Rehabilitation of Gait and Balance in Cerebral Palsy: A Scoping Review on the Use of Robotics with Biomechanical Implications
Abstract
:1. Introduction
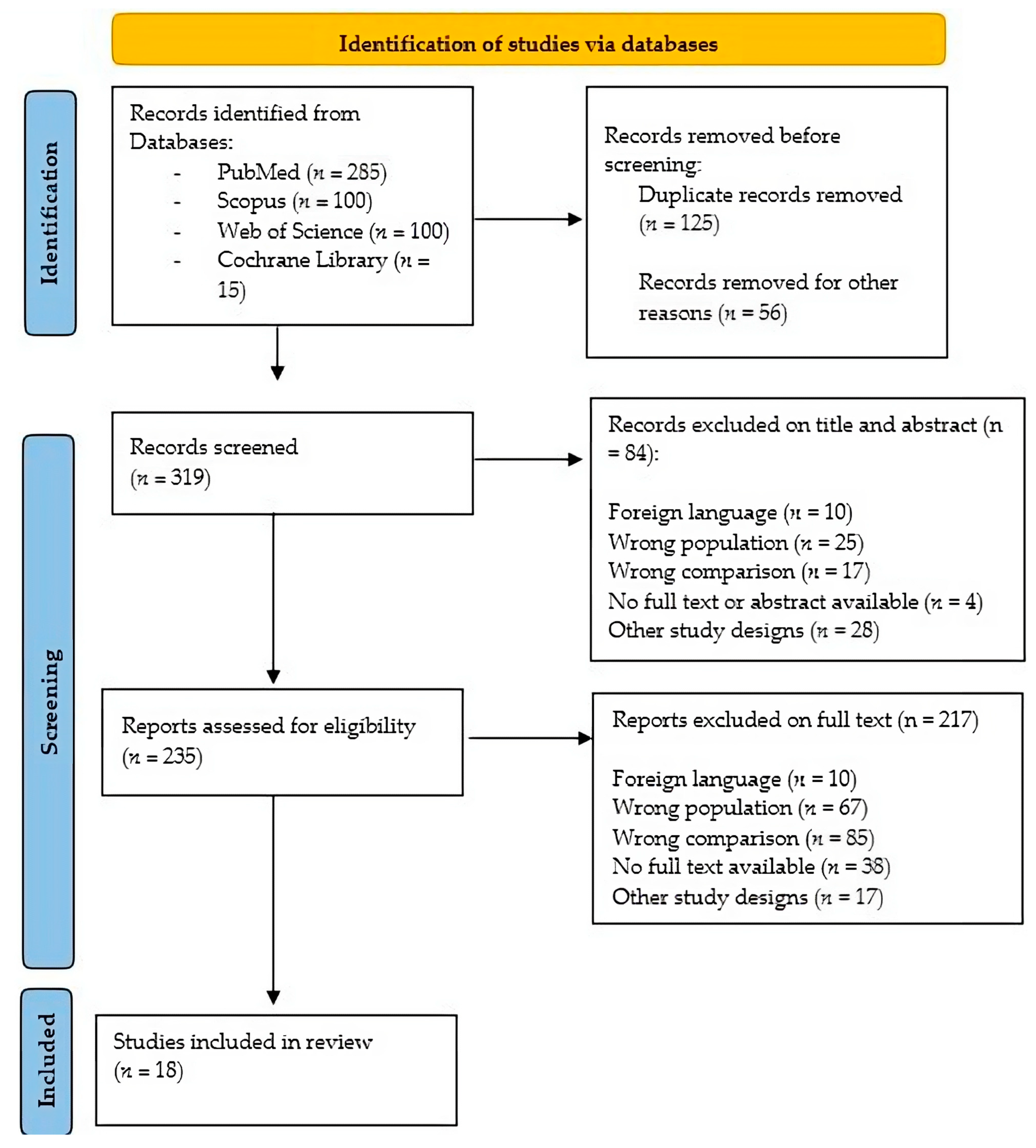
2. Materials and Methods
3. Results
3.1. Trunk Control and Balance Robotic Training
3.2. Robotic Gait Training: A Biomechanical Perspective
4. Discussion
- CP patients with levels I and/or II of GMFCS are characterized by fatigue over long walking distances with mild limitations in gait and balance. They, therefore, could benefit from a treadmill (with or without BWS) and/or Alter G for gait training to improve endurance and gait velocity. VR exercises may further stimulate motivation and longer rehabilitation sessions. In fact, virtual gaming platforms could enhance postural stability, also in patients with ataxic CP.
