What Is Known about Community Pharmacy-Based Take-Home Naloxone Programs and Program Interventions? A Scoping Review
Abstract
1. Introduction
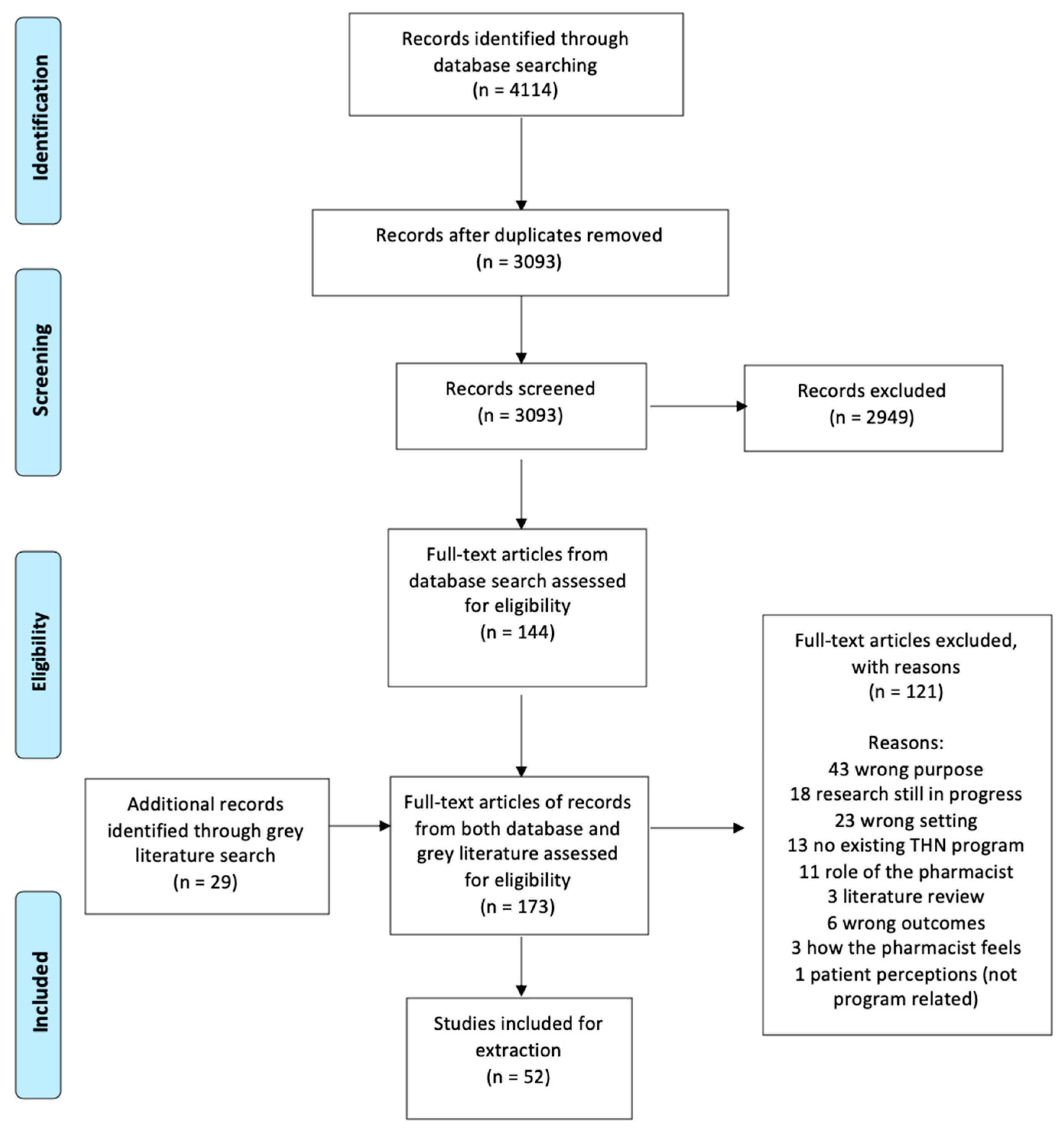
2. Materials and Methods
3. Results
3.1. Take-Home Naloxone Programs and Program Interventions
3.2. THN Programs: Laws
3.3. THN Programs: Opt-Out Dispensing
3.4. THN Programs: Education of Pharmacy Teams and Screening Tools
3.5. THN Programs: Checklists and Pocket-Guides
3.6. Naloxone Availability and Dispensing
3.7. Facilitators and Barriers
3.8. Barriers: Cost
3.9. Barriers: Stigma
3.10. Barriers: Education and Training for Pharmacists
3.11. Facilitators
3.12. Knowledge Gaps
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
EMBASE Search Strategy (Performed 1 June 2020)
- exp “pharmacy (shop)”/
- exp pharmacist/
- (Pharmacist* or Pharmacy or Pharmacie* or Pharmaceutical service*).mp. [mp=title, abstract, heading word, drug trade name, original title, device manufacturer, drug manufacturer, device trade name, keyword, floating subheading word, candidate term word]
- 1 or 2 or 3
- exp narcotic antagonist/
- exp opiate antagonist/
- (Naloxone or Narcan or Naloxon or Nalone or Antidote).mp. [mp=title, abstract, heading word, drug trade name, original title, device manufacturer, drug manufacturer, device trade name, keyword, floating subheading word, candidate term word]
- 5 or 6 or 7
- exp drug overdose/
- exp harm reduction/
- exp counseling/
- exp drug dependence/
- exp opiate addiction/
- exp drug abuse/
- exp narcotic dependence/
- (Addiction or Counsel* or Abus* or Dependenc* or Overdos* or Death* or Harm* or Naloxone distribution or Program* or Safe* or Poisoning or Preventative Health Service* or Substance abuse or Take home or Take-home or THN or Train* or Prevent*).mp. [mp=title, abstract, heading word, drug trade name, original title, device manufacturer, drug manufacturer, device trade name, keyword, floating subheading word, candidate term word]
- 9 or 10 or 11 or 12 or 13 or 14 or 15 or 16
- 4 and 8 and 17
Appendix B
| Study Name |
|---|
| Author |
| Year |
| Study type |
| Country |
| Objective(s) |
| Population studied |
| Sample size |
| Methods |
| Intervention/comparator |
| Duration of intervention |
| Outcomes studied |
| Key Findings: Facilitators/barriers for existing THN programs |
| Key Findings: THN program details |
| Key Findings: Knowledge gaps about THN programs |
Appendix C. Intervention Studies
| Author | Year | Location | Population Studied | Methods | Intervention and Comparator | Outcomes Studied | Key Findings |
|---|---|---|---|---|---|---|---|
| Cohort studies | |||||||
| Gangal [19] | 2020 | USA | Patients | Cohort study | I: Pharmacist prescriptive authority C: Baseline | Naloxone dispensing rate | - Naloxone dispensing rate/month/county increased significantly. - Patients in low income or high poverty areas were significantly more likely to obtain naloxone post-policy. |
| Champaloux [20] | 2018 | USA | Patients at high risk of overdose | Prospective cohort study | I: Opioid safety guide (OSG) opioid dispensing C: Non-OSG opioid dispensing | - Naloxone dispensing rate - Opioid discontinuation | - The OSG included education about safe opioid use, disposal, storage, and naloxone. - The odds of a patient receiving naloxone were 4 times higher compared to control. |
| Mixed Methods | |||||||
| Eldridge [21] | 2020 | USA | Pharmacies | Looking at pharmacy censuses, naloxone stocking/dispensing rates, naloxone policies, and educational programs | I: Statewide standing order C: Baseline | Naloxone stocking and dispensing | - Naloxone dispensing rates tripled between 2016 and 2018. - Corporate education efforts have the potential to have an impact on stocking and dispensing; chain drug stores were more likely to dispense and stock naloxone. |
| Intervention and Implementation Study | |||||||
| Akers1 [29] | 2017 | USA | N/A | Implementation study | I: Pharmacist training and dispensing checklist | Implementation and early results of the first THN program in a community pharmacy in Washington | - Education program coupled with dispensing checklist to standardize patient counselling including risk factors for and recognizing opioid overdose, providing basic life support, naloxone administration, recovery position, post-overdose monitoring, and Good Samaritan law review. - The main population accessing the program are family/friends and are generally older population. |
| Wilkerson [34] | 2020 | USA | N/A | Implementation study | I: Pharmacist training and patient counselling checklist | Implementation of a naloxone dispensing program in which pharmacists and pharmacy interns (under the direct supervision of a pharmacist) can dispense naloxone without a prescription. | - All pharmacists and interns completed a training program about overdose prevention and naloxone rescue kits, naloxone resources, patient education checklist form, and a training video. - To dispense, eligible patients are identified or can ask for naloxone. - If identified, the patient fills a consent form with qualifying information, which acts as a prescription. - A note is added to the pharmacy software serving as a hard-stop. - At pickup, pharmacy staff reviews the checklist form, counsels, provides naloxone and a brochure. - The pharmacist must sign off that counselling has been completed, and documentation is scanned into pharmacy software. |
| Freeman [30] | 2017 | CND | N/A | Implementation study in which a number of groups worked together to coordinate policy changes | N/A | - Implementation of Alberta’s THN program - Number of sites distributing naloxone that were pharmacies - Ease of naloxone access at pharmacies | - From 2015 to 2016, THN kits were dispensed through 953 registered sites, 759 of them community pharmacies. - Initial feedback showed there was variation in accessing THN kits. - To support assessment of the program, people who use a THN kit are asked to call a toll-free nursing line to report use of kits and outcome. - Some pharmacies unaware that people could access kits without providing a provincial healthcare number. |
| Shafer [22] | 2017 | USA | Walgreen’s pharmacies | Intervention study employing 3 programs at Walgreens evaluated using the RE-AIM framework | I: 3-pronged approach taken by Walgreens: (1) provide safe medication disposal kiosks (2) expand national access to naloxone (3) provide education on the risk and avoidance of opioid overdose. | Naloxone prescriptions dispensed How naloxone-prescribing policies in select states have positively affected naloxone dispensing through Walgreens | - Early results are safe medication disposal kiosks in more than 43 states, naloxone-dispensing program in 33 states. - The naloxone training program is required for all pharmacists. - It includes policies, risk factors for, and recognition of overdose; how to use naloxone products; procedures for handling an overdose; and the impact of overdose in the USA. - The pharmacist counsels every patient who is receiving naloxone and provides them with written educational materials. |
