Intraventricular Hemorrhage in Very Preterm Infants: A Comprehensive Review
Abstract
:1. Introduction
2. Experimental Section
2.1. Literature Analysis
2.2. Manual Curation: Inclusion and Exclusion Criteria
3. Results
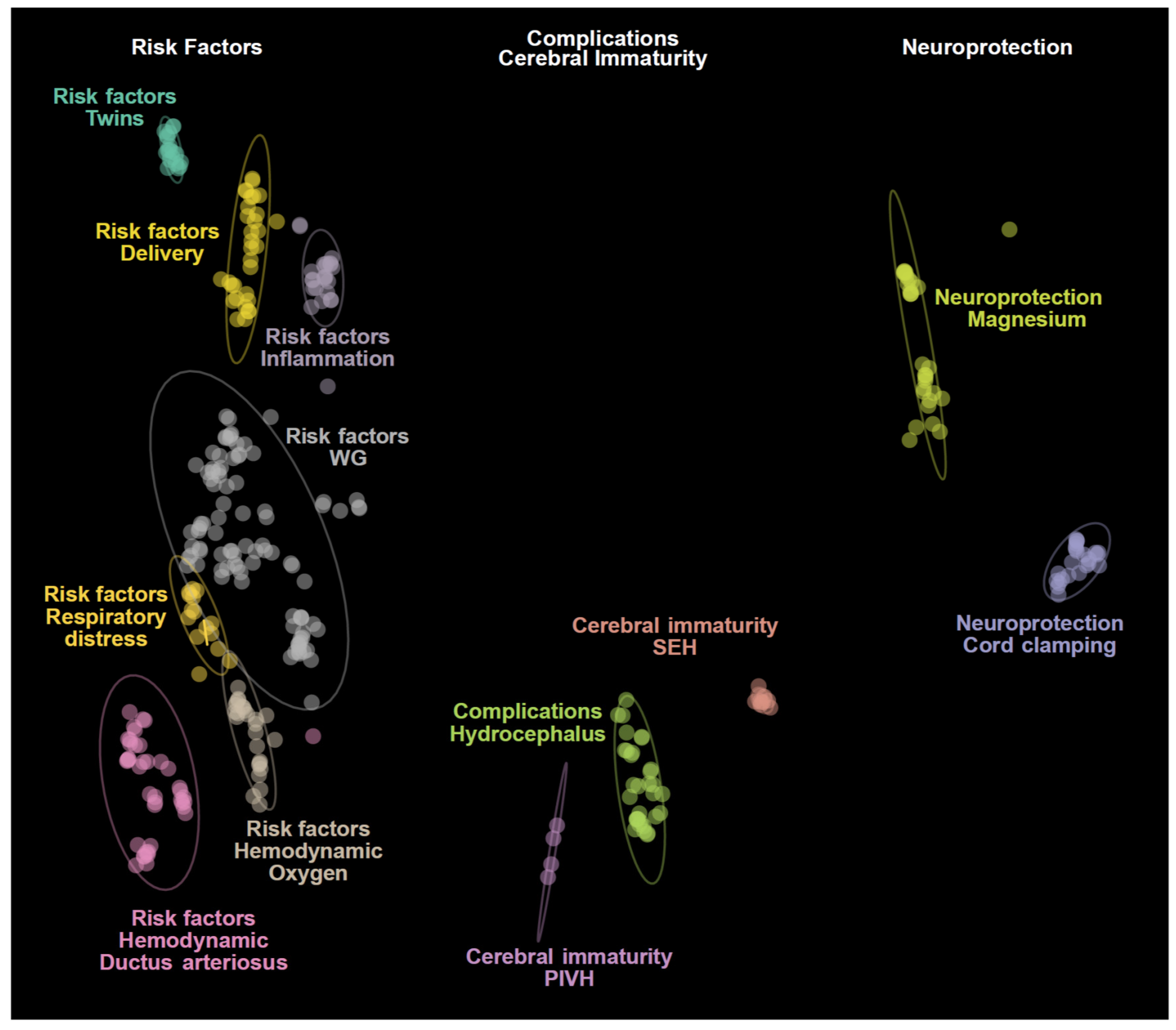
3.1. Literature Mining and Topic Clusters
3.2. Pathogenesis of GMH-IVH-IPH
3.2.1. Immaturity of the Germinal Matrix
3.2.2. Disruption of Cerebral Homeostasis
3.2.3. Coagulation Impairment
3.2.4. Genetic Factors
3.3. Complications of GMH-IVH-IPH
3.4. Neuroprotection
3.5. Biomarkers
3.6. A New Era: Omics-Based Approaches
4. Limits
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Adams-Chapman, I.; Hansen, N.I.; Stoll, B.J.; Higgins, R. Neurodevelopmental Outcome of Extremely Low Birth Weight Infants with Posthemorrhagic Hydrocephalus Requiring Shunt Insertion. Pediatrics 2008, 121, e1167–e1177. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chevallier, M.; Debillon, T.; Pierrat, V.; Delorme, P.; Kayem, G.; Durox, M.; Goffinet, F.; Marret, S.; Ancel, P.Y.; Arnaud, C.; et al. Leading causes of preterm delivery as risk factors for intraventricular hemorrhage in very preterm infants: Results of the EPIPAGE 2 cohort study. Am. J. Obstet. Gynecol. 2017, 216, 518.e1–518.e12. [Google Scholar] [CrossRef] [PubMed]
- Vohr, B.; Ment, L.R. Intraventricular hemorrhage in the preterm infant. Early Hum. Dev. 1996, 44, 1–16. [Google Scholar] [CrossRef]
- Ancel, P.Y.; Goffinet, F.; Kuhn, P.; Langer, B.; Matis, J.; Hernandorena, X.; Chabanier, P.; Joly-Pedespan, L.; Lecomte, B.; Vendittelli, F.; et al. Survival and Morbidity of Preterm Children Born at 22 Through 34 Weeks’ Gestation in France in 2011. JAMA Pediatr. 2015, 169, 230. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Christian, E.A.; Jin, D.L.; Attenello, F.; Wen, T.; Cen, S.; Mack, W.J.; Krieger, M.D.; McComb, J.G. Trends in hospitalization of preterm infants with intraventricular hemorrhage and hydrocephalus in the United States, 2000–2010. J. Neurosurg. Pediatrics 2016, 17, 260–269. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baird, L.C.; Mazzola, C.A.; Auguste, K.I.; Klimo, P., Jr.; Flannery, A.M. Pediatric hydrocephalus: Systematic literature review and evidence-based guidelines. Part 5: Effect of valve type on cerebrospinal fluid shunt efficacy. J. Neurosurg. Pediatrics 2014, 14 (Suppl. 1), 35–43. [Google Scholar] [CrossRef] [Green Version]
- Dykes, F.D.; Dunbar, B.; Lazarra, A.; Ahmann, P.A. Posthemorrhagic hydrocephalus in high-risk preterm infants: Natural history, management, and long-term outcome. J. Pediatrics 1989, 114 Pt 1, 611–618. [Google Scholar] [CrossRef]
- Papile, L.A.; Burstein, J.; Burstein, R.; Koffler, H. Incidence and evolution of subependymal and intraventricular hemorrhage: A study of infants with birth weights less than 1500 gm. J. Pediatrics 1978, 92, 529–534. [Google Scholar] [CrossRef]
