1. Introduction
The development of antimicrobial resistance (AMR) and the consequent prospect of future limits to medical treatments was highlighted by England’s Chief Medical Officer, Professor Dame Sally Davies, who described it as a ticking time bomb that could prevent healthcare such as cancer treatments and organ transplants in the future [
1]. AMR continues to be a major public health concern: there were 178 AMR infections diagnosed per day in England in 2019, an increase of 8 per day from 2018 [
2]. Although the rise in treatment-resistant infections in humans may be driven primarily by the use of antibiotics in hospital/healthcare settings [
3], antibiotic use in livestock can also contribute to the development of bacterial resistance to antibiotics [
4,
5,
6]. The influential UK report established by the then Prime Minister as an independent review, chaired by Lord O’Neill [
7], advocated reducing antibiotic use in livestock production as a part of the measures aimed at mitigating the potential development of AMR. The livestock industry in the UK has responded by substantially reducing antibiotic use in recent years, with sales of veterinary medicines for food-producing animals reducing by 55% between 2014 and 2021, although this may now be reaching a plateau [
8]. Data on clinical antimicrobial resistance in animals are not really available.
Potential routes for the entry of antibiotic-resistant bacteria into the human population from animal sources are various and include direct contact with animals (including pets), some foods (e.g., raw meat) and through environmental exposure (e.g., water) [
9,
10]. However, these linkages are not well understood. Although the focus of research is often on transmission possibilities from meat and milk, other foods (such as prawns and fruit) may also be implicated [
9]. Contact with food handlers within the food chain is another potential route of transmission, although the direction of transmission is not clear [
9].
Hocknell et al. [
11] report that UK retailers have been proactive in addressing risks from antibiotic resistance emerging from food sources. However, little is known about UK consumer knowledge and perceptions about AMR and food. For example, do consumers prioritise the necessity of antibiotic use for animal welfare, or the risk of the development of antibiotic resistance? The survey reported here is intended to fill this knowledge gap. This work was carried out under the aegis of the Food Industry Initiative on Antimicrobials (FIIA) and benefits from the large consumer base available to supermarkets. Set up in 2018, the FIIA is a collaborative network of retailers, manufacturers, processors and food service companies in the UK, seeking to support responsible antibiotic use and reduce the prospect of AMR development.
Research on consumer perspectives around AMR has been limited to date, and is reviewed in the next section. We reflect further on the findings in a discussion section and draw our findings together in a final concluding section.
2. Literature Review
Efforts to prevent resistance by reducing antibiotic use in livestock face a central paradox: antibiotics are a valuable tool to prevent and treat animal disease, but their use carries a risk of the development of bacterial resistance. The objective of responsible antimicrobial use, as reflected in the aspirations of the FIIA and others in the food chain (including veterinarians and farmers), is to minimise usage while safeguarding animal health.
Much of the work around behavioural change to reduce antibiotic use has focused on decisions on the use of antibiotics by those on the front line in livestock production—veterinarians and farmers—and recognises the challenges that they face [
12,
13]. There is evidence that both groups are concerned about the potential for resistance due to antibiotic use in livestock production, but ultimately prioritise animal health and welfare [
14]. Attitudes and knowledge vary widely between key groups, e.g., veterinarians, farmers, and the general public [
15], but the reduction in antibiotic use in the UK livestock sector has been driven by voluntary agriculture and food industry initiatives [
11,
16]. Regulation has played a more significant role in other jurisdictions, notably in Denmark [
17,
18]. While veterinarians did not identify consumers as an important driving force for changing antibiotic practices [
19], there is evidence that broader social, political and economic factors contribute to decisions about antibiotic use [
20], and public perception may be a contributing factor.
Studies of consumers have highlighted their lack of knowledge and widespread misconceptions about the nature of antibiotic resistance and the multitude of potential pathways to resistance [
10,
11,
21,
22]. Nevertheless, AMR is widely perceived by consumers to be a potential threat to human health, e.g., in Chile [
23], China [
24], the USA [
25,
26], Italy [
26], Germany [
26,
27], the UK [
28], Canada [
27,
29] and the European Union [
29]. Swiss consumers were generally not aware of any risks of AMR from food, having a high degree of trust that their food was safe, although expressing some concern about food from other countries [
10]; however, this qualitative research was conducted using a very small sample of 14 consumers.
