Multidisciplinary Management of Opioid Use–Related Infective Endocarditis: Treatment, QTc Values, and Cardiac Arrests due to Ventricular Fibrillation
Abstract
1. Introduction
2. Materials and Methods
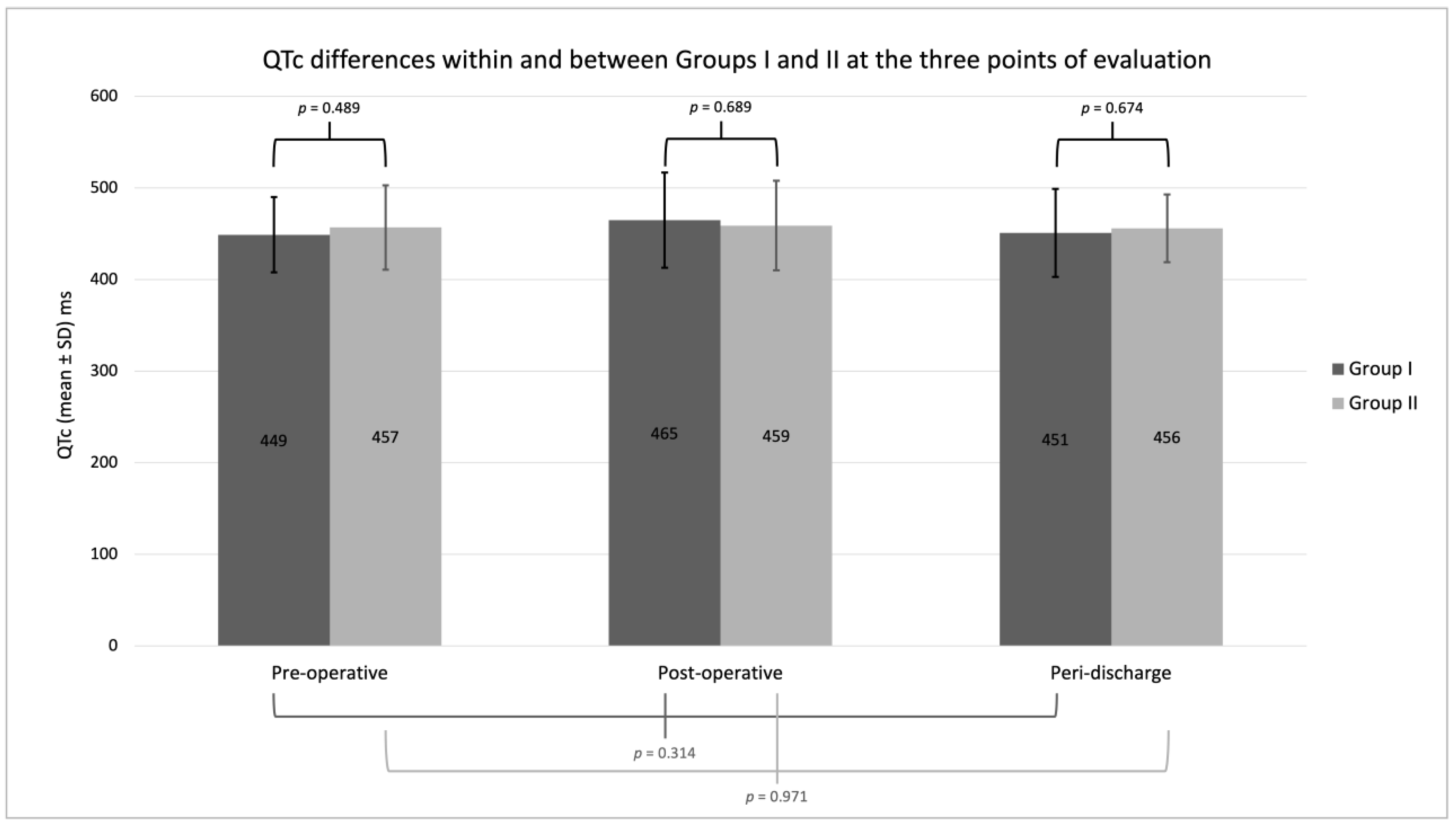
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mattson, C.L.; Tanz, L.J.; Quinn, K.; Kariisa, M.; Patel, P.; Davis, N.L. Trends and geographic patterns in drug and synthetic opioid overdose deaths—United States, 2013–2019. Morb. Mortal. Wkly. Rep. 2021, 70, 202–207. [Google Scholar] [CrossRef] [PubMed]
- Mori, M.; Brown, K.J.; Bin Mahmood, S.U.; Geirsson, A.; Mangi, A.A. Trends in Infective Endocarditis Hospitalizations, Characteristics, and Valve Operations in Patients With Opioid Use Disorders in the United States: 2005–2014. J. Am. Heart Assoc. 2020, 9, e012465. [Google Scholar] [CrossRef] [PubMed]
- Springer, S.A.; Korthuis, P.T.; del Rio, C. Integrating Treatment at the Intersection of Opioid Use Disorder and Infectious Disease Epidemics in Medical Settings: A Call for Action after a National Academies of Sciences, Engineering, and Medicine Workshop. Ann. Intern. Med. 2018, 169, 335–336. [Google Scholar] [CrossRef] [PubMed]
- Weimer, M.B.D.; Falker, C.G.; Seval, N.; Golden, M.; Hull, S.C.M.; Geirsson, A.; Vallabhajosyula, P.M. The Need for Multidisciplinary Hospital Teams for Injection Drug Use-related Infective Endocarditis. J. Addict. Med. 2021, 16, 375–378. [Google Scholar] [CrossRef] [PubMed]
- Quaye, A.N.-A.; Zhang, Y. Perioperative management of buprenorphine: Solving the conundrum. Pain Med. 2019, 20, 1395–1408. [Google Scholar] [CrossRef]
- Pearson, E.C.; Woosley, R.L. QT prolongation and torsades de pointes among methadone users: Reports to the FDA spontaneous reporting system. Pharmacoepidemiol. Drug Saf. 2005, 14, 747–753. [Google Scholar] [CrossRef]
- Wedam, E.F.; Bigelow, G.E.; Johnson, R.E.; Nuzzo, P.A.; Haigney, M.C.P. QT-Interval Effects of Methadone, Levomethadyl, and Buprenorphine in a Randomized Trial. Arch. Intern. Med. 2007, 167, 2469–2475. [Google Scholar] [CrossRef]
- Fareed, A.; Vayalapalli, S.; Scheinberg, K.; Gale, R.; Casarella, J.; Drexler, K. QTc interval prolongation for patients in methadone maintenance treatment: A five years follow-up study. Am. J. Drug Alcohol Abus. 2013, 39, 235–240. [Google Scholar] [CrossRef]
- Titus-Lay, E.N.; Jaynes, H.A.; Muensterman, E.T.; Walroth, T.A.; Ott, C.A.; Desta, Z.; Williams, G.; Moe, P.R.; Wilbrandt, M.; Tisdale, J.E. Methadone-associated QT interval prolongation in patients undergoing maintenance therapy in an urban opioid treatment program. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2020, 41, 238–246. [Google Scholar] [CrossRef]
