Efficacy of Robot-Assisted Gait Training Combined with Robotic Balance Training in Subacute Stroke Patients: A Randomized Clinical Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants’ Recruitment
2.2. Randomization
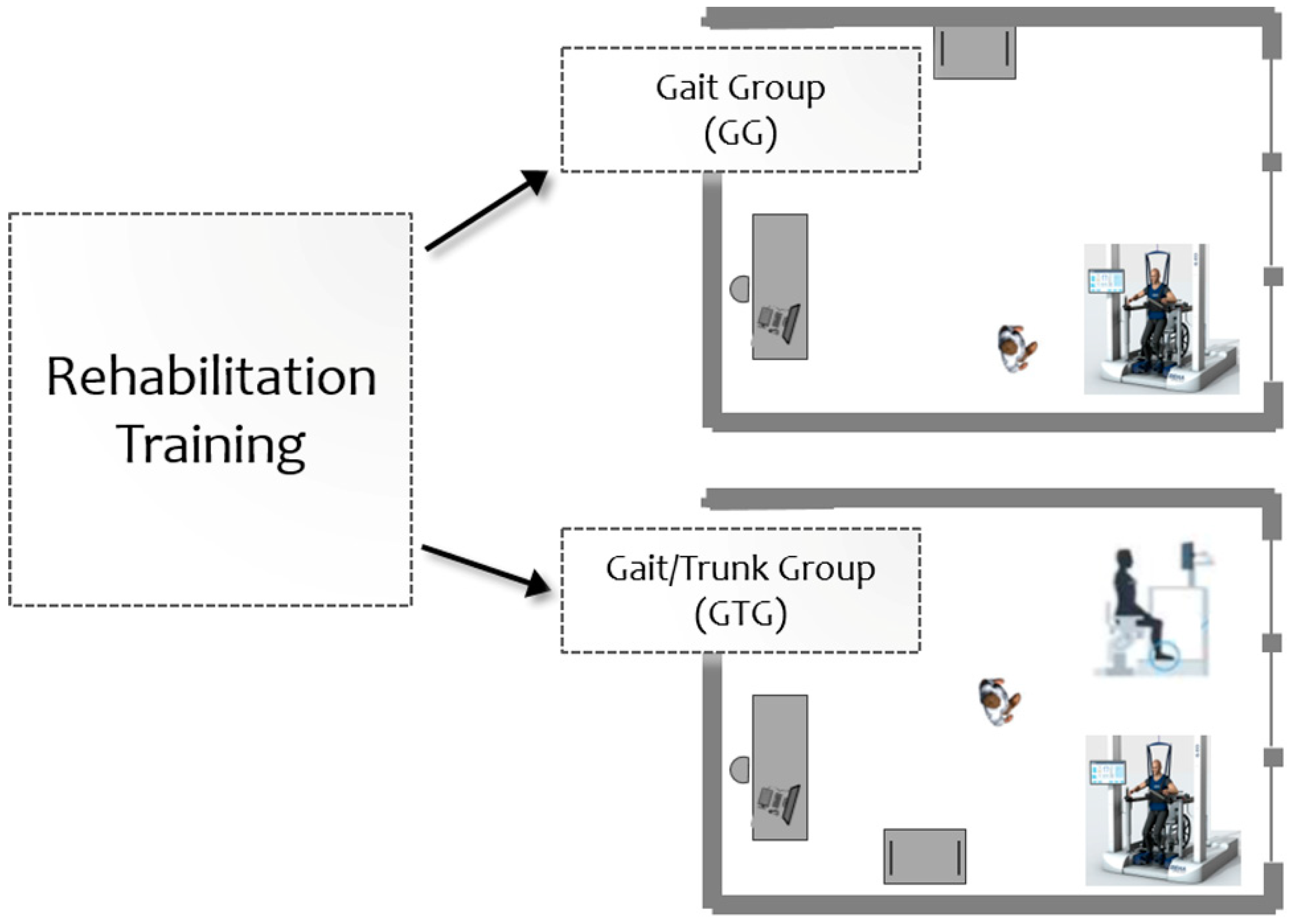
2.3. Therapeutic Interventions
- Exercises in static mode with the blocked “seat platform” or “floor platform” where the patient is positioned as still as possible in the Closed Eyes (CE) and Open Eyes (OE) condition;
- Exercises in dynamic mode with the unblocked “seat platform” or “floor platform” where the patient is positioned as still as possible;
- Exercises in dynamic mode (the “seat platform” or “floor platform are unblocked along one or more axis).
