Association between Vitamin D and Heart Failure Mortality in 10,974 Hospitalized Individuals
Abstract
1. Introduction
2. Materials and Methods
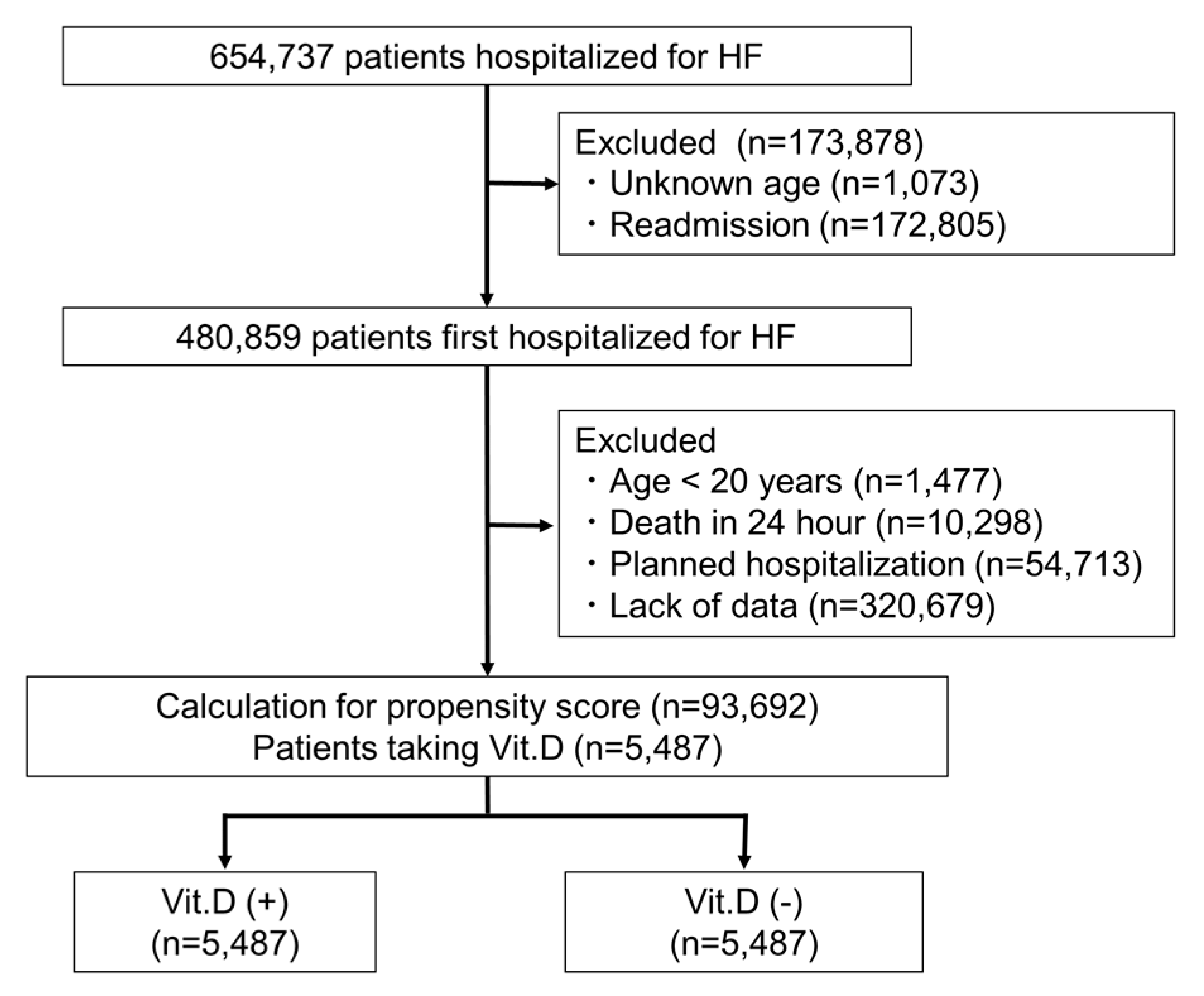
2.1. Study Population
2.2. Clinical Outcomes
2.3. Sample Matching
2.4. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Outcomes
3.3. Subgroup-Analysis
4. Discussion
4.1. Impact of Vitamin D on HF Mortality
4.2. Mechanisms of Vitamin D for HF
4.3. Clinical Implication
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Tsutsui, H.; Isobe, M.; Ito, H.; Okumura, K.; Ono, M.; Kitakaze, M.; Kinugawa, K.; Kihara, Y.; Goto, Y.; Komuro, I.; et al. JCS 2017/JHFS 2017 Guideline on Diagnosis and Treatment of Acute and Chronic Heart Failure- Digest Version. Circ. J. 2019, 83, 2084–2184. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Albert, N.M.; Allen, L.A.; Bluemke, D.A.; Butler, J.; Fonarow, G.C.; Ikonomidis, J.S.; Khavjou, O.; Konstam, M.A.; Maddox, T.M.; et al. Forecasting the impact of heart failure in the United States: A policy statement from the American Heart Association. Circ. Heart Fail. 2013, 6, 606–619. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.J. Vitamin D and Cardiovascular Disease. Annu. Rev. Med. 2016, 67, 261–272. [Google Scholar] [CrossRef] [PubMed]
- Krul-Poel, Y.H.; Ter Wee, M.M.; Lips, P.; Simsek, S. Management of Endocrine Disease: The effect of vitamin D supplementation on glycaemic control in patients with type 2 diabetes mellitus: A systematic review and meta-analysis. Eur. J. Endocrinol. 2017, 176, R1–R14. [Google Scholar] [CrossRef] [PubMed]
- Hewison, M. An update on vitamin D and human immunity. Clin. Endocrinol. 2012, 76, 315–325. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.H.; Sabour, S.; Sagar, U.N.; Adams, S.; Whellan, D.J. Prevalence of hypovitaminosis D in cardiovascular diseases (from the National Health and Nutrition Examination Survey 2001 to 2004). Am. J. Cardiol. 2008, 102, 1540–1544. [Google Scholar] [CrossRef] [PubMed]
- Ameri, P.; Ronco, D.; Casu, M.; Denegri, A.; Bovio, M.; Menoni, S.; Ferone, D.; Murialdo, G. High prevalence of vitamin D deficiency and its association with left ventricular dilation: An echocardiography study in elderly patients with chronic heart failure. Nutr. Metab. Cardiovasc. Dis. 2010, 20, 633–640. [Google Scholar] [CrossRef]