- Chollat, C.; Marret, S. Magnesium sulfate and fetal neuroprotection: Overview of clinical evidence. Neural Regen. Res. 2018, 13, 2044. [Google Scholar] [CrossRef]
- Desplanches, T.; Blondel, B.; Morgan, A.S.; Burguet, A.; Kaminski, M.; Lecomte, B.; Marchand-Martin, L.; Rozé, J.C.; Sagot, P.; Truffert, P.; et al. Volume of Neonatal Care and Survival without Disability at 2 Years in Very Preterm Infants: Results of a French National Cohort Study. J. Pediatrics 2019, 213, 22–29. [Google Scholar] [CrossRef]
- Pinto Cardoso, G.; Houivet, E.; Marchand-Martin, L.; Kayem, G.; Sentilhes, L.; Ancel, P.Y.; Lorthe, E.; Marret, S. Association of Intraventricular Hemorrhage and Death with Tocolytic Exposure in Preterm Infants. JAMA Netw. Open 2018, 1, e182355. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dorner, R.A.; Burton, V.J.; Allen, M.C.; Robinson, S.; Soares, B.P. Preterm neuroimaging and neurodevelopmental outcome: A focus on intraventricular hemorrhage, post-hemorrhagic hydrocephalus, and associated brain injury. J. Perinatol. 2018, 38, 1431–1443. [Google Scholar] [CrossRef] [PubMed]
- Gilard, V.; Chadie, A.; Ferracci, F.X.; Brasseur-Daudruy, M.; Proust, F.; Marret, S.; Curey, S. Post hemorrhagic hydrocephalus and neurodevelopmental outcomes in a context of neonatal intraventricular hemorrhage: An institutional experience in 122 preterm children. BMC Pediatrics 2018, 18, 288. [Google Scholar] [CrossRef]
- Van de Bor, M.; Verloove-Vanhorick, S.; Baerts, W.; Brand, R.; Ruys, J. Outcome of Periventricular-Intraventricular Hemorrhage at 2 Years of Age in 484 Very Preterm Infants Admitted to 6 Neonatal Intensive Care Units in The Netherlands. Neuropediatrics 1988, 19, 183–185. [Google Scholar] [CrossRef]
- Leijser, L.M.; Vries, L.S. Preterm brain injury: Germinal matrix–intraventricular hemorrhage and post-hemorrhagic ventricular dilatation. In Neonatal Neurology; Elsevier: Amsterdam, The Netherlands, 2019; Volume 162, pp. 173–199. [Google Scholar]
- Marret, S.; Vanhulle, C.; Laquerriere, A. Pathophysiology of cerebral palsy. In Pediatric Neurology Part I; Elsevier: Amsterdam, The Netherlands, 2013; Volume 111, pp. 169–176. [Google Scholar]
- McCrea, H.J.; Ment, L.R. The Diagnosis, Management, and Postnatal Prevention of Intraventricular Hemorrhage in the Preterm Neonate. Clin. Perinatol. 2008, 35, 777–792. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Crisan, A.; Munzner, T.; Gardy, J.L.; Wren, J. Adjutant: An R-based tool to support topic discovery for systematic and literature reviews. Bioinformatics 2019, 35, 1070–1072. [Google Scholar] [CrossRef]
- Van Der Maaten, L. Accelerating t-SNE using Tree-Based Algorithms. J. Mach. Learn. Res. 2014, 15, 3221–3245. [Google Scholar]
