Dynamic Changes in Dietary Guideline Adherence and Its Association with All-Cause Mortality among Middle-Aged Chinese: A Longitudinal Study from the China Health and Nutrition Survey
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Baseline Characteristics in Three Classes
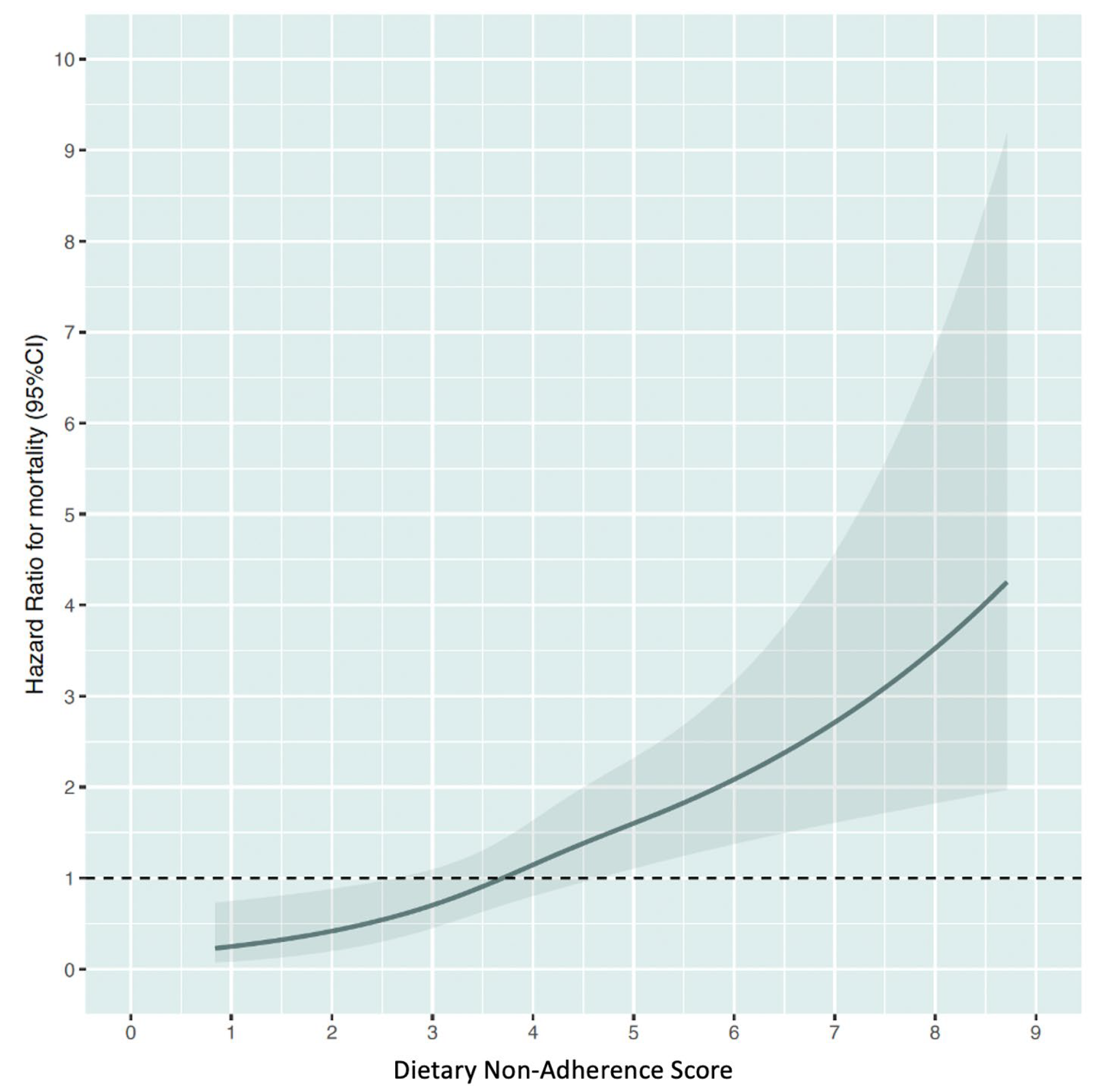
3.2. Association of DNAS with Mortality
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Class 1 (Low DNAS) | Class 2 (Medium DNAS) | Class 3 (High DNAS) | |
|---|---|---|---|
| N = 378 | N = 3522 | N = 633 | |
| Cereals and tubers | 341 (269–433) | 446 (350–558) | 608 (439–792) |
| Vegetables | 307 (217–383) | 340 (240–480) | 267 (166–412) |
| Fruits | 83 (0–183) | 0 (0–0) | 0 (0–0) |
| Meat | 97 (60–160) | 66 (17–133) | 0 (0–47) |
| Aquatic products | 33 (0–83) | 0 (0–50) | 0 (0–0) |
| Eggs | 40 (16–67) | 16 (0–40) | 0 (0–20) |
| Dairy products | 83 (0–200) | 0 (0–0) | 0 (0–0) |
| Soybeans and nuts | 42 (0–88) | 33 (0–80) | 0 (0–50) |
| Salt | 8 (5–12) | 9 (6–14) | 10 (7–13) |
| Oil | 44 (27–69) | 42 (27–63) | 33 (19–53) |
| Population | Component | Criteria for Minimum Score (0) | Criteria for Maximum Score | Maximum Score Value |
|---|---|---|---|---|
| American | Vegetables, servings/d | 0 | ≥5 | 10 |
| Fruit, servings/d | 0 | ≥4 | 10 | |
| Whole grains, g/d | 0 | 10 | ||
| Women | 75 | |||
| Men | 90 | |||
| Sugar-sweetened beverages and fruit juice, servings/d | ≥1 | 0 | 10 | |
| Nuts and legumes, servings/d | 0 | ≥1 | 10 | |
| Red/processed meat, servings/d | ≥1.5 | 0 | 10 | |
| trans Fat, % of energy | ≥4 | ≤0.5 | 10 | |
| Long-chain (n-3) fats (EPA + DHA), mg/d | 0 | 250 | 10 | |
| PUFA, % of energy | ≤2 | ≥10 | 10 | |
| Sodium, mg/d | Highest decile | Lowest decile | 10 | |
| Alcohol, drinks/d | 10 | |||
| Women | ≥2.5 | 0.5–1.5 | ||
| Men | ≥3.5 | 0.5–2.0 | ||
| Total | 110 |
| Class 1 | Class 2 | Class 3 | |
|---|---|---|---|
| (Low DNAS) | (Medium DNAS) | (High DNAS) | |
| N = 378 | N = 3522 | N = 633 | |
| Model 5 (all confounders + AHEI) | 1.0 (ref) | 1.2 (1.1, 9.0) | 3.1 (1.9, 5.1) |
| Food Groups | Ranges (gram) | Taking Values (gram) | Percentage |
|---|---|---|---|
| Cereals and tubers | Cereals 200–300, tubers 50–100 | 325 | 19.9 |
| Vegetables | 300–500 | 400 | 24.5 |
| Fruits | 200–350 | 275 | 16.8 |
| Meat | 120–200 (including aquatic products) | 60 | 3.7 |
