1. Introduction
COVID-19 (Coronavirus Disease 2019) was announced by World Health Organization (WHO) as a global pandemic, and infections continue to increase around the globe. It first originated in Wuhan, China, in November 2019 and spread across the world at a rapid rate. Some of the common strategies as advised by WHO in slowing the rate of the infection included preventive measures such as the limitation of movement in the infected area, interruption of human–human transmission using social distancing, early identification and isolation, and providing appropriate care for patients. During this pandemic period, information regarding the virus spread faster and more extensively compared to the SARS outbreak in 2003 due to modernization and globalization. This may have resulted in increased public fear, panic, anxiety, and stress, especially in people who are more susceptible to psychological distress [
1].
The virus has caused a certain vulnerable population to have higher rates of morbidity and mortality; for example, substance use disorder patients and people who use drugs [
1]. It also has made proper rehabilitation, diagnosis, and treatment of patients with substance use disorder difficult [
2]. This may be due to the responses towards the pandemic, including movement restriction orders, total lockdowns, and quarantine [
3]. In addition to these responses, the COVID-19 period has negatively affected people, especially those with prior psychological problems, and has resulted in maladaptive behavior, psychological distress, and poor coping mechanisms. Looking back at history, during the time of SARS (Severe Acute Respiratory Syndrome), a study conducted in Beijing, China on the psychological impacts of the outbreak/epidemic/pandemic period shows that around 40% of those studied suffered from post-traumatic stress disorder, even 3 years after the outbreak [
4]. The association between adverse life events such as an outbreak and the brain stress system plays a leading role in addiction. People who use drugs (PWUD) are much more vulnerable to stress, which may cause relapse among existing or previous drug users [
1].
A study in China from January to February 2020 indicates that about 54% of respondents rated the psychological impact of COVID-19 as moderate to severe, which may impact the pattern of substance usage of people who already used substances before the pandemic period [
5]. Based on public and health provider observation, there is informal evidence that there were changes in patterns and behavior of people who use drugs during this pandemic period as a result of the government responses towards the escalation of COVID-19 [
3].
The lockdowns, isolation, and restriction of movement implemented by governments around the globe may cause an increase in substance use due to feeling distressed and anxious, as reported by a previous study during the SARS outbreak [
6], or drug users may use this time to free themselves from the substance as it may be difficult for them to access their respective substances.
From multiple studies’ perspectives, there are many psychosocial factors contributing to substance and alcohol use relapses among users, including low self-efficacy, attitude, poor knowledge of drug abuse, poor family and social support, peer pressure, unemployment, as well as lack of well-established drug rehabilitation centers [
7]. These could be some of the confounding factors that are associated with a change in the patterns of substance abuse or relapse. However, the limitation of these studies is the lack of attention to the individual characteristics or mental well-being that may exacerbate the possibility of relapse in individuals who use substances.
Other consequences of COVID-19 were the devastating economic effects, which resulted in income and employment losses for millions of people around the globe. The direct and indirect outcome of this was the emergence and increase of both psychological symptoms and disorders, including stress, anxiety, depression, substance use/abuse, and many others. Moreover, COVID-19 as well as other pandemics are postulated to hinder substance use disorder treatment, causing probable growth in withdrawal symptoms and relapses among substance users worldwide [
8]. According to the Anxiety and Depression Association of America, 20% of Americans who have an anxiety or depressive disorder also have a substance use disorder, and 20% of those who have a substance use disorder also have an anxiety or depressive disorder. Substance users may also increase or change their patterns of substance use as a coping mechanism due to COVID-related worry or anxiety [
8].
Furthermore, the increased overdose mortality and morbidity due to substance use resulting from possible psychological implications of COVID-19 itself e.g. social distancing, isolation or quarantine would cause a further increase in the risk of respiratory distress and lung disease which complicates the COVID-19 cases among substance users [
9]. Some of the COVID-19 complications such as acute respiratory distress syndrome (ARDS), renal failure, and death were increased in people who uses substances, particularly those using alcohol and drugs such as opioids, benzodiazepines, and methamphetamines which damage the lungs and impaired the respiratory system [
10].