- Fayyad, U.M.; Piatetsky-Shapiro, G.; Smyth, P.; Uthurusamy, R. Advances in knowledge discovery and data mining. In American Association for Artificial Intelligence; Springer: Berlin/Heidelberg, Germany, 1996. [Google Scholar]
- Léger, C.; Dupré, N.; Aligny, C.; Bénard, M.; Lebon, A.; Henry, V.; Hauchecorne, M.; Galas, L.; Frebourg, T.; Leroux, P.; et al. Glutamate controls vessel-associated migration of GABA interneurons from the pial migratory route via NMDA receptors and endothelial protease activation. Cell. Mol. Life Sci. 2019, 77, 1959–1986. [Google Scholar] [CrossRef] [Green Version]
- Fagiani, E.; Christofori, G. Angiopoietins in angiogenesis. Cancer Lett. 2013, 328, 18–26. [Google Scholar] [CrossRef]
- Lecuyer, M.; Laquerriere, A.; Bekri, S.; Lesueur, C.; Ramdani, Y.; Jegou, S.; Uguen, A.; Marcorelles, P.; Marret, S.; Gonzalez, B.J. PLGF, a placental marker of fetal brain defects after in utero alcohol exposure. Acta Neuropathol. Commun. 2017, 5, 44. [Google Scholar] [CrossRef] [Green Version]
- Delgado, A.C.; Ferrón, S.R.; Vicente, D.; Porlan, E.; Perez-Villalba, A.; Trujillo, C.M.; D’Ocón, P.; Fariñas, I. Endothelial NT-3 Delivered by Vasculature and CSF Promotes Quiescence of Subependymal Neural Stem Cells through Nitric Oxide Induction. Neuron 2014, 83, 572–585. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tata, M.; Wall, I.; Joyce, A.; Vieira, J.M.; Kessaris, N.; Ruhrberg, C. Regulation of embryonic neurogenesis by germinal zone vasculature. Proc. Natl. Acad. Sci. USA 2016, 113, 13414–13419. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bell, A.H.; Miller, S.L.; Castillo-Melendez, M.; Malhotra, A. The Neurovascular Unit: Effects of Brain Insults During the Perinatal Period. Front. Neurosci. 2020, 13, 1452. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Peng, Z.; Seven, E.S.; Leblanc, R.M. Crossing the blood-brain barrier with nanoparticles. J. Control. Release 2018, 270, 290–303. [Google Scholar] [CrossRef]
- Ballabh, P. Intraventricular Hemorrhage in Premature Infants: Mechanism of Disease. Pediatric Res. 2010, 67, 1–8. [Google Scholar] [CrossRef] [Green Version]
- El-Khoury, N.; Braun, A.; Hu, F.; Pandey, M.; Nedergaard, M.; Lagamma, E.F.; Ballabh, P. Astrocyte End-Feet in Germinal Matrix, Cerebral Cortex, and White Matter in Developing Infants. Pediatric Res. 2006, 59, 673–679. [Google Scholar] [CrossRef] [Green Version]
- Xu, H.; Hu, F.; Sado, Y.; Ninomiya, Y.; Borza, D.B.; Ungvari, Z.; Lagamma, E.F.; Csiszar, A.; Nedergaard, M.; Ballabh, P. Maturational changes in laminin, fibronectin, collagen IV, and perlecan in germinal matrix, cortex, and white matter and effect of betamethasone. J. Neurosci. Res. 2008, 86, 1482–1500. [Google Scholar] [CrossRef]
- Guerra, M.; Blázquez, J.L.; Rodríguez, E.M. Blood–brain barrier and foetal-onset hydrocephalus, with a view on potential novel treatments beyond managing CSF flow. Fluids Barriers CNS 2017, 14, 1–15. [Google Scholar] [CrossRef]
