Elevated Troponins after COVID-19 Hospitalization and Long-Term COVID-19 Symptoms: Incidence, Prognosis, and Clinical Outcomes—Results from a Multi-Center International Prospective Registry (HOPE-2)
Abstract
:1. Introduction
2. Material and Methods
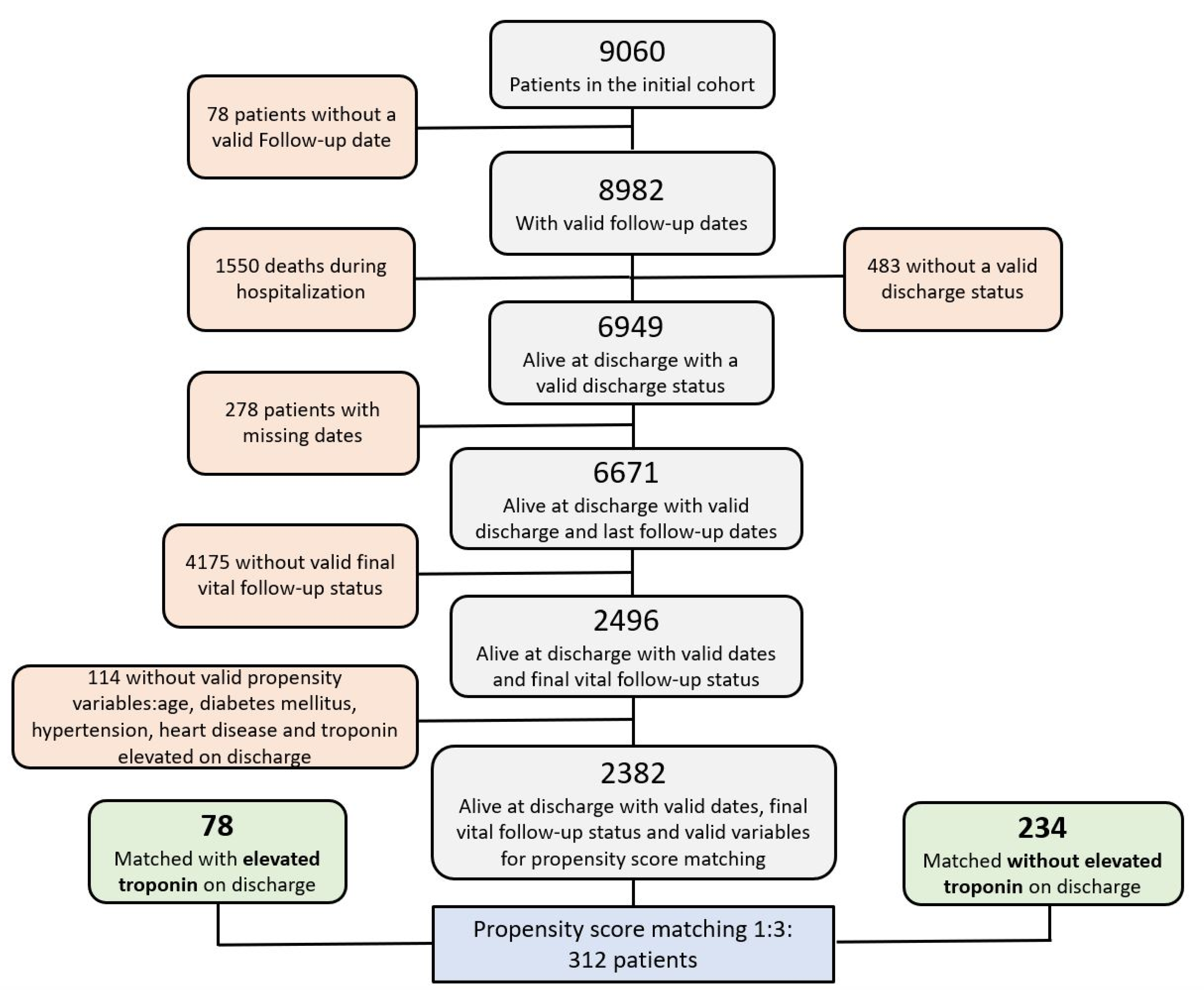
2.1. Study Design and Participation Criteria
2.2. Data Acquisition and Study Definitions
2.3. Study Follow-Up and Outcomes
2.4. Statistical Analysis
3. Results
4. Discussion
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. Available online: https://covid19.who.int/ (accessed on 17 February 2024).