As for the Malaysian setting, to date (13 April 2022), there have been (4,342,559) positive COVID-19 cases reported nationwide, with (35,341) people dying due to the virus. It has been observed that the pandemic period has affected people psychologically, especially those in contact with or contracting the virus. There are ongoing studies regarding the mental health effects of the COVID-19 pandemic in Malaysia as well as substance use patterns among Malaysians who uses substances. Currently, there is limited data regarding the number of substance user relapses or changes of patterns during the pandemic period. Hence, it is important to identify these changes among substance/drug users to initiate proper management plans and rehabilitation at the University Malaya Medical Centre (UMMC) setting during this global pandemic or any prolonged containment in the future.
In this study, we aim to study the effects of the COVID-19 pandemic on patterns of substance usage among people who use drugs (PWUD) at the University Malaya Medical Centre (UMMC). Specifically, we looked at the association of isolation status, anxiety, and depression on the pattern of substance use during the pandemic as well as the different coping mechanisms used.
4. Discussion
The COVID-19 pandemic has had devastating effects on the world in terms of physical and mental health, the economy, and many other elements. The world was basically ‘halted’ during the pandemic era, which affected different populations in many ways. [
17]. Some of the populations, such as people who use substances, are much more vulnerable and at risk of contracting the disease compared to other populations. The negative impacts of the restrictions and pandemic response measures toward people who use drugs (PWUD) were devastating. Due to the reduction of drug supply and production worldwide, many dealers reduced the purity of the substances and increased the cost, which could result in poisoning, drug withdrawal, serious health problems, and increased risk of overdose [
18]. Based on a recent study by the Centers for Disease Control and Prevention, there has been a 13% increase in substance use among the American population in recent years [
19]. In addition, about 31% of adults in the United States suffer from anxiety or depression; at least 26% suffer from stress-related disorder symptoms and 11% have strong suicidal ideation [
20], which also notable from the study done by SAMHSA [
21].
Looking at the types of substances used before COVID-19, most of the respondents of this study used multiple substances (42.3%), followed by heroin and other types of substances. This prevalence was comparable to other studies, where multiple substance use was reported in 45.8% of participants who meet the criteria for substance use disorder [
22].
For the general pattern of illicit substance/alcohol usage during COVID-19 restrictions, most of the respondents did not use or stopped taking the illicit substance/alcohol during the COVID-19 restriction period, followed by increased and decreased usage. These were similar results to other similar studies, which reported most of their web survey respondents declared using the same amount (21.3%) and increased usage of substances (21.2%). However, the same study also reported different percentages of people who decreased or stopped their usage. These findings might suggest some of the users were adapting their usage to a new restrictive environment due to the pandemic itself, although this is not applicable to the whole population [
23].
In this study, we also looked at the pattern of use for the specific substances most commonly used by our respondents. The four most common substances were heroin, alcohol, amphetamine-type stimulants, and cannabis. For heroin use, we can see most of the users stopped their usage during the COVID-19 pandemic period (20.8%). Although these numbers and percentages were not comparable to other studies, the ratio and pattern for both categories are noted in a study from Luxemburg as well [
23]. The reason behind this is most likely the scarcity of heroin during the pandemic, due to border restrictions as well as confinement policies [
24].
For the pattern of alcohol use, most did not change their pattern of use (10%), followed closely by an increased intake of the same substance. This was in line with findings by various studies. For example, a study in Italy within a vulnerable group of substance users suggested that with COVID-19 and its restrictions, the shifting towards alcohol use and maintaining its use were inevitable during this pandemic times, as alcohol was one of the most readily available substances [
25]. Similarly, a study in Amsterdam of changing patterns of substance use during COVID-19 reported similar trends [
26].
The amphetamine-type stimulant (ATS) use pattern was also affected in some ways due to the COVID-19 pandemic. Most maintained their usage (13.8%) during this time, and 7.7% increased their usage. However, interestingly, among all other substances, 1.5% of respondents started using ATS during the COVID-19 pandemic. This was in line with other similar surveys done by the United Nations, which found that ATS and other synthetic drug users maintained usage; however, shifts occurred from traditional illicit drugs (that required illegal import) towards synthetic drugs, especially ATS, due to the availability of this kind of drug not being affected by the COVID-19 pandemic [
27].