- In level III, CP patients need more support to walk, especially outside. In this context, wearable exoskeletons, such as the Ekso-GT (Figure 2a), are useful to promote overground walking and autonomy in ambulation (when possible). The motor function can also be improved using the Lokomat, one of the most adaptable robotic tools in neurorehabilitation, thanks to its characteristics (Figure 3) that allow training patients with moderate to severe motor alterations. In addition, Lokomat equipped with a VR screen can provide more challenging training sessions, thus further increasing concentration but also enjoinment.
- CP children between III and IV GMFCS levels present more balance and gait limitations, and the active achievement of an upright position is not always possible. This is why they could benefit from gait training with Innowalk Pro, which supports the patients from sitting to verticalization, in addition to a BWS system. Moreover, exoskeletons like the Lokomat and/or Robogait may help in guaranteeing gait movements in a more passive modality, also reducing efforts for little patients.
- CP patients with level IV present important motor impairments, which tend to confine them to wheelchairs. Then, they could benefit from passive robotic gait training using exoskeletons equipped with BWS (i.e., Lokomat and Robogait), providing constant assistance and monitoring vital signs (blood pressure and oxygen saturation). In addition, the use of HRS with or without VR can be a valid instrument to improve balance functions, postural reactions and abduction hip ROM.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rosenbaum, P.; Paneth, N.; Leviton, A.; Goldstein, M.; Bax, M.; Damiano, D.; Dan, B.; Jacobsson, B. A report: The definition and classification of cerebral palsy April 2006. Dev. Med. Child Neurol. Suppl. 2007, 49, 8–14. [Google Scholar]
- Ophelders, D.R.M.G.; Gussenhoven, R.; Klein, L.; Jellema, R.K.; Westerlaken, R.J.J.; Hütten, M.C.; Vermeulen, J.; Wassink, G.; Gunn, A.G.; Wolfs, T.G.A.M. Preterm Brain Injury, Antenatal Triggers, and Therapeutics: Timing Is Key. Cells 2020, 9, 1871. [Google Scholar] [CrossRef] [PubMed]
- Sheu, J.; Cohen, D.; Sousa, T.; Pham, K.L.D. Cerebral Palsy: Current Concepts and Practices in Musculoskeletal Care. Pediatr. Rev. 2022, 43, 572–581. [Google Scholar] [CrossRef] [PubMed]
- Monica, S.; Nayak, A.; Joshua, A.M.; Mithra, P.; Amaravadi, S.K.; Misri, Z.; Unnikrishnan, B. Relationship between Trunk Position Sense and Trunk Control in Children with Spastic Cerebral Palsy: A Cross-Sectional Study. Rehabil. Res. Pract. 2021, 2021, 9758640. [Google Scholar] [CrossRef]
- Wren, T.A.L.; Rethlefsen, S.; Kay, R.M. Prevalence of specific gait abnormalities in children with cerebral palsy. J. Pediatr. Orthop. 2005, 25, 79–83. [Google Scholar]
- Tracy, J.B.; Petersen, D.A.; Pigman, J.; Conner, B.C.; Wright, H.G.; Modlesky, C.M.; Miller, F.; Johnson, C.L.; Crenshaw, J.R. Dynamic stability during walking in children with and without cerebral palsy. Gait Posture 2019, 72, 182–187. [Google Scholar] [CrossRef]
- Manikowska, F.; Brazevic, S.; Krzyżańska, A.; Jóźwiak, M. Effects of Robot-Assisted Therapy on Gait Parameters in Pediatric Patients with Spastic Cerebral Palsy. Front. Neurol. 2021, 12, 724009. [Google Scholar] [CrossRef]
- Balcı, N.Ç. Current Rehabilitation Methods for Cerebral Palsy. In Cerebral Palsy—Current Steps [Internet]; Gunel, M.K., Ed.; IntechOpen: London, UK, 2016; Available online: https://www.intechopen.com/chapters/51973 (accessed on 11 November 2022).
