Sitafloxacin for Third-Line Helicobacter pylori Eradication: A Systematic Review
Abstract
1. Introduction
2. Methods
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Data Extraction
2.4. Assessment of Methodological Quality
2.5. Statistical Analysis
3. Results
3.1. Search Results
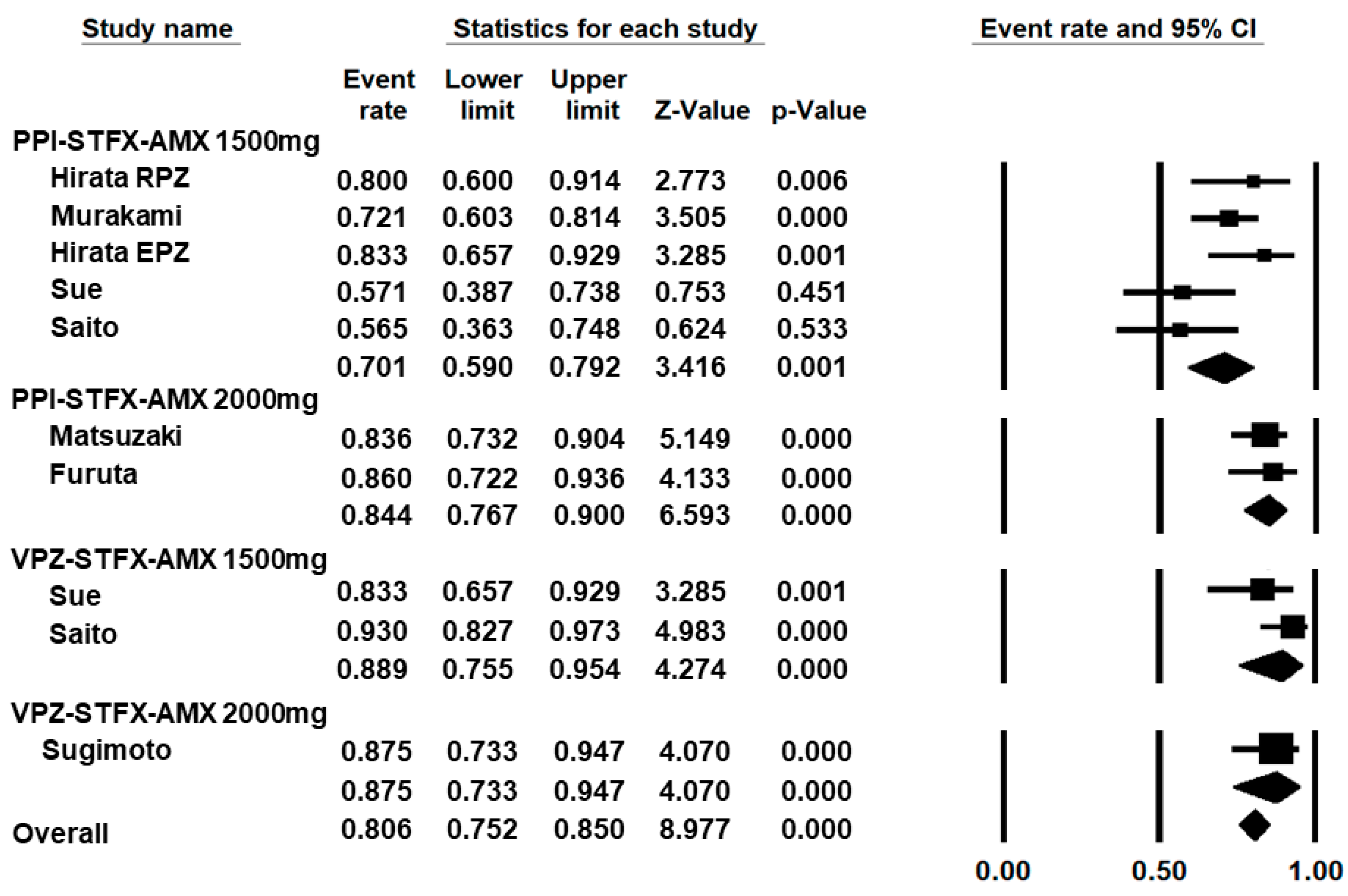
3.2. Efficacy of PPI–Sitafloxacin–Amoxicillin
3.3. Efficacy of PPI–Sitafloxacin–Metronidazole
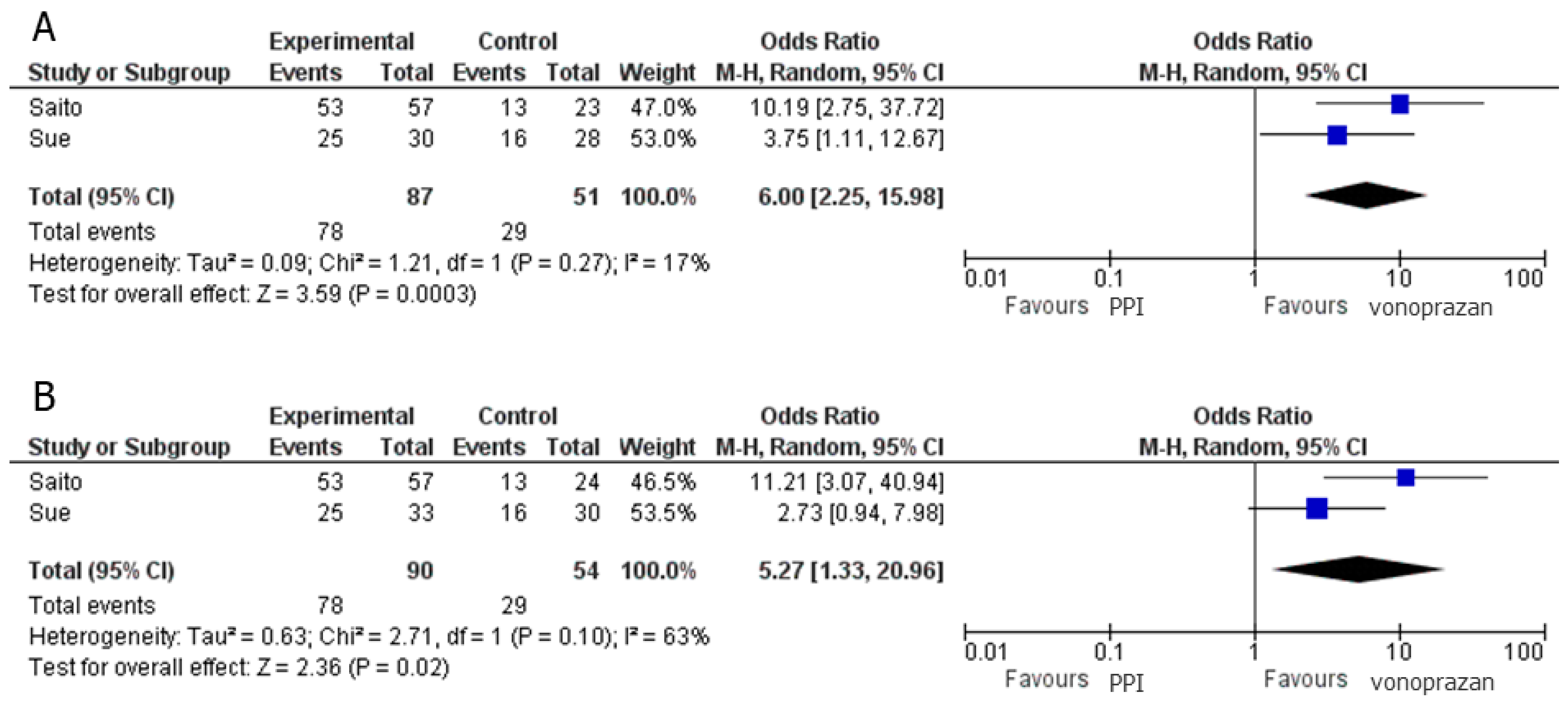
3.4. PPI–Amoxicillin–Sitafloxacin versus PPI–Metronidazole–Sitafloxacin
3.5. Adverse Events
3.6. Quality Assessment
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Suzuki, H.; Mori, H. World trends for H. pylori eradication therapy and gastric cancer prevention strategy by H. pylori test-and-treat. J. Gastroenterol. 2018, 53, 354–361. [Google Scholar] [CrossRef]
- Suzuki, H.; Nishizawa, T.; Tsugawa, H.; Hibi, T. Molecular approaches and modern clinical strategies for the management of Helicobacter pylori infection in Japan. Keio J. Med. 2012, 61, 109–119. [Google Scholar] [CrossRef]
- Watanabe, T.; Nadatani, Y.; Suda, W.; Higashimori, A.; Otani, K.; Fukunaga, S.; Hosomi, S.; Tanaka, F.; Nagami, Y.; Taira, K.; et al. Long-term persistence of gastric dysbiosis after eradication of Helicobacter pylori in patients who underwent endoscopic submucosal dissection for early gastric cancer. Gastric Cancer 2021, 24, 710–720. [Google Scholar] [CrossRef] [PubMed]
- Ford, A.C.; Yuan, Y.; Moayyedi, P. Helicobacter pylori eradication therapy to prevent gastric cancer: Systematic review and meta-analysis. Gut 2020, 69, 2113–2121. [Google Scholar] [CrossRef]
- Suzuki, H.; Nishizawa, T.; Hibi, T. Helicobacter pylori eradication therapy. Future Microbiol. 2010, 5, 639–648. [Google Scholar] [CrossRef]
- Farzi, N.; Yadegar, A.; Sadeghi, A.; Asadzadeh Aghdaei, H.; Marian Smith, S.; Raymond, J.; Suzuki, H.; Zali, M.R. High prevalence of antibiotic resistance in iranian Helicobacter pylori isolates: Importance of functional and mutational analysis of resistance genes and virulence genotyping. J. Clin. Med. 2019, 8, 2004. [Google Scholar] [CrossRef]
- Murata, M.; Sugimoto, M.; Mizuno, H.; Kanno, T.; Satoh, K. Clarithromycin versus metronidazole in first-line Helicobacter pylori triple eradication therapy based on resistance to antimicrobial agents: Meta-analysis. J. Clin. Med. 2020, 9, 543. [Google Scholar] [CrossRef] [PubMed]
- Olmedo, L.; Azagra, R.; Aguye, A.; Pascual, M.; Calvet, X.; Gene, E. High effectiveness of a 14-day concomitant therapy for Helicobacter pylori treatment in primary care. An observational multicenter study. J. Clin. Med. 2020, 9, 2410. [Google Scholar] [CrossRef] [PubMed]
