Cardiovascular Risk across Glycemic Categories: Insights from a Nationwide Screening in Mongolia, 2022–2023
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Collection and Study Participants
2.2. Glucose Category Evaluation
2.3. Cardiovascular Disease (CVD) Risk Assessment
2.4. Other Variables
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- do Vale Moreira, N.C.; de Souza, A.M.; Barbosa, L.; de Lima, M.G., Jr.; de Lima, A.A. Prevalence of Metabolic Syndrome by different definitions, and its association with type 2 diabetes, pre-diabetes, and cardiovascular disease risk in Brazil. Diabetes Metab. Syndr. 2020, 14, 1217–1224. [Google Scholar] [CrossRef] [PubMed]
- Sehgal, A.; Goel, S.; Sharma, A.; Kalra, S.; Garg, V.K. A Cross-Sectional Study to Evaluate Cardiovascular Risk Score in Type 2 Diabetes Mellitus. Int. J. Appl. Basic Med. Res. 2020, 10, 213–220. [Google Scholar] [CrossRef] [PubMed]
- Cai, X.; Zhang, Y.; Li, M.; Wu, J.H.; Mai, L.; Li, J.; Yang, Y.; Hu, Y.; Huang, Y. Association between prediabetes and risk of all cause mortality and cardiovascular disease: Updated meta-analysis. BMJ 2020, 370, m2297. [Google Scholar] [CrossRef] [PubMed]
- Suvd, J.; Gerel, B.; Otgooloi, H.; Purevsuren, D.; Zolzaya, H.; Roglic, G.; King, H. Glucose intolerance and associated factors in Mongolia: Results of a national survey. Diabet. Med. 2002, 19, 502–508. [Google Scholar] [CrossRef]
- World Health Organization. Mongolia Completes Its 4th Round of STEPS Survey on the Prevalence of NCD Risk Factors. 2020. Available online: https://www.who.int/mongolia/news/detail/29-06-2020-mongolia-completes-its-4th-round-of-steps-survey-on-the-prevalence-of-ncd-risk-factors (accessed on 25 August 2024).
- Center for Health Development, Mongolia. Health Indicators. 2020. Available online: http://www.hdc.gov.mn/media/uploads/2019-11/2018eng.pdf (accessed on 25 August 2024).
- Ma, C.X.; Ma, X.N.; Guan, C.H.; Li, Y.D.; Mauricio, D.; Fu, S.B. Cardiovascular disease in type 2 diabetes mellitus: Progress toward personalized management. Cardiovasc. Diabetol. 2022, 21, 74. [Google Scholar] [CrossRef]
- Grundlingh, N.; Zewotir, T.T.; Roberts, D.J.; Manda, S. Assessment of prevalence and risk factors of diabetes and pre-diabetes in South Africa. J. Health Popul. Nutr. 2022, 41, 7. [Google Scholar] [CrossRef]
- Palladino, R.; Tabak, A.G.; Khunti, K.; Valabhji, J.; Majeed, A.; Millett, C.; Vamos, E.P. Association between pre-diabetes and microvascular and macrovascular disease in newly diagnosed type 2 diabetes. BMJ Open Diabetes Res. Care 2020, 8, e001061. [Google Scholar] [CrossRef]
- Abdul-Ghani, M.; DeFronzo, R.A.; Del Prato, S.; Chilton, R.; Singh, R.; Ryder, R.E. Cardiovascular disease and type 2 diabetes: Has the dawn of a new era arrived? Diabetes Care 2017, 40, 813–820. [Google Scholar] [CrossRef]
- Enkhtugs, K.; Byambasukh, O.; Boldbaatar, D.; Tsedev-Ochir, T.O.; Enebish, O.; Sereejav, E.; Dangaa, B.; Bayartsogt, B.; Yadamsuren, E.; Nyamdavaa, K. Examining Age-Adjusted Associations between BMI and Comorbidities in Mongolia: Cross-Sectional Prevalence. Healthcare 2024, 12, 1222. [Google Scholar] [CrossRef]
- World Health Organization. HEARTS: Technical Package for Cardiovascular Disease Management in Primary Health Care: Risk-Based CVD Management. Available online: https://www.who.int/publications/i/item/9789240001367 (accessed on 18 September 2024).