| Aquatic products | ≥2 times per week | 60 | 3.7 |
| Soybeans and nuts | 25–35 | 30 | 3.1 |
| Eggs | 1 per day | 50 | 24.5 |
| Dairy products | 300–500 | 400 | 1.8 |
| Edible oil | 25–30 | 27.5 | 1.7 |
| Salt | <5 | 5 | 0.3 |



References
- Collaborators, G.; Ärnlöv, J. Global burden of 87 risk factors in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020, 396, 1223–1249. [Google Scholar]
- Wang, S.-s.; Lay, S.; Yu, H.-n.; Shen, S.-r. Dietary guidelines for Chinese residents (2016): Comments and comparisons. J. Zhejiang Univ. Sci. B 2016, 17, 649–656. [Google Scholar] [CrossRef]
- Yu, D.; Zhang, X.; Xiang, Y.-B.; Yang, G.; Li, H.; Gao, Y.-T.; Zheng, W.; Shu, X.-O. Adherence to dietary guidelines and mortality: A report from prospective cohort studies of 134,000 Chinese adults in urban Shanghai. Am. J. Clin. Nutr. 2014, 100, 693–700. [Google Scholar] [CrossRef]
- Wang, F.; Cai, H.; Gu, K.; Shi, L.; Yu, D.; Zhang, M.; Zheng, W.; Zheng, Y.; Bao, P.; Shu, X.-O. Adherence to dietary recommendations among long-term breast cancer survivors and cancer outcome associations. Cancer Epidemiol. Biomark. Prev. 2020, 29, 386–395. [Google Scholar]
- Yuna He, P.; Li, Y.; Xiaoguang Yang, P.; Hemler, E.C.; Fang, Y.; Liyun Zhao, P.; Jian Zhang, P.; Zhenyu Yang, P.; Zhu Wang, P.; Li He, P. The dietary transition and its associated cardiometabolic mortality among Chinese adults from 1982–2012: A cross-sectional population-based study. Lancet. Diabetes Endocrinol. 2019, 7, 540. [Google Scholar]
- Arvaniti, F.; Panagiotakos, D.B. Healthy indexes in public health practice and research: A review. Crit. Rev. Food Sci. Nutr. 2008, 48, 317–327. [Google Scholar] [CrossRef]
- Toft, U.; Kristoffersen, L.; Lau, C.; Borch-Johnsen, K.; Jørgensen, T. The Dietary Quality Score: Validation and association with cardiovascular risk factors: The Inter99 study. Eur. J. Clin. Nutr. 2007, 61, 270–278. [Google Scholar] [PubMed]
- Trichopoulou, A.; Orfanos, P.; Norat, T.; Bueno-de-Mesquita, B.; Ocké, M.C.; Peeters, P.H.; van der Schouw, Y.T.; Boeing, H.; Hoffmann, K.; Boffetta, P. Modified Mediterranean diet and survival: EPIC-elderly prospective cohort study. Bmj 2005, 330, 991. [Google Scholar] [CrossRef] [PubMed]
- He, Y.; Zhai, F.; Yang, X.; Ge, K. The Chinese Diet Balance Index revised. Acta Nutr. Sin. 2009, 31, 532–536. [Google Scholar]
