No Gender Differences in Pain Perception and Medication after Lumbar Spine Sequestrectomy—A Reanalysis of a Randomized Controlled Clinical Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patients
2.2. Pain Medication and Outcomes
2.3. Statistical Analysis
3. Results
3.1. Pain Severity
3.2. Affective and Sensory Pain Perception
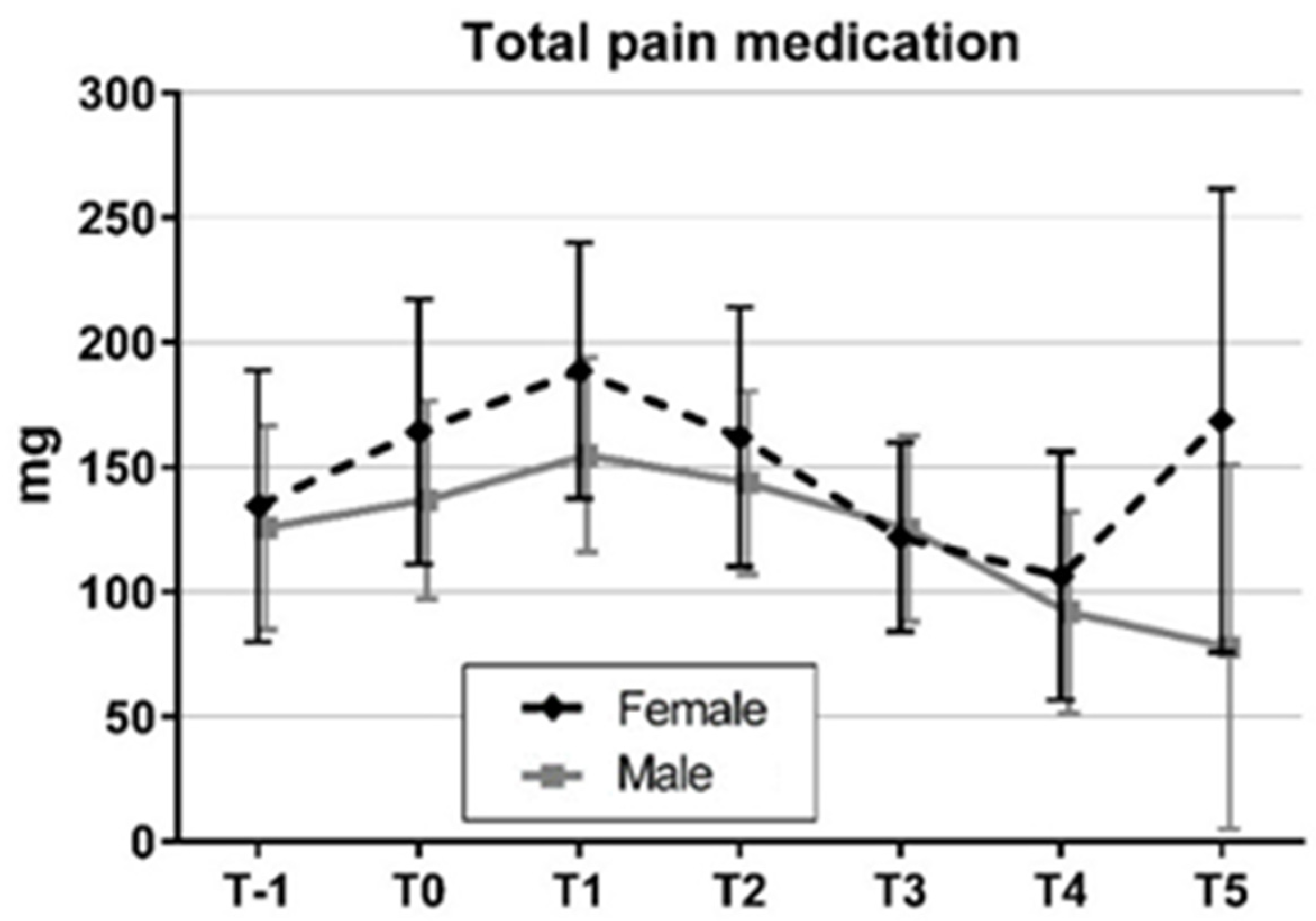
3.3. Pain Medication
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dydyk, A.M.; Ngnitewe Massa, R.; Mesfin, F.B. StatPearls: Disc Herniation; StatPearls Publishing: Treasure Island, FL, USA, 2022. [Google Scholar]
- Fjeld, O.R.; Grøvle, L.; Helgeland, J.; Småstuen, M.C.; Solberg, T.K.; Zwart, J.-A.; Grotle, M. Complications, reoperations, readmissions, and length of hospital stay in 34 639 surgical cases of lumbar disc herniation. Bone Jt. J. 2019, 101-B, 470–477. [Google Scholar] [CrossRef] [PubMed]
- Volbracht, E.; Fürchtenicht, A.; Grote-Westrick, M. Back Surgery: Place of residence determines if patients are admitted to hospital, receive conservative treatment, or undergo an operation. Spotlight Healthc. 2017, 7, 1–8. [Google Scholar]
- Fillingim, R.B.; King, C.D.; Ribeiro-Dasilva, M.C.; Rahim-Williams, B.; Riley, J.L., III. Sex, Gender, and Pain: A Review of Recent Clinical and Experimental Findings. J. Pain 2009, 10, 447–485. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Templeton, K.J. Sex and Gender Issues in Pain Management. J. Bone Jt. Surg. 2020, 102, 32–35. [Google Scholar] [CrossRef]
- Lövgren, A.; Häggman-Henrikson, B.; Fjellman-Wiklund, A.; Begic, A.; Landgren, H.; Lundén, V.; Svensson, P.; Österlund, C. The impact of gender of the examiner on orofacial pain perception and pain reporting among healthy volunteers. Clin. Oral Investig. 2021, 26, 3033–3040. [Google Scholar] [CrossRef]
- Khan, F.A.; Hussain, A.M.; Ahmed, A.; Chawla, T.; Azam, S.I. Effect of gender on pain perception and analgesic consumption in laparoscopic cholecystectomy: An observational study. J. Anaesthesiol. Clin. Pharmacol. 2013, 29, 337–341. [Google Scholar] [CrossRef]
- Pieretti, S.; Di Giannuario, A.; Di Giovannandrea, R.; Marzoli, F.; Piccaro, G.; Minosi, P.; Aloisi, A.M. Gender differences in pain and its relief. Ann. Dell’istituto Super. Di Sanita 2016, 52, 184–189. [Google Scholar] [CrossRef]
