A Nomogram for Predicting ADHD and ASD in Child and Adolescent Mental Health Services (CAMHS)
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Outcome Variables
2.3. Potential Predictors
2.4. Statistical Analyses
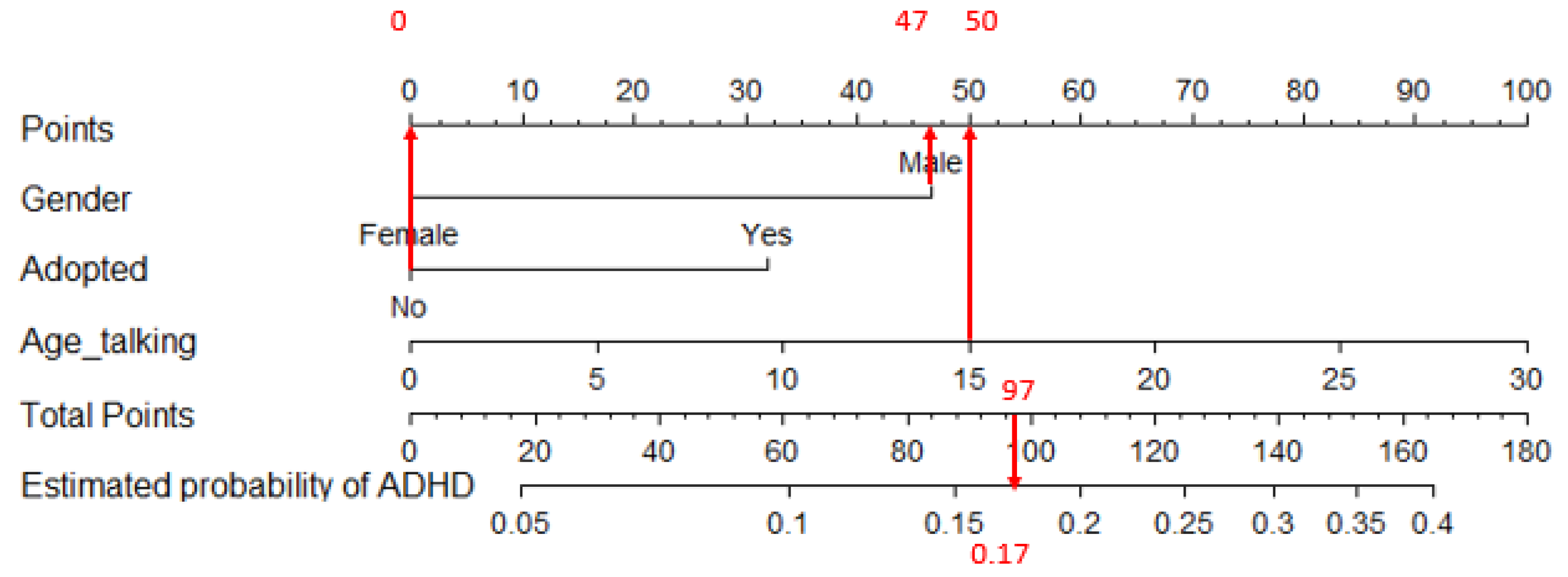
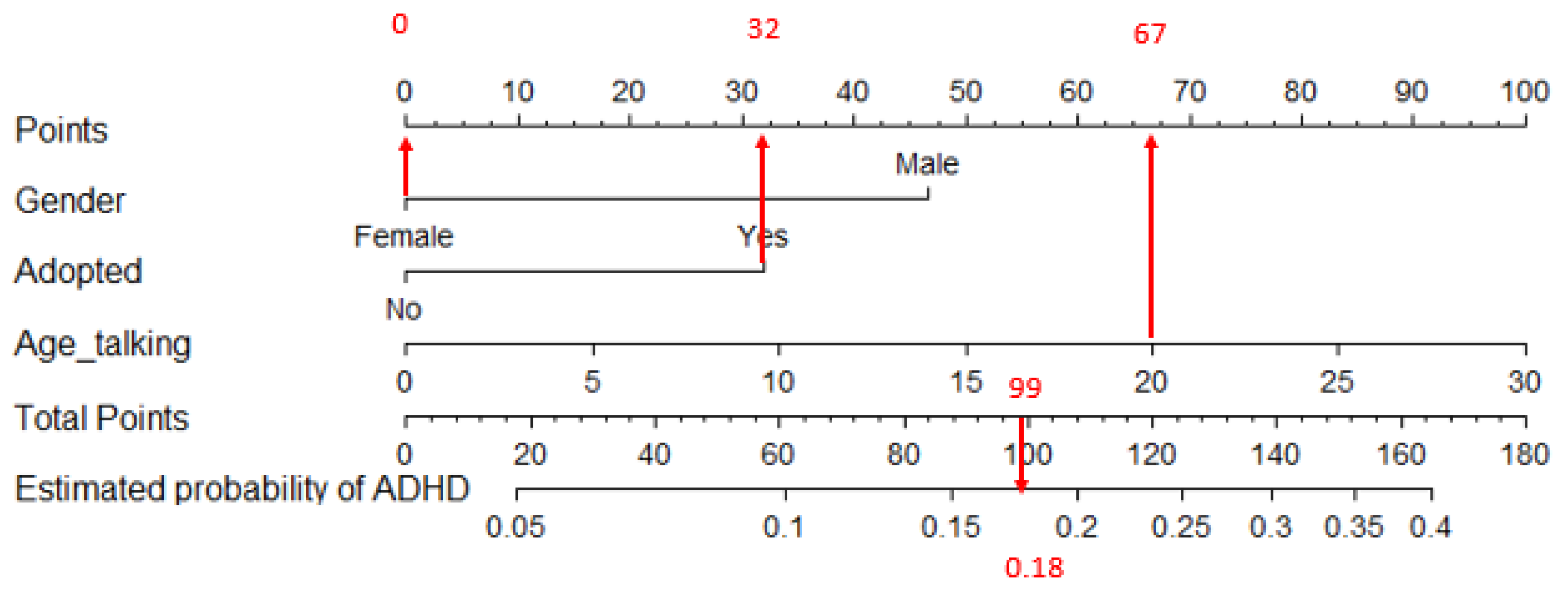
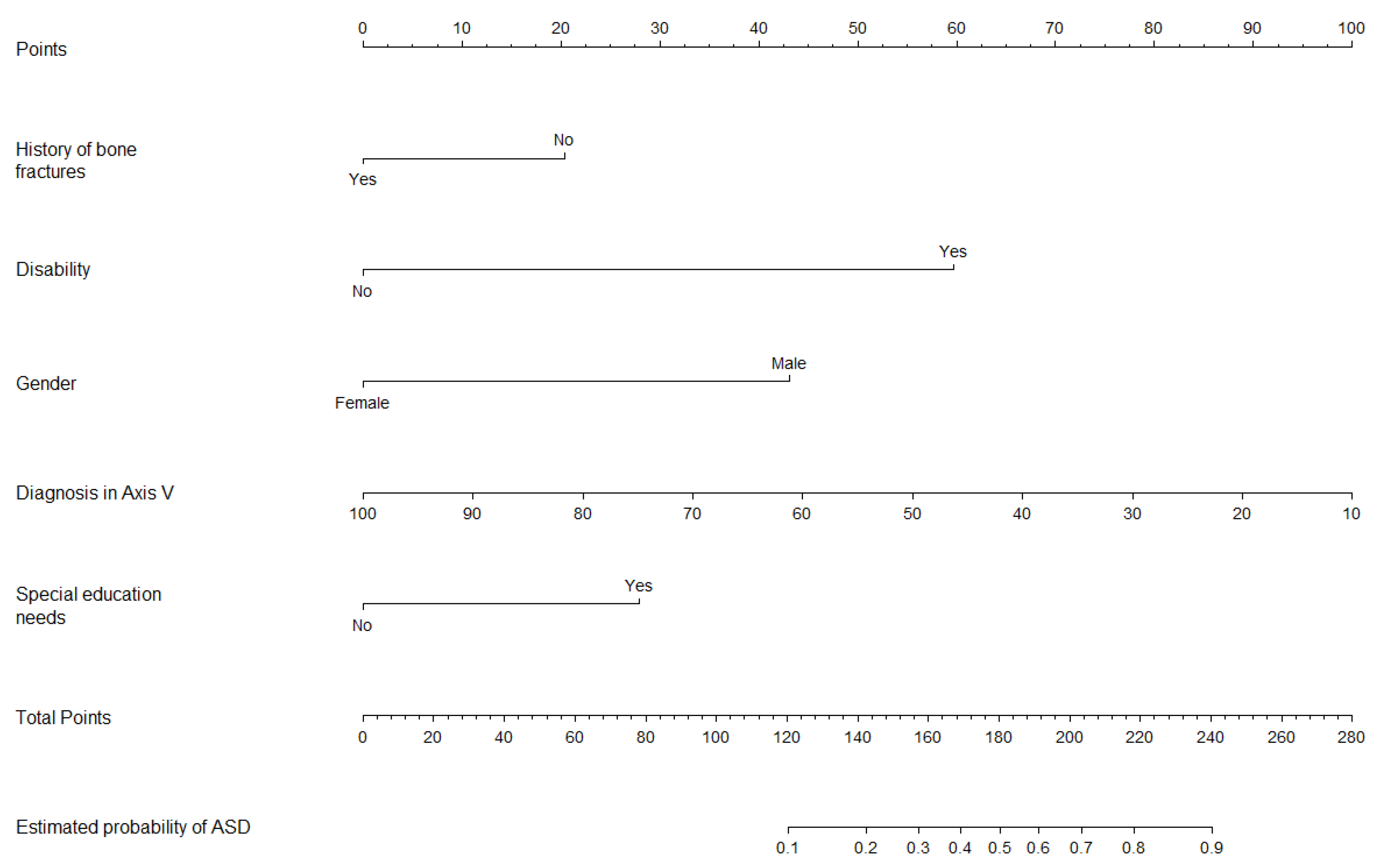
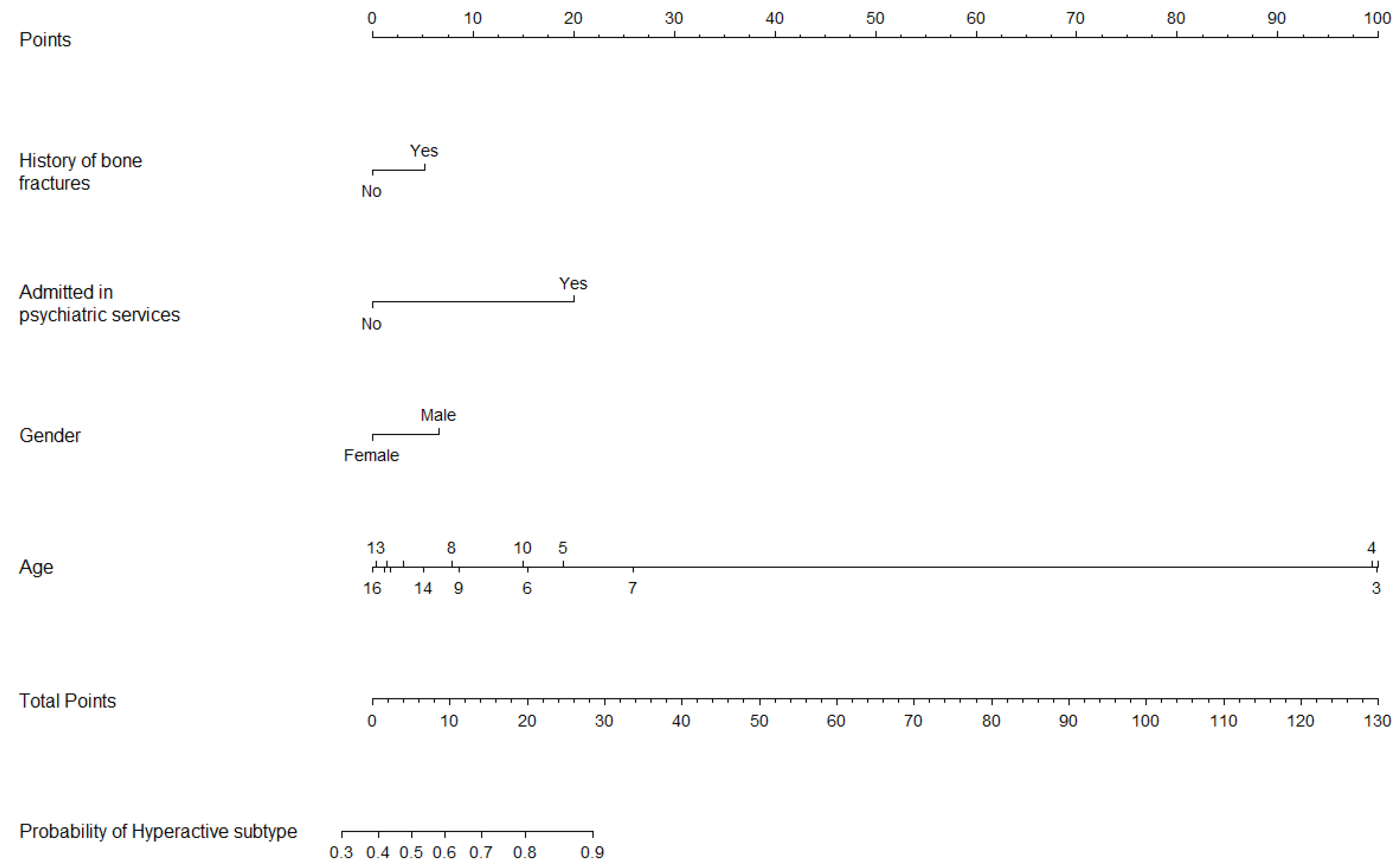
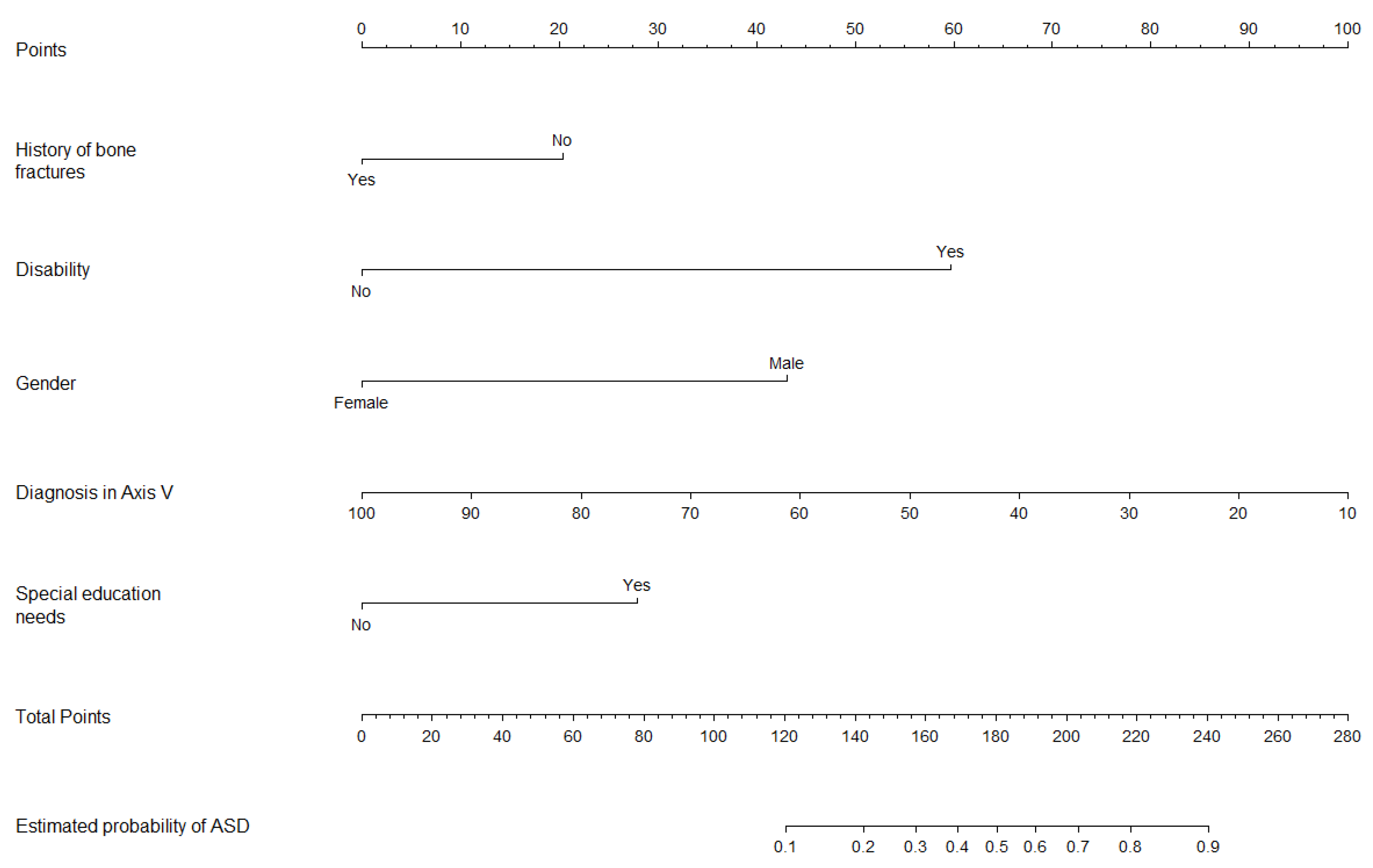
2.5. Graphical Outcomes: Nomograms
3. Results
4. Discussion
4.1. Predictors of ADHD
4.2. Predictors of ADHD, Hyperactive/Combined Subtype
4.3. Predictors of ASD
4.4. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Polanczyk, G.; De Lima, M.S.; Horta, B.L.; Biederman, J.; Rohde, L.A. The worldwide prevalence of ADHD: A systematic review and metaregression analysis. Am. J. Psychiatry 2007, 164, 942–948. [Google Scholar] [CrossRef] [PubMed]
- Polanczyk, G.V.; Willcutt, E.G.; Salum, G.A.; Kieling, C.; Rohde, L.A. ADHD prevalence estimates across three decades: An updated systematic review and meta-regression analysis. Int. J. Epidemiol. 2014, 43, 434–442. [Google Scholar] [CrossRef] [PubMed]
- Knopf, A. Autism prevalence increases from 1 in 60 to 1 in 54: CDC. Brown Univ. Child Adolesc. Behav. Lett. 2020, 36, 4. [Google Scholar]
- Sciberras, E.; DePetro, A.; Mensah, F.; Hiscock, H. Association between sleep and working memory in children with ADHD: A cross-sectional study. Sleep Med. 2015, 16, 1192–1197. [Google Scholar] [CrossRef]
- Kim, J.H.; Kim, J.Y.; Lee, J.; Jeong, G.H.; Lee, E.; Lee, S.; Lee, K.H.; Kronbichler, A.; Stubbs, B.; Solmi, M. Environmental risk factors, protective factors, and peripheral biomarkers for ADHD: An umbrella review. Lancet Psychiatry 2020, 7, 955–970. [Google Scholar] [CrossRef]
- Gurevitz, M.; Geva, R.; Varon, M.; Leitner, Y. Early markers in infants and toddlers for development of ADHD. J. Atten. Disord. 2014, 18, 14–22. [Google Scholar] [CrossRef]
- Modabbernia, A.; Velthorst, E.; Reichenberg, A. Environmental risk factors for autism: An evidence-based review of systematic reviews and meta-analyses. Mol. Autism 2017, 8, 13. [Google Scholar] [CrossRef]
- Lin, Y.; Wang, G.; Yang, Y.; Jin, X.; Huang, H.; Zhang, Y.; Jin, Z. Risk factors for ASD. J. Autism Dev. Disord. 2022, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Association, A.P. Diagnostic and Statistical Manual of Mental Disorders: DSM-5; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Brower, V. Biomarkers: Portents of malignancy. Nature 2011, 471, S19–S20. [Google Scholar] [CrossRef]