- Pilgrim, A.; Robinson, S.; Sayer, A.A.; Roberts, H. An overview of appetite decline in older people. Nurs. Older People 2015, 27, 29. [Google Scholar] [CrossRef]
- Morley, J.E. Decreased food intake with aging. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2001, 56, 81–88. [Google Scholar] [CrossRef]
- Azzolino, D.; Arosio, B.; Marzetti, E.; Calvani, R.; Cesari, M. Nutritional status as a mediator of fatigue and its underlying mechanisms in older people. Nutrients 2020, 12, 444. [Google Scholar] [PubMed]
- Popkin, B.M.; Lu, B.; Zhai, F. Understanding the nutrition transition: Measuring rapid dietary changes in transitional countries. Public Health Nutr. 2002, 5, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Zhai, F.; Wang, H.; Du, S.; He, Y.; Wang, Z.; Ge, K.; Popkin, B.M. Prospective study on nutrition transition in China. Nutr. Rev. 2009, 67, S56–S61. [Google Scholar] [CrossRef] [PubMed]
- Dong, F.; Howard, A.G.; Herring, A.H.; Thompson, A.L.; Adair, L.S.; Popkin, B.M.; Aiello, A.E.; Zhang, B.; Gordon-Larsen, P. Longitudinal associations of away-from-home eating, snacking, screen time, and physical activity behaviors with cardiometabolic risk factors among Chinese children and their parents. Am. J. Clin. Nutr. 2017, 106, 168–178. [Google Scholar] [CrossRef]
- Thompson, A.L.; Adair, L.; Gordon-Larsen, P.; Zhang, B.; Popkin, B. Environmental, dietary, and behavioral factors distinguish Chinese adults with high waist-to-height ratio with and without inflammation. J. Nutr. 2015, 145, 1335–1344. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Adair, L.S.; Cai, J.; Gordon-Larsen, P.; Siega-Riz, A.M.; Zhang, B.; Popkin, B.M. Diet quality is linked to insulin resistance among adults in China. J. Nutr. 2017, 147, 2102–2108. [Google Scholar] [CrossRef] [PubMed]
- Zhang, B.; Zhai, F.; Du, S.; Popkin, B.M. The C hina H ealth and N utrition S urvey, 1989–2011. Obes. Rev. 2014, 15, 2–7. [Google Scholar] [CrossRef]
- Marengoni, A.; Rizzuto, D.; Wang, H.X.; Winblad, B.; Fratiglioni, L. Patterns of chronic multimorbidity in the elderly population. J. Am. Geriatr. Soc. 2009, 57, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Center, C.P. China Health and Nutrition Survey. Available online: http://www.cpc.unc.edu/projects/china (accessed on 1 December 2013).