- MacLean, M.A.; Touchette, C.J.; Han, J.H.; Christie, S.D.; Pickett, G.E. Gender differences in the surgical management of lumbar degenerative disease: A scoping review. J. Neurosurg. Spine 2020, 32, 799–816. [Google Scholar] [CrossRef]
- Adogwa, O.; Davison, M.A.; Vuong, V.; Desai, S.A.; Lilly, D.T.; Moreno, J.; Cheng, J.; Bagley, C. Sex Differences in Opioid Use in Patients With Symptomatic Lumbar Stenosis or Spondylolisthesis Undergoing Lumbar Decompression and Fusion. Spine 2019, 44, E800–E807. [Google Scholar] [CrossRef]
- Strömqvist, F.; Strömqvist, B.; Jönsson, B.; Karlsson, M.K. Gender differences in patients scheduled for lumbar disc herniation surgery: A National Register Study including 15,631 operations. Eur. Spine J. 2015, 25, 162–167. [Google Scholar] [CrossRef]
- Strömqvist, F.; Strömqvist, B.; Jönsson, B.; Karlsson, M.K. Gender differences in the surgical treatment of lumbar disc herniation in elderly. Eur. Spine J. 2016, 25, 3528–3535. [Google Scholar] [CrossRef] [PubMed]
- Raak, C.K.; Scharbrodt, W.; Berger, B.; Büssing, A.; Schönenberg-Tu, A.; Martin, D.D.; Robens, S.; Ostermann, T. Hypericum perforatum to Improve Postoperative Pain Outcome After Monosegmental Spinal Sequestrectomy (HYPOS): Results of a Randomized, Double-Blind, Placebo-Controlled Trial. J. Integr. Complement. Med. 2022; Advance online publication. [Google Scholar] [CrossRef] [PubMed]
- Raak, C.; Scharbrodt, W.; Berger, B.; Büssing, A.; Geißen, R.; Ostermann, T. Hypericum perforatum to improve post-operative Pain Outcome after monosegmental Spinal microdiscectomy (HYPOS): A study protocol for a randomised, double-blind, placebo-controlled trial. Trials 2018, 19, 253. [Google Scholar] [CrossRef] [PubMed]
- Geissner, E. The Pain Perception Scale—A differentiated and change-sensitive scale for assessing chronic and acute pain. Die Rehabil. 1995, 34, XXXV–XLIII. [Google Scholar]
- Lofrese, G.; Mongardi, L.; Cultrera, F.; Trapella, G.; De Bonis, P. Surgical treatment of intraforaminal/extraforaminal lumbar disc herniations: Many approaches for few surgical routes. Acta Neurochir. 2017, 159, 1273–1281. [Google Scholar] [CrossRef]
- Sedighi, M.; Haghnegahdar, A. Lumbar Disk Herniation Surgery: Outcome and Predictors. Glob. Spine J. 2014, 4, 233–243. [Google Scholar] [CrossRef] [Green Version]
- Dammers, R.; Koehler, P.J. Lumbar disc herniation: Level increases with age. Surg. Neurol. 2002, 58, 209–212. [Google Scholar] [CrossRef]