Consumers often lack understanding about why antibiotics are used in agriculture [
11,
25,
28] and are unaware of the withdrawal periods required after treating animals with antibiotics to ensure antibiotic residues are not present in food ([
11,
22]). The acceptability of antibiotic use seems to depend on beliefs around the value of antibiotics to improve animal welfare. Some consumers appear to be broadly supportive of the use of antibiotics for animal welfare reasons, e.g., in Cornejo et al [
23] (focus group data in Chile). But acceptance can vary with the use of the antibiotic. Meerza et al. [
30] found that only 14% of US consumers found antibiotic use as a growth promoter acceptable, but over 50% found the use of antibiotics to treat and control infections acceptable. Some consumers expect that no use of antibiotics means better animal welfare, when the opposite may well be true [
28,
30]. Meerza et al. [
30], for example, found that US respondents who believed antibiotic use reduces animal welfare were more likely to be concerned about the use of antibiotics to treat, prevent and control disease than respondents who viewed antibiotics as contributing to better animal welfare. Antibiotic use may be associated in the public mind with the rise in intensive farming. Kirchelle [
31], for example, suggests antibiotics made intensive farming possible, although this has been contested [
32], and so antibiotic use may be associated with poorer welfare because of the intensive nature of production. There is also a degree of scepticism about claims of responsible use; for example, Bush et al. [
26] reported widespread belief among consumers (including in Germany and Italy) that antibiotics are used for growth promotion, although the practice has been banned in the EU since 2006.
Based on a survey in Ireland [
22], Regan et al. found that people tended to view antibiotics, in part, through the lens of a medical model, so that their experience of General Practitioners (doctors) prescribing antibiotics to themselves and their family, reluctantly, and only in the presence of disease, contrasts with the idea of prophylactic use in agriculture [
22]. The prophylactic use of antibiotics, as is common in animal production, is therefore difficult for consumers to accept. Since the study was conducted, the EU banned the routine use of antibiotics in animals in 2022 [
33].
The lack of understanding about the use of antibiotics in agriculture leads to further confusion as to what is meant if the term “antibiotic-free” is used: this can be interpreted by consumers to mean that there are no antibiotic residues [
26], or that no antibiotics are used during the production process. A shift towards antibiotic-free production was perceived as preferable by consumers in the USA, but had negative impacts on the health, welfare and productivity of livestock [
34], demonstrating the potential trade-off between a reduction in antibiotic use and animal health and welfare. However, consumers may be unaware of the potential negative consequences of reducing antibiotic use [
27]. The antibiotic-free paradigm is not one that has been embraced by UK retailers [
11,
35] who have instead adopted an approach of industry-wide action for the more discriminating use of antibiotics across production systems. Hocknell et al. [
11] note that although retailers are able to influence, at least to some degree, the way in which antibiotics are used on farms, they have little ability to control AMR elsewhere in the broader environment of widespread antibiotic use.
Limited evidence exists relating specifically to UK consumer preferences on antibiotic use in livestock systems and how they perceive the conflicting demands of animal welfare and managing the spread of AMR. This study, therefore, aimed to explore UK consumers’ knowledge of and attitudes towards antibiotic use in livestock, and to assess the impact on their purchasing preferences.