Some changes were also noted in the pattern of cannabis use during this pandemic era. In this study, 13.8% of respondents reported they had stopped their usage during the COVID-19 pandemic, which is most of the users. This result was comparable to another study in Amsterdam, where around 16.3% of users stopped using cannabis during the COVID-19 period. However, the discontinuation of cannabis was less common compared to other drugs [
28]. A study done in Canada among cannabis users found that around half of the users increased their usage, which contradicts our findings. This might be a result of the availability of cannabis in Canada, where the legality of cannabis is much more accepted as compared to Malaysia [
29].
As the COVID-19 pandemic hit the world, it caused a major stir in the drug market around the globe, especially in the countries that were most affected by the outbreak, including Malaysia. The stirs in the drug market due to restrictions and COVID-19 itself caused changes in purity, price, as well as the amounts of illicit substances/alcohol obtained since the outbreak of COVID-19. Most of the respondents found that the purity of substances generally decreased since the COVID-19 outbreak (36.2%). In terms of the price of the substances obtained, most of the users found it to be the same (40%), although the purity was lower. As for the general amount of substances obtained at the same price, the majority (44.6%) reported it to be the same amount as the pre-pandemic period. These results were noted to be different from other parts of the world, for example, Luxemburg, where most of the respondents to a web survey reported that the purity of the substances was the same (32.4%) but the price was higher (26.2%) and the quantity was the same (30.5%). This shows the drug market in this country adapted quickly during the COVID-19 pandemic period; the same pattern can be observed in other parts of Europe, for example, Switzerland [
22]. This also was noted in Southeast Asia, where the drug market, especially methamphetamines, was not greatly affected, resulting in little change in price; however, the purity of the substances was affected, especially in the initial part of the pandemic, due to availability and mobility restrictions [
27].
The depression and anxiety symptoms among people who use drugs/alcohol were also noted to be prevalent in this study. These were comparable to other studies, which also indicate a prevalence of anxiety and depression of around 41.1% within the community [
30]. A study published by Czeisler et al. also suggested that anxiety and depression are prevalent among substance users, reported at around 42% [
19].
As for the coping skills and strategies, most of the respondents adapted dysfunctional coping strategies, followed closely by emotion-focused and problem-focused coping strategies. As in other studies, most substance users used some sort of pathological way of coping, specifically dysfunctional coping [
31]. Poor emotional regulation is one of the main causes of dysfunctional coping among substance users, and this association works bidirectionally [
32].
Based on this study, there was no significant association between sociodemographic status and change in pattern of substance use. However, the association was prominent and even significant between sociodemographic data and increase in substance use during the COVID-19 pandemic period. There was a significant association between the age of the respondents and an increase in substance use, with a
p-value of 0.04 (<0.05) in the bivariate analysis. According to a study by the National Institute of Drug Abuse in 2020, there is a significant association between age and increased substance use among substance users [
33]. Substance use is also prevalent for users aged around 35 years and above, partly due to adulthood roles, previous use, and experiences with advancing age [
34].
However, in our multivariate analysis, advancing age was protective against the increase in alcohol/illicit substance usage among PWUD in the UMMC. A postulated hypothesis for this is, as the substance users grow older, they may develop a sense of guilt as well as multiple medical issues that may prohibit and prevent them from increasing their substance usage. The prevalence of substance users among older adults is also quite low compared to the previous generation, according to several studies [
35]. However, several risk factors may increase the likelihood of them increasing or maintaining use in older age, such as comorbid mental health disorders, coping styles, and social factors [
35].
Another notable sociodemographic factor associated with the increased usage of substances is isolation status, which was associated with a three-fold increased risk of increasing substance use during this COVID-19 pandemic period. There are significant data to support this association; a study involving US national data suggests a strong association between isolation during COVID-19 and prevalence or increase in substance use [
36]. Isolation and solitary confinement during the pandemic also affected people who use drugs/alcohol, which then further changes their substance use pattern, specifically, increasing their usage [
37].
