Salivary IL-6 mRNA is a Robust Biomarker in Oral Squamous Cell Carcinoma
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patients and Control Subjects
2.2. Saliva Collection and Processing
2.3. Reverse Transcription and Real-Time Quantitative PCR (qPCR)
2.4. Enzyme-Linked Immune-Sorbent Assay (ELISA)
2.5. Immunohistochemistry (IHC)
2.6. Statistical Analysis
3. Results
3.1. Characteristics of Study Participants
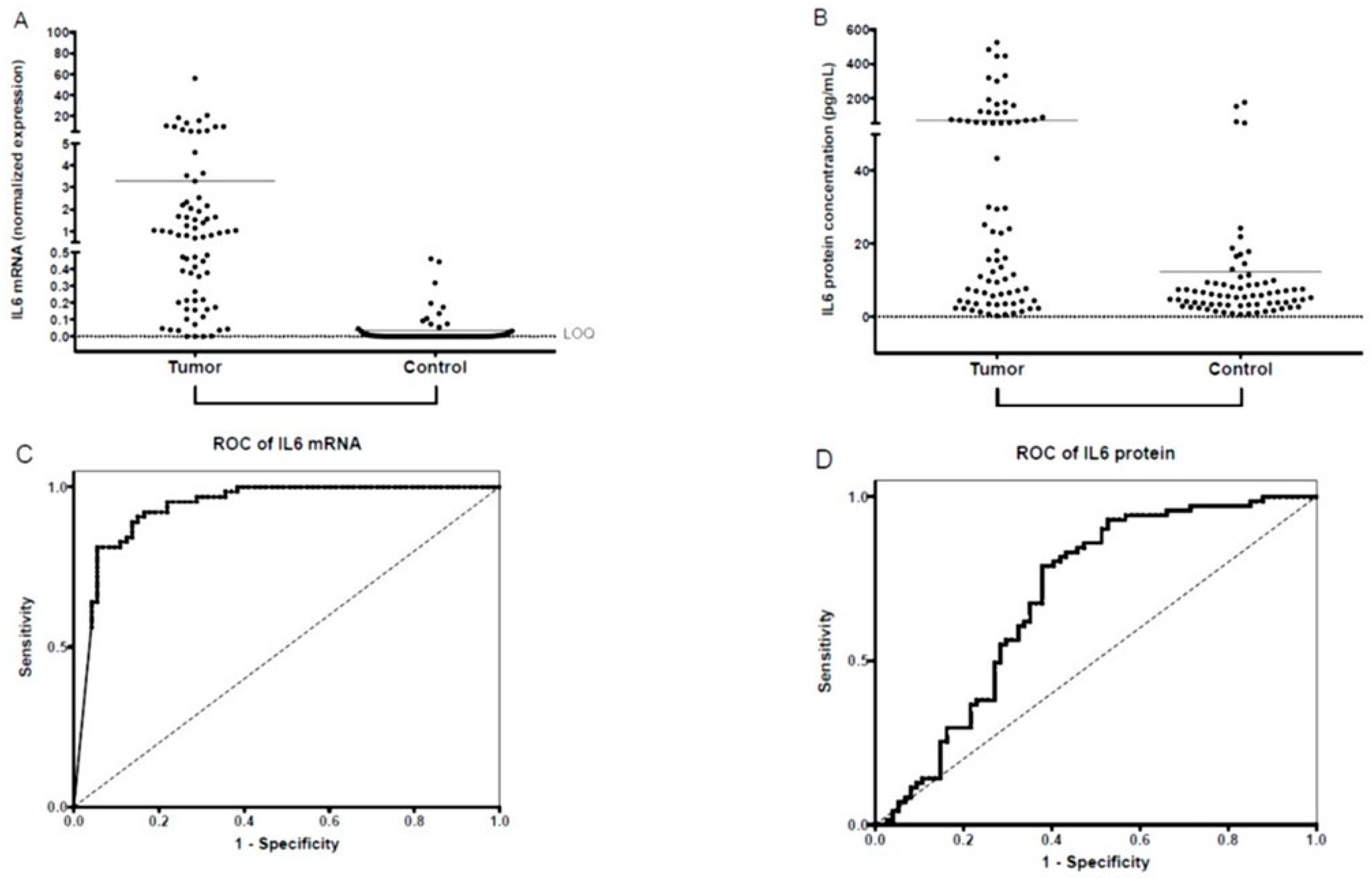
3.2. Salivary IL-6 mRNA and IL-6 Protein Expression
3.3. IL-6 Protein Expression in OSCC Tumor Tissue
4. Discussion
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Diz, P.; Meleti, M.; Diniz-Freitas, M.; Vescovi, P.; Warnakulasuriya, S.; Johnson, N.W.; Kerr, A.R. Oral and pharyngeal cancer in Europe: Incidence, mortality and trends as presented to the Global Oral Cancer Forum. Trans. Res. Oral Oncol. 2017, 2, 1–13. [Google Scholar] [CrossRef]
- Zhang, H.; Dziegielewski, P.T.; Biron, V.L.; Szudek, J.; Al-Qahatani, K.H.; O’Connell, D.A. Survival outcomes of patients with advanced oral cavity squamous cell carcinoma treated with multimodal therapy: A multi-institutional analysis. J. Otolaryngol. Head Neck Surg. 2013, 42, 30. [Google Scholar] [CrossRef] [PubMed]
- Carreras-Torras, C.; Gay-Escoda, C. Techniques for early diagnosis of oral squamous cell carcinoma: Systematic review. Med. Oral Patol. Oral Cir. Bucal. 2015, 20, e305–e315. [Google Scholar] [CrossRef] [PubMed]
- SahebJamee, M.; Eslami, M.; AtarbashiMoghadam, F.; Sarafnejad, A. Salivary concentration of TNFalpha, IL1 alpha, IL6, and IL8 in oral squamous cell carcinoma. Med. Oral Patol. Oral Cir. Bucal. 2008, 13, E292–E295. [Google Scholar] [PubMed]
- Wu, J.Y.; Yi, C.; Chung, H.R.; Wang, D.J.; Chang, W.C.; Lee, S.Y.; Lin, C.T.; Yang, Y.C.; Yang, W.C. Potential biomarkers in saliva for oral squamous cell carcinoma. Oral Oncol. 2010, 46, 226–231. [Google Scholar] [CrossRef]
- Panta, P.; Venna, V.R. Salivary RNA signatures in oral cancer detection. Anal. Cell. Pathol. 2014, 2014, 450629. [Google Scholar] [CrossRef]
- Khan, R.S.; Khurshid, Z.; Akhbar, S.; Faraz Moin, S. Advances of Salivary Proteomics in Oral Squamous Cell Carcinoma (OSCC) Detection: An Update. Proteomes 2016, 4, 41. [Google Scholar] [CrossRef]
- Radhika, T.; Jeddy, N.; Nithya, S.; Muthumeenakshi, R.M. Salivary biomarkers in oral squamous cell carcinoma—An insight. J. Oral Biol. Craniofac. Res. 2016, 6, S51–S54. [Google Scholar] [CrossRef]
- Lohavanichbutr, P.; Zhang, Y.; Wang, P.; Gu, H.; Nagana Gowda, G.A.; Djukovic, D.; Buas, M.F.; Raftery, D.; Chen, C. Salivary metabolite profiling distinguishes patients with oral cavity squamous cell carcinoma from normal controls. PLoS ONE 2018, 13, e0204249. [Google Scholar] [CrossRef]