- Zhai, F.; Du, S.; Wang, Z.; Zhang, J.; Du, W.; Popkin, B.M. Dynamics of the C hinese diet and the role of urbanicity, 1991–2011. Obes. Rev. 2014, 15, 16–26. [Google Scholar] [CrossRef]
- Zhai, F.; Guo, X.; Popkin, B.M.; Ma, L.; Wang, Q.; Shuigao, W.Y.; Ge, J.; Keyou. Evaluation of the 24-hour individual recall method in China. Food Nutr. Bull. 1996, 17, 1–7. [Google Scholar] [CrossRef]
- D’Agostino, M.; Dardanoni, V. What’s so special about Euclidean distance? Soc. Choice Welf. 2009, 33, 211–233. [Google Scholar] [CrossRef]
- Santini, S.; Jain, R. Similarity measures. IEEE Trans. Pattern Anal. Mach. Intell. 1999, 21, 871–883. [Google Scholar] [CrossRef]
- Parimbelli, E.; Marini, S.; Sacchi, L.; Bellazzi, R. Patient similarity for precision medicine: A systematic review. J. Biomed. Inform. 2018, 83, 87–96. [Google Scholar] [PubMed]
- David, G.; Bernstein, L.; Coifman, R.R. Generating Evidence Based Interpretation of Hematology Screens via Anomaly Characterization. Am. J. Clin. Pathol. 2010, 134, 668. [Google Scholar] [CrossRef]
- Chattopadhyay, S.; Ray, P.; Chen, H.; Lee, M.; Chiang, H. Suicidal risk evaluation using a similarity-based classifier. In Proceedings of the International Conference on Advanced Data Mining and Applications, Chengdu, China, 8–10 October 2008; pp. 51–61. [Google Scholar]
- Andruff, H.; Carraro, N.; Thompson, A.; Gaudreau, P.; Louvet, B. Latent class growth modelling: A tutorial. Tutor. Quant. Methods Psychol. 2009, 5, 11–24. [Google Scholar] [CrossRef]
- Lennon, H.; Kelly, S.; Sperrin, M.; Buchan, I.; Cross, A.J.; Leitzmann, M.; Cook, M.B.; Renehan, A.G. Framework to construct and interpret latent class trajectory modelling. BMJ Open 2018, 8, e020683. [Google Scholar] [CrossRef] [PubMed]
- Proust-Lima, C.; Philipps, V.; Liquet, B. Estimation of extended mixed models using latent classes and latent processes: The R package lcmm. arXiv 2015, arXiv:1503.00890. [Google Scholar] [CrossRef]
- Bier, D.M.; Derelian, D.; German, J.B.; Katz, D.L.; Pate, R.R.; Thompson, K.M. Improving compliance with dietary recommendations: Time for new, inventive approaches? Nutr. Today 2008, 43, 180–187. [Google Scholar] [CrossRef]
- Nicklas, T.A.; Jahns, L.; Bogle, M.L.; Chester, D.N.; Giovanni, M.; Klurfeld, D.M.; Laugero, K.; Liu, Y.; Lopez, S.; Tucker, K.L. Barriers and facilitators for consumer adherence to the dietary guidelines for Americans: The HEALTH study. J. Acad. Nutr. Diet. 2013, 113, 1317–1331. [Google Scholar] [CrossRef]
- Rowe, S.; Alexander, N.; Almeida, N.; Black, R.; Burns, R.; Bush, L.; Crawford, P.; Keim, N.; Kris-Etherton, P.; Weaver, C. Food science challenge: Translating the Dietary Guidelines for Americans to bring about real behavior change. J. Food Sci. 2011, 76, R29–R37. [Google Scholar] [CrossRef]
- Paddon-Jones, D.; Campbell, W.W.; Jacques, P.F.; Kritchevsky, S.B.; Moore, L.L.; Rodriguez, N.R.; Van Loon, L.J. Protein and healthy aging. Am. J. Clin. Nutr. 2015, 101, 1339S–1345S. [Google Scholar] [CrossRef]