- Lee, C.-W.; Lo, Y.T.; Devi, S.; Seo, Y.; Simon, A.; Zborovancik, K.; Alsheikh, M.Y.; Lamba, N.; Smith, T.R.; Mekary, R.A.; et al. Gender Differences in Preoperative Opioid Use in Spine Surgery Patients: A Systematic Review and Meta-analysis. Pain Med. 2020, 21, 3292–3300. [Google Scholar] [CrossRef]
- Siccoli, A.; Staartjes, V.E.; De Wispelaere, M.P.; Schröder, M.L. Gender differences in degenerative spine surgery: Do female patients really fare worse? Eur. Spine J. 2018, 27, 2427–2435. [Google Scholar] [CrossRef]
- Patel, D.V.; Yoo, J.S.; Karmarkar, S.S.; Lamoutte, E.H.; Singh, K. Sex Differences on Postoperative Pain and Disability Following Minimally Invasive Lumbar Discectomy. Clin. Spine Surg. A Spine Publ. 2019, 32, E444–E448. [Google Scholar] [CrossRef]
- Zheng, H.; Schnabel, A.; Yahiaoui-Doktor, M.; Meissner, W.; Van Aken, H.; Zahn, P.; Pogatzki-Zahn, E. Age and preoperative pain are major confounders for sex differences in postoperative pain outcome: A prospective database analysis. PLoS ONE 2017, 12, e0178659. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Triebel, J.; Snellman, G.; Sandén, B.; Strömqvist, F.; Robinson, Y. Women do not fare worse than men after lumbar fusion surgery: Two-year follow-up results from 4780 prospectively collected patients in the Swedish National Spine Register with lumbar degenerative disc disease and chronic low back pain. Spine J. 2017, 17, 656–662. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tschugg, A.; Lener, S.; Wildauer, M.; Hartmann, S.; Neururer, S.; Thomé, C.; Löscher, W.N. Gender differences after lumbar sequestrectomy: A prospective clinical trial using quantitative sensory testing. Eur. Spine J. 2016, 26, 857–864. [Google Scholar] [CrossRef] [Green Version]
- Olsen, M.B.; Jacobsen, L.M.; Schistad, E.I.; Pedersen, L.M.; Rygh, L.J.; Røe, C.; Gjerstad, J. Pain Intensity the First Year after Lumbar Disc Herniation Is Associated with the A118G Polymorphism in the Opioid Receptor Mu 1 Gene: Evidence of a Sex and Genotype Interaction. J. Neurosci. 2012, 32, 9831–9834. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kwon, A.H.; Flood, P. Genetics and Gender in Acute Pain and Perioperative Opioid Analgesia. Anesthesiol. Clin. 2020, 38, 341–355. [Google Scholar] [CrossRef]
- Meucci, R.D.; Fassa, A.G.; Faria, N.M.X. Prevalence of chronic low back pain: Systematic review. Rev. Saude Publica 2015, 49, 1. [Google Scholar] [CrossRef]
