Paroxysmal Dystonic Posturing Mimicking Nocturnal Leg Cramps as a Presenting Sign in an Infant with DCC Mutation, Callosal Agenesis and Mirror Movements
Abstract
:1. Introduction
2. Materials and Methods
2.1. Ethics Consideration
2.2. Standardized Measures and Clinical Scales
2.3. Exome Sequencing (ES)
3. Results
3.1. Clinical Report
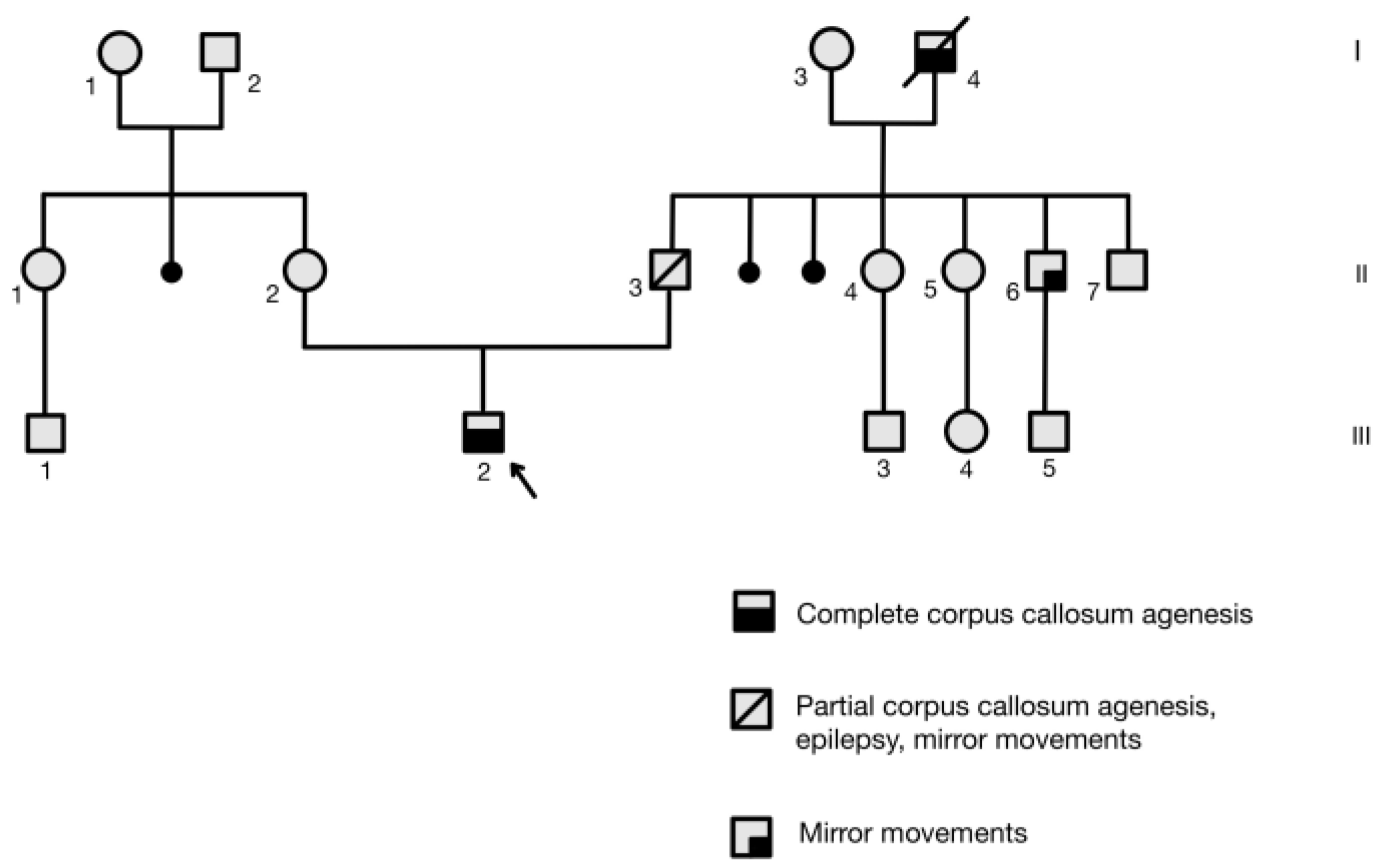
3.2. Family Background
3.3. Genetic Findings
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Glass, H.C.; Shaw, G.M.; Ma, C.; Sherr, E.H. Agenesis of the corpus callosum in California 1983–2003: A population-based study. Am. J. Med. Genet. Part A 2008, 146A, 2495–2500. [Google Scholar] [CrossRef]
- Doussal, L.F.-L.; Chadie, A.; Brasseur-Daudruy, M.; Verspyck, E.; Saugier-Veber, P.; Marret, S.; Perinatal Network of Haute-Normandie. Neurodevelopmental outcome in prenatally diagnosed isolated agenesis of the corpus callosum. Early Hum. Dev. 2018, 116, 9–16. [Google Scholar] [CrossRef]
- Luders, E.; Thompson, P.M.; Toga, A.W. The Development of the Corpus Callosum in the Healthy Human Brain. J. Neurosci. 2010, 30, 10985–10990. [Google Scholar] [CrossRef]
- Knight, J.L.; Barker, M.S.; Edwards, T.J.; Barnby, J.M.; Richards, L.J.; Robinson, G.A. Mirror movements and callosal dysgenesis in a family with a DCC mutation: Neuropsychological and neuroimaging outcomes. Cortex 2023, 161, 38–50. [Google Scholar] [CrossRef] [PubMed]