2.4. Clinical Evaluation and Instrumental Assessments
2.5. Safety and Possible Side-Effects during Study Participation
2.6. Statistical Analysis
3. Results
3.1. Sample
3.2. Clinical Outcomes
3.3. Instrumental Outcomes
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Palmieri, L.; Barchielli, A.; Cesana, G.; de Campora, E.; Goldoni, C.A.; Spolaore, P.; Uguccioni, M.; Vancheri, F.; Vanuzzo, D.; Ciccarelli, P.; et al. The Italian Register of Cardiovascular Diseases: Attack Rates and Case Fatality for Cerebrovascular Events. Cereb. Dis. 2007, 24, 530–539. [Google Scholar] [CrossRef] [PubMed]
- Swinnen, E.; Beckwée, D.; Meeusen, R.; Baeyens, J.P.; Kerckhofs, E. Does Robot-Assisted Gait Rehabilitation Improve Balance in Stroke Patients? A Systematic Review. Top. Stroke Rehabil. 2014, 21, 87–100. [Google Scholar] [CrossRef] [PubMed]
- Langhorne, P.; Sandercock, P.; Prasad, K. Evidence-Based Practice for Stroke. Lancet Neurol. 2009, 8, 308–309. [Google Scholar] [CrossRef]
- Pournajaf, S.; Goffredo, M.; Agosti, M.; Massucci, M.; Ferro, S.; Franceschini, M. Community Ambulation of Stroke Survivors at 6 Months Follow-up: An Observational Study on Sociodemographic and Sub-Acute Clinical Indicators. Eur. J. Phys. Rehabil. Med. 2019, 55, 433–441. [Google Scholar] [CrossRef]
- Aprile, I.; Di Stasio, E.; Romitelli, F.; Lancellotti, S.; Caliandro, P.; Tonali, P.; Gilardi, A.; Padua, L. Effects of Rehabilitation on Quality of Life in Patients with Chronic Stroke. Brain Inj. 2008, 22, 451–456. [Google Scholar] [CrossRef] [PubMed]
- Aprile, I.; Di Stasio, E.; Tonali, P.; Padua, L.; Piazzini, D.B.; Bertolini, C. Long-Term Outcome after Stroke Evaluating Health-Related Quality of Life Using Utility Measurement. Stroke 2006, 37, 2218–2219. [Google Scholar] [CrossRef][Green Version]
- Tang, A.; Eng, J.J. Physical Fitness Training After Stroke. Phys. Ther. 2014, 94, 9–13. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Park, J.; Kim, T.H. The Effects of Balance and Gait Function on Quality of Life of Stroke Patients. NeuroRehabilitation 2019, 44, 37–41. [Google Scholar] [CrossRef]
- Vostrý, M.; Zilcher, L. Combined therapy for patients after ischemic stroke from the point view of comprehensive rehabilitation. J. Educ. Cult. Soc. 2020, 11, 119–125. [Google Scholar] [CrossRef]
- Vostrý, M.; Fischer, S.; Cmorej, P.C.; Nesvadba, M.; Peřan, D.; Šín, R. Combined Therapy for Patients after Ischemic Stroke as a Support of Social Adaptability. Neuroendocr. Lett 2019, 40, 32304370–32407819. [Google Scholar]
- Morone, G.; Bragoni, M.; Iosa, M.; De Angelis, D.; Venturiero, V.; Coiro, P.; Pratesi, L.; Paolucci, S. Who May Benefit from Robotic-Assisted Gait Training?: A Randomized Clinical Trial in Patients with Subacute Stroke. Neurorehabil Neural Repair 2011, 25, 636–644. [Google Scholar] [CrossRef] [PubMed]
- Mehrholz, J.; Thomas, S.; Elsner, B. Treadmill Training and Body Weight Support for Walking after Stroke. Cochrane Database of Syst. Rev. 2017, 2017. [Google Scholar] [CrossRef] [PubMed]
- Pons, J.L. Wearable Robots: Biomechatronic Exoskeletons; Wiley: Hoboken, NJ, USA, 2008; ISBN 9780470512944. [Google Scholar]