- Lee, D.; Jang, H.I.; Kim, H.J.; Bae, J.; Park, J.H. Development of a Machine-Learning Predictive Model for First-Grade Children at Risk for ADHD. Korean J. Childcare Educ. 2021, 17, 83–103. [Google Scholar]
- Tachmazidis, I.; Chen, T.; Adamou, M.; Antoniou, G. A hybrid AI approach for supporting clinical diagnosis of attention deficit hyperactivity disorder (ADHD) in adults. Health Inf. Sci. Syst. 2021, 9, 1. [Google Scholar] [CrossRef] [PubMed]
- Slobodin, O.; Yahav, I.; Berger, I. A machine-based prediction model of ADHD using CPT data. Front. Hum. Neurosci. 2020, 14, 560021. [Google Scholar] [CrossRef] [PubMed]
- Sen, B.; Borle, N.C.; Greiner, R.; Brown, M.R. A general prediction model for the detection of ADHD and Autism using structural and functional MRI. PLoS ONE 2018, 13, e0194856. [Google Scholar] [CrossRef] [PubMed]
- Maniruzzaman, M.; Shin, J.; Hasan, M.A.M. Predicting Children with ADHD Using Behavioral Activity: A Machine Learning Analysis. Appl. Sci. 2022, 12, 2737. [Google Scholar] [CrossRef]
- Garcia-Argibay, M.; Zhang-James, Y.; Cortese, S.; Lichtenstein, P.; Larsson, H.; Faraone, S.V. Predicting childhood and adolescent attention-deficit/hyperactivity disorder onset: A nationwide deep learning approach. Mol. Psychiatry 2023, 28, 1232–1239. [Google Scholar] [CrossRef] [PubMed]
- Silverstein, M.; Hironaka, L.K.; Feinberg, E.; Sandler, J.; Pellicer, M.; Chen, N.; Cabral, H. Using clinical data to predict accurate ADHD diagnoses among urban children. Clin. Pediatr. 2016, 55, 326–332. [Google Scholar] [CrossRef]
- Caye, A.; Agnew-Blais, J.; Arseneault, L.; Gonçalves, H.; Kieling, C.; Langley, K.; Menezes, A.; Moffitt, T.; Passos, I.; Rocha, T. A risk calculator to predict adult attention-deficit/hyperactivity disorder: Generation and external validation in three birth cohorts and one clinical sample. Epidemiol. Psychiatr. Sci. 2020, 29, e37. [Google Scholar] [CrossRef] [PubMed]
- Jagannatha, S.; Sargsyan, D.; Manyakov, N.V.; Skalkin, A.; Bangerter, A.; Ness, S.; Lewin, D.; Johnson, K.; Durham, K.; Pandina, G. A practical application of data mining methods to build predictive models for autism spectrum disorder based on biosensor data from Janssen Autism Knowledge Engine (JAKE®). Stat. Biopharm. Res. 2019, 11, 111–117. [Google Scholar] [CrossRef]
