Development of Hallux Valgus Classification Using Digital Foot Images with Machine Learning
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Materials
2.2. Severity of Hallux Valgus
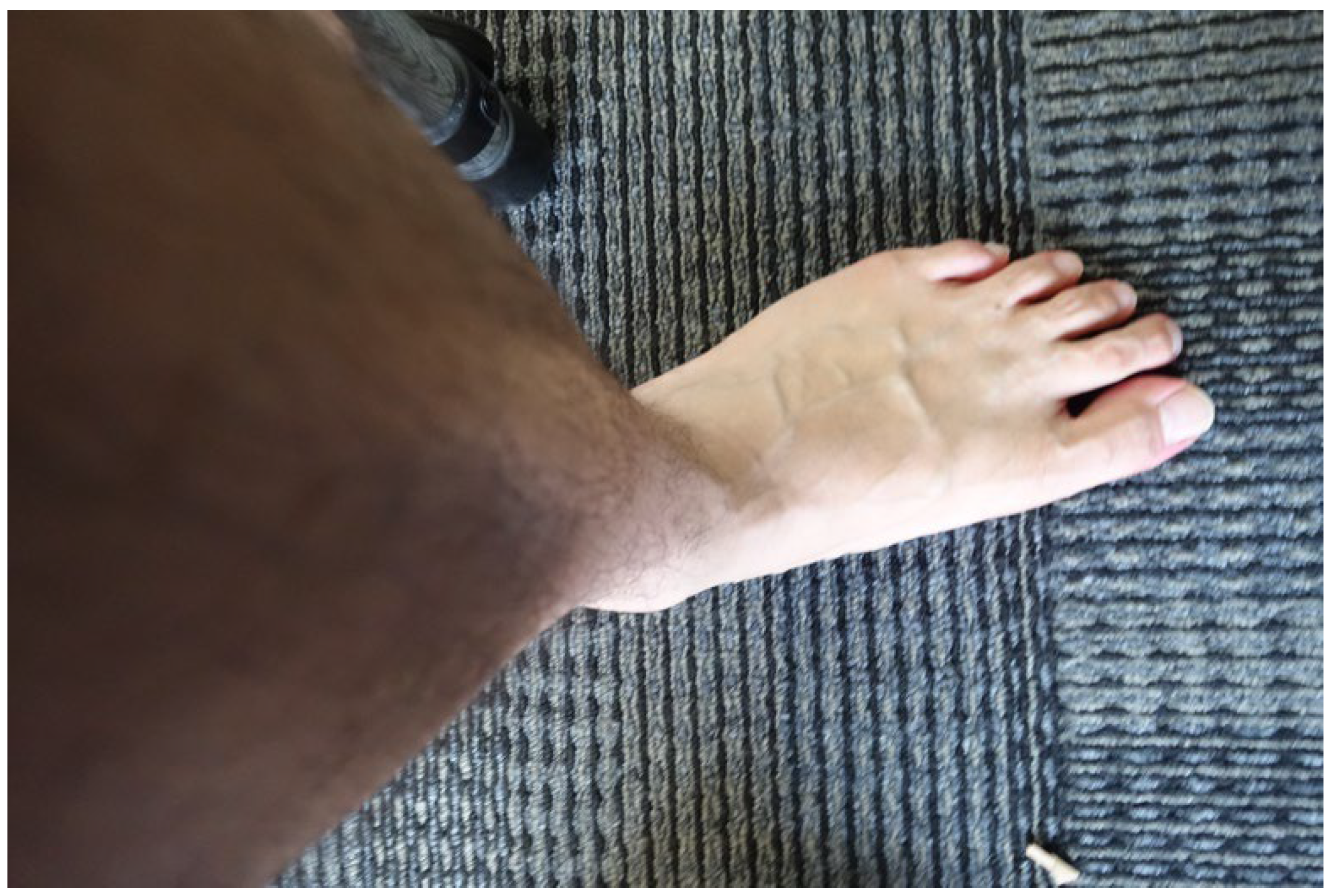
2.3. Foot Imaging
- Pattern A (Figure 4A)
- (1)
- The image was converted to a size width of 640 pixels and the background was digitally removed. The foot image was adjusted to horizontal orientation. The image was cropped so that only the area from the toes to the midfoot area was included.