4. Discussion
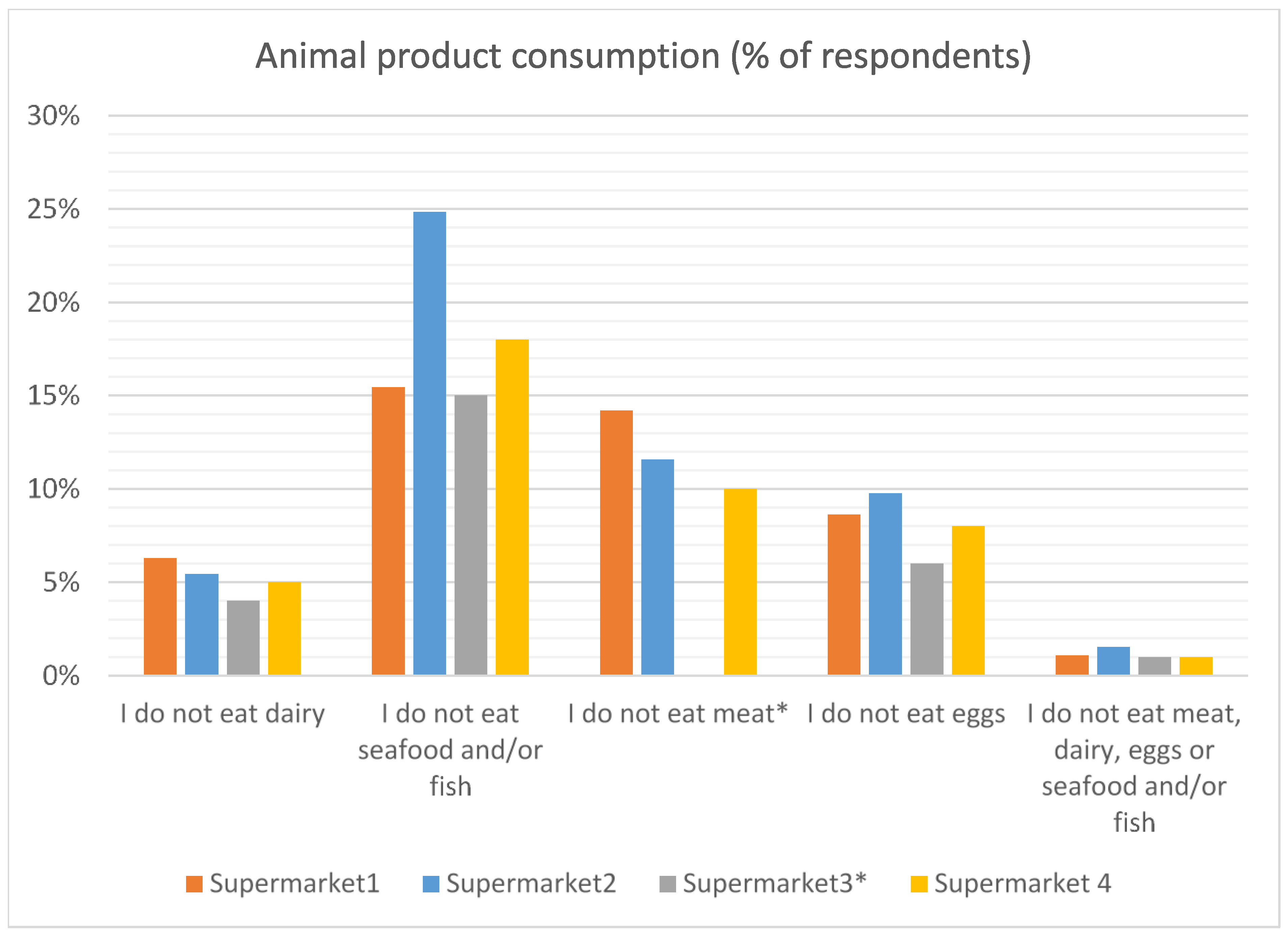
There was general agreement with the use of animals for human benefit, with around 50% agreeing that it is acceptable for cattle, sheep and/or pigs to be raised for human consumption. The number of consumers self-reporting that they do not eat meat was higher (at 10–14%) than those reported by Goddard et al. [
27] at 8% in Canada and 4.8% in Germany. One possible explanation is that this is a reflection of the recent increasing emphasis on reducing meat eating to reduce climate change impacts.
