The presented study shows what protocols are used by Polish orthodontists in the retention phase, what features, according to Polish orthodontists, present various orthodontic wires, and how orthodontists fabricate fixed orthodontic retainers. It should be noted that, when it comes to materials for bonding fixed retention, Polish orthodontists trust their skills and follow the principle “it works in my hands”. This seems important from the point of view of the orthodontic materials sales market.
4.1. Study Group
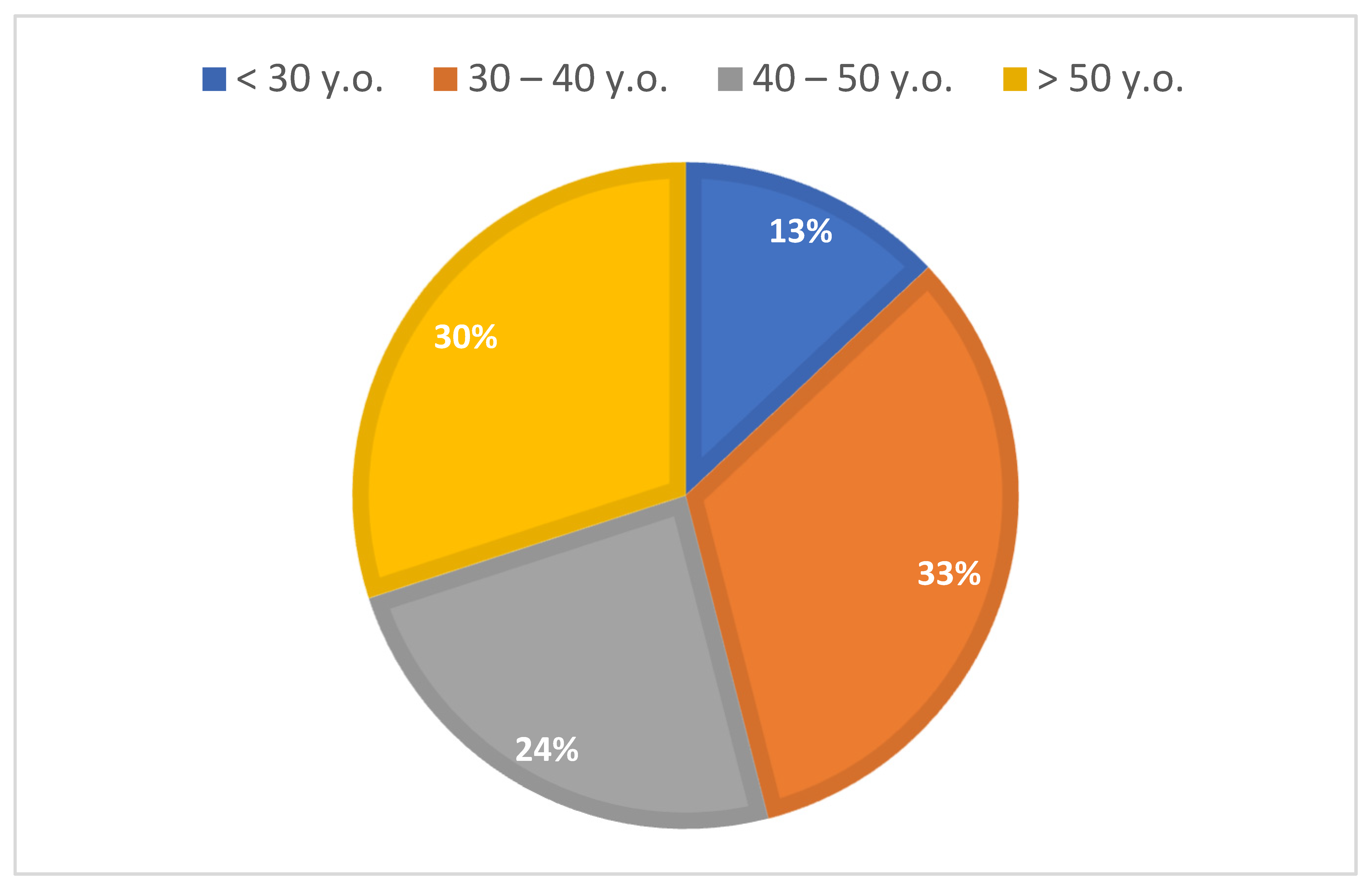
The first question was used to determine the age group. Questions 2–6 were asked to provide information on the type of retention appliances used, the scope of the duration of the retention phase, and the frequency of follow-up visits. The latter questions referred to the type of fixed retention used, detailing the wire or FRC used, and the bonding material used. In questions 1, 2, and 4, selecting only one answer was possible, while, in questions 3 and 5–17, choosing multiple answers was allowed.
Sample size assessment was not possible in the present study because the authors were dealing with a multi-path analysis of non-parametric data, which includes the opinions of Polish clinicians concerning the use various materials for fixed retention appliances. According to the Supreme Medical Council in Poland, there are 1296 clinically active specialists in orthodontics [
23]. Thus, the present study on 104 clinicians can be considered representative for all Polish orthodontic treatment providers, as they constitute more than 8% of the whole group.