- Marsh, A.P.L.; Edwards, T.J.; Galea, C.; Cooper, H.M.; Engle, E.C.; Jamuar, S.S.; Méneret, A.; Moutard, M.; Nava, C.; Rastetter, A.; et al. DCC mutation update: Congenital mirror movements, isolated agenesis of the corpus callosum, and developmental split brain syndrome. Hum. Mutat. 2018, 39, 23–39. [Google Scholar] [CrossRef] [PubMed]
- Fearon, E.R.; Cho, K.R.; Nigro, J.M.; Kern, S.E.; Simons, J.W.; Ruppert, J.M.; Hamilton, S.R.; Preisinger, A.C.; Thomas, G.; Kinzler, K.W.; et al. Identification of a Chromosome 18q Gene that Is Altered in Colorectal Cancers. Science 1990, 247, 49–56. [Google Scholar] [CrossRef] [PubMed]
- Marsh, A.P.L.; Heron, D.; Edwards, T.J.; Quartier, A.; Galea, C.; Nava, C.; Rastetter, A.; Moutard, M.-L.; Anderson, V.; Bitoun, P.; et al. Mutations in DCC cause isolated agenesis of the corpus callosum with incomplete penetrance. Nat. Genet. 2017, 49, 511–514. [Google Scholar] [CrossRef] [PubMed]
- Méneret, A.; Trouillard, O.; Dunoyer, M.; Depienne, C.; Roze, E. Congenital Mirror Movements. In GeneReviews®; Adam, M.P., Feldman, J., Mirzaa, G.M., Pagon, R.A., Wallace, S.E., Bean, L.J.H., Gripp, K.W., Amemiya, A., Eds.; University of Washington: Seattle, WA, USA, 2015. Available online: https://www.ncbi.nlm.nih.gov/books/NBK279760 (accessed on 15 October 2023).