- Gardner, D.G.; Chen, S.; Glenn, D.J. Vitamin D and the heart. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2013, 305, R969–R977. [Google Scholar] [CrossRef]
- Schleithoff, S.S.; Zittermann, A.; Tenderich, G.; Berthold, H.K.; Stehle, P.; Koerfer, R. Vitamin D supplementation improves cytokine profiles in patients with congestive heart failure: A double-blind, randomized, placebo-controlled trial. Am. J. Clin. Nutr. 2006, 83, 754–759. [Google Scholar] [CrossRef]
- Witham, M.D.; Crighton, L.J.; Gillespie, N.D.; Struthers, A.D.; McMurdo, M.E. The effects of vitamin D supplementation on physical function and quality of life in older patients with heart failure: A randomized controlled trial. Circ. Heart Fail. 2010, 3, 195–201. [Google Scholar] [CrossRef]
- Witte, K.K.; Byrom, R.; Gierula, J.; Paton, M.F.; Jamil, H.A.; Lowry, J.E.; Gillott, R.G.; Barnes, S.A.; Chumun, H.; Kearney, L.C.; et al. Effects of Vitamin D on Cardiac Function in Patients With Chronic HF: The VINDICATE Study. J. Am. Coll. Cardiol. 2016, 67, 2593–2603. [Google Scholar] [CrossRef] [PubMed]
- Win, S.; Hussain, I.; Hebl, V.B.; Dunlay, S.M.; Redfield, M.M. Inpatient Mortality Risk Scores and Postdischarge Events in Hospitalized Heart Failure Patients: A Community-Based Study. Circ. Heart Fail. 2017, 10. [Google Scholar] [CrossRef] [PubMed]
- Peterson, P.N.; Rumsfeld, J.S.; Liang, L.; Albert, N.M.; Hernandez, A.F.; Peterson, E.D.; Fonarow, G.C.; Masoudi, F.A.; American Heart Association Get With the Guidelines-Heart Failure Program. A validated risk score for in-hospital mortality in patients with heart failure from the American Heart Association get with the guidelines program. Circ. Cardiovasc. Qual. Outcomes 2010, 3, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Hannan, E.L.; Wu, C.; Bennett, E.V.; Carlson, R.E.; Culliford, A.T.; Gold, J.P.; Higgins, R.S.; Smith, C.R.; Jones, R.H. Risk index for predicting in-hospital mortality for cardiac valve surgery. Ann. Thorac. Surg. 2007, 83, 921–929. [Google Scholar] [CrossRef]
- Fonarow, G.C. Clinical risk prediction tools in patients hospitalized with heart failure. Rev. Cardiovasc. Med. 2012, 13, e14–e23. [Google Scholar]