- Maremmani, I.; Pacini, M.; Cesaroni, C.; Lovrecic, M.; Perugi, G.; Tagliamonte, A. QTc Interval Prolongation in Patients on Long-Term Methadone Maintenance Therapy. Eur. Addict. Res. 2004, 11, 44–49. [Google Scholar] [CrossRef]
- DHQP.CDC/NHSN. CDC/NHSN Surveillance Definitions for Specific Types of Infections Introduction; CDC: Atlanta, GA, USA, 2018. [Google Scholar]
- Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [CrossRef]
- Bogossian, H.; Frommeyer, G.; Ninios, I.; Hasan, F.; Nguyen, Q.S.; Karosiene, Z.; Mijic, D.; Kloppe, A.; Suleiman, H.; Bandorski, D.; et al. New formula for evaluation of the QT interval in patients with left bundle branch block. Heart Rhythm 2014, 11, 2273–2277. [Google Scholar] [CrossRef]
- Tiako, M.J.N.; Mori, M.; Bin Mahmood, S.U.; Shioda, K.; Mangi, A.; Yun, J.; Geirsson, A. Recidivism Is the Leading Cause of Death Among Intravenous Drug Users Who Underwent Cardiac Surgery for Infective Endocarditis. Semin. Thorac. Cardiovasc. Surg. 2019, 31, 40–45. [Google Scholar] [CrossRef]
- Rosenthal, E.S.; Karchmer, A.W.; Theisen-Toupal, J.; Castillo, R.A.; Rowley, C.F. Suboptimal Addiction Interventions for Patients Hospitalized with Injection Drug Use-Associated Infective Endocarditis. Am. J. Med. 2016, 129, 481–485. [Google Scholar] [CrossRef]
- Jo, Y.; Nosal, R.; Vittori, A.; Cordova, L.; Vandever, C.; Alvarez, C.; Bartholomew, T.S.; Tookes, H.E. Effect of initiation of medications for opioid use disorder on hospitalization outcomes for endocarditis and osteomyelitis in a large private hospital system in the United States, 2014–2018. Addiction 2021, 116, 2127–2134. [Google Scholar] [CrossRef]
- Suzuki, J.; Johnson, J.A.; Montgomery, M.W.; Hayden, M.C.; Price, C.N.; Solomon, D.A.; Liebschutz, J.M.; Schnipper, J.L.; Weiss, R.D. Long-term Outcomes of Injection Drug-related Infective Endocarditis Among People Who Inject Drugs. J. Addict. Med. 2020, 14, 282–286. [Google Scholar] [CrossRef]
- Rodger, L.; Glockler-Lauf, S.D.; Shojaei, E.; Sherazi, A.; Hallam, B.; Koivu, S.; Gupta, K.; Hosseini-Moghaddam, S.M.; Silverman, M. Clinical Characteristics and Factors Associated With Mortality in First-Episode Infective Endocarditis Among Persons Who Inject Drugs. JAMA Netw. Open 2018, 1, e185220. [Google Scholar] [CrossRef]
