A Structural Analysis of AI Implementation Challenges in Healthcare
Abstract
1. Introduction
2. Literature Review
2.1. Insufficient Data
2.2. Social Issues
2.3. Clinical Implementations
2.4. High Costs
2.5. Black-Box Scenario
2.6. Data Acquisition
2.7. Introduction of Innovative and New-Generation Tools
2.8. Missing Compassion
2.9. Data Misuse
2.10. Data Privacy and Security
2.11. Technology Development
3. Methodology
3.1. Data Collection
3.2. Interpretive Structural Modeling (ISM)
3.2.1. Structural Self-Interaction Matrix (SSIM)
3.2.2. Reachability Matrix
- (i)
- if the (x, y) entry in the SSIM is V, the reachability matrix entry becomes 1, and the (y, x) entry is 0;
- (ii)
- if the (x, y) entry in SSIM is A, the reachability matrix entry becomes 0, and the (y, x) entry becomes 1;
- (iii)
- if the (x, y) entry is X in the SSIM, the reachability matrix entry becomes 1, and the (y, x) entry is also 1;
- (iv)
- if the (x, y) entry is O in the SSIM, the reachability matrix entry becomes 0, and the (y, x) entry is 0.
3.2.3. Level Partition
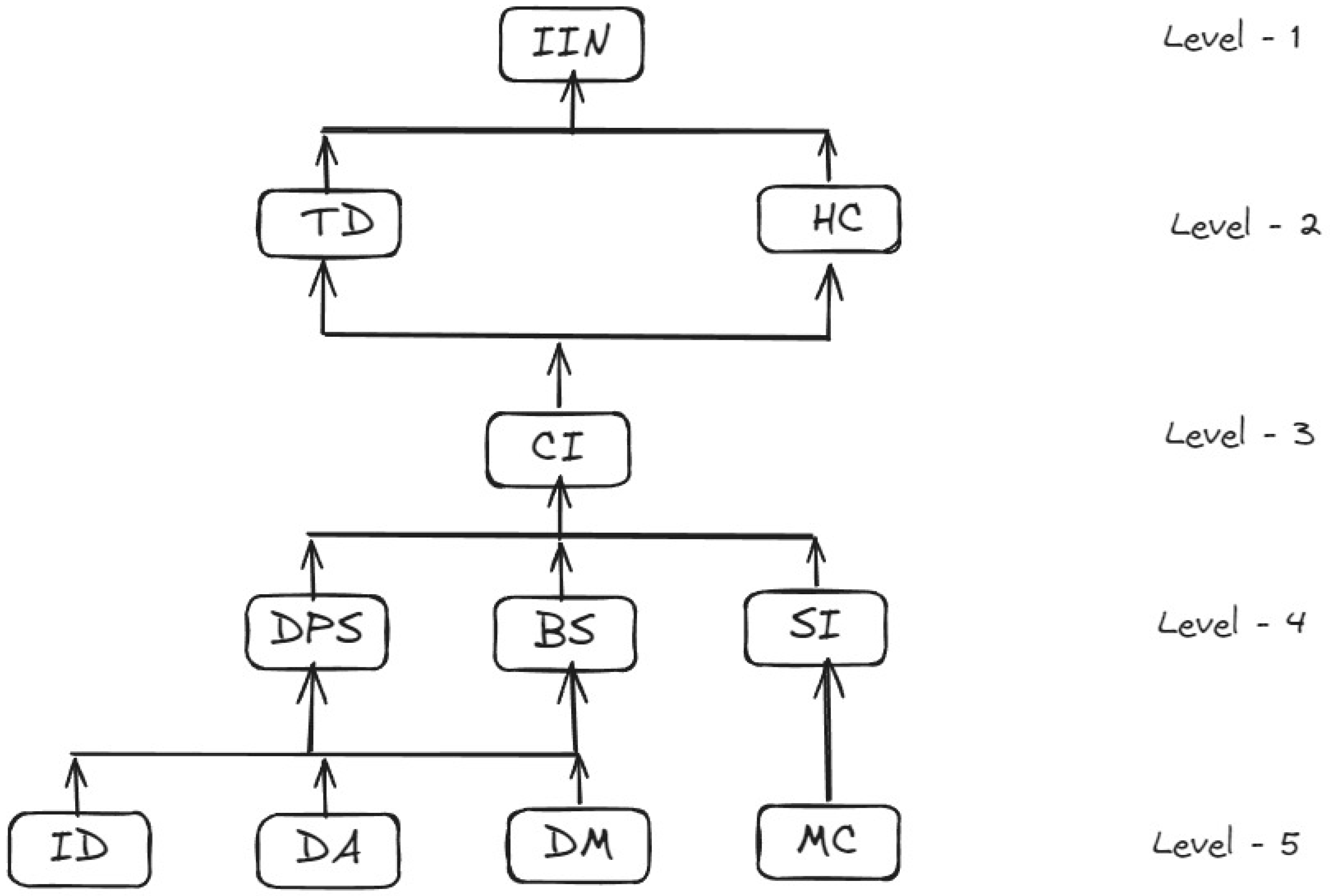
3.2.4. Formation of Interpretive Structural Model
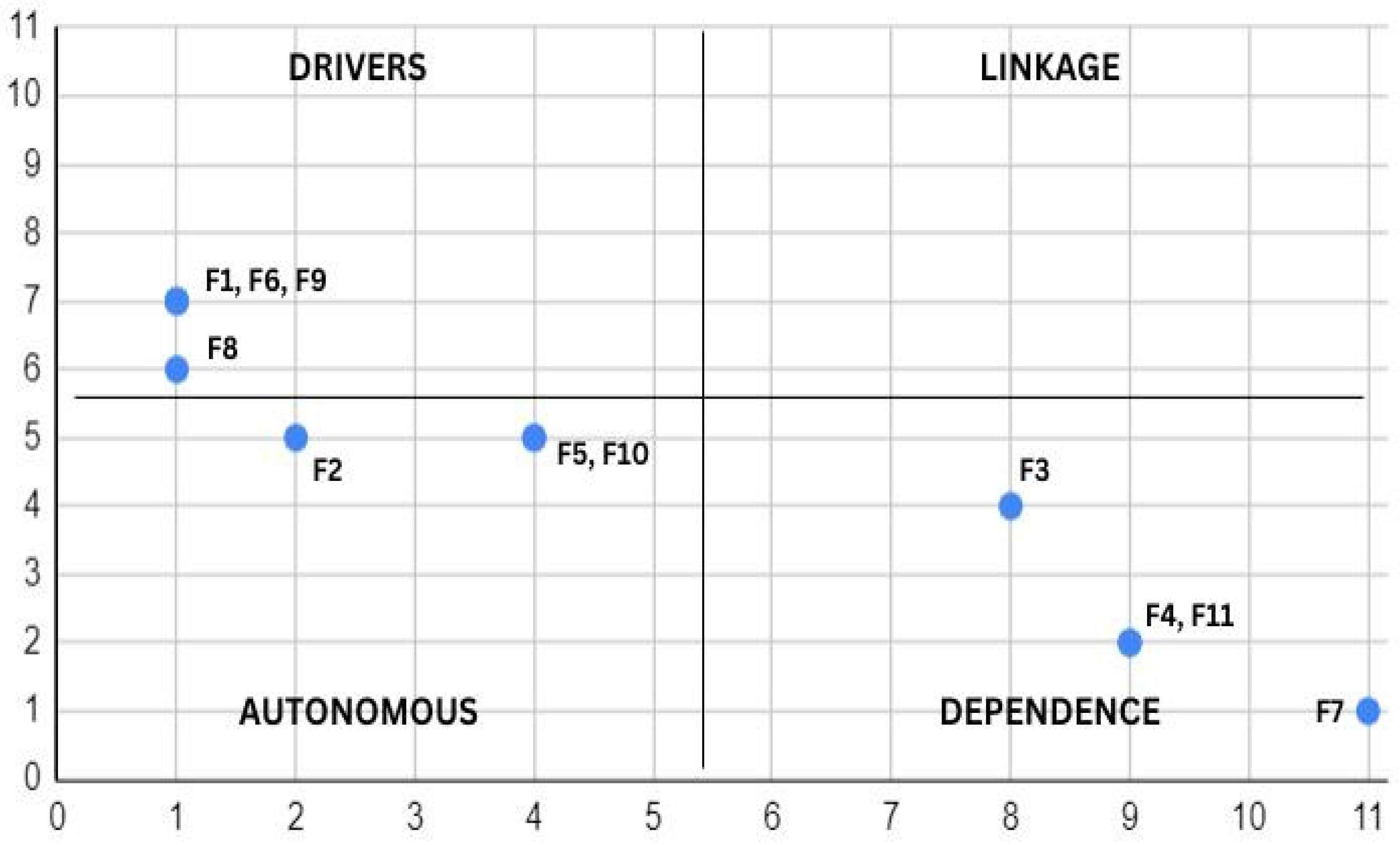
3.2.5. MICMAC Analysis
4. Results and Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Zahlan, A.; Ranjan, R.P.; Hayes, D. Artificial intelligence innovation in healthcare: Literature review, exploratory analysis, and future research. Technol. Soc. 2023, 74, 102321. [Google Scholar] [CrossRef]
- Stewart, J.; Sprivulis, P.; Dwivedi, G. Artificial intelligence and machine learning in emergency medicine. Emerg. Med. Australas. 2018, 30, 870–874. [Google Scholar] [CrossRef]
- Jimma, B.L. Artificial intelligence in healthcare: A bibliometric analysis. Telemat. Inform. Rep. 2023, 9, 100041. [Google Scholar] [CrossRef]
- Aung, Y.Y.M.; Wong, D.C.S.; Ting, D.S.W. The promise of artificial intelligence: A review of the opportunities and challenges of artificial intelligence in healthcare. Br. Med. Bull. 2021, 139, 4–15. [Google Scholar] [CrossRef]
