ICU Patients’ Perception of Sleep and Modifiable versus Non-Modifiable Factors That Affect It: A Prospective Observational Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Setting
2.3. Questionnaire
2.4. Sound and Light
2.5. Statistical Analysis
3. Results
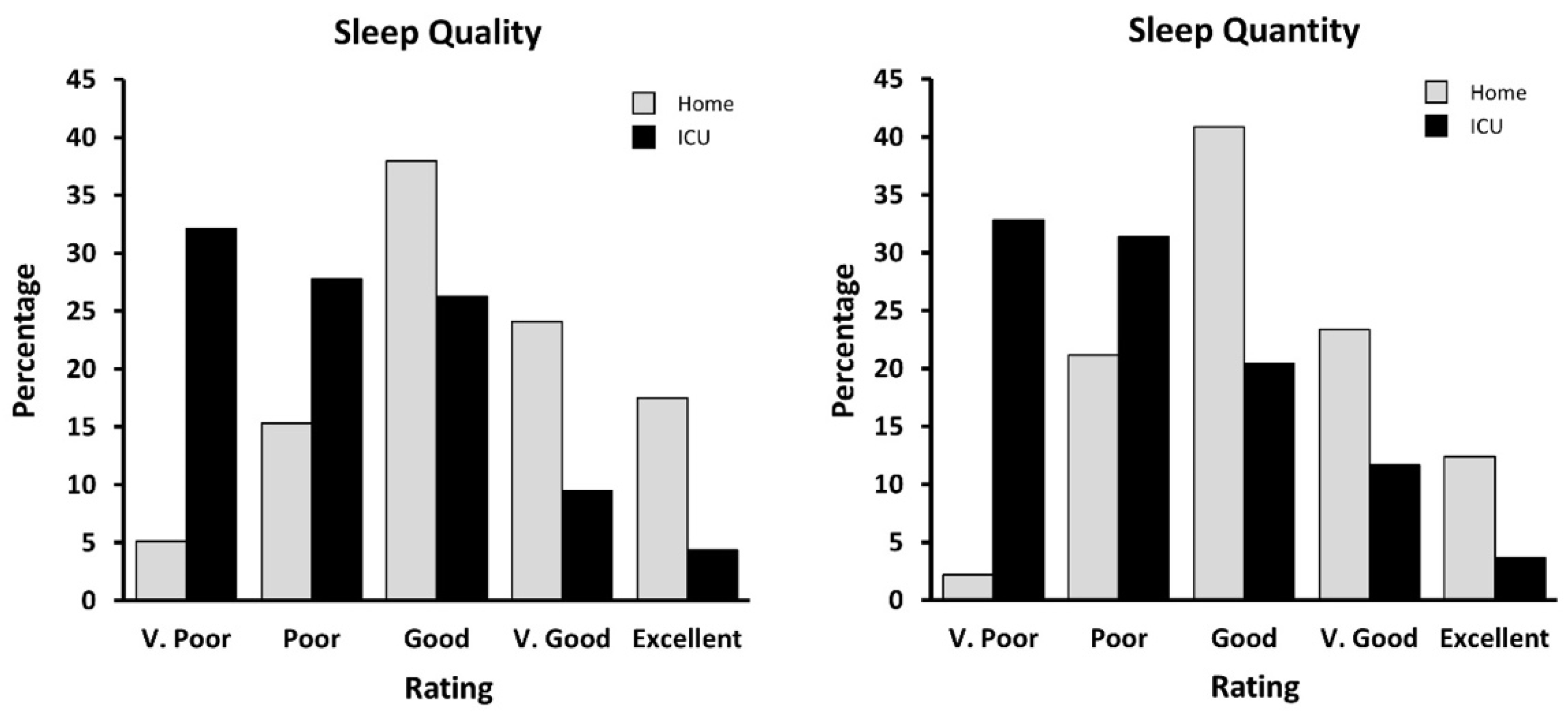
3.1. Questionnaire
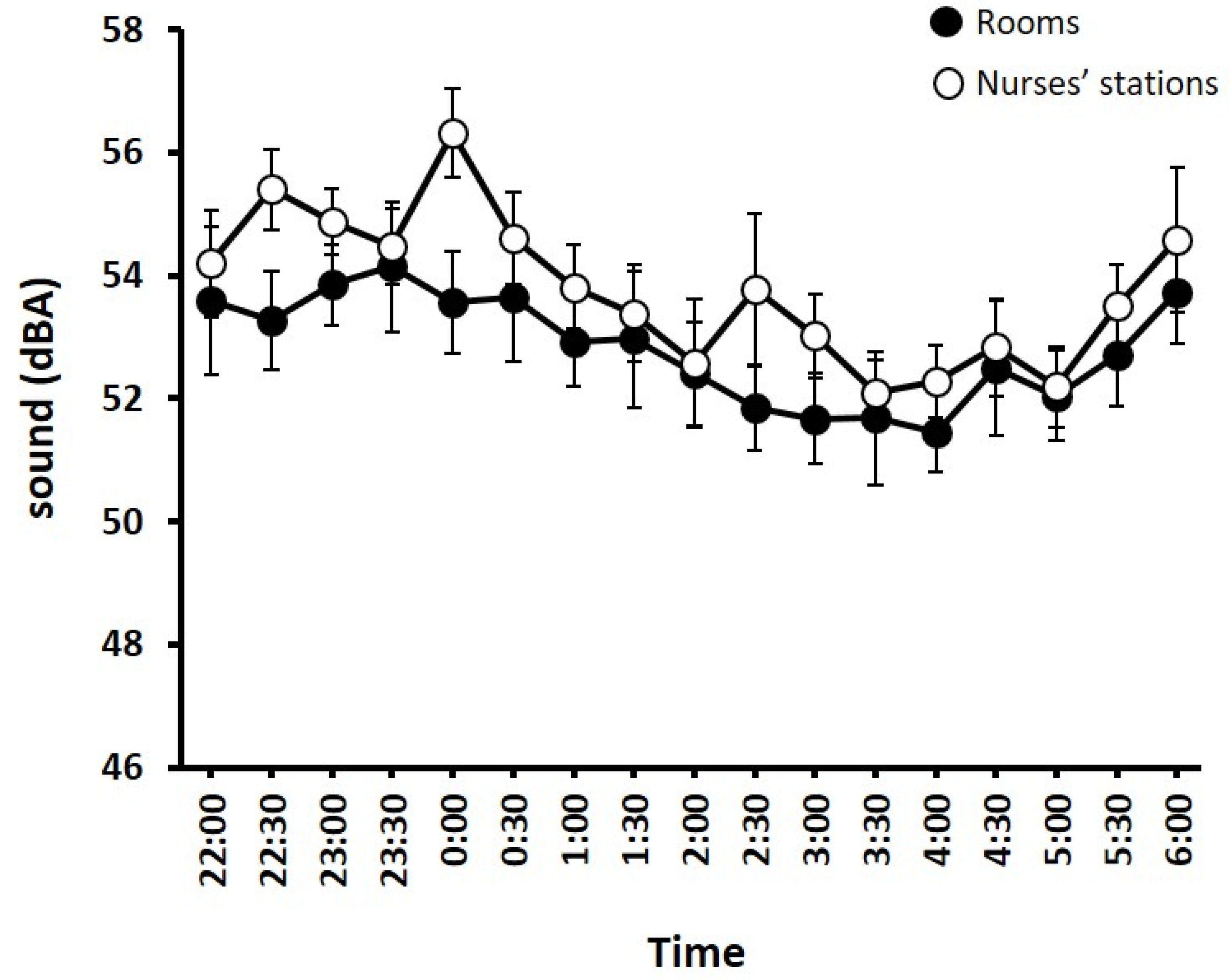
3.2. Sound
3.3. Light
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Krueger, J.M.; Frank, M.G.; Wisor, J.P.; Roy, S. Sleep function: Toward elucidating an enigma. Sleep Med. Rev. 2016, 28, 46–54. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Knauert, M.P.; Weinhouse, G.L.; Pisani, M.A.; Heideman, B.E.; Watson, P.L. Sleep in the Critically Ill Patient. In Principles and Practice of Sleep Medicine; Kryger, M., Roth, T., Goldstein, C., Dement, W., Eds.; Elsevier: Amsterdam, The Netherlands, 2022; pp. 1540–1556. [Google Scholar]
- Simini, B. Patients’ perceptions of intensive care. Lancet 1999, 354, 571–572. [Google Scholar] [CrossRef]