- Kimmel, S.D.; Walley, A.Y.; Li, Y.; Linas, B.P.; Lodi, S.; Bernson, D.; Weiss, R.D.; Samet, J.H.; LaRochelle, M.R. Association of Treatment With Medications for Opioid Use Disorder with Mortality after Hospitalization for Injection Drug Use–Associated Infective Endocarditis. JAMA Netw. Open 2020, 3, e2016228. [Google Scholar] [CrossRef]
- Pani, P.P.; Trogu, E.; Maremmani, I.; Pacini, M. QTc interval screening for cardiac risk in methadone treatment of opioid dependence (Review). Cochrane Database Syst. Rev. 2013, 20, CD008939. [Google Scholar] [CrossRef]
- Vallecillo, G.; Mojal, S.; Roquer, A.; Martinez, D.; Rossi, P.; Fonseca, F.; Muga, R.; Torrens, M. Risk of QTc Prolongation in a Cohort of Opioid-Dependent HIV-Infected Patients on Methadone Maintenance Therapy. Clin. Infect. Dis. 2013, 57, 1189–1194. [Google Scholar] [CrossRef]
- Perrin-Terrin, A.; Pathak, A.; Lapeyre-Mestre, M. QT interval prolongation: Prevalence, risk factors and pharmacovigilance data among methadone-treated patients in France. Fundam. Clin. Pharmacol. 2011, 25, 503–510. [Google Scholar] [CrossRef]
- Tran, P.N.; Sheng, J.; Randolph, A.L.; Baron, C.A.; Thiebaud, N.; Ren, M.; Wu, M.; Johannesen, L.; Volpe, D.A.; Patel, D.; et al. Mechanisms of QT prolongation by buprenorphine cannot be explained by direct hERG channel block. PLoS ONE 2020, 15, e0241362. [Google Scholar] [CrossRef] [PubMed]
- Weimer, M.B.D.; Guerra, M.; Morrow, G.; Adams, K. Hospital-based Buprenorphine Micro-dose Initiation. J. Addict. Med. 2021, 15, 255–257. [Google Scholar] [CrossRef] [PubMed]
- Huntley, G.D.; Deshmukh, A.J.; Warnes, C.A.; Kapa, S.; Egbe, A.C. Longitudinal Outcomes of Epicardial and Endocardial Pacemaker Leads in the Adult Fontan Patient. Pediatr. Cardiol. 2018, 39, 1476–1483. [Google Scholar] [CrossRef]
- Scoblionko, D.P.; Rolett, E.L.; DeTurk, S. Short-Term Threshold Behavior of Human Ventricular Pacing Electrodes: Noninvasive Monitoring with a Multiprogrammable Pacing System. Pacing Clin. Electrophysiol. 1981, 4, 631–637. [Google Scholar] [CrossRef] [PubMed]
| Group I | Group II | p | |
| n = 38 Unique Patients | n = 24 Unique Patients | ||
| Age, Yrs (median, IQR) | 33.5 (29.25–49) | 33.5 (25–43) | 0.699 |
| Gender, Female n, (%) | 8 (21.1) | 10 (41.7) | 0.084 |
| Reduced EF n, (%) | 1 (2.6) | 6 (25) | 0.007 |
| Hepatitis C n, (%) | 26 (68.4) | 16 (66.7) | 0.890 |
| HIV n, (%) | 3 (7.9) | 1 (4.2) | 0.567 |
| Group I | Group II | p | |
| n = 43 IE-CS episodes | n = 24 IE-CS episodes | ||
| Pre-surgery | |||
| Paced Rhythm n, (%) | 3 (6.9) | 2 (8.3) | 1 |
