Exploring the Pattern of Immunization Dropout among Children in India: A District-Level Comparative Analysis
Abstract
:1. Introduction
2. Method and Materials
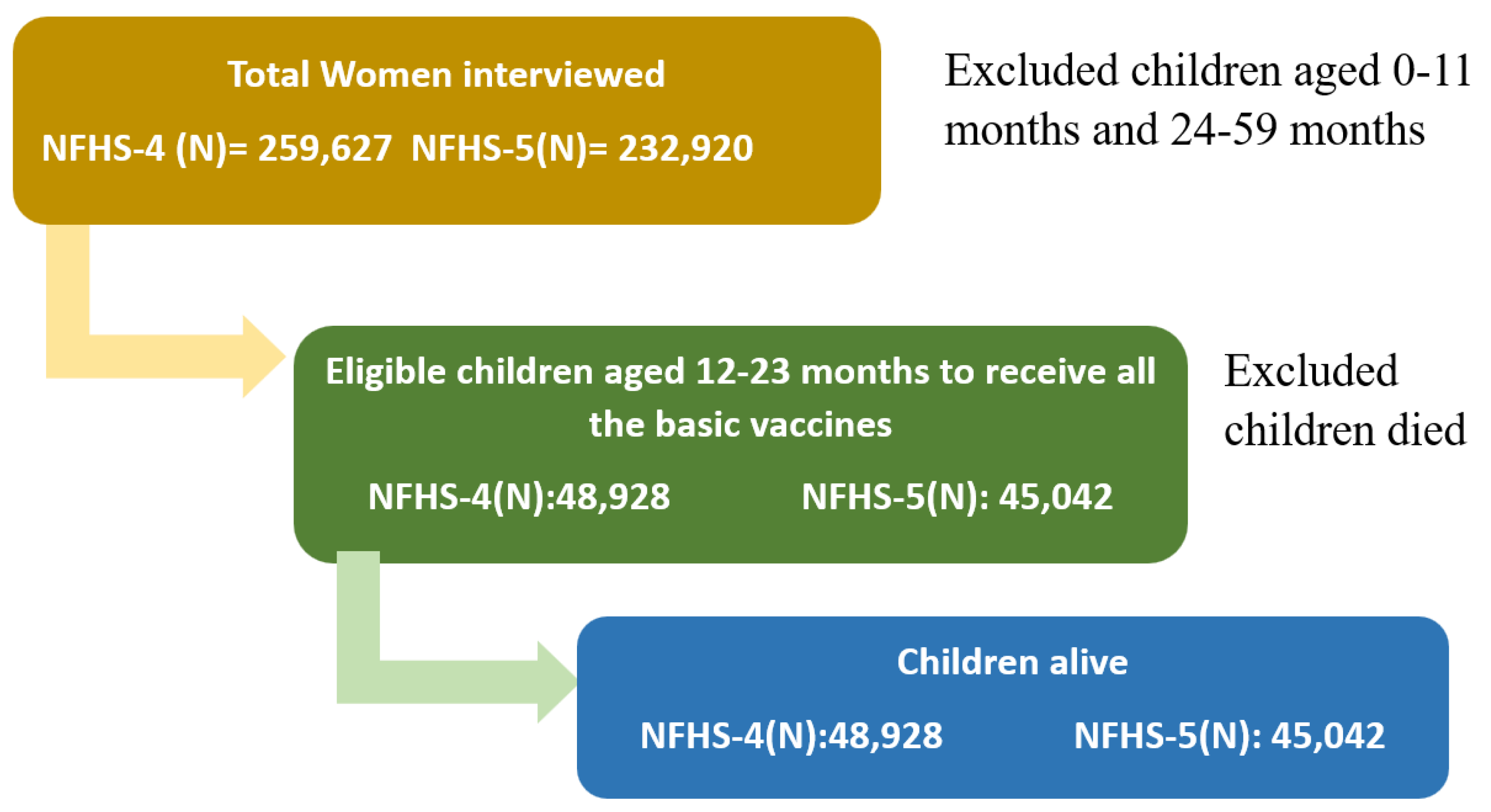
2.1. Data Source
2.2. Immunization Services in India
2.3. Dependent Variable
2.4. Independent Variables
2.5. Statistical Analysis
3. Results
3.1. Study Characteristics of the Sample
3.2. Antigen-Wise Coverage and Dropout Rates
3.3. State-Wise Dropout Rates
3.4. District-Level Dropout Rates in NFHS-4 and NFHS-5
3.5. Dropout Rates by Background Characteristics
3.6. Factors Affecting Dropout Rates
3.7. Decomposition Result of Gap in the Dropout Rate
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wondimu, A.; Cao, Q.; Asuman, D.; Almansa, J.; Postma, M.J.; van Hulst, M. Understanding the improvement in full childhood vaccination coverage in Ethiopia using Oaxaca–blinder decomposition analysis. Vaccines 2020, 8, 505. [Google Scholar] [CrossRef]
- Ali, H.A.; Hartner, A.M.; Echeverria-Londono, S.; Roth, J.; Li, X.; Abbas, K.; Portnoy, A.; Vynnycky, E.; Woodruff, K.; Ferguson, N.M.; et al. Vaccine equity in low and middle income countries: A systematic review and meta-analysis. Int. J. Equity Health 2022, 21, 82. [Google Scholar] [CrossRef] [PubMed]
- Greenwood, B. The contribution of vaccination to global health: Past, present and future. Philos. Trans. R. Soc. B Biol. Sci. 2014, 369, 20130433. [Google Scholar] [CrossRef] [PubMed]
- Wallace, A.S.; Ryman, T.K.; Privor-Dumm, L.; Morgan, C.; Fields, R.; Garcia, C.; Sodha, S.; Lindstrand, A.; Lochlainn, L.N. Leaving no one behind: Defining and implementing an integrated life course approach to vaccination across the next decade as part of the immunization Agenda 2030. Vaccine, 2022; in press. [Google Scholar] [CrossRef] [PubMed]
- Favin, M.; Steinglass, R.; Fields, R.; Banerjee, K.; Sawhney, M. Why children are not vaccinated: A review of the grey literature. Int. Health 2012, 4, 229–238. [Google Scholar] [CrossRef] [PubMed]
- Périères, L.; Séror, V.; Boyer, S.; Sokhna, C.; Peretti-Watel, P. Reasons given for non-vaccination and under-vaccination of children and adolescents in sub-Saharan Africa: A systematic review. Hum. Vaccines Immunother. 2022, 18, 2076524. [Google Scholar] [CrossRef] [PubMed]
- Feikin, D.R.; Flannery, B.; Hamel, M.J.; Stack, M.; Hansen, P.M. Vaccines for children in low-and middle-income countries. In Reproductive, Maternal, Newborn, and Child Health: Disease Control Priorities; The World Bank: Washington, DC, USA, 2006; Volume 2, pp. 187–205. [Google Scholar]