- World Health Organization (WHO). STEPS Manual: The WHO STEPwise Approach to Chronic Disease Risk Factor Surveillance; World Health Organization: Geneva, Switzerland, 2008; Available online: https://www.who.int/teams/noncommunicable-diseases/surveillance/systems-tools/steps (accessed on 25 August 2024).
- Tudor-Locke, C.; Craig, C.L.; Brown, W.J.; Clemes, S.A.; De Cocker, K.; Giles-Corti, B.; Hatano, Y.; Inoue, S.; Matsudo, S.M.; Mutrie, N.; et al. How many steps/day are enough? For adults. Int. J. Behav. Nutr. Phys. Act. 2011, 8, 79. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Obesity: Preventing and Managing the Global Epidemic. Report of a WHO Consultation. In WHO Technical Report Series; World Health Organization: Geneva, Switzerland, 2000; 894p. [Google Scholar]
- Alberti, K.G.M.M.; Zimmet, P.; Shaw, J. The metabolic syndrome—A new worldwide definition. Lancet 2005, 366, 1059–1062. [Google Scholar] [CrossRef] [PubMed]
- Zuo, Y.; Han, X.; Tian, X.; Chen, S.; Wu, S.; Wang, A. Association of impaired fasting glucose with cardiovascular disease in the absence of risk factor. J. Clin. Endocrinol. Metab. 2022, 107, e1710–e1718. [Google Scholar] [CrossRef] [PubMed]
- Seshasai, S.R.; Kaptoge, S.; Thompson, A.; Di Angelantonio, E.; Gao, P.; Sarwar, N.; Whincup, P.H.; Mukamal, K.J.; Gillum, R.F.; Holme, I.; et al. Diabetes mellitus, fasting glucose, and risk of cause-specific death. N. Engl. J. Med. 2011, 364, 829–841. [Google Scholar] [CrossRef]
- Vikramaditya, B.; Satija, M.; Chaudhary, A.; Sharma, S.; Girdhar, S.; Bansal, P. A community based cross-sectional study to estimate total cardiovascular risk in rural Punjab. Int. J. Community Med. Public Health 2017, 4, 1295. [Google Scholar] [CrossRef]
- Nwose, E.U.; Richards, R.S.; Digban, K.; Bwititi, P.T.; Ennis, G.; Yee, K.C.; Oguoma, V.M.; Liberato, S. Cardiovascular risk assessment in prediabetes and undiagnosed diabetes mellitus study: International collaboration research overview. N. Am. J. Med. Sci. 2013, 5, 625–628. [Google Scholar] [CrossRef]