- Gille, F.; Jobin, A.; Ienca, M. What we talk about when we talk about trust: Theory of trust for AI in healthcare. Intell.-Based Med. 2020, 1, 100001. [Google Scholar]
- Paul, D.; Sanap, G.; Shenoy, S.; Kalyane, D.; Kalia, K.; Tekade, R.K. Artificial intelligence in drug discovery and development. Drug Discov. Today 2021, 26, 80–93. [Google Scholar]
- Sun, T.Q.; Medaglia, R. Mapping the challenges of Artificial Intelligence in the public sector: Evidence from public healthcare. Gov. Inf. Q. 2019, 36, 368–383. [Google Scholar] [CrossRef]
- Neyigapula, B.S. AI in Healthcare: Enhancing Diagnosis, Treatment, and Healthcare Systems for a Smarter Future in India. Adv. Bioeng. Biomed. Sci. Res. 2023, 6, 171–177. [Google Scholar]
- Bartoletti, I. AI in healthcare: Ethical and privacy challenges. In Artificial Intelligence in Medicine: 17th Conference on Artificial Intelligence in Medicine, AIME 2019, Poznan, Poland, 26–29 June 2019; Proceedings 17; Springer International Publishing: Cham, Switzerland, 2019; pp. 7–10. [Google Scholar]
- Shah, R.; Chircu, A. IoT and AI in healthcare: A systematic literature review. Issues Inf. Syst. 2018, 19, 33–41. [Google Scholar]
- Khaled, N.; Turki, A.; Aidalina, M. Implications of artificial intelligence in healthcare delivery in the hospital settings. Int. J. Public Health Clin. Sci. 2019, 6, 22–38. [Google Scholar]
- Reddy, S.; Fox, J.; Purohit, M.P. Artificial intelligence-enabled healthcare delivery. J. R. Soc. Med. 2018, 112, 22–28. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.-C.; Chen, T.-C.T.; Chiu, M.-C. An improved explainable artificial intelligence tool in healthcare for hospital recommendation. Healthc. Anal. 2023, 3, 100147. [Google Scholar] [CrossRef]
- Srinivasu, P.N.; Sandhya, N.; Jhaveri, R.H.; Raut, R. From blackbox to explainable AI in healthcare: Existing tools and case studies. Mob. Inf. Syst. 2022, 2022, 167821. [Google Scholar]
- Mueller, B.; Kinoshita, T.; Peebles, A.; Graber, M.A.; Lee, S. Artificial intelligence and machine learning in emergency medicine: A narrative review. Acute Med. Surg. 2022, 9, e740. [Google Scholar] [CrossRef]