- Ma, S.; Santhosh, D.; Kumar, T.P.; Huang, Z. A Brain-Region-Specific Neural Pathway Regulating Germinal Matrix Angiogenesis. Dev. Cell 2017, 41, 366–381. [Google Scholar] [CrossRef] [Green Version]
- Del Bigio, M.R. Cell proliferation in human ganglionic eminence and suppression after prematurity-associated haemorrhage. Brain 2011, 134, 1344–1361. [Google Scholar] [CrossRef] [Green Version]
- Xue, M.; Del Bigio, M.R. Immune pre-activation exacerbates hemorrhagic brain injury in immature mouse brain. J. Neuroimmunol. 2005, 165, 75–82. [Google Scholar] [CrossRef] [PubMed]
- Garton, T.P.; He, Y.; Garton, H.J.L.; Keep, R.F.; Xi, G.; Strahle, J.M. Hemoglobin-induced neuronal degeneration in the hippocampus after neonatal intraventricular hemorrhage. Brain Res. 2016, 1635, 86–94. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dupré, N.; Arabo, A.; Orset, C.; Maucotel, J.; Detroussel, Y.; Hauchecorne, M.; Gonzalez, B.J.; Marret, S.; Vivien, D.; Leroux, P. Neonatal cerebral hypoxia-ischemia in mice triggers age-dependent vascular effects and disabilities in adults; implication of tissue plasminogen activator (tPA). Exp. Neurol. 2020, 323, 113087. [Google Scholar]
- Omouendze, P.L.; Henry, V.J.; Porte, B.; Dupré, N.; Carmeliet, P.; Gonzalez, B.J.; Marret, S.; Leroux, P. Hypoxia-Ischemia or Excitotoxin-Induced Tissue Plasminogen Activator-Dependent Gelatinase Activation in Mice Neonate Brain Microvessels. PLoS ONE 2013, 8, e71263. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Virgintino, D.; Errede, M.; Girolamo, F.; Capobianco, C.; Robertson, D.; Vimercati, A.; Serio, G.; Di Benedetto, A.; Yonekawa, Y.; Frei, K.; et al. Fetal blood-brain barrier P-glycoprotein contributes to brain protection during human development. J. Neuropathol. Exp. Neurol. 2008, 67, 50–61. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vazana, U.; Veksler, R.; Pell, G.S.; Prager, O.; Fassler, M.; Chassidim, Y.; Roth, Y.; Shahar, H.; Zangen, A.; Raccah, R.; et al. Glutamate-Mediated Blood-Brain Barrier Opening: Implications for Neuroprotection and Drug Delivery. J. Neurosci. 2016, 36, 7727–7739. [Google Scholar] [CrossRef]
- Yang, D.; Baumann, J.M.; Sun, Y.Y.; Tang, M.; Dunn, R.S.; Akeson, A.L.; Kernie, S.G.; Kallapur, S.; Lindquist, D.M.; Huang, E.J.; et al. Overexpression of Vascular Endothelial Growth Factor in the Germinal Matrix Induces Neurovascular Proteases and Intraventricular Hemorrhage. Sci. Transl. Med. 2013, 5, 193ra90. [Google Scholar] [CrossRef]
- Ment, L.R.; Ådén, U.; Bauer, C.R.; Bada, H.S.; Carlo, W.A.; Kaiser, J.R.; Lin, A.; Cotten, C.M.; Murray, J.; Page, G.; et al. Genes and environment in neonatal intraventricular hemorrhage. Semin. Perinatol. 2015, 39, 592–603. [Google Scholar] [CrossRef] [Green Version]