- Lu, J.Q.; Lu, J.Y.; Wang, W.; Liu, Y.; Buczek, A.; Fleysher, R.; Hoogenboom, W.S.; Zhu, W.; Hou, W.; Rodriguez, C.J.; et al. Clinical predictors of acute cardiac injury and normalization of troponin after hospital discharge from COVID-19: Predictors of acute cardiac injury recovery in COVID-19. eBioMedicine 2022, 76, 103821. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [PubMed]
- Eggers, K.M.; Jernberg, T.; Lindahl, B. Cardiac Troponin Elevation in Patients without a Specific Diagnosis. J. Am. Coll. Cardiol. 2019, 73, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Nunez-Gil, I.J.; Fernandez-Perez, C.; Estrada, V.; Becerra-Munoz, V.M.; El-Battrawy, I.; Uribarri, A.; Fernandez-Rozas, I.; Feltes, G.; Viana-Llamas, M.C.; Trabattoni, D.; et al. Mortality risk assessment in Spain and Italy, insights of the HOPE COVID-19 registry. Intern. Emerg. Med. 2021, 16, 957–966. [Google Scholar] [CrossRef] [PubMed]
- Tersalvi, G.; Vicenzi, M.; Calabretta, D.; Biasco, L.; Pedrazzini, G.; Winterton, D. Elevated Troponin in Patients with Coronavirus Disease 2019: Possible Mechanisms. J. Card. Fail. 2020, 26, 470–475. [Google Scholar] [CrossRef] [PubMed]
- Shi, S.; Qin, M.; Cai, Y.; Liu, T.; Shen, B.; Yang, F.; Cao, S.; Liu, X.; Xiang, Y.; Zhao, Q.; et al. Characteristics and clinical significance of myocardial injury in patients with severe coronavirus disease 2019. Eur. Heart J. 2020, 41, 2070–2079. [Google Scholar] [CrossRef] [PubMed]
- Shi, S.; Qin, M.; Shen, B.; Cai, Y.; Liu, T.; Yang, F.; Gong, W.; Liu, X.; Liang, J.; Zhao, Q.; et al. Association of Cardiac Injury with Mortality in Hospitalized Patients with COVID-19 in Wuhan, China. JAMA Cardiol. 2020, 5, 802–810. [Google Scholar] [CrossRef] [PubMed]
- De Michieli, L.; Jaffe, A.S.; Sandoval, Y. Use and Prognostic Implications of Cardiac Troponin in COVID-19. Cardiol. Clin. 2022, 40, 287–300. [Google Scholar] [CrossRef] [PubMed]
- Kotecha, T.; Knight, D.S.; Razvi, Y.; Kumar, K.; Vimalesvaran, K.; Thornton, G.; Patel, R.; Chacko, L.; Brown, J.T.; Coyle, C.; et al. Patterns of myocardial injury in recovered troponin-positive COVID-19 patients assessed by cardiovascular magnetic resonance. Eur. Heart J. 2021, 42, 1866–1878. [Google Scholar] [CrossRef] [PubMed]
- Artico, J.; Shiwani, H.; Moon, J.C.; Gorecka, M.; McCann, G.P.; Roditi, G.; Morrow, A.; Mangion, K.; Lukaschuk, E.; Shanmuganathan, M.; et al. Myocardial Involvement after Hospitalization for COVID-19 Complicated by Troponin Elevation: A Prospective, Multicenter, Observational Study. Circulation 2023, 147, 364–374. [Google Scholar] [CrossRef] [PubMed]
- Chidambaram, V.; Kumar, A.; Calcaterra, G.; Mehta, J.L. Persistent cardiac injury—An important component of long COVID-19 syndrome. eBioMedicine 2022, 77, 103892. [Google Scholar] [CrossRef] [PubMed]
- Munblit, D.; O’Hara, M.E.; Akrami, A.; Perego, E.; Olliaro, P.; Needham, D.M. Long COVID: Aiming for a consensus. Lancet Respir Med. 2022, 10, 632–634. [Google Scholar] [CrossRef] [PubMed]
- Núñez-Gil, I.J.; Feltes, G.; Viana-Llamas, M.C.; Al, E. Post-COVID-19 Symptoms and Heart Disease: Incidence, Prognostic Factors, Outcomes and Vaccination: Results from a Multi-Center International Prospective Registry (HOPE 2). J. Clin. Med. 2023, 12, 706. [Google Scholar]