- Sugimoto, M.; Sahara, S.; Ichikawa, H.; Kagami, T.; Ban, H.; Otsuka, T.; Andoh, A.; Furuta, T. Four-times-daily dosing of rabeprazole with sitafloxacin, high-dose amoxicillin, or both for metronidazole-resistant infection with Helicobacter pylori in Japan. Helicobacter 2017, 22, e12319. [Google Scholar] [CrossRef]
- Nishizawa, T.; Suzuki, H.; Hibi, T. Quinolone-based third-line therapy for Helicobacter pylori eradication. J. Clin. Biochem. Nutr. 2009, 44, 119–124. [Google Scholar] [CrossRef]
- Mori, H.; Suzuki, H. Update on quinolone-containing rescue therapies for Helicobacter pylori infection. World J. Gastroenterol. 2020, 26, 1733–1744. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, T.; Suzuki, H.; Nakagawa, I.; Iwasaki, E.; Masaoka, T.; Hibi, T. Gatifloxacin-based triple therapy as a third-line regimen for Helicobacter pylori eradication. J. Gastroenterol. Hepatol. 2008, 23, S167–S170. [Google Scholar] [CrossRef] [PubMed]
- Mori, H.; Suzuki, H.; Matsuzaki, J.; Tsugawa, H.; Fukuhara, S.; Miyoshi, S.; Hirata, K.; Seino, T.; Matsushita, M.; Nishizawa, T. Rifabutin-based 10-day and 14-day triple therapy as a third-line and fourth-line regimen for Helicobacter pylori eradication: A pilot study. United Eur. Gastroenterol. J. 2016, 4, 380–387. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, H.; Nishizawa, T.; Muraoka, H.; Hibi, T. Sitafloxacin and garenoxacin may overcome the antibiotic resistance of Helicobacter pylori with gyrA mutation. Antimicrob. Agents Chemother. 2009, 53, 1720–1721. [Google Scholar] [CrossRef]
- Matsuzaki, J.; Suzuki, H.; Tsugawa, H.; Nishizawa, T.; Hibi, T. Homology model of the DNA gyrase enzyme of Helicobacter pylori, a target of quinolone-based eradication therapy. J. Gastroenterol. Hepatol. 2010, 25, S7–S10. [Google Scholar] [CrossRef]
- Murakami, K.; Furuta, T.; Ando, T.; Nakajima, T.; Inui, Y.; Oshima, T.; Tomita, T.; Mabe, K.; Sasaki, M.; Suganuma, T.; et al. Multi-center randomized controlled study to establish the standard third-line regimen for Helicobacter pylori eradication in Japan. J. Gastroenterol. 2013, 48, 1128–1135. [Google Scholar] [CrossRef] [PubMed]
- Kato, M.; Ota, H.; Okuda, M.; Kikuchi, S.; Satoh, K.; Shimoyama, T.; Suzuki, H.; Handa, O.; Furuta, T.; Mabe, K.; et al. Guidelines for the management of Helicobacter pylori infection in Japan: 2016 revised edition. Helicobacter 2019, 24, e12597. [Google Scholar] [CrossRef]
- Hirata, Y.; Ohmae, T.; Yanai, A.; Sakitani, K.; Hayakawa, Y.; Yoshida, S.; Sugimoto, T.; Mitsuno, Y.; Akanuma, M.; Yamaji, Y.; et al. Sitafloxacin resistance in Helicobacter pylori isolates and sitafloxacin-based triple therapy as a third-line regimen in Japan. Int. J. Antimicrob. Agents 2012, 39, 352–355. [Google Scholar] [CrossRef]