- Rebelo, A.D.; Verboom, D.E.; dos Santos, N.R.; de Graaf, J.W. The impact of artificial intelligence on the tasks of mental healthcare workers: A scoping review. Comput. Hum. Behav. Artif. Hum. 2023, 1, 100008. [Google Scholar]
- Bertsimas, D.; Bjarnadóttir, M.V.; Kane, M.A.; Kryder, J.C.; Pandey, R.; Vempala, S.; Wang, G. Algorithmic prediction of health-care costs. Oper. Res. 2008, 56, 1382–1392. [Google Scholar] [CrossRef]
- van Mens, K.; Kwakernaak, S.; Janssen, R.; Cahn, W.; Lokkerbol, J.; Tiemens, B. Predicting future service use in Dutch mental healthcare: A machine learning approach. Adm. Policy Ment. Health Ment. Health Serv. Res. 2021, 49, 116–124. [Google Scholar]
- Mangla, S.K.; Luthra, S.; Mishra, N.; Singh, A.; Rana, N.P.; Dora, M.; Dwivedi, Y. Barriers to effective circular supply chain management in a developing country context. Prod. Plan. Control. 2018, 29, 551–569. [Google Scholar]
- Mishra, A.; Dutta, P.; Kakoti, S. Exploring key success factors of Indian pharmaceutical supply chain using interpretive structural modeling. In Multi-Criteria Decision Analysis in Management; IGI Global: Hershey, PA, USA, 2020; pp. 46–61. [Google Scholar]
- Diabat, A.; Govindan, K. An analysis of the drivers affecting the implementation of green supply chain management. Resour. Conserv. Recycl. 2011, 55, 659–667. [Google Scholar] [CrossRef]
- Tripathy, S.; Sahu, S.; Ray, P.K. Interpretive structural modelling for critical success factors of R&D performance in Indian manufacturing firms. J. Model. Manag. 2013, 8, 212–240. [Google Scholar] [CrossRef]
- Chakraborty, K.; Mondal, S.; Mukherjee, K. Critical analysis of enablers and barriers in extension of useful life of automotive products through remanufacturing. J. Clean. Prod. 2019, 227, 1117–1135. [Google Scholar]
- Sushil. Interpreting the interpretive structural model. Glob. J. Flex. Syst. Manag. 2012, 13, 87–106. [Google Scholar]
- Thakkar, J.; Deshmukh, S.G.; Gupta, A.D.; Shankar, R. Selection of third-party logistics (3PL): A hybrid approach using interpretive structural modeling (ISM) and analytic network process (ANP). Supply Chain Forum Int. J. 2005, 6, 32–46. [Google Scholar] [CrossRef]
