Changes in High-Density Lipoproteins Related to Outcomes in Patients with Acute Stroke
Abstract
:1. Introduction
2. Material and Methods
2.1. Patient Selection
2.2. Plasma Sampling
2.3. Plasma Cytokines and Chemokines Quantification
2.4. Lipid Assay
2.5. HDL Isolation by Ultracentrifugation
2.6. Western Blot Analyses of HDL
2.7. In Vitro BBB-Functionality Assay
2.8. RNA Isolation/RT-PCR Analysis
2.9. Determination of the Capacity of HDLs to Inhibit LDL Oxidation
2.10. Statistical Analysis
3. Results
3.1. Patient Characteristics
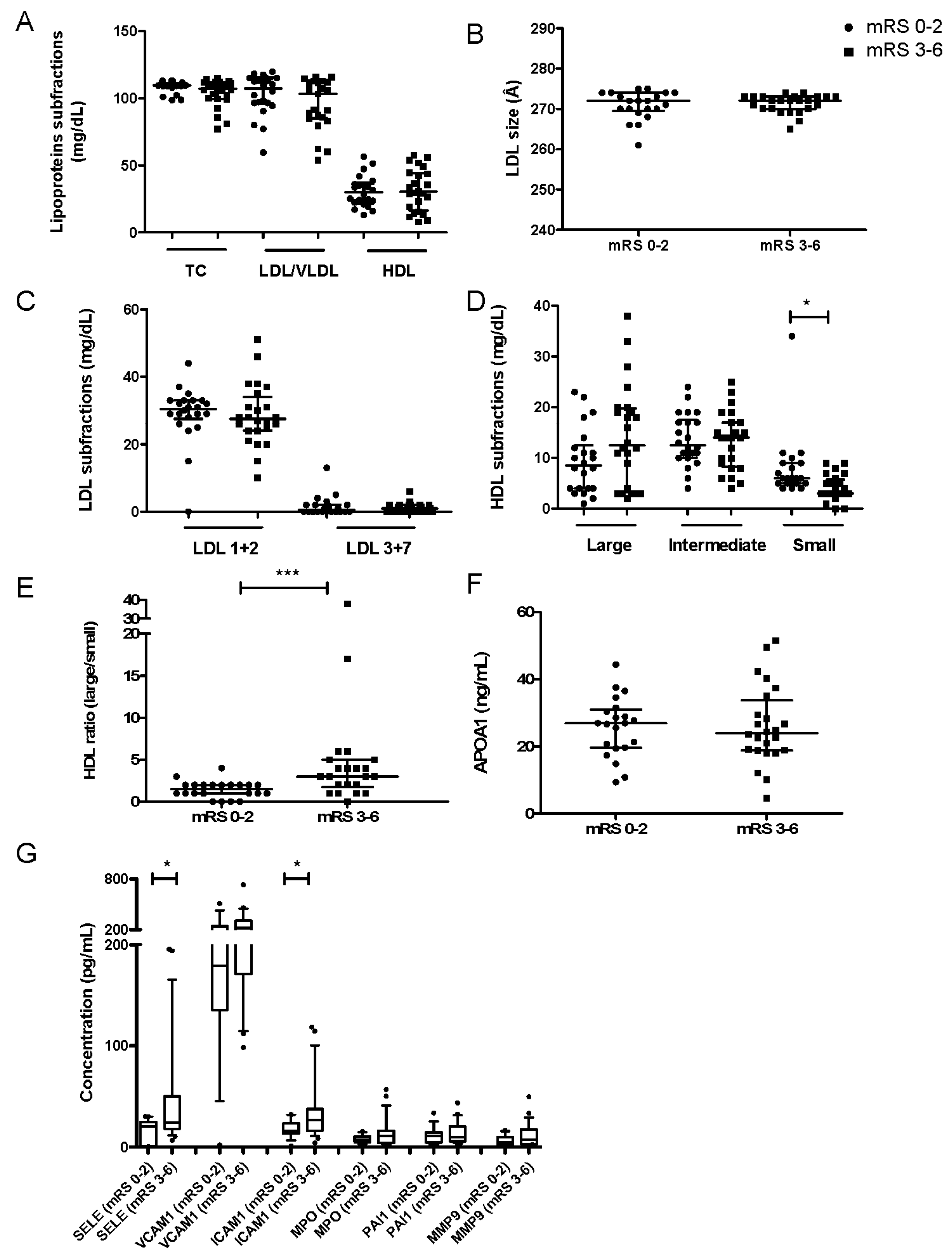
3.2. Plasmatic Parameters
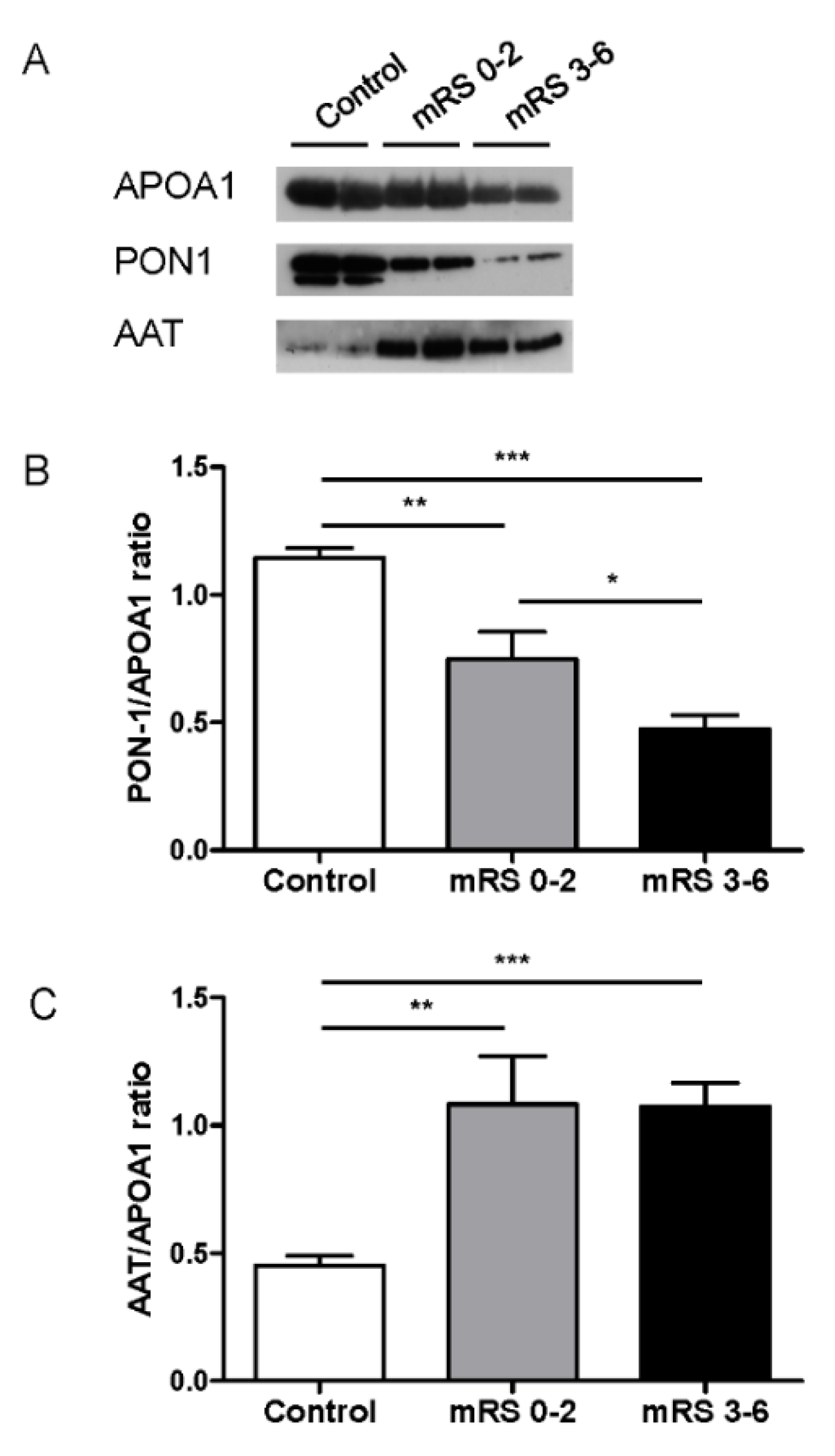
3.3. HDL-Associated Proteins
3.4. Correlations
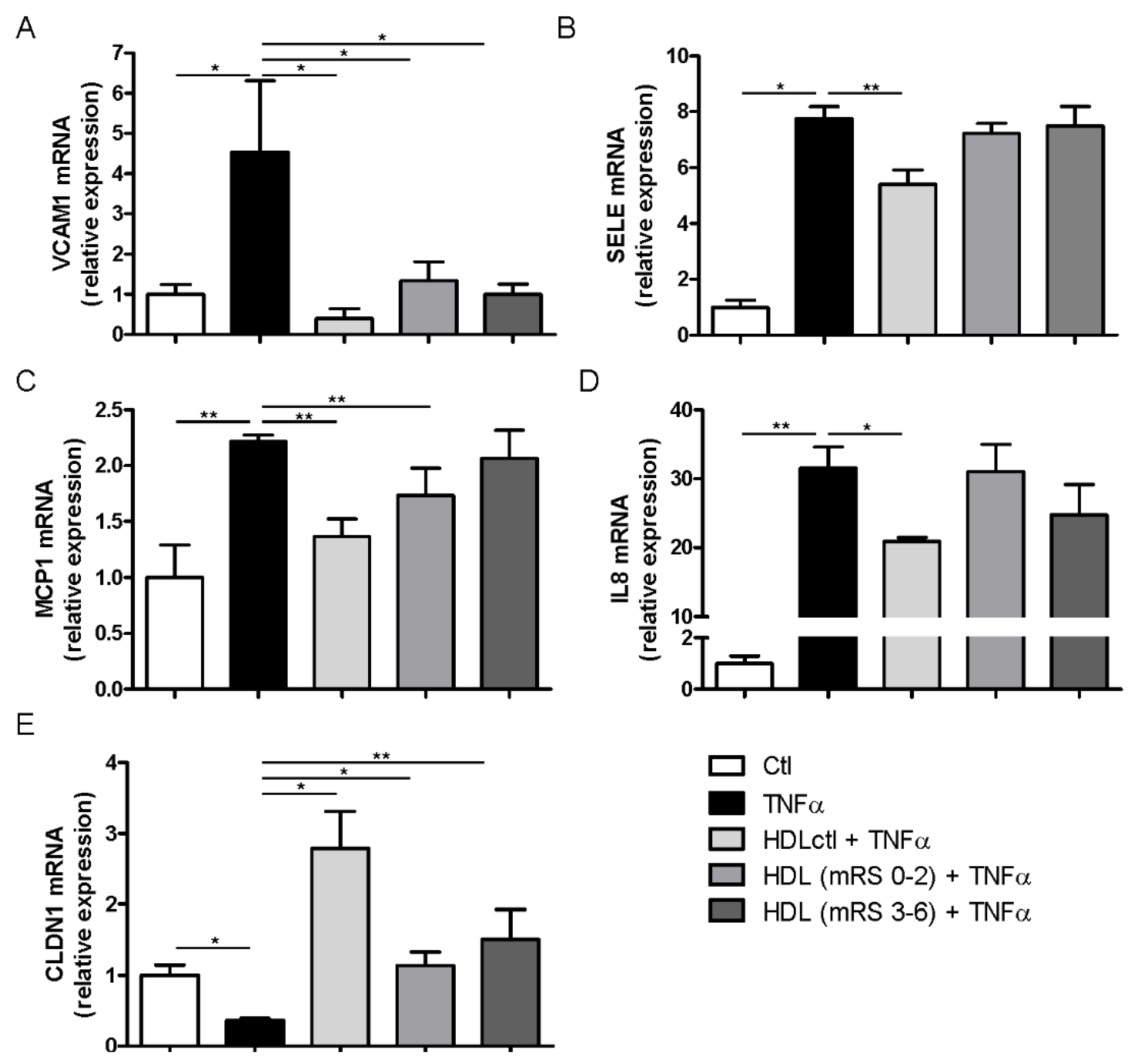
3.5. HDL Anti-Inflammatory Activity
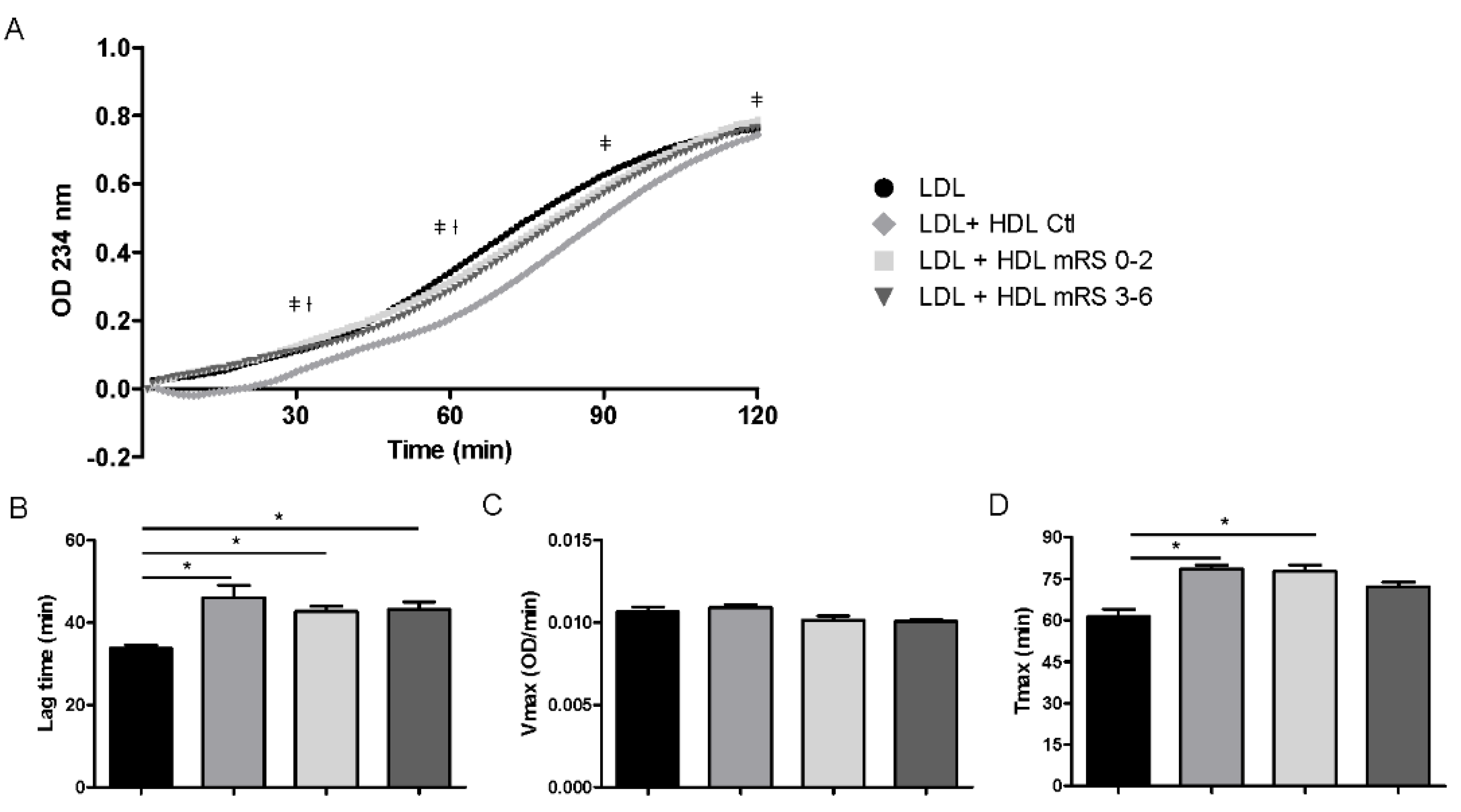
3.6. Antioxidant Activity of HDL
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Data Availability Statement
References
- Ronsein, G.E.; Heinecke, J.W. Time to ditch HDL-C as a measure of HDL function? Curr. Opin. Lipidol. 2017, 28, 414–418. [Google Scholar] [CrossRef] [PubMed]
- Lüscher, T.F.; Landmesser, U.; von Eckardstein, A.; Fogelman, A.M. High-Density Lipoprotein. Circ. Res. 2014, 114, 171–182. [Google Scholar] [CrossRef] [Green Version]
- Meilhac, O. High-Density Lipoproteins in Stroke. Handb. Exp. Pharmacol. 2015, 224, 509–526. [Google Scholar] [PubMed] [Green Version]
- Choi, H.Y.; Hafiane, A.; Schwertani, A.; Genest, J. High-Density Lipoproteins: Biology, Epidemiology, and Clinical Management. Can. J. Cardiol. 2017, 33, 325–333. [Google Scholar] [CrossRef] [PubMed]
- Chei, C.-L.; Yamagishi, K.; Kitamura, A.; Kiyama, M.; Imano, H.; Ohira, T.; Cui, R.; Tanigawa, T.; Sankai, T.; Ishikawa, Y.; et al. High-density lipoprotein subclasses and risk of stroke and its subtypes in Japanese population: The Circulatory Risk in Communities Study. Stroke 2013, 44, 327–333. [Google Scholar] [CrossRef] [Green Version]
- Mahrooz, A. Pharmacological Interactions of Paraoxonase 1 (PON1): A HDL-Bound Antiatherogenic Enzyme. Curr. Clin. Pharmacol. 2016, 11, 259–264. [Google Scholar] [CrossRef]