- Jiao, Y.; Chen, R.; Ke, X.; Chu, K.; Lu, Z.; Herskovits, E.H. Predictive models of autism spectrum disorder based on brain regional cortical thickness. Neuroimage 2010, 50, 589–599. [Google Scholar] [CrossRef]
- Wingfield, B.; Miller, S.; Yogarajah, P.; Kerr, D.; Gardiner, B.; Seneviratne, S.; Samarasinghe, P.; Coleman, S. A predictive model for paediatric autism screening. Health Inform. J. 2020, 26, 2538–2553. [Google Scholar] [CrossRef]
- Association, A.P. Diagnostic and Statistical Manual of Mental Disorders: DSM-IV; American Psychiatric Association: Washington, DC, USA, 1994; Volume 4. [Google Scholar]
- Kim, J.H. Multicollinearity and misleading statistical results. Korean J. Anesthesiol. 2019, 72, 558–569. [Google Scholar] [CrossRef] [PubMed]
- Pencina, M.J.; D’Agostino, R.B. Evaluating discrimination of risk prediction models: The C statistic. JAMA 2015, 314, 1063–1064. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Felix, B.; García-Esquinas, E.; Muriel, A.; Royuela, A.; Zamora, J. Bootstrap internal validation command for predictive logistic regression models. Stata J. 2021, 21, 498–509. [Google Scholar] [CrossRef]
- Harrell, F.E., Jr.; Harrell, M.F.E., Jr.; Hmisc, D. Package ‘rms’. Vanderbilt Univ. 2017, 229, Q8. [Google Scholar]
- Salmerón-Gómez, R.; García-García, C.; García-Pérez, J. A guide to using the r package “multicoll” for detecting multicollinearity. Comput. Econ. 2021, 57, 529–536. [Google Scholar] [CrossRef]
- Pohlabeln, H.; Rach, S.; De Henauw, S.; Eiben, G.; Gwozdz, W.; Hadjigeorgiou, C.; Molnár, D.; Moreno, L.A.; Russo, P.; Veidebaum, T. Further evidence for the role of pregnancy-induced hypertension and other early life influences in the development of ADHD: Results from the IDEFICS study. Eur. Child Adolesc. Psychiatry 2017, 26, 957–967. [Google Scholar] [CrossRef] [PubMed]
- Von Gontard, A.; Equit, M. Comorbidity of ADHD and incontinence in children. Eur. Child Adolesc. Psychiatry 2015, 24, 127–140. [Google Scholar] [CrossRef] [PubMed]
- Baeyens, D.; Roeyers, H.; Demeyere, I.; Verte, S.; Hoebeke, P.; Walle, J.V. Attention-deficit/hyperactivity disorder (ADHD) as a risk factor for persistent nocturnal enuresis in children: A two-year follow-up study. Acta Paediatr. 2005, 94, 1619–1625. [Google Scholar] [CrossRef] [PubMed]