- Dong, W.; Tse, T.Y.E.; Mak, L.I.; Wong, C.K.H.; Wan, Y.F.E.; Tang, H.M.E.; Chin, W.Y.; Bedford, L.E.; Yu, Y.T.E.; Ko, W.K.W.; et al. Non-laboratory-based risk assessment model for case detection of diabetes mellitus and pre-diabetes in primary care. J. Diabetes Investig. 2022, 13, 1374–1386. [Google Scholar] [CrossRef]
- Huang, Y.; Cai, X.; Mai, W.; Li, M.; Hu, Y. Association between prediabetes and risk of cardiovascular disease and all-cause mortality: Systematic review and meta-analysis. BMJ 2016, 355, i5953. [Google Scholar] [CrossRef]
- Mando, R.; Waheed, M.; Michel, A.; Karabon, P.; Halalau, A. Prediabetes as a risk factor for major adverse cardiovascular events. Ann. Med. 2021, 53, 2090–2098. [Google Scholar] [CrossRef]
- Sasaki, N.; Ozono, R.; Higashi, Y.; Maeda, R.; Kihara, Y. Association of insulin resistance, plasma glucose level, and serum insulin level with hypertension in a population with different stages of impaired glucose metabolism. J. Am. Heart Assoc. 2020, 9, e015546. [Google Scholar] [CrossRef]
- Liu, X.C.; He, G.D.; Lo, K.; Huang, Y.Q.; Feng, Y.Q. The triglyceride-glucose index, an insulin resistance marker, was non-linear associated with all-cause and cardiovascular mortality in the general population. Front. Cardiovasc. Med. 2021, 7, 628109. [Google Scholar] [CrossRef]
- Wang, A.; Tian, X.; Zuo, Y.; Chen, S.; Meng, X.; Wu, S.; Wang, Y. Change in triglyceride-glucose index predicts the risk of cardiovascular disease in the general population: A prospective cohort study. Cardiovasc. Diabetol. 2021, 20, 113. [Google Scholar] [CrossRef] [PubMed]
- Gadekar, T.; Dudeja, P.; Basu, I.; Vashisht, S.; Mukherji, S. Correlation of visceral body fat with waist–hip ratio, waist circumference and body mass index in healthy adults: A cross sectional study. Med. J. Armed Forces India 2020, 76, 41–46. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Wang, Z.; Wang, X.; Chen, Z.; Shao, L.; Tian, Y.; Zheng, C.; Li, S.; Zhu, M.; Gao, R. Prevalence of overweight and obesity in China: Results from a cross-sectional study of 441 thousand adults, 2012–2015. Obes. Res. Clin. Pract. 