4.2. Retention Protocols
The finding that almost all respondents used double retention, fixed and removable, is inconsistent with previous reports, where doctors who used double retention were in the minority of those surveyed. Most clinicians preferred to use removable retention [
8,
9,
10,
11,
14,
18,
19]. Scientific evidence shows that it is permanent retention that ensures the best maintenance of treatment results for a longer period of time [
24]. Interestingly, only recently, in light of new scientific evidence, have orthodontists begun to declare a routine use of fixed retention [
8,
14].
The use of double retention by most Polish practitioners confirms the high attention they pay to maintaining the results of the active treatment. Double retention is also gaining popularity outside Europe; however, it is still not a standard [
25]. Retention type is usually based on the doctor’s clinical judgment and experience [
9,
10,
11,
19]. Factors influencing the final decision on the type of retention used include oral hygiene, case “severity”, type of malocclusion, and use of extraction during treatment, especially in maxilla [
9,
12,
16,
19]. However, Malaysian orthodontists do not believe that the use of extractions should have an impact on the type of retention used [
10]. Interestingly, Al-Moghrabi et al. [
26] pointed out that double retention was widely prescribed, even if little was known about its additional benefits, and it required more attention to oral hygiene. However, there are publications reporting that double retention for a prolonged period noticeably reduces tooth displacement, especially of the lower anterior teeth [
27]. It is evident that there is a lack of high quality clinical scientific studies, especially randomized clinical trials or cohort studies, which makes it difficult to provide clinical recommendations based on scientific evidence.
Dental aesthetics is one of the key needs leading a patient to the dental chair, and high aesthetic demands are common among patients [
28,
29]. The number of lawsuits against orthodontists has dramatically increased in the recent years [
30]. Therefore, it seems rational and economically justified to introduce double retention in everyday practice to maintain positions of the teeth achieved during the active phase of treatment. A fixed retainer and a thermally-formed splint are often recommended, since a fixed retainer holds the teeth in the anterior region while the patient is not wearing a removable retainer, and the splint is able to additionally protect the patient from displacement of posterior teeth (as well as anterior teeth in the event of fixed retention failure). In association with the results of the survey, it should be noted that, according to the respondents, the GC is the type of wire that detaches the least frequently. This can be very important for everyday orthodontic practice. A low probability of detachment allows the doctor to convince the patient of the effectiveness of this type of fixed retention, regardless of the physical characteristics of the wire, causing a potential risk to the stability of treatment outcomes in the future, known only to the doctor from scientific reports.
As far as the duration of retention is concerned, more than 50% of the practitioners declared recommending life-long retention to their patients. This approach is similar to that reported in the studies by Pratt et al. [
16] and Padmos et al. [
31]. On the other side, quite a high percentage of clinicians chose different retention periods: “at least as active treatment”, “at least two times longer as active treatment”, or “at least a half of the active treatment”. According to scientific evidence on the stability of orthodontic alignment, ceasing retention at any time does not guarantee stable orthodontic alignment [
32]. Any malalignment of the anterior teeth may be esthetically unacceptable for the patient. On the other side, retention is associated with cost, discomfort, and potential iatrogenic effects [
33], and it requires cooperation [
34]. Thus, individual approach, as in “it depends on the case”, is also reflected in the present study.
In a 1984 Polish textbook on orthodontics by Łabiszewska-Jaruzelska, it is stated that a fixed appliance should be left passive in the mouth for several months, and then it should be replaced by a removable appliance; however, how long the retention phase should last is not recommended [
35]. This statement seemed to influence the responses within the questionnaire.
The phrases: “at least as long as active treatment” and “at least a half of the active treatment”, describing the length of the retention period, come from another Polish orthodontic textbook, “Zarys współczesnej ortodoncji”, by Karłowska, published in 2016 [
36], which is currently used in under- and postgraduate teaching. The mentioned recommendations on retention duration do not refer to fixed appliance treatment; they refer to prolonged use of functional appliances after achieving the desired effect of treatment. None of the two handbooks provides a source citation as scientific background for the recommendation of orthodontic retention. In the latest handbook edition [
36], it is indicated that the retention phase after treatment with fixed appliances requires a longer period. Thus, it can be supposed that, due to a misunderstanding, some practitioners choose retention protocols not recommended to fixed but, rather, to removable appliance treatment.
Most respondents declared seeing their patients one month following debonding fixed appliances, then after 3 months, and then every 6 months. From the point of view of the scientific evidence, this approach seems optimal. The most frequently chosen answers indicated that clinicians know about the need of frequent controls during the first six-months period, which is scientifically valid [
15]. A recent meta-analysis [
15] showed that most failures of fixed retention occur within the first 6 months after bonding retainer, and, during that time the patient should be under frequent supervision. However, almost 30% of the clinicians declared recommending the first appointment with fixed retention after 3 months, and 17.3% after 6 months. This approach relies on the patient’s cooperation and “emergency” visits in case of a failure. Thus, the patient could be seen earlier and more often to avoid possible relapse of malocclusion. A similar approach to follow-up was described in the study by Padmos from 2018 [
31]. However, in most of the survey papers in the literature on orthodontic retention [
9,
10,
12,
14,
16,
17,
18,
19], the authors pointed out the need for more frequent follow-up visits (at least four) during the first year. Further monitoring of retention tends to be delegated to general practitioners, or even left to the patient’s self-monitoring. Nevertheless, unwanted tooth movement has been shown to occur, despite proper adhesion of retainers in the oral cavity, especially in the maxilla [
37]. This means that, if the patient was monitored long-term by the orthodontist, the latter, having the appropriate documentation, could detect these displacements earlier; thus, the orthodontist could introduce less aggressive and cheaper retreatment, for example, in the form of several aligners [
38].