- Thakkar, J.; Deshmukh, S.G.; Gupta, A.D.; Shankar, R. Development of balanced scorecard: An integrated approach of interpretive structural modeling (ISM) and analytic network process (ANP). Int. J. Product. Perform. Manag. 2007, 56, 25–59. [Google Scholar]
- Iqbal, M.; Ma, J.; Ahmad, N.; Ullah, Z.; Hassan, A. Energy-Efficient supply chains in construction industry: An analysis of critical success factors using ISM-MICMAC approach. Int. J. Green Energy 2022, 20, 265–283. [Google Scholar]
- Akpinar, H.; Caylan, D.O. Modeling organizational resilience in maritime business: An ISM and MICMAC approach. Bus. Process. Manag. J. 2023, 29, 597–629. [Google Scholar] [CrossRef]
- Agarwal, R.; Bhadauria, A.; Kaushik, H.; Swami, S.; Rajwanshi, R. ISM-MICMAC-based study on key enablers in the adoption of solar renewable energy products in India. Technol. Soc. 2023, 75, 102375. [Google Scholar] [CrossRef]
- Gadekar, R.; Sarkar, B.; Gadekar, A. Model development for assessing inhibitors impacting Industry 4.0 implementation in Indian manufacturing industries: An integrated ISM-Fuzzy MICMAC approach. Int. J. Syst. Assur. Eng. Manag. 2022, 15, 646–671. [Google Scholar] [CrossRef]
- Asif, M.; Sarim, M.; Khan, W.; Khan, S. ISM- and MICMAC-based modelling of dairy supply chain: A study of enablers in Indian economy perspective. Br. Food J. 2023, 126, 578–594. [Google Scholar] [CrossRef]
- Feng, X.; Li, E.; Li, J. Critical factors identification of digital innovation in manufacturing enterprises: Three stage hybrid DEMATEL–ISM–MICMAC approach. Soft Comput. 2024, 28, 7341–7361. [Google Scholar] [CrossRef]
- Govindan, K.; Palaniappan, M.; Zhu, Q.; Kannan, D. Analysis of third party reverse logistics provider using interpretive structural modeling. Int. J. Prod. Econ. 2012, 140, 204–211. [Google Scholar] [CrossRef]
- Attri, R.; Dev, N.; Sharma, V. Interpretive structural modeling (ISM) approach: An overview. Res. J. Manag. Sci. 2013, 2319, 1171. [Google Scholar]