- Hirata, Y.; Serizawa, T.; Shichijo, S.; Suzuki, N.; Sakitani, K.; Hayakawa, Y.; Yamada, A.; Koike, K. Efficacy of triple therapy with esomeprazole, amoxicillin, and sitafloxacin as a third-line Helicobacter pylori eradication regimen. Int. J. Infect. Dis. 2016, 51, 66–69. [Google Scholar] [CrossRef]
- Sue, S.; Shibata, W.; Sasaki, T.; Kaneko, H.; Irie, K.; Kondo, M.; Maeda, S. Randomized trial of vonoprazan-based versus proton-pump inhibitor-based third-line triple therapy with sitafloxacin for Helicobacter pylori. J. Gastroenterol. Hepatol. 2019, 34, 686–692. [Google Scholar] [CrossRef]
- Matsuzaki, J.; Suzuki, H.; Nishizawa, T.; Hirata, K.; Tsugawa, H.; Saito, Y.; Okada, S.; Fukuhara, S.; Hibi, T. Efficacy of Sitafloxacin-based rescue therapy for Helicobacter pylori after failures of first- and second-line therapies. Antimicrob. Agents Chemother. 2011, 56, 1643–1645. [Google Scholar] [CrossRef]
- Saito, Y.; Konno, K.; Sato, M.; Nakano, M.; Kato, Y.; Saito, H.; Serizawa, H. Vonoprazan-based third-line therapy has a higher eradication rate against sitafloxacin-resistant Helicobacter pylori. Cancers 2019, 11, 116. [Google Scholar] [CrossRef]
- Furuta, T.; Sugimoto, M.; Kodaira, C.; Nishino, M.; Yamade, M.; Uotani, T.; Sahara, S.; Ichikawa, H.; Yamada, T.; Osawa, S.; et al. Sitafloxacin-based third-line rescue regimens for Helicobacter pylori infection in Japan. J. Gastroenterol. Hepatol. 2014, 29, 487–493. [Google Scholar] [CrossRef] [PubMed]
- Mori, H.; Suzuki, H.; Matsuzaki, J.; Tsugawa, H.; Fukuhara, S.; Miyoshi, S.; Hirata, K.; Seino, T.; Matsushita, M.; Masaoka, T.; et al. Efficacy of 10-day Sitafloxacin-containing third-line rescue therapies for Helicobacter pylori strains containing the gyrA mutation. Helicobacter 2016, 21, 286–294. [Google Scholar] [CrossRef]
- Mori, H.; Suzuki, H.; Matsuzaki, J.; Masaoka, T.; Kanai, T. 10-Year trends in Helicobacter pylori eradication rates by Sitafloxacin-based third-line rescue therapy. Digestion 2020, 101, 644–650. [Google Scholar] [CrossRef] [PubMed]
- Sugimoto, M.; Sahara, S.; Ichikawa, H.; Kagami, T.; Uotani, T.; Furuta, T. High Helicobacter pylori cure rate with Sitafloxacin-based triple therapy. Aliment. Pharmacol. Ther. 2015, 42, 477–483. [Google Scholar] [CrossRef] [PubMed]
- Sugimoto, M.; Hira, D.; Murata, M.; Kawai, T.; Terada, T. Effect of antibiotic susceptibility and CYP3A4/5 and CYP2C19 genotype on the outcome of vonoprazan-containing Helicobacter pylori eradication therapy. Antibiotics 2020, 9, 645. [Google Scholar] [CrossRef] [PubMed]