- Núñez-Gil, I.J.; Fernández-Ortiz, A.; Eid, C.M.; Huang, J.; Romero, R.; Becerra-Muñoz, V.M.; Uribarri, A.; Feltes, G.; Trabatoni, D.; Fernandez-Rozas, I.; et al. Underlying heart diseases and acute COVID-19 outcomes. Cardiol. J. 2021, 28, 202–214. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Leon, S.; Wegman-Ostrosky, T.; Perelman, C.; Sepulveda, R.; Rebolledo, P.A.; Cuapio, A.; Villapol, S. More than 50 long-term effects of COVID-19: A systematic review and meta-analysis. Sci. Rep. 2021, 11, 16144. [Google Scholar] [CrossRef] [PubMed]
- Santoro, F.; Núñez-Gil, I.J.; Vitale, E.; Viana-Llamas, M.C.; Romero, R.; Maroun Eid, C.; Feltes Guzman, G.; Becerra-Muñoz, V.M.; Fernández Rozas, I.; Uribarri, A.; et al. Aspirin Therapy on Prophylactic Anticoagulation for Patients Hospitalized with COVID-19: A Propensity Score-Matched Cohort Analysis of the HOPE-COVID-19 Registry. J. Am. Heart Assoc. 2022, 11, e024530. [Google Scholar] [CrossRef] [PubMed]
- Anon. Available online: https://www.cdc.gov/coronavirus/2019ncov/needextraprecautions/peopleathigherrisk.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fspecific-groups%2Fhigh-riskcomplications.html (accessed on 5 March 2024).
- Kim, D.H.; Park, H.C.; Cho, A.; Kim, J.; Yun, K.S.; Kim, J.; Lee, Y.K. Age-adjusted Charlson comorbidity index score is the best predictor for severe clinical outcome in the hospitalized patients with COVID-19 infection. Medicine 2021, 100, e25900. [Google Scholar] [CrossRef] [PubMed]
- Sonaglioni, A.; Lombardo, M.; Albini, A.; Noonan, D.M.; Re, M.; Cassandro, R.; Elia, D.; Caminati, A.; Nicolosi, G.L.; Harari, S. Charlson comorbidity index, neutrophil-to-lymphocyte ratio and undertreatment with renin-angiotensin-aldosterone system inhibitors predict in-hospital mortality of hospitalized COVID-19 patients during the omicron dominant period. Front. Immunol. 2022, 13, 958418. [Google Scholar] [CrossRef] [PubMed]
- Anon Madjid, M.; Solomon, S.; Vardeny, O. Cardiac Implications of Novel Coronavirus (COVID-19). In ACC Clinical Bulletin; Committee ASaQ, Ed.; American College of Cardiology: Washington, DC, USA; Available online: https://www.acc.org/latest-in-cardiology/articles/2020/02/13/12/42/acc-clinical-bulletin-focuses-on-cardiac-implications-of-coronavirus-2019-ncov (accessed on 18 February 2024).
- Zochios, V.; Valchanov, K. Raised cardiac troponin in intensive care patients with sepsis, in the absence of angiographically documented coronary artery disease: A systematic review. J. Intensive Care Soc. 2015, 16, 52–57. [Google Scholar] [CrossRef] [PubMed]
- Aleksova, A.; Fluca, A.L.; Gagno, G.; Pierri, A.; Padoan, L.; Derin, A.; Moretti, R.; Noveska, E.A.; Azzalini, E.; D’Errico, S.; et al. Long-term effect of SARS-CoV-2 infection on cardiovascular outcomes and all-cause mortality. Life Sci. 2022, 310, 121018. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Anon. Available online: https://www.who.int/publications-detail-redirect/WHO-2019-nCoV-Post_COVID19_condition-Clinical_case_definition2021.1#:~:text=Post%20COVID%2D19%20condition%20occurs,explained%20by%20an%20alterative%20diagnosis (accessed on 5 March 2024).
