Bacterial Contamination in Total Joint Replacement: Should We Change into a New Set of Clean Scrub Suits Whenever Entering the Operating Room?
Abstract
:1. Introduction
2. Methods
2.1. Samples
2.2. Bacterial Contamination Analysis
2.3. Statistical Analysis
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ayliffe, G.A. Role of the environment of the operating suite in surgical wound infection. Rev. Infect. Dis. 1991, 13 (Suppl. 10), S800–S804. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Health and Care Excellence. Surgical Site Infections: Prevention and Treatment; NICE: London, UK, 2019; Available online: https://www.nice.org.uk/guidance/ng125/resources/surgical-site-infections-prevention-and-treatment-pdf-66141660564421 (accessed on 6 April 2023).
- Proceeding of the Second International Consensus Meeting on Musculoskeletal Infection. 2018. Available online: https://icmphilly.com/questions/question-7-does-strict-adherence-to-not-wearing-operating-room-or-attire-outside-the-hospital-or-outside-the-restricted-or-area-reduce-the-risk-of-surgical-site-infections-periprosthetic-joint-inf/ (accessed on 15 August 2022).
- American College of Surgeons. Statement on Operating Room Attire. Bull. Am. Coll. Surg. 2016. Available online: https://cms.acs.siteworx.com/about-acs/statements/87-surgical-attire (accessed on 6 April 2023).
- Roxburgh, M.; Gall, P.; Lee, K. A cover up? Potential risks of wearing theatre clothing outside theatre. J. Perioper. Pract. 2006, 16, 30–33, 35–41. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Humphreys, H.; Bak, A.; Mugglestone, M.A.; Pinkney, T.D.; Skelton, L.; Vos, M.C.; Ridgway, E.J. Operating theatre attire (scrub suits) worn outside the operating theatre: Infection risk or not? Hosp. Infect. 2021, 108, 209–211. [Google Scholar] [CrossRef] [PubMed]
- Sogawa, K.; Watanabe, M.; Sato, K.; Segawa, S.; Ishii, C.; Miyabe, A.; Murata, S.; Saito, T.; Nomura, F. Use of the MALDI BioTyper system with MALDI-TOF mass spectrometry for rapid identification of microorganisms. Anal. Bioanal. Chem. 2011, 400, 1905–1911. [Google Scholar] [CrossRef]
- Nickinson, R.S.J.; Board, T.N.; Gambhir, A.K.; Porter, M.L.; Kay, P.R. The microbiology of the infected knee arthroplasty. Int. Orthop. 2010, 34, 505–510. [Google Scholar] [CrossRef] [Green Version]
- Drago, L.; De Vecchi, E.; Bortolin, M.; Zagra, L.; Romanò, C.L.; Cappelletti, L. Epidemiology and antibiotic resistance of late prosthetic knee and hip infections. J. Arthroplast. 2017, 32, 2496–2500. [Google Scholar] [CrossRef]
- Stefánsdóttir, A.; Johansson, D.; Knutson, K.; Lidgren, L.; Robertsson, O. Microbiology of the infected knee arthroplasty: Report from the Swedish Knee Arthroplasty Register on 426 surgically revised cases. Scand J. Infect. Dis. 2009, 41, 831–840. [Google Scholar] [CrossRef]
- Hickson, C.J.; Metcalfe, D.; Elgohari, S.; Oswald, T.; Masters, J.P.; Rymaszewska, M.; Reed, M.R.; Sprowson, A.P. Prophylactic antibiotics in elective hip and knee arthroplasty: An analysis of organisms reported to cause infections and National survey of clinical practice. Bone Jt. Res. 2015, 4, 181–189. [Google Scholar] [CrossRef] [Green Version]
- Gao, Z.; Du, Y.; Piao, S.; Sun, J.; Li, X.; Zhou, Y. Comparison between the staphylococci aureus and coagulase-negative staphylococci infected total joint arthroplasty treated by two-stage revision: A retrospective study with two year minimum follow-up. J. Orthop. Sci. 2019, 24, 109–115. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Morse, D.T. MINSIZE2: A computer program for determining effect size and minimum sample size for statistical significance for univariate, multivariate, and nonparametric tests. Educ. Psychol. Meas. 1999, 59, 518–531. [Google Scholar] [CrossRef]
- Braswell, M.L.; Spruce, L. Implementing AORN recommended practices for surgical attire. AORN J. 2012, 95, 122–137. [Google Scholar] [CrossRef]
- Lafrenière, R.; Bohnen, J.M.; Pasieka, J.; Spry, C.C. Infection control in the operating room: Current practices or sacred cows? J. Am. Coll. Surg. 2001, 193, 407–416. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, N.J.; Evans, D.S.; Kerr, A. Reduction of skin bacteria in theatre air with comfortable, non-woven disposable clothing for operating-theatre staff. Br. Med. J. 1978, 1, 696–698. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hee, H.I.; Lee, S.; Chia, S.N.; Lu, Q.S.; Liew, A.P.; Ng, A. Bacterial contamination of surgical scrub suits worn outside the operating theatre: A randomised crossover study. Anaesthesia 2014, 69, 816–825. [Google Scholar] [CrossRef]
- Proceeding of the International Consensus Meeting on Peri-prosthetic Joint Infection. 2013. Available online: https://www.efort.org/wpcontent/uploads/2013/10/Philadelphia_Consensus.pdf (accessed on 6 April 2023).