- Murakami, K.; Sakurai, Y.; Shiino, M.; Funao, N.; Nishimura, A.; Asaka, M. Vonoprazan, a novel potassium-competitive acid blocker, as a component of first-line and second-line triple therapy for Helicobacter pylori eradication: A phase III, randomised, double-blind study. Gut 2016, 65, 1439–1446. [Google Scholar] [CrossRef]
- Sugimoto, M.; Yamaoka, Y. Role of vonoprazan in Helicobacter pylori eradication therapy in Japan. Front. Pharmacol. 2019, 9, 1560. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, T.; Nishizawa, Y.; Yahagi, N.; Kanai, T.; Takahashi, M.; Suzuki, H. Effect of supplementation with rebamipide for Helicobacter pylori eradication therapy: A systematic review and meta-analysis. J. Gastroenterol. Hepatol. 2014, 29, 20–24. [Google Scholar] [CrossRef]
- Moher, D.; Jadad, A.R.; Nichol, G.; Penman, M.; Tugwell, P.; Walsh, S. Assessing the quality of randomized controlled trials: An annotated bibliography of scales and checklists. Control. Clin. Trials 1995, 16, 62–73. [Google Scholar] [CrossRef]
- Nishizawa, T.; Mori, K.; Yoshida, S.; Ebinuma, H.; Toyoshima, O.; Suzuki, H. Additional mosapride to proton pump inhibitor for gastroesophageal reflux disease: A meta-analysis. J. Clin. Med. 2020, 9, 2705. [Google Scholar] [CrossRef]
- Andreev, D.N.; Maev, I.V.; Dicheva, D.T. Efficiency of the inclusion of rebamipide in the eradication therapy for Helicobacter pylori infection: Meta-analysis of randomized controlled studies. J. Clin. Med. 2019, 8, 1498. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, T.; Suzuki, H.; Higuchi, H.; Ebinuma, H.; Toyoshima, O. Effects of encircled abdominal compression device in colonoscopy: A meta-analysis. J. Clin. Med. 2019, 9, 11. [Google Scholar] [CrossRef]
- Sue, S.; Sasaki, T.; Kaneko, H.; Irie, K.; Kondo, M.; Maeda, S. Helicobacter pylori rescue treatment with vonoprazan, metronidazole, and sitafloxacin in the presence of penicillin allergy. JGH Open 2021, 5, 307–311. [Google Scholar] [CrossRef] [PubMed]
- Mori, H.; Suzuki, H.; Matsuzaki, J.; Masaoka, T.; Kanai, T. Antibiotic resistance and gyrA mutation affect the efficacy of 10-day sitafloxacin-metronidazole-esomeprazole therapy for Helicobacter pylori in penicillin allergic patients. United Eur. Gastroenterol. J. 2017, 5, 796–804. [Google Scholar] [CrossRef]
- Ono, S.; Kato, M.; Nakagawa, S.; Mabe, K.; Sakamoto, N. Vonoprazan improves the efficacy of Helicobacter pylori eradication therapy with a regimen consisting of clarithromycin and metronidazole in patients allergic to penicillin. Helicobacter 2017, 22, e12374. [Google Scholar] [CrossRef] [PubMed]