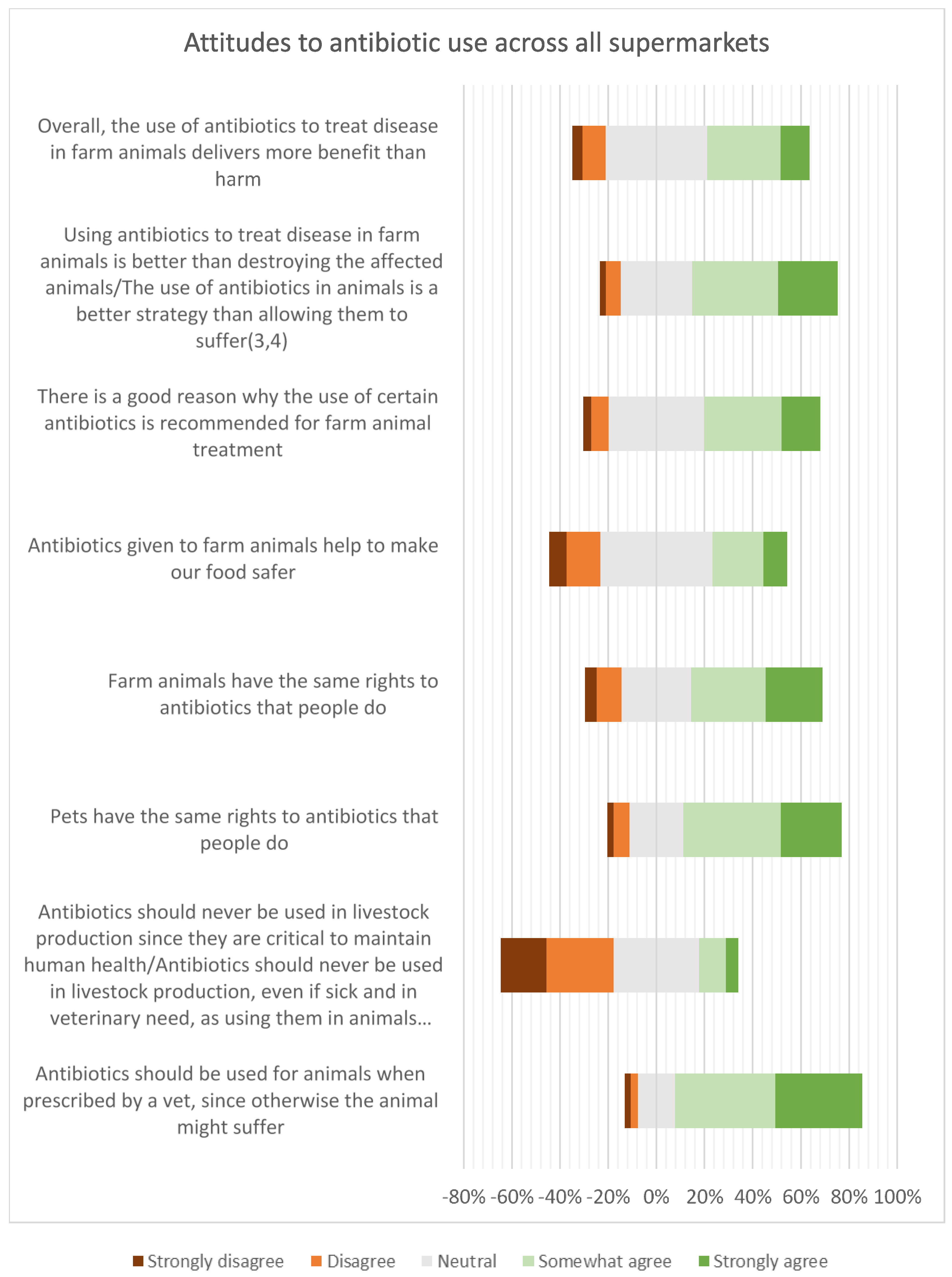
Forty percent of the respondents agreed that, overall, the use of antibiotics to treat disease in farm animals delivers more benefit than harm, but 44% neither agreed nor disagreed, indicating a high level of uncertainty. Consumers who keep animals, have greater knowledge of antibiotic use and resistance, and have received antibiotic treatment in the last 12 months were more likely to agree that antibiotic use was more beneficial than harmful. However, the high proportion of neutral responses to attitudinal questions may indicate a situation that is not stable and could swing in different directions. Around 65% of consumers were concerned about being affected by AMR personally. However, the high levels of concern about animal welfare may be ameliorating this personal focus, resulting in a strong recognition that antibiotics should be available for treating animals when necessary. Around 50% of the respondents agreed that farm animals have the same rights to antibiotics as people do (this figure was very slightly lower than the rights of pets to antibiotics). Perhaps as a result, there was general lack of support for antibiotic-free production among these UK respondents. The data on concern about the use of antibiotics should also be viewed in the context of perceptions of risk from alternative interventions, such as vaccination (viewed as high or very high risk by 50% of the respondents in this survey) and even vitamins (viewed as high or very high risk by 40% of the respondents).
The perception that UK farmers use antibiotics more responsibly than in some other countries (around 50% agreement) may result in a stronger level of trust in the food chain. This would fit with the data from Swiss consumers [
10] who trusted their food sources and where antibiotic use in agriculture is low, and US consumers who preferred antibiotic-free production [
25] where, until 2017, antibiotics important for human health have been permitted for use for growth promotion [
30]. This is an important finding given that consumers have a vested interest in how their food is produced, while they have limited control over production systems and any risks they may inadvertently be exposed to. Food is, of course, traded internationally, and the small number of Swiss consumers interviewed [
10] expressed greater concern about AMR spread from consuming food produced elsewhere in the world.