- Ungureanu, A.; Rusu, L.; Rusu, M.R.; Marin, M.I. Balance Rehabilitation Approach by Bobath and Vojta Methods in Cerebral Palsy: A Pilot Study. Children 2022, 9, 1481. [Google Scholar] [CrossRef]
- Chen, Y.T.; Zhang, C.; Liu, Y.; Magat, E.; Verduzco-Gutierrez, M.; Francisco, G.E.; Zhou, P.; Zhang, Y.; Li, S. The Effects of Botulinum Toxin Injections on Spasticity and Motor Performance in Chronic Stroke with Spastic Hemiplegia. Toxins 2020, 12, 492. [Google Scholar] [CrossRef]
- Merino-Andrés, J.; García de Mateos-López, A.; Damiano, D.L.; Sánchez-Sierra, A. Effect of muscle strength training in children and adolescents with spastic cerebral palsy: A systematic review and meta-analysis. Clin. Rehabil. 2022, 36, 4–14. [Google Scholar] [CrossRef]
- Bartík, P.; Vostrý, M.; Hudáková, Z.; Šagát, P.; Lesňáková, A.; Dukát, A. The Effect of Early Applied Robot-Assisted Physiotherapy on Functional Independence Measure Score in Post-Myocardial Infarction Patients. Healthcare 2022, 10, 937. [Google Scholar] [CrossRef] [PubMed]
- De Luca, R.; Bonanno, M.; Settimo, C.; Muratore, R.; Calabrò, R.S. Improvement of Gait after Robotic-Assisted Training in Children with Cerebral Palsy: Are We Heading in the Right Direction? Med. Sci. 2022, 10, 59. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef] [PubMed]
- Curtis, D.J.; Woollacott, M.; Bencke, J.; Lauridsen, H.B.; Saavedra, S.; Bandholm, T.; Sonne-Holm, S. The functional effect of segmental trunk and head control training in moderate-to-severe cerebral palsy: A randomized controlled trial. Dev. Neurorehabil. 2018, 21, 91–100. [Google Scholar] [CrossRef] [PubMed]
- Santamaria, V.; Khan, M.; Luna, T.; Kang, J.; Dutkowsky, J.; Gordon, A.M.; Agrawal, S.K. Promoting Functional and Independent Sitting in Children with Cerebral Palsy Using the Robotic Trunk Support Trainer. IEEE Trans. Neural Syst. Rehabil. Eng. 2020, 28, 2995–3004. [Google Scholar] [CrossRef]
- Abidin, N.; Ünlü Akyüz, E.; Cankurtaran, D.; Karaahmet, Ö.Z.; Tezel, N. The effect of robotic rehabilitation on posture and trunk control in non-ambulatory cerebral palsy. Assist. Technol. 2022, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Baronchelli, F.; Zucchella, C.; Serrao, M.; Intiso, D.; Bartolo, M. The Effect of Robotic Assisted Gait Training with Lokomat® on Balance Control After Stroke: Systematic Review and Meta-Analysis. Front. Neurol. 2021, 12, 661815. [Google Scholar] [CrossRef]
- Rasooli, A.H.; Birgani, P.M.; Azizi, S.; Shahrokhi, A.; Mirbagheri, M.M. Therapeutic effects of an anti-gravity locomotor training (AlterG) on postural balance and cerebellum structure in children with Cerebral Palsy. IEEE Int. Conf. Rehabil. Robot. 2017, 2017, 101–105. [Google Scholar]
- Azizi, S.; Rasooli, A.H.; Soleimani, M.; Irani, A.; Shahrokhi, A.; Mirbagheri, M.M. The impact of AlterG training on balance and structure of vestibulospinal tract in cerebral palsy children. In Proceedings of the 2018 40th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Honolulu, HI, USA, 18–21 July 2018; pp. 2499–2502. [Google Scholar]
- Zadnikar, M.; Kastrin, A. Effects of hippotherapy and therapeutic horseback riding on postural control or balance in children with cerebral palsy: A meta-analysis. Dev. Med. Child Neurol. 2011, 53, 684–691. [Google Scholar] [CrossRef]
- Dominguez-Romero, J.G.; Molina-Aroca, A.; Moral-Munoz, J.A.; Luque-Moreno, C.; Lucena-Anton, D. Effectiveness of Mechanical Horse-Riding Simulators on Postural Balance in Neurological Rehabilitation: Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2019, 17, 165. [Google Scholar] [CrossRef]