This study found that there is a significant association between depression status and the increase in illicit substance/alcohol use during the COVID-19 pandemic period/restrictions but not with anxiety. Around 25% of people with alcohol addiction and 50% of people with substance addiction in the United States have co-morbid depression. Anxiety disorders can be identified in around 25% of cases of alcohol dependence and 43% of cases of drug dependence. Alcohol dependency may be accompanied by co-morbid mental illnesses, such as severe anxiety or depression, which can have a poor influence on the quality of life, functioning, and ability to react to treatment [
38].
For the association between coping strategies and the change of pattern and increase substance usage, interestingly, our study found there was no significant associations. Although there are many studies suggesting that there is an association between dysfunctional coping mechanisms and an increase in substance/alcohol use, other studies found one-sixth of individuals (17.4%) used at least one substance to cope with stress regularly, showing the prevalence of substance-use coping in middle-aged and older persons. However, there was no link between frequent alcohol-use coping and self-rated health, which was in line with earlier research by Lin et al. [
39].
In this study, we found there was a significant correlation between coping skills, particularly problem-focused coping, with anxiety and depression status among people who used drugs/alcohol (PWUD) in the UMMC. Other studies have shown that denial, behavioral disengagement, self-blame, self-distraction, drug use, acceptance, positive reframing, active coping, and seeking emotional support were all found to be strongly linked to anxiety, concerns, and sadness. The study showed regulating stressful emotions (emotion-focused coping strategies such as passive and active avoidance, escaping, seeking social support, and positively reappraising the stressor) and managing the problem that is causing the distress are two widely recognized major functions of coping (problem-focused coping strategies such as planning how to change the stressor, seeking practical or informational support, and confronting the stressful situation). Problem-focused coping strategies have been linked to improved adjustment, while emotion-focused strategies have been linked to poor adjustment [
40]. This is similar to the findings in our study, which showed emotion-focused strategies linked with more depressive states and vice versa.
Specifically, the association between the dysfunctional coping strategies and no change in illicit substance/alcohol usage was noted to be significant in our findings. This shows that people who used substances with dysfunctional coping mechanisms tended to continue their usage patterns, especially during the COVID-19 pandemic period. The people who use dysfunctional coping mechanisms tend to not change their usage patterns. As mentioned earlier, some PWUD reduced or even stopped their usage due to multiple reasons, including