- Gaksch, M.; Jorde, R.; Grimnes, G.; Joakimsen, R.; Schirmer, H.; Wilsgaard, T.; Mathiesen, E.B.; Njolstad, I.; Lochen, M.L.; Marz, W.; et al. Vitamin D and mortality: Individual participant data meta-analysis of standardized 25-hydroxyvitamin D in 26916 individuals from a European consortium. PLoS ONE 2017, 12, e0170791. [Google Scholar] [CrossRef]
- Jiang, W.L.; Gu, H.B.; Zhang, Y.F.; Xia, Q.Q.; Qi, J.; Chen, J.C. Vitamin D Supplementation in the Treatment of Chronic Heart Failure: A Meta-analysis of Randomized Controlled Trials. Clin. Cardiol. 2016, 39, 56–61. [Google Scholar] [CrossRef]
- Barbarawi, M.; Kheiri, B.; Zayed, Y.; Barbarawi, O.; Dhillon, H.; Swaid, B.; Yelangi, A.; Sundus, S.; Bachuwa, G.; Alkotob, M.L. Vitamin D supplementation and cardiovascular disease risks in more than 83,000 individuals in 21 randomized clinical trials: A meta-analysis. JAMA Cardiol. 2019, 4, 765–775. [Google Scholar] [CrossRef]
- Stuart, E.A.; Bradshaw, C.P.; Leaf, P.J. Assessing the generalizability of randomized trial results to target populations. Prev. Sci. 2015, 16, 475–485. [Google Scholar] [CrossRef]
- Davies, N.M.; Holmes, M.V.; Davey Smith, G. Reading Mendelian randomisation studies: A guide, glossary, and checklist for clinicians. BMJ 2018, 362, k601. [Google Scholar] [CrossRef]
- Weishaar, R.E.; Simpson, R.U. Involvement of vitamin D3 with cardiovascular function. II. Direct and indirect effects. Am. J. Physiol. 1987, 253, E675–E683. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.; Law, C.S.; Grigsby, C.L.; Olsen, K.; Hong, T.T.; Zhang, Y.; Yeghiazarians, Y.; Gardner, D.G. Cardiomyocyte-specific deletion of the vitamin D receptor gene results in cardiac hypertrophy. Circulation 2011, 124, 1838–1847. [Google Scholar] [CrossRef] [PubMed]
- Vaidya, A.; Williams, J.S. The relationship between vitamin D and the renin-angiotensin system in the pathophysiology of hypertension, kidney disease, and diabetes. Metabolism 2012, 61, 450–458. [Google Scholar] [CrossRef]
- Zhang, Y.; Leung, D.Y.; Richers, B.N.; Liu, Y.; Remigio, L.K.; Riches, D.W.; Goleva, E. Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1. J. Immunol. 2012, 188, 2127–2135. [Google Scholar] [CrossRef] [PubMed]
- Caprio, M.; Mammi, C.; Rosano, G.M. Vitamin D: A novel player in endothelial function and dysfunction. Arch. Med. Sci. 2012, 8, 4–5. [Google Scholar] [CrossRef]