| Gandhi [23] | 2020 | USA | Pharmacists | Intervention study | I: Communication technique training (CTT) C: Baseline before training | Dispensing rates of naloxone and pharmacist and pharmacy-related factors that may affect the dispensing rates of naloxone | - The CTT consisted of a pocket card reference and patient-case scenario activity. - The cases emphasized the points found on the card and were taught as a teach-back method. - The CTT caused 4-fold increase in naloxone dispensing. |
| Morton [24] | 2017 | USA | Pharmacies | Intervention study with a top-down approach of expanding legislation to include a standing order for naloxone and a bottom-up approach of pharmacy staff training | I: Expanding legislation by allowing standing order for naloxone and with pharmacy staff naloxone training C: Dispensing patterns of same pharmacies in previous years | Number of: - pharmacies dispensing naloxone - naloxone doses dispensed - counties in which naloxone was available through pharmacies | Barriers: pharmacy reimbursement, affordability for patients, and lack of patient interest. - 9-fold increase in the first half of 2016 of naloxone Medicaid claims over 2014. - The bottom-up approach included pharmacy staff training, free resources for pharmacies, and peer-to-peer coaching/support. - The Human Services Department initiated a public awareness campaign to promote opioid overdose death and naloxone awareness. |
| Skoy [25] | 2019 | USA | Patients | Intervention study at three pharmacies | I: Opt-out naloxone dispensing C: None | -Implementation of an opt-out naloxone dispensing program - Patients prescribed and dispensed naloxone | Barriers: lack of patient perceived need due to chronic opioid use without problems Facilitators: having all pharmacists working authorized to prescribe naloxone, not labeling the naloxone kit until the patient accepted the service, involving technicians in the training process, automatic calculation of Morphine Milliequivalents (MME)/day within the dispensing software - Naloxone nasal spray was most commonly prescribed. - Each patient presenting to the pharmacy with an opioid prescription written for ≥ 50 MME/day was prescribed and dispensed naloxone by the pharmacist if not already on their profile. - If prescribed and dispensed, a form called “Naloxone Worksheet” was attached to the final prescription bag to serve as a hard-stop. - Even if a patient denies naloxone, a handout on naloxone was provided. Moreover, if refused, the naloxone stays on file for future review. - Pharmacists reported increased comfort in recommending and dispensing naloxone. -RPhs mentioned that technicians should be involved in the training process since they are typically involved at intake and point of sale. |
| Strand [32] | 2019 | USA | Pharmacies | Intervention study employing a statewide risk assessment program called ONE Rx | N/A | -Implementation of the ONE Rx program - Populations impacted by the program - Future implications of the program | - The program involves screening patients who receive an opioid prescription for the risk of opioid misuse and accidental overdose and offering interventions which can include discussing benefits of naloxone and offering a naloxone kit. - The screening was completed by each patient before receiving an opioid medication. - Based upon screening results, pharmacists provided education and interventions using a clinical decision-making triage tool. - Pharmacist interventions with included: opioid prescription partially filled, discuss community support services, explain benefits of naloxone, dispense naloxone, discuss opioid use disorder, discuss accidental overdose. |
| Taylor [26] | 2020 | USA | Patients | Intervention study at a community pharmacy within a healthcare clinic serving low socioeconomic status patients | I: Naloxone screening tool (3 months) C: Baseline (previous 3 and 12 months) | Naloxone dispensing | Barriers: availability of naloxone, cost, pharmacist lack of comfort with naloxone - Survey consisted of 3 questions that were read to patients upon each visit. - Those deemed eligible for naloxone received a naloxone training session along with a free kit. - Dispensing rates of naloxone improved with active identification of patients who qualify or need access to naloxone, despite active naloxone advertisement in the pharmacy. - Providing naloxone free of cost lifted barriers for patients. |
| Bachyrycz [31] | 2015 | USA | Pharmacists | Intervention study evaluated using a brief reporting form | I: Pharmacist training and naloxone dispensing | Trends in opioid overdose prevention | - Majority of the patients accessing naloxone noted it was their first time. - Most common reason for naloxone prescription was due to high dose prescription opioids, followed by chronic opioid use. - Request for naloxone by a patient was primarily from patients on opioid maintenance therapy. |
| Green [27] | 2020 | USA | CVS Pharmacies | Intervention study | I: Naloxone mandated co-prescription C: Standard of practice | Pharmacy naloxone provision | - Naloxone-prescribing mandates tripled pharmacy naloxone provision - This approach engaged more prescribers, complemented ongoing naloxone provision under pharmacy standing orders, expanded geographic reach, and broadened the naloxone payor mix. |
| Griffin [28] | 2019 | USA | Patients on Opioid Agonist Therapy, chronic opioid therapy, high-risk, or >= 50 MME/day | Intervention study | 3-month pre-intervention period 1-month staff training intervention 3-month post-intervention period. | Naloxone prescriptions dispensed | Barrier: Stigma (not wanting to be labeled an addict) - Patients were tagged in the pharmacy software if they met inclusion criteria and then guided toward the pharmacy consultation room when they presented at the pharmacy. - Patients did not think they needed naloxone because they had been taking opioid medications for years or they had stopped their opioid prescription. |