2020, 14, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Ma, N.; Lin, Q.; Chen, K.; Zheng, F.; Wu, J.; Dong, X.; Niu, W. Body roundness index and all-cause mortality among US adults. JAMA Netw. Open 2024, 7, e2415051. [Google Scholar] [CrossRef] [PubMed]
- Dziopa, K.; Asselbergs, F.W.; Gratton, J.; Chaturvedi, N.; Schmidt, A.F. Cardiovascular risk prediction in type 2 diabetes: A comparison of 22 risk scores in primary care settings. Diabetologia 2022, 65, 644–656. [Google Scholar] [CrossRef]
| Findings | Total | Glycemic Status | ||||
|---|---|---|---|---|---|---|
| NGT | IFG | Newly DM | Old DM | p-Value | ||
| Frequency, n | 120,266 | 71,215 | 40,080 | 7990 | 981 | - |
| Age (years) | 44.3 ± 15.2 | 42.5 ± 15.3 | 50.5 ± 12.3 | 52.3 ± 11.8 | 53.7 ± 12.4 | <0.001 |
| Male, % (n) | 39.4 (47,370) | 37.9 (36,584) | 46.2 (7078) | 48.0 (1106) | 41.9 (2602) | <0.001 |
| Living area: urban, % (n) | 41.4 (49,749) | 41.7 (40,234) | 32.8 (5022) | 35.9 (827) | 59.0 (3666) | <0.001 |
| Education: lower, % (n) | 8.6 (10,351) | 8.4 (8126) | 10.2 (1562) | 7.1 (163) | 8.0 (500) | <0.001 |
| BMI (kg/m2) | 26.7 ± 4.9 | 26.1 ± 4.7 | 28.6 ± 4.9 | 29.7 ± 5.5 | 29.1 ± 5.3 | <0.001 |
| Obesity, % (n) | 22.7 (27,318) | 19.1 (18,388) | 35.8 (5488) | 44.8 (1031) | 38.8 (2411) | <0.001 |
| Waist Circumference (male, cm) | 89.0 ± 14.1 | 87.2 ± 13.6 | 94.3 ± 13.9 | 98.4 ± 14.6 | 96.8 ± 14.1 | <0.001 |
| Waist Circumference (female, cm) | 84.9 ± 13.7 | 83.4 ± 13.2 | 90.6 ± 13.6 | 93.3 ± 14.5 | 92.9 ± 13.8 | <0.001 |
| Central Obesity, % (n) | 55.9 (67,179) | 51.8 (49,979) | 70.9 (10,871) | 78.5 (1806) | 72.8 (4523) | <0.001 |
| Systolic (mmHg) | 120.2 ± 16.0 | 118.9 ± 15.4 | 124.8 ± 16.9 | 128.6 ± 18.4 | 127.0 ± 17.0 | <0.001 |
| Diastolic (mmHg) | 77.6 ± 10.6 | 76.7 ± 10.3 | 80.5 ± 10.8 | 82.4 ± 11.6 | 82.0 ± 11.1 | <0.001 |
| Total cholesterol (mmol/L) | 5.1 ± 1.2 | 5.0 ± 1.2 | 5.3 ± 1.3 | 5.4 ± 1.4 | 5.5 ± 1.3 | <0.001 |