- Weinhouse, G.L.; Schwab, R.J. Sleep in the Critically ill Patient. Sleep 2006, 29, 707–716. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pisani, M.A.; Friese, R.S.; Gehlbach, B.K.; Schwab, R.J.; Weinhouse, G.L.; Jones, S.F. Sleep in the intensive care unit. Am. J. Respir. Crit. Care Med. 2015, 191, 731–738. [Google Scholar] [CrossRef] [Green Version]
- Nilius, G.; Richter, M.; Schroeder, M. Updated Perspectives on the Management of Sleep Disorders in the Intensive Care Unit. Nat. Sci. Sleep 2021, 13, 751–762. [Google Scholar] [CrossRef]
- Banks, S.; Dinges, D.F. Behavioral and Physiological Consequences of Sleep Restriction. J. Clin. Sleep Med. 2007, 3, 519–528. [Google Scholar] [CrossRef] [Green Version]
- Kamdar, B.B.; Needham, D.M.; Collop, N.A. Sleep Deprivation in Critical Illness: Its Role in Physical and Psychological Recovery. J. Intensive Care Med. 2011, 27, 97–111. [Google Scholar] [CrossRef]
- Little, A.; Ethier, C.; Ayas, N.; Thanachayanont, T.; Jiang, D.; Mehta, S. A patient survey of sleep quality in the Intensive Care Unit. Minerva Anestesiol. 2012, 78, 406–414. [Google Scholar]
- Stewart, J.A.; Green, C.; Stewart, J.; Tiruvoipati, R. Factors influencing quality of sleep among non-mechanically ventilated patients in the Intensive Care Unit. Aust. Crit. Care 2017, 30, 85–90. [Google Scholar] [CrossRef]
- Missildine, K.; Bergstrom, N.; Meininger, J.; Richards, K.; Foreman, M.D. Sleep in Hospitalized Elders: A Pilot Study. Geriatr. Nurs. 2010, 31, 263–271. [Google Scholar] [CrossRef]
- Darbyshire, J.L.; Young, J.D. An investigation of sound levels on intensive care units with reference to the WHO guidelines. Crit. Care 2013, 17, R187. [Google Scholar] [CrossRef] [Green Version]
- Stafford, A.; Haverland, A.; Bridges, E. Noise in the ICU. Am. J. Nurs. Sci. 2014, 114, 57–63. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jaiswal, S.J.; Garcia, S.; Owens, R.L. Sound and Light Levels Are Similarly Disruptive in ICU and non-ICU Wards. J. Hosp. Med. 2017, 12, 798–804. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- White, B.L.; Zomorodi, M. Perceived and actual noise levels in critical care units. Intensive Crit. Care Nurs. 2017, 38, 18–23. [Google Scholar] [CrossRef] [Green Version]
- Berglund, B.; Lindvall, T.; Schwela, D.H. Guidelines for Community Noise; World Health Organization: Geneva, Switzerland, 1999.