- Soran, H.; Schofield, J.D.; Durrington, P.N. Antioxidant properties of HDL. Front. Pharmacol. 2015, 6, 222. [Google Scholar] [CrossRef] [Green Version]
- Dang, Q.B.; Lapergue, B.; Tran-Dinh, A.; Diallo, D.; Moreno, J.A.; Mazighi, M.; Romero, I.A.; Weksler, B.; Michel, J.B.; Amarenco, P.; et al. High-Density Lipoproteins Limit Neutrophil-Induced Damage to the Blood–Brain Barrier in Vitro. J. Cereb. Blood Flow Metab. 2013, 33, 575–582. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tajbakhsh, A.; Rezaee, M.; Rivandi, M.; Forouzanfar, F.; Afzaljavan, F. Paraoxonase 1 (PON1) and stroke; the dilemma of genetic variation. Clin. Biochem. 2017, 50, 1298–1305. [Google Scholar] [CrossRef] [PubMed]
- Furtado, J.D.; Yamamoto, R.; Melchior, J.T.; Andraski, A.B.; Gamez-Guerrero, M.; Mulcahy, P.; He, Z.; Cai, T.; Davidson, W.S.; Sacks, F.M. Distinct Proteomic Signatures in 16 HDL (High-Density Lipoprotein) Subspecies. Arterioscler. Thromb. Vasc. Biol. 2018, 38, 2827–2842. [Google Scholar] [CrossRef] [Green Version]
- Gordon, S.M.; McKenzie, B.; Kemeh, G.; Sampson, M.; Perl, S.; Young, N.S.; Fessler, M.B.; Remaley, A.T. Rosuvastatin Alters the Proteome of High Density Lipoproteins: Generation of alpha-1-antitrypsin Enriched Particles with Anti-inflammatory Properties. Mol. Cell. Proteom. 2015, 14, 3247–3257. [Google Scholar] [CrossRef] [Green Version]
- Moreno, J.A.; Ortega-Gómez, A.; Delbosc, S.; Beaufort, N.; Sorbets, E.; Louedec, L.; Esposito-Farèse, M.; Tubach, F.; Nicoletti, A.; Steg, P.G.; et al. In vitro and in vivo evidence for the role of elastase shedding of CD163 in human atherothrombosis. Eur. Heart J. 2012, 33, 252–263. [Google Scholar] [CrossRef] [Green Version]
- Tran-Dinh, A.; Diallo, D.; Delbosc, S.; Varela-Perez, L.M.; Dang, Q.B.; Lapergue, B.; Burillo, E.; Michel, J.B.; Levoye, A.; Martin-Ventura, J.L.; et al. HDL and endothelial protection. Br. J. Pharmacol. 2013, 169, 493–511. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cockerill, G.W.; Rye, K.A.; Gamble, J.R.; Vadas, M.A.; Barter, P.J. High-density lipoproteins inhibit cytokine-induced expression of endothelial cell adhesion molecules. Arterioscler. Thromb. Vasc. Biol. 1995, 15, 1987–1994. [Google Scholar] [CrossRef]