- Kelley, C.P.; Childress, J.; Boake, C.; Noser, E.A. Over-Ground and Robotic-Assisted Locomotor Training in Adults with Chronic Stroke: A Blinded Randomized Clinical Trial. In Proceedings of the Disability and Rehabilitation: Assistive Technology; Taylor & Francis: Abingdon, UK, 2013; Volume 8, pp. 161–168. [Google Scholar]
- Bonnyaud, C.; Zory, R.; Boudarham, J.; Pradon, D.; Bensmail, D.; Roche, N. Effect of a Robotic Restraint Gait Training versus Robotic Conventional Gait Training on Gait Parameters in Stroke Patients. Expe. Brain Res. 2014, 232, 31–42. [Google Scholar] [CrossRef]
- Li, L.; Ding, L.; Chen, N.; Mao, Y.; Huang, D.; Li, L. Improved Walking Ability with Wearable Robot-Assisted Training in Patients Suffering Chronic Stroke1. Biomed. Mater. Eng. 2015, 26, S329–S340. [Google Scholar] [CrossRef]
- Lonini, L.; Shawen, N.; Scanlan, K.; Rymer, W.Z.; Kording, K.P.; Jayaraman, A. Accelerometry-Enabled Measurement of Walking Performance with a Robotic Exoskeleton: A Pilot Study. J. Neuroeng. Rehabil. 2016, 13, 35. [Google Scholar] [CrossRef] [PubMed]
- Sale, P.; Russo, E.F.; Russo, M.; Masiero, S.; Piccione, F.; Calabrò, R.S.; Filoni, S. Effects on Mobility Training and De-Adaptations in Subjects with Spinal Cord Injury Due to a Wearable Robot: A Preliminary Report. BMC Neurol. 2016, 16, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Goffredo, M.; Guanziroli, E.; Pournajaf, S.; Gaffuri, M.; Gasperini, G.; Filoni, S.; Baratta, S.; Damiani, C.; Franceschini, M.; Molteni, F. Overground Wearable Powered Exoskeleton for Gait Training in Subacute Stroke Subjects: Clinical and Gait Assessments. Eur. J. Phys. Rehabil. Med. 2019, 55, 710–721. [Google Scholar] [CrossRef]
- Cho, M.K.; Kim, J.H.; Chung, Y.; Hwang, S. Treadmill Gait Training Combined with Functional Electrical Stimulation on Hip Abductor and Ankle Dorsiflexor Muscles for Chronic Hemiparesis. Gait Posture 2015, 42, 73–78. [Google Scholar] [CrossRef]
- Aprile, I.; Iacovelli, C.; Padua, L.; Galafate, D.; Criscuolo, S.; Gabbani, D.; Cruciani, A.; Germanotta, M.; di Sipio, E.; de Pisi, F.; et al. Efficacy of Robotic-Assisted Gait Training in Chronic Stroke Patients: Preliminary Results of an Italian Bi-Centre Study. NeuroRehabilitation 2017, 41, 775–782. [Google Scholar] [CrossRef]
- Dundar, U.; Toktas, H.; Solak, O.; Ulasli, A.; Eroglu, S. A Comparative Study of Conventional Physiotherapy versus Robotic Training Combined with Physiotherapy in Patients with Stroke. Top. Stroke Rehabil. 2014, 21, 453–461. [Google Scholar] [CrossRef]
- Hornby, T.G.; Campbell, D.D.; Kahn, J.H.; Demott, T.; Moore, J.L.; Roth, H.R. Enhanced Gait-Related Improvements after Therapist- versus Robotic-Assisted Locomotor Training in Subjects with Chronic Stroke: A Randomized Controlled Study. Stroke 2008, 39, 1786–1792. [Google Scholar] [CrossRef] [PubMed]
- Cattaneo, D.; Gervasoni, E.; Pupillo, E.; Bianchi, E.; Aprile, I.; Imbimbo, I.; Russo, R.; Cruciani, A.; Turolla, A.; Jonsdottir, J.; et al. Educational and Exercise Intervention to Prevent Falls and Improve Participation in Subjects With Neurological Conditions: The NEUROFALL Randomized Controlled Trial. Front. Neurol. 2019, 10, 865. [Google Scholar] [CrossRef] [PubMed]
- Beghi, E.; Gervasoni, E.; Pupillo, E.; Bianchi, E.; Montesano, A.; Aprile, I.; Agostini, M.; Rovaris, M.; Cattaneo, D.; Iacobone, G.; et al. Prediction of Falls in Subjects Suffering From Parkinson Disease, Multiple Sclerosis, and Stroke. Arch. Phys. Med. Rehabil. 2018, 99, 641–651. [Google Scholar] [CrossRef] [PubMed]
