Falls from Height. Analysis of Predictors of Death in a Single-Center Retrospective Study
Abstract
1. Introduction
2. Materials and Methods
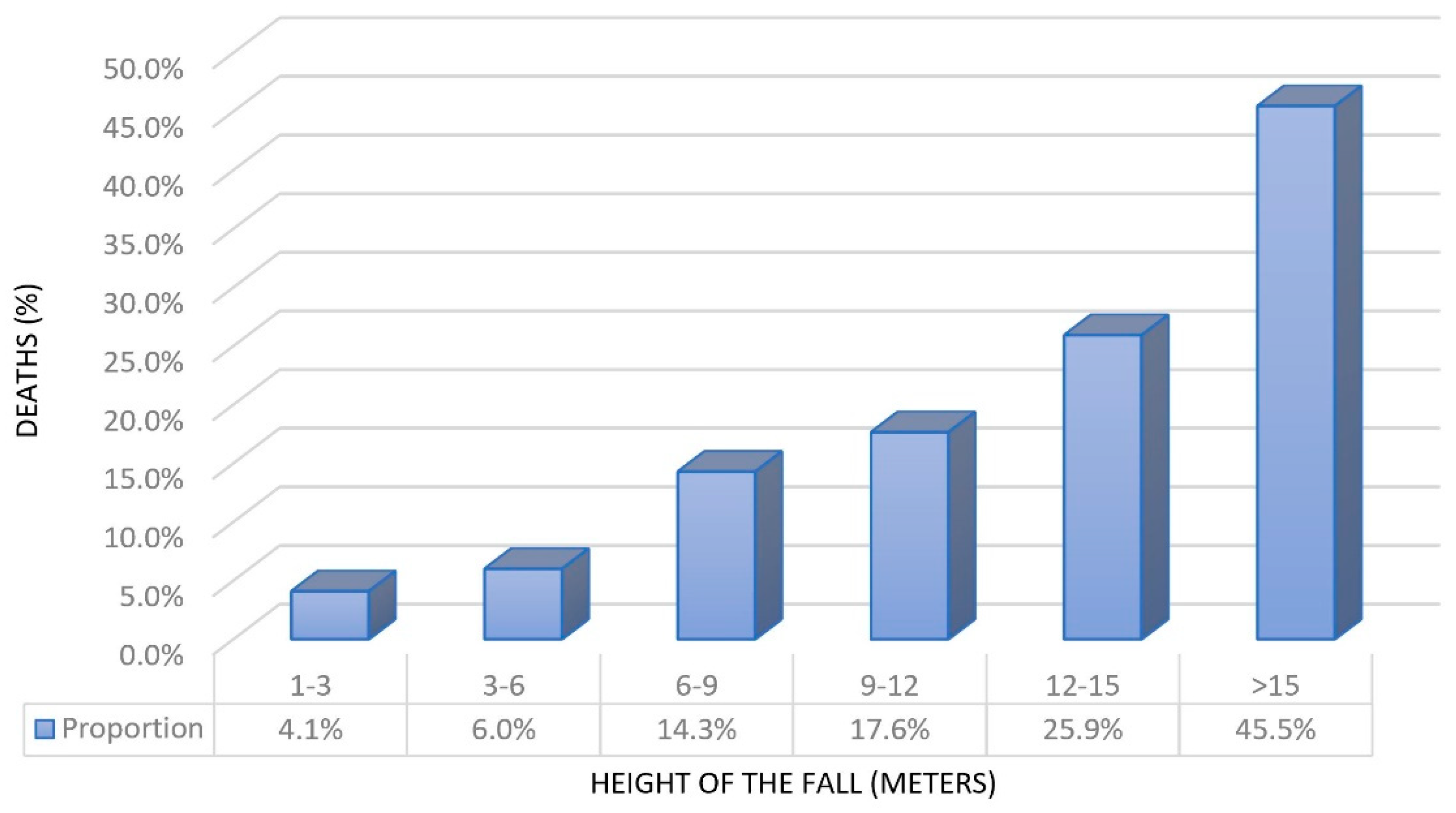
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. WHO Global Report on Falls Prevention in Older Age; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- Goren, S.; Subasi, M.; Týrasci, Y.; Gurkan, F. Fatal falls from heights in and around Diyarbakir, Turkey. Forensic Sci. Int. 2003, 137, 37–40. [Google Scholar] [CrossRef]
- Piazzalunga, D.; Rubertà, F.; Fugazzola, P.; Allievi, N.; Ceresoli, M.; Magnone, S.; Pisano, M.; Coccolini, F.; Tomasoni, M.; Montori, G.; et al. Suicidal fall from heights trauma: Difficult management and poor results. Eur. J. Trauma Emerg. Surg. 2019, 46, 383–388. [Google Scholar] [CrossRef] [PubMed]
- Richter, D.; Hahn, M.P.; Ostermann, P.A.W.; Ekkernkamp, A.; Muhr, G. Vertical deceleration injuries: A comparative study: A comparative study of the injury patterns of 101 patients after accidental and intentional high falls. Injury 1996, 27, 655–659. [Google Scholar] [CrossRef]
- Demetriades, D.; Murray, J.; Brown, C.; Velmahos, G.; Salim, A.; Alo, K.; Rhee, P. High-level falls: Type and severity of injuries and survival outcome according to age. J. Trauma-Inj. Infect. Crit. Care 2005, 58, 342–345. [Google Scholar] [CrossRef] [PubMed]
- Agalar, F.; Cakmakci, M.; Sayek, I. Factors effecting mortality in urban vertical free falls: Evaluation of 180 cases. Int. Surg. 1999, 84, 271–274. [Google Scholar] [PubMed]
- Centers for Disease Control. Report from the trauma registry workshop, including reccomendations for hospital based trauma registries. J. Trauma 1989, 29, 827–834. [Google Scholar] [CrossRef]
- Cothren, C.C.; Moore, E.E.; Hedegaard, H.B.; Meng, K. Epidemiology of urban trauma deaths: A comprehensive reassessment 10 years later. World J. Surg. 2007, 31, 1507–1511. [Google Scholar] [CrossRef] [PubMed]
- Lecomte, D.; Fornes, P. Suicide Among Youth and Young Adults, 15 Through 24 Years of Age, A Report of 392 Cases from Paris, 1989–1996. J. Forensic Sci. 1998, 43, 964–968. [Google Scholar] [CrossRef] [PubMed]
- Behera, C.; Rautji, R.; Dogra, T.D. Fatal accidental fall from height in infants and children: A study from South Delhi. Med. Sci. Law 2010, 50, 22–24. [Google Scholar] [CrossRef] [PubMed]