- Cockerill, G.W.; McDonald, M.C.; Mota-Filipe, H.; Cuzzocrea, S.; Miller, N.E.; Thiemermann, C. High density lipoproteins reduce organ injury and organ dysfunction in a rat model of hemorrhagic shock. FASEB J. 2001, 15, 1941–1952. [Google Scholar] [CrossRef] [PubMed]
- Murphy, A.J.; Woollard, K.J.; Hoang, A.; Mukhamedova, N.; Stirzaker, R.A.; McCormick, S.P.; Remaley, A.T.; Sviridov, D.; Chin-Dusting, J. High-density lipoprotein reduces the human monocyte inflammatory response. Arterioscler. Thromb. Vasc. Biol. 2008, 28, 2071–2077. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Murphy, A.J.; Woollard, K.J.; Suhartoyo, A.; Stirzaker, R.A.; Shaw, J.; Sviridov, D.; Chin-Dusting, J. Neutrophil activation is attenuated by high-density lipoprotein and apolipoprotein A-I in in vitro and in vivo models of inflammation. Arterioscler. Thromb. Vasc. Biol. 2011, 31, 1333–1341. [Google Scholar] [CrossRef] [Green Version]
- Lapergue, B.; Moreno, J.A.; Dang, B.Q.; Coutard, M.; Delbosc, S.; Raphaeli, G.; Auge, N.; Klein, I.; Mazighi, M.; Michel, J.B.; et al. Protective Effect of High-Density Lipoprotein-Based Therapy in a Model of Embolic Stroke. Stroke 2010, 41, 1536–1542. [Google Scholar] [CrossRef] [Green Version]
- Jin, R.; Liu, L.; Zhang, S.; Nanda, A.; Li, G. Role of inflammation and its mediators in acute ischemic stroke. J. Cardiovasc. Transl. Res. 2013, 6, 834–851. [Google Scholar] [CrossRef] [Green Version]
- van Swieten, J.C.; Koudstaal, P.J.; Visser, M.C.; Schouten, H.J.; van Gijn, J. Interobserver agreement for the assessment of handicap in stroke patients. Stroke 1988, 19, 604–607. [Google Scholar] [CrossRef] [Green Version]