- Bartley, E.J.; Fillingim, R. Sex differences in pain: A brief review of clinical and experimental findings. Br. J. Anaesth. 2013, 111, 52–58. [Google Scholar] [CrossRef] [Green Version]
- Keogh, E.; Herdenfeldt, M. Gender, coping and the perception of pain. Pain 2002, 97, 195–201. [Google Scholar] [CrossRef]
- Keogh, E.; Eccleston, C. Sex differences in adolescent chronic pain and pain-related coping. Pain 2006, 123, 275–284. [Google Scholar] [CrossRef]
- Donner, N.C.; Lowry, C.A. Sex differences in anxiety and emotional behavior. Pflügers Archiv.-Eur. J. Physiol. 2013, 465, 601–626. [Google Scholar] [CrossRef]
- Racine, M.; Tousignant-Laflamme, Y.; Kloda, L.A.; Dion, D.; Dupuis, G.; Choinière, M. A systematic literature review of 10 years of research on sex/gender and experimental pain perception—Part 1: Are there really differences between women and men? Pain 2012, 153, 602–618. [Google Scholar] [CrossRef] [PubMed]


| Total n = 88 | Female n = 42 | Male n = 46 | p-Value | |
|---|---|---|---|---|
| Age (years) | ||||
| n | 88 | 42 | 46 | |
| M ± SD | 51.57 ± 13.66 | 52.74 ± 12.85 | 50.5 ± 14.42 | 0.446 |
| Median | 53 | 53.5 | 53 | |
| Minimum | 18 | 25 | 18 | |
| Maximum | 82 | 82 | 79 | |
| Surgery duration | ||||
| n | 88 | 42 | 46 | |
| M ± SD | 64.70 ± 24.73 | 60.83 ± 23.35 | 68.24 ± 25.66 | 0.162 |
| Median | 60 | 57.5 | 65 | |
| Minimum | 26 | 26 | 33 | |
| Maximum | 158 | 158 | 133 | |
| BMI | ||||
| n | 86 | 42 | 44 | |
| M ± SD | 27.48 ± 4.67 | 26.93 ± 5.01 | 28.02 ± 4.30 | 0.283 |
| Median | 27.05 | 25.31 | 28.54 | |
| Minimum | 19.13 | 19.13 | 19.15 | |
| Maximum | 40.09 | 40.09 | 38.58 | |
| Level of disc herniation | ||||
| n | 88 | 42 | 46 | |
| L1–L2 | 1 (1.1%) | 1 (2.4%) | 0 (0.0%) | |
| L2–L3 | 5 (5.7%) | 2 (4.8%) | 3 (6.5%) | |
| L3–L4 | 14 (15.9%) | 7 (16.7%) | 7 (15.2%) | 0.828 |
| L4–L5 | 34 (38.6%) | 17 (40.5%) | 17 (37.0%) | |
| L5–S1 | 34 (38.6%) | 15 (35.7%) | 19 (41.3%) | |
| Side | ||||
| n | 88 | 42 | 46 | |
| right | 33 (37.5%) | 15 (35.7%) | 18 (39.1%) | 0.741 |
| left | 55 (62.5%) | 27 (64.3%) | 28 (60.9%) | |
| Location | ||||
| n | 88 | 42 | 46 | |
| exclusively intraforaminal | 2 (2.3%) | 1 (2.4%) | 1 (2.2%) | |
| intra-extraforaminal | 1 (1.1%) | 0 (0.0%) | 1 (2.2%) | 0.629 |
| intraspinal | 85 (96.6%) | 41 (97.6%) | 44 (95.6%) |
| SES-A | Total n = 88 | Female n = 42 | Male n = 46 | t-Test p-Value | |
|---|---|---|---|---|---|
| T-1 | n | 88 | 42 | 46 | |