- Depienne, C.; Cincotta, M.; Billot, S.; Bouteiller, D.; Groppa, S.; Brochard, V.; Flamand, C.; Hubsch, C.; Meunier, S.; Giovannelli, F.; et al. A novel DCC mutation and genetic heterogeneity in congenital mirror movements. Neurology 2011, 76, 260–264. [Google Scholar] [CrossRef] [PubMed]
- Srour, M.; Rivière, J.-B.; Pham, J.M.T.; Dubé, M.-P.; Girard, S.; Morin, S.; Dion, P.A.; Asselin, G.; Rochefort, D.; Hince, P.; et al. Mutations in DCC Cause Congenital Mirror Movements. Science 2010, 328, 592. [Google Scholar] [CrossRef] [PubMed]
- Welniarz, Q.; Morel, M.-P.; Pourchet, O.; Gallea, C.; Lamy, J.-C.; Cincotta, M.; Doulazmi, M.; Belle, M.; Méneret, A.; Trouillard, O.; et al. Non cell-autonomous role of DCC in the guidance of the corticospinal tract at the midline. Sci. Rep. 2017, 7, 410. [Google Scholar] [CrossRef] [PubMed]
- Jamuar, S.S.; Schmitz-Abe, K.; D’Gama, A.M.; Drottar, M.; Chan, W.-M.; Peeva, M.; Servattalab, S.; Lam, A.-T.N.; Delgado, M.R.; Clegg, N.J.; et al. Biallelic mutations in human DCC cause developmental split-brain syndrome. Nat. Genet. 2017, 49, 606–612. [Google Scholar] [CrossRef] [PubMed]
- Bierhals, T.; Korenke, G.C.; Baethmann, M.; Marín, L.L.; Staudt, M.; Kutsche, K. Novel DCC variants in congenital mirror movements and evaluation of disease-associated missense variants. Eur. J. Med. Genet. 2018, 61, 329–334. [Google Scholar] [CrossRef] [PubMed]
- Vosberg, D.E.; Beaulé, V.; Torres-Berrío, A.; Cooke, D.; Chalupa, A.; Jaworska, N.; Cox, S.M.L.; Larcher, K.; Zhang, Y.; Allard, D.; et al. Neural function in DCC mutation carriers with and without mirror movements. Ann. Neurol. 2019, 85, 433–442. [Google Scholar] [CrossRef] [PubMed]
- Spencer-Smith, M.; Knight, J.L.; Lacaze, E.; Irc5 Consortium; Depienne, C.; Lockhart, P.J.; Richards, L.J.; Heron, D.; Leventer, R.J.; A Robinson, G.; et al. Callosal agenesis and congenital mirror movements: Outcomes associated with DCC mutations. Dev. Med. Child Neurol. 2020, 62, 758–762. [Google Scholar] [CrossRef] [PubMed]
- Huntley, M. Griffiths Mental Development Scales from Birth to 2 Years—Manual; ARICD: Oxford, UK, 1996. [Google Scholar]
- Green, E.; Stroud, L.; Bloomfield, S.; Cronje, J.; Foxcroft, C.; Hurter, K.; Lane, H.; Marais, R.; Marx, C.; McAlinden, P.; et al. Griffiths Scales of Child Development, 3rd ed. (Griffiths III); Hogrefe Ltd.: Oxford, UK, 2016. [Google Scholar]
- Wechsler, D. Wechsler Intelligence Scale for Children—Fourth Edition (WISC-IV); The Psychological Corporation: San Antonio, TX, USA, 2003. [Google Scholar]
- Higgins, L.; Mannion, A.; Chen, J.L.; Leader, G. Adaptation of Parents Raising a Child with ASD: The Role of Positive Perceptions, Coping, Self-efficacy, and Social Support. J. Autism Dev. Disord. 2023, 53, 1224–1242. [Google Scholar] [CrossRef] [PubMed]
- Redmond, S.M.; Ash, A.C. A cross-etiology comparison of the socio-emotional behavioral profiles associated with attention-deficit/hyperactivity disorder and specific language impairment. Clin. Linguist. Phon. 2014, 28, 346–365. [Google Scholar] [CrossRef] [PubMed]
- Woods, B.T.; Teuber, H.-L. Mirror movements after childhood hemiparesis. Neurology 1978, 28, 1152. [Google Scholar] [CrossRef] [PubMed]