- Sorrentino, S.A.; Besler, C.; Rohrer, L.; Meyer, M.; Heinrich, K.; Bahlmann, F.H.; Mueller, M.; Horváth, T.; Doerries, C.; Heinemann, M.; et al. Endothelial-vasoprotective effects of high-density lipoprotein are impaired in patients with type 2 diabetes mellitus but are improved after extended-release niacin therapy. Circulation 2010, 121, 110–122. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cardner, M.; Yalcinkaya, M.; Goetze, S.; Luca, E.; Balaz, M.; Hunjadi, M.; Hartung, J.; Shemet, A.; Kränkel, N.; Radosavljevic, S.; et al. Structure-function relationships of HDL in diabetes and coronary heart disease. JCI Insight. 2020, 16, e131491. [Google Scholar] [CrossRef] [Green Version]
- Schneider, C.A.; Rasband, W.S.; Eliceiri, K.W. NIH Image to ImageJ: 25 years of image analysis. Nat. Methods. 2012, 9, 671–675. [Google Scholar] [CrossRef] [PubMed]
- Xie, F.; Xiao, P.; Chen, D.; Xu, L.; Zhang, B. miRDeepFinder: A miRNA Analysis Tool for Deep Sequencing of Plant Small RNAs. Plant Mol. Biol. 2012, 80, 75–84. [Google Scholar] [CrossRef] [PubMed]
- Delbosc, S.; Diallo, D.; Dejouvencel, T.; Lamiral, Z.; Louedec, L.; Martin-Ventura, J.L.; Rossignol, P.; Leseche, G.; Michel, J.B.; Meilhac, O. Impaired high-density lipoprotein anti-oxidant capacity in human abdominal aortic aneurysm. Cardiovasc. Res. 2013, 100, 307–315. [Google Scholar] [CrossRef] [Green Version]
- Ortiz-Munoz, G.; Couret, D.; Lapergue, B.; Bruckert, E.; Meseguer, E.; Amarenco, P.; Meilhac, O. Dysfunctional HDL in acute stroke. Atherosclerosis 2016, 253, 75–80. [Google Scholar] [CrossRef]
- Soran, H.; Hama, S.; Yadav, R.; Durrington, P.N. HDL functionality. Curr. Opin. Lipidol. 2012, 23, 353–366. [Google Scholar] [CrossRef]
- Wu, B.J.; Chen, K.; Shrestha, S.; Ong, K.L.; Barter, P.J.; Rye, K.A. High-Density Lipoproteins Inhibit Vascular Endothelial Inflammation by Increasing 3β-Hydroxysteroid-Δ24 Reductase Expression and Inducing Heme Oxygenase-1. Circ. Res. 2013, 112, 278–288. [Google Scholar] [CrossRef] [Green Version]
- Pandey, A.; Shrivastava, A.; Solanki, A. Study of atherogenic lipid profile, high sensitive C-reactive protein neurological deficit and short-term outcome in stroke subtypes. Iran. J. Neurol. 2016, 15, 146–152. [Google Scholar]
- Bandeali, S.; Farmer, J. High-density lipoprotein and atherosclerosis: The role of antioxidant activity. Curr. Atheroscler. Rep. 2012, 14, 101–107. [Google Scholar] [CrossRef]