| Triglycerides (mmol/L) | 1.3 ± 0.9 | 1.2 ± 0.8 | 1.6 ± 1.1 | 2.0 ± 1.4 | 1.8 ± 1.2 | <0.001 |
| Smoking, % (n) | 19.5 (23,494) | 18.9 (18,272) | 22.4 (3425) | 23.8 (549) | 20.1 (1248) | <0.001 |
| Alcohol use, % (n) | 9.3 (11,168) | 8.8 (8478) | 12.4 (1900) | 10.2 (235) | 8.9 (555) | 0.024 |
| Fruit and vegetable daily use, % (n) | 25.4 (30,499) | 25.4 (24,485) | 24.9 (3816) | 26.1 (600) | 25.7 (1598) | 0.022 |
| Regular exercise and PA, % (n) | 60.0 (72,181) | 59.8 (57,690) | 60.0 (9201) | 59.9 (1380) | 62.9 (3910) | <0.001 |
| Gender | Age Category | N | CVD Risk Category, % (n) | ||||
|---|---|---|---|---|---|---|---|
| Low | Moderate | High | Very High | p-Value | |||
| Male | T1 (18–36) | 18,702 | 78.2% (14,621) | 19.8% (3706) | 1.7% (314) | 0.3% (61) | <0.0001 |
| T2 (37–52) | 14,085 | 52.3% (7365) | 39.3% (5532) | 7.6% (1070) | 0.8% (118) | ||
| T3 (53–94) | 14,583 | 39.0% (5694) | 44.5% (6492) | 14.8% (2154) | 1.7% (243) | ||
| Female | T1 (18–36) | 22,393 | 79.7% (17,848) | 18.9% (4225) | 1.0% (229) | 0.4% (91) | <0.0001 |
| T2 (37–52) | 26,079 | 59.9% (15,611) | 35.0% (9120) | 4.6% (1196) | 0.6% (152) | ||
| T3 (53–94) | 24,424 | 41.3% (10,076) | 45.1% (11,005) | 12.4% (3027) | 1.3% (316) | ||
| Gender and Age | Glucose Status | N | CVD Risk Category, % (n) | ||||
| Low | Moderate | High | Very High | p-Value | |||
| Male | |||||||
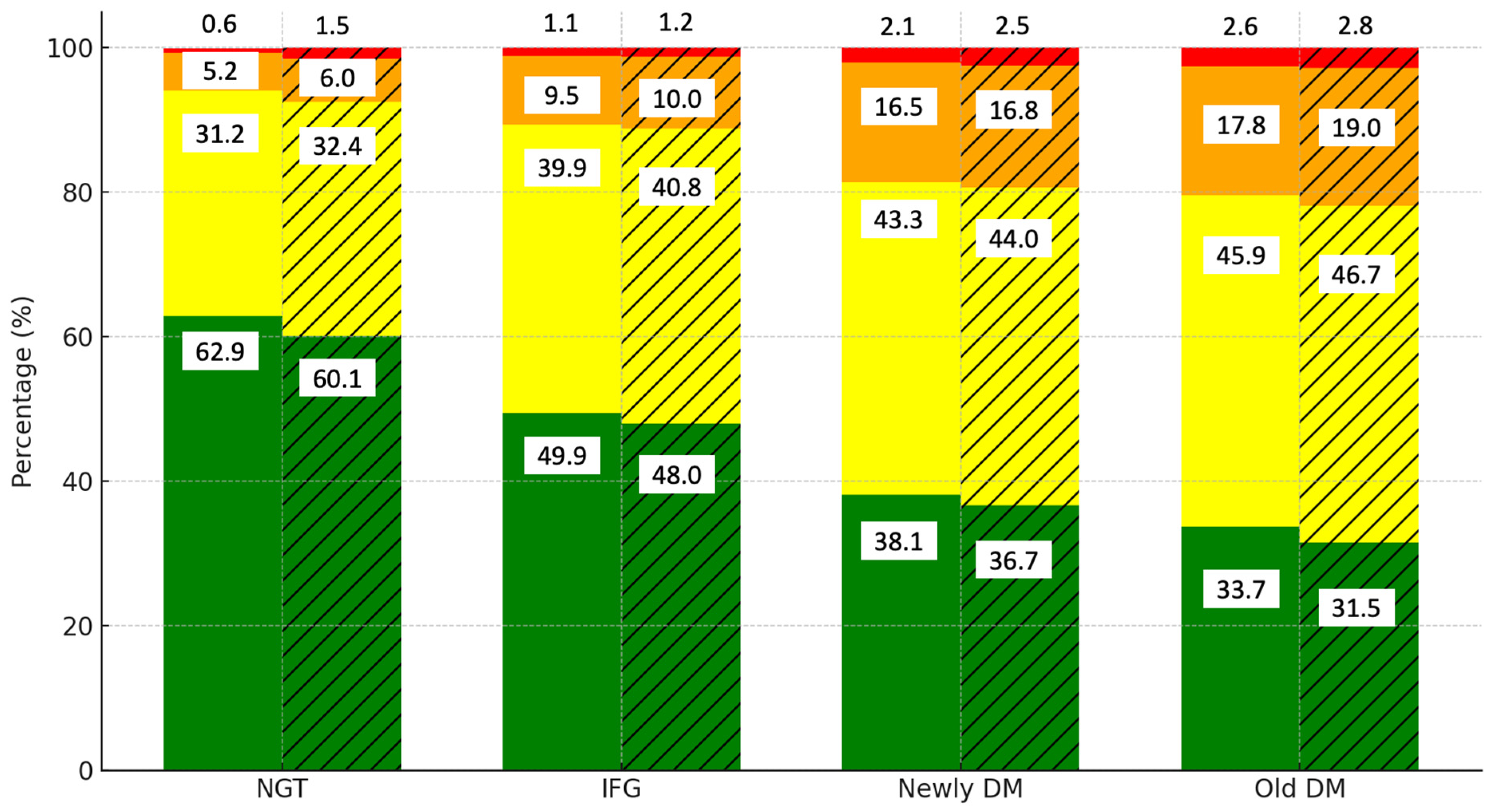
| T1 (18–36) | NGT | 17,169 | 79.4% (13,626) | 18.9% (3246) | 1.4% (246) | 0.3% (51) | <0.0001 |
| IFG | 1160 | 66.6% (772) | 29.1% (338) | 3.7% (43) | 0.6% (7) | ||
| New DM | 118 | 59.3% (70) | 30.5% (36) | 10.2% (12) | 0.0% (0) | ||
| Old DM | 255 | 60.0% (153) | 33.7% (86) | 5.1% (13) | 1.2% (3) | ||
| T2 (37–52) | NGT | 9811 | 55.2% (5420) | 37.9% (3719) | 6.2% (610) | 0.6% (62) | <0.0001 |
| IFG | 2959 | 50.1% (1483) | 41.0% (1214) | 8.0% (236) | 0.9% (26) | ||
| New DM | 433 | 38.1% (165) | 43.6% (189) | 16.4% (71) | 1.8% (8) | ||
| Old DM | 882 | 33.7% (297) | 46.5% (410) | 17.3% (153) | 2.5% (22) | ||