- Tateiwa, T.; Masaoka, T.; Ishida, T.; Shishido, T.; Takahashi, Y.; Yamamoto, K. Impact of surgical clothing and footwear on operating room contamination during standstill and intraoperative stepping motion. J. Orthop. Surg. 2020, 28, 2309499020976232. [Google Scholar] [CrossRef]
- Wright, S.N.; Gerry, J.S.; Busowski, M.T.; Klochko, A.Y.; McNulty, S.G.; Brown, S.A.; Sieger, B.E.; Ken Michaels, P.; Wallace, M.R. Gordonia bronchialis sternal wound infection in 3 patients following open heart surgery: Intraoperative transmission from a healthcare worker. Infect. Control Hosp. Epidemiol. 2012, 33, 1238–1241. [Google Scholar] [CrossRef] [PubMed]
- Sivanandan, I.; Bowker, K.E.; Bannister, G.C.; Soar, J. Reducing the risk of surgical site infection: A case controlled study of contamination of theatre clothing. J. Perioper. Pract. 2011, 21, 69–72. [Google Scholar] [CrossRef]
- National Association of Theatre Nurses. NATN: 1998 Principles of Safe Practice in the Perioperative Environment; NATN: Harrogate, UK, 1998. [Google Scholar]
- Association of periOperative Registered Nurses. AORN: 2020 Guidelines for Perioperative Practice. Available online: https://pdihc.com/wp-content/uploads/2019/10/AORN-Guideline-for-Surgical-Attire.pdf (accessed on 6 April 2023).
- Hafiani, E.M.; Cassier, P.; Aho, S.; Albaladejo, P.; Beloeil, H.; Boudot, E.; Carenco, P.; Lallemant, F.; Leroy, M.G.; Muret, J.; et al. Guidelines for clothing in the operating theatre, 2021. Anaesth. Crit. Care Pain Med. 2022, 41, 101084. [Google Scholar] [CrossRef]
- Weinbroum, A.A.; Ezri, T.; Harow, E.; Tsivian, A.; Serour, F.J. Wearing surgical attire outside the operating room: A survey of habits of anesthesiologists and surgeons in Israel. Am. Coll. Surg. 2007, 205, 314–318. [Google Scholar] [CrossRef]
- McHugh, S.M.; Corrigan, M.A.; Hill, A.D.; Humphreys, H. Surgical attire, practices and their perception in the prevention of surgical site infection. Surgeon 2014, 12, 47–52. [Google Scholar] [CrossRef]
- Kaplan, C.; Mendiola, R.; Ndjatou, V.; Chapnick, E.; Minkoff, H. The role of covering gowns in reducing rates of bacterial contamination of scrub suits. Am. J. Obstet. Gynecol. 2003, 188, 1154–1155. [Google Scholar] [CrossRef] [PubMed]
- Practice Guidelines for Surgical Care, Third Ed. 2019. Available online: http://jaom.kenkyuukai.jp/images/sys/information/20210616135951-48BD57DC717273CD728785686C6592D9FF323FBF97D4BAC7ECA952EB16C01D2B.pdf (accessed on 6 April 2023).
