Restless Leg Syndrome Is Underdiagnosed in Hereditary Hemorrhagic Telangiectasia—Results of an Online Survey
Abstract
1. Introduction
2. Materials and Methods
Statistical Methods
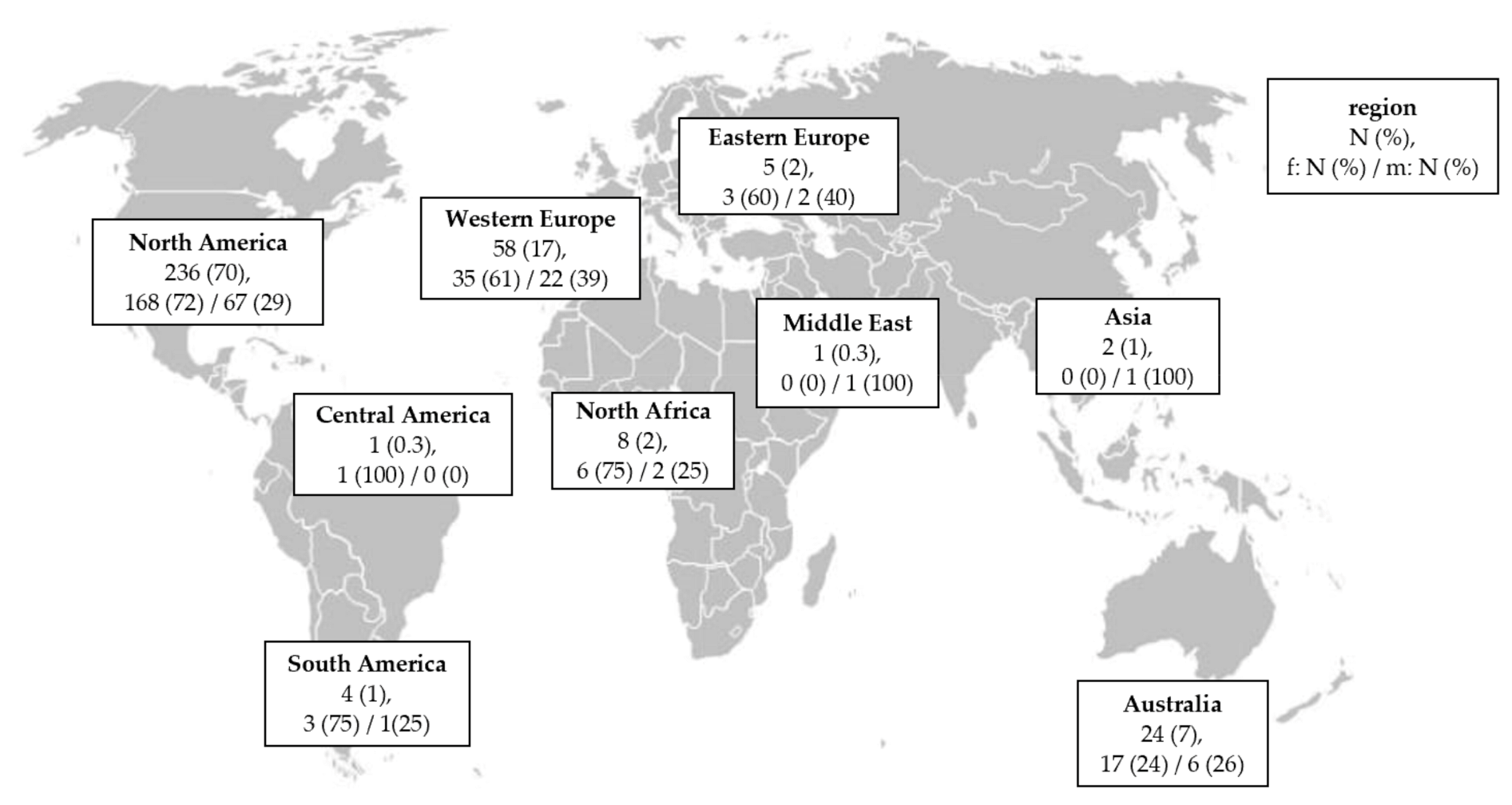
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kjeldsen, A.D.; Vase, P.; Green, A. Hereditary hemorrhagic telangiectasia. A population-based study on prevalence and mortality among Danish HHT patients. Ugeskr Laeger 2000, 162, 3597–3601. [Google Scholar] [PubMed]
- Shovlin, C.L.; Guttmacher, A.E.; Buscarini, E.; Faughnan, M.E.; Hyland, R.H.; Westermann, C.J.; Kjeldsen, A.D.; Plauchu, H. Diagnostic criteria for hereditary hemorrhagic telangiectasia (Rendu-Osler-Weber syndrome). Am. J. Med. Genet. 2000, 91, 66–67. [Google Scholar] [CrossRef]
- McDonald, J.; Wooderchak-Donahue, W.; VanSant Webb, C.; Whitehead, K.; Stevenson, D.A.; Bayrak-Toydemir, P. Hereditary hemorrhagic telangiectasia: Genetics and molecular diagnostics in a new era. Front. Genet. 2015, 6, 1. [Google Scholar] [CrossRef] [PubMed]
- Allen, R.P.; Earley, C.J. The role of iron in restless legs syndrome. Mov. Disord. 2007, 22 (Suppl. 18), S440–S448. [Google Scholar] [CrossRef] [PubMed]
- Aspenstroem, G. Pica and Restless Legs in Iron Deficiency. Sven Lakartidn 1964, 61, 1174–1177. [Google Scholar]
- Akyol, A.; Kiylioglu, N.; Kadikoylu, G.; Bolaman, A.Z.; Ozgel, N. Iron deficiency anemia and restless legs syndrome: Is there an electrophysiological abnormality? Clin. Neurol. Neurosurg. 2003, 106, 23–27. [Google Scholar] [CrossRef]
- Earley, C.J.; Silber, M.H. Restless legs syndrome: Understanding its consequences and the need for better treatment. Sleep Med. 2010, 11, 807–815. [Google Scholar] [CrossRef]