- Wariri, O.; Edem, B.; Nkereuwem, E.; Nkereuwem, O.O.; Umeh, G.; Clark, E.; Idoko, O.T.; Nomhwange, T.; Kampmann, B. Tracking coverage, dropout and multidimensional equity gaps in immunisation systems in West Africa, 2000–2017. BMJ Glob. Health 2019, 4, e001713. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Routine Immunization Strategies and Practices (GRISP): A Companion Document to the Global Vaccine Action Plan (GVAP); WHO: Geneva, Switzerland, 2016. [Google Scholar]
- Ateudjieu, J.; Yakum, M.N.; Goura, A.P.; Tembei, A.M.; Ingrid, D.K.; Bita’a Landry, B.; Kenfack, B.; Amada, L.; Tadzong, I.; Bissek, A.C. EPI immunization coverage, timeliness and dropout rate among children in a West Cameroon health district: A cross-sectional study. BMC Public Health 2020, 20, 228. [Google Scholar] [CrossRef]
- Chanie, M.G.; Ewunetie, G.E.; Molla, A.; Muche, A. Determinants of vaccination dropout among children 12–23 months age in north Gondar zone, northwest Ethiopia, 2019. PLoS ONE 2021, 16, e0246018. [Google Scholar] [CrossRef]
- Mane, A.B. Letter to Editor: Immunization Dropout Rates: Some Issues. Ann. Med. Health Sci. Res. 2015, 5, 153. [Google Scholar]
- Baguune, B.; Ndago, J.A.; Adokiya, M.N. Immunization dropout rate and data quality among children 12–23 months of age in Ghana. Arch. Public Health 2017, 75, 18. [Google Scholar] [CrossRef]
- Feldstein, L.R.; Mariat, S.; Gacic-Dobo, M.; Diallo, M.S.; Conklin, L.M.; Wallace, A.S. Global routine vaccination coverage, 2016. Morb. Mortal. Wkly. Rep. 2017, 66, 1252. [Google Scholar] [CrossRef]
- Mmanga, K.; Mwenyenkulu, T.E.; Nkoka, O.; Ntenda, P.A. Tracking immunization coverage, dropout and equity gaps among children ages 12–23 months in Malawi–bottleneck analysis of the Malawi Demographic and Health Survey. Int. Health 2022, 14, 250–259. [Google Scholar] [CrossRef] [PubMed]
- Atnafu, N.; Asmare Adela, G.; Dagnaw Tegegne, K.; Birhan Assfaw, B. Vaccination dropout among children in Sub-Saharan Africa: Systematic review and meta-analysis. Hum. Vaccin. Immunother. 2022, 18, 2145821. [Google Scholar]
- Zewdie, A.; Letebo, M.; Mekonnen, T. Reasons for defaulting from childhood immunization program: A qualitative study from Hadiya zone, Southern Ethiopia. BMC Public Health 2016, 16, 1240. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Sahu, D.; Agrawal, A.; Vashi, M.D. Evaluation of vaccination coverage and dropout rates among children aged 12–23 months in the slums of Mumbai, India: Preliminary analysis of a cross sectional study. Int. J. Manag. Soc. Sci. 2017, 5, 112–123. [Google Scholar]
- Imran, W.; Abbas, F.; Javed, S.A. What is causing high polio vaccine dropout among Pakistani children? Public Health 2018, 164, 16–25. [Google Scholar] [CrossRef]