- Fantini, S.; Sassaroli, A.; Tgavalekos, K.T.; Kornbluth, J. Cerebral blood flow and autoregulation: Current measurement techniques and prospects for noninvasive optical methods. Neurophotonics 2016, 3, 031411. [Google Scholar] [CrossRef]
- Kooi, E.M.W.; Verhagen, E.A.; Elting, J.W.J.; Czosnyka, M.; Austin, T.; Wong, F.Y.; Aries, M.J.H. Measuring cerebrovascular autoregulation in preterm infants using near-infrared spectroscopy: An overview of the literature. Expert Rev. Neurother. 2017, 17, 801–818. [Google Scholar] [CrossRef] [Green Version]
- Cohen, E.; Baerts, W.; Caicedo Dorado, A.; Naulaers, G.; van Bel, F.; Lemmers, P.M.A. Cerebrovascular autoregulation in preterm fetal growth restricted neonates. Arch. Dis. Child.-Fetal Neonatal Ed. 2019, 104, F467–F472. [Google Scholar] [CrossRef] [PubMed]
- Wong, F.Y.; Leung, T.S.; Austin, T.; Wilkinson, M.; Meek, J.H.; Wyatt, J.S.; Walker, A.M. Impaired Autoregulation in Preterm Infants Identified by Using Spatially Resolved Spectroscopy. Pediatrics 2008, 121, e604–e611. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, T.W.; Azhibekov, T.; Seri, I. Transitional Hemodynamics in Preterm Neonates: Clinical Relevance. Pediatrics Neonatol. 2016, 57, 7–18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Katz, N.; Schreiber, L.; Oron, A.; Halachmi, S.; Kohelet, D. Inflammatory Response in Preterm Newborns Born after Prolonged Premature Rupture of Membranes: Is There a Correlation with Placental Histological Findings? Isr. Med. Assoc. J. 2017, 19, 610–613. [Google Scholar]
- Capozzi, G.; Santoro, G. Patent ductus arteriosus: Patho-physiology, hemodynamic effects and clinical complications. J. Matern. Fetal Neonatal Med. 2011, 24 (Suppl. 1), 15–16. [Google Scholar] [CrossRef]
- Kluckow, M. The Pathophysiology of Low Systemic Blood Flow in the Preterm Infant. Front. Pediatrics 2018, 6, 29. [Google Scholar] [CrossRef] [Green Version]
- Ghazi-Birry, H.S.; Brown, W.R.; Moody, D.M.; Challa, V.R.; Block, S.M.; Reboussin, D.M. Human germinal matrix: Venous origin of hemorrhage and vascular characteristics. AJNR Am. J. Neuroradiol. 1997, 18, 219–229. [Google Scholar]
- Andrew, M.; Castle, V.; Saigal, S.; Carter, C.; Kelton, J.G. Clinical impact of neonatal thrombocytopenia. J. Pediatrics 1987, 110, 457–464. [Google Scholar] [CrossRef]
- Sola, M.C.; Rimsza, L.M. Mechanisms underlying thrombocytopenia in the neonatal intensive care unit. Acta Paediatr. 2002, 91, 66–73. [Google Scholar] [CrossRef]
- Kalagiri, R.; Choudhury, S.; Carder, T.; Govande, V.; Beeram, M.; Uddin, M. Neonatal Thrombocytopenia as a Consequence of Maternal Preeclampsia. Am. J. Perinatol. Rep. 2016, 6, e42–e47. [Google Scholar] [CrossRef] [Green Version]
- Duppré, P.; Sauer, H.; Giannopoulou, E.Z.; Gortner, L.; Nunold, H.; Wagenpfeil, S.; Geisel, J.; Stephan, B.; Meyer, S. Cellular and humoral coagulation profiles and occurrence of IVH in VLBW and ELWB infants. Early Hum. Dev. 2015, 91, 695–700. [Google Scholar] [CrossRef] [PubMed]