- Richards, S.; Aziz, N.; Bale, S.; Bick, D.; Das, S.; Gastier-Foster, J.; Grody, W.W.; Hegde, M.; Lyon, E.; Spector, E.; et al. Standards and guidelines for the interpretation of sequence variants: A joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 2015, 17, 405–424. [Google Scholar] [CrossRef]
- Meneret, A.; Trouillard, O.; Brochard, V.; Roze, E. Congenital mirror movements caused by a mutation in the DCC gene. Dev. Med. Child Neurol. 2015, 57, 776. [Google Scholar] [CrossRef]
- Franz, E.A.; Chiaroni-Clarke, R.; Woodrow, S.; Glendining, K.A.; Jasoni, C.L.; Robertson, S.P.; Gardner, R.M.; Markie, D. Congenital mirror movements: Phenotypes associated with DCC and RAD51 mutations. J. Neurol. Sci. 2015, 351, 140–145. [Google Scholar] [CrossRef]
- Méneret, A.; Depienne, C.; Riant, F.; Trouillard, O.; Bouteiller, D.; Cincotta, M.; Bitoun, P.; Wickert, J.; Lagroua, I.; Westenberger, A.; et al. Congenital mirror movements: Mutational analysis of RAD51 and DCC in 26 cases. Neurology 2014, 82, 1999–2002. [Google Scholar] [CrossRef]
- Sagi-Dain, L.; Kurolap, A.; Ilivitzki, A.; Mory, A.; Paperna, T.; Kedar, R.; Gonzaga-Jauregui, C.; Peleg, A.; Feldman, H.B.; Regeneron Genetics Center. A novel heterozygous loss-of-function DCC Netrin 1 receptor variant in prenatal agenesis of corpus callosum and review of the literature. Am. J. Med. Genet. Part A 2020, 182, 205–212. [Google Scholar] [CrossRef]
- Thams, S.; Islam, M.; Lindefeldt, M.; Nordgren, A.; Granberg, T.; Tesi, B.; Barbany, G.; Nilsson, D.; Paucar, M. Heterozygous variants in DCC: Beyond congenital mirror movements. Neurol. Genet. 2020, 6, e526. [Google Scholar] [CrossRef]
- Nissenkorn, A.; Yosovich, K.; Leibovitz, Z.; Hartman, T.G.; Zelcer, I.; Hugirat, M.; Lev, D.; Lerman-Sagie, T.; Blumkin, L. Congenital Mirror Movements Associated with Brain Malformations. J. Child Neurol. 2021, 36, 545–555. [Google Scholar] [CrossRef]
- Solmaz, B.; Özyurt, M.G.; Ata, D.B.; Akçimen, F.; Shabsog, M.; Türker, K.S.; Dalçik, H.; Algin, O.; Başak, A.N.; Özgür, M.; et al. Assessment of the corticospinal fiber integrity in mirror movement disorder. J. Clin. Neurosci. 2018, 54, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Koerte, I.; Pelavin, P.; Kirmess, B.; Fuchs, T.; Berweck, S.; Laubender, R.P.; Borggraefe, I.; Schroeder, S.; Danek, A.; Rummeny, C.; et al. Anisotropy of transcallosal motor fibres indicates functional impairment in children with periventricular leukomalacia. Dev. Med. Child Neurol. 2011, 53, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Weinstein, M.; Green, D.; Geva, R.; Schertz, M.; Fattal-Valevski, A.; Artzi, M.; Myers, V.; Shiran, S.; Gordon, A.M.; Gross-Tsur, V.; et al. Interhemispheric and intrahemispheric connectivity and manual skills in children with unilateral cerebral palsy. Brain Struct. Funct. 2013, 219, 1025–1040. [Google Scholar] [CrossRef] [PubMed]
- Simon-Martinez, C.; Decraene, L.; Zielinski, I.; Hoare, B.; Williams, J.; Mailleux, L.; Steenbergen, B.; Ortibus, E.; Feys, H.; Klingels, K. The impact of brain lesion characteristics and the corticospinal tract wiring on mirror movements in unilateral cerebral palsy. Sci. Rep. 2022, 12, 16301. [Google Scholar] [CrossRef] [PubMed]
- Leung, A.K.; Wong, B.E.; Chan, P.Y.; Cho, H.Y. Nocturnal leg cramps in children: Incidence and clinical characteristics. J. Natl. Med. Assoc. 1999, 91, 329–332. Available online: https://pubmed.ncbi.nlm.nih.gov/10388258 (accessed on 7 November 2023).