- Bernhofer, E.I.; Higgins, P.A.; Daly, B.J.; Burant, C.J.; Hornick, T.R. Hospital lighting and its association with sleep, mood and pain in medical inpatients. J. Adv. Nurs. 2014, 70, 1164–1173. [Google Scholar] [CrossRef] [PubMed]
- Meyer, T.J.; Eveloff, S.E.; Bauer, M.S.; Schwartz, W.A.; Hill, N.S.; Millman, R.P. Adverse Environmental Conditions in the Respiratory and Medical ICU Settings. Chest 1994, 105, 1211–1216. [Google Scholar] [CrossRef]
- Lavie, P. Sleep-wake as a biological rhythm. Annu. Rev. Psychol. 2001, 52, 277–303. [Google Scholar] [CrossRef] [Green Version]
- Freedman, N.S.; Kotzer, N.; Schwab, R.J. Patient Perception of Sleep Quality and Etiology of Sleep Disruption in the Intensive Care Unit. Am. J. Respir. Crit. Care Med. 1999, 159, 1155–1162. [Google Scholar] [CrossRef]
- Bihari, S.; McEvoy, R.D.; Matheson, E.; Kim, S.; Woodman, R.J.; Bersten, A.D. Factors Affecting Sleep Quality of Patients in Intensive Care Unit. J. Clin. Sleep Med. 2012, 8, 301–307. [Google Scholar] [CrossRef]
- Åkerstedt, T.; Nilsson, P.M. Sleep as restitution: An introduction. J. Intern. Med. 2003, 254, 6–12. [Google Scholar] [CrossRef]
- Carrera-Hernández, L.; Aizpitarte-Pejenaute, E.; Zugazagoitia-Ciarrusta, N.; Goñi-Viguria, R. Patients’ perceptions of sleep in a Critical Care Unit. Enferm. Intensiva 2018, 29, 53–63. [Google Scholar] [CrossRef] [PubMed]
- Boivin, D.B.; Duffy, J.F.; Kronauer, R.E.; Czeisler, C.A. Dose-response relationships for resetting of human circadian clock by light. Nature 1996, 379, 540–542. [Google Scholar] [CrossRef] [PubMed]
- Gronfier, C.; Wright, K.P., Jr.; Kronauer, R.E.; Jewett, M.E.; Czeisler, C.A. Efficacy of a single sequence of intermittent bright light pulses for delaying circadian phase in humans. Am. J. Physiol. Endocrinol. Metab. 2004, 287, E174–E181. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Czeisler, C.; Allan, J.; Strogatz, S.; Ronda, J.; Sanchez, R.; Rios, C.; Freitag, W.; Richardson, G.; Kronauer, R. Bright light resets the human circadian pacemaker independent of the timing of the sleep-wake cycle. Science 1986, 233, 667–671. [Google Scholar] [CrossRef] [Green Version]
- Vincent, J.-L. Give your patient a fast hug (at least) once a day. Crit. Care Med. 2005, 33, 1225–1229. [Google Scholar] [CrossRef]
- Locihová, H.; Axmann, K.; Padyšáková, H.; Fejfar, J. Effect of the use of earplugs and eye mask on the quality of sleep in intensive care patients: A systematic review. J. Sleep Res. 2018, 27, e12607. [Google Scholar] [CrossRef]
- Buysse, D.J. Insomnia. JAMA 2013, 309, 706–716. [Google Scholar] [CrossRef] [Green Version]
- Lewis, S.R.; Pritchard, M.W.; Schofield-Robinson, O.J.; Alderson, P.; Smith, A.F. Melatonin for the promotion of sleep in adults in the intensive care unit. Cochrane Database Syst. Rev. 2018, 5, CD012455. [Google Scholar] [CrossRef]
- Wibrow, B.; Martinez, F.E.; Myers, E.; Chapman, A.; Litton, E.; Ho, K.M.; Regli, A.; Hawkins, D.; Ford, A.; van Haren, F.M.P.; et al. Prophylactic melatonin for delirium in intensive care (Pro-MEDIC): A randomized controlled trial. Intensive Care Med. 2022, 48, 414–425. [Google Scholar] [CrossRef]
- Lockley, S.W.; Brainard, G.C.; Czeisler, C.A. High sensitivity of the human circadian melatonin rhythm to resetting by short wavelength light. J. Clin. Ednocrinol. Metab. 2003, 88, 4502. [Google Scholar] [CrossRef]