- Uyttenboogaart, M.; Koch, M.W.; Koopman, K.; Vroomen, P.C.; Luijckx, G.J.; De Keyser, J. Lipid profile, statin use, and outcome after intravenous thrombolysis for acute ischaemic stroke. J. Neurol. 2008, 255, 875–880. [Google Scholar] [CrossRef] [PubMed]
- Oravec, S.; Krivosikova, Z.; Krivosik, M.; Gruber, K.; Gruber, M.; Dukát, A.; Gavorníket, P. Lipoprotein profile in patients who survive a stroke. Neuro Endocrinol. Lett. 2011, 32, 496–501. [Google Scholar] [PubMed]
- Zeljkovic, A.; Vekic, J.; Spasojevic-Kalimanovska, V.; Jelic-Ivanovic, Z.; Bogavac-Stanojevic, N.; Gulan, B.; Spasic, S. LDL and HDL subclasses in acute ischemic stroke: Prediction of risk and short-term mortality. Atherosclerosis 2010, 210, 548–554. [Google Scholar] [CrossRef] [PubMed]
- Song, T.-J.; Cho, H.-J.; Chang, Y.; Youn, M.; Shin, M.J.; Jo, I.; Heo, J.H.; Kim, Y.J. Low-density-lipoprotein particle size predicts a poor outcome in patients with atherothrombotic stroke. J. Clin. Neurol. 2015, 11, 80–86. [Google Scholar] [CrossRef] [Green Version]
- Varady, K.A.; Lamarche, B. Lipoprint Adequately Estimates LDL Size Distribution, but Not Absolute Size, Versus Polyacrylamide Gradient Gel Electrophoresis. Lipids 2011, 46, 1163–1167. [Google Scholar] [CrossRef]
- von Eckardstein, A.; Kardassis, D. High Density Lipoproteins From Biological Understanding to Clinical Exploitation. Springer Open. Handb. Exp. Pharmacol. 2015, 224. [Google Scholar]
- Pirillo, A.; Norata, G.D.; Catapano, A.L. High-Density Lipoprotein Subfractions-What the Clinicians Need to Know. Cardiology 2013, 124, 116–125. [Google Scholar] [CrossRef]
- Ganjali, S.; Abbas, A.; Momtazi-Borojeni, A.A.; Banach, M.; Kovanen, P.T.; Gotto, A.M.; Sahebkar, A. HDL functionality in familial hypercholesterolemia: Effects of treatment modalities and pharmacological interventions. Drug. Discov. Today 2018, 23, 171–180. [Google Scholar] [CrossRef]
