History Taking in Non-Acute Vestibular Symptoms: A 4-Step Approach
Abstract
:1. Introduction
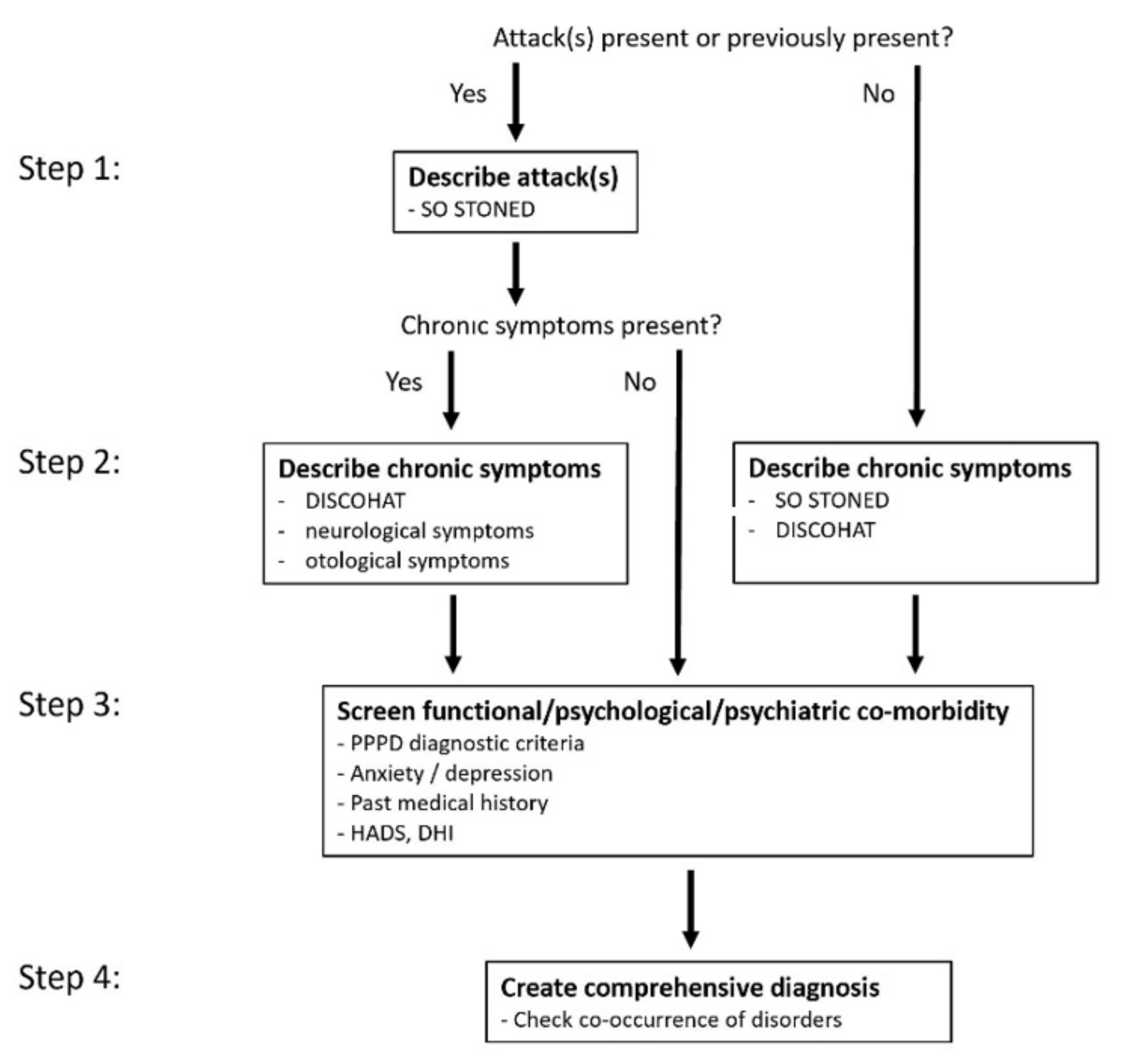
2. Overview of the 4-Step Approach
- The first step is to investigate whether there are, or have been, any attacks of vertigo and/or dizziness. If so, the attacks are described.
- The second step involves exploring any chronic vestibular symptoms.
- The third step screens for functional, psychological, and/or psychiatric co-morbidity.
- During the fourth step, the diagnosis is established by explicitly taking into account the possibility of multiple co-occurring vestibular disorders.