| Skoy [33] | 2019 | USA | Pharmacies | Intervention study employing a statewide risk assessment program called ONE Rx | I: The ONE Rx program C: None | Number of: - Patients screened for opioid misuse and accidental overdose with the ONE Rx program -Pharmacists/technicians who participated in the training - Pharmacies who chose to implement ONE Rx | Barriers: Time, workflow - Pharmacy staff completed a training, and then implemented the program through screening patients at risk of opioid misuse and accidental overdose. - Every patient receiving an opioid prescription is screened for the following: risk of opioid use disorder using Opioid Risk Tool and risk of accidental overdose based on age, concurrent medications, and disease states. - The patient completes a screening tool before receiving an opioid medication. - Pharmacist reviews the screening results and provides patient-specific education and interventions using a clinical decision-making triage tool - Potential interventions can include counselling on (1) dispensing of naloxone, (2) substance use disorder, (3) referral to community support services, (4) partial fill of opioid prescription, (5) and providing pharmacy medication disposal. |
| Sexton [35] | 2019 | USA | Patients at risk of opioid overdose | Intervention study | I: Standardized team-based approach to identify naloxone-eligible persons. C1: Standard practice at control store. C2: Previous year dispensing numbers at both stores. | - Naloxone kits dispensed - Access to naloxone - Pharmacist–patient relationship | Barriers: cost - The program consisted of the pharmacy receiving training, a MME conversion chart, eligibility checklist, a list of relevant opioids. - Patients were screened for naloxone eligibility during prescription intake, if presented an opioid prescription. - Potential candidates were flagged for the pharmacist and put in the pharmacy software, creating a hard-stop. - All eligible patients—including those who refused naloxone—were provided with an educational handout. - Some patients who accepted a kit reported that they needed to use it and were thankful that they had received a kit. |
| Laird [18] | 2014 | Scotland | Injection Equipment Provision (IEP) Pharmacies serving Injection Drug Users | Pilot intervention using pre and post questionnaires to evaluate knowledge | I: Extending provision of staff training and supplies to IEP pharmacies | Feasibility of providing naloxone in community IEP pharmacies | - Injection Equipment Provision (IEP) pharmacies are ideal for offering naloxone training and supply. - None of the pharmacy staff answered the prequestionnaire correctly before training. |
Appendix D. Non-Intervention Studies
| Author | Year | Location | Population Studied | Methods | Outcomes Measured | Key Findings |
|---|---|---|---|---|---|---|
| Cross-sectional survey | ||||||
| Shedd [65] | 2019 | USA | Pharmacists | Emailed survey | Barriers and attitudes | Facilitator: pharmacy protocols |
| Carpenter [26] | 2019 | USA | Pharmacists | Online survey | Factors associated with how often pharmacists offer and dispense naloxone | Barriers: time, inadequate training, perceived lack of patient comprehension Facilitators: comfort discussing naloxone, naloxone training for pharmacists - Most pharmacists stocked naloxone, but few offer and even fewer dispense it - Pharmacists working in smaller chain pharmacies dispense/offer naloxone less often than other pharmacy types - Pharmacists request training for: methods naloxone counselling, standing orders, choosing between formulations, and identifying patients who would benefit from naloxone |
| Graves [40] | 2019 | USA | Pharmacy staff | Survey with interviewers posing as customers | - Naloxone availability/price - Pharmacy staff knowledge of standing order | Barriers: education - National pharmacies are more likely to carry and have knowledgeable staff. - Some pharmacy staff incorrectly stated that a prescription was required for naloxone, or it could not be obtained for a third party. |
| Guadamuz [41] | 2019 | USA | Pharmacies | Telephone survey | Availability and cost of naloxone nasal spray | Barriers: cost - Naloxone was less likely to be available in districts with elevated rates of opioid overdose deaths, minority neighborhoods. - Despite the standing order, many pharmacists required a prescription. |
| Egan [49] | 2020 | USA | Pharmacies | Survey using mystery caller protocol | Pharmacy and neighborhood characteristics associated with pharmacy stocking and willingness to sell naloxone | - An estimated 2 out of 3 North Carolina retail pharmacies have naloxone available without a prescription. - The odds of naloxone availability were lower for independent pharmacies than chains. - Most recommended going to a chain pharmacy for naloxone if it was unavailable at their pharmacy. |
| Lozo [44] | 2019 | USA | Pharmacies | Survey with scripted questions | Naloxone availability and sociodemographic factors associated with it | Barriers: insurance, cost - Higher median household income indicated more naloxone availability - Cities identified with severe opioid-related public health concerns but limited naloxone access |
| Spivey [54] | 2020 | USA | Pharmacies | Telephone survey | - Availability and pricing - Barriers to naloxone dispensing - Strategies to improve access | Barriers: cost, patient refusal, lack of insurance coverage, stigma, issues with prescribers, and lack of patient education interest or awareness about naloxone. Facilitators: improved insurance coverage, improving naloxone-related education for patients, pharmacists, and other providers - Most pharmacies reported recommending naloxone ≥50% of patients taking an opioid with a dose of 50MMEs/day - For patients co-prescribed benzodiazepines or with respiratory conditions, less than the majority of pharmacies recommended naloxone to ≥50% of that patient population |
| Nichols [37] | 2019 | USA | Pharmacists | Online survey | Pharmacist utilization, knowledge, attitude, and barriers to the naloxone standing order | Barriers: lack of patients asking for naloxone Facilitators: resources to increase awareness of naloxone access without a prescription and pharmacist comfort |
| Darracq [38] | 2019 | USA | Pharmacies | Survey | - RPh knowledge of naloxone-dispensing law, participation, and future plans for participation - Naloxone availability - Out of pocket charges to consumers | - Despite high rates of knowledge, current and future participation was low, especially in areas with high rates of prescription opioid-related deaths - Most pharmacies reported naloxone in stock and immediately available. - Counties with higher rates of pharmacy participation were associated with participation by a regional or national pharmacy chain. |
| Melaragni [63] | 2019 | USA | Pharmacists | Verbal survey | Pharmacist education and training associated with dispensing naloxone | Barriers: Education - Pharmacists demonstrated knowledge gaps for: calling 9-1-1 when witnessing an overdose, starting rescue breathing, placing patients in the recovery position, whether naloxone can be administered for minors or in pregnancy or in alcohol or barbiturate overdoses. - Majority of pharmacists said they would benefit from more training. |