All the participants declared that they bonded fixed retainers directly. Since two answers were possible, indirect bonding was indicated by a small percentage of the respondents, as well. According to a recent systematic review [
15], there is no difference concerning the frequency of failures referring to direct versus indirect bonding. However, indirect bonding saves chair time [
39]. The reason why Polish orthodontists bond their retainers directly may be the desire to avoid the laboratory costs (which may not seem cost-effective). An interesting, recently reported novelty is finding application in fixed post-orthodontic retention bonding using 3D printed materials [
40]. These devices, appropriately designed on a 3D virtual model, could greatly facilitate direct bonding of retention wires in the future.
4.3. Materials Used for Fixed Retention
Two survey studies could be found asking about the type of wire used; both the studies were performed by the same group of authors [
8,
31]. However, they asked only about type of wire chosen, not reasons for such a choice. The popularity of the material reported in this article was similar to that in the present study. Steel rectangular wire, steel round wire, and gold chain were the most popular, similar to that among Polish clinicians, wherein steel rectangular braided wire was also the most popular, followed by a gold chain and a round steel wire (the difference between the last two is statistically insignificant).
The fact that more than 50% of the practitioners believed that they could perfectly maintain the results of the active treatment may indicate that the clinicians believe in the effectiveness of retention appliances. On the other side, almost 50% agreed that maintaining perfect positions of the teeth was difficult. It is possible that the clinicians see the main reasons for their problems with retention in patients’ cooperation, since more than 50% declared that their patients fail to cooperate during the retention phase.
The diversity of wires used for fixed retention reflects a lack of clinical scientific evidence proving a lower failure rate of any wire [
18,
32]. Most of the survey studies drew attention to the lack of clear clinical guidelines and sought the guidelines on which type of retention should be applied [
9,
11,
14].
Most clinicians using fiber-reinforced composite preferred a tape to a knot. No studies have been found in the literature that could be used for the comparison with this finding of the present questionnaire study. No studies have reported on a lower failure rate of a tape versus knot. However, tape may require less occlusal space and, therefore, is chosen more often. A recent report has shown that FRC retention can be as stable as the one obtained with steel wires [
41]. FRC retention is more sensitive to operator skills, and, with imperfect bonding, the failure rate could be much higher [
15]. As an example, when composite resin is fully polymerized, high-quality fiber strips strongly fuse with one another and, thus, can significantly increase the resin strength and durability by up to 300% compared to inaccurately polymerized material [
42].
The most popular type of wire used in the present questionnaire is stainless steel braided wire, but nearly 36% of clinicians do not know its dimensions. It can be supposed that they buy marketed, popular retention wires available on the market and do not check their sizes nor the clinical characteristics of the material used. The respondents mentioned that stainless steel braided wire was easy to bend and bond, rarely detached from the teeth, and usually correctly maintained the position of the teeth. This is consistent with the findings of Arnold et al. [
43], who reported that braided 0.016 × 0.022-inch stainless steel wire was torque resistant and should replace multistranded round wires. The use of multistranded round wires was declared by only 13% of the practitioners. The interviewed group believed that a round wire retainer was difficult to bend and bond, detached more often from the teeth, did not maintain the position of the teeth satisfactorily, and easily became deformed. It may indicate that most clinicians were familiar with reports on adverse effects described, including wire untwisting and torquing teeth [
44,
45]. Interestingly, doctors who use gold chains were the group that was most convinced to the material of their choice, and they most negatively assessed the other wire types. The comparison of the proportions in the responses showed that, according to the respondents, it is the gold chain that best maintains the position of the teeth. This is contrary to many in-vitro studies that indicate that gold chain wire has the lowest bending and torsional stiffness, and it is not resistant to the masticatory forces, which may lead to activation in long-term clinical use [
46].
The most popular type of material used to bond fixed retention was flowable composite; however, it can be supposed that the respondents did not consider it necessary to use a specialized composite dedicated to retention. Moreover, less than 10% used condensable composites, and 5.7% used chemically-cured composites for indirect bonding. The use of composite materials dedicated to bonding retainers confirmed knowledge of new specialized products; the wide use of flowable composite dedicated to dental restorations may be caused by high prices of orthodontic materials.
Retention with the use of fiber-einforced composite (FRC) was performed by approximately 30% of the respondents, mainly in periodontal patients. In addition, in these cases, a flowable composite was most often used to bond to the tooth surface. No questionnaire studies reporting on the use of different bonding materials for fixed retention could be found and used for discussion.