- Hernáez, A.; Soria-Florido, M.T.; Schröder, H.; Ros, E.; Pintó, E.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Arós, F.; Serra-Majem, L.; et al. Role of HDL function and LDL atherogenicity on cardiovascular risk: A comprehensive examination. PLoS ONE 2019, 14, e0218533. [Google Scholar] [CrossRef]
- Camont, L.; Chapman, M.J.; Kontush, A. Biological activities of HDL subpopulations and their relevance to cardiovascular disease. Trends Mol. Med. 2011, 17, 594–603. [Google Scholar] [CrossRef]
- Kontush, A.; Chapman, M.J. Functionally Defective High-density lipoprotein: A new therapeutic target at the crossroads of dyslipidemia, inflammation, and atherosclerosis. Pharmacol. Rev. 2006, 58, 342–374. [Google Scholar] [CrossRef] [PubMed]
- Moreno, J.-A.; Ortega-Gomez, A.; Rubio-Navarro, A.; Louedec, L.; Ho-Tin-Noé, B.; Caligiuri, G.; Nicoletti, A.; Levoye, A.; Plantier, L.; Meilhac, O. High-density lipoproteins potentiate α1 -antitrypsin therapy in elastase-induced pulmonary emphysema. Am. J. Respir. Cell Mol. Biol. 2014, 51, 536–549. [Google Scholar] [CrossRef] [PubMed]
- Turgay, F.; Şişman, A.R.; Aksu, A.Ç. Effects of anaerobic training on paraoxonase-1 enzyme (pon1) activities of high density lipoprotein subgroups and its relationship with PON1-Q192R phenotype. J. Atheroscler. Thromb. 2015, 22, 313–326. [Google Scholar] [CrossRef] [PubMed]
- Cai, W.; Liu, S.; Hu, M.; Huang, F.; Zhu, Q.; Qiu, W.; Hu, X.; Colello, J.; Guo Zheng, S.; Lu, Z. Functional Dynamics of Neutrophils After Ischemic Stroke. Transl. Stroke Res. 2020, 11, 108–121. [Google Scholar] [CrossRef] [PubMed]
- Jickling, G.C.; Liu, D.; Ander, B.P.; Stamova, B.; Zhan, X.; Sharp, F.R. Targeting Neutrophils in Ischemic Stroke: Translational Insights from Experimental Studies. J. Cereb. Blood Flow Metab. 2015, 35, 888–901. [Google Scholar] [CrossRef] [Green Version]
- Förster, C.; Burek, M.; Romero, I.A.; Weksler, B.; Couraud, P.O.; Drenckhahn, D. Differential effects of hydrocortisone and TNFα on tight junction proteins in an in vitro model of the human blood-brain barrier. J. Physiol. 2008, 586, 1937–1949. [Google Scholar]