- Giovannini, S.; Brau, F.; Galluzzo, V.; Santagada, D.A.; Loreti, C.; Biscotti, L.; Laudisio, A.; Zuccalà, G.; Bernabei, R. Falls among Older Adults: Screening, Identification, Rehabilitation, and Management. Applied Sciences 2022, 12, 7934. [Google Scholar] [CrossRef]
- De Athayde Costa E Silva, A.; Viana Da Cruz Júnior, A.T.; Cardoso Do Nascimento, N.I.; Andrade Candeira, S.R.; Do Socorro Soares Cardoso Almeida, A.; Santana De Castro, K.J.; Costa De Lima, R.; Generoso Campos Pinho Barroso, T.; Da Silva Souza, G.; Callegari, B. Positive Balance Recovery in Ischemic Post-Stroke Patients with Delayed Access to Physical Therapy. Biomed. Res. Int. 2020, 2020, 9153174 . [Google Scholar] [CrossRef]
- Winstein, C.J.; Stein, J.; Arena, R.; Bates, B.; Cherney, L.R.; Cramer, S.C.; Deruyter, F.; Eng, J.J.; Fisher, B.; Harvey, R.L.; et al. Guidelines for Adult Stroke Rehabilitation and Recovery: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke 2016, 47, e98–e169. [Google Scholar] [CrossRef]
- Hobbs, B.; Artemiadis, P. A Review of Robot-Assisted Lower-Limb Stroke Therapy: Unexplored Paths and Future Directions in Gait Rehabilitation. Front. Neurorobot 2020, 14, 19. [Google Scholar] [CrossRef]
- Olenšek, A.; Zadravec, M.; Rudolf, M.; Humar, M.G.; Tomšič, I.; Bizovičar, N.; Goljar, N.; Matjačić, Z. A Novel Approach to Robot-Supported Training of Symmetry, Propulsion and Balance during Walking after Stroke: A Case Study. In Proceedings of the IEEE RAS and EMBS International Conference on Biomedical Robotics and Biomechatronics, Pisa, Italy, 20–22 February 2006; pp. 408–413. [Google Scholar]
- Matjačić, Z.; Zadravec, M.; Olenšek, A. Feasibility of Robot-Based Perturbed-Balance Training during Treadmill Walking in a High-Functioning Chronic Stroke Subject: A Case-Control Study. J. Neuroeng. Rehabil. 2018, 15, 32. [Google Scholar] [CrossRef]
- Saglia, J.A.; De Luca, A.; Squeri, V.; Ciaccia, L.; Sanfilippo, C.; Ungaro, S.; Michieli, L. De Design and Development of a Novel Core, Balance and Lower Limb Rehabilitation Robot: Hunova®. In Proceedings of the IEEE International Conference on Rehabilitation Robotics, Toronto, ON, Canada, 24–28 June 2019; pp. 417–422. [Google Scholar]
- De Luca, A.; Squeri, V.; Barone, L.M.; Vernetti Mansin, H.; Ricci, S.; Pisu, I.; Cassiano, C.; Capra, C.; Lentino, C.; de Michieli, L.; et al. Dynamic Stability and Trunk Control Improvements Following Robotic Balance and Core Stability Training in Chronic Stroke Survivors: A Pilot Study. Front. Neurol. 2020, 11, 494. [Google Scholar] [CrossRef]
- Hesse, S.; Mach, H.; Fröhlich, S.; Behrend, S.; Werner, C.; Melzer, I. An Early Botulinum Toxin A Treatment in Subacute Stroke Patients May Prevent a Disabling Finger Flexor Stiffness Six Months Later: A Randomized Controlled Trial. Clin. Rehabil. 2012, 26, 237–245. [Google Scholar] [CrossRef]
- Paanalahti, M.; Lundgren-Nilsson, Å.; Arndt, A.; Sunnerhagen, K.S. Applying the Comprehensive International Classification of Functioning, Disability and Health Core Sets for Stroke Framework to Stroke Survivors Living in the Community. J. Rehabil. Med. 2013, 45, 331–340. [Google Scholar] [CrossRef] [PubMed]