- Furuta, T.; Sugimoto, M.; Yamade, M.; Uotani, T.; Sahara, S.; Ichikawa, H.; Kagami, T.; Yamada, T.; Osawa, S.; Sugimoto, K.; et al. Eradication of H. pylori infection in patients allergic to penicillin using triple therapy with a PPI, metronidazole and sitafloxacin. Intern. Med. 2014, 53, 571–575. [Google Scholar] [CrossRef]
- Murai, R.; Matsuhisa, T. Clinical practice for Helicobacter pylori at Endoscopy clinic in Hachioji, Tokyo. Helicobacter Res. 2012, 16, 546–552. [Google Scholar]
- Tokunaga, K.; Tanaka, A.; Takahashi, S. Clinical problems of H. pylori eradication therapy after application expansion of the health insurance. J. Germfree Life Gnotobiol. 2014, 44, 38–40. [Google Scholar]
- Ikeda, F. Antibioactivity of sitafloxacin to Helicobacter pylori. Jpn. J. Helicobacter Res. 2011, 12, 58–62. [Google Scholar]
- Athamna, A.; Athamna, M.; Medlej, B.; Bast, D.J.; Rubinstein, E. In vitro post-antibiotic effect of fluoroquinolones, macrolides, beta-lactams, tetracyclines, vancomycin, clindamycin, linezolid, chloramphenicol, quinupristin/dalfopristin and rifampicin on Bacillus anthracis. J. Antimicrob. Chemother. 2004, 53, 609–615. [Google Scholar] [CrossRef]
- Nishizawa, T.; Suzuki, H.; Maekawa, T.; Harada, N.; Toyokawa, T.; Kuwai, T.; Ohara, M.; Suzuki, T.; Kawanishi, M.; Noguchi, K.; et al. Dual therapy for third-line Helicobacter pylori eradication and urea breath test prediction. World J. Gastroenterol. 2012, 18, 2735–2738. [Google Scholar] [CrossRef]
- Furuta, T.; Sugimoto, M.; Yamade, M.; Uotani, T.; Sahara, S.; Ichikawa, H.; Yamada, T.; Osawa, S.; Sugimoto, K.; Watanabe, H.; et al. Effect of dosing schemes of amoxicillin on eradication rates of Helicobacter pylori with amoxicillin-based triple therapy. J. Clin. Pharm. 2014, 54, 258–266. [Google Scholar] [CrossRef]
- Yuan, Y.; Ford, A.C.; Khan, K.J.; Gisbert, J.P.; Forman, D.; Leontiadis, G.I.; Tse, F.; Calvet, X.; Fallone, C.; Fischbach, L.; et al. Optimum duration of regimens for Helicobacter pylori eradication. Cochrane Database Syst. Rev. 2010, 12, 008337. [Google Scholar]
- Noh, H.M.; Hong, S.J.; Han, J.P.; Park, K.W.; Lee, Y.N.; Lee, T.H.; Ko, B.M.; Lee, J.S.; Lee, M.S. Eradication rate by duration of third-line rescue therapy with levofloxacin after Helicobacter pylori treatment failure in clinical practice. Korean J. Gastroenterol. 2016, 68, 260–264. [Google Scholar] [CrossRef] [PubMed]
- Ercin, C.N.; Uygun, A.; Toros, A.B.; Kantarcioglu, M.; Kilciler, G.; Polat, Z.; Bagci, S. Comparison of 7- and 14-day first-line therapies including levofloxacin in patients with Helicobacter pylori positive non-ulcer dyspepsia. Turk. J. Gastroenterol. 2010, 21, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Miehlke, S.; Krasz, S.; Schneider-Brachert, W.; Kuhlisch, E.; Berning, M.; Madisch, A.; Laass, M.W.; Neumeyer, M.; Jebens, C.; Zekorn, C.; et al. Randomized trial on 14 versus 7 days of esomeprazole, moxifloxacin, and amoxicillin for second-line or rescue treatment of Helicobacter pylori infection. Helicobacter 2011, 16, 420–426. [Google Scholar] [CrossRef]