- Kotur-Stevuljevic, J.; Bogavac-Stanojevic, N.; Jelic-Ivanovic, Z.; Stefanovic, A.; Gojkovic, T.; Joksic, J.; Sopic, M.; Gulan, B.; Janac, J.; Milosevic, S. 3Oxidative stress and paraoxonase 1 status in acute ischemic stroke patients. Atherosclerosis 2015, 241, 192–198. [Google Scholar] [CrossRef]
- Linton, M.F.; Yancey, P.G.; Davies, S.S.; Jerome, W.G.; Linton, E.F.; Song, W.L.; Doran, A.C.; Vickers, K.C. The Role of Lipids and Lipoproteins in Atherosclerosis; MDText.com, Inc.: South Dartmouth, MA, USA, 2000. [Google Scholar]
- Mackness, M.I.; Durrington, P.N.; Mackness, B. The role of paraoxonase 1 activity in cardiovascular disease: Potential for therapeutic intervention. Am. J. Cardiovasc. Drugs 2004, 4, 211–217. [Google Scholar] [CrossRef]
| Gene | RefSeq. | Forward Primer (5′ to 3) | Reverse Primer (5′ to 3′) | Annealing Temperature (°C) | Amplicon Size (bp) | Efficiency (%) | R2 |
|---|---|---|---|---|---|---|---|
| VCAM1 | NM_001078 | AAGGCAGGCTGTAAAAGAATTG | GTAGACCCTCGCTGGAACAG | 60 | 125 | 98.6 | 0.997 |
| SELE | NM_000450 | AGCCCAGAGCCTTCAGTGTA | AACTGGGATTTGCTGTGTCC | 60 | 244 | 102.8 | 0.996 |
| MCP1 | NM_002982 | TCAGCCAGATGCAATCAATG | TCCTGAACCCACTTCTGCTT | 60 | 186 | 98.1 | 0.987 |
| IL8 | NM_000584 | AGACAGCAGAGCACACAAGC | ATGGTTCCTTCCGGTGGT | 60 | 62 | 99.9 | 0.972 |
| CLDN1 | NM_021101 | CCGTTGGCATGAAGTGTATG | AAGGCAGAGAGAAGCAGCAG | 60 | 233 | 99.1 | 0.996 |
| GAPDH | NM_002046 | GAGTCAACGGATTTGGTCGT | GATCTCGCTCCTGGAAGATG | 60 | 225 | 99.8 | 0.998 |
| HPRT | NM_000194 | ACCCCACGAAGTGTTGGATA | AAGCAGATGGCCACAGAACT | 60 | 248 | 91.2 | 0.944 |
| 18S | NR_145820 | AAACGGCTACCACATCCAAG | CCTCCAATGGATCCTCGTTA | 60 | 155 | 104.8 | 0.991 |
| RPL13A | NM_012423 | CCTGGAGGAGAAGAGGAAAGAGA | GAGGACCTCTGTGTATTTGTCAA | 60 | 124 | 96.6 | 0.999 |
| mRS 0–2 (n = 22) | mRS 3–6 (n = 24) | pa | |
|---|---|---|---|
| Age, yr, mean (range) | 67 (35–94) | 75 (42–96) | 0.86 |
| Male gender, %(n) | 64 (14) | 50 (12) | 0.39 |
| Weight, kg, mean (SD) | 75 (15) | 70 (22) | 0.08 |
| Hypertension, %(n) | 50 (11) | 58 (14) | 0.77 |
| Hypercholesterolemia, %(n) | 32 (7) | 42 (10) | 0.46 |
| Smoking, %(n) | |||
| Never | 64 (14) | 75 (18) | 0.41 |