- Franceschini, M.; Colombo, R.; Posteraro, F.; Sale, P. A Proposal for an Italian Minimum Data Set Assessment Protocol for Robot-Assisted Rehabilitation: A Delphi Study. Eur. J. Phys. Rehabil. Med. 2015, 51, 745–753. [Google Scholar] [CrossRef]
- Aprile, I.; Iacovelli, C.; Goffredo, M.; Cruciani, A.; Galli, M.; Simbolotti, C.; Pecchioli, C.; Padua, L.; Galafate, D.; Pournajaf, S.; et al. Efficacy of End-Effector Robot-Assisted Gait Training in Subacute Stroke Patients: Clinical and Gait Outcomes from a Pilot Bi-Centre Study. NeuroRehabilitation 2019, 45, 201–212. [Google Scholar] [CrossRef] [PubMed]
- Morone, G.; Paolucci, S.; Cherubini, A.; de Angelis, D.; Venturiero, V.; Coiro, P.; Iosa, M. Robot-Assisted Gait Training for Stroke Patients: Current State of the Art and Perspectives of Robotics. Neuropsychiatr. Dis. Treat. 2017, 13, 1303–1311. [Google Scholar] [CrossRef] [PubMed]
- Van Criekinge, T.; Saeys, W.; Vereeck, L.; de Hertogh, W.; Truijen, S. Are Unstable Support Surfaces Superior to Stable Support Surfaces during Trunk Rehabilitation after Stroke? A Systematic Review. Disabil. Rehabil. 2018, 40, 1981–1988. [Google Scholar] [CrossRef] [PubMed]
- Yom, C.; Cho, H.Y.; Lee, B.H. Effects of Virtual Reality-Based Ankle Exercise on the Dynamic Balance, Muscle Tone, and Gait of Stroke Patients. J. Phys. Sci 2015, 27, 845–849. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Thompson, M.; Medley, A. Forward and Lateral Sitting Functional Reach in Younger, Middle-Aged, and Older Adults. J. Geriatr. Phys. 2007, 30, 43–48. [Google Scholar] [CrossRef]
- Masiero, S.; Avesani, R.; Armani, M.; Verena, P.; Ermani, M. Predictive Factors for Ambulation in Stroke Patients in the Rehabilitation Setting: A Multivariate Analysis. Clin. Neurol. Neurosurg. 2007, 109, 763–769. [Google Scholar] [CrossRef]
- Tyson, S.F.; Hanley, M.; Chillala, J.; Selley, A.B.; Tallis, R.C. The Relationship between Balance, Disability, and Recovery after Stroke: Predictive Validity of the Brunel Balance Assessment. Neurorehabil Neural Repair 2007, 21, 341–346. [Google Scholar] [CrossRef]
- Kirker, S.G.B.; Jenner, J.R.; Simpson, D.S.; Wing, A.M. Changing Patterns of Postural Hip Muscle Activity during Recovery from Stroke. Clin. Rehabil. 2000, 14, 618–626. [Google Scholar] [CrossRef]
- Seo, K.C.; Park, S.H.; Park, K. The Effects of Stair Gait Training Using Proprioceptive Neuromuscular Facilitation on Stroke Patients’ Dynamic Balance Ability. J. Phys. Sci. 2015, 27, 1459–1462. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.Y.; Yang, L.; Park, I.J.; Kim, E.J.; Park, M.S.; You, S.H.; Kim, Y.H.; Ko, H.Y.; Shin, Y.I. Effects of Innovative WALKBOT Robotic-Assisted Locomotor Training on Balance and Gait Recovery in Hemiparetic Stroke: A Prospective, Randomized, Experimenter Blinded Case Control Study With a Four-Week Follow-Up. IEEE Trans. Neural. Syst. Rehabil. Eng. 2015, 23, 636–642. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.Y.; Shin, J.H.; Yang, S.P.; Shin, M.A.; Lee, S.H. Robot-Assisted Gait Training for Balance and Lower Extremity Function in Patients with Infratentorial Stroke: A Single-Blinded Randomized Controlled Trial. J. Neuroeng. Rehabil. 2019, 16, 1–12. [Google Scholar] [CrossRef] [PubMed]


| A: Characteristics | |||
| GG | GTG | p-value | |
