Antibacterial Activity of Cerium Oxide Nanoparticles against ESKAPE Pathogens
Abstract
:1. Introduction
2. Materials and Methods
2.1. The Synthesis and Characterization of CeO2 Nanoparticles
2.2. Microbial Strains
2.3. Antimicrobial Susceptibility Test
2.4. Antibacterial Activity of CeO2 Nanoparticles
2.5. Minimum Inhibitory Concentration (MIC) Determination
2.6. Data Analysis
3. Results and Discussion
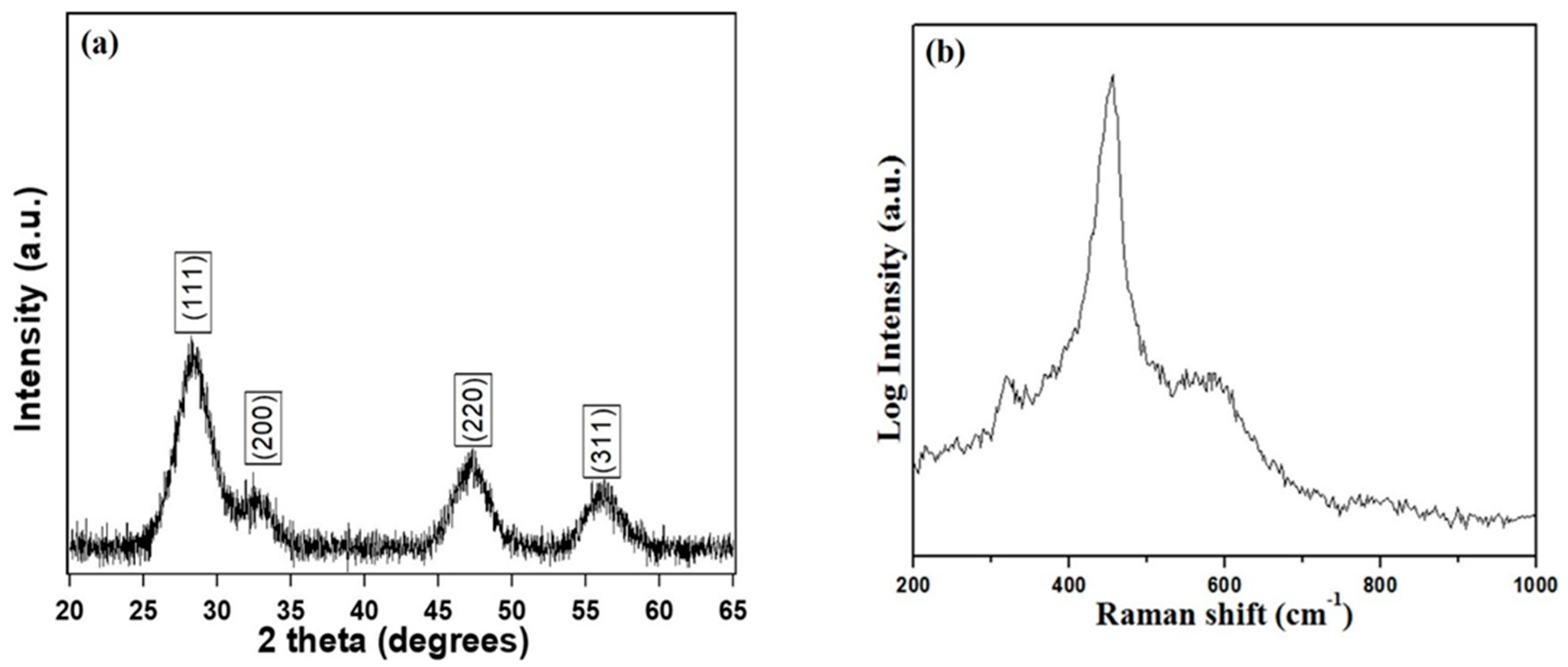
3.1. Structural Properties of CeO2 Nanoparticles
3.2. Antimicrobial Susceptibility of ESKAPE Pathogens
3.3. Antibacterial Activity of CeO2 Nanoparticles against the ESKAPE Pathogens
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Prestinaci, F.; Pezzotti, P.; Pantosti, A. Antimicrobial resistance: A global multifaceted phenomenon. Pathog. Glob. Health 2015, 109, 309–318. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Abadi, A.T.B.; Rizvanov, A.A.; Haertlé, T.; Blatt, N.L. World Health Organization report: Current crisis of antibiotic resistance. BioNanoScience 2019, 9, 778–788. [Google Scholar] [CrossRef]
- Buchy, P.; Ascioglu, S.; Buisson, Y.; Datta, S.; Nissen, M.; Tambyah, P.A.; Vong, S. Impact of vaccines on antimicrobial resistance. Int. J. Infect. Dis. 2020, 90, 188–196. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- World Health Organization. Global Priority List of Antibiotic-Resistant Bacteria to Guide Research, Discovery and Development of New Antibiotics. Available online: https://www.who.int/medicines/publications/WHO-PPL-Short_Summary_25Feb-ET_NM_WHO.pdf (accessed on 15 December 2021).