- Li, B.Z.; Threapleton, D.E.; Wang, J.Y.; Xu, J.M.; Yuan, J.Q.; Zhang, C.; Li, P.; Ye, Q.L.; Guo, B.; Mao, C.; et al. Comparative effectiveness and tolerance of treatments for Helicobacter pylori: Systematic review and network meta-analysis. BMJ 2015, 351, h4052. [Google Scholar] [CrossRef]
- Chuah, S.K.; Tai, W.C.; Hsu, P.I.; Wu, D.C.; Wu, K.L.; Kuo, C.M.; Chiu, Y.C.; Hu, M.L.; Chou, Y.P.; Kuo, Y.H.; et al. The efficacy of second-line anti-Helicobacter pylori therapy using an extended 14-day levofloxacin/amoxicillin/proton-pump inhibitor treatment—A pilot study. Helicobacter 2012, 17, 374–381. [Google Scholar] [CrossRef]
- Liao, J.; Zheng, Q.; Liang, X.; Zhang, W.; Sun, Q.; Liu, W.; Xiao, S.; Graham, D.Y.; Lu, H. Effect of fluoroquinolone resistance on 14-day levofloxacin triple and triple plus bismuth quadruple therapy. Helicobacter 2013, 18, 373–377. [Google Scholar] [CrossRef]
- Ozdil, K.; Calhan, T.; Sahin, A.; Senates, E.; Kahraman, R.; Yuzbasioglu, B.; Demirdag, H.; Demirsoy, H.; Sokmen, M.H. Levofloxacin based sequential and triple therapy compared with standard plus probiotic combination for Helicobacter pylori eradication. Hepatogastroenterology 2011, 58, 1148–1152. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, T.; Suzuki, H.; Kurabayashi, K.; Masaoka, T.; Muraoka, H.; Mori, M.; Iwasaki, E.; Kobayashi, I.; Hibi, T. Gatifloxacin resistance and mutations in gyra after unsuccessful Helicobacter pylori eradication in Japan. Antimicrob. Agents Chemother. 2006, 50, 1538–1540. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nishizawa, T.; Suzuki, H.; Tsugawa, H.; Muraoka, H.; Matsuzaki, J.; Hirata, K.; Ikeda, F.; Takahashi, M.; Hibi, T. Enhancement of amoxicillin resistance after unsuccessful Helicobacter pylori eradication. Antimicrob. Agents Chemother. 2011, 55, 3012–3014. [Google Scholar] [CrossRef]
- Rimbara, E.; Noguchi, N.; Kawai, T.; Sasatsu, M. Fluoroquinolone resistance in Helicobacter pylori: Role of mutations at position 87 and 91 of GyrA on the level of resistance and identification of a resistance conferring mutation in GyrB. Helicobacter 2012, 17, 36–42. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, T.; Suzuki, H. Mechanisms of Helicobacter pylori antibiotic resistance and molecular testing. Front. Mol. Biosci. 2014, 1, 19. [Google Scholar] [CrossRef]