- Francis, M.R.; Nuorti, J.P.; Kompithra, R.Z.; Larson, H.; Balraj, V.; Kang, G.; Mohan, V.R. Vaccination coverage and factors associated with routine childhood vaccination uptake in rural Vellore, southern India, 2017. Vaccine 2019, 37, 3078–3087. [Google Scholar] [CrossRef]
- International Institute for Population Sciences (IIPS) and ICF. National Family Health Survey (NFHS-5), 2019–2021; IIPS: Mumbai, India, 2021; Volume I. [Google Scholar]
- Wahl, B.; Gupta, M.; Erchick, D.J.; Patenaude, B.N.; Holroyd, T.A.; Sauer, M.; Blunt, M.; Santosham, M.; Limaye, R.J. Change in full immunization inequalities in Indian children 12–23 months: An analysis of household survey data. BMC Public Health 2021, 21, 841. [Google Scholar] [CrossRef]
- Utazi, C.E.; Pannell, O.; Aheto, J.M.; Wigley, A.; Tejedor-Garavito, N.; Wunderlich, J.; Hagedorn, B.; Hogan, D.; Tatem, A.J. Assessing the characteristics of un-and under-vaccinated children in low-and middle-income countries: A multi-level cross-sectional study. PLOS Glob. Public Health 2022, 2, e0000244. [Google Scholar] [CrossRef]
- Thapa, K.; Adhikary, P.; Faruquee, M.H.; Suwal, B.R. Associated Factors for Dropout of First Vs Third Doses of Diphtheria Tetanus Pertussis (DPT) Vaccination in Nepal. Adv. Prev. Med. 2021, 2021, 1319090. [Google Scholar] [CrossRef]
- Madhavi, N.; Manikyamba, D. Evaluation of immunization status and factors responsible for drop outs in primary immunization in children between 1–2 years–A hospital based study. Pediatr. Rev. Int. J. Pediatr. Res. 2016, 3, 332. [Google Scholar] [CrossRef]
- Ntenda, P.A.; Sixpence, A.; Mwenyenkulu, T.E.; Mmanga, K.; Chirambo, A.C.; Bauleni, A.; Nkoka, O. Determinants of pentavalent and measles vaccination dropouts among children aged 12–23 months in The Gambia. BMC Public Health 2022, 22, 520. [Google Scholar] [CrossRef]
- Hong, R.; Chhea, V. Trend and inequality in immunization dropout among young children in Cambodia. Matern. Child Health J. 2010, 14, 446–452. [Google Scholar] [CrossRef]
- International Institute for Population Sciences (IIPS) and ICF. National Family Health Survey (NFHS-4), 2015–2016; IIPS: Mumbai, India, 2017. [Google Scholar]
- Ghosh, A.; Laxminarayan, R. Demand-and supply-side determinants of diphtheria-pertussis-tetanus nonvaccination and dropout in rural India. Vaccine 2017, 35, 1087–1093. [Google Scholar] [CrossRef] [PubMed]
- Kayembe-Ntumba, H.C.; Vangola, F.; Ansobi, P.; Kapour, G.; Bokabo, E.; Mandja, B.A.; Bompangue, D. Vaccination dropout rates among children aged 12–23 months in Democratic Republic of the Congo: A cross-sectional study. Arch. Public Health 2022, 80, 18. [Google Scholar] [CrossRef] [PubMed]