- McKeown, C.; Hisle-Gorman, E.; Eide, M.; Gorman, G.H.; Nylund, C.M. Association of constipation and fecal incontinence with attention-deficit/hyperactivity disorder. Pediatrics 2013, 132, e1210–e1215. [Google Scholar] [CrossRef]
- Niemczyk, J.; Equit, M.; Hoffmann, L.; Von Gontard, A. Incontinence in children with treated attention-deficit/hyperactivity disorder. J. Pediatr. Urol. 2015, 11, 141.e1–141.e6. [Google Scholar] [CrossRef]
- Mellon, M.W.; Natchev, B.E.; Katusic, S.K.; Colligan, R.C.; Weaver, A.L.; Voigt, R.G.; Barbaresi, W.J. Incidence of enuresis and encopresis among children with attention-deficit/hyperactivity disorder in a population-based birth cohort. Acad. Pediatr. 2013, 13, 322–327. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Seens, H.; Modarresi, S.; MacDermid, J.C.; Walton, D.M.; Grewal, R. Prevalence of bone fractures among children and adolescents with attention-deficit/hyperactivity disorder: A systematic review and meta-analysis. BMC Pediatr. 2021, 21, 354. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.-W.; Shen, D.; Yan, Y.-t. ADHD, stimulant medication use, and the risk of fracture: A systematic review and meta-analysis. Arch. Osteoporos. 2021, 16, 81. [Google Scholar] [CrossRef] [PubMed]
- Chen, V.C.-H.; Yang, Y.-H.; Liao, Y.-T.; Kuo, T.-Y.; Liang, H.-Y.; Huang, K.-Y.; Huang, Y.-C.; Lee, Y.; McIntyre, R.S.; Lin, T.-C. The association between methylphenidate treatment and the risk for fracture among young ADHD patients: A nationwide population-based study in Taiwan. PLoS ONE 2017, 12, e0173762. [Google Scholar]
- Schermann, H.; Gurel, R.; Ankory, R.; Kadar, A.; Yoffe, V.; Snir, N.; Sternheim, A.; Karakis, I. Lower risk of fractures under methylphenidate treatment for ADHD: A dose–response effect. J. Orthop. Res. 2018, 36, 3328–3333. [Google Scholar] [CrossRef] [PubMed]
- Schermann, H.; Ankory, R.; Shlaifer, A.; Dolkart, O.; Rotman, D.; Yoffe, V.; Karakis, I.; Chechik, O. Lower risk of stress fractures in young adults with ADHD under chronic treatment with methylphenidate. Bone 2019, 120, 20–24. [Google Scholar] [CrossRef] [PubMed]
- Mattison, R.E.; Mayes, S.D. Relationships between learning disability, executive function, and psychopathology in children with ADHD. J. Atten. Disord. 2012, 16, 138–146. [Google Scholar] [CrossRef] [PubMed]
