Clinically Based Classification and Positioning Indication for Single-Piece Compressive Implants Placement in Regard to Extraction Socket
Abstract
:1. Introduction
2. Materials and Methods
2.1. Classification
2.2. Implant vs. Extraction Socket Position
2.3. Implant Site vs. Available Bone
2.3.1. Type I
2.3.2. Type II
2.3.3. Type III
2.3.4. Type IV
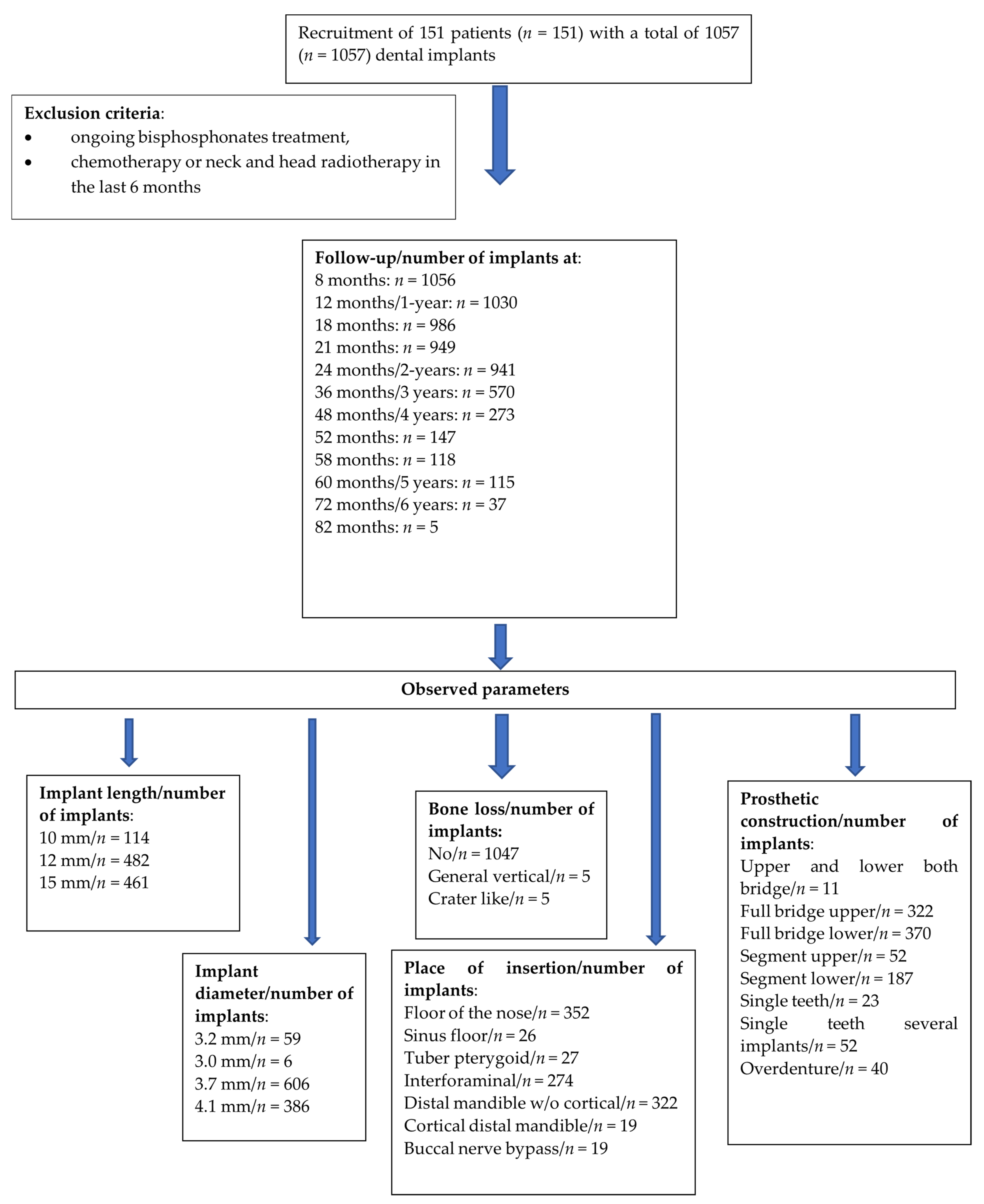
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Albrektsson, T.; Brånemark, P.-I.; Hansson, H.-A.; Lindström, J. Osseointegrated Titanium Implants: Requirements for Ensuring a Long-Lasting, Direct Bone-to-Implant Anchorage in Man. Acta Orthop. Scand. 1981, 52, 155–170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pasqualini, U.; Pasqualini, M.E. Treatise of Implant Dentistry: The Italian Tribute to Modern Implantology; Carimate (IT), Ariesdue: Milan, Italy, 2009. [Google Scholar] [PubMed]
- Abraham, C.M. A Brief Historical Perspective on Dental Implants, Their Surface Coatings and Treatments. Open Dent. J. 2014, 8, 50–55. [Google Scholar] [CrossRef]
- Lorenzoni, M.; Pertl, C.; Zhang, K.; Wimmer, G.; Wegscheider, W.A. Immediate loading of single-tooth implants in the anterior maxilla. Preliminary results after one year. Clin. Oral Implant. Res. 2003, 14, 180–187. [Google Scholar] [CrossRef] [PubMed]
- Schnitman, P.A.; Wohrle, P.S.; Rubenstein, J.E. Immediate fixed interim prostheses supported by two-stage threaded implants: Methodology and results. J. Oral Implantol. 1990, 16, 96–105. [Google Scholar] [PubMed]
- Mangano, C.; Mangano, F.G.; Shibli, J.A.; Roth, L.A.; Addazio, G.D.; Piattelli, A.; Iezzi, G. Immunohistochemical Evaluation of Peri-Implant Soft Tissues around Machined and Direct Metal Laser Sintered (DMLS) Healing Abutments in Humans. Int. J. Environ. Res. Public Health 2018, 15, 1611. [Google Scholar] [CrossRef] [Green Version]
- Sinjari, B.; D’Addazio, G.; De Tullio, I.; Traini, T.; Caputi, S. Peri-Implant Bone Resorption during Healing Abutment Placement: The Effect of a 0.20% Chlorhexidine Gel vs. Placebo—A Randomized Double-Blind Controlled Human Study. BioMed Res. Int. 2018, 2018, 1–13. [Google Scholar] [CrossRef] [Green Version]
- Resnik, R.R.; Misch, C.E. Misch’s Avoiding Complications in Oral Implantology; Elsevier: Amsterdam, The Netherlands, 2017. [Google Scholar]
- Summers, R.B. A new concept in maxillary implant surgery: The osteotome technique. Compendium 1994, 15, 152–154. [Google Scholar]
- Ihde, S.; Ihde, A. Introduction into the Work with the Strategic Implant; International Implant Foundation: Munich, Germany, 2015. [Google Scholar]
- Donath, K.; Laass, M.; Günzl, H.-J. The histopathology of different foreign-body reactions in oral soft tissue and bone tissue. Virchows Arch. A Pathol. Anat. Histopathol. 1992, 420, 131–137. [Google Scholar] [CrossRef]
- Trindade, R.; Albrektsson, T.; Tengvall, P.; Wennerberg, A. Foreign Body Reaction to Biomaterials: On Mechanisms for Buildup and Breakdown of Osseointegration. Clin. Implant Dent. Relat. Res. 2014, 18, 192–203. [Google Scholar] [CrossRef]