- Tipton, P.W.; Wszołek, Z.K. Restless legs syndrome and nocturnal leg cramps: Review and guide to diagnosis and treatment. Pol. Arch. Intern. Med. 2017, 127, 865–872. [Google Scholar] [CrossRef]
- Hawke, F.; McKay, M.J.; Baldwin, J.N.; Chiu, S.; Sadler, S.; Oldmeadow, C.; Chuter, V.; Burns, J. Correlates of night-time and exercise-associated lower limb cramps in healthy adults. Muscle Nerve 2021, 64, 301–308. [Google Scholar] [CrossRef] [PubMed]
- D’antonio, F.; Pagani, G.; Familiari, A.; Khalil, A.; Sagies, T.-L.; Malinger, G.; Leibovitz, Z.; Garel, C.; Moutard, M.L.; Pilu, G.; et al. Outcomes Associated with Isolated Agenesis of the Corpus Callosum: A Meta-analysis. Pediatrics 2016, 138, e20160445. [Google Scholar] [CrossRef] [PubMed]
- Siffredi, V.; Anderson, V.; McIlroy, A.; Wood, A.G.; Leventer, R.J.; Spencer-Smith, M.M. A Neuropsychological Profile for Agenesis of the Corpus Callosum? Cognitive, Academic, Executive, Social, and Behavioral Functioning in School-Age Children. J. Int. Neuropsychol. Soc. 2018, 24, 445–455. [Google Scholar] [CrossRef] [PubMed]

| Patient- Gender/Age | Ethnicity | Development | Cognition | MMs | Other Neurological Manifestations | CC | Other Brain Abnormalities | DCC Variant | Reference |
|---|---|---|---|---|---|---|---|---|---|
| M/10 | Caucasian | Normal | Normal | + | Difficulties in fine bimanual activities | NA | NA | c.3835_3836delCT/p.Leu1279ProfsX24 | Depienne et al., 2011 [9] |
| M/18 | Turkish | NA | NA | + | Difficulties in fine bimanual activities | NA | NA | c.2000 G>A/p.Arg667His | Meneret et al., 2014 [25] |
| M/6 | Caucasian | NA | NA | + | Difficulties in fine bimanual activities; general clumsiness | NA | NA | c.1336_1337insAGCC/p.Arg446GlnfsX27 | Meneret et al., 2014 [25] |
| F/8 | Caucasian | NA | NA | + | Difficulties in fine bimanual activities | NA | NA | c.2871_2875dup/p.Pro960GlyfsX8 | Meneret et al., 2014 [25] |
| F/3 | Caucasian | NA | NA | + | Difficulties in fine bimanual activities; general clumsiness | NA | NA | c.823C>T/p.Arg275X | Meneret et al., 2014 [25] |
| F/6 | North African | NA | NA | + | Retinal dystrophy; difficulties in fine bimanual activities and writing; general clumsiness | NA | NA | c.823C>T/p.Arg275X | Meneret et al., 2014 [25] |
| F/11 | North African | NA | NA | + | Retinal dystrophy; difficulties in fine bimanual activities; general clumsiness | cACC | - | c.823C>T/p.Arg275X | Meneret et al., 2014 [25] |
| M/7 | Caucasian | NA | NA | + | Difficulties in fine bimanual activities and everyday tasks | NA | NA | c.377C>A/p.Ser126X | Meneret et al., 2014 [25] |
| F/6 | Caucasian | Normal | Normal | + | Clumsiness; inability to perform unimanual or skilled dissociated movements of the two hands | NA | NA | c.823C>T/p.Arg275X | Meneret et al., 2015 [23] |
| M/6 | Caucasian | Normal | Normal | + | Clumsiness; difficulties in fine bimanual activities | NA | NA | c.1999dupC/p.Arg667Profs*4 | Bierhals et al., 2018 [13] |
| M/6 | Caucasian | Motor delay | Normal | + | Clumsiness; difficulties in fine bimanual activities | NA | NA | c.1962delT/p.Phe654Leufs*46 | Bierhals et al., 2018 [13] |
| M/11 | Caucasian | Normal | Normal | + | Difficulties in fine bimanual activities, migraine | NA | NA | c.4211_4215dup/p.Ser1406Lysfs*22 | Bierhals et al., 2018 [13] |
| F/13 | Caucasian | Normal | NA | + | NA | NA | NA | c.4211_4215dup/p.Ser1406Lysfs*22 | Bierhals et al., 2018 [13] |
| M/4 | Ethiopian | Normal | Normal | + | - | Normal | - | c.2774dupA/Asn925Lysfs*17 | Sagi-Dain et al., 2020 [26] |
| F/9 | Iranian | Normal | NA | + | NA | Normal | - | c.1729delG/p.Glu577Argfs*12 | Thams et al., 2020 [27] |
