. [Google Scholar] [CrossRef] [PubMed]
- Vallittu, P.K.; Lassila, V.P.; Lappalainen, R. Wetting the repair surface with methyl methacrylate affects the transverse strength of repaired heat-polymerized resin. J. Prosthet. Dent. 1994, 72, 639–643. [Google Scholar] [CrossRef]
- Perea-Lowery, L.; Vallittu, P.K. Resin adjustment of three-dimensional printed thermoset occlusal splints: Bonding properties—Short communication. J. Mech. Behav. Biomed. Mater. 2019, 95, 215–219. [Google Scholar] [CrossRef]
- Li, P.; Krämer-Fernandez, P.; Klink, A.; Xu, Y.; Spintzyk, S. Repairability of a 3D printed denture base polymer: Effects of surface treatment and artificial aging on the shear bond strength. J. Mech. Behav. Biomed. Mater. 2021, 114, 104227. [Google Scholar] [CrossRef]
- Younis, M.; Unkovskiy, A.; ElAyouti, A.; Geis-Gerstorfer, J.; Spintzyk, S. The Effect of various plasma gases on the shear bond strength between unfilled polyetheretherketone (PEEK) and veneering composite following artificial aging. Materials 2019, 12, 1447. [Google Scholar] [CrossRef] [Green Version]
- Alkurt, M.; Yeşil Duymuş, Z.; Gundogdu, M. Effect of repair resin type and surface treatment on the repair strength of heat-polymerized denture base resin. J. Prosthet. Dent. 2014, 111, 71–78. [Google Scholar] [CrossRef]
- Qaw, M.S.; Abushowmi, T.H.; Almaskin, D.F.; AlZaher, Z.A.; Gad, M.M.; Al-Harbi, F.A.; Abualsaud, R.; Ammar, M.M. A novel approach to improve repair bond strength of repaired acrylic resin: An in vitro study on the shear bond strength. J. Prosthodont. 2020, 29, 323–333. [Google Scholar] [CrossRef] [PubMed]
- Curtis, D.A.; Eggleston, T.L.; Marshall, S.J.; Watanabe, L.G. Shear bond strength of visible-light-cured resin relative to heat-cured resin. Dent. Mater. 1989, 5, 314–318. [Google Scholar] [CrossRef]
- Besegato, J.F.; Jussiani, E.I.; Andrello, A.C.; Fernandes, R.V.; Salomão, F.M.; Vicentin, B.L.S.; Dezan-Garbelini, C.C.; Hoeppner, M.G. Effect of light-curing protocols on the mechanical behavior of bulk-fill resin composites. J. Mech. Behav. Biomed. Mater. 2019, 90, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Shortall, A.C.; Hadis, M.A.; Palin, W.M. On the inaccuracies of dental radiometers. PLoS ONE 2021, 16, e0245830. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, Y.; Chai, J.; Kawaguchi, M. Effect of water sorption on the resistance to plastic deformation of a denture base material relined with four different denture reline materials. Int. J. Prosthodont. 1998, 11, 49–54. [Google Scholar]