- Zhao, S.Y.; Wang, J.; Ouyang, S.B.; Huang, Z.K.; Liao, L. Salivary Circular RNAs Hsa_Circ_0001874 and Hsa_Circ_0001971 as Novel Biomarkers for the Diagnosis of Oral Squamous Cell Carcinoma. Cell. Physiol. Biochem. 2018, 47, 2511–2521. [Google Scholar] [CrossRef]
- Sahibzada, H.A.; Khurshid, Z.; Khan, R.S.; Naseem, M.; Siddique, K.M.; Mali, M.; Zafar, M.S. Salivary IL-8, IL-6 and TNF-α as potential diagnostic biomarkers for oral cancer. Diagnostics 2017, 7, 21. [Google Scholar] [CrossRef] [PubMed]
- Horváth, J.; Szabó, A.; Tar, I.; Dezső, B.; Kiss, C.; Márton, I.; Scholtz, B. Oral health may affect the performance of mRNA-based saliva biomarkers for oral squamous cell cancer. Pathol. Oncol. Res. 2018, 24, 833–842. [Google Scholar] [CrossRef] [PubMed]
- Csősz, É.; Lábiscsák, P.; Kalló, G.; Márkus, B.; Emri, M.; Szabó, A.; Tar, I.; Tőzsér, J.; Kiss, C.; Márton, I. Proteomics investigation of OSCC-specific salivary biomarkers in a Hungarian population highlights the importance of identification of population-tailored biomarkers. PLoS ONE 2017, 12, e0177282. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Oral Health Surveys: Basic Methods, 4th ed.; World Health Organization: Geneva, Switzerland, 1997. [Google Scholar]
- Lang, N.P.; Corbet, E.F. Periodontal diagnosis in daily practice. Int. Dent. J. 1995, 45, 3–15. [Google Scholar] [PubMed]
- Pindborg, J.J.; Reichart, P.A.; Smith, C.J.; Van der Waal, I. Histological Typing of Cancer and Precancer of the Oral Mucosa. WHO International Histological Classification of Tumours, 2nd ed.; Springer: Berlin, Germany, 1997. [Google Scholar]
- Sobin, L.H.; Gospodarowitz, M.K.; Wittekind, C. Head and Neck Tumours: Lip and oral cavity. In TNM Classification of Malignant Tumours, 7th ed.; Wiley-Blackwell: Chichester, UK, 2010; pp. 25–29. [Google Scholar]
- Tsakiris, I.; Torocsik, D.; Gyongyosi, A.; Dozsa, A.; Szatmari, I.; Szanto, A.; Soos, G.; Nemes, Z.; Igali, L.; Marton, I.; et al. Carboxypeptidase-M is regulated by lipids and CSFs in macrophages and dendritic cells and expressed selectively in tissue granulomas and foam cells. Lab. Investig. 2012, 92, 345–361. [Google Scholar] [CrossRef] [PubMed]
- Szabó, K.; Papp, G.; Dezso, B.; Zeher, M. The histopathology of labial salivary glands in primary Sjögren’ syndrome: Focusing on follicular helper T cells in the inflammatory infiltrates. Mediators Inflamm. 2014, 2014, 631787. [Google Scholar] [CrossRef]
- Nemes, J.A.; Redl, P.; Boda, R.; Kiss, C.; Márton, I.J. Oral cancer report from Northeastern Hungary. Pathol. Oncol. Res. 2008, 14, 85–92. [Google Scholar] [CrossRef]
- Németh, Z.; Turi, K.; Léhner, G.; Veres, D.S.; Csurgay, K. The prognostic role of age in oral cancer. A clinical study. Magy. Onkol. 2013, 57, 166–172. (In Hungarian) [Google Scholar]