- Corbalán, J.A.; Feltes, G.; Silva, D.; Gómez-Utrero, E.; Núñez-Gil, I.J. A Quick and Practical Approach to Secure a Chronic Fatigue Syndrome Diagnosis: The Novel Functional Limitation Index. J. Clin. Med. 2023, 12, 7157. [Google Scholar] [CrossRef] [PubMed]
- Fulcher, K.Y.; White, P.D. Strength and physiological response to exercise in patients with chronic fatigue syndrome. J. Neurol. Neurosurg. Psychiatry 2000, 69, 302–307. [Google Scholar] [CrossRef] [PubMed]
- Banerjee, I.; Robinson, J.; Sathian, B. Treatment of Long COVID or Post COVID syndrome: A pharmacological approach. Nepal. J. Epidemiol. 2022, 12, 1220–1223. [Google Scholar] [CrossRef] [PubMed]
- Fernández-de-las-Peñas, C.; Martín-Guerrero, J.D.; Cancela-Cilleruelo, I.; Rodríguez-Jiménez, J.; Moro-López-Menchero, P.; Pellicer-Valero, O.J. Exploring trajectory recovery curves of post-COVID cognitive symptoms in previously hospitalized COVID-19 survivors: The LONG-COVID-EXP-CM multicenter study. J. Neurol. 2022, 269, 4613–4617. [Google Scholar] [CrossRef] [PubMed]
- Charman, S.J.; Velicki, L.; Okwose, N.C.; Harwood, A.; McGregor, G.; Ristic, A.; Banerjee, P.; Seferovic, P.M.; MacGowan, G.A.; Jakovljevic, D.G. Insights into heart failure hospitalizations, management, and services during and beyond COVID-19. ESC Heart Fail. 2021, 8, 175–182. [Google Scholar] [CrossRef] [PubMed]

| Matched Population (n = 312) | Elevated Troponin on Discharge (n = 78) | Not Elevated Troponin on Discharge (n = 234) | p-Value | ||
|---|---|---|---|---|---|
| Age (years) | 65.76 ± 14.90 | 65.69 ± 14.49 | 65.78 ± 14.73 | 0.966 | |
| Male | 188 (60.3%) | 46 (59%) | 142 (60.7%) | 0.789 | |
| Hypertension | 196 (62.8%) | 50 (64.1%) | 146 (62.4%) | 0.787 | |
| Obesity | 60 (19.2%) | 14 (17.9%) | 46 (19.7%) | 0.740 | |
| Diabetes Mellitus | 63 (20.2%) | 17 (21.8%) | 46 (19.7%) | 0.684 | |
| Dislipidaemia | 107 (34.3%) | 27 (34.6%) | 80 (34.2%) | 0.945 | |
| Active smoking | 42 (14%) | 19 (25.7%) | 23 (10.2%) | 0.001 | |
| Renal failure | 21 (6.7%) | 8 (10.3%) | 13 (5.6%) | 0.151 | |
| Lung disease | 68 (23.7%) | 14 (20.3%) | 54 (24.8%) | 0.446 | |
| Heart disease | 130 (41.67%) | 32 (41%) | 98 (41.9%) | 0.895 | |
| Cerebrovascular disease | 22 (7.1%) | 6 (7.7%) | 16 (6.8%) | 0.798 | |
| Connectivopathy | 8 (2.6%) | 1 (1.3%) | 7 (3%) | 0.684 | |
| Liver disease | 7 (2.2%) | 2 (2.6%) | 5 (2.1%) | 1.000 | |
| Cancer status | 34 (10.9%) | 8 (10.3%) | 26 (11.1%) | 0.834 | |
| Inmunosupression | 21 (6.7%) | 6 (7.7%) | 15 (6.4%) | 0.696 | |
| In hospital complications | Respiratory insufficiency | 135 (43.5%) | 38 (48.7%) | 97 (41.5%) | 0.262 |
| Heart failure | 29 (9.3%) | 16 (20.5%) | 13 (5.6%) | <0.001 | |
| Renal failure | 41 (13.1%) | 15 (19.2%) | 26 (11.1%) | 0.066 | |
| Upper respiratory tract infection | 39 (12.5%) | 11 (14.1%) | 28 (12%) | 0.621 | |