- Araújo, M.G.; Silva, C.; Misawa, M.; Sukekava, F. Alveolar socket healing: What can we learn? Periodontology 2000 2015, 68, 122–134. [Google Scholar] [CrossRef]
- Ducheyne, P.; Grainger, D.; Healy, K.; Hutmacher, D.W.; Kirkpatrick, C.J. Comprehensive Biomaterials II, 2nd ed.; Elsevier: Amsterdam, The Netherlands, 2017; Volume 2, pp. 452–470. [Google Scholar]
- Branemark, P.-I. Tissue-integrated prostheses. Quintessence 1985, 99–115. [Google Scholar]
- Resnik, R.R.; Misch, C.E. Bone Density: A Key Determinant for Treatment Planning. In Misch’s Contemporary Implant Dentistry, 4th ed.; Resnik, R.R., Ed.; Elsevier: St Louis, MO, USA, 2020; pp. 450–466. [Google Scholar]
- Chatvaratthana, K.; Thaworanunta, S.; Seriwatanachai, D.; Wongsirichat, N. Correlation between the thickness of the crestal and buccolingual cortical bone at varying depths and implant stability quotients. PLoS ONE 2017, 12, e0190293. [Google Scholar] [CrossRef] [Green Version]
- E Misch, C.; Qu, Z.; Bidez, M.W. Mechanical properties of trabecular bone in the human mandible: Implications for dental implant treatment planning and surgical placement. J. Oral Maxillofac. Surg. 1999, 57, 700–706. [Google Scholar] [CrossRef]
- Norton, M.R.; Gamble, C. Bone classification: An objective scale of bone density using the computerized tomography scan. Clin. Oral Implant. Res. 2001, 12, 79–84. [Google Scholar] [CrossRef] [PubMed]
- Kan, J.Y.K.; Roe, P.; Rungcharassaeng, K.; Patel, R.D.; Waki, T.; Lozada, J.L.; Zimmerman, G. Classification of sagittal root position in relation to the anterior maxillary osseous housing for immediate implant placement: A cone beam computed tomography study. Int. J. Oral Maxillofac. Implant. 2011, 26. [Google Scholar]
- Moy, P.K.; Medina, D.; Shetty, V.; Aghaloo, T.L. Dental implant failure rates and associated risk factors. Int. J. Oral Maxillofac. Implant. 2005, 20, 569–577. [Google Scholar]
- Iezzi, G.; Mangano, C.; Barone, A.; Tirone, F.; Baggi, L.; Tromba, G.; Piattelli, A.; Giuliani, A. Jawbone remodeling: A conceptual study based on Synchrotron High-resolution Tomography. Sci. Rep. 2020, 10, 1–12. [Google Scholar] [CrossRef] [Green Version]
- Greenstein, G.; Cavallaro, J. Implant Insertion Torque: Its Role in Achieving Primary Stability of Restorable Dental Implants. Compend. Contin. Educ. Dent. 2017, 38, 88–95. [Google Scholar]
- A Smith, R.; Berger, R.; Dodson, T.B. Risk factors associated with dental implants in healthy and medically compromised patients. Int. J. Oral Maxillofac. Implant. 1992, 7, 142–153. [Google Scholar]
- Braut, V.; Bornstein, M.M.; Lauber, R.; Buser, D. Bone dimensions in the posterior mandible: A retrospective radiographic study using cone beam computed tomography. Part 1—analysis of dentate sites. Int. J. Periodontics Restor. Dent. 2012, 32, 175. [Google Scholar] [CrossRef] [Green Version]
- Yang, H.-S.; Lang, L.A.; Felton, D.A. Finite element stress analysis on the effect of splinting in fixed partial dentures. J. Prosthet. Dent. 1999, 81, 721–728. [Google Scholar] [CrossRef]