| Factors | Count n = 137 | % |
|---|---|---|
| Modifiable | ||
| Noise (staff, alarms, TV) | 69 | 50.4 |
| Lights | 62 | 45.3 |
| Loud talking | 52 | 38.0 |
| Time disorientation | 50 | 36.5 |
| Temperature (too cold/hot) | 41 | 29.9 |
| Bed/pillow | 40 | 29.2 |
| Hungry | 26 | 19.0 |
| Visitors | 18 | 13.1 |
| Bathing | 7 | 5.1 |
| Potentially Modifiable | ||
| Pain | 64 | 46.7 |
| Thirsty/dry mouth | 61 | 44.5 |
| Discomfort in position | 43 | 31.4 |
| People in room | 34 | 24.8 |
| Touch/move | 28 | 20.4 |
| Medication administration | 27 | 19.7 |
| Absence of partner | 27 | 19.7 |
| Tests/X-rays | 25 | 18.2 |
| Team rounding | 24 | 17.5 |
| Bed inflation and deflation | 14 | 10.2 |
| Restrained/confined | 12 | 8.8 |
| Non-modifiable factors | ||
| IV lines | 58 | 42.3 |
| Anxiety | 44 | 32.1 |
| Procedures/measurements | 42 | 30.7 |
| Confusion | 40 | 29.2 |
| Nightmares/hallucinations | 36 | 26.3 |
| Tubes (nose/rectal/bladder) | 29 | 21.2 |
| Not being tired | 24 | 17.5 |
| Other patients | 21 | 15.3 |
| Suctioning | 18 | 13.1 |
| Endotracheal tube | 17 | 12.4 |
| Breathing machine | 13 | 9.5 |
| Sleep disorder | 4 | 2.9 |
| Factors | Count n = 137 | % |
|---|---|---|
| Easy to Implement | ||
| Dimmed light | 80 | 58.4 |
| Sleeping pill | 71 | 51.8 |
| Closing doors/blinds at night | 58 | 42.3 |
| Personal pillow/keepsake | 49 | 35.8 |
| Clock in the room | 48 | 35.0 |
| Ear plugs | 43 | 31.4 |
| Relaxation techniques | 43 | 31.4 |
| Eye mask/blindfolds | 34 | 24.8 |
| Music therapy | 34 | 24.8 |
| White noise | 30 | 21.9 |
| More blankets | 28 | 20.4 |
| Potentially Implementable | ||
| Pain/more pain medication | 48 | 35.0 |
| Removal of monitors/alarms | 47 | 34.3 |
| No interruptions/unnecessary interruptions | 41 | 29.9 |
| Different bed | 34 | 24.8 |
| Window in room (if none) | 16 | 11.7 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martinez, F.E.; Poulter, A.-L.; Seneviratne, C.; Chrimes, A.; Havill, K.; Balogh, Z.J.; Paech, G.M. ICU Patients’ Perception of Sleep and Modifiable versus Non-Modifiable Factors That Affect It: A Prospective Observational Study. J. Clin. Med. 2022, 11, 3725. https://doi.org/10.3390/jcm11133725
Martinez FE, Poulter A-L, Seneviratne C, Chrimes A, Havill K, Balogh ZJ, Paech GM. ICU Patients’ Perception of Sleep and Modifiable versus Non-Modifiable Factors That Affect It: A Prospective Observational Study. Journal of Clinical Medicine. 2022; 11(13):3725. https://doi.org/10.3390/jcm11133725
Chicago/Turabian StyleMartinez, F. Eduardo, Amber-Louise Poulter, Charuni Seneviratne, Abbey Chrimes, Kenneth Havill, Zsolt J. Balogh, and Gemma M. Paech. 2022. "ICU Patients’ Perception of Sleep and Modifiable versus Non-Modifiable Factors That Affect It: A Prospective Observational Study" Journal of Clinical Medicine 11, no. 13: 3725. https://doi.org/10.3390/jcm11133725
APA StyleMartinez, F. E., Poulter, A.-L., Seneviratne, C., Chrimes, A., Havill, K., Balogh, Z. J., & Paech, G. M. (2022). ICU Patients’ Perception of Sleep and Modifiable versus Non-Modifiable Factors That Affect It: A Prospective Observational Study. Journal of Clinical Medicine, 11(13), 3725. https://doi.org/10.3390/jcm11133725