| Pneumonia | 231 (76.2%) | 60 (76.9%) | 171 (76%) | 0.869 | |
| Sepsis | 36 (11.5%) | 26 (33.3%) | 10 (4.3%) | <0.001 | |
| Systemic inflammatory response syndrome | 36 (11.5%) | 7 (9%) | 29 (12.4%) | 0.413 | |
| Relevant bleeding | 11 (3.5%) | 6 (7.7%) | 5 (2.1%) | 0.032 | |
| Hemoptysis | 9 (2.9%) | 6 (7.7%) | 3 (1.3%) | 0.009 * | |
| Embolic events | 6 (1.9%) | 3 (3.8%) | 3 (1.3%) | 0.168 | |
| Hospital readmission for any cause | 81 (26%) | 37 (47.4%) | 44 (18.8%) | <0.001 | |
| All-cause death | 19 (6.1%) | 14 (17.9%) | 5 (2.1%) | <0.001 | |
| Follow-up | 12.97; 8.60–14.79 | 12.60; 7.07–13.23 | 13; 9.60–15.54 | - | |
| Matched Population (n = 312) | Elevated Troponin on Discharge (n = 78) | Not Elevated Troponin on Discharge (n = 234) | p-Value | ||
|---|---|---|---|---|---|
| Any long-term COVID-19 symptoms | 210 (67.3%) | 57 (73.1%) | 153 (65.4%) | 0.210 | |
| Long-term COVID-19 cardiovascular traits | Fatigue | 140 (44.9%) | 45 (57.7%) | 95 (40.6%) | 0.009 |
| Dyspnea | 123 (39.4%) | 49 (62.8%) | 74 (31.6%) | <0.001 | |
| Dizziness | 48 (15.4%) | 23 (29.5%) | 25 (10.7%) | <0.001 | |
| Chest pain | 36 (11.5%) | 15 (19.2%) | 21 (9%) | 0.014 | |
| Acute coronary syndrome | 9 (2.9%) | 6 (7.7%) | 3 (1.3%) | 0.009 * | |
| Palpitations | 47 (15.1%) | 23 (29.5%) | 24 (10.3%) | <0.001 | |
| Increased resting heart rate | 13 (10.6%) | 14 (17.9%) | 19 (8.1%) | 0.015 | |
| Syncope | 6 (1.9%) | 2 (2.6%) | 4 (1.7%) | 0.642 * | |
| Arrhythmia | 41 (13.1%) | 20 (25.6%) | 21 (9%) | <0.001 | |
| Atrial fibrillation | 32 (10.3%) | 10 (12.8%) | 22 (9.4%) | 0.389 | |
| Peri/myocarditis | 5 (1.6%) | 5 (6.4%) | 0 (0%) | 0.001 * | |
| Inferior limb edema | 24 (7.7%) | 12 (15.4%) | 12 (5.1%) | 0.003 | |
| New onset hypertension | 13 (4.2%) | 3 (3.8%) | 10 (4.3%) | 1.000 | |
| New onset ventricular dysfunction | 21 (6.7%) | 15 (19.2%) | 6 (2.6%) | <0.001 | |
| Relevant bleeding | 2 (0.6%) | 1 (1.3%) | 1 (0.4%) | 0.438 * | |
| Long-term COVID-19 neuro-psychological traits | Headache | 27 (8.7%) | 3 (3.8%) | 24 (10.3%) | 0.081 * |
| Migraine | 13 (4.2%) | 1 (1.3%) | 12 (5.1%) | 0.197 * | |
| Ageusia | 22 (7.1%) | 5 (6.4%) | 17 (7.3%) | 0.798 | |
| Anosmia | 19 (6.1%) | 7 (9%) | 12 (5.1%) | 0.272 | |
| Attention disorder | 26 (8.3%) | 9 (11.5%) | 7 (7.3%) | 0.237 | |
| Memory loss | 11 (9.9%) | 10 (12.8%) | 21 (9%) | 0.325 | |
| Cognitive impairment | 21 (6.7%) | 8 (10.3%) | 13 (5.6%) | 0.151 | |
| Anxiety | 50 (16%) | 17 (21.8%) | 33 (14.1%) | 0.109 | |
| Depression | 33 (10.6%) | 13 (16.7%) | 20 (8.5%) | 0.043 | |
| Tinnitus or hearing loss | 13 (4.2%) | 6 (7.7%) | 7 (3%) | 0.098 * | |
| Sleep disorder | 46 (14.7%) | 10 (12.8%) | 36 (15.4%) | 0.580 | |
| Mood disorder | 39 (12.5%) | 14 (17.9%) | 25 (10.7%) | 0.093 | |