- Streif, W.; Paes, B.; Berry, L.; Andrew, M.; Andreasen, R.B.; Chan, A.K. Influence of exogenous factor VIIa on thrombin generation in cord plasma of full-term and pre-term newborns. Blood Coagul. Fibrinolysis 2000, 11, 349–357. [Google Scholar] [CrossRef] [PubMed]
- Bilguvar, K.; DiLuna, M.L.; Bizzarro, M.J.; Bayri, Y.; Schneider, K.C.; Lifton, R.P.; Gunel, M.; Ment, L.R. COL4A1 Mutation in Preterm Intraventricular Hemorrhage. J. Pediatrics 2009, 155, 743–745. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mine, M.; Tournier-Lasserve, E. Intracerebral hemorrhage and COL4A1 mutations, from preterm infants to adult patients. Ann. Neurol. 2009, 65, 1. [Google Scholar] [CrossRef]
- Szpecht, D.; Szymankiewicz, M.; Seremak-Mrozikiewicz, A.; Gadzinowski, J. The role of genetic factors in the pathogenesis of neonatal intraventricular hemorrhage. Folia Neuropathol. 2015, 1, 1–7. [Google Scholar] [CrossRef]
- Szpecht, D.; Gadzinowski, J.; Seremak-Mrozikiewicz, A.; Kurzawińska, G.; Szymankiewicz, M. Role of endothelial nitric oxide synthase and endothelin-1 polymorphism genes with the pathogenesis of intraventricular hemorrhage in preterm infants. Sci. Rep. 2017, 7, 42541. [Google Scholar] [CrossRef] [Green Version]
- Yoon, B.H.; Jun, J.K.; Romero, R.; Park, K.H.; Gomez, R.; Choi, J.H.; Kim, I.O. Amniotic fluid inflammatory cytokines (interleukin-6, interleukin-1beta, and tumor necrosis factor-alpha), neonatal brain white matter lesions, and cerebral palsy. Am. J. Obstet. Gynecol. 1997, 177, 19–26. [Google Scholar] [CrossRef]
- Göpel, W.; Gortner, L.; Kohlmann, T.; Schultz, C.; Möller, J. Low prevalence of large intraventricular haemorrhage in very low birthweight infants carrying the factor V Leiden or prothrombin G20210A mutation. Acta Paediatr. 2001, 90, 1021–1024. [Google Scholar] [CrossRef]
- De Vries, L.S.; Liem, K.D.; van Dijk, K.; Smit, B.J.; Sie, L.; Rademaker, K.J.; Gavilanes, A.W. Early versus late treatment of posthaemorrhagic ventricular dilatation: Results of a retrospective study from five neonatal intensive care units in The Netherlands. Acta Paediatr. 2002, 91, 212–217. [Google Scholar] [CrossRef]
- Kazan, S.; Güra, A.; Uçar, T.; Korkmaz, E.; Ongun, H.; Akyuz, M. Hydrocephalus after intraventricular hemorrhage in preterm and low-birth weight infants: Analysis of associated risk factors for ventriculoperitoneal shunting. Surg. Neurol. 2005, 64, S77–S81. [Google Scholar] [CrossRef]