- Liddelow, G.; Klineberg, I. Patient-related risk factors for implant therapy. A critique of pertinent literature. Aust. Dent. J. 2011, 56, 417–426. [Google Scholar] [CrossRef] [PubMed]
- Pałka, Ł.R.; Lazarov, A. Immediately loaded bicortical implants inserted in fresh extraction and healed sites in patients with and without a history of periodontal disease. Ann. Maxillofac. Surg. 2019, 9, 371–378. [Google Scholar] [CrossRef] [PubMed]
- Esposito, M.; Hirsch, J.-M.; Lekholm, U.; Thomsen, P. Biological factors contributing to failures of osseointegrated oral implants, (II). Etiopathogenesis. Eur. J. Oral Sci. 1998, 106, 721–764. [Google Scholar] [CrossRef]
- Winkler, S.; Morris, H.F.; Ochi, S. Implant Survival to 36 Months as Related to Length and Diameter. Ann. Periodontol. 2000, 5, 22–31. [Google Scholar] [CrossRef]
- Renouard, F.; Nisand, D. Impact of implant length and diameter on survival rates. Clin. Oral Implant. Res. 2006, 17, 35–51. [Google Scholar] [CrossRef]
- Draenert, F.G.; Sagheb, K.; Baumgardt, K.; Kämmerer, P.W. Retrospective analysis of survival rates and marginal bone loss on short implants in the mandible. Clin. Oral Implant. Res. 2011, 23, 1063–1069. [Google Scholar] [CrossRef]







| Implant Type | Follow-Up Period (in Month/Year) | No. of Implants with This Follow-Up | Cumulative No. of Failures | Cumulative Survival Rate |
|---|---|---|---|---|
| Compressive screw | 8 months | 1056 | 2 | 99.8% |
| 12 months/1 year | 1030 | 2 | 99.8% | |
| 18 months | 986 | 2 | 99.8% | |
| 21 months | 949 | 3 | 99.7% | |
| 24 months/2 years | 941 | 3 | 99.7% | |
| 36 months/3 years | 570 | 3 | 99.7% | |
| 48 months/4 years | 273 | 3 | 99.7% | |
| 52 months | 147 | 4 | 99.0% | |
| 58 months | 118 | 4 | 99.0% | |
| 60 months/5 years | 115 | 4 | 99.0% | |
| 72 months/6 years | 37 | 4 | 99.0% | |
| 82 months | 5 | 4 | 99.0% |
| Observed Parameter | n (%)/(X ± SD; (Med; Min-Max)) | |
|---|---|---|
| Number of patients | 151 | |
| Number of implants | 1057 | |
| Number of implants in full function | 1041 (98.5%) | |
| Age | 51.26 ± 17.33 (53; 21–91) | |
| Gender | Male/Female | 80 (53.0%)/71 (47.0%) |
| Hypertension | Yes/No | 49 (32.5%)/102 (67.5%) |
| Diabetes mellitus | Yes/No | 63 (41.7%)/89 (58.3%) |
| Smoker | Yes/No | 17 (11.3%)/134 (88.7%) |
| Available Bone | Survival Prediction | Best Position | ||
|---|---|---|---|---|
| Type I | >4 mm bone | Excellent | I, II, III |  |
| Type II | 2–4 mm bone | Good | II, III |  |
| Type III | 1–2 mm bone | Medium | I or bicortical implant advised |  |
| Type IV | <1 mm bone | Low | Bicortical implant advised |  |
| Observed Parameters | Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up | |
|---|---|---|---|---|
| Overall Survival Rate for all Implants | 99.0% | 99.0% | 99.0% | |
| Gender | Male | 100% | 100% | 100% |
| Female | 98.0% | 98.0% | 98.0% | |
| Significance | p = 0.027 * | p = 0.027 * | p = 0.027 * | |
| Hypertension | Yes | 100% | 100% | 100% |
| No | 98.1% | 98.1% | 98.1% | |
| Significance | p = 0.051 | p = 0.051 | p = 0.051 | |
| Diabetes mellitus | Yes | 100% | 100% | 100% |
| No | 97.7% | 97.7% | 97.7% | |