- Ehrnthaller, C.; Gebhard, F. 35 m Vertical Free Fall: How Impact Surface Influences Survival. Case Rep. Orthop. 2014, 2014, 805213. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Goodacre, S.; Than, M.; Goyder, E.C.; Joseph, A.P. Can the distance fallen predict serious injury after a fall from a height? J. Trauma-Inj. Infect. Crit. Care 1999, 46, 1055–1058. [Google Scholar] [CrossRef] [PubMed]
- Mathis, R.D.; Levine, S.H.; Phifer, S. An analysis of accidental free falls from a height: The ‘spring break’ syndrome. J. Trauma-Inj. Infect. Crit. Care 1993, 34, 123–126. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.C.; Wang, C.Y.; Shih, H.C.; Wen, Y.S.; Wu, J.J.K.; Huang, C.I.; Hsu, H.S.; Huang, M.H.; Huang, M.S. Prognostic factors for mortality following falls from height. Injury 2009, 40, 595–597. [Google Scholar] [CrossRef] [PubMed]
- Velmahos, G.C.; Demetriades, D.; Theodorou, D.; Cornwell, E.E.; Belzberg, H.; Asensio, J.; Murray, J.; Berne, T.V. Patterns of injury in victims of urban free-falls. World J. Surg. 1997, 21, 816–821. [Google Scholar] [CrossRef] [PubMed]
- Alizo, G.; Sciarretta, J.D.; Gibson, S.; Muertos, K.; Romano, A.; Davis, J.; Pepe, A. Fall from heights: Does height really matter? Eur. J. Trauma Emerg. Surg. 2018, 44, 411–416. [Google Scholar] [CrossRef] [PubMed]
- Lapostolle, F.; Gere, C.; Borron, S.W.; Pétrovic, T.; Dallemagne, F.; Beruben, A.; Lapandry, C.; Adnet, F. Prognostic factors in victims of falls from height. Crit. Care Med. 2005, 33, 1239–1242. [Google Scholar] [CrossRef] [PubMed]
- Chiara, O.; Mazzali, C.; Lelli, S.; Mariani, A.; Cimbanassi, S. A population based study of hospitalised seriously injured in a region of Northern Italy. World J. Emerg. Surg. 2013, 8, 32. [Google Scholar] [CrossRef] [PubMed]
- Teh, J.; Firth, M.; Sharma, A.; Wilson, A.; Reznek, R.; Chan, O. Jumpers and fallers: A comparison of the distribution of skeletal injury. Clin. Radiol. 2003, 58, 482–486. [Google Scholar] [CrossRef]
| Variables | Fallers (n = 733) | Jumpers (n = 215) | Total (n = 948) | p | |||
|---|---|---|---|---|---|---|---|
| Value | % | Value | % | Value | % | ||
| Gender | <0.001 | ||||||
| Male | 563 | 76.8 | 119 | 55.4 | 682 | 71.9 | |
| Female | 170 | 23.1 | 96 | 44.6 | 266 | 28.1 | |
| Age (median—IQR) | 42 | 19–60 | 39 | 26–55 | 42 | 22–59 | 0.732 |
| Median age (IQR) | |||||||
| Male | 44 | 23–59 | 38 | 28–54 | 42 | 25–58 | 0.72 |