- Awasthi, A.; Pandey, C.M.; Singh, U.; Kumar, S.; Singh, T.B. Maternal determinants of immunization status of children aged 12–23 months in urban slums of Varanasi, India. Clin. Epidemiol. Glob. Health 2015, 3, 110–116. [Google Scholar] [CrossRef]
- Datta, A.; Mog, C.; Das, S.; Datta, S. A cross-sectional study to assess the immunization coverage and vaccine dropout rates among 12 to 23 months old children in a rural area of Tripura. Int. J. 2017, 6, 394. [Google Scholar] [CrossRef]
- Haji, A.; Lowther, S.; Ngan’Ga, Z.; Gura, Z.; Tabu, C.; Sandhu, H.; Arvelo, W. Reducing routine vaccination dropout rates: Evaluating two interventions in three Kenyan districts, 2014. BMC Public Health 2016, 16, 152. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, S.; Thampi, V.; Deshmukh, D.; Gadhari, M.; Chandrasekar, R.; Phadke, M. Trends in Urban Immunization Coverage in India: A Meta-Analysis and Meta-Regression. Indian J. Pediatr. 2021, 90, 38–48. [Google Scholar] [CrossRef]
- Ekouevi, D.K.; Gbeasor-Komlanvi, F.A.; Yaya, I.; Zida-Compaore, W.I.; Boko, A.; Sewu, E.; Lacle, A.; Ndibu, N.; Toke, Y.; Landoh, D.E. Incomplete immunization among children aged 12–23 months in Togo: A multilevel analysis of individual and contextual factors. BMC Public Health 2018, 18, 952. [Google Scholar] [CrossRef] [PubMed]
- Ntenda, P.A.M.; Chuang, K.Y.; Tiruneh, F.N.; Chuang, Y.C. Analysis of the effects of individual and community level factors on childhood immunization in Malawi. Vaccine 2017, 35, 1907–1917. [Google Scholar] [CrossRef] [PubMed]









| Schedule | Vaccinations |
|---|---|
| At birth | Bacillus Calmette Guerin (BCG), Hepatitis B-Birth Dose, Oral Polio vaccine (OPV)-0 |
| At 6 weeks | OPV-1, DPT/Pentavalent-1, Rotavirus vaccine (RVV)-1 |
| At 10 weeks | OPV-2, DPT/Pentavalent-2, RVV-2 |
| At 14 weeks | OPV-3, DPT/Pentavalent-3, RVV-3 |
| At 9 months | Measles/MR1 |
| NFHS-4 | NFHS-5 | |||
|---|---|---|---|---|
| % | N | % | N | |
| Mother’s Age | ||||
| 15–19 years | 3.9 | 1718 | 3.6 | 1353 |
| 20–29 years | 75.6 | 35,822 | 75.3 | 31,899 |
| 30 and above years | 20.5 | 11,388 | 21.2 | 10,184 |
| Place of residence | ||||
| Urban | 28.4 | 11,700 | 26.9 | 8879 |
| Rural | 71.6 | 37,228 | 73.1 | 34,557 |
| Mother’s Education Level | ||||
| No education | 27.6 | 13,974 | 19.0 | 8475 |
| Primary education | 13.9 | 6985 | 11.3 | 5171 |
| Secondary education | 46.9 | 22,876 | 52.5 | 23,209 |
| Higher education | 11.6 | 5093 | 17.2 | 6581 |
| Religion | ||||
| Hindu | 78.3 | 35,172 | 79.6 | 32,212 |
| Muslim | 16.9 | 7822 | 16.1 | 6106 |
| Others | 4.8 | 5934 | 4.3 | 5118 |
| Wealth Index | ||||
| Poorest | 24.6 | 12,497 | 23.9 | 11,386 |
| Poorer | 21.6 | 11,306 | 21.4 | 10,073 |
| Middle | 20.2 | 9946 | 19.9 | 8518 |
| Richer | 18.7 | 8366 | 18.8 | 7446 |