- Sivaprakasam, R.; Selladurai, V.; Sasikumar, P. Implementation of interpretive structural modelling methodology as a strategic decision making tool in a Green Supply Chain Context. Ann. Oper. Res. 2014, 233, 423–448. [Google Scholar] [CrossRef]
- Raj, T.; Shankar, R.; Suhaib, M. An ISM approach for modelling the enablers of flexible manufacturing system: The case for India. Int. J. Prod. Res. 2008, 46, 6883–6912. [Google Scholar] [CrossRef]
- .Kasula, B.Y. AI applications in healthcare a comprehensive review of advancements and challenges. Int. J. Manag. Educ. Sustain. Dev. 2023, 6, 2023. [Google Scholar]
- Iliashenko, O.; Bikkulova, Z.; Dubgorn, A. Opportunities and challenges of artificial intelligence in healthcare. E3S Web Conf. 2019, 110, 02028. [Google Scholar] [CrossRef]
- Dumitrașcu, L.M.; Lespezeanu, D.A.; Zugravu, C.A.; Constantin, C. Perceptions of the Impact of Artificial Intelligence among Internal Medicine Physicians as a Step in Social Responsibility Implementation: A Cross-Sectional Study. Healthcare 2024, 12, 1502. [Google Scholar] [CrossRef]
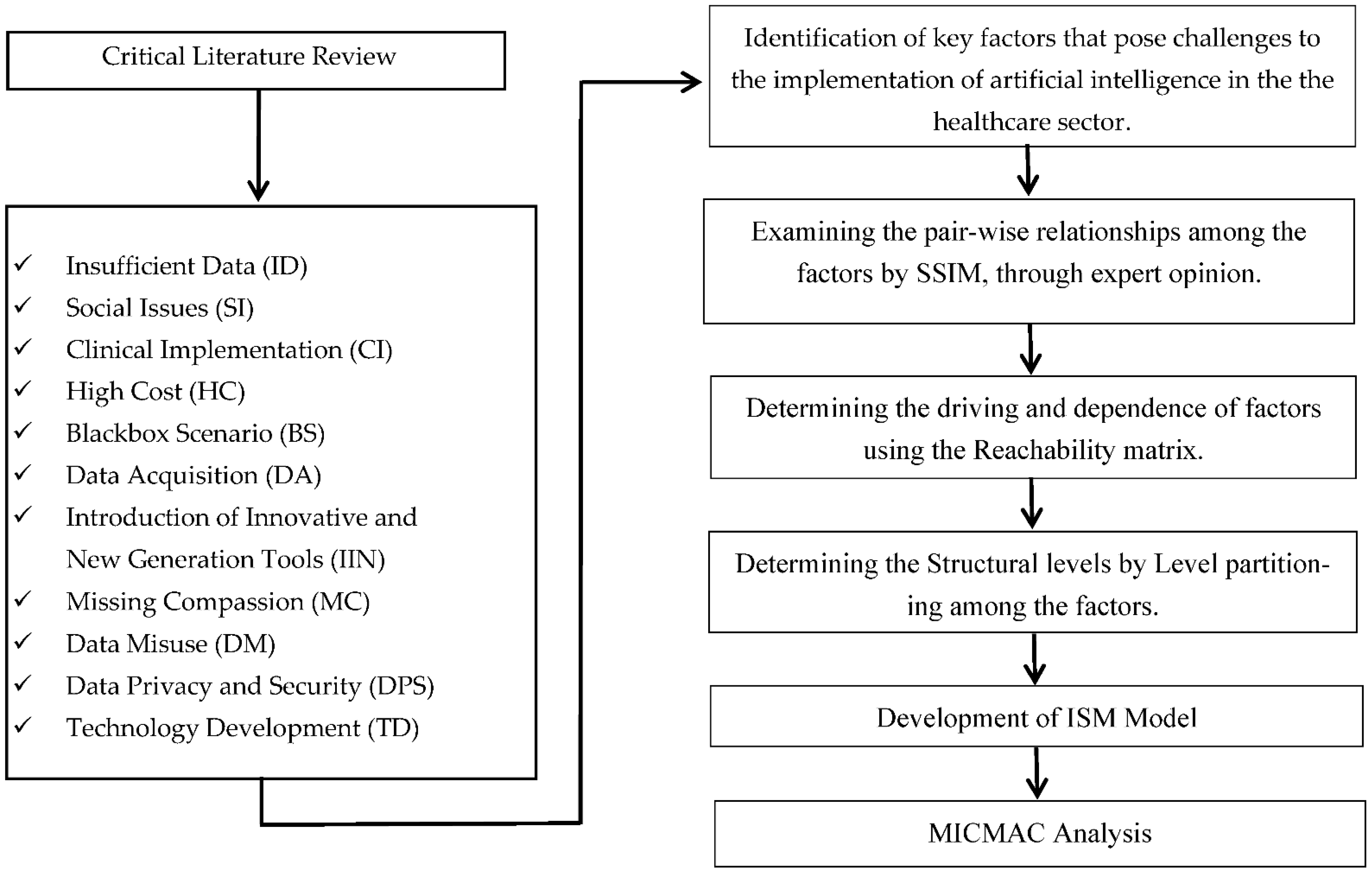
| Identified Challenges | Notations | Key Resources |
|---|---|---|
| Insufficient data | ID | Neyigapula, 2023 [8], Paul et al., 2020 [6], Bartoletti, 2019 [9], Shah and Chircu, 2018 [10] |
| Social issues | SI | Gille et al., 2020 [5], Khaled et al., 2019 [11] |
| Clinical implementation | CI | Aung et al., 2021 [4], Reddy et al., 2019 [12], Shah and Chircu, 2018 [10] |
| High cost | HC | Aung et al., 2021 [4], Jimma, 2023 [3] |
| Black-box scenario | BS | Wang et al., 2023 [13], Srinivasu et al., 2022 [14], Reddy et al., 2019 [12] |
| Data acquisition | DA | Aung et al., 2021 [4], Mueller et al., 2022 [15] |
| Introduction of innovative and new-generation tools | IIN | Wang et al., 2023 [13], Rebelo et al., 2023 [16], Van Mens et al., 2022 [17] |
| Missing compassion | MC | Aung et al., 2021 [4], Khaled et al., 2019 [11] |
| Data misuse | DM | Bartoletti, 2019 [9], Aung et al., 2021 [4] |
| Data privacy and security | DPS | Shah and Chircu, 2018 [10], Bartoletti, 2019 [9], Sun et al., 2019 [7] |