- Woodhead, K.; Taylor, E.W.; Bannister, G.; Chesworth, T.; Hoffman, P.; Humphreys, H. Behaviours and rituals in the operating theatre. A report from the Hospital Infection Society Working Party on Infection Control in Operating Theatres. J. Hosp. Infect. 2002, 51, 241–255. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wilson, J.A.; Loveday, H.P.; Hoffman, P.N.; Pratt, R.J. Uniform: An evidence review of the microbiological significance of uniforms and uniform policy in the prevention and control of healthcare-associated infections. Report to the Department of Health (England). J. Hosp. Infect. 2007, 66, 301–307. [Google Scholar] [CrossRef] [PubMed]

| Group | The Duration of Wearing the Same Suit (Hours), Median (IQR) |
|---|---|
| Control | 0.0 (0.0 to 0.0) |
| IN(sp)_ST | 2.0 (2.0 to 2.0) |
| IN_MID | 4.0 (3.5 to 4.6) |
| IN_LO | 8.0 (8.0 to 8.5) |
| IN(sp) + OUT(w)_ST | 3.0 (2.5 to 4.0) |
| OUT(w)_LO | 14.5 (14.0 to 14.5) |
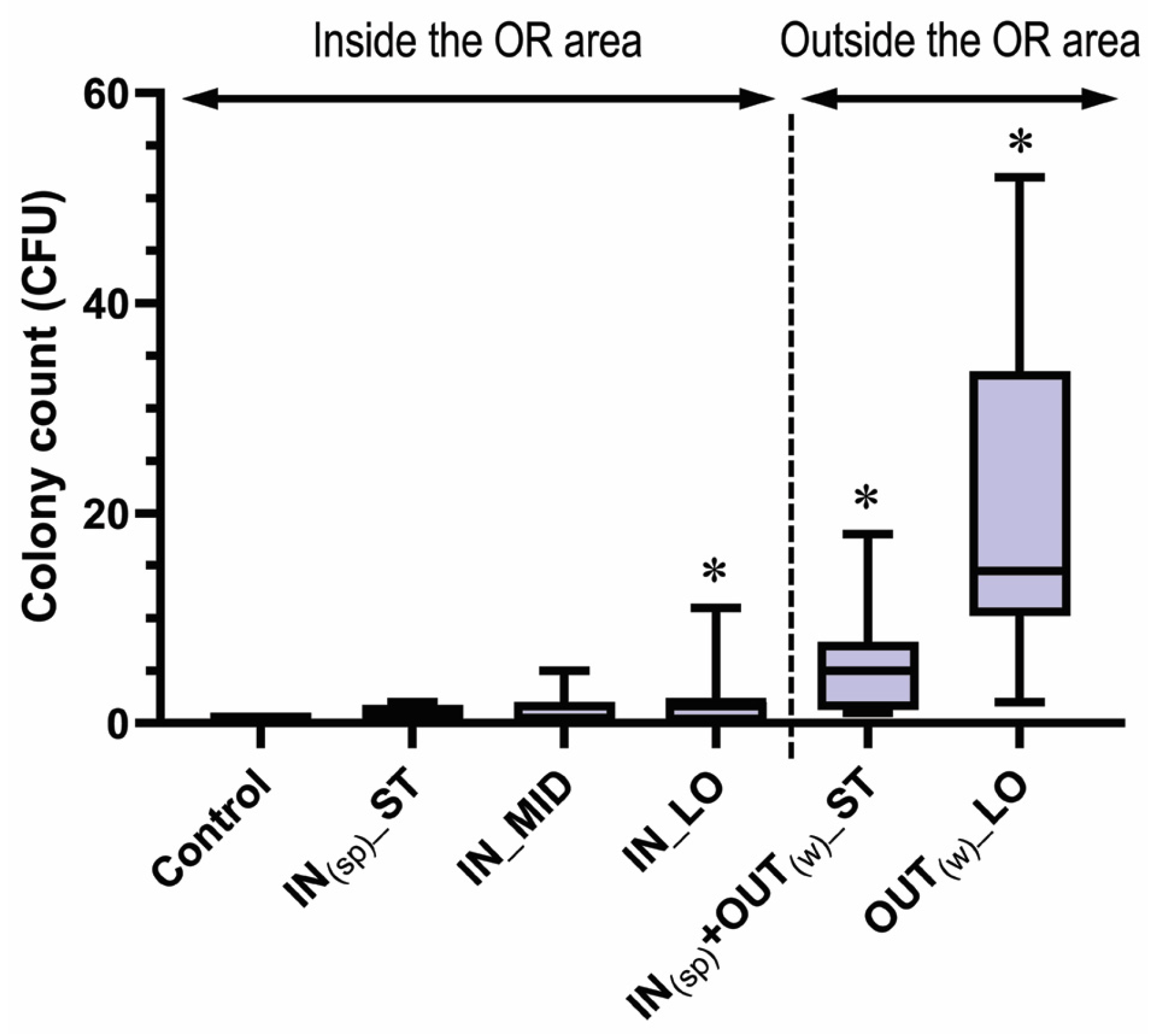
| Group | Bacterial Colony Count (CFU), Median (IQR) | p-Value | Effect Size, r |
|---|---|---|---|
| Control | 0.0 (0.0 to 1.0) | N/A | N/A |
| IN(sp)_ST | 1.0 (0.0 to 1.3) | 0.142 | 0.35 |
| IN_MID | 0.5 (0.0 to 2.0) | 0.348 | 0.21 |
| IN_LO | 2.0 (0.3 to 2.0) | 0.019 * | 0.51 † |
| IN(sp) + OUT(w)_ST | 5.0 (1.8 to 7.3) | <0.0001 * | 0.73 † |
| OUT(w)_LO | 14.5 (11.3 to 29.8) | <0.0001 * | 0.85 † |
| Group | Bacterial Colony Species (the Number of Cases Detected) |
|---|---|
| Control (n = 10) | GPR (2), Bacillus subtilis (1), Micrococcus luteus (1) |
| IN(sp)_ST (n = 12) | Bacillus subtilis (3), Bacillus cereus (2), Bacillus species (1), Staphylococcus hominis * (1), Micrococcus luteus (1) |
| IN_MID (n = 12) | Bacillus subtilis (4), Micrococcus luteus (2), Staphylococcus epidermidis * (1), CNS * (1), Bacillus megaterium (1), Sporosarcina koreensis (1) |
| IN_LO (n = 11) | Bacillus subtilis (4), Micrococcus luteus (3), Staphylococcus epidermidis * (1), Staphylococcus capitis * (1), Bacillus cereus (1), Bacillus megaterium (1), Roseomonas mucosa (1), Moraxella osloensis (1) |