| Richest | 14.9 | 6813 | 16.1 | 6013 |
| Birth Order | ||||
| First | 38.0 | 18,045 | 39.7 | 16,941 |
| Second | 33.2 | 15,558 | 34.3 | 14,463 |
| Third | 15.3 | 7793 | 14.9 | 6654 |
| Fourth and above | 13.5 | 7532 | 11.1 | 5378 |
| Sex of the Child | ||||
| Male | 51.9 | 25,431 | 52.0 | 22,537 |
| Female | 48.1 | 23,497 | 48.0 | 20,899 |
| Antenatal visits | ||||
| No visits | 16.3 | 7980 | 5.9 | 2559 |
| 1–3 visits | 32.2 | 16,259 | 34.7 | 14,371 |
| 4 and above visits | 51.5 | 21,970 | 59.4 | 23,887 |
| Place of delivery | ||||
| Home | 17.8 | 10,384 | 9.3 | 4937 |
| Public health facilities | 54.6 | 27,821 | 63.2 | 28,623 |
| Private health facilities | 27.5 | 10,604 | 27.6 | 9786 |
| Place of vaccination | ||||
| Public health facilities | 92.7 | 42,423 | 85.6 | 11,869 |
| Private health facilities | 7.3 | 2354 | 14.4 | 1175 |
| NFHS-4 | NFHS-5 | NFHS-4 | NFHS-5 | NFHS-4 | NFHS-5 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| DO BCG-MCV1 | DO BCG-MCV1 | DO OPV1-OPV3 | DO OPV1-OPV3 | DO DPT1-DPT3 | DO DPT1-DPT3 | |||||||
| % | N | % | N | % | N | % | N | % | N | % | N | |
| Mother’s Age | ||||||||||||
| 15–19 years | 13.4 | 248 | 9.5 | 141 | 19.3 | 350 | 15.9 | 193 | 12.9 | 233 | 8.0 | 125 |
| 20–29 years | 12.4 | 4418 | 8.5 | 2553 | 19.4 | 6453 | 12.8 | 3604 | 12.0 | 4152 | 7.1 | 2129 |
| 30 and above years | 14.3 | 1502 | 9.1 | 842 | 20.9 | 2063 | 12.9 | 1142 | 13.7 | 1347 | 8.1 | 684 |
| Place of Residence | ||||||||||||
| Urban | 11.5 | 1370 | 8.8 | 724 | 20.0 | 2008 | 13.7 | 1043 | 11.2 | 1269 | 7.1 | 558 |
| Rural | 13.3 | 4798 | 8.5 | 2812 | 19.5 | 6858 | 12.6 | 3896 | 12.9 | 4463 | 7.5 | 2380 |
| Mother’s Education Level | ||||||||||||
| No education | 18.4 | 2286 | 13.3 | 1002 | 24.3 | 2992 | 17.3 | 1232 | 17.5 | 2084 | 10.3 | 779 |
| Primary education | 14.2 | 1000 | 9.7 | 494 | 21.0 | 1346 | 13.6 | 645 | 13.2 | 885 | 8.7 | 408 |
| Secondary education | 10.7 | 2495 | 7.5 | 1694 | 17.5 | 3777 | 11.5 | 2430 | 10.6 | 2364 | 6.5 | 1435 |
| Higher education | 7.2 | 387 | 6.5 | 346 | 16.5 | 751 | 12.1 | 632 | 8.0 | 399 | 6.3 | 316 |
| Religion | ||||||||||||
| Hindu | 12.0 | 4103 | 7.9 | 2271 | 19.5 | 6363 | 12.5 | 3467 | 12.0 | 4023 | 7.0 | 1989 |
| Muslim | 17.1 | 1242 | 12.7 | 719 | 21.8 | 1490 | 15.3 | 814 | 15.2 | 1045 | 9.6 | 543 |
| Others | 11.4 | 823 | 7.0 | 546 | 14.9 | 1013 | 10.9 | 658 | 9.7 | 664 | 5.9 | 406 |
| Wealth Index | ||||||||||||
| Poorest | 17.1 | 1969 | 11.5 | 1237 | 23.4 | 2708 | 16.1 | 1607 | 16.7 | 1822 | 9.4 | 1024 |
| Poorer | 14.5 | 1628 | 9.1 | 887 | 20.4 | 2226 | 13.0 | 1160 | 13.3 | 1469 | 8.1 | 739 |
| Middle | 12.1 | 1160 | 7.2 | 582 | 18.9 | 1656 | 11.3 | 874 | 11.7 | 1062 | 5.9 | 475 |