- Pattern B (Figure 4B)
- (2)
- The right foot image was vertically inverted to match the orientation of the left and right feet.
- (3)
- The image was converted to grayscale, the edges were enhanced, and the image was cropped so that only the midfoot area from the tip of the hallux was included.
- (4)
- The normal group (n = 304) and the HV group (n = 203) have different numbers of images, which could negatively affect the accuracy. Data augmentation was therefore performed on the images in the HV group. This involved changing the contrast and saturation of 101 randomly selected images in the HV group. Color jittering, such as varying of saturation and contrast, is common in data augmentation used in machine learning research [18].
2.4. Classification by Machine Learning
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mann, R.A.; Coughlin, M.J. Hallux valgus—Etiology, anatomy, treatment and surgical considerations. Clin. Orthop. Relat. Res. 1981, 157, 31–41. [Google Scholar] [CrossRef]
- Nix, S.; Smith, M.; Vicenzino, B. Prevalence of hallux valgus in the general population: A systematic review and meta-analysis. J. Foot Ankle Res. 2010, 3, 21. [Google Scholar] [CrossRef] [PubMed]
- Cho, N.H.; Kim, S.; Kwon, D.J.; Kim, H.A. The prevalence of hallux valgus and its association with foot pain and function in a rural Korean community. J. Bone Jt. Surg. Br. 2009, 91, 494–498. [Google Scholar] [CrossRef] [PubMed]
- Menz, H.B.; Roddy, E.; Thomas, E.; Croft, P.R. Impact of hallux valgus severity on general and foot-specific health-related quality of life. Arthritis Care Res. 2011, 63, 396–404. [Google Scholar]
- Abhishek, A.; Roddy, E.; Zhang, W.; Doherty, M. Are hallux valgus and big toe pain associated with impaired quality of life? A cross-sectional study. Osteoarthr. Cartil. 2010, 18, 923–926. [Google Scholar] [CrossRef] [PubMed]
- Nix, S.E.; Vicenzino, B.T.; Smith, M.D. Foot pain and functional limitation in healthy adults with hallux valgus: A cross-sectional study. BMC Musculoskelet. Disord. 2012, 13, 197. [Google Scholar] [CrossRef]
- Menz, H.B.; Morris, M.E.; Lord, S.R. Foot and ankle risk factors for falls in older people: A prospective study. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 61, 866–870. [Google Scholar] [CrossRef]
- Shinohara, M.; Yamaguchi, S.; Ono, Y.; Kimura, S.; Kawasaki, Y.; Sugiyama, H.; Akagi, R.; Sasho, T.; Ohtori, S. Anatomical factors associated with progression of hallux valgus. Foot Ankle Surg. 2022, 28, 240–244. [Google Scholar] [CrossRef]
- Coughlin, M.J.; Saltzman, C.L.; Nunley, J.A., 2nd. Angular measurements in the evaluation of hallux valgus deformities: A report of the ad hoc committee of the American Orthopaedic Foot & Ankle Society on angular measurements. Foot Ankle Int. 2002, 23, 68–74. [Google Scholar]
- Menz, H.B.; Harrison, C.; Britt, H.; Whittaker, G.A.; Landorf, K.B.; Munteanu, S.E. Management of Hallux Valgus in General Practice in Australia. Arthritis Care Res. 2020, 72, 1536–1542. [Google Scholar] [CrossRef]
- Kario, K. Home Blood Pressure Monitoring: Current Status and New Developments. Am. J. Hypertens. 2021, 34, 783–794. [Google Scholar] [CrossRef] [PubMed]
- Garrow, A.P.; Papageorgiou, A.; Silman, A.J.; Thomas, E.; Jayson, M.I.; Macfarlane, G.J. The grading of hallux valgus. The Manchester Scale. J. Am. Podiatr. Med. Assoc. 2001, 91, 74–78. [Google Scholar] [CrossRef] [PubMed]