- Marret, S.; Chollat, C.; Levèque, C.; Marpeau, L. Prévention de la paralysie cérébrale du grand prématuré par le sulfate de magnésium. Arch. Pédiatrie 2011, 18, 324–330. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.C.; Catalano, R.; Profit, J.; Gould, J.B.; Lee, H.C. Impact of antenatal steroids on intraventricular hemorrhage in very-low-birth weight infants. J. Perinatol. 2016, 36, 352–356. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Osborn, D.A.; Evans, N.J. Early volume expansion for prevention of morbidity and mortality in very preterm infants. Cochrane Database Syst. Rev. 2004. [Google Scholar] [CrossRef] [PubMed]
- Fowlie, P.W.; Davis, P.G.; McGuire, W. Prophylactic intravenous indomethacin for preventing mortality and morbidity in preterm infants. Cochrane Database Syst. Rev. 2010. [Google Scholar] [CrossRef]
- Brion, L.P.; Bell, E.F.; Raghuveer, T.S. Vitamin E supplementation for prevention of morbidity and mortality in preterm infants. Cochrane Database Syst. Rev. 2003. [Google Scholar] [CrossRef]
- Juul, S.E.; Comstock, B.A.; Wadhawan, R.; Mayock, D.E.; Courtney, S.E.; Robinson, T.; Ahmad, K.A.; Bendel-Stenzel, E.; Baserga, M.; Lagamma, E.F.; et al. A Randomized Trial of Erythropoietin for Neuroprotection in Preterm Infants. N. Engl. J. Med. 2020, 382, 233–243. [Google Scholar] [CrossRef]
- Katheria, A.; Reister, F.; Essers, J.; Mendler, M.; Hummler, H.; Subramaniam, A.; Carlo, W.; Tita, A.; Truong, G.; Davis-Nelson, S.; et al. Association of Umbilical Cord Milking vs. Delayed Umbilical Cord Clamping With Death or Severe Intraventricular Hemorrhage Among Preterm Infants. JAMA 2019, 322, 1877. [Google Scholar] [CrossRef]
- Rabe, H.; Reynolds, G. Early versus delayed cord clamping in preterm infants. In The Cochrane Database of Systematic Reviews; John Wiley & Sons, Ltd.: Chichester, UK, 1996. [Google Scholar]
- De Bijl-Marcus, K.; Brouwer, A.J.; De Vries, L.S.; Groenendaal, F.; Wezel-Meijler, G.V. Neonatal care bundles are associated with a reduction in the incidence of intraventricular haemorrhage in preterm infants: A multicentre cohort study. Arch. Dis. Child.-Fetal Neonatal Ed. 2019, 105, 419–424. [Google Scholar] [CrossRef]
- Kochan, M.; Leonardi, B.; Firestine, A.; McPadden, J.; Cobb, D.; Shah, T.A.; Vazifedan, T.; Bass, W.T. Elevated midline head positioning of extremely low birth weight infants: Effects on cardiopulmonary function and the incidence of periventricular-intraventricular hemorrhage. J. Perinatol. 2019, 39, 54–62. [Google Scholar] [CrossRef]
- Bersani, I.; Pluchinotta, F.; Dotta, A.; Savarese, I.; Campi, F.; Auriti, C.; Chuklantseva, N.; Piersigilli, F.; Gazzolo, F.; Varrica, A.; et al. Early predictors of perinatal brain damage: The role of neurobiomarkers. Clin. Chem. Lab. Med. (CCLM) 2020, 58, 471–486. [Google Scholar] [CrossRef] [Green Version]
- Zhou, W.; Li, W.; Qu, L.H.; Tang, J.; Chen, S.; Rong, X. Relationship of plasma S100B and MBP with brain damage in preterm infants. Int. J. Clin. Exp. Med. 2015, 8, 16445–16453. [Google Scholar] [PubMed]