| Sisson [46] | 2019 | USA | Pharmacists | Telephone survey | - Pharmacist attitudes toward naloxone - Potential barriers to pharmacy naloxone distribution | Barriers: cost, negative beliefs about naloxone, low demand by patients. - Rural pharmacies required more time to obtain naloxone and offered less extensive training. - Independent pharmacies were less likely to stock naloxone, especially rural locations. - Pharmacist negative beliefs about naloxone allow opioid user to conduct riskier practices, avoid seeking substance use treatment, and avoid emergency treatment after an overdose. |
| Jimenez [45] | 2019 | USA | Pharmacies | Simulated a routine conversation between pharmacy staff and a potential customer about the immediate availability of and requirements to purchase naloxone using a semi structured questionnaire. | - Availability of naloxone in pharmacies - Pharmacy staff knowledge regarding naloxone dispensing protocols | Barriers: lack of availability, ambiguity of the standing order. - Most pharmacies only carry naloxone nasal spray. - In states with highest opioid overdose deaths, about a quarter do not stock naloxone. - Only half of pharmacy employees knew there was no minimum age requirement to purchase naloxone |
| Kuhn [67] | 2019 | USA | Pharmacies | Phone survey | - Naloxone availability - Pharmacist familiarity with naloxone standing order, knowledge, and educational compliance | - Most pharmacies had naloxone available and were familiar with the standing order. - Most pharmacies did not have previous knowledge of the Opioid Assistance and Referral Line. |
| Meyerson [39] | 2018 | USA | Pharmacists | Census | Factors associated with community pharmacy naloxone stocking and dispensing | - More pharmacists stocked naloxone than dispensed it. - Chain pharmacies significantly more likely to stock naloxone. - Naloxone stocking more likely in pharmacies with ≥1 full-time pharmacist. - Pharmacy manager having naloxone education associated with higher likelihood of pharmacy stocking naloxone. |
| Bachyrycz [47] | 2017 | USA | Patients | Data from NRK prescriptions | Prescription patterns of Naloxone Rescue Kits (NRKs) | Barriers: optional naloxone certification for pharmacists and variable insurance coverage Facilitator: pharmacy accessibility - Most patients indicated it was their first NRK - Most common reason for a NRK was the patient’s request - Few NRK prescriptions given to patients with polysubstance use - NRK program is under-utilized in rural areas |
| Rudolph [55] | 2018 | USA | Pharmacists | Online survey | - Barriers to dispensing naloxone - Identify areas for additional training | Barriers: discomfort dispensing, inadequate training, workflow concerns, lack of management support, cost/reimbursement, and ethical concerns. - Positive correlation found between pharmacists’ knowledge of naloxone and opioid overdose and willingness to dispense naloxone. - There are no correlations between level of comfort for dispensing naloxone with type of pharmacy practice setting or number of opioids dispensed daily. - Additional training needs included: information regarding naloxone/opioid overdose, strategies to initiate patient discussion, identifying eligible patients, and workflow implementation. |
| Cressman [11] | 2017 | CND | Pharmacies | Telephone survey | Availability, cost, and need for a prescription for naloxone | Barriers: stigma, cost, perceived lack of demand, pharmacist lack of training. - Availability was highest in BC, followed by the Maritimes, ON and Central and Northern Canada. - QC had the lowest availability. - Some pharmacies who did not carry naloxone referenced not having received the education. |
| Thornton [66] | 2017 | USA | Pharmacists | Survey administered at Continuing Pharmacy Education events | - Educational needs relating to naloxone provision in community pharmacies | - Most pharmacists agree that letting patients purchase naloxone OTC will increase opioid overdoses. - Majority of pharmacists are not comfortable selling naloxone without a prescription despite knowing it is effective. |
| Stone [50] | 2018 | USA | Pharmacies | Telephone survey | - Availability of naloxone in retail pharmacies | - Independent pharmacies less likely to have naloxone compared to chains. |
| Grey literature | ||||||
| CDC [42] | 2019 | USA | N/A | N/A | Naloxone dispensing | - Wide variations in pharmacy dispensing, despite consistent state laws. - Rural counties had the lowest dispensing rates. - One naloxone prescription dispensed per 70 high dose opioid prescriptions |
| CPhA [43] | 2017 | CND | Canada | Environmental scan | Naloxone accessibility | - At every purchase, provincial regulations require pharmacists to review a patient’s history of opioid use, naloxone use/response, allergies, and offer counselling. - In all provinces, pharmacists are required to train patients. - Only the Northwest Territories and Yukon have THN kits available in every pharmacy. - The Alberta and Quebec programs enable patients to get a naloxone kit without a health card. |
| Moustaqim-Barrette [60] | 2019 | CND | N/A | Environmental scan and conversations with key informants | - Uptake of naloxone programs - Knowledge and operational barriers | Barriers: Expiry/temperature of naloxone, stigma in rural areas, minimum training standards, withdrawal/adverse effects Facilitator: Political will - The injectable formulation is available in all THN programs. - Ontario, Quebec, and NWT provide nasal naloxone. |
| Alberta College of Pharmacy [64] | 2019 | CND | N/A | N/A | Naloxone kits distributed | Facilitator: not asking for identification - Identification is not needed when requesting a kit, which reduces stigma. - Improvements are contemplated based on feedback from the naloxone kit usage forms; feedback is only used to improve the program. |
| BC CDC [48] | 2019 | CND | N/A | Mixed methods with administrative data and discussions with stakeholders | - Strengths and barriers of THN program implementation and management - Stakeholder attitudes, perceptions, and beliefs | Barriers: lack of remuneration, communication gaps, and logistical challenges (lag in data entry) Facilitators: modifying implementation procedures (introducing electronic records), refresher training for pharmacists, handouts, intranasal kits - In just one year (2018), over 3000 kits were distributed by 562 pharmacies - Most recipients at pharmacy sites were receiving their first kit - Majority of kits are distributed to individuals not at risk of overdose themselves |
| Roberts [59] | 2019 | USA | N/A | Structured internet searches | Naloxone training mandates | Barrier: lack of standardized naloxone training requirements for pharmacists - Oregon and Vermont require people who purchase naloxone from community pharmacies to verify that they have completed naloxone education. |
| Longitudinal study | ||||||