Key Points of the 4-Step Approach
3. Background, Pearls, and Pitfalls of the 4-Step Approach
3.1. Step 1: Describe Any Attack(s) of Vertigo and/or Dizziness
3.1.1. Background
3.1.2. Pearls and Pitfalls
3.2. Step 2: Describe Any Chronic Vestibular Symptoms
3.2.1. Background
3.2.2. Pearls and Pitfalls
3.3. Step 3: Screen for Functional, Psychological, and Psychiatric Co-Morbidity
3.3.1. Background
3.3.2. Pearls and Pitfalls
3.4. Step 4: Create a Comprehensive Diagnosis
3.4.1. Background
- Step 1:
- For two years, symptoms of vertigo and dizziness, including multiple spontaneous attacks of vertigo.
- The average attack features:
- -
- Sudden sensation of vertigo
- -
- Triggers: none
- -
- Hearing loss on the left, aural pressure, and tinnitus (high-pitched sound)
- -
- No headache, no photo- or phonophobia, no visual auras, no migraines
- -
- No other neurological symptoms (including the ‘deadly Ds’)
- -
- Duration: minimum 5 min, maximum 2 h
- -
- Frequency: 2–5 times each month, frequency increased the last couple of months
- Step 2:
- Chronic symptoms between attacks:
- -
- Darkness does not worsen symptoms; imbalance; supermarket effect (=visually induced dizziness); no problems with concentration or memory; no oscillopsia; fast head movements worsen symptoms; no autonomic complaints, not very tired
- -
- Persistent hearing loss and tinnitus on the left ear, no neurological symptoms
- Step 3:
- -
- Significant distress resulting from chronic ‘fuzziness’ and the supermarket effect (=visually induced dizziness); no avoidance behavior or symptoms of anxiety or depression; no previous history of functional/psychological/psychiatric co-morbidity
- Step 4:
- -
- Possible diagnosis based on history taking only: Menière’s disease on the left ear + vestibular hypofunction + PPPD
- Description of the attacks: symptoms might indicate Menière’s disease on the left ear.
- Description of chronic symptoms: imbalance and stronger symptoms in relation to fast head movements might indicate vestibular hypofunction; visually induced dizziness might indicate PPPD.
- Screening for functional, psychological, and psychiatric co-morbidity: apart from significant distress resulting from chronic ‘fuzziness’ and visually induced dizziness, which indicate PPPD, no indications of other functional/psychological/psychiatric co-morbidity.
- Creating a comprehensive diagnosis: Menière’s disease, vestibular hypofunction, and PPPD all feature in the final diagnosis.
3.4.2. Pearls and Pitfalls
3.5. Other Relevant Questions
4. First Experiences and Final Remarks
Author Contributions
Funding
Institutional Review Board Statement
Acknowledgments
Conflicts of Interest
References
- Bisdorff, A. Vestibular symptoms and history taking. Handb. Clin. Neurol. 2016, 137, 83–90. [Google Scholar]
- Agrawal, Y.; Van de Berg, R.; Wuyts, F.; Walther, L.; Magnusson, M.; Oh, E.; Sharpe, M.; Strupp, M. Presbyvestibulopathy: Diagnostic criteria Consensus document of the Classification Committee of the Barany Society. J. Vestib. Res. 2019, 29, 161–170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bisdorff, A.; Von Brevern, M.; Lempert, T.; Newman-Toker, D.E. Classification of vestibular symptoms: Towards an international classification of vestibular disorders. J. Vestib. Res. 2009, 19, 1–13. [Google Scholar] [CrossRef] [Green Version]
- Cha, Y.H.; Baloh, R.W.; Cho, C.; Magnusson, M.; Song, J.J.; Strupp, M.; Wuyts, F.; Staab, J.P. Mal de debarquement syndrome diagnostic criteria: Consensus document of the Classification Committee of the Barany Society. J. Vestib. Res. 2020, 30, 285–293. [Google Scholar] [CrossRef]