- Nishizawa, T.; Suzuki, H.; Umezawa, A.; Muraoka, H.; Iwasaki, E.; Masaoka, T.; Kobayashi, I.; Hibi, T. Rapid detection of point mutations conferring resistance to fluoroquinolone in gyrA of Helicobacter pylori by allele-specific PCR. J. Clin. Microbiol. 2006, 45, 303–305. [Google Scholar] [CrossRef][Green Version]
- Mori, H.; Suzuki, H.; Matsuzaki, J.; Masaoka, T.; Kanai, T. Acquisition of double mutation in gyrA caused high resistance to sitafloxacin in Helicobacter pylori after unsuccessful eradication with sitafloxacin-containing regimens. United Eur. Gastroenterol. J. 2018, 6, 391–397. [Google Scholar] [CrossRef]
- Hirata, Y.; Yamada, A.; Niikura, R.; Shichijo, S.; Hayakawa, Y.; Koike, K. Efficacy and safety of a new rifabutin-based triple therapy with vonoprazan for refractory Helicobacter pylori infection: A prospective single-arm study. Helicobacter 2020, 25, e12719. [Google Scholar] [CrossRef]
- Gingold-Belfer, R.; Niv, Y.; Levi, Z.; Boltin, D. Rifabutin triple therapy for first-line and rescue treatment of Helicobacter pylori infection: A systematic review and meta-analysis. J. Gastroenterol. Hepatol. 2020. [Google Scholar] [CrossRef]
- Nishizawa, T.; Suzuki, H.; Matsuzaki, J.; Muraoka, H.; Tsugawa, H.; Hirata, K.; Hibi, T. Helicobacter pylori resistance to rifabutin in the last 7 years. Antimicrob. Agents Chemother. 2011, 55, 5374–5375. [Google Scholar] [CrossRef] [PubMed]
- Buehrle, D.J.; Wagener, M.M.; Clancy, C.J. Outpatient fluoroquinolone prescription fills in the United States, 2014–2020: Assessing the impact of food and drug administration safety warnings. Antimicrob. Agents Chemother. 2021. [Google Scholar] [CrossRef] [PubMed]



| Author | Year | Drug Combination | Days | Eradication Rate | STFX | |||
| PPI | STFX | AMX | ITT | PP | Resistant Rate | |||
| Hirata | 2012 | RPZ 20 m | 200 mg | 1500 mg | 7 | 75.0 | 80.0 | 25.0 |
| Murakami | 2013 | LPZ 60 mg | 200 mg | 1500 mg | 7 | 70.0 | 72.1 | ― |
| Hirata | 2016 | EPZ 40 mg | 200 mg | 1500 mg | 7 | 83.3 | 83.3 | 50.0 |
| Sue | 2019 | PPI | 200 mg | 1500 mg | 7 | 53.3 | 57.1 | ― |
| Saito | 2019 | PPI | 200 mg | 1500 mg | 7 | 54.2 | 56.5 | 21.7 |
| Matsuzaki | 2012 | RPZ 40 mg | 200 mg | 2000 mg | 7 | 78.2 | 83.6 | 42.5 |
| Furuta | 2014 | RPZ 20–40 mg | 200 mg | 2000 mg | 7 | 84.1 | 86.4 | ― |
| Tokunaga | 2014 | RPZ 30 mg | 200 mg | 1500 mg | 10 | ― | 87.1 | ― |
| Mori | 2016 | EPZ 40 mg | 200 mg | 2000 mg | 10 | 81.0 | 82.0 | 60.3 |
| Mori | 2020 | EPZ 40 mg | 200 mg | 2000 mg | 10 | 81.6 | 81.6 | 50.0 |
| Furuta | 2014 | RPZ 20–40 mg | 200 mg | 2000 mg | 14 | 88.9 | 90.9 | ― |
| Author | Year | Drug Combination | Days | Eradication Rate | STFX | |||
|---|---|---|---|---|---|---|---|---|