| Green [51] | 2019 | USA | Pharmacies | Longitudinal analysis of pharmacy naloxone dispensing | Characteristics associated with increased likelihood of naloxone dispensing | Factors associated with an increased likelihood of naloxone dispensing: – rurality - high opioid prescription volume and syringe sales - drive-throughs - long weekend hours - younger patient population |
| Population-based study | ||||||
| Choremis [12] | 2019 | CND | Ontario residents | Cross-sectional analysis and descriptive analysis | - Uptake of THN program - Characteristics of the patients and pharmacies | - Only half of Ontario’s pharmacies dispense/offer naloxone. - Highest uptake for patients on opioid agonist therapy. - Minimal uptake for patients on prescription opioids, past opioid exposure, or unknown opioid exposure. - The majority of pharmacies offering naloxone are in urban areas. |
| Qualitative studies | ||||||
| Green [52] | 2017 | USA | Patients taking opioids for chronic pain, people with opioid use disorders, caregivers, and pharmacists | Focus groups, semi-structured interviews | Perceptions and experiences of pharmacy naloxone from various groups | Barriers: Stigma, patients fearing future consequences, pharmacists fearing offending the patient, time, space constraints. - Practice modification suggested to reduce stigma: pharmacists universally ask patients about naloxone (with some criteria), as opposed to always waiting for the patient to initiate the conversation. - Pharmacists expressed a lack of clarity on logistics, insufficient training and demonstration materials. - Some patients reported believing naloxone was only meant for heroin users and others were unaware that pharmacies could provide it. |
| Olsen [53] | 2019 | Australia | Pharmacists | Survey and semi-structured interviews | Pharmacists’ attitudes to and experiences of OTC naloxone. | Barriers: low confidence, stigma, limited understanding of opioid overdose, business concerns. - Some pharmacists were unsure of how to advise a patient who requested naloxone, educate patients about naloxone availability, and approach the topic of overdose. - Some pharmacists were unable to correctly state the purpose of naloxone, others had negative views such as attracting an undesirable clientele. - Half of pharmacists were aware that naloxone changed to OTC status. |
| Donovan [56] | 2020 | USA | Pharmacy leaders | Semi-structured interviews | Pharmacy leader perception of pharmacies and how staff can optimize naloxone dispensing | Barriers: stigma (in general), stigma (within the context of a rural community), comfort, workflow, time, lack of compensation for counselling patients. Facilitators: standardized trainings, state regulations and federal initiatives, co-prescribing of naloxone by physicians, pharmacists as public health leaders |
| Donovan [61] | 2019 | USA | Obtained naloxone from the pharmacy or high-risk patient as per study criteria | Semi-structured interviews | Factors impacting the likelihood of obtaining pharmacy-based naloxone (PBN) | Barriers: Pharmacist education, stigma, disempowerment for patients prescribed opioids. Facilitators: Empowerment for people who use drugs. - People prescribed opioids do not feel they are at risk of overdose or need naloxone and feel that their family members are not at risk of an overdose. - Participants also noted a lack of staff training, including confusion about dispensing and billing procedures. |
| Green [58] | 2020 | USA | Patients taking opioids for chronic pain, people with opioid use disorders, caregivers, and pharmacists | Focus groups, semi-structured interviews | - Experiences obtaining naloxone at the pharmacy - Reactions to pharmacy tools and patient outreach materials | Barriers: Fear of future consequences when requesting naloxone, stigma, discomfort in asking pharmacy staff for naloxone Facilitators: practice made pharmacists more comfortable in dispensing, creating privacy for patients, interprofessional collaboration - Participants were accepting of a program that included display pads which patients could present to the pharmacist to reduce the stigma of verbally asking for a naloxone kit. - Pharmacists expressed a desire for further education because they still felt uncomfortable engaging naloxone discussions even with previous experience/training. - Pharmacy technicians lack sufficient program training. |
| Mixed Methods | ||||||
| Hammett [62] | 2014 | USA | N/A | Interviews, review of legal and policy documents, and information on stakeholders. | - Feasibility of expanded pharmacy services for people who inject drugs - Legal and policy barriers | Barriers: stigma, prescription status - At the time of this study, naloxone was a prescription in all study locations and seldom stocked in pharmacies. |
| Bakhireva [57] | 2018 | USA | Pharmacists | Structured, quantitative survey created after focus group | Barriers and facilitators | Barriers: cost, time, inadequate pharmacy reimbursement, inadequate privacy for patient counselling, lack of access to full medical records of patients, pharmacy manager does not allow naloxone dispensing, attracting undesirable clientele Facilitators: increased awareness among patients about the need for naloxone, education for the general public, and additional training for pharmacists on how to initiate discussions with high-risk patients - Majority of community pharmacists never dispensed naloxone before despite prescriptive authority and standing orders. - Some pharmacists reported fear that dispensing Intranasal Naloxone would promote opioid abuse and attract undesirable clientele to the pharmacy. |
References
- Government of Canada. Opioid Related Harms in Canada. 2020. Available online: https://health-infobase.canada.ca/substance-related-harms/opioids/ (accessed on 12 August 2020).
- Centers for Disease Control and Prevention. Drug Overdose Deaths. 2020. Available online: https://www.cdc.gov/drugoverdose/data/statedeaths.html (accessed on 12 August 2020).
- Government of Canada. Measuring the Impact of the Opioid Overdose Epidemic on Life Expectancy at Birth in Canada. 2020. Available online: https://www.canada.ca/en/health-canada/services/substance-use/problematic-prescription-drug-use/opioids/data-surveillance-research/harms-deaths/measuring-impact-on-life-expectancy.html (accessed on 22 February 2019).
- Belzak, L.; Halverson, J. Evidence synthesis—The opioid crisis in Canada: A national perspective. Health Promot. Chronic Dis. Prev. Can. 2018, 38, 224–233. [Google Scholar] [CrossRef] [PubMed]
- Government of Canada. Prescription Drug List: Naloxone. 2020. Available online: https://hpr-rps.hres.ca/pdl.php?lang=en (accessed on 12 August 2020).
- National Alliance of State Pharmacy Associations. Pharmacist Prescribing: Naloxone. 2019. Available online: https://naspa.us/resource/naloxone-access-community-pharmacies/ (accessed on 12 August 2020).