| Former | 14 (3) | 13 (3) | |
| Current | 23 (5) | 8 (2) | |
| NIHSS at admission, median (IQR) | 8 (9) | 16 (7) | <0.001 |
| Systolic BP, mean (SD) | 159 (15) | 150 (22) | 0.15 |
| Diastolic BP, mean (SD) | 86 (14) | 80 (16) | 0.25 |
| Glucose, median (IQR) | 116 (34) | 132 (38) | 0.11 |
| Hemorrhagic transformation, %(n) | |||
| None | 86 (19) | 58 (14) | 0.07 |
| Asymptomatic | 14 (3) | 29 (7) | |
| Symptomatic | -- | 13 (3) | |
| 90-day mortality, %(n) | -- | 16 (73) | <0.001 |
| Variables | Correlation Coefficent (R) | p-Value |
|---|---|---|
| LDL 1 + 2 (mg/dL) | −0.1289 | 0.3932 |
| LDL 3 + 7 (mg/dL) | −0.0569 | 0.7068 |
| Large HDL (mg/dL) | 0.3871 | 0.0079 |
| Intermediate HDL (mg/dL) | 0.1360 | 0.3674 |
| Small HDL (mg/dL) | −0.4217 | 0.0035 |
| HDL ratio (large/small) | 0.5786 | <0.0001 |
| Plasmatic APOA1 (ng/dL) | 0.0301 | 0.8425 |
| APOA1 in HDL (ng/dL) | −0.0107 | 0.9435 |
| Plasmatic SELE (ng/mL) | 0.4096 | 0.0071 |
| Plasmatic VCAM1 (ng/mL) | 0.2626 | 0.1218 |
| Plasmatic ICAM1 (ng/mL) | 0.3136 | 0.0587 |
| Plasmatic MPO (ng/mL) | 0.2097 | 0.2197 |
| Plasmatic tPAI-1 (ng/mL) | 0.0554 | 0.7485 |
| Plasmatic MMP9 (ng/mL) | 0.2584 | 0.1225 |
| PON1/APOA1 ratio in HDL | −0.3912 | 0.0072 |
| AAT/APOA1 ratio in HDL | 0.1880 | 0.2110 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Varela, L.M.; Meseguer, E.; Lapergue, B.; Couret, D.; Amarenco, P.; Meilhac, O. Changes in High-Density Lipoproteins Related to Outcomes in Patients with Acute Stroke. J. Clin. Med. 2020, 9, 2269. https://doi.org/10.3390/jcm9072269
Varela LM, Meseguer E, Lapergue B, Couret D, Amarenco P, Meilhac O. Changes in High-Density Lipoproteins Related to Outcomes in Patients with Acute Stroke. Journal of Clinical Medicine. 2020; 9(7):2269. https://doi.org/10.3390/jcm9072269
Chicago/Turabian StyleVarela, Lourdes M., Elena Meseguer, Bertrand Lapergue, David Couret, Pierre Amarenco, and Olivier Meilhac. 2020. "Changes in High-Density Lipoproteins Related to Outcomes in Patients with Acute Stroke" Journal of Clinical Medicine 9, no. 7: 2269. https://doi.org/10.3390/jcm9072269