- Schluter, K.D.; Piper, H.M. Left ventricular hypertrophy and parathyroid hormone: A causal connection? Cardiovasc. Res. 1998, 39, 523–524. [Google Scholar] [CrossRef]
- Haden, S.T.; Brown, E.M.; Hurwitz, S.; Scott, J.; El-Hajj Fuleihan, G. The effects of age and gender on parathyroid hormone dynamics. Clin. Endocrinol. 2000, 52, 329–338. [Google Scholar] [CrossRef]
- Yamana, H.; Moriwaki, M.; Horiguchi, H.; Kodan, M.; Fushimi, K.; Yasunaga, H. Validity of diagnoses, procedures, and laboratory data in Japanese administrative data. J. Epidemiol. 2017, 27, 476–482. [Google Scholar] [CrossRef]


| Non Matching | Matching | |||||||
|---|---|---|---|---|---|---|---|---|
| All | Vit.D (+) | Vit.D (−) | std.diff (%) | Vit.D (+) | Vit.D (−) | std.diff (%) | ||
| Number | (n = 93,692) | (n = 5487) | (n = 88,205) | (n = 5487) | (n = 5487) | |||
| Age average(years) | 79 ± 12 | 80 ± 11 | 79 ± 13 | 10.6 | 80 ± 11 | 81 ± 11 | 8.4 | |
| Age(%) | 20–30 | 0.2 | 0.1 | 0.2 | −1.7 | 0.1 | 0.1 | 2.7 |
| 30–40 | 0.8 | 0.4 | 0.8 | −6.2 | 0.4 | 0.4 | −0.2 | |
| 40–50 | 2.4 | 1.4 | 2.4 | −7.8 | 1.4 | 1.1 | 2.5 | |
| 50–60 | 4.8 | 3.6 | 4.8 | −6.3 | 3.6 | 3.1 | 2.6 | |
| 60–70 | 12.1 | 10.8 | 12.2 | −4.4 | 10.8 | 9.8 | 3.3 | |
| 70–80 | 23.0 | 23.8 | 22.9 | 2.0 | 23.8 | 22.1 | 3.9 | |
| 80–90 | 39.8 | 42.4 | 39.7 | 5.5 | 42.4 | 44.2 | −3.8 | |
| >90 | 17.0 | 17.6 | 17.0 | 1.7 | 17.6 | 19.3 | −4.2 | |
| Male (%) | 52.2 | 33.9 | 53.4 | −40.1 | 33.9 | 31.4 | 5.3 | |
| BMI | 22.7 ± 5.0 | 21.8 ± 4.1 | 22.7 ± 5.0 | −20.8 | 21.8 ± 4.1 | 21.7 ± 4.1 | 1.9 | |
| Smoking | 30.2 | 21.1 | 30.8 | −22.1 | 21.1 | 18.9 | 5.7 | |
| NYHA | 1 | 12.2 | 12.8 | 12.2 | 1.9 | 12.8 | 13.2 | −1.0 |
| 2 | 24.4 | 24.5 | 24.3 | 0.3 | 24.5 | 25.0 | −1.2 | |
| 3 | 32.2 | 32.1 | 32.2 | −0.2 | 32.1 | 31.8 | 0.8 | |
| 4 | 31.2 | 30.5 | 31.2 | −1.5 | 30.5 | 30.0 | 1.1 | |
| Comorbidities (%) | ||||||||
| Hypertension | 52.9 | 48.8 | 53.2 | −8.8 | 48.8 | 47.8 | 2.0 | |
| Diabetes mellitus | 26.8 | 26.1 | 26.8 | −1.7 | 26.1 | 25.1 | 2.2 | |
| Dyslipidemia | 18.6 | 16.2 | 18.8 | −6.7 | 16.2 | 14.9 | 3.7 | |
| Osteoporosis | 3.0 | 24.5 | 1.7 | 72.1 | 24.5 | 21.2 | 7.1 | |
| Hypoparathyroidism | <0.1 | 0.2 | <0.1 | 5.0 | 0.2 | <0.1 | 4.5 | |
| HCM | 3.4 | 1.4 | 3.5 | −14.1 | 1.4 | 1.6 | −2.0 | |
| DCM | 1.2 | 1.0 | 1.3 | −2.9 | 1.0 | 1.2 | −2.8 | |
| Cardiac Amyloidosis | 0.1 | 0.1 | 0.1 | −0.8 | 0.1 | 0.1 | <0.1 | |