| Richer | 10.5 | 866 | 7.7 | 488 | 17.8 | 1311 | 11.6 | 710 | 10.2 | 853 | 7.3 | 419 |
| Richest | 7.6 | 545 | 6.6 | 342 | 16.3 | 965 | 11.7 | 588 | 8.3 | 526 | 5.6 | 281 |
| Birth Order | ||||||||||||
| First | 10.5 | 1936 | 6.8 | 1121 | 17.2 | 2990 | 11.6 | 1719 | 10.2 | 1833 | 5.8 | 938 |
| Second | 11.9 | 1857 | 8.4 | 1114 | 19.0 | 2770 | 12.6 | 1599 | 11.5 | 1753 | 7.5 | 961 |
| Third | 15.5 | 1134 | 10.5 | 641 | 23.4 | 1553 | 14.9 | 847 | 15.0 | 1033 | 8.6 | 523 |
| Fourth and above | 18.9 | 1241 | 13.7 | 660 | 24.6 | 1553 | 16.4 | 774 | 18.5 | 1113 | 11.0 | 516 |
| Sex of the Child | ||||||||||||
| Male | 12.2 | 3129 | 8.5 | 1795 | 20.3 | 4690 | 12.8 | 2503 | 12.7 | 3018 | 7.3 | 1503 |
| Female | 13.4 | 3039 | 8.8 | 1741 | 18.9 | 4176 | 13.1 | 2436 | 12.1 | 2714 | 7.5 | 1435 |
| Antenatal visits | ||||||||||||
| No visits | 21.4 | 1444 | 14.5 | 360 | 26.3 | 1768 | 18.8 | 421 | 20.7 | 1323 | 11.5 | 270 |
| 1–3 visits | 14.8 | 2325 | 10.9 | 1399 | 22.0 | 3297 | 15.7 | 1920 | 14.5 | 2189 | 9.3 | 1203 |
| 4 or above visits | 9.2 | 2066 | 6.8 | 1556 | 16.2 | 3278 | 10.6 | 2280 | 8.8 | 1890 | 6.0 | 1292 |
| Place of delivery | ||||||||||||
| Home | 18.6 | 1703 | 13.8 | 662 | 24.0 | 2205 | 18.9 | 821 | 19.1 | 1630 | 12.2 | 548 |
| Public health facilities | 12.4 | 3360 | 8.3 | 2192 | 18.7 | 4844 | 12.0 | 2998 | 11.5 | 2988 | 7.0 | 1821 |
| Private health facilities | 10.2 | 1084 | 7.8 | 676 | 19.0 | 1792 | 13.1 | 1111 | 10.5 | 1091 | 6.9 | 564 |
| Place of vaccination | ||||||||||||
| Public health facilities | 12.6 | 5632 | 9.9 | 1151 | 19.4 | 8181 | 12.9 | 1409 | 12.2 | 5247 | 7.2 | 819 |
| Private health facilities | 12.0 | 319 | 13.8 | 151 | 23.6 | 492 | 20.0 | 213 | 12.0 | 289 | 10.5 | 92 |
| NFHS-4 | NFHS-5 | NFHS-4 | NFHS-5 | NFHS-4 | NFHS-5 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| DO BCG-MCV1 | DO BCG-MCV1 | DO OPV1-OPV3 | DO OPV1-OPV3 | DO DPT1-DPT3 | DO DPT1-DPT3 | |||||||
| Odds Ratio | 95% CI | Odds Ratio | 95% CI | Odds Ratio | 95% CI | Odds Ratio | 95% CI | Odds Ratio | 95% CI | Odds Ratio | 95% CI | |
| Mother’s Age | ||||||||||||
| 15–19 years® | ||||||||||||
| 20–29 years | 0.81 *** | (0.69–0.94) | 0.56 *** | (0.4–0.78) | 0.85 ** | (0.74–0.97) | 0.70** | (0.5–0.97) | 0.79 *** | (0.66–0.91) | 0.53 *** | (0.36–0.77) |
| 30 and above years | 0.73 *** | (0.61–0.86) | 0.42 *** | (0.29–0.61) | 0.80 *** | (0.69–0.92) | 0.56 *** | (0.39–0.79) | 0.70 *** | (0.58–0.83) | 0.41 *** | (0.27–0.62) |
| Place of Residence | ||||||||||||
| Urban® | ||||||||||||
| Rural | 0.81 *** | (0.75–0.88) | 0.74 *** | (0.64–0.86) | 0.87 *** | (0.82–0.93) | 0.78 *** | (0.68–0.89) | 0.83 *** | (0.76–0.9) | 0.85 * | (0.72–1.02) |
| Mother’s Education Level | ||||||||||||