| T3 (53–94) | NGT | 9604 | 43.0% (4125) | 43.4% (4167) | 12.4% (1195) | 1.2% (117) | <0.0001 |
| IFG | 2959 | 35.1% (1038) | 47.7% (1411) | 15.5% (458) | 1.8% (52) | ||
| New DM | 555 | 27.6% (153) | 46.1% (256) | 23.2% (129) | 3.1% (17) | ||
| Old DM | 1465 | 25.8% (378) | 44.9% (658) | 25.4% (372) | 3.9% (57) | ||
| Glucose Status | N | CVD Risk Category, % (n) | |||||
| Low | Moderate | High | Very High | p-Value | |||
| Female | |||||||
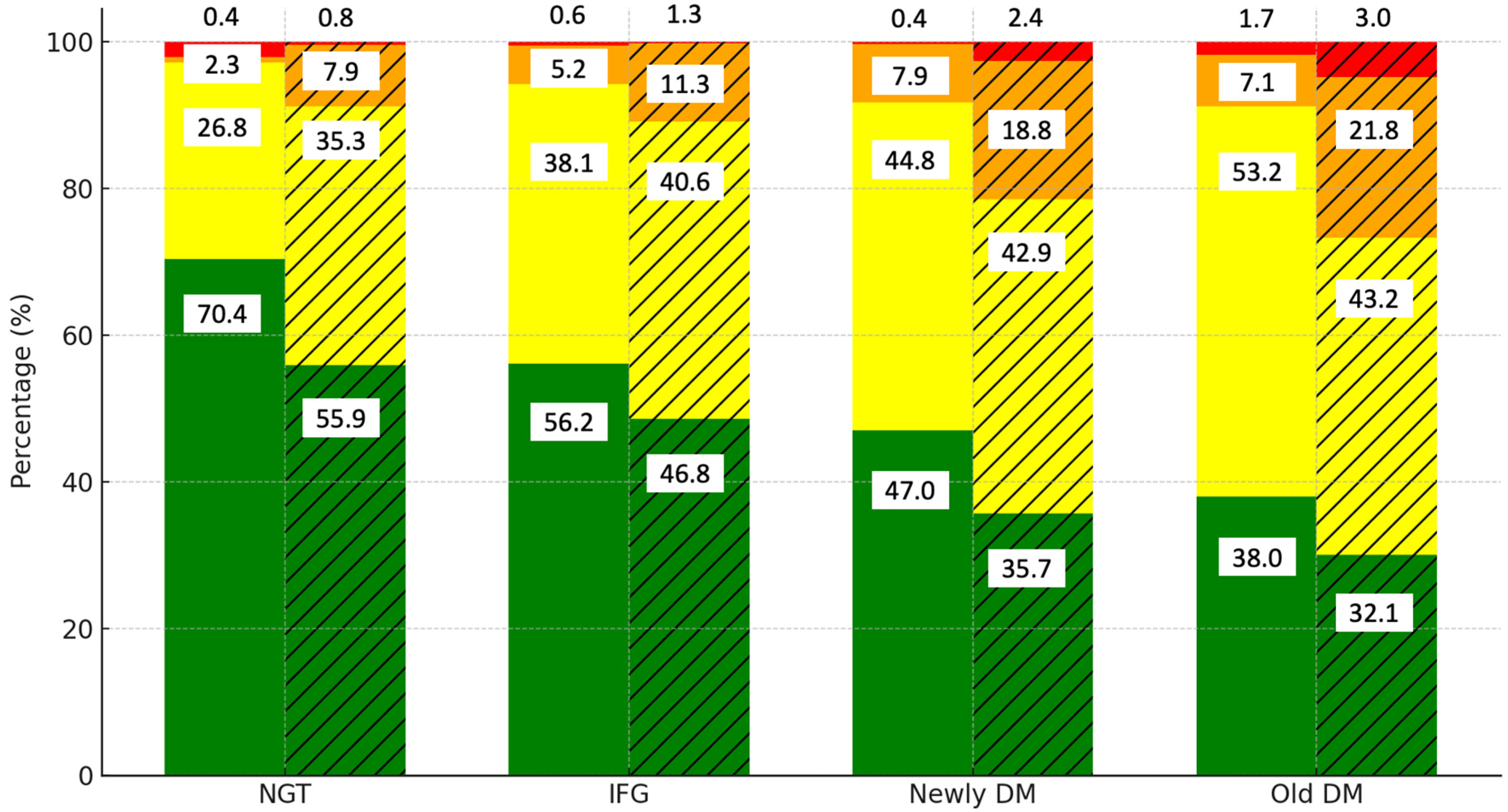
| T1 (18–36) | NGT | 20,799 | 80.3% (16,695) | 18.5% (3838) | 0.9% (183) | 0.4% (83) | <0.0001 |
| IFG | 1093 | 76.5% (836) | 21.0% (229) | 2.2% (24) | 0.4% (4) | ||
| New DM | 132 | 70.5% (93) | 22.7% (30) | 6.1% (8) | 0.8% (1) | ||
| Old DM | 369 | 60.7% (224) | 34.7% (128) | 3.8% (14) | 0.8% (3) | ||
| T2 (37–52) | NGT | 21,161 | 61.5% (13,012) | 34.0% (7191) | 4.0% (849) | 0.5% (109) | <0.0001 |
| IFG | 3339 | 57.5% (1920) | 36.5% (1219) | 5.4% (179) | 0.6% (21) | ||
| New DM | 458 | 46.5% (213) | 40.8% (187) | 12.0% (55) | 0.7% (3) | ||
| Old DM | 1121 | 41.6% (466) | 46.7% (523) | 10.1% (113) | 1.7% (19) | ||
| T3 (53–94) | NGT | 17,884 | 43.5% (7779) | 44.5% (7960) | 11.0% (1961) | 1.0% (184) | <0.0001 |
| IFG | 3813 | 40.3% (1538) | 44.6% (1699) | 13.7% (522) | 1.4% (54) | ||
| New DM | 606 | 30.4% (184) | 49.3% (299) | 17.2% (104) | 3.1% (19) | ||
| Old DM | 2121 | 27.1% (575) | 49.4% (1047) | 20.7% (440) | 2.8% (59) | ||
| Association of Glycemic Status with Moderate to High CVD Risk | Odds Ratio | 95% CI | p Value | |
|---|---|---|---|---|
| Lower Bound | Upper Bound | |||
| Unadjusted | ||||
| Normal fasting glycemia | 1.0 (reference) | - | - | - |
| Impaired fasting glycemia | 1.73 | 1.67 | 1.79 | <0.001 |
| Newly diagnosed diabetes | 2.75 | 2.53 | 2.99 | <0.001 |
| Pre-existing diabetes (old) | 3.34 | 3.16 | 3.52 | <0.001 |
| Adjusted for age | ||||
| Normal fasting glycemia | 1.0 (reference) | - | - | - |
| Impaired fasting glycemia | 1.26 | 1.22 | 1.31 | <0.001 |
| Newly diagnosed diabetes | 1.91 | 1.75 | 2.08 | <0.001 |
| Pre-existing diabetes (old) | 2.19 | 2.07 | 2.32 | <0.001 |