- Loyer Carbonneau, M.; Demers, M.; Bigras, M.; Guay, M.-C. Meta-analysis of sex differences in ADHD symptoms and associated cognitive deficits. J. Atten. Disord. 2021, 25, 1640–1656. [Google Scholar] [CrossRef] [PubMed]
- Shilon, Y.; Pollak, Y.; Aran, A.; Shaked, S.; Gross-Tsur, V. Accidental injuries are more common in children with attention deficit hyperactivity disorder compared with their non-affected siblings. Child Care Health Dev. 2012, 38, 366–370. [Google Scholar] [CrossRef]
- Max, J.E.; Schachar, R.J.; Levin, H.S.; Ewing-Cobbs, L.; Chapman, S.B.; Dennis, M.; Saunders, A.; Landis, J. Predictors of attention-deficit/hyperactivity disorder within 6 months after pediatric traumatic brain injury. J. Am. Acad. Child Adolesc. Psychiatry 2005, 44, 1032–1040. [Google Scholar] [CrossRef]
- Sabuncuoglu, O.; Taser, H.; Berkem, M. Relationship between traumatic dental injuries and attention-deficit/hyperactivity disorder in children and adolescents: Proposal of an explanatory model. Dent. Traumatol. 2005, 21, 249–253. [Google Scholar] [CrossRef] [PubMed]
- Nordström, T.; Hurtig, T.; Moilanen, I.; Taanila, A.; Ebeling, H. Disruptive behaviour disorder with and without attention deficit hyperactivity disorder is a risk of psychiatric hospitalization. Acta Paediatr. 2013, 102, 1100–1103. [Google Scholar] [CrossRef] [PubMed]
- Werling, D.M.; Geschwind, D.H. Sex differences in autism spectrum disorders. Curr. Opin. Neurol. 2013, 26, 146. [Google Scholar] [CrossRef] [PubMed]
- Giarelli, E.; Wiggins, L.D.; Rice, C.E.; Levy, S.E.; Kirby, R.S.; Pinto-Martin, J.; Mandell, D. Sex differences in the evaluation and diagnosis of autism spectrum disorders among children. Disabil. Health J. 2010, 3, 107–116. [Google Scholar] [CrossRef] [PubMed]
- Jensen, M.; Smolen, C.; Girirajan, S. Gene discoveries in autism are biased towards comorbidity with intellectual disability. J. Med. Genet. 2020, 57, 647–652. [Google Scholar] [CrossRef] [PubMed]
- Bertelli, M.O. ASD and intellectual disability. In Psychopathology in Adolescents and Adults with Autism Spectrum Disorders; Springer: Berlin/Heidelberg, Germany, 2019; pp. 111–130. [Google Scholar]
- McDonald, C.A.; Donnelly, J.P.; Feldman-Alguire, A.L.; Rodgers, J.D.; Lopata, C.; Thomeer, M.L. Special education service use by children with autism spectrum disorder. J. Autism Dev. Disord. 2019, 49, 2437–2446. [Google Scholar] [CrossRef] [PubMed]