- Lin, C.H.; Lin, Y.M.; Lai, Y.L.; Lee, S.Y. Mechanical properties, accuracy, and cytotoxicity of UV-polymerized 3D printing resins composed of Bis-EMA, UDMA, and TEGDMA. J. Prosthet. Dent. 2020, 123, 349–354. [Google Scholar] [CrossRef]
- Lutz, A.M.; Hampe, R.; Roos, M.; Lümkemann, N.; Eichberger, M.; Stawarczyk, B. Fracture resistance and 2-body wear of 3-dimensional-printed occlusal devices. J. Prosthet. Dent. 2019, 121, 166–172. [Google Scholar] [CrossRef]
- Schulte, J.K.; Anderson, G.C.; Sakaguchi, R.L.; DeLong, R. Wear resistance of isosit and polymethyl methacrylate occlusal splint material. Dent. Mater. 1987, 3, 82–84. [Google Scholar] [CrossRef]
- Casey, J.; Dunn, W.J.; Wright, E. In vitro wear of various orthotic device materials. J. Prosthet. Dent. 2003, 90, 498–502. [Google Scholar] [CrossRef]
- Danesh, G.; Lippold, C.; Ziebura, T.; Reinhardt, K.J.; Schäfer, E.; Ehmer, U. In-vitro investigation on suitability of light-cured resins for interocclusal splints: Part II: Surface hardness. J. Orofac. Orthop. 2006, 67, 138–147. [Google Scholar] [CrossRef]
- Wiegand, A.; Stucki, L.; Hoffmann, R.; Attin, T.; Stawarczyk, B. Repairability of CAD/CAM high-density PMMA- and composite-based polymers. Clin. Oral Investig. 2015, 19, 2007–2013. [Google Scholar] [CrossRef] [PubMed]
- Rosca, B.; Ramalho, S.; Sampaio-Fernandes, J.C.; Portugal, J. Reparability of two different CAD/CAM polymer materials using a light-cured composite and universal adhesives. Rev. Port. Estomatol. Med. Dentária Cir. Maxilofac. 2016, 57, 189–196. [Google Scholar] [CrossRef] [Green Version]
- Edelhoff, D.; Schweiger, J.; Prandtner, O.; Trimpl, J.; Stimmelmayr, M.; Güth, J.F. CAD/CAM splints for the functional and esthetic evaluation of newly defined occlusal dimensions. Quintessence Int. 2017, 48, 181–191. [Google Scholar] [CrossRef] [PubMed]
- Lagouvardos, P.E.; Polyzois, G.L. Shear bond strength between composite resin and denture teeth: Effect of tooth type and surface treatments. Int. J. Prosthodont. 2003, 16, 499–504. [Google Scholar]
- Zhang, Z.C.; Li, P.L.; Chu, F.T.; Shen, G. Influence of the three-dimensional printing technique and printing layer thickness on model accuracy. J. Orofac. Orthop. 2019, 80, 194–204. [Google Scholar] [CrossRef] [PubMed]