- St John, M.A.; Li, Y.; Zhou, X.; Denny, P.; Ho, C.M.; Montemagno, C.; Shi, W.; Qi, F.; Wu, B.; Sinha, U.; et al. Interleukin 6 and interleukin 8 as potential biomarkers for oral cavity and oropharyngeal squamous cell carcinoma. Arch. Otolaryngol. Head Neck Surg. 2004, 130, 929–935. [Google Scholar] [CrossRef]
- Brinkmann, O.; Kastratovic, D.A.; Dimitrijevic, M.V.; Konstantinovic, V.S.; Jelovac, D.B.; Antic, J.; Nesic, V.S.; Markovic, S.Z.; Martinovic, Z.R.; Akin, D.; et al. Oral squamous cell carcinoma detection by salivary biomarkers in Serbian population. Oral Oncol. 2011, 47, 51–55. [Google Scholar] [CrossRef]
- Gai, C.; Camussi, F.; Broccoletti, R.; Gambino, A.; Cabras, M.; Molinaro, L.; Carossa, S.; Camussi, G.; Arduino, P.G. Salivary extracellular vesicle-associated miRNAs as potential biomarkers in oral squamous cell carcinoma. BMC Cancer 2018, 18, 439. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.; Li, Q.; Chen, J.; Yi, P.; Xu, X.; Fan, Y.; Cui, B.; Yu, Y.; Li, X.; Du, Y.; et al. Salivary protease spectrum biomarkers of oral cancer. Int. J. Oral Sci. 2019, 11, 7. [Google Scholar] [CrossRef] [PubMed]
- Rhodus, N.L.; Ho, V.; Miller, C.S.; Myers, S.; Ondrey, F. NF-kappaB dependent cytokine levels in saliva of patients with oral paraneoplastic lesions and oral squamous cell carcinoma. Cancer Detect. Prev. 2005, 29, 42–45. [Google Scholar] [CrossRef] [PubMed]
- Duffy, S.A.; Taylor, J.M.; Terrell, J.E.; Islam, M.; Li, Y.; Wolf, G.T.; Teknos, T.N. Interleukin-6 predicts recurrence and survival among head and neck cancer patients. Cancer 2008, 113, 750–757. [Google Scholar] [CrossRef] [PubMed]
- Katakura, A.; Kamiyama, I.; Takano, N.; Shibahara, T.; Muramatsu, T.; Ishihara, K.; Takagi, R.; Shouno, T. Comparison of salivary cytokine levels in oral cancer patients and healthy subjects. Bull. Tokyo Dent. Coll. 2007, 48, 199–203. [Google Scholar] [CrossRef] [PubMed]
- Sato, J.; Goto, J.; Murata, T.; Kitamori, S.; Yamazaki, Y.; Satoh, A.; Kitagawa, Y. Changes in saliva interleukin-6 levels in patients with oral squamous cell carcinoma. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2010, 110, 330–336. [Google Scholar] [CrossRef] [PubMed]
- Korostoff, A.; Reder, L.; Masood, R.; Sinha, U.K. The role of salivary cytokine biomarkers in tongue cancer invasion and mortality. Oral Oncol. 2011, 47, 282–287. [Google Scholar] [CrossRef]
- Brailo, V.; Vucicevic-Boras, V.; Lukac, J.; Biocina-Lukenda, D.; Zilic-Alajbeg, I.; Milenovic, A.; Balija, M. Salivary and serum interleukin 1 beta, interleukin 6 and tumor necrosis factor alpha in patients with leukoplakia and oral cancer. Med. Oral Patol. Oral Cir. Bucal 2012, 17, e10–e15. [Google Scholar] [CrossRef]