| Technology development | TD | Wang et al., 2023, Rebelo et al., 2023 [16] |
| Factor No. | Notations | Different Challenges |
|---|---|---|
| F1 | ID | INSUFFICIENT DATA |
| F2 | SI | SOCIAL ISSUES |
| F3 | CI | CLINICAL IMPLEMENTATION |
| F4 | HC | HIGH COST |
| F5 | BS | BLACK-BOX SCENARIO |
| F6 | DA | DATA ACQUISITION |
| F7 | IIN | INTRODUCTION OF INNOVATIVE AND NEW-GENERATION TOOLS |
| F8 | MC | MISSING COMPASSION |
| F9 | DM | DATA MISUSE |
| F10 | DPS | DATA PRIVACY AND SECURITY |
| F11 | TD | TECHNOLOGY DEVELOPMENT |
| Resources | Objectives |
|---|---|
| Iqbal et al., 2023 [27] | Energy efficient supply chain in the construction industry |
| Akpinar et al., 2023 [28] | Resilience in maritime business |
| Agarwal et al., 2023 [29] | Adoption of solar renewable energy products in India |
| Gadekar et al., 2024 [30] | Study of the inhibitors that affect Industry 4.0 implementation in manufacturing industries of India |
| Asif et al., 2024 [31] | Dairy supply chain |
| Feng et al., 2024 [32] | Digital innovation in manufacturing enterprises |
| Notation | F1- ID | F2- SI | F3- CI | F4- HC | F5- BS | F6- DA | F7- IIN | F8- MC | F9- DM | F10- DPS | F11- TD |
|---|---|---|---|---|---|---|---|---|---|---|---|
| F1-ID | O | V | V | V | O | V | O | O | V | V | |
| F2-SI | V | V | O | O | V | O | O | O | V | ||
| F3-CI | V | A | A | V | O | O | A | V | |||
| F4-HC | A | V | O | O | A | O | |||||
| F5-BS | A | V | O | O | O | V | |||||
| F6-DA | V | O | O | V | V | ||||||
| F7-IIN | A | A | A | A | |||||||
| F8-MC | O | O | V | ||||||||
| F9-DM | V | V | |||||||||
| F10-DPS | V | ||||||||||
| F11-TD |
| F1- ID | F2- SI | F3- CI | F4- HC | F5- BS | F6- DA | F7- IIN | F8- MC | F9- DM | F10- DPS | F11- TD | Driving Power | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| F1-ID | 1 | 0 | 1 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 7 |
| F2-SI | 0 | 1 | 1 | 1 | 0 | 0 | 1 | 0 | 0 | 0 | 1 | 5 |
| F3-CI | 0 | 0 | 1 | 1 | 0 | 0 | 1 | 0 | 0 | 0 | 1 | 4 |
| F4-HC | 0 | 0 | 0 | 1 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 2 |