- Unkovskiy, A.; Bui, P.H.; Schille, C.; Geis-Gerstorfer, J.; Huettig, F.; Spintzyk, S. Objects build orientation, positioning, and curing influence dimensional accuracy and flexural properties of stereolithographically printed resin. Dent. Mater. 2018, 34, e324–e333. [Google Scholar] [CrossRef]
- Reymus, M.; Fabritius, R.; Keßler, A.; Hickel, R.; Edelhoff, D.; Stawarczyk, B. Fracture load of 3D-printed fixed dental prostheses compared with milled and conventionally fabricated ones: The impact of resin material, build direction, post-curing, and artificial aging-an in vitro study. Clin. Oral Investig. 2020, 24, 701–710. [Google Scholar] [CrossRef]
- Alifui-Segbaya, F.; Bowman, J.; White, A.R.; George, R.; Fidan, I.; Love, R.M. Chemical characterization of additively manufactured methacrylates for dental devices. Addit. Manuf. 2020, 31, 100944. [Google Scholar] [CrossRef]
- Revilla-León, M.; Meyers, M.J.; Zandinejad, A.; Özcan, M. A review on chemical composition, mechanical properties, and manufacturing work flow of additively manufactured current polymers for interim dental restorations. J. Esthet. Restor. Dent. 2019, 31, 51–57. [Google Scholar] [CrossRef] [Green Version]
- Revilla-León, M.; Özcan, M. Additive manufacturing technologies used for processing polymers: Current status and potential application in prosthetic dentistry. J. Prosthodont. 2019, 28, 146–158. [Google Scholar] [CrossRef] [Green Version]
- Cattoni, F.; Teté, G.; Calloni, A.M.; Manazza, F.; Gastaldi, G.; Capparè, P. Milled versus moulded mock-ups based on the superimposition of 3D meshes from digital oral impressions: A comparative in vitro study in the aesthetic area. BMC Oral Health 2019, 19, 230. [Google Scholar] [CrossRef] [PubMed]
- Capparè, P.; Tetè, G.; Sberna, M.T.; Panina-Bordignon, P. The emerging role of stem cells in regenerative dentistry. Curr. Gene Ther. 2020, 20, 259–268. [Google Scholar] [CrossRef] [PubMed]
- Gao, J.; Liu, L.; Gao, P.; Zheng, Y.; Hou, W.; Wang, J. Intelligent occlusion stabilization splint with stress-sensor system for bruxism diagnosis and treatment. Sensors 2019, 20, 89. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Capparé, P.; Vinci, R.; di Stefano, D.A.; Traini, T.; Pantaleo, G.; Gherlone, E.F.; Gastaldi, G. Correlation between initial BIC and the insertion torque/depth integral recorded with an instantaneous torque-measuring implant motor: An in vivo study. Clin. Implant. Dent. Relat. Res. 2015, 17, e613–e620. [Google Scholar] [CrossRef] [PubMed]