- Iliou, K.; Paraskevas, G.; Kanavaros, P.; Barbouti, A.; Vrettakos, A.; Gekas, C.; Kitsoulis, P. Correlation between Manchester Grading Scale and American Orthopaedic Foot and Ankle Society Score in Patients with Hallux Valgus. Med. Princ. Pract. 2016, 25, 21–24. [Google Scholar] [CrossRef] [PubMed]
- Menz, H.B.; Fotoohabadi, M.R.; Wee, E.; Spink, M.J. Validity of self-assessment of hallux valgus using the Manchester scale. BMC Musculoskelet. Disord. 2010, 11, 215. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Han, Z.; Wang, J.; Yang, C. The emerging roles of machine learning in cardiovascular diseases: A narrative review. Ann. Transl. Med. 2022, 10, 611. [Google Scholar] [CrossRef]
- Sakai, K.; Gilmour, S.; Hoshino, E.; Nakayama, E.; Momosaki, R.; Sakata, N.; Yoneoka, D. A Machine Learning-Based Screening Test for Sarcopenic Dysphagia Using Image Recognition. Nutrients 2021, 13, 4009. [Google Scholar] [CrossRef]
- Lopez, D.L.; Callejo Gonzalez, L.; Losa Iglesias, M.E.; Canosa, J.L.; Sanz, D.R.; Lobo, C.C.; Becerro de Bengoa Vallejo, R. Quality of Life Impact Related to Foot Health in a Sample of Older People with Hallux Valgus. Aging Dis. 2016, 7, 45–52. [Google Scholar] [CrossRef]
- Shorten, C.; Khoshgoftaar, T.M. A survey on Image Data Augmentation for Deep Learning. J. Big Data 2019, 6, 60. [Google Scholar] [CrossRef]
- Alshammari, A. Construction of VGG16 Convolution Neural Network (VGG16_CNN) Classifier with NestNet-Based Segmentation Paradigm for Brain Metastasis Classification. Sensors 2022, 22, 8076. [Google Scholar] [CrossRef]
- Ding, I.J.; Zheng, N.W. CNN Deep Learning with Wavelet Image Fusion of CCD RGB-IR and Depth-Grayscale Sensor Data for Hand Gesture Intention Recognition. Sensors 2022, 22, 803. [Google Scholar] [CrossRef]
- Khandakar, A.; Chowdhury, M.E.H.; Reaz, M.B.I.; Ali, S.H.M.; Abbas, T.O.; Alam, T.; Ayari, M.A.; Mahbub, Z.B.; Habib, R.; Rahman, T.; et al. Thermal Change Index-Based Diabetic Foot Thermogram Image Classification Using Machine Learning Techniques. Sensors 2022, 22, 1793. [Google Scholar] [CrossRef] [PubMed]
- Özkaraca, O.; Bağrıaçık, O.İ.; Gürüler, H.; Khan, F.; Hussain, J.; Khan, J.; Laila, U.E. Multiple Brain Tumor Classification with Dense CNN Architecture Using Brain MRI Images. Life 2023, 13, 349. [Google Scholar] [CrossRef] [PubMed]
- Qin, Y.; Wu, J.; Xiao, W.; Wang, K.; Huang, A.; Liu, B.; Yu, J.; Li, C.; Yu, F.; Ren, Z. Machine Learning Models for Data-Driven Prediction of Diabetes by Lifestyle Type. Int. J. Environ. Res. Public Health 2022, 19, 15027. [Google Scholar] [CrossRef] [PubMed]
- Kong, Y.; Kong, X.; He, C.; Liu, C.; Wang, L.; Su, L.; Gao, J.; Guo, Q.; Cheng, R. Constructing an automatic diagnosis and severity-classification model for acromegaly using facial photographs by deep learning. J. Hematol. Oncol. 2020, 13, 88. [Google Scholar] [CrossRef]
- Esteva, A.; Kuprel, B.; Novoa, R.A.; Ko, J.; Swetter, S.M.; Blau, H.M.; Thrun, S. Dermatologist-level classification of skin cancer with deep neural networks. Nature 2017, 542, 115–118. [Google Scholar] [CrossRef] [PubMed]
- Duong, D.L.; Kabir, M.H.; Kuo, R.F. Automated caries detection with smartphone color photography using machine learning. Health Inform. 2021, 27, 14604582211007530. [Google Scholar] [CrossRef]