- Choi, H.J.; Kim, K.J.; Nam, K.W. The Effects of a Horseback Riding Simulation Exercise on the Spinal Alignment of Children with Cerebral Palsy. J. Korean Soc. Phys. Ther. 2014, 26, 209–215. [Google Scholar]
- Sterba, J.A. Does horseback riding therapy or therapist-directed hippotherapy rehabilitate children with cerebral palsy? Dev. Med. Child Neurol. 2007, 49, 68–73. [Google Scholar] [CrossRef]
- Yoo, J.H.; Kim, S.E.; Lee, M.G.; Jin, J.J.; Hong, J.; Choi, Y.T.; Kim, M.H.; Jee, Y.S. The effect of horse simulator riding on visual analogue scale, body composition and trunk strength in the patients with chronic low back pain. Int. J. Clin. Pract. 2014, 68, 941–949. [Google Scholar] [CrossRef]
- Sung, Y.H.; Kim, C.J.; Yu, B.K.; Kim, K.M. A hippotherapy simulator is effective to shift weight bearing toward the affected side during gait in patients with stroke. NeuroRehabilitation 2013, 33, 407–412. [Google Scholar] [CrossRef]
- Park, J.H.; You, J.S.H. Innovative robotic hippotherapy improves postural muscle size and postural stability during the quiet stance and gait initiation in a child with cerebral palsy: A single case study. NeuroRehabilitation 2018, 42, 247–253. [Google Scholar] [CrossRef]
- Hemachithra, C.; Meena, N.; Ramanathan, R.; Felix, A.J.W. Immediate effect of horse riding simulator on adductor spasticity in children with cerebral palsy: A randomized controlled trial. Physiother. Res. Int. 2020, 25, e1809. [Google Scholar] [CrossRef]
- Jung, Y.G.; Chang, H.J.; Jo, E.S.; Kim, D.H. The Effect of a Horse-Riding Simulator with Virtual Reality on Gross Motor Function and Body Composition of Children with Cerebral Palsy: Preliminary Study. Sensors 2022, 22, 2903. [Google Scholar] [CrossRef]
- Tsitlakidis, S.; Horsch, A.; Schaefer, F.; Westhauser, F.; Goetze, M.; Hagmann, S.; Klotz, M.C.M. Gait Classification in Unilateral Cerebral Palsy. J. Clin. Med. 2019, 8, 1652. [Google Scholar] [CrossRef]
- Molteni, F.; Gasperini, G.; Cannaviello, G.; Guanziroli, E. Exoskeleton and End-Effector Robots for Upper and Lower Limbs Rehabilitation: Narrative Review. PM&R 2018, 10 (Suppl. S2), S174–S188. [Google Scholar]
- Žarković, D.; Šorfová, M.; Tufano, J.J.; Kutílek, P.; Vítečková, S.; Ravnik, D.; Groleger-Sršen, K.; Cikajlo, I.; Otáhal, J. Gait changes following robot-assisted gait training in children with cerebral palsy. Physiol. Res. 2021, 70, S397–S408. [Google Scholar] [CrossRef]
- Wallard, L.; Dietrich, G.; Kerlirzin, Y.; Bredin, J. Effect of robotic-assisted gait rehabilitation on dynamic equilibrium control in the gait of children with cerebral palsy. Gait Posture 2018, 60, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Conner, B.C.; Remec, N.M.; Lerner, Z.F. Is robotic gait training effective for individuals with cerebral palsy? A systematic review and meta-analysis of randomized controlled trials. Clin. Rehabil. 2022, 36, 873–882. [Google Scholar] [CrossRef] [PubMed]
- Yazıcı, M.; Livanelioğlu, A.; Gücüyener, K.; Tekin, L.; Sümer, E.; Yakut, Y. Effects of robotic rehabilitation on walking and balance in pediatric patients with hemiparetic cerebral palsy. Gait Posture 2019, 70, 397–402. [Google Scholar] [CrossRef] [PubMed]
- Sucuoglu, H. Effects of robot-assisted gait training alongside conventional therapy on the development of walking in children with cerebral palsy. J. Pediatr. Rehabil. Med. 2020, 13, 127–135. [Google Scholar] [CrossRef]