- Droege, F.; Thangavelu, K.; Stuck, B.A.; Stang, A.; Lang, S.; Geisthoff, U. Life expectancy and comorbidities in patients with hereditary hemorrhagic telangiectasia. Vasc. Med. 2018, 23, 377–383. [Google Scholar] [CrossRef]
- Sabba, C.; Pasculli, G.; Suppressa, P.; D’Ovidio, F.; Lenato, G.M.; Resta, F.; Assennato, G.; Guanti, G. Life expectancy in patients with hereditary haemorrhagic telangiectasia. QJM 2006, 99, 327–334. [Google Scholar] [CrossRef]
- Circo, S.; Gossage, J.R. Pulmonary vascular complications of hereditary haemorrhagic telangiectasia. Curr. Opin. Pulm. Med. 2014, 20, 421–428. [Google Scholar] [CrossRef]
- Hosman, A.E.; Shovlin, C.L. Cancer and hereditary haemorrhagic telangiectasia. J. Cancer Res. Clin. Oncol. 2017, 143, 369–370. [Google Scholar] [CrossRef]
- Droege, F.; Lueb, C.; Thangavelu, K.; Stuck, B.A.; Lang, S.; Geisthoff, U. Nasal self-packing for epistaxis in Hereditary Hemorrhagic Telangiectasia increases quality of life. Rhinology 2019, 57, 231–239. [Google Scholar] [CrossRef]
- Hoag, J.B.; Terry, P.; Mitchell, S.; Reh, D.; Merlo, C.A. An epistaxis severity score for hereditary hemorrhagic telangiectasia. Laryngoscope 2010, 120, 838–843. [Google Scholar] [CrossRef]
- Benes, H.; Kohnen, R. Validation of an algorithm for the diagnosis of Restless Legs Syndrome: The Restless Legs Syndrome-Diagnostic Index (RLS-DI). Sleep Med. 2009, 10, 515–523. [Google Scholar] [CrossRef]
- WHO. Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity. In Vitamin and Mineral Nutrition Information System; World Health Organization: Geneva, Switzerland, 2011. [Google Scholar]
- Softonic. Available online: https://free-editable-worldmap-for-powerpoint.de.softonic.com/ (accessed on 16 September 2020).