- Lisa Cheng, Y.S.; Jordan, L.; Gorugantula, L.M.; Schneiderman, E.; Chen, H.S.; Rees, T. Salivary interleukin-6 and -8 in patients with oral cancer and patients with chronic oral inflammatory diseases. J. Periodontol. 2014, 85, 956–965. [Google Scholar] [CrossRef]
- Arduino, P.G.; Menegatti, E.; Cappello, N.; Martina, E.; Gardino, N.; Tanteri, C.; Cavallo, F.; Scully, C.; Broccoletti, R. Possible role for interleukins as biomarkers for mortality and recurrence in oral cancer. Int. J. Biol. Markers 2015, 30, e262–e266. [Google Scholar] [CrossRef]
- Panneer Selvam, N.; Sadaksharam, J. Salivary interleukin-6 in the detection of oral cancer and precancer. Asia. Pac. J. Clin. Oncol. 2015, 11, 236–241. [Google Scholar] [CrossRef]
- Rao, M.; Ramesh, A.; Adapa, S.; Thomas, B.; Shetty, J. Correlation of salivary levels of interleukin-6 and albumin with oral squamous cell carcinoma. J. Health Res. Rev. 2016, 3, 11–14. [Google Scholar] [CrossRef]
- Juretic, M.; Cerovic, R.; Belusic-Gobic, M.; Brekalo Prso, I.; Kqiku, L.; Spalj, S.; Pezelj-Ribaric, S. Salivary levels of TNF-α and IL-6 in patients with oral premalignant and malignant lesions. Folia Biol. 2013, 59, 99–102. [Google Scholar]
- Dikova, V.R.; Principe, S.; Bagan, J.V. Salivary inflammatory proteins in patients with oral potentially malignant disorders. J. Clin. Exp. Dent. 2019, 11, e659–e664. [Google Scholar] [CrossRef] [PubMed]
- Jinno, T.; Kawano, S.; Maruse, Y.; Matsubara, R.; Goto, Y.; Sakamoto, T.; Hashiguchi, Y.; Kaneko, N.; Tanaka, H.; Kitamura, R. Increased expression of interleukin-6 predicts poor response to chemoradiotherapy and unfavorable prognosis in oral squamous cell carcinoma. Oncol. Rep. 2015, 33, 2161–2168. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, T.; Kimura, T.; Ueta, E.; Tatemoto, Y.; Osaki, T. Characteristic cytokine generation patterns in cancer cells and infiltrating lymphocytes in oral squamous cell carcinomas and the influence of chemoradiation combined with immunotherapy on these patterns. Oncology 2003, 64, 407–415. [Google Scholar] [CrossRef]
- Petruzzi, M.N.; Cherubini, K.; Salum, F.G.; de Figueiredo, M.A. Role of tumour-associated macrophages in oral squamous cells carcinoma progression: An update on current knowledge. Diagn. Pathol. 2017, 12, 32. [Google Scholar] [CrossRef] [Green Version]
- Rossi, J.F.; Lu, Z.Y.; Jourdan, M.; Klein, B. Interleukin-6 as a therapeutic target. Clin. Cancer Res. 2015, 21, 1248–1257. [Google Scholar] [CrossRef]

| - | Patients (N = 95) | Controls (N = 80) | P | |
|---|---|---|---|---|
| Sex | Male | 60 (63%) | 30 (37%) | 0.004 * |
| Female | 35 (37%) | 50 (63%) | ||
| Age | (years; mean ± SD) | 61.7 ± 9.8 | 61.7 ± 9.2 | 0.982 ** |
| OSCC stage | ||||
| N = 70 | St I | 14 (20%) | – | na *** |
| St II | 22 (31%) | – | na *** | |
| St III | 13 (19%) | – | na*** | |
| St IV | 21 (30%) | – | na *** | |