- Rubenstein, E.; Daniels, J.; Schieve, L.A.; Christensen, D.L.; Van Naarden Braun, K.; Rice, C.E.; Bakian, A.V.; Durkin, M.S.; Rosenberg, S.A.; Kirby, R.S. Trends in special education eligibility among children with autism spectrum disorder, 2002–2010. Public Health Rep. 2018, 133, 85–92. [Google Scholar] [CrossRef]
- DiGuiseppi, C.; Levy, S.E.; Sabourin, K.R.; Soke, G.N.; Rosenberg, S.; Lee, L.-C.; Moody, E.; Schieve, L.A. Injuries in children with autism spectrum disorder: Study to Explore Early Development (SEED). J. Autism Dev. Disord. 2018, 48, 461–472. [Google Scholar] [CrossRef]
| Variable | Operationalization | Categories | Frequencies or Mean (sd) * |
|---|---|---|---|
| Age | How old (in years) is the patient? | Continuous variable | 11.1 (3.9) |
| Gender | What is the gender of the patient? | Male (0) or Female (1) | Male = 593 Female = 276 |
| Adopted | Was the child adopted? | Yes (1) or No (0) | No = 798 Yes = 52 |
| Family (first grade) psychiatric antecedents | Does the patient have any first-grade relative formally diagnosed with any mental disorder? | Yes (1) or No (0) | No = 332 Yes = 471 |
| Risky pregnancy | Was the patient’s gestation a risky pregnancy? | Yes (1) or No (0) | No = 608 Yes = 236 |
| Use of toxic substances by the mother during pregnancy | Did the patient’s mother take any toxic substances during pregnancy? | Yes (1) or No (0) | No = 783 Yes = 18 |
| Stress/depression during pregnancy | Did the patient’s mother suffer stress or depression during pregnancy? | Yes (1) or No (0) | No = 644 Yes = 192 |
| Preeclampsia during pregnancy | Did the patient’s mother suffer preeclampsia during pregnancy? | Yes (1) or No (0) | No = 805 Yes = 23 |
| Comorbidity in Axis I (Clinical Disorders) | Does the patient have a second Axis I diagnosis? | Yes (1) or No (0) | No = 245 Yes = 616 |
| Diagnosis in Axis III | Does the patient have a diagnosis of a disorder included in Axis III (general medical condition)? | No = 59 Yes = 809 | |
| Atopy | Did the patient suffer atopy? | Yes (1) or No (0) | No = 485 Yes = 371 |
| History of bone fractures or repetitive injuries evaluated or not at the ER? | Has the patient ever suffered a bone fracture? Has the patient had repetitive injuries evaluated at the ER? | Yes (1) or No (0) | No = 469 Yes = 378 |
| Diagnosis in Axis IV | Does the patient have a diagnosis of a disorder included in Axis IV (psychosocial problems)? | Yes (1) or No (0) | No = 187 Yes = 661 |