| n (%) Mean ± SD | |||
| Subjects | 17 (47.20) | 19 (52.80) | |
| Gender. Male/Female | 9 (52.94)/8 (47.06) | 12 (63.16)/7 (36.84) | 0.616 |
| Age (years) | 66.64 ± 9.61 | 66.11 ± 8.76 | 0.778 |
| Time post the acute event (days) | 119.9 ± 38.9 | 134.3 ± 36.1 | 0.129 |
| Aetiology. Ischemic/Haemorrhagic | 9 (52.94)/8 (47.06) | 13 (68.42)/6 (31.58) | 0.265 |
| Lesion Side. Left/Right | 10 (58.82)/7 (41.18) | 10 (52.64)/9 (47.36) | 0.754 |
| B: Clinical Outcomes at T0 | |||
| GG | GTG | p-value | |
| Median [25th;75th percentiles] | |||
| MI-LL | 42 [27–66] | 53 [42–75] | 0.285 |
| MAS-LL | 2 [1–4] | 2 [0–4] | 0.531 |
| FAC | 0 [0–1] | 1 [0–2] | 0.165 |
| TIN-B | 8 [6–9] | 11 [4–14] | 0.219 |
| BBS | 13 [8–27] | 22 [8–38] | 0.452 |
| TCT | 61 [37–62] | 61 [37–74] | 0.639 |
| WHS | 1 [1–1] | 1 [1–2] | 0.066 |
| 10 MWT velocity m/s | 0.44 [0.33–0.67] | 0.30 [0.17–0.42] | 1.000 |
| 6 MWT distance (m) | 117 [44–154] | 72 [25–144] | 0.539 |
| AI | 1 [0–1] | 1 [1–2] | 0.076 |
| TUG time (s) | 24 [16–36] | 29 [22–47] | 0.373 |
| BI | 36 [22–50] | 42 [26–67] | 0.330 |
| NRS | 4 [1–6] | 3 [0–5] | 0.415 |
| ID PAIN | 1 [0–2] | 0 [−1–2] | 0.232 |
| GG | GTG | p Value (%∆_GG vs. GTG) | |||||
|---|---|---|---|---|---|---|---|
| T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | ||
| MI-AD | 14 (9–19) | 14 (9–25) | 0.068 | 14 (14–25) | 25 (14–33) | 0.010 | 0.346 |
| MI-KE | 14 (9–25) | 19 (12–25) | 0.059 | 14 (14–25) | 25 (14–33) | 0.005 | 0.100 |
| MI-HF | 14 (9–25) | 25 (9–25) | 0.126 | 19 (14–25) | 25 (19–33) | 0.011 | 0.433 |
| MI-LL | 42 (27–66) | 58 (32–70) | 0.065 | 53 (42–75) | 72 (47–91) | 0.002 | 0.156 |
| MAS-H | 0 (0–2) | 0 (0–1) | 0.083 | 0 (0–1) | 0 (0–0) | 0.096 | 0.754 |
| MAS-K | 0 (0–1) | 0 (0–1) | 0.582 | 0 (0–1) | 0 (0–0) | 0.038 | 0.490 |
| MAS-A | 1 (0–2) | 1 (1–2) | 0.558 | 1 (0–2) | 1 (0–2) | 0.102 | 0.802 |
| MAS-LL | 2 (1–4) | 2(1–3) | 0.277 | 2 (0–4) | 1 (0–3) | 0.026 | 0.552 |
| FAC | 0 (0–1) | 1 (1–3) | 0.004 | 1 (0–2) | 2 (1–4) | 0.000 | 0.684 |
| TIN-B | 8 (6–9) | 11 (7–14) | 0.021 | 11 (4–14) | 12 (8–16) | 0.004 | 0.975 |
| BBS | 13 (8–27) | 24 (10–36) | 0.007 | 22 (8–38) | 31 (12–48) | 0.003 | 0.900 |
| TCT | 61 (37–62) | 62 (37–80) | 0.018 | 61 (37–74) | 74 (49–100) | 0.009 | 0.778 |
| WHS | 1 (1–1) | 1 (1–2) | 0.010 | 1 (1–2) | 2 (1–4) | 0.020 | 0.616 |
| 10 MWT | 0.44 (0.33–0.67) | 0.49 (0.30–0.75) | 0.500 | 0.30 (0.17–0.42) | 0.37 (0.26–0.53) | 0.575 | 0.093 |
| 6 MWT | 117 (44–154) | 175 (51–328) | 0.068 | 72 (25–144) | 119 (71–195) | 0.007 | 0.839 |
| AI | 1 (0–1) | 3 (1–5) | 0.001 | 1 (1–2) | 3 (3–3) | 0.000 | 0.616 |
| TUG | 24 (16–36) | 17 (7–35) | 0.593 | 29 (22–47) | 21 (14–39) | 0.015 | 1.000 |
| BI | 36 (22–50) | 52 (44–71) | 0.001 | 42 (26–67) | 68 (45–80) | 0.000 | 0.684 |
| NRS | 4 (1–6) | 2 (0–4) | 0.018 | 3 (0–5) | 2 (0–4) | 0.178 | 0.300 |
| ID PAIN | 1 (0–2) | 1 (−0–1) | 0.174 | 0 (−1–2) | 0 (0–1) | 0.796 | 0.397 |
| GG | GTG | p Value (%∆_GG vs. GTG) | |||||
|---|---|---|---|---|---|---|---|
| T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | ||
| CoP sway Area OE [cm2] | 0.2 (0.1–1.2) | 0.2 (0.1–0.5) | 0.756 | 0.2 (0.2–0.5) | 0.2(0.1–1.0) | 0.959 | 0.897 |
| CoP sway Area CE [cm2] | 0.2 (0.0–0.6) | 0.1 (0.05–0.3) | 0.605 | 0.1(0–1.2) | 0.1(0.0–0.4) | 0.469 | 0.669 |