- Baud, R.; Manzoori, A.R.; Ijspeert, A.; Bouri, M. Review of control strategies for lower-limb exoskeletons to assist gait. J. Neuroeng. Rehabil. 2021, 18, 119. [Google Scholar] [CrossRef]
- Hunt, M.; Everaert, L.; Brown, M.; Muraru, L.; Hatzidimitriadou, E.; Desloovere, K. Effectiveness of robotic exoskeletons for improving gait in children with cerebral palsy: A systematic review. Gait Posture 2022, 98, 343–354. [Google Scholar] [CrossRef]
- Hong, J.; Lee, J.; Choi, T.; Choi, W.; Kim, T.; Kwak, K.; Kim, S.; Kim, K.; Kim, D. Feasibility of Overground Gait Training Using a Joint-Torque-Assisting Wearable Exoskeletal Robot in Children with Static Brain Injury. Sensors 2022, 22, 3870. [Google Scholar] [CrossRef]
- Kawasaki, S.; Ohata, K.; Yoshida, T.; Yokoyama, A.; Yamada, S. Gait improvements by assisting hip movements with the robot in children with cerebral palsy: A pilot randomized controlled trial. J. Neuroeng. Rehabil. 2020, 17, 87. [Google Scholar] [CrossRef]
- Cherni, Y.; Ballaz, L.; Lemaire, J.; Dal Maso, F.; Begon, M. Effect of low dose robotic-gait training on walking capacity in children and adolescents with cerebral palsy. Neurophysiol. Clin. 2020, 50, 507–519. [Google Scholar] [CrossRef]
- Llamas-Ramos, R.; Sánchez-González, J.L.; Llamas-Ramos, I. Robotic Systems for the Physiotherapy Treatment of Children with Cerebral Palsy: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 5116. [Google Scholar] [CrossRef]
- McCrum, C.; Bhatt, T.S.; Gerards, M.H.G.; Karamanidis, K.; Rogers, M.W.; Lord, S.R.; Okubo, Y. Perturbation-based balance training: Principles, mechanisms and implementation in clinical practice. Front. Sports Act. Living 2022, 4, 1015394. [Google Scholar] [CrossRef] [PubMed]
- Cho, C.; Hwang, W.; Hwang, S.; Chung, Y. Treadmill Training with Virtual Reality Improves Gait, Balance, and Muscle Strength in Children with Cerebral Palsy. Tohoku J. Exp. Med. 2016, 238, 213–218. [Google Scholar] [CrossRef] [PubMed]
- Fu, W.S.; Song, Y.C.; Wu, B.A.; Qu, C.H.; Zhao, J.F. Virtual reality combined with robot-assisted gait training to improve walking ability of children with cerebral palsy: A randomized controlled trial. Technol. Health Care 2022, 30, 1525–1533. [Google Scholar] [CrossRef]
- Calabrò, R.S.; Müller-Eising, C.; Diliberti, M.L.; Manuli, A.; Parrinello, F.; Rao, G.; Barone, V.; Civello, T. Who Will Pay for Robotic Rehabilitation? The Growing Need for a Cost-effectiveness Analysis. Innov. Clin. Neurosci. 2020, 17, 14–16. [Google Scholar]
- Pavel, M.; Jimison, H.B.; Wactlar, H.D.; Hayes, T.L.; Barkis, W.; Skapik, J.; Kaye, J. The role of technology and engineering models in transforming healthcare. IEEE Rev. Biomed. Eng. 2013, 6, 156–177. [Google Scholar] [CrossRef] [PubMed]
- Volpini, M.; Bartenbach, V.; Pinotti, M.; Riener, R. Clinical evaluation of a low-cost robot for use in physiotherapy and gait training. J. Rehabil. Assist. Technol. Eng. 2017, 4, 2055668316688410. [Google Scholar] [CrossRef]
- Elbanna, S.T.; Elshennawy, S.; Ayad, M.N. Noninvasive Brain Stimulation for Rehabilitation of Pediatric Motor Disorders Following Brain Injury: Systematic Review of Randomized Controlled Trials. Arch. Phys. Med. Rehabil. 2019, 100, 1945–1963. [Google Scholar] [CrossRef] [PubMed]
- Tugui, R.D.; Antonescu, D. Cerebral palsy gait, clinical importance. Maedica 2013, 8, 388–393. [Google Scholar] [PubMed]
- Collantes, I.; Asin, G.; Moreno, J.C.; Pons, J.L. Analysis of biomechanical data to determine the degree of users participation during robotic-assisted gait rehabilitation. In Proceedings of the 2012 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Diego, CA, USA, 28 August–1 September 2012; pp. 4855–4858. [Google Scholar]