- Slavin, J.L. Whole grains, refined grains and fortified refined grains: What’s the difference? Asia Pac. J. Clin. Nutr. 2000, 9, S23–S27. [Google Scholar] [CrossRef] [PubMed]
- Zhao, J.; Li, Z.; Gao, Q.; Zhao, H.; Chen, S.; Huang, L.; Wang, W.; Wang, T. A review of statistical methods for dietary pattern analysis. Nutr. J. 2021, 20, 37. [Google Scholar]
- Sofi, F.; Cesari, F.; Abbate, R.; Gensini, G.F.; Casini, A. Adherence to Mediterranean diet and health status: Meta-analysis. BMJ 2008, 337, a1344. [Google Scholar] [CrossRef]
- McCullough, M.L.; Feskanich, D.; Stampfer, M.J.; Giovannucci, E.L.; Rimm, E.B.; Hu, F.B.; Spiegelman, D.; Hunter, D.J.; Colditz, G.A.; Willett, W.C. Diet quality and major chronic disease risk in men and women: Moving toward improved dietary guidance. Am. J. Clin. Nutr. 2002, 76, 1261–1271. [Google Scholar] [PubMed]
- Chiuve, S.E.; Fung, T.T.; Rimm, E.B.; Hu, F.B.; McCullough, M.L.; Wang, M.; Stampfer, M.J.; Willett, W.C. Alternative dietary indices both strongly predict risk of chronic disease. J. Nutr. 2012, 142, 1009–1018. [Google Scholar]
- Onvani, S.; Haghighatdoost, F.; Surkan, P.; Larijani, B.; Azadbakht, L. Adherence to the Healthy Eating Index and Alternative Healthy Eating Index dietary patterns and mortality from all causes, cardiovascular disease and cancer: A meta-analysis of observational studies. J. Hum. Nutr. Diet. 2017, 30, 216–226. [Google Scholar] [PubMed]
- Zhong, V.W.; Ning, H.; Van Horn, L.; Carnethon, M.R.; Wilkins, J.T.; Lloyd-Jones, D.M.; Allen, N.B. Diet quality and long-term absolute risks for incident cardiovascular disease and mortality. Am. J. Med. 2021, 134, 490–498.e424. [Google Scholar]
- Milajerdi, A.; Namazi, N.; Larijani, B.; Azadbakht, L. The association of dietary quality indices and cancer mortality: A systematic review and meta-analysis of cohort studies. Nutr. Cancer 2018, 70, 1091–1105. [Google Scholar] [CrossRef]
- Patterson, B.H.; Block, G.; Rosenberger, W.F.; Pee, D.; Kahle, L.L. Fruit and vegetables in the American diet: Data from the NHANES II survey. Am. J. Public Health 1990, 80, 1443–1449. [Google Scholar] [CrossRef]
- Murphy, S.P.; Rose, D.; Hudes, M.; Viteri, F.E. Demographic and economic factors associated with dietary quality for adults in the 1987-88 Nationwide Food Consumption Survey. J. Am. Diet. Assoc. 1992, 92, 1352–1358. [Google Scholar] [CrossRef]
- Elahi, V.K.; Elahi, D.; Andres, R.; Tobin, J.D.; Butler, M.G.; Norris, A.H. A longitudinal study of nutritional intake in men. J. Gerontol. 1983, 38, 162–180. [Google Scholar] [CrossRef]
- Popkin, B.M.; Haines, P.S.; Patterson, R.E. Dietary changes in older Americans, 1977–1987. Am. J. Clin. Nutr. 1992, 55, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Sobell, J.; Block, G.; Koslowe, P.; Tobin, J.; Andres, R. Validation of a retrospective questionnaire assessing diet 10–15 years ago. Am. J. Epidemiol. 1989, 130, 173–187. [Google Scholar] [CrossRef] [PubMed]