| Disability | Does the patient suffer any disability? | Yes (1) or No (0) | No = 717 Yes = 140 |
| Urine control (day and evening) | Does the patient control his/her urine? | Yes (1) or No (0) | No = 112 Yes = 713 |
| Fecal control | Does the patient control his/her feces? | Yes (1) or No (0) | No = 162 Yes = 761 |
| Started walking | Age (in months) at which the patient started walking | Continuous | 15.76 (8.35) |
| Special education needs | Does the patient have any special education needs? | Yes (1) or No (0) | No = 716 Yes = 108 |
| Genetics | Any confirmed genetic disease? | Yes (1) or No (0) | No = 801 Yes = 43 |
| Physically active | Does the patient exercise regularly? | Yes (1) or No (0) | No = 259 Yes = 573 |
| Admitted to the psychiatric acute inpatient unit? | Has the patient ever been admitted to the psychiatric acute inpatient unit? | Yes (1) or No (0) | No = 794 Yes = 50 |
| Admitted (hospitalization) in pediatric services | Has the patient ever been hospitalized in pediatric services? | Yes (1) or No (0) | No = 709 Yes = 130 |
| Medical treatment | Is the patient taking any medication regarding a general medical condition? | Yes (1) or No (0) | No = 399 Yes = 461 |
| Axis V score | Which is the global assessment scale? (0–100) | Continuous | 68.98 (12.16) |
| Total | ADHD (n = 599) | No ADHD (n = 246) | p | Hyperactive/Combined (n = 414) | Inattentive (n = 185) | p | ASD (n = 84) | No ASD (n = 84) | p | |
|---|---|---|---|---|---|---|---|---|---|---|
| Age | 11.1 (3.9) | 11.6 (3.5) 3–18 | 9.8 (4.6) 1.5–22 | <0.001 | 11.1 (3.5) | 12.7 (3.0) | <0.001 | 8.6 (4.4) | 11.3 (3.7) | <0.001 |
| Sex (% Female) | 31.7% | 29.9% | 35.4% | 0.139 | 29.6% | 39.5% | <0.001 | 11.9% | 33.6% | <0.001 |
| Nationality (% Spanish) | 84.9% | 85.0% | 84.5% | 0.9375 | 86.4% | 84.4% | 0.599 | 76.2% | 85.8% | 0.029 |
| Model | Factor | OR (95% CI) | VIF | Condition Number |
|---|---|---|---|---|
| ADHD (n = 632) | Constant | 11.68 | ||
| Risky pregnancy (No = 0, Yes = 1) | 1.85 (1.14, 3.00) | 1.063 | ||
| Age of first words (in months) | 0.86 (0.73, 1.02) | 1.125 | ||
| Urine control (No = 0, Yes = 1) | 0.32 (0.13, 0.88) | 1.630 | ||
| Fecal control (No = 0, Yes = 1) | 7.14 (2.56, 19.23) | 1.623 | ||
| Special educational needs (No = 0, Yes = 1) | 0.29 (0.13, 0.63) | 1.445 | ||
| Disability (No = 0, Yes = 1) | 0.34 (0.18, 0.67) | 1.425 | ||