| VPZ | STFX | AMX | ITT | PP | Resistant Rate | |||
| Sue | 2016 | VPZ 40 mg | 200 mg | 1500 mg | 7 | 75.8 | 83.3 | ― |
| Saito | 2019 | VPZ 40 mg | 200 mg | 1500 mg | 7 | 93.0 | 93.0 | 30.0 |
| Sugimoto | 2020 | VPZ 40 mg | 200 mg | 2000 mg | 7 | ― | 87.5 | ― |
| Author | Year | Drug Combination | Days | Eradication Rate | STFX | |||
|---|---|---|---|---|---|---|---|---|
| PPI | STFX | MNZ | ITT | PP | Resistant Rate | |||
| Furuta | 2014 | RPZ 20–40 mg | 200 mg | 500 mg | 7 | 90.9 | 90.9 | ― |
| Sugimoto | 2015 | RPZ 40 mg | 200 mg | 500 mg | 7 | ― | 88.3 | ― |
| Mori | 2016 | EPZ 40 mg | 200 mg | 500 mg | 10 | 72.4 | 76.4 | 56.9 |
| Furuta | 2014 | RPZ 20–40 mg | 200 mg | 500 mg | 14 | 87.2 | 91.1 | ― |
| Author | Year | Type of Study | Quality Assessment | |
|---|---|---|---|---|
| Jadad Scale * | QATCSS Score † | |||
| Murakami | 2013 | Randomised controlled study: open label | 3 | ― |
| Furuta | 2014 | Randomised controlled study: open label | 3 | ― |
| Sue | 2019 | Randomised controlled study: open label | 3 | ― |
| Matsuzaki | 2012 | Prospective single centre open label study | ― | 9 |
| Hirata | 2012 | Prospective single center open label study | ― | 9 |
| Tokunaga | 2014 | Single center open label study | ― | 6 |
| Mori | 2015 | Prospective single center open label study | ― | 9 |
| Sugimoto | 2015 | Single center open label study | ― | 8 |
| Hirata | 2016 | Prospective multi-center open label study | ― | 9 |
| Saito | 2019 | Single center open label study | ― | 8 |
| Mori | 2020 | Prospective single center open label study | ― | 9 |
| Sugimoto | 2020 | Single center open label study | ― | 8 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nishizawa, T.; Munkjargal, M.; Ebinuma, H.; Toyoshima, O.; Suzuki, H. Sitafloxacin for Third-Line Helicobacter pylori Eradication: A Systematic Review. J. Clin. Med. 2021, 10, 2722. https://doi.org/10.3390/jcm10122722
Nishizawa T, Munkjargal M, Ebinuma H, Toyoshima O, Suzuki H. Sitafloxacin for Third-Line Helicobacter pylori Eradication: A Systematic Review. Journal of Clinical Medicine. 2021; 10(12):2722. https://doi.org/10.3390/jcm10122722
Chicago/Turabian StyleNishizawa, Toshihiro, Munkhbayar Munkjargal, Hirotoshi Ebinuma, Osamu Toyoshima, and Hidekazu Suzuki. 2021. "Sitafloxacin for Third-Line Helicobacter pylori Eradication: A Systematic Review" Journal of Clinical Medicine 10, no. 12: 2722. https://doi.org/10.3390/jcm10122722
APA StyleNishizawa, T., Munkjargal, M., Ebinuma, H., Toyoshima, O., & Suzuki, H. (2021). Sitafloxacin for Third-Line Helicobacter pylori Eradication: A Systematic Review. Journal of Clinical Medicine, 10(12), 2722. https://doi.org/10.3390/jcm10122722