| CoP sway Path OE [cm] | 8.4 (3.5–13.5) | 8.2 (4.4–14.65) | 0.438 | 9.5 (5.5–12.3) | 7.9(6.6–11.9) | 0.796 | 0.287 |
| CoP sway Path CE [cm] | 7.3 (3.4–10.2) | 7.6 (4.3–11.2) | 0.959 | 7.7 (4.0–11.3) | 7.2 (6.0–8.8) | 0.569 | 1.000 |
| Romberg Index | 2.7 (1.6–5.2) | 1.7 (1.1–4.5) | 0.469 | 2.5 (1.5–4.0) | 2.6 (1.2–13.3) | 0.535 | 0.491 |
| CoP Oscillation AP OE [cm] | 0.7 (0.3–1.3) | 0.7 (0.4–1.1) | 0.501 | 0.9 (0.7–1.4) | 0.6 (0.3–1.1) | 0.408 | 0.184 |
| CoP Oscillation AP CE [cm] | 0.5 (0.3–0.8) | 0.6 (0.4–1.2) | 0.234 | 0.9 (0.5–1.9) | 0.7 (0.4–1.7) | 0.352 | 0.184 |
| CoP Oscillation ML OE [cm] | 0.7 (0.3–1.2) | 0.6 (0.4–0.9) | 0.959 | 0.8 (0.5–1.4) | 0.5 (0.4–1.0) | 0.352 | 0.515 |
| CoP Oscillation ML CE [cm] | 0.7 (0.3–1.1) | 0.6 (0.3–0.9) | 0.379 | 0.5 (0.4–1.4) | 0.6 (0.4–0.9) | 0.959 | 0.724 |
| Ellipse axes ratio OE [%] | 45.5 (41.4–61) | 50.7 (34.6–57.3) | 0.756 | 50.1 (32.2–63.6) | 46.0 (40.1–50.4) | 0.569 | 0.809 |
| Ellipse axes ratio CE [%] | 44.0 (36.9–57.6) | 40.7 (28.4–55.8) | 0.234 | 52.5 (46.6–66.3) | 48.5 (40.4–53.8) | 0.109 | 0.616 |
| CoP Mean velocity AP OE [cm/s] | 0. 3 (0.1–0.5) | 0.3 (0.2–0.5) | 0.756 | 0.4 (0.2–0.5) | 0.3 (0.2–0.4) | 0.717 | 0.361 |
| CoP Mean velocity AP CE [cm/s] | 0.3 (0.1–0.4) | 0.3 (0.1–0.4) | 0.836 | 0.3 (0.2–0.5) | 0.3 (0.2–0.3) | 0.650 | 0.402 |
| CoP Mean velocity ML OE [cm/s] | 0.29 (0.17–0.54) | 0.32 (0.21–0.56) | 0.379 | 0.35(0.25–0.47) | 0.32 (0.26–0.54) | 0.600 | 0.047 |
| CoP Mean velocity ML CE [cm/s] | 0.3 (0.2–0.4) | 0.3 (0.2–0.4) | 0.918 | 0.3 (0.2–0.4) | 0.3 (0.2–0.4) | 0.753 | 0.491 |
| Trunk Displacement OE [deg2] | 0.04 (0.03–0.1) | 0.04 (0.03–0.05) | 0.877 | 0.04 (0.03–0.05) | 0.04 (0.03–0.06) | 0.733 | 0.520 |
| Trunk Displacement CE [deg2] | 0.03 (0.03–0.04) | 0.03 (0.03–0.04) | 0.605 | 0.03 (0.03–0.05) | 0.03 (0.03–0.04) | 0.233 | 0.572 |
| Trunk Oscillation AP OE [deg] | 3.0 (1.6–4.0) | 3.3 (2.3–4.3) | 0.918 | 3.4 (2.2–7.4) | 3.3 (1.8–6.5) | 0.691 | 0.545 |
| Trunk Oscillation AP CE [deg] | 2.9 (1.3–3.5) | 3.3 (2.2–5.3) | 0.056 | 2.9 (1.5–5.7) | 3.4 (2.5–4.4) | 0.650 | 0.264 |
| Trunk Oscillation ML OE [deg] | 1.8 (0. 9–4.1) | 2.2 (1.2–4.4) | 0.352 | 1.8 (1.3–2.3) | 2.2 (1.2–3.9) | 0.955 | 0.520 |
| Trunk Oscillation ML CE [deg] | 1.6 (0.9–4.6) | 1.9 (1.2–2.8) | 0.959 | 2.2 (1.0–3.1) | 1.9 (1.4–2.9) | 0.910 | 1.000 |
| GG | GTG | ||||||
|---|---|---|---|---|---|---|---|
| T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | T0 Median (IQR) | T1 Median (IQR) | p Value (T0 vs. T1) | p Value (%∆_GG vs. GTG) | |
| CoP swayArea OE [cm2] | 125.3 (18.5–573.4) | 235.7 (57.6–383.5) | 0.717 | 392.4 (43.2–512.1) | 79.7 (5.6–426.7) | 0.281 | 0.140 |
| CoP swayArea CE [cm2] | 170 (43.7–431.7) | 137.5 (50.2–327.1) | 0.918 | 301.3 (69.3–677.8) | 92 (4.3–248.1) | 0.017 | 0.086 |
| CoP sway Path OE [cm] | 41.3 (21.1–82.4) | 50 (35.8–75.2) | 0.501 | 67.7 (22.1–85.0) | 43 (10.2–72.5) | 0.156 | 0.140 |
| CoP sway Path CE [cm] | 50.8 (28.8–82.2) | 37.4 (29–74.6) | 0.836 | 68 (42.9–99.6) | 31.5 (9.1–72.3) | 0.078 | 0.188 |
| Romberg Index | 1.4 (0.6–3.6) | 3.5 (1.7–5.1) | 0.098 | 2.3 (1.0–5.0) | 1.8 (0.6–4.7) | 0.650 | 0.247 |
| CoP Oscillation AP OE [cm] | 10.7 (5–15.1) | 11.1 (7.4–17.5) | 0.569 | 14.4 (6.8–20.3) | 7.1 (2.5–18.3) | 0.112 | 0.101 |