| Physically active (No = 0, Yes = 1) | 1.63 (1.05, 2.52) | 1.052 | ||
| History of bone fractures (No = 0, Yes = 1) | 2.20 (1.44, 3.37) | 1.036 | ||
| Medical treatment (No = 0, Yes = 1) | 3.33 (2.17, 5.05) | 1.065 | ||
| Pediatric admission (No = 0, Yes = 1) | 0.44 (0.26, 0.74) | 1.023 | ||
| Psychiatric admission (No = 0, Yes = 1) | 0.29 (0.12, 0.70) | 1.023 | ||
| Comorbidity with Axis I diagnose (No = 0, Yes = 1) | 3.70 (2.32, 5.54) | 1.070 | ||
| ADHD subtype: Hyperactive/Combined (n = 551) | Constant | 2.79 | ||
| History of bone fractures (No = 0, Yes = 1) | 1.66 (1.14, 2.54) | 1.020 | ||
| Psychiatric admission (No = 0, Yes = 1) | 6.43 (1.36, 28.31) | 1.007 | ||
| Sex (Male = 0, Female = 1) | 0.60 (0.41, 0.89) | 1.058 | ||
| Age (in years) | 0.86 (0.81, 0.91) | 2.896 * | ||
| ASD (n = 634) | Constant | 3.02 | ||
| Special educational needs (No = 0, Yes = 1) | 2.78 (1.25, 6.20) | 1.685 | ||
| History of bone fractures (No = 0, Yes = 1) | 0.47 (0.24, 0.93) | 1.013 | ||
| Disability (No = 0, Yes = 1) | 8.90 (3.91, 20.28) | 1.723 | ||
| Sex (Male = 0, Female = 1) | 0.21 (0.09, 0.48) | 1.026 | ||
| Diagnostic in Axis V (No = 0, Yes = 1) | 0.66 (0.50, 0.89) | 1.751 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Blasco-Fontecilla, H.; Li, C.; Vizcaino, M.; Fernández-Fernández, R.; Royuela, A.; Bella-Fernández, M. A Nomogram for Predicting ADHD and ASD in Child and Adolescent Mental Health Services (CAMHS). J. Clin. Med. 2024, 13, 2397. https://doi.org/10.3390/jcm13082397
Blasco-Fontecilla H, Li C, Vizcaino M, Fernández-Fernández R, Royuela A, Bella-Fernández M. A Nomogram for Predicting ADHD and ASD in Child and Adolescent Mental Health Services (CAMHS). Journal of Clinical Medicine. 2024; 13(8):2397. https://doi.org/10.3390/jcm13082397
Chicago/Turabian StyleBlasco-Fontecilla, Hilario, Chao Li, Miguel Vizcaino, Roberto Fernández-Fernández, Ana Royuela, and Marcos Bella-Fernández. 2024. "A Nomogram for Predicting ADHD and ASD in Child and Adolescent Mental Health Services (CAMHS)" Journal of Clinical Medicine 13, no. 8: 2397. https://doi.org/10.3390/jcm13082397
APA StyleBlasco-Fontecilla, H., Li, C., Vizcaino, M., Fernández-Fernández, R., Royuela, A., & Bella-Fernández, M. (2024). A Nomogram for Predicting ADHD and ASD in Child and Adolescent Mental Health Services (CAMHS). Journal of Clinical Medicine, 13(8), 2397. https://doi.org/10.3390/jcm13082397