| IN(sp) + OUT(w)_ST (n = 20) | Bacillus subtilis (11), Micrococcus luteus (8), Bacillus species (3), Acinetobacter species (2), Micrococcus species (2), Staphylococcus hominis * (2), Staphylococcus lugdunensis * (1), Staphylococcus saprophyticus * (1), Bacillus flexus (1), Bacillus cereus (1), Roseomonas mucosa (1), Kocuria species (1), Streptococcus species (1) |
| OUT(w)_LO (n = 10) | Bacillus subtilis (9), Micrococcus luteus (4), Staphylococcus epidermidis * (3), Staphylococcus saprophyticus * (2), Staphylococcus hominis * (1), Aerococcus viridans (1), Enterococcus faecalis (1), Roseomonas mucosa (1), Pantoea septica (1) |
| Group | Any Bacterial Contamination | CNS Contamination | ||||
|---|---|---|---|---|---|---|
| Probability (%) | p-Value | Effect Size, φ | Probability (%) | p-Value | Effect Size, φ | |
| Control (n = 10) | 40.0 (4/10) | N/A | N/A | 0 (0/10) | N/A | N/A |
| IN(sp)_ST (n = 12) | 66.7 (8/12) | 0.211 | 0.27 | 8.3 (1/12) | 0.350 | 0.20 |
| IN_MID (n = 12) | 66.7 (8/12) | 0.211 | 0.27 | 16.7 (2/12) | 0.176 | 0.29 |
| IN_LO (n = 11) | 72.7 (8/11) | 0.130 | 0.32 | 18.2 (2/11) | 0.156 | 0.31 |
| IN(sp) + OUT(w)_ST (n = 20) | 100 (20/20) | 0.0001 * | 0.71 † | 20 (4/20) | 0.129 | 0.28 |
| OUT(w)_LO (n = 10) | 100 (10/10) | 0.003 * | 0.66 † | 50 (5/10) | 0.010 * | 0.58 † |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tateiwa, T.; Takahashi, Y.; Ishida, T.; Masaoka, T.; Shishido, T.; Yamamoto, K. Bacterial Contamination in Total Joint Replacement: Should We Change into a New Set of Clean Scrub Suits Whenever Entering the Operating Room? Life 2023, 13, 1615. https://doi.org/10.3390/life13071615
Tateiwa T, Takahashi Y, Ishida T, Masaoka T, Shishido T, Yamamoto K. Bacterial Contamination in Total Joint Replacement: Should We Change into a New Set of Clean Scrub Suits Whenever Entering the Operating Room? Life. 2023; 13(7):1615. https://doi.org/10.3390/life13071615
Chicago/Turabian StyleTateiwa, Toshiyuki, Yasuhito Takahashi, Tsunehito Ishida, Toshinori Masaoka, Takaaki Shishido, and Kengo Yamamoto. 2023. "Bacterial Contamination in Total Joint Replacement: Should We Change into a New Set of Clean Scrub Suits Whenever Entering the Operating Room?" Life 13, no. 7: 1615. https://doi.org/10.3390/life13071615