| M ± SD | 35.60 ± 11.50 | 36.71 ± 12.32 | 34.59 ± 10.74 | 0.389 | |
| Median | 36.00 | 40.00 | 35.50 | ||
| T1 | n | 88 | 42 | 46 | |
| M ± SD | 24.30 ± 10.43 | 24.14 ± 10.24 | 24.43 ± 10.71 | 0.897 | |
| Median | 20.00 | 20.00 | 20.50 | ||
| T3 | n | 87 | 42 | 45 | |
| M ± SD | 20.55 ± 8.61 | 20.14 ± 9.38 | 20.93 ± 7.92 | 0.671 | |
| Median | 17.00 | 16.50 | 18.00 | ||
| T5 | n | 37 | 19 | 18 | |
| M ± SD | 22.81 ± 10.75 | 22.53 ± 11.15 | 23.11 ± 10.62 | 0.871 | |
| Median | 18.00 | 17.00 | 18.50 |
| SES-S | Total n = 88 | Female n = 42 | Male n = 46 | t-Test p-Value | |
|---|---|---|---|---|---|
| T-1 | n | 87 | 41 | 46 | |
| M ± SD | 21.10 ± 7.55 | 21.29 ± 7.35 | 20.93 ± 7.80 | 0.827 | |
| Median | 20.00 | 20.00 | 19.50 | ||
| T1 | n | 86 | 41 | 45 | |
| M ± SD | 16.51 ± 6.70 | 16.63 ± 6.59 | 16.40 ± 6.88 | 0.873 | |
| Median | 14.50 | 14.00 | 15.00 | ||
| T3 | n | 86 | 42 | 44 | |
| M ± SD | 14.06 ± 5.23 | 14.00 ± 5.06 | 14.11 ± 5.44 | 0.920 | |
| Median | 12.00 | 12.00 | 12.00 | ||
| T5 | n | 37 | 19 | 18 | |
| M ± SD | 15.32 ± 6.21 | 15.32 ± 5.53 | 15.33 ± 7.02 | 0.993 | |
| Median | 13.00 | 14.00 | 13.00 |
| Total n = 88 | Female n = 42 | Male n = 46 | t-Test | |
|---|---|---|---|---|
| Sum of day 1 to day 5 | Mean (SD) | Mean (SD) | Mean (SD) | p-value |
| Medication | 569.57 (543.78) | 614.09 (596.95) | 528.92 (498.42) | 0.47 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Raak, C.K.; Ostermann, T.; Schönenberg-Tu, A.-L.; Fricke, O.; Martin, D.D.; Robens, S.; Scharbrodt, W. No Gender Differences in Pain Perception and Medication after Lumbar Spine Sequestrectomy—A Reanalysis of a Randomized Controlled Clinical Trial. J. Clin. Med. 2022, 11, 2333. https://doi.org/10.3390/jcm11092333
Raak CK, Ostermann T, Schönenberg-Tu A-L, Fricke O, Martin DD, Robens S, Scharbrodt W. No Gender Differences in Pain Perception and Medication after Lumbar Spine Sequestrectomy—A Reanalysis of a Randomized Controlled Clinical Trial. Journal of Clinical Medicine. 2022; 11(9):2333. https://doi.org/10.3390/jcm11092333
Chicago/Turabian StyleRaak, Christa K., Thomas Ostermann, Anna-Li Schönenberg-Tu, Oliver Fricke, David D. Martin, Sibylle Robens, and Wolfram Scharbrodt. 2022. "No Gender Differences in Pain Perception and Medication after Lumbar Spine Sequestrectomy—A Reanalysis of a Randomized Controlled Clinical Trial" Journal of Clinical Medicine 11, no. 9: 2333. https://doi.org/10.3390/jcm11092333