- Rice, L.B. Federal funding for the study of antimicrobial resistance in nosocomial pathogens: No ESKAPE. J. Infect. Dis. 2008, 197, 1079–1081. [Google Scholar] [CrossRef] [PubMed]
- Mulani, M.S.; Kamble, E.E.; Kumkar, S.N.; Tawre, M.S.; Pardesi, K.R. Emerging strategies to combat ESKAPE pathogens in the era of antimicrobial resistance: A review. Front. Microbiol. 2019, 10, 539. [Google Scholar] [CrossRef]
- Santaniello, A.; Sansone, M.; Fioretti, A.; Menna, L.F. Systematic review and meta-analysis of the occurrence of ESKAPE bacteria group in dogs, and the related zoonotic risk in animal-assisted therapy, and in animal-assisted activity in the health context. Int. J. Environ. Res. Public Health 2020, 17, 3278. [Google Scholar] [CrossRef]
- Benkő, R.; Gajdács, M.; Matuz, M.; Bodó, G.; Lázár, A.; Hajdú, E.; Papfalvi, E.; Hannauer, P.; Erdélyi, P.; Pető, Z. Prevalence and antibiotic resistance of ESKAPE pathogens isolated in the emergency department of a tertiary care teaching hospital in hungary: A 5-year retrospective survey. Antibiotics 2020, 9, 624. [Google Scholar] [CrossRef] [PubMed]
- Read, A.F.; Woods, R.J. Antibiotic resistance management. Evol. Med. Public Health 2014, 2014, 147. [Google Scholar] [CrossRef]
- Nature, E. The antibiotic alarm. Nature 2013, 495, 141. [Google Scholar]
- Kamaruzzaman, N.F.; Tan, L.P.; Hamdan, R.H.; Choong, S.S.; Wong, W.K.; Gibson, A.J.; Chivu, A.; Pina, M.F. Antimicrobial polymers: The potential replacement of existing antibiotics? Int. J. Mol. Sci. 2019, 20, 2747. [Google Scholar] [CrossRef] [Green Version]
- Beyth, N.; Houri-Haddad, Y.; Domb, A.; Khan, W.; Hazan, R. Alternative antimicrobial approach: Nano-antimicrobial materials. Evid. Based Complement. Altern. Med. 2015, 2015, 246012. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hemeg, H.A. Nanomaterials for alternative antibacterial therapy. Int. J. Nanomed. 2017, 12, 8211. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dar, M.A.; Gul, R.; Alfadda, A.A.; Karim, M.R.; Kim, D.W.; Cheung, C.L.; Almajid, A.A.; Alharthi, N.; Pulakat, L. Size-dependent effect of nanoceria on their antibacterial activity towards Escherichia coli. Sci. Adv. Mater. 2017, 9, 1248–1253. [Google Scholar] [CrossRef]
- Nastyshyn, S.; Raczkowska, J.; Stetsyshyn, Y.; Orzechowska, B.; Bernasik, A.; Shymborska, Y.; Brzychczy-Włoch, M.; Gosiewski, T.; Lishchynskyi, O.; Ohar, H.; et al. Non-cytotoxic, temperature-responsive and antibacterial POEGMA based nanocomposite coatings with silver nanoparticles. RSC Adv. 2020, 10, 10155–10166. [Google Scholar] [CrossRef]
- Raczkowska, J.; Stetsyshyn, Y.; Awsiuk, K.; Brzychczy-Włoch, M.; Gosiewski, T.; Jany, B.; Lishchynskyi, O.; Shymborska, Y.; Nastyshyn, S.; Bernasikd, A.; et al. “Command” surfaces with thermo-switchable antibacterial activity. Mater. Sci. Eng. C 2019, 103, 109806. [Google Scholar] [CrossRef] [PubMed]
- Thakur, N.; Manna, P.; Das, J. Synthesis and biomedical applications of nanoceria, a redox active nanoparticle. J. Nanobiotechnol. 2019, 17, 84. [Google Scholar] [CrossRef]