| Cardiac Sarcoidosis | 0.3 | 0.5 | 0.3 | 3.0 | 0.5 | 0.2 | 4.5 | |
| Af/AFL | 35.5 | 27.5 | 36.0 | −18.3 | 27.5 | 27.2 | 0.8 | |
| AT | 0.9 | 0.6 | 0.9 | −2.9 | 0.6 | 0.7 | −0.9 | |
| Stroke | 8.3 | 7.5 | 8.3 | −3.3 | 7.5 | 7.2 | 1.1 | |
| MI | 10.3 | 7.9 | 10.5 | −9.1 | 7.9 | 7.2 | 2.6 | |
| PVD | 3.8 | 4.8 | 3.7 | 5.1 | 4.8 | 3.9 | 4.3 | |
| CKD | 14.1 | 38.6 | 12.6 | 62.5 | 38.6 | 35.3 | 6.9 | |
| Liver failure | 0.1 | 0.1 | 0.1 | −0.8 | 0.1 | 0.2 | −2.7 | |
| COPD | 7.4 | 6.1 | 7.5 | −5.6 | 6.1 | 5.3 | 3.6 | |
| RA | 1.3 | 4.2 | 1.2 | 19.0 | 4.2 | 4.9 | −3.2 | |
| Dementia | 6.2 | 6.9 | 6.2 | 3.1 | 6.9 | 7.0 | −0.4 | |
| Cancer | 11.0 | 11.0 | 11.0 | 0.1 | 11.0 | 10.6 | 1.3 | |
| Treatment (%) | ||||||||
| Catecholamine | 12.4 | 11.3 | 12.5 | −3.8 | 11.3 | 10.6 | 2.1 | |
| IABP | 1.0 | 0.9 | 1.0 | −1.1 | 0.9 | 1.1 | −1.7 | |
| PCPS | 0.1 | 0.0 | 0.2 | −3.6 | 0.0 | 0.1 | −0.5 | |
| Artificial Ventilation | 21.3 | 21.1 | 21.3 | −0.5 | 21.1 | 20.8 | 0.7 | |
| Hemodialysis | 4.6 | 29.5 | 3.1 | 76.8 | 29.5 | 28.3 | 2.6 | |
| PCI | 4.9 | 5.2 | 4.9 | 1.6 | 5.2 | 5.1 | 0.7 | |
| Drug (%) | ||||||||
| ACE-i/ARB | 19.7 | 19.4 | 19.8 | −0.8 | 19.4 | 21.0 | −3.9 | |
| βblocker | 9.1 | 8.0 | 9.2 | −4.1 | 8.0 | 8.6 | −1.9 | |
| Loop diuretic | 19.4 | 18.4 | 19.4 | −2.6 | 18.4 | 20.3 | −4.8 | |
| K-sparing diuretic | 10.1 | 7.4 | 10.3 | −10.3 | 7.4 | 8.4 | −3.7 | |
| Statin | 13.1 | 13.5 | 13.0 | 1.2 | 13.5 | 13.7 | −0.7 | |
| Hospital length (days) | 18 (12–28) | 19 (12–31) | 17 (12–27) | 13.1 | 19 (12–31) | 18 (11–30) | 14.9 | |
| Non Matching | Matching | |||||||
|---|---|---|---|---|---|---|---|---|
| In-Hospital Mortality | Vit.D (+) | Vit.D (−) | OR (95%CI) | p-Value | Vit.D (+) | Vit.D (−) | OR (95%CI) | p-Value |
| Total (%) | 357 (6.5) | 7256 (8.2) | 0.79 (0.71–0.88) | <0.0001 | 357 (6.5) | 515 (9.4) | 0.67 (0.58–0.77) | <0.0001 |
| 7 days (%) | 48 (0.9) | 1761 (2.0) | 0.44 (0.33–0.58) | <0.0001 | 48 (0.9) | 138 (2.5) | 0.34 (0.25–0.48) | <0.0001 |
| 30 days (%) | 207 (3.8) | 5171 (5.9) | 0.64 (0.55–0.73) | <0.0001 | 207 (3.8) | 358 (6.5) | 0.56 (0.47–0.67) | <0.0001 |
| A: In all patients. See abbreviations in Table 1. | ||||
| All | ||||
| OR | Lower | Higher | p | |
| Vit.D | 0.63 | 0.49 | 0.81 | 0.0003 |
| Age | 1.06 | 1.05 | 1.08 | <0.0001 |