Although there was broad acceptance for the use of antibiotics in food production among these UK respondents, a minority (7%) perceived that the use of antibiotics in animals represented a level of risk to the consumer that meant the benefits did not outweigh the harm. These consumers should not be neglected.
The results of these surveys are consistent with those from other countries that found that consumers generally have limited knowledge about antibiotic use in agriculture and AMR, with over 50% responding “don’t know” to questions about these aspects. Consumers’ knowledge was strongest around the potential for the frequent use of antibiotics to lead to resistance. The knowledge was weaker around antibiotic residues in animal products, antibiotic use in organic production and the relative quantities of antibiotics used in people and animals.
Redding et al. [
37] suggested educating consumers more effectively on the processes taken to limit the occurrence of antibiotic residues in food (milk, in their specific case) to effect behavioural change, leading to reduced concern about antibiotic use. They based this conclusion on testing out the impacts of providing brochures or videos with information on antibiotic residue mitigation methods, and found that these approaches altered US consumer behaviour. However, while potentially reassuring consumers about residues, education does not impact on any principle- or value-based concerns around the use of antibiotics in livestock production. Meerza [
30] further found that consumers with little knowledge about antibiotic use in animal agriculture were likely to avoid this kind of information. This approach also assumes that antibiotic residue mitigation methods are uniformly practised, and this may not always be the case.
The question as to whether food produced without the use of antibiotics should be identified by labels is one area where supermarkets could act. The data from this survey suggest a great deal of uncertainty as to whether such labelling would be desirable or not, with 32% of respondents agreeing that they would prefer food labelled as never having received antibiotic treatments, whereas 50% were neither supportive nor unsupportive of this initiative. Data from other research [
38] suggest that while US consumers are generally supportive of such labels, they are less willing to pay for them. Goddard [
27] found that 9% of German and 15% of Canadian respondents indicated they would be willing to pay for reduced antibiotic use, while Ding et al. [
24] found that an astonishing 79.8% of Chinese respondents were willing to pay extra for products free from antibiotics. Whether such stated willingness would be repeated in making purchases remains a question. There are some initiatives to provide antibiotic-treatment-free products in the UK [
28], so the success or otherwise of these in the market place will also test the desirability of labelling. An alternative, as reportedly implemented in Sweden [
39], is to use on-line sustainability declarations that are available to the supermarkets, but not the consumers, in order to track the exposure of animals to antibiotics.
Another alternative would be for supermarkets to provide financial incentives to livestock producers to implement alternative strategies to reduce antimicrobial use, such as increased hygiene and biosecurity or vaccination, which may incur additional costs for the producer compared to antibiotics. However, as noted earlier, vaccination was viewed as high or very high risk by 50% of the respondents in this survey. The involvement of veterinarians may also be critical for assuring the responsible use of antibiotics. The surveys reported here found around 70% agreement that antibiotics should be used when prescribed by a veterinarian. Similarly, other research suggested that the responsible use of antibiotics was contingent on the verification of a bacterial infection by either a veterinary surgeon or a test [
26]. These types of initiatives would require supermarkets to have a direct supply chain with a clear and long-term link to their suppliers, and consumers willing to pay for such measures. Hughes et al. [
35] emphasised how different supply chain structures impact on the ability of retailers to influence antibiotic use in global value chains.
The focus on people as consumers rather than citizens places the emphasis and responsibility for AMR on the consumers who have the least information available to them. But people are also citizens, and if treated as such, the views of those who do not consume products from animals also become important. From the perspective of citizens, AMR will continue to be an important focus, and something that cannot be neglected. The pressure to reduce use of antibiotics in animal agriculture will continue. To quote:
“It would be a brave politician who, after having made the electorate and their children jump through inconvenient and expensive hoops before being prescribed an antibiotic, would not expect livestock and companion animals to jump even higher”
Further research is needed on the practicalities of continuing to reduce antibiotic use and in what consumers and citizens understand as responsible use. Having a better understanding of the balance point where the benefits outweigh the risks requires an understanding of the degree of “harm” that is deemed acceptable (e.g., when an animal has accidentally harmed itself versus specific disease conditions), whether this varies between species (e.g., pigs versus beef cattle), among different production systems (extensive versus intensive) or among antibiotics with greater or lesser propensity to drive the evolution of resistance or result in environmental exposure (e.g., how the antibiotic is metabolised and excreted).