- Gazzolo, D.; Marinoni, E.; Giovannini, L.; Letizia, C.; Serra, G.; Di Iorio, R. Circulating Adrenomedullin Is Increased in Preterm Newborns Developing Intraventricular Hemorrhage. Pediatric Res. 2001, 50, 544–547. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Douglas-Escobar, M.; Weiss, M.D. Biomarkers of Brain Injury in the Premature Infant. Front. Neurol. 2013, 3, 185. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Risso, F.M.; Sannia, A.; Gavilanes, D.A.W.; Vles, H.J.; Colivicchi, M.; Ricotti, A.; Li Volti, G.; Gazzolo, D. Biomarkers of brain damage in preterm infants. J. Matern. Fetal Neonatal Med. 2012, 25 (Suppl. 4), 93–96. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, N.D.; Wang, D. Multiview learning for understanding functional multiomics. PLoS Comput. Biol. 2020, 16, e1007677. [Google Scholar] [CrossRef] [PubMed]
- Tebani, A.; Afonso, C.; Bekri, S. Advances in metabolome information retrieval: Turning chemistry into biology. Part I: Analytical chemistry of the metabolome. J. Inherit. Metab. Dis. 2018, 41, 379–391. [Google Scholar] [CrossRef] [Green Version]
- Fanos, V.; Antonucci, R.; Barberini, L.; Noto, A.; Atzori, L. Clinical application of metabolomics in neonatology. J. Matern. Fetal Neonatal Med. 2012, 25 (Suppl. 1), 104–109. [Google Scholar] [CrossRef]
- Gil, A.M.; Duarte, D. Biofluid Metabolomics in Preterm Birth Research. Reprod. Sci. 2018, 25, 967–977. [Google Scholar] [CrossRef]
- Gracie, S.; Pennell, C.; Ekman-Ordeberg, G.; Lye, S.; McManaman, J.; Williams, S.; Palmer, L.; Kelley, M.; Menon, R.; Gravett, M. An integrated systems biology approach to the study of preterm birth using “-omic” technology—A guideline for research. BMC Pregnancy Childbirth 2011, 11, 71. [Google Scholar] [CrossRef] [Green Version]
- Sarafidis, K.; Begou, O.; Deda, O.; Gika, H.; Agakidis, C.; Efstathiou, N.; Theodoridis, G. Targeted urine metabolomics in preterm neonates with intraventricular hemorrhage. J. Chromatogr. B 2019, 1104, 240–248. [Google Scholar] [CrossRef]
- Mussap, M.; Noto, A.; Cibecchini, F.; Fanos, V. The importance of biomarkers in neonatology. Semin. Fetal Neonatal Med. 2013, 18, 56–64. [Google Scholar] [CrossRef] [PubMed]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gilard, V.; Tebani, A.; Bekri, S.; Marret, S. Intraventricular Hemorrhage in Very Preterm Infants: A Comprehensive Review. J. Clin. Med. 2020, 9, 2447. https://doi.org/10.3390/jcm9082447
Gilard V, Tebani A, Bekri S, Marret S. Intraventricular Hemorrhage in Very Preterm Infants: A Comprehensive Review. Journal of Clinical Medicine. 2020; 9(8):2447. https://doi.org/10.3390/jcm9082447
Chicago/Turabian StyleGilard, Vianney, Abdellah Tebani, Soumeya Bekri, and Stéphane Marret. 2020. "Intraventricular Hemorrhage in Very Preterm Infants: A Comprehensive Review" Journal of Clinical Medicine 9, no. 8: 2447. https://doi.org/10.3390/jcm9082447