coping with the pandemic situation and difficulties in obtaining certain substances. However, people that exhibited dysfunctional coping continued their usage despite many restrictions imposed by government policies. The severity of drug abuse was not found to be related to coping style. Furthermore, based on a study by Ingmar et al., after three months of inpatient substance misuse treatment, maladaptive coping methods declined, while more adaptive coping styles remained steady for another three months [
41].
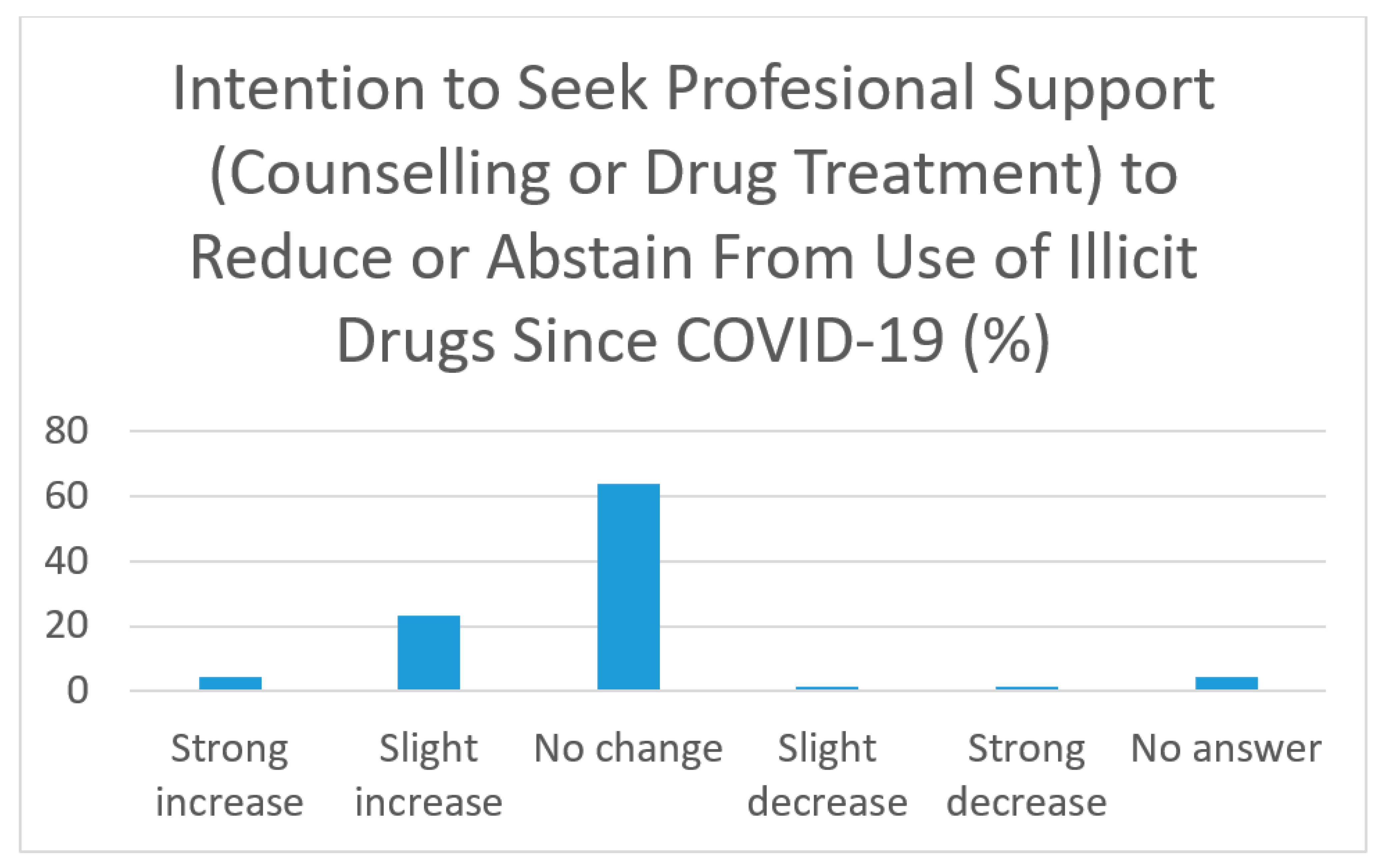
It was also noted that the intention to seek professional help and support for drug treatment/counselling was associated with a reduction in substance usage itself during the COVID-19 pandemic. This was in line with other studies that suggested motivation-boosting tactics and strategies can promote substance users’ treatment participation and retention, as well as good treatment outcomes such as decreased alcohol and drug use, a higher abstinence rate, and successful referral to treatment [
42]. The Transtheoretical Model is the most commonly used model for operationalizing patient motivation to change in drug use therapy. This Stages of Change model depicts categories that patients tend to fall into when making significant changes in their lives, such as entering treatment, and it can be viewed as a continuum along which an individual can move toward long-term or permanent change, such as reducing or even stopping substance use [
43].
There are several limitations that should be highlighted in this study. The main limitation of this study was that it used a cross-sectional study design in which the study of causality or causal relationship between the studied factor may not be determined accurately. The other possible limitation includes errors of representation, specifically coverage errors. Coverage errors are usually caused by using a survey sampling frame that does not include all members of the population being researched, or alternatively, by using methods that do not provide all members of the population some chance of being sampled. This risk of falling into a prospective sample frame is linked to drug use behaviors in some situations; substance use research may be particularly sensitive to coverage error [
44]. In the case of our study, most of the sample was from the UMMC addiction/substance psychiatry clinic and most were heroin users who came for methadone replacement therapy. Due to this factor, the studied population may not be as heterogenous as it should be, which affects certain aspects of the study results. This is also because the sampling method use was non-probability, convenient sampling. However, many other substance-related studies have used this method as a sampling technique. When research questions focus on certain populations thought to be at higher risk for substance use and misuse, non-probability samples are typically used. There are many well-known non-probability, or convenience sample designs that are frequently employed in practice [
44].