- Post, M.C.; Letteboer, T.G.; Mager, J.J.; Plokker, T.H.; Kelder, J.C.; Westermann, C.J. A pulmonary right-to-left shunt in patients with hereditary hemorrhagic telangiectasia is associated with an increased prevalence of migraine. Chest 2005, 128, 2485–2489. [Google Scholar] [CrossRef][Green Version]
- Ulfberg, J.; Bjorvatn, B.; Leissner, L.; Gyring, J.; Karlsborg, M.; Regeur, L.; Skeidsvoll, H.; Polo, O.; Partinen, M.; Nordic, R.L.S.S.G. Comorbidity in restless legs syndrome among a sample of Swedish adults. Sleep Med. 2007, 8, 768–772. [Google Scholar] [CrossRef]
- Park, Y.M.; Lee, H.J.; Kang, S.G.; Choi, H.S.; Choi, J.E.; Cho, J.H.; Kim, L. Prevalence of idiopathic and secondary restless legs syndrome in Korean Women. Gen. Hosp. Psychiatry 2010, 32, 164–168. [Google Scholar] [CrossRef]
- Chen, N.H.; Chuang, L.P.; Yang, C.T.; Kushida, C.A.; Hsu, S.C.; Wang, P.C.; Lin, S.W.; Chou, Y.T.; Chen, R.S.; Li, H.Y.; et al. The prevalence of restless legs syndrome in Taiwanese adults. Psychiatry Clin. Neurosci. 2010, 64, 170–178. [Google Scholar] [CrossRef]
- Allen, R.P.; Auerbach, S.; Bahrain, H.; Auerbach, M.; Earley, C.J. The prevalence and impact of restless legs syndrome on patients with iron deficiency anemia. Am. J. Hematol. 2013, 88, 261–264. [Google Scholar] [CrossRef]
- Ferri, R.; Lanuzza, B.; Cosentino, F.I.; Iero, I.; Tripodi, M.; Spada, R.S.; Toscano, G.; Marelli, S.; Arico, D.; Bella, R.; et al. A single question for the rapid screening of restless legs syndrome in the neurological clinical practice. Eur. J. Neurol. 2007, 14, 1016–1021. [Google Scholar] [CrossRef]
- Winkelman, J.W.; Shahar, E.; Sharief, I.; Gottlieb, D.J. Association of restless legs syndrome and cardiovascular disease in the Sleep Heart Health Study. Neurology 2008, 70, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Faraut, B.; Boudjeltia, K.Z.; Vanhamme, L.; Kerkhofs, M. Immune, inflammatory and cardiovascular consequences of sleep restriction and recovery. Sleep Med. Rev. 2012, 16, 137–149. [Google Scholar] [CrossRef] [PubMed]
- Cubo, E.; Gallego-Nieto, C.; Elizari-Roncal, M.; Barroso-Perez, T.; Collazo, C.; Calvo, S.; Delgado-Lopez, P.D. Is Restless Legs Syndrome Associated with an Increased Risk of Mortality? A Meta-Analysis of Cohort Studies. Tremor Other Hyperkinet Mov. 2019, 9. [Google Scholar] [CrossRef]
- Erikson, K.M.; Jones, B.C.; Beard, J.L. Iron deficiency alters dopamine transporter functioning in rat striatum. J. Nutr. 2000, 130, 2831–2837. [Google Scholar] [CrossRef] [PubMed]
- Connor, J.R.; Wang, X.S.; Allen, R.P.; Beard, J.L.; Wiesinger, J.A.; Felt, B.T.; Earley, C.J. Altered dopaminergic profile in the putamen and substantia nigra in restless leg syndrome. Brain 2009, 132, 2403–2412. [Google Scholar] [CrossRef] [PubMed]
- Alvarez-Ossorio, L.; Kirchner, H.; Kluter, H.; Schlenke, P. Low ferritin levels indicate the need for iron supplementation: Strategy to minimize iron-depletion in regular blood donors. Transfus. Med. 2000, 10, 107–112. [Google Scholar] [CrossRef] [PubMed]
- Guyatt, G.H.; Patterson, C.; Ali, M.; Singer, J.; Levine, M.; Turpie, I.; Meyer, R. Diagnosis of iron-deficiency anemia in the elderly. Am. J. Med. 1990, 88, 205–209. [Google Scholar] [CrossRef]
- Means, R.T., Jr.; Allen, J.; Sears, D.A.; Schuster, S.J. Serum soluble transferrin receptor and the prediction of marrow aspirate iron results in a heterogeneous group of patients. Clin. Lab. Haematol. 1999, 21, 161–167. [Google Scholar] [CrossRef]
- Shovlin, C.L.; Buscarini, E.; Kjeldsen, A.D.; Mager, H.J.; Sabba, C.; Droege, F.; Geisthoff, U.; Ugolini, S.; Dupuis-Girod, S. European Reference Network For Rare Vascular Diseases (VASCERN) Outcome Measures For Hereditary Haemorrhagic Telangiectasia (HHT). Orphanet J. Rare Dis. 2018, 13, 136. [Google Scholar] [CrossRef]