| No education® | ||||||||||||
| Primary education | 0.92 * | (0.84–1.01) | 0.85 | (0.68–1.06) | 0.92 ** | (0.85–0.99) | 0.87 | (0.7–1.09) | 0.88 *** | (0.8–0.97) | 0.95 | (0.72–1.24) |
| Secondary education | 0.77 *** | (0.72–0.84) | 0.69 *** | (0.58–0.82) | 0.83 *** | (0.78–0.89) | 0.82 ** | (0.69–0.97) | 0.79 *** | (0.73–0.86) | 0.85 | (0.69–1.06) |
| Higher education | 0.63 *** | (0.54–0.72) | 0.56 *** | (0.44–0.72) | 0.82 *** | (0.73–0.92) | 0.74 *** | (0.59–0.92) | 0.70 *** | (0.6–0.8) | 0.77 * | (0.57–1.03) |
| Religion | ||||||||||||
| Hindu® | ||||||||||||
| Muslim | 1.53 *** | (1.42–1.65) | 1.45 *** | (1.23–1.71) | 1.13 *** | (1.05–1.21) | 1.13 | (0.96–1.32) | 1.27 *** | (1.17–1.38) | 1.39 *** | (1.14–1.68) |
| Others | 1.49 *** | (1.36–1.62) | 1.25 *** | (1.07–1.46) | 1.03 | (0.95–1.12) | 1.19 ** | (1.03–1.37) | 1.16 *** | (1.05–1.28) | 1.16 | (0.97–1.39) |
| Wealth Index | ||||||||||||
| Poorest® | ||||||||||||
| Poorer | 1.01 | (0.93–1.09) | 0.78 *** | (0.65–0.93) | 0.96 | (0.9–1.03) | 0.86 | (0.72–1.04) | 0.97 | (0.89–1.05) | 0.83 * | (0.67–1.03) |
| Middle | 0.88 *** | (0.8–0.96) | 0.59 *** | (0.48–0.72) | 0.81 *** | (0.75–0.88) | 0.72 *** | (0.59–0.87) | 0.86 *** | (0.78–0.94) | 0.63 *** | (0.5–0.8) |
| Richer | 0.78 *** | (0.7–0.87) | 0.55 *** | (0.44–0.69) | 0.76 *** | (0.7–0.84) | 0.62 *** | (0.5–0.77) | 0.84 *** | (0.75–0.93) | 0.59 *** | (0.46–0.77) |
| Richest | 0.61 *** | (0.53–0.69) | 0.44 *** | (0.34–0.57) | 0.65 *** | (0.58–0.73) | 0.69 *** | (0.55–0.87) | 0.60 *** | (0.52–0.69) | 0.55 *** | (0.41–0.74) |
| Birth Order | ||||||||||||
| First® | ||||||||||||
| Second | 1.06 | (0.98–1.14) | 1.16 ** | (1–1.35) | 1.05 | (0.99–1.12) | 1.11 | (0.97–1.26) | 1.07 | (0.99–1.15) | 1.15 | (0.96–1.37) |
| Third | 1.22 *** | (1.12–1.34) | 1.50 *** | (1.23–1.82) | 1.13 *** | (1.05–1.22) | 1.37 *** | (1.14–1.64) | 1.16 *** | (1.06–1.27) | 1.40 *** | (1.11–1.75) |
| Fourth and above | 1.26 *** | (1.14–1.39) | 1.88 *** | (1.51–2.36) | 1.14 *** | (1.04–1.24) | 1.48 *** | (1.19–1.84) | 1.24 *** | (1.11–1.38) | 1.73 *** | (1.33–2.26) |
| Sex of the Child | ||||||||||||
| Male® | ||||||||||||
| Female | 1.04 | (0.98–1.1) | 0.95 | (0.84–1.07) | 0.94 *** | (0.89–0.99) | 1.02 | (0.91–1.14) | 0.94 ** | (0.89–1) | 1.02 | (0.88–1.17) |
| Antenatal visits | ||||||||||||
| No visits® | ||||||||||||
| 1–3 visits | 0.67 *** | (0.62–0.73) | 0.89 | (0.71–1.12) | 0.80 *** | (0.74–0.86) | 0.95 | (0.76–1.19) | 0.69 *** | (0.63–0.74) | 0.91 | (0.69–1.19) |
| 4 or above visits | 0.47 *** | (0.43–0.51) | 0.55 *** | (0.44–0.69) | 0.57 *** | (0.53–0.62) | 0.62 *** | (0.5–0.77) | 0.45 *** | (0.41–0.49) | 0.60 *** | (0.46–0.78) |
| Place of delivery | ||||||||||||
| Home® | ||||||||||||