| Histological grade | ||||
| N = 70 | G1 | 17 (24%) | – | na *** |
| G2 | 42 (60%) | – | na *** | |
| G3 | 11 (16%) | – | na *** | |
| DMFT | (N; mean ± SD) | 64; 27.6 ± 6.4 | 47; 24.8 ± 6.9 | 0.011 ** |
| GI | (N; mean ± SD) | 36; 0.53 ± 0.49 | 41; 0.42 ± 0.34 | 0.79 ** |
| Ethanol consumption | at least once a week | 46 (48%) | 14 (30%) | 0.035 * |
| less than once a week | 49 (52%) | 33 (70%) | ||
| Smoking | regular smoking | 62 (65%) | 8 (17%) | <0.001 * |
| non-smoker or occasional smoker | 33 (35%) | 40 (83%) |
| IL-6 mRNA Normalized Values | IL-6 Protein [pg/mL] | |||||||
|---|---|---|---|---|---|---|---|---|
| Sample | N | mean | SE | p * | N | mean | SE | p * |
| OSCC | ||||||||
| St I-II | 31 | 1.634 | 0.400 | <0.001 | 30 | 59.72 | 18.09 | <0.001 |
| St III-IV | 23 | 23.694 | 19.850 | <0.001 | 28 | 102.44 | 28.22 | <0.001 |
| G1 | 9 | 1.440 | 0.501 | <0.001 | 16 | 39.08 | 10.92 | 0.005 |
| G2 | 34 | 16.327 | 13.550 | <0.001 | 35 | 102.56 | 26.24 | <0.001 |
| G3 | 11 | 2.505 | 1.540 | <0.001 | 7 | 63.58 | 22.45 | 0.010 |
| Total | 74 | 3.301 | 0.885 | <0.001 | 74 | 70.98 | 14.06 | <0.001 |
| Control | 64 | 0.037 | 0.012 | 71 | 12.45 | 3.29 | ||
| In Transformed IL-6 mRNA | In Transformed IL-6 Protein | ||||
|---|---|---|---|---|---|
| Adjusted linear regression coefficient | p-value | Adjusted linear regression coefficient | p-value | ||
| Sex | female/male | −0.181 | 0.1 | −0.159 | 0.11 |
| Age | Year | 0.234 | 0.037 | 0.174 | 0.094 |
| DMFT | 0.234 | 0.037 | 0.174 | 0.094 | |
| Gingival index | 0.094 | 0.488 | 0.201 | 0.1 | |
| Alcohol consumption | |||||
| at least once a | |||||
| week/less than | 0.561 | 0.07 | −0.1 | 0.375 | |
| once a week | |||||
| Smoking | |||||
| regular smoking | |||||
| non-smoker or | −0.134 | 0.232 | 0.005 | 0.959 | |
| Occasional | |||||
| smoker | |||||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Márton, I.J.; Horváth, J.; Lábiscsák, P.; Márkus, B.; Dezső, B.; Szabó, A.; Tar, I.; Piffkó, J.; Jakus, P.; Barabás, J.; et al. Salivary IL-6 mRNA is a Robust Biomarker in Oral Squamous Cell Carcinoma. J. Clin. Med. 2019, 8, 1958. https://doi.org/10.3390/jcm8111958
Márton IJ, Horváth J, Lábiscsák P, Márkus B, Dezső B, Szabó A, Tar I, Piffkó J, Jakus P, Barabás J, et al. Salivary IL-6 mRNA is a Robust Biomarker in Oral Squamous Cell Carcinoma. Journal of Clinical Medicine. 2019; 8(11):1958. https://doi.org/10.3390/jcm8111958
Chicago/Turabian StyleMárton, Ildikó Judit, József Horváth, Péter Lábiscsák, Bernadett Márkus, Balázs Dezső, Adrienn Szabó, Ildikó Tar, József Piffkó, Petra Jakus, József Barabás, and et al. 2019. "Salivary IL-6 mRNA is a Robust Biomarker in Oral Squamous Cell Carcinoma" Journal of Clinical Medicine 8, no. 11: 1958. https://doi.org/10.3390/jcm8111958