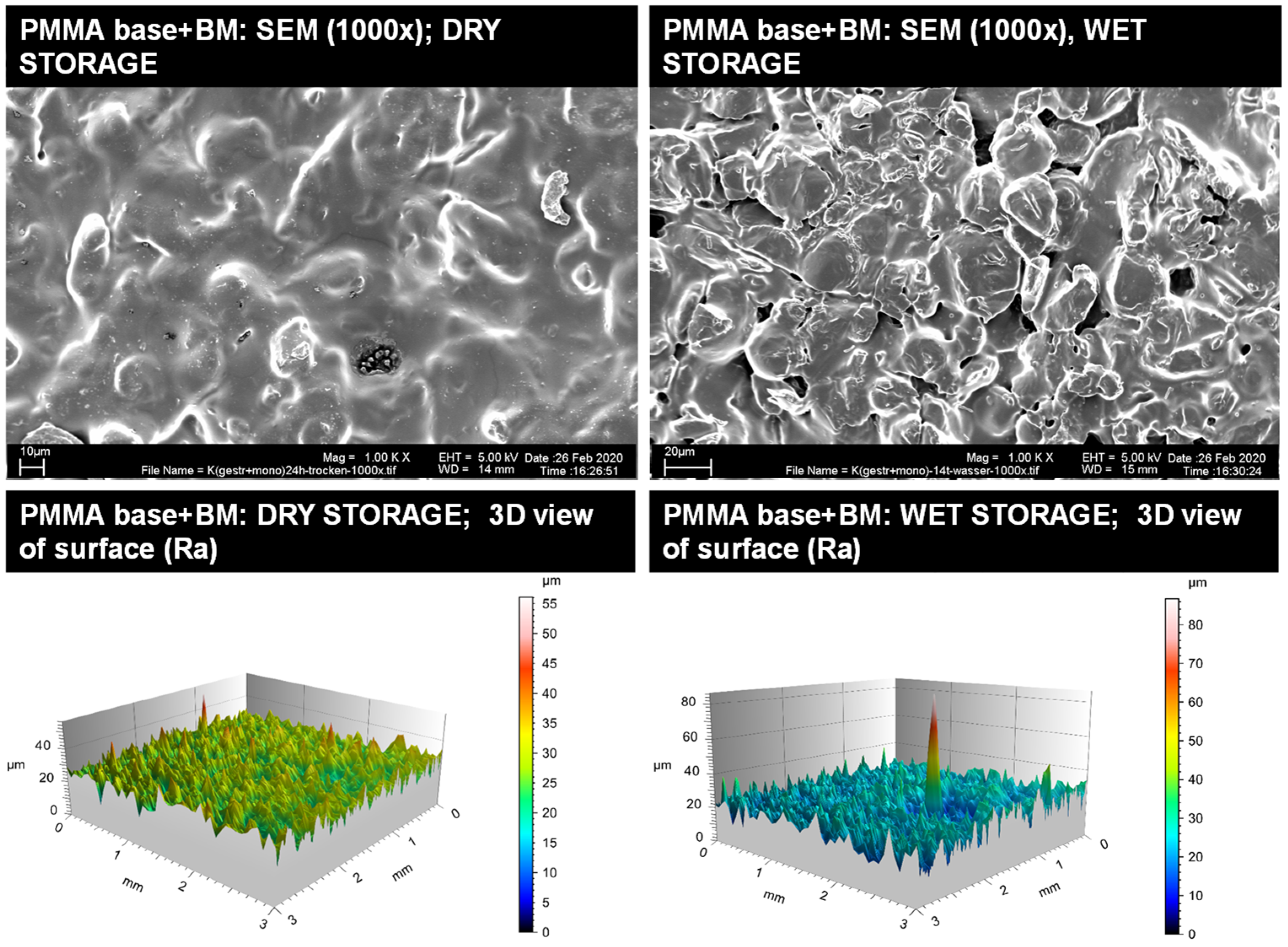





| Base Material and Conditioning | Dry Storage Ra (n Profile Lines 1, Mean, SD) | Wet Storage Ra (n Profile Lines 1, Mean, SD) | p-Value |
|---|---|---|---|
| PMMA base + BM | 240, 3.37, 0.5 | 240, 3.69, 0.89 | <0.0001 |
| AM base + B | 240, 4.89, 1.5 | 240, 6.23, 1.07 | <0.0001 |
| AM base + B-FB | 0, n.a., n.a. | 240, 0.77, 0.79 | n.a. |
| AM base + BM | 240, 5.23, 1.33 | 240, 5.89, 0.89 | <0.0001 |
| AM base + B-PS | 240, 1.74, 1.08 | 240, 1.68, 2.17 | <0.0001 |
| AM base + FB | 0, n.a., n.a. | 240, 0.6, 0.7 | n.a. |
| AM base + M | 240, 0.93, 0.18 | 240, 0.5, 0.2 | <0.0001 |
| AM base + NC | 240, 0.75, 0.39 | 240, 0.68, 0.31 | <0.0001 |
| AM base + PS | 240, 1.13, 0.79 | 240, 0.26, 0.23 | <0.0001 |
| Light Curing Repair Material (Resin) 2.5 mm of Thickness | Light Intensity on the Bonding Interface mW/cm2 (Mean) |
|---|---|
| no material in cylinder (air) | 780 |
| freeform fixgel in brass cylinder without cylinder | 125 560 |
| freeform plast in brass cylinder without cylinder | 113 510 |
| Primosplint in brass cylinder without cylinder | 116 480 |
| freeprint splint in brass cylinder without cylinder | 158 510 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kuscu, E.; Klink, A.; Spintzyk, S.; Kraemer Fernandez, P.; Huettig, F. Bonding Interface and Repairability of 3D-Printed Intraoral Splints: Shear Bond Strength to Current Polymers, with and without Ageing. Materials 2021, 14, 3935. https://doi.org/10.3390/ma14143935
Kuscu E, Klink A, Spintzyk S, Kraemer Fernandez P, Huettig F. Bonding Interface and Repairability of 3D-Printed Intraoral Splints: Shear Bond Strength to Current Polymers, with and without Ageing. Materials. 2021; 14(14):3935. https://doi.org/10.3390/ma14143935
Chicago/Turabian StyleKuscu, Ebru, Andrea Klink, Sebastian Spintzyk, Pablo Kraemer Fernandez, and Fabian Huettig. 2021. "Bonding Interface and Repairability of 3D-Printed Intraoral Splints: Shear Bond Strength to Current Polymers, with and without Ageing" Materials 14, no. 14: 3935. https://doi.org/10.3390/ma14143935