- Drużbicki, M.; Rusek, W.; Szczepanik, M.; Dudek, J.; Snela, S. Assessment of the impact of orthotic gait training on balance in children with cerebral palsy. Acta Bioeng. Biomech. 2010, 12, 53–58. [Google Scholar]
- Ma, Y.; Liang, Y.; Kang, X.; Shao, M.; Siemelink, L.; Zhang, Y. Gait Characteristics of Children with Spastic Cerebral Palsy during Inclined Treadmill Walking under a Virtual Reality Environment. Appl. Bionics Biomech. 2019, 2019, 8049156. [Google Scholar] [CrossRef]
- Aycardi, L.F.; Cifuentes, C.A.; Múnera, M.; Bayón, C.; Ramírez, O.; Lerma, S.; Frizera, A.; Rocon, E. Evaluation of biomechanical gait parameters of patients with Cerebral Palsy at three different levels of gait assistance using the CPWalker. J. Neuroeng. Rehabil. 2019, 16, 15. [Google Scholar] [CrossRef]
- Kim, S.K.; Park, D.; Yoo, B.; Shim, D.; Choi, J.O.; Choi, T.Y.; Park, E.S. Overground Robot-Assisted Gait Training for Pediatric Cerebral Palsy. Sensors 2021, 21, 2087. [Google Scholar] [CrossRef]
- Panibatla, S.; Kumar, V.; Narayan, A. Relationship Between Trunk Control and Balance in Children with Spastic Cerebral Palsy: A Cross-Sectional Study. J. Clin. Diagn. Res. 2017, 11, YC05–YC08. [Google Scholar] [CrossRef]
- Vostrý, M.; Lanková, B.; Zilcher, L.; Jelinková, J. The Effect of Individual Combination Therapy on Children with Motor Deficits from the Perspective of Comprehensive Rehabilitation. Appl. Sci. 2022, 12, 4270. [Google Scholar] [CrossRef]


| Reference n° | Robotic Device | Clinical Evaluation | Biomechanical Parameters |
|---|---|---|---|
| Robotic balance training | |||
| 16 | TruST—cable-driven robot which provides assist-as-needed forces. | SP&R-co; BBT; MFRT; | Lower-thorax orientation during sitting (flexion–extension plane) |
| 17 | RAGT (authors not specified the robotic system) | GMFM and TIS | Sitting balance |
| 18 | Lokomat—(description focused on balance) a fixed gait rehabilitation exoskeleton which facilitates a bilateral symmetrical gait, as the individual actively tries to advance each limb, during walking. | BBS, TUG, RMI, mEFAP, MM, PASS, POMA-B, SPPB, RMA | Walking speed and covered distance. |
| 19 | AlterG—it is a treadmill which enables patients to walk/run at low percentage of their body weight, thanks to its microgravity envinronment. | Romberg test and DTI evaluation | Center of Pressure (CoP) |
| 20 | AlterG—mentioned above | BBT, TUG, DTI evaluation | Balance and posture |
| 22 | HRS—is a robotic device with a dynamic saddle. | Stabilometric platform, GMFM, Sitting assessment scale (SAS), BBS, B-POMA, SATCo, Romberg test | Balance, pelvic torsion, and pelvic tilt |
| 23 | Horseback riding simulator JOBA–robotic simulator of horse movement. | NA | Spinal posture: trunk imbalance, pelvic torsion, and pelvic tilt |
| 27 | Robotic HPOT system (FORTIS-102)—This robotic system simulates live horse movements (I.e. walk, trot, and gallop) and the partecipant is instructed to the different patterns of movement. | Ultrasound imaging of EO, IO, TrA, LM. | CoP, CoM |
| 28 | horse riding simulator U-Gallop—indoor exercise equipment, which uses the oscillatory action of the seat to simulate the horse riding experience. | MAS and PROM in hip abduction | NA |
| Robotic assisted gait training evidence | |||