- Compton, W.M.; Jones, C.M.; Stein, J.B.; Wargo, E.M. Promising roles for pharmacists in addressing the U.S. opioid crisis. Res. Social Adm. Pharm. 2019, 15, 910–916. [Google Scholar] [CrossRef] [PubMed]
- Fairbairn, N.; Coffin, P.O.; Walley, A.Y. Naloxone for heroin, prescription opioid, and illicitly made fentanyl overdoses: Challenges and innovations responding to a dynamic epidemic. Int. J. Drug Policy 2017, 46, 172–179. [Google Scholar] [CrossRef] [PubMed]
- Sporer, K.A.; Kral, A.H. Prescription naloxone: A novel approach to heroin overdose prevention. Ann. Emerg. Med. 2007, 49, 172–177. [Google Scholar] [CrossRef] [PubMed]
- Clark, A.K.; Wilder, C.M.; Winstanley, E.L. A systematic review of community opioid overdose prevention and naloxone distribution programs. J. Addict. Med. 2014, 8, 153–163. [Google Scholar] [CrossRef]
- Cressman, A.M.; Mazereeuw, G.; Guan, Q.; Jia, W.; Gomes, T.; Juurlink, D.N. Availability of naloxone in Canadian pharmacies:a population-based survey. CMAJ Open. 2017, 5, E779–E784. [Google Scholar] [CrossRef][Green Version]
- Choremis, B.; Campbell, T.; Tadrous, M.; Martins, D.; Antoniou, T.; Gomes, T. The uptake of the pharmacy-dispensed naloxone kit program in Ontario: A population-based study. PLoS ONE 2019, 14, e0223589. [Google Scholar] [CrossRef]
- Nielsen, S.; Van Hout, M.-C. What is known about community pharmacy supply of naloxone? A scoping review. Int. J. Drug Policy 2016, 32, 24–33. [Google Scholar] [CrossRef]
- Muzyk, A.; Smothers, Z.; Collins, K.; MacEachern, M.; Wu, L. Pharmacists’ attitudes toward dispensing naloxone and medications for opioid use disorder: A scoping review of the literature. Subst. Abus. 2019, 40, 476–483. [Google Scholar] [CrossRef]
- Thakur, T.; Frey, M.; Chewning, B. Pharmacist roles, training, and perceived barriers in naloxone dispensing: A systematic review. J. Am. Pharm. Assoc. 2020, 60, 178–194. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.; The PRISMA Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Laird, A.; Hunter, C. Glasgow city injecting equipment provision (IEP) pharmacy naloxone training pilot. Int. J. Pharm. Prac. 2014, S1, 2–27. [Google Scholar]
- Gangal, N.S.; Hincapie, A.L.; Jandarov, R.; Frede, S.; Boone, J.; Mackinnon, N.; Koechlin, K.; DeFiore-Hyrmer, J.; Holthusen, A.; Heaton, P. Association Between a State Law Allowing Pharmacists to Dispense Naloxone Without a Prescription and Naloxone Dispensing Rates [published correction appears in JAMA Netw Open. 2020 Mar 2;3(3):e201568]. JAMA Netw. Open. 2020, 3, e1920310. [Google Scholar] [CrossRef] [PubMed]
- Champaloux, S.; Taitel, M.; Gleason, P.; McClelland, S. Impact of Distributing an Opioid Safety Guide at Prescription Pickup. J. Manag. Care Spec. Pharm. 2018, 24 (Suppl. S10-a), S1–S112. [Google Scholar] [CrossRef]
- Eldridge, L.A.; Agley, J.; Meyerson, B.E. Naloxone availability and dispensing in Indiana pharmacies 2 years after the implementation of a statewide standing order. J. Am. Pharm. Assoc. 2020, 60, 470–474. [Google Scholar] [CrossRef]
- Shafer, E.; Bergeron, N.; Smith-Ray, R.; Robson, C.; O’Koren, R. A nationwide pharmacy chain responds to the opioid epidemic. J. Am. Pharm. Assoc. 2017, 57, S123–S129. [Google Scholar] [CrossRef]
- Gandhi, N.; Hanes, S.; Candelario, D.; Clough, C.; Highland, J. Impact of a communication technique training on rates of naloxone dispensing. J. Am. Pharm. Assoc. 2020, 60, S37–S40.e1. [Google Scholar] [CrossRef]
- Morton, K.J.; Harrand, B.; Floyd, C.C.; Schaefer, C.; Acosta, J.; Logan, B.C.; Clark, K. Pharmacy-based statewide naloxone distribution: A novel “top-down, bottom-up” approach. J. Am. Pharm. Assoc. 2017, 57, S99–S106.e5. [Google Scholar] [CrossRef]
- Skoy, E. A pilot evaluation of incorporating “opt-out” naloxone dispensing within a chain community pharmacy. Res. Soc. Adm. Pharm. 2019, 15, 1043–1046. [Google Scholar] [CrossRef]
- Taylor, S.R.; Chaplin, M.D.; Hoots, K.; Roberts, C.; Smiths, K. Effectiveness of Implementing a Naloxone Screening Tool in a Community Pharmacy. Addict. Disord. Their Treat. 2020, 19, 142–145. [Google Scholar] [CrossRef]
- Green, T.C.; Davis, C. Laws Mandating Coprescription of Naloxone and Their Impact on Naloxone Prescription in Five US States, 2014–2018. Am. J. Public Health 2020, 110, 881–887. [Google Scholar] [CrossRef] [PubMed]
- Griffin, S.; Wishart, B.; Bricker, K.; Luebchow, A. Impact of a pharmacist-driven intervention on the outpatient dispensing of naloxone. J. Am. Pharm. Assoc. 2019, 59, S161–S166. [Google Scholar] [CrossRef] [PubMed]
- Akers, J.L.; Hansen, R.N.; Oftebro, R.D. Implementing take-home naloxone in an urban community pharmacy. J. Am. Pharm. Assoc. 2017, 57, S161–S167. [Google Scholar] [CrossRef] [PubMed]
- Freeman, L.K.; Bourque, S.; Etches, N.; Goodison, K.; O’Gorman, C.; Rittenbach, K.; Sikora, C.A.; Yarema, M. Alberta’s provincial take-home naloxone program: A multi-sectoral and multi-jurisdictional response to overdose. Can. J. Public Health 2017, 108, e398–e402. [Google Scholar] [CrossRef] [PubMed]
- Bachyrcz, A.; Shrestha, S.; Shah, D.; Tinker, D.; Bakhireva, L. Naloxone pharmacist prescriptive authority program: Early successes with prescribing Naloxone rescue kits in New Mexico. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2015, 35, e175–e325. [Google Scholar] [CrossRef]
- Strand, M.A.; Eukel, H.; Frenzel, O.; Skoy, E.; Steig, J.; Werremeyer, A. Program evaluation of the Opioid and Naloxone Education (ONE Rx) program using the RE-AIM model. Res. Soc. Adm. Pharm. 2020, 16, 1248–1254. [Google Scholar] [CrossRef]
- Skoy, E.; Eukel, H.; Werremeyer, A.; Strand, M.; Frenzel, O.; Steig, J. Implementation of a statewide program within community pharmacies to prevent opioid misuse and accidental overdose. J. Am. Pharm. Assoc. 2020, 60, 117–121. [Google Scholar] [CrossRef]
- Wilkerson, D.M.; Groves, B.K.; Mehta, B.H. Implementation of a naloxone dispensing program in a grocery store-based community pharmacy. Am. J. Health Syst. Pharm. 2020, 77, 511–514. [Google Scholar] [CrossRef]
- Sexton, S.M.; Armstrong, A.; Gatton, O.; Rhodes, L.A.; Marciniak, M.W. A standardized team-based approach for identifying naloxone-eligible patients in a grocery store pharmacy. J. Am. Pharm. Assoc. 2019, 59, S95–S100. [Google Scholar] [CrossRef]
- Carpenter, D.M.; Dhamanaskar, A.K.; Gallegos, K.L.; Shepherd, G.; Mosley, S.L.; Roberts, C.A. Factors associated with how often community pharmacists offer and dispense naloxone. Res. Soc. Adm. Pharm. 2019, 15, 1415–1418. [Google Scholar] [CrossRef] [PubMed]
- Nichols, G.S. Illinois Pharmacists’ Awareness of and Barriers to Dispensing Naloxone under Standing Order. J. Addict. Med. 2019, 13, E1–E42. [Google Scholar] [CrossRef]
- Darracq, M.A.; Lee, J.; Wilson, T.; Lasoff, D.; Armenian, P. Pharmacist dispensed naloxone: Knowledge, availability, participation and cost in selected California counties. Int. J. Drug Policy 2019, 71, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Meyerson, B.E.; Agley, J.D.; Davis, A.; Jayawardene, W.; Hoss, A.; Shannon, D.J.; Ryder, P.T.; Ritchie, K.; Gassman, R. Predicting pharmacy naloxone stocking and dispensing following a statewide standing order, Indiana 2016. Drug Alcohol Depend. 2018, 188, 187–192. [Google Scholar] [CrossRef]
- Graves, R.L.; Andreyeva, E.; Perrone, J.; Shofer, F.S.; Merchant, R.M.; Meisel, Z.F. Naloxone Availability and Pharmacy Staff Knowledge of Standing Order for Naloxone in Pennsylvania Pharmacies. J. Addict. Med. 2019, 13, 272–278. [Google Scholar] [CrossRef]
- Guadamuz, J.S.; Alexander, C.G.; Chaudhri, T.; Trotzky-Sirr, R.; Qato, D.M. Availability and Cost of Naloxone Nasal Spray at Pharmacies in Philadelphia, Pennsylvania, 2017. JAMA Netw. Open. 2019, 2, e195388. [Google Scholar] [CrossRef]
- Still Not Enough Naloxone Where It’s Most Needed. Center for Disease Control and Prevention. 2019. Available online: https://www.cdc.gov/media/releases/2019/p0806-naloxone.html (accessed on 6 August 2020).