| Female | 33 | 11–63 | 41 | 22–57 | 38 | 17–61 | 0.161 |
| ISS (median—IQR) | 9 | 4–21 | 29 | 13–43 | 12 | 5–26 | <0.001 |
| Height of fall | 2 | 2–4 | 7 | 5–9 | 3 | 2–6 | <0.001 |
| Anatomical districts of injuries (AIS ≥ 3) | |||||||
| Head | 183 | 25.0 | 66 | 30.7 | 249 | 26.3 | 0.095 |
| Chest | 179 | 24.4 | 128 | 59.5 | 307 | 32.4 | <0.001 |
| Abdomen | 56 | 7.6 | 63 | 29.3 | 119 | 12.6 | <0.001 |
| Extremity (AIS ≥ 2) | 278 | 37.9 | 166 | 77.2 | 444 | 46.8 | <0.001 |
| Outcome | <0.001 | ||||||
| Survived | 695 | 94.8 | 171 | 79.5 | 866 | 91.4 | |
| Deceased | 38 | 5.2 | 44 | 20.5 | 82 | 8.6 | |
| Variables | Survived (n = 866) | Dead (n = 82) | Total (n = 948) | p | |||
|---|---|---|---|---|---|---|---|
| Value | % | Value | % | Value | % | ||
| Age (median—IQR) | 40 | 20–57 | 60 | 40–76 | 42 | 22–59 | <0.001 |
| Age groups | <0.001 | ||||||
| ≤17 | 192 | 22.2 | 4 | 4.9 | 196 | 20.7 | |
| 18–64 | 545 | 62.9 | 43 | 52.4 | 588 | 62 | |
| ≥65 | 129 | 14.9 | 35 | 42.7 | 164 | 17.3 | |
| Gender | 0.125 | ||||||
| Male | 629 | 72.6 | 53 | 64.6 | 682 | 71.9 | |
| Female | 237 | 27.4 | 29 | 35.4 | 266 | 28.1 | |
| ASA score | 0.001 | ||||||
| ASA ≤ 2 | 798 | 92.1 | 65 | 7.5 | 863 | 91.0 | |
| ASA ≥ 3 | 68 | 7.9 | 17 | 20.7 | 85 | 9.0 | |
| Intentionality of the fall | <0.001 | ||||||
| Accidental | 695 | 80.3 | 38 | 46.3 | 733 | 77.3 | |
| Intentional | 171 | 19.7 | 44 | 53.7 | 215 | 22.7 | |
| Anatomical districts of injuries (AIS ≥ 3) | |||||||
| Head | 191 | 22.1 | 58 | 70.7 | 249 | 26.3 | <0.001 |
| Chest | 245 | 28.3 | 62 | 75.6 | 307 | 32.4 | <0.001 |
| Abdomen | 95 | 11.0 | 24 | 29.3 | 119 | 12.6 | <0.001 |
| Extremity (AIS ≥ 2) | 389 | 44.9 | 55 | 67.1 | 444 | 46.8 | <0.001 |
| ISS (median—IQR) | 9 | 4–22 | 42 | 29–59 | 12 | 5–26 | <0.001 |
| Height of the fall (m)—(Median/IQR) | 3 | 2–5 | 6 | 3–9 | 3 | 2–6 | <0.001 |
| Variables | p | OR | 95% CI | |
|---|---|---|---|---|
| Lower | Upper | |||
| Age | <0.001 | 1.04 | 1.03 | 1.06 |
| Height of the fall (m) | <0.001 | 1.16 | 1.08 | 1.25 |
| Intentional fall | 0.003 | 2.73 | 1.42 | 5.26 |
| Head injuries AIS ≥ 3 | <0.001 | 7.64 | 4.28 | 13.64 |
| Chest injuries AIS ≥ 3 | 0.003 | 2.69 | 1.41 | 5.13 |
| Abdomen AIS ≥ 3 | 0.71 | 1.14 | 0.57 | 2.26 |
| Extremities AIS ≥ 2 | 0.56 | 0.82 | 0.42 | 1.60 |
| ASA score ≥ 3 | 0.26 | 1.52 | 0.73 | 3.13 |
| Age Group ≤ 17 (196 Patients) | ||||