| CoP Oscillation AP CE [cm] | 9.5 (5.2–18.2) | 11.9 (6.8–15.1) | 1.000 | 14.1 (7.1–17.6) | 7.7 (3.2–10.6) | 0.023 | 0.078 |
| CoP Oscillation ML OE [cm] | 14.3 (6.2–19.8) | 18.4 (10.3–21.2) | 0.501 | 19.7 (9.4–29.3) | 14.1 (2.5–18.3) | 0.012 | 0.072 |
| CoP Oscillation ML CE [cm] | 18.9 (12.3–24.4) | 17 (7.8–24) | 0.756 | 21.8 (9.9–28.2) | 13.5 (3.7–18) | 0.041 | 0.216 |
| Ellipse axes ratio OE [%] | 33.3 (14.3–44.8) | 32.9 (17.7–37.5) | 0.605 | 24.9 (18.6–39.3) | 29.7 (23.2–40.9) | 0.427 | 0.545 |
| Ellipse axes ratio CE [%] | 33.7 (20.1–46.2) | 28.4 (19.3–36.7) | 0.352 | 37.4 (24.9–50.5) | 39.1 (26.3–50.3) | 0.427 | 0.830 |
| CoP Mean velocity AP OE [cm/s] | 1.5 (0.7–2.2) | 1.9 (0.7–2.2) | 0.570 | 1.5 (0.7–2.8) | 1.2 (0.3–2.3) | 0.140 | 0.299 |
| CoP Mean velocity AP CE [cm/s] | 1.2 (0.8–2.2) | 1.4 (0.8–2.4) | 0.865 | 1.7 (0.8–2.6) | 0.9 (0.3–1.5) | 0.036 | 0.140 |
| CoP Mean velocity ML OE [cm/s] | 2.1 (0.6–3.4) | 2.2 (1.2–4) | 0.776 | 2.9 (0.7–4.9) | 2.2 (0.3–3.3) | 0.233 | 0.830 |
| CoP Mean velocity ML CE [cm/s] | 2.4 (1.2–3.3) | 1.8 (0.8–3.2) | 0.820 | 3.1 (2.1–4.0) | 1.4 (0.2–3.9) | 0.125 | 0.599 |
| Trunk Displacement OE [deg2] | 0.12 (0.08–0.20) | 0.12 (0.09–0.14) | 0.379 | 0.123 (0.084–0.204) | 0.120 (0.090–0.141) | 0.009 | 0.131 |
| Trunk Displacement CE [deg2] | 0.09 (0.06–0.14) | 0.09 (0.06–0.13) | 0.326 | 0.092 (0.062–0.140) | 0.091 (0.060–0.138) | 0.004 | 0.038 |
| Trunk Oscillation AP OE [deg] | 12.6 (7–19.2) | 12.8 (8.6–15.3) | 0.535 | 14.6 (6.5–18.5) | 7.1 (3.2–11.6) | 0.006 | 0.038 |
| Trunk Oscillation AP CE [deg] | 11.8 (7–16.4) | 11 (5.6–16.2) | 0.642 | 12.4 (7.6–16.5) | 6 (3.4–10.5) | 0.022 | 0.028 |
| Trunk Oscillation ML OE [deg] | 11.5 (6.9–20.8) | 11.3 (7.5–17) | 0.877 | 12 (9.2–18.3) | 6 (2.3–10.1) | 0.026 | 0.101 |
| Trunk Oscillation ML CE [deg] | 9.6 (6–15.4) | 9.8 (3.9–17.7) | 0.642 | 10.2(6.1–21.9) | 4.9 (2–11.4) | 0.056 | 0.110 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aprile, I.; Conte, C.; Cruciani, A.; Pecchioli, C.; Castelli, L.; Insalaco, S.; Germanotta, M.; Iacovelli, C. Efficacy of Robot-Assisted Gait Training Combined with Robotic Balance Training in Subacute Stroke Patients: A Randomized Clinical Trial. J. Clin. Med. 2022, 11, 5162. https://doi.org/10.3390/jcm11175162
Aprile I, Conte C, Cruciani A, Pecchioli C, Castelli L, Insalaco S, Germanotta M, Iacovelli C. Efficacy of Robot-Assisted Gait Training Combined with Robotic Balance Training in Subacute Stroke Patients: A Randomized Clinical Trial. Journal of Clinical Medicine. 2022; 11(17):5162. https://doi.org/10.3390/jcm11175162
Chicago/Turabian StyleAprile, Irene, Carmela Conte, Arianna Cruciani, Cristiano Pecchioli, Letizia Castelli, Sabina Insalaco, Marco Germanotta, and Chiara Iacovelli. 2022. "Efficacy of Robot-Assisted Gait Training Combined with Robotic Balance Training in Subacute Stroke Patients: A Randomized Clinical Trial" Journal of Clinical Medicine 11, no. 17: 5162. https://doi.org/10.3390/jcm11175162
APA StyleAprile, I., Conte, C., Cruciani, A., Pecchioli, C., Castelli, L., Insalaco, S., Germanotta, M., & Iacovelli, C. (2022). Efficacy of Robot-Assisted Gait Training Combined with Robotic Balance Training in Subacute Stroke Patients: A Randomized Clinical Trial. Journal of Clinical Medicine, 11(17), 5162. https://doi.org/10.3390/jcm11175162