- Environmental Scan: Access to Naloxone across Canada. Canadian Pharmacists Association. Updated November, 2017. Available online: https://www.pharmacists.ca/cpha-ca/assets/File/cpha-on-the-issues/Environmental%20Scan%20-%20Access%20to%20Naloxone%20Across%20Canada_Final.pdf (accessed on 6 August 2020).
- Lozo, K.W.; Nelson, L.S.; Ramdin, C.; Calello, D.P. Naloxone Deserts in NJ Cities: Sociodemographic Factors Which May Impact Retail Pharmacy Naloxone Availability. J. Med. Toxicol. 2019, 15, 108–111. [Google Scholar] [CrossRef]
- Jimenez, D.E.; Singer, M.R.; Adesman, A. Availability of Naloxone in Pharmacies and Knowledge of Pharmacy Staff Regarding Dispensing Naloxone to Younger Adolescents. J. Adolesc. Health 2019, 65, 698–701. [Google Scholar] [CrossRef]
- Sisson, M.L.; McMahan, K.B.; Chichester, K.R.; Galbraith, J.W.; Cropsey, K.L. Attitudes and availability: A comparison of naloxone dispensing across chain and independent pharmacies in rural and urban areas in Alabama. Int. J. Drug Policy 2019, 74, 229–235. [Google Scholar] [CrossRef]
- Bachyrycz, A.; Shrestha, S.; Bleske, B.E.; Tinker, D.; Bakhireva, L.N. Opioid overdose prevention through pharmacy-based naloxone prescription program: Innovations in health care delivery. Subst. Abus. 2017, 38, 55–60. [Google Scholar] [CrossRef]
- Mamdani, Z.; Buxton, J.A. Evaluation of British Columbia’s Take Home Naloxone Program in Community Pharmacies. BC Centre for Disease Control. 2019. Available online: https://www.bcpharmacists.org/readlinks/bc-take-home-naloxone-thn-program-update-evaluation-expansion-community-pharmacies (accessed on 6 August 2020).
- Egan, K.L.; Foster, S.E.; Knudsen, A.N.; Lee, J.G.L. Naloxone Availability in Retail Pharmacies and Neighborhood Inequities in Access. Am. J. Prev. Med. 2020, 58, 699–702. [Google Scholar] [CrossRef] [PubMed]
- Stone, R.; Hur, S.; Young, H.N. Assessment of naloxone stock status in Georgia retail pharmacies. J. Am. Coll. Clin. Pharm. 2018, 1, 122–353. [Google Scholar] [CrossRef]
- Green, T.C.; Bratberg, J.; Baird, J.; Burstein, D.; Lenz, K.; Case, P.; Walley, A.Y.; Xuan, Z. Rurality and differences in pharmacy characteristics and community factors associated with provision of naloxone in the pharmacy. Int. J. Drug Policy 2019, 85, 102602. [Google Scholar] [CrossRef] [PubMed]
- Green, T.C.; Case, P.; Fiske, H.; Baird, J.; Cabral, S.; Burstein, D.; Schwartz, V.; Potter, N.; Walley, A.Y.; Bratberg, J. Perpetuating stigma or reducing risk? Perspectives from naloxone consumers and pharmacists on pharmacy-based naloxone in 2 states. J. Am. Pharm. Assoc. 2017, 57, S19–S27.e4. [Google Scholar] [CrossRef]
- Olsen, A.; Lawton, B.; Dwyer, R.; Taing, M.W.; Chun, K.L.J.; Hollingworth, S.; Nielsen, S. Why aren’t Australian pharmacists supplying naloxone? Findings from a qualitative study. Int. J. Drug Policy 2019, 69, 46–52. [Google Scholar] [CrossRef]
- Spivey, C.A.; Wilder, A.; Chisholm-Burns, M.A.; Stallworth, S.; Wheeler, J. Evaluation of naloxone access, pricing, and barriers to dispensing in Tennessee retail community pharmacies. J. Am. Pharm. Assoc. 2020, 60, 694–701.e1. [Google Scholar] [CrossRef]
- Rudolph, S.E.; Branham, A.R.; Rhodes, L.A.; Hayes Jr, H.; Moose, J.S.; Marciniak, M.W. Identifying barriers to dispensing naloxone: A survey of community pharmacists in North Carolina. J. Am. Pharm. Assoc. 2018, 58, S55–S58.e3. [Google Scholar] [CrossRef]
- Donovan, E.; Bratberg, J.; Baird, J.; Burstein, D.; Case, P.; Walley, A.Y.; Green, T.C. Pharmacy leaders’ beliefs about how pharmacies can support a sustainable approach to providing naloxone to the community. Res. Social Adm. Pharm. 2020, 16, 1493–1497. [Google Scholar] [CrossRef]
- Bakhireva, L.N.; Bautista, A.; Cano, S.; Shrestha, S.; Bachyrycz, A.M.; Cruz, T.H. Barriers and facilitators to dispensing of intranasal naloxone by pharmacists. Subst. Abus. 2018, 39, 331–341. [Google Scholar] [CrossRef]
- Green, T.C.; Donovan, E.; Klug, B.; Case, C.; Baird, J.; Burstein, D.; Tapper, A.; Walley, A.Y.; Bratberg, J. Revisiting pharmacy-based naloxone with pharmacists and naloxone consumers in 2 states: 2017 perspectives and evolving approaches. J. Am. Pharm. Assoc. 2020, 60, 740–749. [Google Scholar] [CrossRef]
- Roberts, A.W.; Carpenter, D.M.; Smith, A.; Look, K.A. Reviewing state-mandated training requirements for naloxone-dispensing pharmacists. Res. Social Adm. Pharm. 2019, 15, 222–225. [Google Scholar] [CrossRef] [PubMed]
- Environmental Scan: Naloxone Access and Distribution in Canada. Vancouver: Canadian Research Initiative in Substance Misuse (CRISM). 2019. Available online: https://crism.ca/wp-content/uploads/2019/06/CRISM_Enviro-Scan_Final-Draft_June18.pdf (accessed on 6 August 2020).