- Pop, O.L.; Mesaros, A.; Vodnar, D.C.; Suharoschi, R.; Tăbăran, F.; Magerușan, L.; Tódor, I.S.; Diaconeasa, Z.; Balint, A.; Ciontea, L.; et al. Cerium oxide nanoparticles and their efficient antibacterial application in vitro against gram-positive and gram-negative pathogens. Nanomaterials 2020, 10, 1614. [Google Scholar] [CrossRef]
- Kirby, B. Kirby-Bauer disk diffusion susceptibility test protocol. Am. Soc. Microbiol. 2009, 66, 208. [Google Scholar]
- Clinical and Laboratory Standards Institute (CLSI). Performance Standards for Antimicrobial Susceptibility Testing, 30th ed.; CLSI Supplement M100; Clinical and Laboratory Standards Institute: Wayne, PA, USA, 2020. [Google Scholar]
- Clinical and Laboratory Standards Institute (CLSI). Methods for Antimicrobial Susceptibility Testeding of Anaerobic bacteria, 9th ed.; CLSI standard M11; Clinical and Laboratory Standards Institute: Wayne, PA, USA, 2018. [Google Scholar]
- Al-Bayati, F.A.; Al-Mola, H.F. Antibacterial and antifungal activities of different parts of Tribulus terrestris L. growing in Iraq. J. Zhejiang Univ. Sci. B 2008, 9, 154–159. [Google Scholar] [CrossRef] [Green Version]
- McBride, J.R.; Hass, K.C.; Poindexter, B.D.; Weber, W.H. Raman and x-ray studies of Ce1−x RE x O2−y, where RE = La, Pr, Nd, Eu, Gd, and Tb. J. Appl. Phy. 1994, 76, 2435–2441. [Google Scholar] [CrossRef]
- Bharathi, R.N.; Sankar, S. Investigation of transport properties of Pr doped cerium oxide nanoparticles as a solid electrolyte for IT-SOFC applications. J. Inorg. Organomet. Polym. 2018, 28, 1829–1838. [Google Scholar] [CrossRef]
- Wu, N.-C.; Shi, E.-W.; Zheng, Y.-Q.; Li, W.-J. Effect of pH of medium on hydrothermal synthesis of nanocrystalline cerium(IV) oxide powders. J. Am. Ceram. Soc. 2002, 85, 2462–2468. [Google Scholar] [CrossRef]
- Xu, J.; Li, G.; Li, L. CeO2 nanocrystals: Seed-mediated synthesis and size control. Mater. Res. Bull. 2008, 43, 990–995. [Google Scholar] [CrossRef]
- Arbune, M.; Gurau, G.; Niculet, E.; Iancu, A.V.; Lupasteanu, G.; Fotea, S.; Vasile, M.C.; Tatu, A.L. Prevalence of antibiotic resistance of ESKAPE pathogens over five years in an infectious diseases hospital from South-East of Romania. Infect. Drug Resist. 2021, 14, 2369. [Google Scholar] [CrossRef]
- Kannan, S.K.; Sundrarajan, M. A green approach for the synthesis of a cerium oxide nanoparticle: Characterization and antibacterial activity. Int. J. Nanosci. 2014, 13, 1450018. [Google Scholar] [CrossRef]
- Arumugam, A.; Karthikeyan, C.; Hameed, A.S.H.; Gopinath, K.; Gowri, S.; Karthika, V. Synthesis of cerium oxide nanoparticles using Gloriosa superba L. leaf extract and their structural, optical and antibacterial properties. Mater. Sci. Eng. C 2015, 49, 408–415. [Google Scholar] [CrossRef]
- Yadav, L.R.; Manjunath, K.; Archana, B.; Madhu, C.; Naika, H.R.; Nagabhushana, H.; Nagaraju, G. Fruit juice extract mediated synthesis of CeO 2 nanoparticles for antibacterial and photocatalytic activities. Eur. Phys. J. Plus. 2016, 131, 154. [Google Scholar] [CrossRef]