- Lalehzarian, S.P.; Gowd, A.K.; Liu, J.N. Machine learning in orthopaedic surgery. World J. Orthop. 2021, 12, 685–699. [Google Scholar] [CrossRef]
- Lau, L.C.M.; Chui, E.C.S.; Man, G.C.W.; Xin, Y.; Ho, K.K.W.; Mak, K.K.K.; Ong, M.T.Y.; Law, S.W.; Cheung, W.H.; Yung, P.S.H. A novel image-based machine learning model with superior accuracy and predictability for knee arthroplasty loosening detection and clinical decision making. J. Orthop. Translat. 2022, 36, 177–183. [Google Scholar] [CrossRef]
- Xue, Y.; Zhang, R.; Deng, Y.; Chen, K.; Jiang, T. A preliminary examination of the diagnostic value of deep learning in hip osteoarthritis. PLoS ONE 2017, 12, e0178992. [Google Scholar] [CrossRef]
- Yunus, U.; Amin, J.; Sharif, M.; Yasmin, M.; Kadry, S.; Krishnamoorthy, S. Recognition of Knee Osteoarthritis (KOA) Using YOLOv2 and Classification Based on Convolutional Neural Network. Life 2022, 12, 1126. [Google Scholar] [CrossRef]
- Goyal, S.; Singh, R. Detection and classification of lung diseases for pneumonia and Covid-19 using machine and deep learning techniques. J. Ambient. Intell. Humaniz. Comput. 2021, 14, 3239–3259. [Google Scholar] [CrossRef] [PubMed]
- Yedjou, C.G.; Tchounwou, S.S.; Aló, R.A.; Elhag, R.; Mochona, B.; Latinwo, L. Application of Machine Learning Algorithms in Breast Cancer Diagnosis and Classification. Int. J. Sci. Acad. Res. 2021, 2, 3081–3086. [Google Scholar] [PubMed]



| Category | Number | Classification |
|---|---|---|
| No deformity | 243 | Normal |
| Mild deformity | 61 | |
| Moderate deformity | 122 | Hallux valgus |
| Severe deformity | 81 |
| Pattern A | Prediction | ||
|---|---|---|---|
| HV | Normal | ||
| Result | HV | 72 | 157 |
| Normal | 13 | 206 | |
| Pattern B | Prediction | ||
| HV | Normal | ||
| Result | HV | 102 | 128 |
| Normal | 28 | 423 | |
| Accuracy | Precision | Recall | F1 Score | |
|---|---|---|---|---|
| Pattern A | 0.62 | 0.56 | 0.94 | 0.71 |
| Pattern B | 0.79 | 0.77 | 0.96 | 0.86 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hida, M.; Eto, S.; Wada, C.; Kitagawa, K.; Imaoka, M.; Nakamura, M.; Imai, R.; Kubo, T.; Inoue, T.; Sakai, K.; et al. Development of Hallux Valgus Classification Using Digital Foot Images with Machine Learning. Life 2023, 13, 1146. https://doi.org/10.3390/life13051146
Hida M, Eto S, Wada C, Kitagawa K, Imaoka M, Nakamura M, Imai R, Kubo T, Inoue T, Sakai K, et al. Development of Hallux Valgus Classification Using Digital Foot Images with Machine Learning. Life. 2023; 13(5):1146. https://doi.org/10.3390/life13051146
Chicago/Turabian StyleHida, Mitsumasa, Shinji Eto, Chikamune Wada, Kodai Kitagawa, Masakazu Imaoka, Misa Nakamura, Ryota Imai, Takanari Kubo, Takao Inoue, Keiko Sakai, and et al. 2023. "Development of Hallux Valgus Classification Using Digital Foot Images with Machine Learning" Life 13, no. 5: 1146. https://doi.org/10.3390/life13051146
APA StyleHida, M., Eto, S., Wada, C., Kitagawa, K., Imaoka, M., Nakamura, M., Imai, R., Kubo, T., Inoue, T., Sakai, K., Orui, J., Tazaki, F., Takeda, M., Hasegawa, A., Yamasaka, K., & Nakao, H. (2023). Development of Hallux Valgus Classification Using Digital Foot Images with Machine Learning. Life, 13(5), 1146. https://doi.org/10.3390/life13051146