| Adjusted for age, gender | ||||
| Normal fasting glycemia | 1.0 (reference) | - | - | - |
| Impaired fasting glycemia | 1.24 | 1.19 | 1.28 | <0.001 |
| Newly diagnosed diabetes | 1.87 | 1.71 | 2.04 | <0.001 |
| Pre-existing diabetes (old) | 2.17 | 2.05 | 2.30 | <0.001 |
| Adjusted for age, gender, central obesity | ||||
| Normal fasting glycemia | 1.0 (reference) | - | - | - |
| Impaired fasting glycemia | 1.13 | 1.09 | 1.18 | <0.001 |
| Newly diagnosed diabetes | 1.63 | 1.49 | 1.78 | <0.001 |
| Pre-existing diabetes (old) | 1.94 | 1.83 | 2.05 | <0.001 |
| Adjusted for age, gender, central obesity, fasting blood glucose level | ||||
| Normal fasting glycemia | 1.0 (reference) | - | - | - |
| Impaired fasting glycemia | 1.11 | 1.06 | 1.15 | <0.001 |
| Newly diagnosed diabetes | 1.37 | 1.24 | 1.52 | <0.001 |
| Pre-existing diabetes (old) | 1.76 | 1.65 | 1.88 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Batmunkh, N.; Enkhtugs, K.; Munkhbat, K.; Davaakhuu, N.; Enebish, O.; Dangaa, B.; Luvsansambuu, T.; Togtmol, M.; Bayartsogt, B.; Batsukh, K.; et al. Cardiovascular Risk across Glycemic Categories: Insights from a Nationwide Screening in Mongolia, 2022–2023. J. Clin. Med. 2024, 13, 5866. https://doi.org/10.3390/jcm13195866
Batmunkh N, Enkhtugs K, Munkhbat K, Davaakhuu N, Enebish O, Dangaa B, Luvsansambuu T, Togtmol M, Bayartsogt B, Batsukh K, et al. Cardiovascular Risk across Glycemic Categories: Insights from a Nationwide Screening in Mongolia, 2022–2023. Journal of Clinical Medicine. 2024; 13(19):5866. https://doi.org/10.3390/jcm13195866
Chicago/Turabian StyleBatmunkh, Nomuuna, Khangai Enkhtugs, Khishignemekh Munkhbat, Narantuya Davaakhuu, Oyunsuren Enebish, Bayarbold Dangaa, Tumurbaatar Luvsansambuu, Munkhsaikhan Togtmol, Batzorig Bayartsogt, Khishigjargal Batsukh, and et al. 2024. "Cardiovascular Risk across Glycemic Categories: Insights from a Nationwide Screening in Mongolia, 2022–2023" Journal of Clinical Medicine 13, no. 19: 5866. https://doi.org/10.3390/jcm13195866