| F5-BS | 0 | 0 | 1 | 1 | 1 | 0 | 1 | 0 | 0 | 0 | 1 | 5 |
| F6-DA | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 7 |
| F7-IIN | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 1 |
| F8-MC | 0 | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 0 | 0 | 1 | 6 |
| F9-DM | 0 | 0 | 1 | 1 | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 7 |
| F10-DPS | 0 | 0 | 1 | 1 | 0 | 0 | 1 | 0 | 0 | 1 | 1 | 5 |
| F11-TD | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 1 | 2 |
| Total dependencies | 1 | 2 | 8 | 9 | 4 | 1 | 11 | 1 | 1 | 4 | 9 | 1 |
| Factor No. | Reachability Set | Antecedent Set | Interaction Set | Level |
|---|---|---|---|---|
| F1-ID | 1,3,4,5,7,10,11 | 1 | 1 | One |
| F2-SI | 2,3,4,7,11 | 2,8 | 2 | Two |
| F3-CI | 3,4,7,11 | 1,2,3,5,6,8,9,10 | 3 | Three |
| F4-HC | 4,7 | 1,2,3,4,5,6,8,9,10 | 4 | Four |
| F5-BS | 3,4,5,7,11 | 1,5,6,9 | 5 | Two |
| F6-DA | 3,4,5,6,7,10,11 | 6 | 6 | One |
| F7-IIN | 7 | 1,2,3,4,5,6,7,8,9,10,11 | 7 | Five |
| F8-MC | 2,3,4,7,8,11 | 8 | 8 | One |
| F9-DM | 3,4,5,7,9,10,11 | 9 | 9 | One |
| F10-DPS | 3,4,7,10,11 | 1,6,9,10 | 10 | Two |
| F11-TD | 7,11 | 1,2,3,5,6,8,9,10,11 | 11 | Four |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Angelina, Q.; Begum, K.; Kim, H.-C.; Tripathy, S.; Singhal, D.; Singh, S. A Structural Analysis of AI Implementation Challenges in Healthcare. Algorithms 2025, 18, 189. https://doi.org/10.3390/a18040189
Angelina Q, Begum K, Kim H-C, Tripathy S, Singhal D, Singh S. A Structural Analysis of AI Implementation Challenges in Healthcare. Algorithms. 2025; 18(4):189. https://doi.org/10.3390/a18040189
Chicago/Turabian StyleAngelina, Q, Khadija Begum, Hee-Cheol Kim, Sushanta Tripathy, Deepak Singhal, and Saranjit Singh. 2025. "A Structural Analysis of AI Implementation Challenges in Healthcare" Algorithms 18, no. 4: 189. https://doi.org/10.3390/a18040189
APA StyleAngelina, Q., Begum, K., Kim, H.-C., Tripathy, S., Singhal, D., & Singh, S. (2025). A Structural Analysis of AI Implementation Challenges in Healthcare. Algorithms, 18(4), 189. https://doi.org/10.3390/a18040189