| Significance | p = 0.018 * | p = 0.007 * | p = 0.007 * | |
| Smoker | Yes/No | 100% | 100% | 100% |
| No | 98.9% | 98.9% | 98.9% | |
| Significance | p = 0.374 | p = 0.374 | p = 0.374 | |
| Implant Length (mm) | Frequency (% of All Implants) | Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up |
|---|---|---|---|---|
| 10 | 114 (10.8%) | 98.1% | 98.1% | 98.1% |
| 12 | 482 (45.6%) | 98.2% | 98.2% | 98.2% |
| 15 | 461 (43.6%) | 100% | 100% | 100% |
| Significance | p = 0.006 * | p = 0.006 * | p = 0.006 * | |
| Implant Diameter | Frequency (% of All Implants) | Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up |
|---|---|---|---|---|
| 3.2 mm | 59 (5.6%) | 96.6% | 99.4% | 99.4% |
| 3.0 mm | 6 (0.6%) | 100% | 100% | 100% |
| 3.7 mm | 606 (57.3%) | 98.8% | 100% | 100% |
| 4.1 mm | 386 (36.5%) | 100% | 100.0% | 100.0% |
| Significance | p = 0.033 * | p = 0.033 * | p = 0.033 * | |
| Observed Parameters | Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up | |
|---|---|---|---|---|
| Bone Loss | No | 99.3% | 99.3% | 99.3% |
| General Vertical | 66.7% | 66.7% | 66.7% | |
| Crater-like | 60.0% | 60.0% | 60.0% | |
| Significance | p < 0.000 * | p < 0.000 * | p < 0.000 * | |
| Place of Insertion | Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up |
|---|---|---|---|
| Floor of the nose | 100% | 100% | 100% |
| Sinus floor | 100% | 100% | 100% |
| Tuber pterygoid | 100% | 100% | 100% |
| Interforaminal | 100% | 100% | 100% |
| Distal mandible w/o cortical | 97.3% | 97.3% | 97.3% |
| Cortical distal mandible | 100% | 100% | 100% |
| Buccal nerve bypass | 100% | 100% | 100% |
| Significance | p = 0.237 | p = 0.237 | p = 0.237 |
| Radiological Follow-Up | Clinical Inspection as Follow-Up | Patient Report as Follow-Up | ||
|---|---|---|---|---|
| Prosthetic construction type | Full bridge upper | 100% | 100% | 100% |
| Full bridge lower | 100% | 100% | 100% | |
| Segment upper | 100% | 100% | 100% | |
| Segment lower | 95.7% | 95.7% | 95.7% | |
| Single tooth | 100% | 100% | 100% | |
| Single tooth (several implants) | 96.2% | 96.2% | 96.2% | |
| Overdenture | 100% | 100% | 100% | |
| Significance | p = 0.007 * | p = 0.007 * | p = 0.007 * | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jani, M.; Gaur, V.; Doshi, A.G.; Patel, K.; Pałka, Ł. Clinically Based Classification and Positioning Indication for Single-Piece Compressive Implants Placement in Regard to Extraction Socket. Healthcare 2022, 10, 598. https://doi.org/10.3390/healthcare10040598
Jani M, Gaur V, Doshi AG, Patel K, Pałka Ł. Clinically Based Classification and Positioning Indication for Single-Piece Compressive Implants Placement in Regard to Extraction Socket. Healthcare. 2022; 10(4):598. https://doi.org/10.3390/healthcare10040598
Chicago/Turabian StyleJani, Mmehul, Vivek Gaur, Anita Gala Doshi, Kiran Patel, and Łukasz Pałka. 2022. "Clinically Based Classification and Positioning Indication for Single-Piece Compressive Implants Placement in Regard to Extraction Socket" Healthcare 10, no. 4: 598. https://doi.org/10.3390/healthcare10040598