- Cha, Y.H.; Golding, J.; Keshavarz, B.; Furman, J.; Kim, J.S.; Lopez-Escamez, J.A.; Magnusson, M.; Yates, B.J.; Lawson, B.D.; Staab, J.; et al. Motion sickness diagnostic criteria: Consensus document of the Classification Committee of the Barany society. J. Vestib. Res. 2021, 1–17. [Google Scholar] [CrossRef]
- Lempert, T.; Olesen, J.; Furman, J.; Waterston, J.; Seemungal, B.; Carey, J.; Bisdorff, A.; Versino, M.; Evers, S.; Newman-Toker, D. Vestibular migraine: Diagnostic criteria. J. Vestib. Res. 2012, 22, 167–172. [Google Scholar] [CrossRef] [Green Version]
- Lopez-Escamez, J.A.; Carey, J.; Chung, W.H.; Goebel, J.A.; Magnusson, M.; Mandala, M.; Newman-Toker, D.E.; Strupp, M.; Suzuki, M.; Trabalzini, F.; et al. Diagnostic criteria for Meniere’s disease according to the Classification Committee of the Barany Society. HNO 2017, 65, 887–893. [Google Scholar] [CrossRef]
- Staab, J.P.; Eckhardt-Henn, A.; Horii, A.; Jacob, R.; Strupp, M.; Brandt, T.; Bronstein, A. Diagnostic criteria for persistent postural-perceptual dizziness (PPPD): Consensus document of the Committee for the Classification of Vestibular Disorders of the Barany Society. J. Vestib. Res. 2017, 27, 191–208. [Google Scholar] [CrossRef] [Green Version]
- Strupp, M.; Kim, J.S.; Murofushi, T.; Straumann, D.; Jen, J.C.; Rosengren, S.M.; Della Santina, C.C.; Kingma, H. Bilateral vestibulopathy: Diagnostic criteria Consensus document of the Classification Committee of the Barany Society. J. Vestib. Res. 2017, 27, 177–189. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strupp, M.; Lopez-Escamez, J.A.; Kim, J.S.; Straumann, D.; Jen, J.C.; Carey, J.; Bisdorff, A.; Brandt, T. Vestibular paroxysmia: Diagnostic criteria. J. Vestib. Res. 2016, 26, 409–415. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Van de Berg, R.; Widdershoven, J.; Bisdorff, A.; Evers, S.; Wiener-Vacher, S.; Cushing, S.L.; Mack, K.J.; Kim, J.S.; Jahn, K.; Strupp, M.; et al. Vestibular migraine of childhood and recurrent vertigo of childhood: Diagnostic criteria Consensus document of the Committee for the Classification of Vestibular Disorders of the Barany Society and the International Headache Society. J. Vestib. Res. 2021, 31, 1–9. [Google Scholar] [CrossRef]
- Von Brevern, M.; Bertholon, P.; Brandt, T.; Fife, T.; Imai, T.; Nuti, D.; Newman-Toker, D. Benign paroxysmal positional vertigo: Diagnostic criteria Consensus document of the Committee for the Classification of Vestibular Disorders of the Barany Society. Acta Otorrinolaringologica Espanola 2017, 68, 349–360. [Google Scholar] [CrossRef] [PubMed]
- Ward, B.K.; van de Berg, R.; van Rompaey, V.; Bisdorff, A.; Hullar, T.E.; Welgampola, M.S.; Carey, J.P. Superior semicircular canal dehiscence syndrome: Diagnostic criteria Consensus document of the Committee for the Classification of Vestibular Disorders of the Barany Society. J. Vestib. Res. 2021, 31, 131–141. [Google Scholar] [CrossRef]
- Kerber, K.A.; Newman-Toker, D.E. Misdiagnosing dizzy patients: Common pitfalls in clinical practice. Neurol. Clin. 2015, 33, 565–575. [Google Scholar] [CrossRef] [PubMed]
- Strobl, R.; Grozinger, M.; Zwergal, A.; Huppert, D.; Filippopulos, F.; Grill, E. A Set of eight key questions helps to classify common vestibular disorders-results from the DizzyReg patient registry. Front. Neurol. 2021, 12, 670944. [Google Scholar] [CrossRef]
- Brandt, T.; Strupp, M.; Dieterich, M. Five keys for diagnosing most vertigo, dizziness, and imbalance syndromes: An expert opinion. J. Neurol. 2014, 261, 229–231. [Google Scholar] [CrossRef] [PubMed]
- Newman-Toker, D.E.; Edlow, J.A. TiTrATE: A novel, evidence-based approach to diagnosing acute dizziness and vertigo. Neurol. Clin. 2015, 33, 577–599. [Google Scholar] [CrossRef] [Green Version]