| BMI | 0.93 | 0.90 | 0.96 | <0.0001 |
| NYHA | 1.18 | 1.04 | 1.33 | 0.0070 |
| Male | 1.00 | 0.74 | 1.35 | 0.9884 |
| Smoking | 0.93 | 0.67 | 1.31 | 0.6867 |
| HT | 0.39 | 0.30 | 0.51 | <0.0001 |
| DM | 0.80 | 0.60 | 1.07 | 0.1398 |
| DL | 0.83 | 0.57 | 1.22 | 0.3445 |
| MI | 1.17 | 0.76 | 1.80 | 0.4721 |
| PVD | 1.88 | 1.19 | 2.96 | 0.0064 |
| Stroke | 0.96 | 0.62 | 1.50 | 0.8659 |
| Dementia | 1.21 | 0.78 | 1.87 | 0.4000 |
| COPD | 0.95 | 0.56 | 1.59 | 0.8370 |
| RA | 1.10 | 0.65 | 1.89 | 0.7187 |
| CKD | 1.65 | 1.19 | 2.30 | 0.0030 |
| Cancer | 0.84 | 0.57 | 1.24 | 0.3764 |
| Hemodialysis | 0.84 | 0.58 | 1.22 | 0.3669 |
| Artificial Ventilation | 2.55 | 1.95 | 3.33 | <0.0001 |
| PCI | 0.22 | 0.10 | 0.47 | <0.0001 |
| IABP | 1.04 | 0.44 | 2.43 | 0.9355 |
| Catecholamines | 4.59 | 3.50 | 6.02 | <0.0001 |
| Osteoporosis | 0.76 | 0.48 | 1.19 | 0.2331 |
| HCM | 0.61 | 0.18 | 2.09 | 0.4338 |
| Sarcoidosis | 2.60 | 0.55 | 12.18 | 0.2253 |
| Af/AFL | 0.68 | 0.51 | 0.92 | 0.0107 |
| B: In patients with vitamin D supplementation. See abbreviations in Table 1. | ||||
| Vitamin D (+) | ||||
| OR | Lower | Higher | p | |
| Age | 1.07 | 1.04 | 1.09 | <0.0001 |
| BMI | 0.97 | 0.92 | 1.02 | 0.2186 |
| NYHA | 1.22 | 1.01 | 1.48 | 0.0379 |
| Male | 0.62 | 0.37 | 1.02 | 0.0589 |
| Smoking | 1.10 | 0.64 | 1.87 | 0.7396 |
| HT | 0.33 | 0.22 | 0.52 | <0.0001 |
| DM | 0.70 | 0.44 | 1.11 | 0.1257 |
| DL | 1.11 | 0.64 | 1.90 | 0.7187 |
| MI | 1.36 | 0.71 | 2.59 | 0.3519 |
| PVD | 2.24 | 1.18 | 4.27 | 0.0138 |
| Stroke | 1.25 | 0.66 | 2.37 | 0.4844 |
| Dementia | 1.17 | 0.59 | 2.31 | 0.6536 |
| COPD | 0.86 | 0.38 | 1.94 | 0.7122 |
| RA | 0.80 | 0.30 | 2.12 | 0.6558 |
| CKD | 1.68 | 0.95 | 2.99 | 0.0746 |
| Cancer | 1.09 | 0.60 | 1.98 | 0.7663 |
| Hemodialysis | 0.98 | 0.52 | 1.85 | 0.9510 |
| Artificial Ventilation | 2.18 | 1.44 | 3.31 | 0.0003 |
| PCI | 0.19 | 0.06 | 0.64 | 0.0075 |
| IABP | 1.34 | 0.40 | 4.49 | 0.6352 |
| Catecholamines | 4.91 | 3.24 | 7.43 | <0.0001 |
| Osteoporosis | 0.61 | 0.36 | 1.04 | 0.0707 |
| HCM | 1.57 | 0.34 | 7.23 | 0.5659 |
| Sarcoidosis | 2.14 | 0.26 | 17.31 | 0.4763 |
| Af/AFL | 0.66 | 0.41 | 1.06 | 0.0822 |
| C: In patients without vitamin D supplementation. See abbreviations in Table 1. | ||||
| Vitamin D (−) | ||||
| OR | Lower | Higher | p | |
| Age | 1.07 | 1.04 | 1.09 | <0.0001 |