- Donovan, E.; Case, P.; Bratberg, J.P.; Baird, J.; Burstein, D.; Walley, A.Y.; Green, T.C. Beliefs Associated with Pharmacy-Based Naloxone: A Qualitative Study of Pharmacy-Based Naloxone Purchasers and People at Risk for Opioid Overdose. J. Urban Health 2019, 96, 367–378. [Google Scholar] [CrossRef] [PubMed]
- Hammett, T.M.; Phan, S.; Gaggin, J.; Case, P.; Zaller, N.; Lutnick, A.; Kral, A.H.; Fedorova, E.V.; Heimer, R.; Small, W.; et al. Pharmacies as providers of expanded health services for people who inject drugs: A review of laws, policies, and barriers in six countries. BMC Health Serv. Res. 2014, 14, 261. [Google Scholar] [CrossRef] [PubMed]
- Melaragni, F.; Levy, C.; Pedrazzi, J.; Andersen, M. Assessing pharmacists’ readiness to dispense naloxone and counsel on responding to opioid overdoses. J. Am. Pharm. Assoc. 2019, 59, 550–554.e2. [Google Scholar] [CrossRef] [PubMed]
- ACP, RxA, and AHS Collaborate to Encourage Anonymity for Naloxone Kit Distribution. Alberta College of Pharmacists. 2019. Available online: https://abpharmacy.ca/articles/community-based-naloxone-partnership-save-lives (accessed on 6 August 2020).
- Shedd, M.; Bozhkova, A.; Kalich, B.A.; Wilkening, G.L. Evaluation of Bexar County community pharmacist attitudes toward harm reduction. Ment. Health Clin. 2019, 9, 383–391. [Google Scholar] [CrossRef] [PubMed]
- Thornton, J.D.; Lyvers, E.; Scott, V.G.G.; Dwibedi, N. Pharmacists’ readiness to provide naloxone in community pharmacies in West Virginia. J. Am. Pharm. Assoc. 2017, 57, S12–S18.e4. [Google Scholar] [CrossRef]
- Kuhn, B. Assessment of the familiarity by retail pharmacists regarding the availability and use of intranasal naloxone within a State. Clin. Toxicol. 2019, 57, 870–1052. [Google Scholar] [CrossRef]
| Objective | Number of Studies (%) |
|---|---|
| Take-Home Naloxone Programs | 18 (35%) |
| Naloxone Availability and Dispensing | 22 (42%) |
| Facilitators and Barriers | 30 (58%) |
| Knowledge Gaps | 17 (33%) |
| Theme | Number of Intervention Studies (%) |
|---|---|
| Laws | |
| Mandatory naloxone co-prescription with opioids | 1 (5.6%) [27] |
| Standing order | 2 (11.1%) [21,24] |
| Prescriptive authority | 4 (22.2%) [19,21,24,31] |
| OTC status of naloxone | 1 (5.6%) [30] |
| Education of pharmacy team prior to implementation | 10 (55.5%) [18,22,23,24,29,31,32,33,34,35] |
| Interventions | |
| PMS used to help flag patients eligible for naloxone | 3 (16.6%) [28,34,35] |
| Checklists (patient eligibility, patient counselling) | 4 (22.2%) [22,25,29,34] |
| Pocketcard | 1 (5.6%) [23] |
| Patient brochure | 4 (22.2%) [20,22,34,35] |
| Screening | 4 (22.2%) [26,32,33,34] |
| Opt-out | 1 (5.6%) [25] |
| Barriers or Facilitators | Number of Studies (%) |
|---|---|
| Top Barriers | |
| Cost/coverage | 12 (40%) [11,24,26,35,41,44,45,46,47,55,56,57] |
| Stigma | 12 (40%) [11,28,45,46,47,52,53,56,58,60,61,62] |
| Education/training for pharmacist | 9 (30%) [11,35,36,40,47,55,57,61,63] |
| Other Barriers | |
| Lack of patients asking for naloxone | 4 (13.3%) [11,24,37,46] |
| Patient refusal | 2 (6.6%) [25,45] |
| Workflow concerns | 3 (10%) [33,55,56] |
| Lack of time/space | 5 (25%) [33,35,36,52,56,57] |
| Lack of support from management | 2 (6.6%) [55,57] |
| Pharmacy reimbursement/remuneration | 5 (25%) [24,46,48,55,57] |
| Facilitators | |
| Pharmacist education/training | 5 (25%) [36,45,48,57,59] |
| Patient education/training | 2 (6.6%) [45,57] |
| Standardization in training | 2 (6.6%) [56,59] |
| Comfort discussing naloxone | 3 (10%) [36,37,58] |
| Interprofessional collaboration | 3 (10%) [25,56,58] |
| Patient private counselling | 1 (3.3%) [58] |
| Not asking for identification | 1 (3.3%) [64] |
| Pharmacy protocols | 1 (3.3%) [65] |
| Knowledge Gap | Number of Studies (%) |
|---|---|
| Patient Knowledge Gaps | |
| Theme: Misinformation | |
| Belief that only people who use substances illicitly need naloxone | 1 (5.8%) [52] |
| Belief that since they have been taking chronic opioid prescriptions for awhile either them or their family members are at risk of opioid overdose | 3 (17.6%) [25,28,61] |
| Theme: Awareness | |
| Unaware pharmacies can provide naloxone | 1 (5.8%) [52] |
| Pharmacist Knowledge Gaps | |
| Theme: Administrative Gaps | |
| Standing order | 3 (17.6%) [36,40,41] |
| Triaging patients to other resources when appropriate | 1 (5.8%) [55] |
| Dispensing requirements | 5 (29%) [30,40,45,52,53,61] |
| Theme: Clinical Gaps | |
| Understanding of the purpose of naloxone | 1 (5.8%) [53] |
| Belief that naloxone increases riskier opioid use practices and overdoses | 4 (23.5%) [46,53,57,66] |
| Specific circumstances of when naloxone can be given (ex: alcohol/barbiturate overdoses, in minors, in pregnancy) | 2 (1.2%) [45,63] |
| Ability to identify eligible patients | 4 (23.5%) [18,36,55,58] |
| Knowledge of different formulations | 2 (1.2%) [36,63] |
| Theme: Counselling Points | |
| Course of action after administering naloxone | 1 (5.8%) [36] |
| Calling 9-1-1 when witnessing an overdose | 1 (5.8%) [63] |
| Starting rescue breathing | 1 (5.8%) [63] |
| Placing patient in the recovery position | 1 (5.8%) [63] |
| Methods for teaching/starting discussions with patients about naloxone | 4 (23.5%) [36,53,55,57] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cid, A.; Daskalakis, G.; Grindrod, K.; Beazely, M.A. What Is Known about Community Pharmacy-Based Take-Home Naloxone Programs and Program Interventions? A Scoping Review. Pharmacy 2021, 9, 30. https://doi.org/10.3390/pharmacy9010030
Cid A, Daskalakis G, Grindrod K, Beazely MA. What Is Known about Community Pharmacy-Based Take-Home Naloxone Programs and Program Interventions? A Scoping Review. Pharmacy. 2021; 9(1):30. https://doi.org/10.3390/pharmacy9010030
Chicago/Turabian StyleCid, Ashley, George Daskalakis, Kelly Grindrod, and Michael A. Beazely. 2021. "What Is Known about Community Pharmacy-Based Take-Home Naloxone Programs and Program Interventions? A Scoping Review" Pharmacy 9, no. 1: 30. https://doi.org/10.3390/pharmacy9010030
APA StyleCid, A., Daskalakis, G., Grindrod, K., & Beazely, M. A. (2021). What Is Known about Community Pharmacy-Based Take-Home Naloxone Programs and Program Interventions? A Scoping Review. Pharmacy, 9(1), 30. https://doi.org/10.3390/pharmacy9010030