- Wuyts, F.L.; Van Rompaey, V.; Maes, L.K. “SO STONED”: Common sense approach of the dizzy patient. front surg. Front. Surg. 2016, 3, 32. [Google Scholar] [CrossRef] [Green Version]
- Paredis, S.; van Stiphout, L.; Remmen, E.; Strupp, M.; Gerards, M.-C.; Kingma, H.; Van Rompaey, V.; Perez-Fornos, A.; Guinand, N.; van de Berg, R. DISCOHAT: An acronym to describe the spectrum of symptoms related to bilateral vestibulopathy. Front. Neurol. 2021. [Google Scholar] [CrossRef]
- Blakley, B.W.; Goebel, J. The meaning of the word “vertigo”. Otolaryngol. Head Neck Surg. 2001, 125, 147–150. [Google Scholar] [CrossRef]
- Newman-Toker, D.E.; Cannon, L.M.; Stofferahn, M.E.; Rothman, R.E.; Hsieh, Y.H.; Zee, D.S. Imprecision in patient reports of dizziness symptom quality: A cross-sectional study conducted in an acute care setting. Mayo Clin. Proc. 2007, 82, 1329–1340. [Google Scholar] [CrossRef] [PubMed]
- Newman-Toker, D. Vertigo and dizziness. In Encyclopedia of the Neurological Sciences; Elsevier Inc.: Amsterdam, The Netherlands, 2014; pp. 629–637. [Google Scholar]
- Newman-Toker, D.E. Symptoms and signs of neuro-otologic disorders. CONTINUUM Lifelong Learn. Neurol. 2012, 18, 1016–1040. [Google Scholar] [CrossRef]
- Roberts, R.A.; Jacobson, G.P.; Hatton, K. Multiple co-occurring vestibular disorders identified using the dizziness symptom profile. Am. J. Audiol. 2020, 29, 410–418. [Google Scholar] [CrossRef]
- Zhu, R.T.; Van Rompaey, V.; Ward, B.K.; Van de Berg, R.; Van de Heyning, P.; Sharon, J.D. The interrelations between different causes of dizziness: A conceptual framework for understanding vestibular disorders. Ann. Otol. Rhinol. Laryngol. 2019, 128, 869–878. [Google Scholar] [CrossRef] [PubMed]
- Lahmann, C.; Henningsen, P.; Brandt, T.; Strupp, M.; Jahn, K.; Dieterich, M.; Eckhardt-Henn, A.; Feuerecker, R.; Dinkel, A.; Schmid, G. Psychiatric comorbidity and psychosocial impairment among patients with vertigo and dizziness. J. Neurol. Neurosurg. Psychiatry 2015, 86, 302–308. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Popkirov, S.; Stone, J.; Holle-Lee, D. Treatment of persistent postural-perceptual dizziness (PPPD) and related disorders. Curr. Treat. Options Neurol. 2018, 20, 50. [Google Scholar] [CrossRef]
- Zingler, V.C.; Cnyrim, C.; Jahn, K.; Weintz, E.; Fernbacher, J.; Frenzel, C.; Brandt, T.; Strupp, M. Causative factors and epidemiology of bilateral vestibulopathy in 255 patients. Ann. Neurol. 2007, 61, 524–532. [Google Scholar] [CrossRef] [PubMed]
- Lucieer, F.; Vonk, P.; Guinand, N.; Stokroos, R.; Kingma, H.; van de Berg, R. Bilateral vestibular hypofunction: Insights in etiologies, clinical subtypes, and diagnostics. Front. Neurol. 2016, 7, 26. [Google Scholar] [CrossRef] [Green Version]
- Lacour, M.; Dutheil, S.; Tighilet, B.; Lopez, C.; Borel, L. Tell me your vestibular deficit, and I’ll tell you how you’ll compensate. Ann. N. Y. Acad. Sci. 2009, 1164, 268–278. [Google Scholar] [CrossRef] [PubMed]
- Lucieer, F.; Duijn, S.; Van Rompaey, V.; Perez Fornos, A.; Guinand, N.; Guyot, J.P.; Kingma, H.; van de Berg, R. Full spectrum of reported symptoms of bilateral vestibulopathy needs further investigation-A systematic review. Front. Neurol. 2018, 9, 352. [Google Scholar] [CrossRef] [Green Version]
- Lucieer, F.M.P.; Van Hecke, R.; van Stiphout, L.; Duijn, S.; Perez-Fornos, A.; Guinand, N.; Van Rompaey, V.; Kingma, H.; Joore, M.; van de Berg, R. Bilateral vestibulopathy: Beyond imbalance and oscillopsia. J. Neurol. 2020, 267, 241–255. [Google Scholar] [CrossRef] [PubMed]