| BMI | 0.91 | 0.87 | 0.95 | <0.0001 |
| NYHA | 1.14 | 0.97 | 1.33 | 0.1111 |
| Male | 1.36 | 0.93 | 2.01 | 0.1153 |
| Smoking | 0.83 | 0.54 | 1.30 | 0.4209 |
| HT | 0.43 | 0.30 | 0.60 | <0.0001 |
| DM | 0.87 | 0.59 | 1.28 | 0.4857 |
| DL | 0.64 | 0.37 | 1.10 | 0.1087 |
| MI | 1.06 | 0.59 | 1.90 | 0.8573 |
| PVD | 1.53 | 0.79 | 2.95 | 0.2038 |
| Stroke | 0.77 | 0.40 | 1.45 | 0.4106 |
| Dementia | 1.20 | 0.67 | 2.15 | 0.5442 |
| COPD | 1.01 | 0.51 | 1.99 | 0.9816 |
| RA | 1.19 | 0.61 | 2.31 | 0.6059 |
| CKD | 1.55 | 1.02 | 2.36 | 0.0386 |
| Cancer | 0.75 | 0.45 | 1.26 | 0.2757 |
| Hemodialysis | 0.78 | 0.48 | 1.26 | 0.3036 |
| Artificial Ventilation | 3.03 | 2.12 | 4.32 | <0.0001 |
| PCI | 0.25 | 0.09 | 0.65 | 0.0048 |
| IABP | 0.74 | 0.21 | 2.59 | 0.6374 |
| Catecholamines | 4.72 | 3.26 | 6.82 | <0.0001 |
| Osteoporosis | 1.85 | 0.76 | 4.50 | 0.1746 |
| HCM | 0.24 | 0.03 | 2.05 | 0.1939 |
| Sarcoidosis | 3.58 | 0.35 | 36.60 | 0.2815 |
| Af/AFL | 0.70 | 0.48 | 1.02 | 0.0632 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kusunose, K.; Okushi, Y.; Okayama, Y.; Zheng, R.; Abe, M.; Nakai, M.; Sumita, Y.; Ise, T.; Tobiume, T.; Yamaguchi, K.; et al. Association between Vitamin D and Heart Failure Mortality in 10,974 Hospitalized Individuals. Nutrients 2021, 13, 335. https://doi.org/10.3390/nu13020335
Kusunose K, Okushi Y, Okayama Y, Zheng R, Abe M, Nakai M, Sumita Y, Ise T, Tobiume T, Yamaguchi K, et al. Association between Vitamin D and Heart Failure Mortality in 10,974 Hospitalized Individuals. Nutrients. 2021; 13(2):335. https://doi.org/10.3390/nu13020335
Chicago/Turabian StyleKusunose, Kenya, Yuichiro Okushi, Yoshihiro Okayama, Robert Zheng, Miho Abe, Michikazu Nakai, Yoko Sumita, Takayuki Ise, Takeshi Tobiume, Koji Yamaguchi, and et al. 2021. "Association between Vitamin D and Heart Failure Mortality in 10,974 Hospitalized Individuals" Nutrients 13, no. 2: 335. https://doi.org/10.3390/nu13020335
APA StyleKusunose, K., Okushi, Y., Okayama, Y., Zheng, R., Abe, M., Nakai, M., Sumita, Y., Ise, T., Tobiume, T., Yamaguchi, K., Yagi, S., Fukuda, D., Yamada, H., Soeki, T., Wakatsuki, T., & Sata, M. (2021). Association between Vitamin D and Heart Failure Mortality in 10,974 Hospitalized Individuals. Nutrients, 13(2), 335. https://doi.org/10.3390/nu13020335