The results from these surveys consist of a large dataset on consumer perceptions. Because each supermarket conducted their own survey, there were some variations between the datasets such as the precise wording of the questions and the level of data aggregation that presented additional challenges for data management and analysis. The authors consider that these minor issues with data quality are offset by the enhanced access to supermarket customers offered through our collaboration with commercial partners to conduct this research. As the survey started from the same questionnaire basis and the limitations in terms of data consistency are described clearly, we suggest that the findings provide a robust evidence base for further discussion about the role of the consumer in driving sustainable antibiotic use in agriculture.
The surveys were initiated by the supermarkets through their respective consumer panels, as opposed to being conducted by external research organisations. It is possible that the answers given may have been influenced by the existing relationship that these consumers have with the supermarket in question, given that consumers in the customer insight panels are likely to have responded to previous questionnaires. However, the response rate to questionnaires conducted by external researchers is often low, and it is therefore possible that the responses from a consumer panel are more representative of the customers of that supermarket than an attempt to recruit consumers to respond to questionnaires by a totally external actor would be to the population as a whole. While responses from a single supermarket may reflect the particular demography of the customers of that supermarket, combining data from four different supermarkets would be expected to compensate for any such effect, and the responses across all four supermarkets were broadly similar. The results of the more detailed inferential analysis possible for data from supermarket 2 may not necessarily apply more generally. However, the available demographic data suggest a reasonably representative sample of the general UK population in the data from supermarket 2, and the sample size from supermarket 2 is of a size comparable with other studies on consumer attitudes towards the use of antibiotics in food production. Furthermore, many people will shop in more than one outlet, so customers of supermarket 2 may also be customers of other retail outlets.
Undertaking a survey of this size and scope from a purely academic source would be challenging to achieve, expensive and very time-consuming. The willingness of the supermarkets to collaborate pre-competitively to obtain these data demonstrates an industry-wide commitment to tackling AMR in the best ways possible. To quote Hocknell et al., “Overcoming the AMR challenge cannot become an industry competitive issue and it cannot be something the UK, or Europe, does by itself. There needs to be continued acceptance across human and animal health, and the whole food system that microbes know no borders” ([
11], p. 11). This viewpoint is now more apparent due to the COVID-19 pandemic than when this statement was written.
6. Conclusions
The development of AMR continues to be a threat to human health. The use of antibiotics in livestock production has the potential to contribute to the development of AMR, but efforts to prevent resistance by reducing antibiotic use in livestock face a central paradox: antibiotics are a valuable tool to prevent and treat animal disease, but their use carries a risk of the development of bacterial resistance. Little is known about UK consumer knowledge and perceptions about AMR and food. For example, do consumers prioritise the necessity of antibiotic use for animal welfare, or the risk of development of antibiotic resistance? The survey reported here is intended to fill this knowledge gap, and benefits from access to the large consumer base available to supermarkets. A survey of 5693 people from the customer insight panels of four major UK supermarkets was used to better understand consumer attitudes and perceptions. Consistent with other surveys, the data indicate that there is limited knowledge about antibiotic use and AMR among consumers. While there was a degree of consumer concern about antibiotic use in food production, it was not a major issue for the majority of the respondents. These data do not indicate a strong drive for a reduction in antibiotic use in farm animals from a consumer perspective, perhaps reflecting the recognition by consumers that the level of antibiotic use in UK agriculture is low by global standards. There was agreement about the benefits of antibiotics outweighing the harm, with 40% agreeing that, overall, the use of antibiotics to treat disease in farm animals delivers more benefit than harm. However, 44% neither agreed nor disagreed, indicating a high level of uncertainty and a situation that is potentially unstable. Combined with the low level of knowledge of antibiotic use and AMR in animal production, attitudes may change.
The study identified factors that influence consumer attitudes towards antibiotic use in agriculture, but further work would also permit a more in-depth exploration of these factors. Antibiotic-free production was not widely supported by UK consumers, particularly if it results in lower levels of health and welfare for production animals, suggesting this may not be an appropriate strategy for the UK market. However, the seriousness of the AMR challenge is such that continued action for the more discriminating use of antibiotics must continue.