| Variables | p | OR | 95% CI | |
| Lower | Upper | |||
| Height of the fall (m) | 0.164 | 1.607 | 0.824 | 3.134 |
| Intentional fall | 0.571 | 0.284 | 0.004 | 22.188 |
| Head injuries AIS ≥ 3 | 0.994 | - | - | - |
| Chest injuries AIS ≥ 3 | 0.992 | - | - | - |
| Abdomen AIS ≥ 3 | 0.998 | - | - | - |
| Extremities AIS ≥ 2 | 0.237 | - | - | - |
| ASA score ≥ 3 | 0.999 | - | - | - |
| Age Group 18–65 (588 Patients) | ||||
| Variables | p | OR | 95% CI | |
| Lower | Upper | |||
| Height of the fall (m) | 0.002 | 1.12 | 1.05 | 1.20 |
| Intentional fall | 0.013 | 2.87 | 1.25 | 6.59 |
| Head injuries AIS ≥ 3 | <0.001 | 8.93 | 4.04 | 19.71 |
| Chest injuries AIS ≥ 3 | 0.005 | 3.48 | 1.45 | 8.38 |
| Abdomen AIS ≥ 3 | 0.83 | 1.10 | 0.46 | 2.61 |
| Extremities AIS ≥ 2 | 0.78 | 0.88 | 0.36 | 2.15 |
| ASA score ≥ 3 | 0.93 | 1.02 | 0.58 | 1.82 |
| Age group ≥ 65 (164 patients) | ||||
| Variables | p | OR | 95% CI | |
| Lower | Upper | |||
| Height of the fall (m) | 0.45 | 1.09 | 0.87 | 1.36 |
| Intentional fall | 0.067 | 3.24 | 0.92 | 11.41 |
| Head injuries AIS ≥ 3 | <0.001 | 5.45 | 2.10 | 14.17 |
| Chest injuries AIS ≥ 3 | 0.19 | 1.93 | 0.72 | 5.17 |
| Abdomen AIS ≥ 3 | 0.42 | 1.69 | 0.47 | 6.07 |
| Extremities AIS ≥ 2 | 0.87 | 0.92 | 0.31 | 2.74 |
| ASA score ≥ 3 | 0.13 | 1.64 | 0.86 | 3.12 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Casati, A.; Granieri, S.; Cimbanassi, S.; Reitano, E.; Chiara, O. Falls from Height. Analysis of Predictors of Death in a Single-Center Retrospective Study. J. Clin. Med. 2020, 9, 3175. https://doi.org/10.3390/jcm9103175
Casati A, Granieri S, Cimbanassi S, Reitano E, Chiara O. Falls from Height. Analysis of Predictors of Death in a Single-Center Retrospective Study. Journal of Clinical Medicine. 2020; 9(10):3175. https://doi.org/10.3390/jcm9103175
Chicago/Turabian StyleCasati, Alberto, Stefano Granieri, Stefania Cimbanassi, Elisa Reitano, and Osvaldo Chiara. 2020. "Falls from Height. Analysis of Predictors of Death in a Single-Center Retrospective Study" Journal of Clinical Medicine 9, no. 10: 3175. https://doi.org/10.3390/jcm9103175
APA StyleCasati, A., Granieri, S., Cimbanassi, S., Reitano, E., & Chiara, O. (2020). Falls from Height. Analysis of Predictors of Death in a Single-Center Retrospective Study. Journal of Clinical Medicine, 9(10), 3175. https://doi.org/10.3390/jcm9103175