- Zhang, M.; Zhang, C.; Zhai, X.; Luo, F.; Du, Y.; Yan, C. Antibacterial mechanism and activity of cerium oxide nanoparticles. Sci. China Mater. 2019, 62, 1727–1739. [Google Scholar] [CrossRef] [Green Version]
- Farias, I.A.P.; Santos, C.C.L.D.; Sampaio, F.C. Antimicrobial activity of cerium oxide nanoparticles on opportunistic microorganisms: A systematic review. BioMed Res. Int. 2018, 2018, 1923606. [Google Scholar] [CrossRef] [Green Version]




| EP # | Antibiotics $/Inhibition Zone (mm) + | ||||||
|---|---|---|---|---|---|---|---|
| CIP | AMX | CPM | CEF | GEN | AK | IPM | |
| Ef | 7.00 ± 0.3 (R) | 9.00 ± 0.2 (R) | 11.00 ± 0.4 (R) | 18.00 ± 0.1 (S) | 9.00 ± 0.1 (I) | 15.00 ± 0.1 (I) | 17.00 ± 0.5 (R) |
| Sa | 10.00 ± 0.5 (R) | 12.00 ± 0.2 (R) | 23.00 ± 0.4 (S) | 21.00 ± 0.5 (R) | 12.00 ± 0.5 (R) | 18.00 ± 0.5 (I) | 22.00 ± 0.6 (R) |
| Kp | 11.00 ± 0.2 (R) | 13.00 ± 0.4 (R) | 17.00 ± 1.0 (R) | 22.00 ± 0.6 (S) | 22.00 ± 0.6 (S) | 12.00 ± 0.6 (R) | 15.00 ± 0.5 (R) |
| Ab | 0.0 (R) | 0.00 (R) | 9.50 ± 0.5 (R) | 15.00 ± 0.5 (R) | 15.00 ± 0.5 (R) | 13.00 ± 0.5 (R) | 19.50 ± 0.5 (I) |
| Pa | 9.00 ± 0.5 (R) | 11.00 ± 0.5 (R) | 19.00 ± 0.5 (S) | 18.50 ± 0.5 (S) | 14.50 ± 0.5 (R) | 18.50 ± 0.5 (S) | 16.00 ± 0.2 (R) |
| Ec | 10.00 ± 0.1 (R) | 12.00 + 0.5 (R) | 15.00 ± 0.4 (R) | 14.00 ± 0.2 (R) | 13.00 ± 0.2 (I) | 12.00 ± 0.2 (R) | 18.00 ± 0.5 (R) |
| ESKAPE Pathogens | Concentration of CeO2-NPs (µg/mL) | Streptomycin (µg/mL) | ||
|---|---|---|---|---|
| 15 | 25 | 50 | 10 | |
| E. faecium ATCC 51559 | 7.53 ± 0.30 *** | 9.25 ± 0.05 *** | 10.92 ± 0.15 *** | 17.83 ± 0.08 |
| S. aureus ATCC 25904 | 9.70 ± 0.40 *** | 11.78 ± 0.15 *** | 19.00 ± 0.40 ** | 19.40 ± 0.05 |
| K. pneumoniae ATCC 13883 | 10.76 ± 0.10 ** | 12.95 ± 0.13 ** | 17.45 ± 0.01 ** | 22.25 ± 0.13 |
| A. baumannii ATCC 1799 | NIZ $ | NIZ | 8.86 ± 0.03 ** | 15.25 ± 0.12 |
| P. aeruginosa ATCC 10145 | 8.96 ± 0.10 ** | 11.55 ± 0.13 ** | 17.83 ± 0.21 NS | 18.50 ± 0.50 |
| E. cloacae ATCC 35549 | 10.45 ± 0.13 *** | 11.95 + 0.08 *** | 14.90 ± 0.08 ** | 20.75 ± 0.13 |
| ESKAPE Pathogens | MIC (µg/mL) | |
|---|---|---|
| CeO2-NPs | Streptomycin | |
| E. faecium ATCC 51559 | 125.0 | 10.0 |
| S. aureus ATCC 25904 | 15.6 | 5.0 |
| K. pneumoniae ATCC 13883 | 31.2 | 5.0 |
| A. baumannii ATCC 1799 | 250.0 | 5.0 |
| P. aeruginosa ATCC 10145 | 31.2 | 5.0 |
| E. cloacae ATCC 35549 | 62.5 | 5.0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dar, M.A.; Gul, R.; Karuppiah, P.; Al-Dhabi, N.A.; Alfadda, A.A. Antibacterial Activity of Cerium Oxide Nanoparticles against ESKAPE Pathogens. Crystals 2022, 12, 179. https://doi.org/10.3390/cryst12020179
Dar MA, Gul R, Karuppiah P, Al-Dhabi NA, Alfadda AA. Antibacterial Activity of Cerium Oxide Nanoparticles against ESKAPE Pathogens. Crystals. 2022; 12(2):179. https://doi.org/10.3390/cryst12020179
Chicago/Turabian StyleDar, Mushtaq A., Rukhsana Gul, Ponmurugan Karuppiah, Naif A. Al-Dhabi, and Assim A. Alfadda. 2022. "Antibacterial Activity of Cerium Oxide Nanoparticles against ESKAPE Pathogens" Crystals 12, no. 2: 179. https://doi.org/10.3390/cryst12020179