| Public health facilities | 0.81 *** | (0.75–0.87) | 0.81 ** | (0.66–1) | 0.83 *** | (0.78–0.89) | 0.72 *** | (0.59–0.88) | 0.70 *** | (0.65–0.75) | 0.66 *** | (0.52–0.83) |
| Private health facilities | 0.78 *** | (0.71–0.87) | 0.8 | (0.62–1.04) | 0.89 *** | (0.82–0.97) | 0.81 * | (0.64–1.02) | 0.78 *** | (0.71–0.87) | 0.71 ** | (0.53–0.95) |
| Place of vaccination | ||||||||||||
| Public health facilities® | ||||||||||||
| Private health facilities | 1.69 *** | (1.46–1.95) | 2.24 *** | (1.78–2.81) | 1.53 *** | (1.36–1.73) | 2.05 *** | (1.69–2.49) | 1.58 *** | (1.36–1.83) | 1.64 *** | (1.25–2.15) |
| DO BCG-MCV1 | DO OPV1-OPV3 | DO DPT1-DPT3 | ||||
|---|---|---|---|---|---|---|
| Covariates | Coeff. | SE | Coeff. | SE | Coeff. | SE |
| Mother’s Age | 0.0006 | 0.0001 | 0.0008 | 0.0002 | 0.0006 | 0.0001 |
| Place of Residence | −0.0031 | 0.0006 | −0.0027 | 0.0007 | −0.0028 | 0.0006 |
| Mother’s Education Level | 0.0081 | 0.0009 | 0.0068 | 0.0012 | 0.0068 | 0.0010 |
| Religion | −0.0089 | 0.0008 | −0.0014 | 0.0006 | −0.0036 | 0.0007 |
| Wealth Index | 0.0056 | 0.0008 | 0.0069 | 0.0009 | 0.0043 | 0.0008 |
| Birth Order | 0.0022 | 0.0004 | 0.0016 | 0.0004 | 0.0016 | 0.0004 |
| Sex of the Child | 0.0000 | 0.0000 | 0.0000 | 0.0000 | 0.0000 | 0.0000 |
| Antenatal Visits | 0.0142 | 0.0008 | 0.0134 | 0.0008 | 0.0137 | 0.0008 |
| Place of Delivery | 0.0024 | 0.0005 | 0.0015 | 0.0005 | 0.0025 | 0.0005 |
| Place of Vaccination | −0.001 | 0.0002 | −0.0019 | 0.0002 | −0.001 | 0.0002 |
| Mean prediction in NFHS-4 | 0.137 | 0.200 | 0.129 | |||
| Mean prediction in NFHS-5 | 0.101 | 0.132 | 0.073 | |||
| Total Gap | 0.036 | 0.069 | 0.057 | |||
| Explained Gap | 0.020 | 0.025 | 0.022 | |||
| Explained Gap (%) | 55.9 | 36.5 | 39.2 | |||
| Sample size | 53,187 | 52,272 | 51,897 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dhalaria, P.; Kapur, S.; Singh, A.K.; Priyadarshini, P.; Dutta, M.; Arora, H.; Taneja, G. Exploring the Pattern of Immunization Dropout among Children in India: A District-Level Comparative Analysis. Vaccines 2023, 11, 836. https://doi.org/10.3390/vaccines11040836
Dhalaria P, Kapur S, Singh AK, Priyadarshini P, Dutta M, Arora H, Taneja G. Exploring the Pattern of Immunization Dropout among Children in India: A District-Level Comparative Analysis. Vaccines. 2023; 11(4):836. https://doi.org/10.3390/vaccines11040836
Chicago/Turabian StyleDhalaria, Pritu, Sanjay Kapur, Ajeet Kumar Singh, Pretty Priyadarshini, Mili Dutta, Himanshu Arora, and Gunjan Taneja. 2023. "Exploring the Pattern of Immunization Dropout among Children in India: A District-Level Comparative Analysis" Vaccines 11, no. 4: 836. https://doi.org/10.3390/vaccines11040836