- Chernoff, R. Micronutrient requirements in older women. Am. J. Clin. Nutr. 2005, 81, 1240S–1245S. [Google Scholar] [CrossRef] [PubMed]

| All | Class 1 (Low DNAS) | Class 2 (Medium DNAS) | Class 3 (High DNAS) | p-Value | |
|---|---|---|---|---|---|
| N = 4533 | N = 378 | N = 3522 | N = 633 | ||
| DNAS | 4.8 (1.0) | 3.3 (1.0) | 4.8 (0.8) | 5.9 (0.9) | <0.001 |
| Age at entry, year | 43.3 (8.3) | 43.8 (8.6) | 43.0 (8.2) | 44.7 (8.3) | 0.17 |
| Physical activity (MET, min/week) | 3099 (2837) | 1518 (1652) | 3158 (2856) | 3714 (2959) | <0.001 |
| BMI (kg/m2) | 23.3 (3.2) | 23.6 (3.1) | 23.4 (3.2) | 23.1 (3.3) | 0.65 |
| Energy intake (cal/day) | 2224 (503) | 2121 (400) | 2236 (501) | 2221 (557) | <0.001 |
| Individual annual income (yuan) | 10,909 (18,056) | 18,393 (16,906) | 10,933 (19,194) | 6307 (7680) | <0.001 |
| Chronic diseases | 32.0% | 35.2% | 32.4% | 30.2% | 0.25 |
| Took medicine | 19.2% | 24.1% | 19.2% | 16.4% | 0.01 |
| Current smoker | 43.1% | 29.6% | 43.1% | 48.7% | <0.001 |
| Current drinker | 52.5% | 52.4% | 52.6% | 52.1% | 0.98 |
| Mortality rate (1000 person-years) (95% CI) | 29.6 (24.8–35.3) | 11.8 (4.5–31.5) | 28.8 (23.5–35.3) | 44.5 (30.6–64.9) | <0.001 |
| Class 1 | Class 2 | Class 3 | |
|---|---|---|---|
| (Low DNAS) | (Medium DNAS) | (High DNAS) | |
| Model 1 | 1.0 (ref) | 4.6 (1.7, 12.5) | 8.3 (3.0, 23.1) |
| Model 2 (+ age, sex, region) | 1.0 (ref) | 4.0 (1.5, 10.8) | 6.5 (2.3, 18.1) |
| Model 3 (+ disease, medicine, smoker, physical activity, energy intake, BMI) | 1.0 (ref) | 3.7 (1.4, 10.2) | 5.9 (2.1, 16.6) |
| Model 4 (+ drinker, income, education) | 1.0 (ref) | 3.0 (1.1, 8.4) | 4.4 (1.5, 12.7) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, X.; Na, X.; Wang, Y.; Du, S.; Zhao, A.; Liang, W. Dynamic Changes in Dietary Guideline Adherence and Its Association with All-Cause Mortality among Middle-Aged Chinese: A Longitudinal Study from the China Health and Nutrition Survey. Nutrients 2023, 15, 1401. https://doi.org/10.3390/nu15061401
Zhang X, Na X, Wang Y, Du S, Zhao A, Liang W. Dynamic Changes in Dietary Guideline Adherence and Its Association with All-Cause Mortality among Middle-Aged Chinese: A Longitudinal Study from the China Health and Nutrition Survey. Nutrients. 2023; 15(6):1401. https://doi.org/10.3390/nu15061401
Chicago/Turabian StyleZhang, Xiao, Xiaona Na, Yanfang Wang, Shufa Du, Ai Zhao, and Wannian Liang. 2023. "Dynamic Changes in Dietary Guideline Adherence and Its Association with All-Cause Mortality among Middle-Aged Chinese: A Longitudinal Study from the China Health and Nutrition Survey" Nutrients 15, no. 6: 1401. https://doi.org/10.3390/nu15061401
APA StyleZhang, X., Na, X., Wang, Y., Du, S., Zhao, A., & Liang, W. (2023). Dynamic Changes in Dietary Guideline Adherence and Its Association with All-Cause Mortality among Middle-Aged Chinese: A Longitudinal Study from the China Health and Nutrition Survey. Nutrients, 15(6), 1401. https://doi.org/10.3390/nu15061401