- Van de Berg, R.; van Tilburg, M.; Kingma, H. Bilateral vestibular hypofunction: Challenges in establishing the diagnosis in adults. ORL J. Otorhinolaryngol. Relat. Spec. 2015, 77, 197–218. [Google Scholar] [CrossRef] [PubMed]
- Yeo, N.L.; White, M.P.; Ronan, N.; Whinney, D.J.; Curnow, A.; Tyrrell, J. Stress and unusual events exacerbate symptoms in Meniere’s disease: A longitudinal study. Otol. Neurotol. 2018, 39, 73–81. [Google Scholar] [CrossRef] [PubMed]
- Brandt, T.; Huppert, D.; Strupp, M.; Dieterich, M. Functional dizziness: Diagnostic keys and differential diagnosis. J. Neurol. 2015, 262, 1977–1980. [Google Scholar] [CrossRef]
- Gofrit, S.G.; Mayler, Y.; Eliashar, R.; Bdolah-Abram, T.; Ilan, O.; Gross, M. The association between vestibular physical examination, vertigo questionnaires, and the electronystagmography in patients with vestibular symptoms. Ann. Otol. Rhinol. Laryngol. 2017, 126, 315–321. [Google Scholar] [CrossRef] [PubMed]
- Yip, C.W.; Strupp, M. The Dizziness Handicap Inventory does not correlate with vestibular function tests: A prospective study. J. Neurol. 2018, 265, 1210–1218. [Google Scholar] [CrossRef]
- Jacobson, G.P.; Newman, C.W. The development of the Dizziness Handicap Inventory. Arch. Otolaryngol. Head Neck Surg. 1990, 116, 424–427. [Google Scholar] [CrossRef] [PubMed]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica 1983, 67, 361–370. [Google Scholar] [CrossRef] [Green Version]
- Frejo, L.; Soto-Varela, A.; Santos-Perez, S.; Aran, I.; Batuecas-Caletrio, A.; Perez-Guillen, V.; Perez-Garrigues, H.; Fraile, J.; Martin-Sanz, E.; Tapia, M.C.; et al. Clinical subgroups in bilateral Meniere disease. Front. Neurol. 2016, 7, 182. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moscicki, E.K.; Elkins, E.F.; Baum, H.M.; McNamara, P.M. Hearing loss in the elderly: An epidemiologic study of the Framingham Heart Study Cohort. Ear Hear. 1985, 6, 184–190. [Google Scholar] [CrossRef]

| Time Course | Trigger | Diagnosis: Less Urgent | Diagnosis: More Urgent |
|---|---|---|---|
| Acute vestibular syndrome | Spontaneous | Acute unilateral vestibulopathy/ vestibular neuritis Labyrinthitis | Stroke or hemorrhage Brainstem encephalitis Multiple sclerosis * Other internal/neuro |
| Postexposure | Labyrinthine concussion | Skull base fracture Postoperative * Vertebral dissection Drugs (e.g., alcohol, anticonvulsants) Carbon monoxide intoxication Wernicke’s | |
| Episodic vestibular syndrome | Spontaneous | Menière’s Disease Vestibular Migraine Vestibular Paroxysmia Vasovagal Panic * | Cardiac arrhythmia TIA (posterior circulation) Hypoglycemia * |
| Trigger | Benign Paroxysmal Positional Vertigo Orthostatic hypotension Third mobile window syndromes * Superior canal dehiscence syndrome | Central positional nystagmus Vertebral artery compression/ occlusion syndrome | |
| Chronic vestibular syndrome | Triggered or spontaneous | e.g., Vestibular hypofunction, Cerebellar dizziness, Functional dizziness | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
van de Berg, R.; Kingma, H. History Taking in Non-Acute Vestibular Symptoms: A 4-Step Approach. J. Clin. Med. 2021, 10, 5726. https://doi.org/10.3390/jcm10245726
van de Berg R, Kingma H. History Taking in Non-Acute Vestibular Symptoms: A 4-Step Approach. Journal of Clinical Medicine. 2021; 10(24):5726. https://doi.org/10.3390/jcm10245726
Chicago/Turabian Stylevan de Berg, Raymond, and Herman Kingma. 2021. "History Taking in Non-Acute Vestibular Symptoms: A 4-Step Approach" Journal of Clinical Medicine 10, no. 24: 5726. https://doi.org/10.3390/jcm10245726
APA Stylevan de Berg, R., & Kingma, H. (2021). History Taking in Non-Acute Vestibular Symptoms: A 4-Step Approach. Journal of Clinical Medicine, 10(24), 5726. https://doi.org/10.3390/jcm10245726