| F/4 | Iranian | NA | NA | + | NA | NA | NA | c.1729delG/p.Glu577Argfs*12 | Thams et al., 2020 [27] |
| M/9 | Caucasian | NA | NA | + | Dyslexia | Normal | - | c.1466_1476del/p.Val489Glufs*15 | Thams et al., 2020 [27] |
| M/7 | Caucasian | Language delay | Normal | + | Language disorder; chorea; seizures | cACC | - | c.1466_1476del/p.Val489Glufs*15 | Thams et al., 2020 [27] |
| F/11 | North African | Language delay | Low average intellectual functioning | - | Reading difficulties; attention deficit | pACC | - | c.925delA/p.Thr309Profs*26 | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15] |
| M/12 | Caucasian | Motor and language delay | Low intellectual functioning | + | Global behavioural/academic impairments; ADHD | cACC | Colpocephaly; absence of cingulate gyrus and posterior commissure | c.2378T>G/p.Val793Gly | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15] |
| M/10 | Caucasian | Language delay | Borderline intellectual functioning | + | Global behavioural/academic impairments; ADHD | cACC | Colpocephaly; absence of cingulate gyrus and posterior commissure | c.2378T>G/p.Val793Gly | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15] |
| M/8 | Caucasian | Motor and language delay | Low intellectual functioning | + | Global behavioural/academic impairments; ADHD | cACC | Colpocephaly; absence of cingulate gyrus | c.2378T>G/p.Val793Gly | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15] |
| M/10 | Caucasian | Motor and language delay | Low intellectual functioning | + | ASD; seizures; behaviour problems; executive-attentive functions deficits; impaired coordination and ability to complete bimanual tasks | pACC | Colpocephaly | c.2414G>A/p.Gly805Glu | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15]; Knight et al., 2023 [4] |
| F/12 | Caucasian | Motor delay | Normal | + | Executive functioning problems; behaviour problems; high anxiety symptoms | Normal | - | c.2414G>A/p.Gly805Glu | Marsh et al., 2017 [7]; Spencer-Smith et al., 2020 [15]; Knight et al., 2023 [4] |
| F/2 | Israelian | Mild gross and fine motor delay | Normal cognitive and communication skills | + | - | pACC | Asymmetric ventriculomegaly | c. 2T>C/p.Met1* | Nissenkorn et al., 2021 [28] |
| M/7 | Caucasian | Global development delay | Low intellectual functioning | + | Alternating strabismus; language disorder; episodes of stiffness with hyperextension of the lower limbs | cACC | Colpocephaly | c.2426A>G/p.Tyr809Cys | This report |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Prato, A.; Cirnigliaro, L.; Maugeri, F.; Luca, A.; Giuliano, L.; Vitiello, G.; Errichiello, E.; Valente, E.M.; Del Giudice, E.; Mostile, G.; et al. Paroxysmal Dystonic Posturing Mimicking Nocturnal Leg Cramps as a Presenting Sign in an Infant with DCC Mutation, Callosal Agenesis and Mirror Movements. J. Clin. Med. 2024, 13, 1109. https://doi.org/10.3390/jcm13041109
Prato A, Cirnigliaro L, Maugeri F, Luca A, Giuliano L, Vitiello G, Errichiello E, Valente EM, Del Giudice E, Mostile G, et al. Paroxysmal Dystonic Posturing Mimicking Nocturnal Leg Cramps as a Presenting Sign in an Infant with DCC Mutation, Callosal Agenesis and Mirror Movements. Journal of Clinical Medicine. 2024; 13(4):1109. https://doi.org/10.3390/jcm13041109
Chicago/Turabian StylePrato, Adriana, Lara Cirnigliaro, Federica Maugeri, Antonina Luca, Loretta Giuliano, Giuseppina Vitiello, Edoardo Errichiello, Enza Maria Valente, Ennio Del Giudice, Giovanni Mostile, and et al. 2024. "Paroxysmal Dystonic Posturing Mimicking Nocturnal Leg Cramps as a Presenting Sign in an Infant with DCC Mutation, Callosal Agenesis and Mirror Movements" Journal of Clinical Medicine 13, no. 4: 1109. https://doi.org/10.3390/jcm13041109