| 13 | Lokomat—(description focused on gait) robotic exoskeleton with active hip–knee actuation and passive ankle control during the swing phase, in addition to a variable level of assistance. | GMFM and Cerebral Palsy Quality of Life Questionnaire (CP QOL) | NA |
| 33 | Lokomat—mentioned above | Clinical gait analysis and GMFM | COP, COM, propulsive forces in anteroposterior and Medio lateral directions |
| 34 | RAGT (authors not specified the robotic devices) | GMFM, 6MWT | Walking speed, |
| 35 | Innowalk Pro—it is an end-effector that supports the user from sitting into a standing position, and provides assisted, guided and repetitive movements in a safe upright, weight-bearing position. | GMFM, 10MWT, 6MWT, standing on one leg test, PBBS, FAQ-WL | Walking speed and endurance, balance, |
| 36 | Robogait— is a fixed lower body hip-knee exoskeleton. The user’s weight is supported by a combination of an overhead attached harness and the support from the exoskeleton. | GMFM and 6MWT | Walking covered distance and gait velocity |
| 38 | tethered knee exoskeleton, pediatric knee exoskeleton (P.REX), untethered ankle exoskeleton, WAKE-Up ankle module, WAKE-Up ankle & knee module and unilateral ankle exosuit— It is not a passive robot but the device can interact actively with patients, correcting also the motor actions on the joint motion; in this way the subject is assisted or less only when requested. | EMG | Walking cadence, stride length and/or step length, gait symmetry, stride to stride vaiability |
| 39 | wearable joint-torque-assisting exoskeletal robot called the Angel Legs M20—wearable walking device that induce proper gait and support of the lower limbs. | GMFM, 6MWT,10MWT, Oxygen consumption | Walking speed |
| 40 | HWA (exoskeleton that assists hip flexion and extension of both limbs during gait)—it detects the gait cycle by the potentiometers (set beside the actuators) and produces flexion and extension torques on swing and stance phases, respectively. | MAS, ROM and MVC of hip flexion, hip extension, knee flexion, knee extension, dorsiflexion, and plantar flexion, GMFM (D and E dimensions), PEDI | Walking speed and gait symmetry |
| 41 | Lokomat—mentioned above. | hand-held dynamometer to test strength of lower limb muscles | Walking speed, cadence, stride length and sagittal joint kinematic gait parameters: pelvis, hip, knee and ankle minimum and maximum angles, as well as range of motion (ROM) during the stance phase. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bonanno, M.; Militi, A.; La Fauci Belponer, F.; De Luca, R.; Leonetti, D.; Quartarone, A.; Ciancarelli, I.; Morone, G.; Calabrò, R.S. Rehabilitation of Gait and Balance in Cerebral Palsy: A Scoping Review on the Use of Robotics with Biomechanical Implications. J. Clin. Med. 2023, 12, 3278. https://doi.org/10.3390/jcm12093278
Bonanno M, Militi A, La Fauci Belponer F, De Luca R, Leonetti D, Quartarone A, Ciancarelli I, Morone G, Calabrò RS. Rehabilitation of Gait and Balance in Cerebral Palsy: A Scoping Review on the Use of Robotics with Biomechanical Implications. Journal of Clinical Medicine. 2023; 12(9):3278. https://doi.org/10.3390/jcm12093278
Chicago/Turabian StyleBonanno, Mirjam, Angela Militi, Francesca La Fauci Belponer, Rosaria De Luca, Danilo Leonetti, Angelo Quartarone, Irene Ciancarelli, Giovanni Morone, and Rocco Salvatore Calabrò. 2023. "Rehabilitation of Gait and Balance in Cerebral Palsy: A Scoping Review on the Use of Robotics with Biomechanical Implications" Journal of Clinical Medicine 12, no. 9: 3278. https://doi.org/10.3390/jcm12093278