| Methadone n, (%) | 16 (37.2) | 18 (75) | 0.005 |
| Buprenorphine n, (%) | 4 (9.3) | 3 (12.5) | 0.695 |
| Surgery | |||
| Paced Rhythm n, (%) | 5 (11.6) | 6 (25) | 0.31 |
| Methadone n, (%) | 14 (32.6) | 20 (83.3) | <0.001 |
| Buprenorphine n, (%) | 1 (2.3) | 2 (8.3) | 0.29 |
| Peri-discharge | |||
| Paced Rhythm n, (%) | 11 (25.6) | 8 (33.3) | 0.576 |
| Methadone n, (%) | 18 (41.9) | 19 (79.2) | 0.005 |
| Buprenorphine n, (%) | 0 (0) | 4 (16.7) | 0.014 |
| Methadone Dose (mg/day) | Pre-Surgery | Surgery | Peri-Discharge | p (within) |
|---|---|---|---|---|
| Group I (median, IQR) | 70 (40–95) | 65 (30–90) | 85 (30–90) | 0.890 |
| Group II (median, IQR) | 47.5 (30–75) | 47.5 (30–65) | 60 (50–90) | 0.484 |
| p (between) | 0.271 | 0.653 | 0.984 |
| Pts with VF | Pts without VF | |
| n | 6 | 56 |
| Gender, Female, n (%) | 4 (66) | 14 (25) |
| Methadone use *, n (%) | 2 (33) | 34 (61) |
| Buprenorphine use at D/C, n (%) | 0 (0) | 4 (7) |
| Pacemaker issues, n (%) | 3 (50) | 0 (0) |
| Corrected QTc: | PM with VF | PM without VF |
| n = 5 | n = 14 | |
| Pre-surgery cQTc, ms (mean) | 477 | 466 |
| Surgery cQTc, ms (mean) | 484 | 448 |
| Peri-discharge cQTc, ms (mean) | 451 | 414 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rosenfeld, L.E.; Jain, S.; Amabile, A.; Geirsson, A.; Krane, M.; Weimer, M.B. Multidisciplinary Management of Opioid Use–Related Infective Endocarditis: Treatment, QTc Values, and Cardiac Arrests due to Ventricular Fibrillation. J. Clin. Med. 2023, 12, 882. https://doi.org/10.3390/jcm12030882
Rosenfeld LE, Jain S, Amabile A, Geirsson A, Krane M, Weimer MB. Multidisciplinary Management of Opioid Use–Related Infective Endocarditis: Treatment, QTc Values, and Cardiac Arrests due to Ventricular Fibrillation. Journal of Clinical Medicine. 2023; 12(3):882. https://doi.org/10.3390/jcm12030882
Chicago/Turabian StyleRosenfeld, Lynda E., Shashank Jain, Andrea Amabile, Arnar Geirsson, Markus Krane, and Melissa B. Weimer. 2023. "Multidisciplinary Management of Opioid Use–Related Infective Endocarditis: Treatment, QTc Values, and Cardiac Arrests due to Ventricular Fibrillation" Journal of Clinical Medicine 12, no. 3: 882. https://doi.org/10.3390/jcm12030882
APA StyleRosenfeld, L. E., Jain, S., Amabile, A., Geirsson, A., Krane, M., & Weimer, M. B. (2023). Multidisciplinary Management of Opioid Use–Related Infective Endocarditis: Treatment, QTc Values, and Cardiac Arrests due to Ventricular Fibrillation. Journal of Clinical Medicine, 12(3), 882. https://doi.org/10.3390/jcm12030882