| Paraonia | 10 (3.2%) | 5 (6.4%) | 5 (2.1%) | 0.128 | |
| Other long-term COVID-19 symptoms | Cough | 47 (15.1%) | 21 (26.9%) | 26 (11.1%) | 0.001 |
| Reduced pulmonary diffusion test | 31 (9.9%) | 13 (16.7%) | 18 (7.7%) | 0.022 | |
| Polypnea | 18 (5.8%) | 8 (10.3%) | 10 (4.3%) | 0.087 | |
| Sleep apnea | 15 (4.8%) | 5 (6.4%) | 10 (4.3%) | 0.540 | |
| Digestive disorders | 22 (7.1%) | 10 (12.8%) | 12 (5.1%) | 0.022 | |
| Nausea/Vomiting | 13 (4.2%) | 5 (6.4%) | 8 (3.4%) | 0.323 | |
| Intermittent fever | 17 (5.4%) | 8 (10.3%) | 9 (3.8%) | 0.042 | |
| Chills | 17 (5.4%) | 9 (11.5%) | 8 (3.4%) | 0.017 | |
| Hair loss | 20 (6.4%) | 5 (6.4%) | 15 (6.4%) | 1.000 | |
| Joint pain | 34 (10.9%) | 7 (9%) | 27 (11.5%) | 0.529 | |
| Myalgias | 34 (10.9%) | 5 (6.4%) | 29 (12.4%) | 0.142 | |
| Significant sweating episodes | 8 (2.6%) | 1 (1.3%) | 7 (3%) | 0.684 * | |
| Significant weight loss | 24 (7.7%) | 3 (3.8%) | 21 (9%) | 0.141 * | |
| Cutaneous involvement | 14 (4.5%) | 3 (3.8%) | 11 (4.7%) | 1.000 * | |
| New onset diabetes mellitus | 7 (2.2%) | 2 (2.6%) | 5 (2.1%) | 1.000 * | |
| New onset renal failure | 22 (7.1%) | 13 (16.7%) | 9 (3.8%) | <0.001 | |
| Red eye symptoms | 4 (1.3%) | 0 (0%) | 4 (1.7%) | 0.575 * | |
| Flushing | 1 (0.3%) | 0 (0%) | 1 (0.4%) | 1.000 * | |
| Incident neoplasia | 6 (1.9%) | 3 (3.8%) | 3 (1.3%) | 0.168 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vazirani, R.; Feltes, G.; Hoyo, R.S.-d.; Viana-Llamas, M.C.; Raposeiras-Roubín, S.; Romero, R.; Alfonso-Rodríguez, E.; Uribarri, A.; Santoro, F.; Becerra-Muñoz, V.; et al. Elevated Troponins after COVID-19 Hospitalization and Long-Term COVID-19 Symptoms: Incidence, Prognosis, and Clinical Outcomes—Results from a Multi-Center International Prospective Registry (HOPE-2). J. Clin. Med. 2024, 13, 2596. https://doi.org/10.3390/jcm13092596
Vazirani R, Feltes G, Hoyo RS-d, Viana-Llamas MC, Raposeiras-Roubín S, Romero R, Alfonso-Rodríguez E, Uribarri A, Santoro F, Becerra-Muñoz V, et al. Elevated Troponins after COVID-19 Hospitalization and Long-Term COVID-19 Symptoms: Incidence, Prognosis, and Clinical Outcomes—Results from a Multi-Center International Prospective Registry (HOPE-2). Journal of Clinical Medicine. 2024; 13(9):2596. https://doi.org/10.3390/jcm13092596
Chicago/Turabian StyleVazirani, Ravi, Gisela Feltes, Rafael Sánchez-del Hoyo, María C. Viana-Llamas, Sergio Raposeiras-Roubín, Rodolfo Romero, Emilio Alfonso-Rodríguez, Aitor Uribarri, Francesco Santoro, Víctor Becerra-Muñoz, and et al. 2024. "Elevated Troponins after COVID-19 Hospitalization and Long-Term COVID-19 Symptoms: Incidence, Prognosis, and Clinical Outcomes—Results from a Multi-Center International Prospective Registry (HOPE-2)" Journal of Clinical Medicine 13, no. 9: 2596. https://doi.org/10.3390/jcm13092596