- Zarrabeitia, R.; Farinas-Alvarez, C.; Santibanez, M.; Senaris, B.; Fontalba, A.; Botella, L.M.; Parra, J.A. Quality of life in patients with hereditary haemorrhagic telangiectasia (HHT). Health Qual. Life Outcomes 2017, 15, 19. [Google Scholar] [CrossRef]
- Geisthoff, U.W.; Heckmann, K.; D’Amelio, R.; Grunewald, S.; Knobber, D.; Falkai, P.; Konig, J. Health-related quality of life in hereditary hemorrhagic telangiectasia. Otolaryngol. Head Neck Surg. 2007, 136, 726–733; discussion 734–725. [Google Scholar] [CrossRef]
- Wang, J.; O’Reilly, B.; Venkataraman, R.; Mysliwiec, V.; Mysliwiec, A. Efficacy of oral iron in patients with restless legs syndrome and a low-normal ferritin: A randomized, double-blind, placebo-controlled study. Sleep Med. 2009, 10, 973–975. [Google Scholar] [CrossRef]
- Seeman, M.V. Why Are Women Prone to Restless Legs Syndrome? Int. J. Environ. Res. Public Health 2020, 17, 368. [Google Scholar] [CrossRef]
- Koo, B.B. Restless legs syndrome: Relationship between prevalence and latitude. Sleep Breath 2012, 16, 1237–1245. [Google Scholar] [CrossRef]

| Number of Answered Questions (n (%)) | Number of Patients (n (%)) | ||
|---|---|---|---|
| sex | 467/474 (99) | males | 148 (32) |
| female | 319 (68) | ||
| genetic testing | 468/474 (99) | yes | 260 (56) |
| no | 208 (44) | ||
| genetic mutation | 190/474 (40) | HHT Type 1 | 72 (38) |
| HHT Type 2 | 114 (60) | ||
| SMAD 4 | 3 (2) | ||
| HHT Type 5 | 1 (1) |
| Diagnosis by RLS-DI | |||||
|---|---|---|---|---|---|
| Yes | Possible | No | Sum | ||
| RLS diagnosis by physician | yes | 23 | 16 | 8 | 47 a,b |
| no | 25 a,b | 43 b | 207 | 275 | |
| sum | 48 | 59 | 215 | 322 | |
| Symptom | Patients | Assumed RLS * | Percent | PR | 95%CI |
|---|---|---|---|---|---|
| gastrointestinal bleeding | |||||
| no | 115 | 13 | 11 | Ref. | |
| yes | 144 | 44 | 31 | 2.70 | 1.53–4.77 |
| epistaxis | |||||
| no | 13 | 1 | 8 | Ref. | |
| yes | 399 | 80 | 20 | 2.61 | 0.39–17.31 |
| anemia | |||||
| no | 71 | 15 | 21 | Ref. | |
| yes | 299 | 63 | 21 | 1.00 | 0.60–1.64 |
| blood transfusions | |||||
| no | 180 | 31 | 17 | Ref. | |
| yes | 125 | 41 | 33 | 1.90 | 1.27–2.86 |
| iron intake (oral and/or intravenous) | |||||
| no | 67 | 7 | 10 | Ref. | |
| yes | 345 | 74 | 21 | 2.05 | 0.99–4.26 |
| genetic mutation † | |||||
| type 1 | 59 | 17 | 29 | 1.34 | 0.77–2.31 |
| type 2 | 102 | 22 | 22 | Ref. | |
| Origin † | |||||
| America | 213 | 56 | 26 | Ref. | |
| Africa | 8 | 4 | 50 | 1.90 | 0.92–3.94 |
| Australia | 20 | 4 | 20 | 0.76 | 0.31–1.88 |
| Europe | 52 | 8 | 15 | 0.59 | 0.30–1.15 |
| sex | |||||
| women | 274 | 55 | 20 | Ref. | |
| men | 132 | 23 | 17 | 0.87 | 0.56–1.35 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Droege, F.; Stang, A.; Thangavelu, K.; Lueb, C.; Lang, S.; Xydakis, M.; Geisthoff, U. Restless Leg Syndrome Is Underdiagnosed in Hereditary Hemorrhagic Telangiectasia—Results of an Online Survey. J. Clin. Med. 2021, 10, 1993. https://doi.org/10.3390/jcm10091993
Droege F, Stang A, Thangavelu K, Lueb C, Lang S, Xydakis M, Geisthoff U. Restless Leg Syndrome Is Underdiagnosed in Hereditary Hemorrhagic Telangiectasia—Results of an Online Survey. Journal of Clinical Medicine. 2021; 10(9):1993. https://doi.org/10.3390/jcm10091993
Chicago/Turabian StyleDroege, Freya, Andreas Stang, Kruthika Thangavelu, Carolin Lueb, Stephan Lang, Michael Xydakis, and Urban Geisthoff. 2021. "Restless Leg Syndrome Is Underdiagnosed in Hereditary Hemorrhagic Telangiectasia—Results of an Online Survey" Journal of Clinical Medicine 10, no. 9: 1993. https://doi.org/10.3390/jcm10091993
APA StyleDroege, F., Stang, A., Thangavelu, K., Lueb, C., Lang, S., Xydakis, M., & Geisthoff, U. (2021). Restless Leg Syndrome Is Underdiagnosed in Hereditary Hemorrhagic Telangiectasia—Results of an Online Survey. Journal of Clinical Medicine, 10(9), 1993. https://doi.org/10.3390/jcm10091993






