Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador
Abstract
:1. Introduction
2. Materials and Methods
2.1. Sample Collection
2.2. Evaluation of Acceptability
2.3. Data Analysis
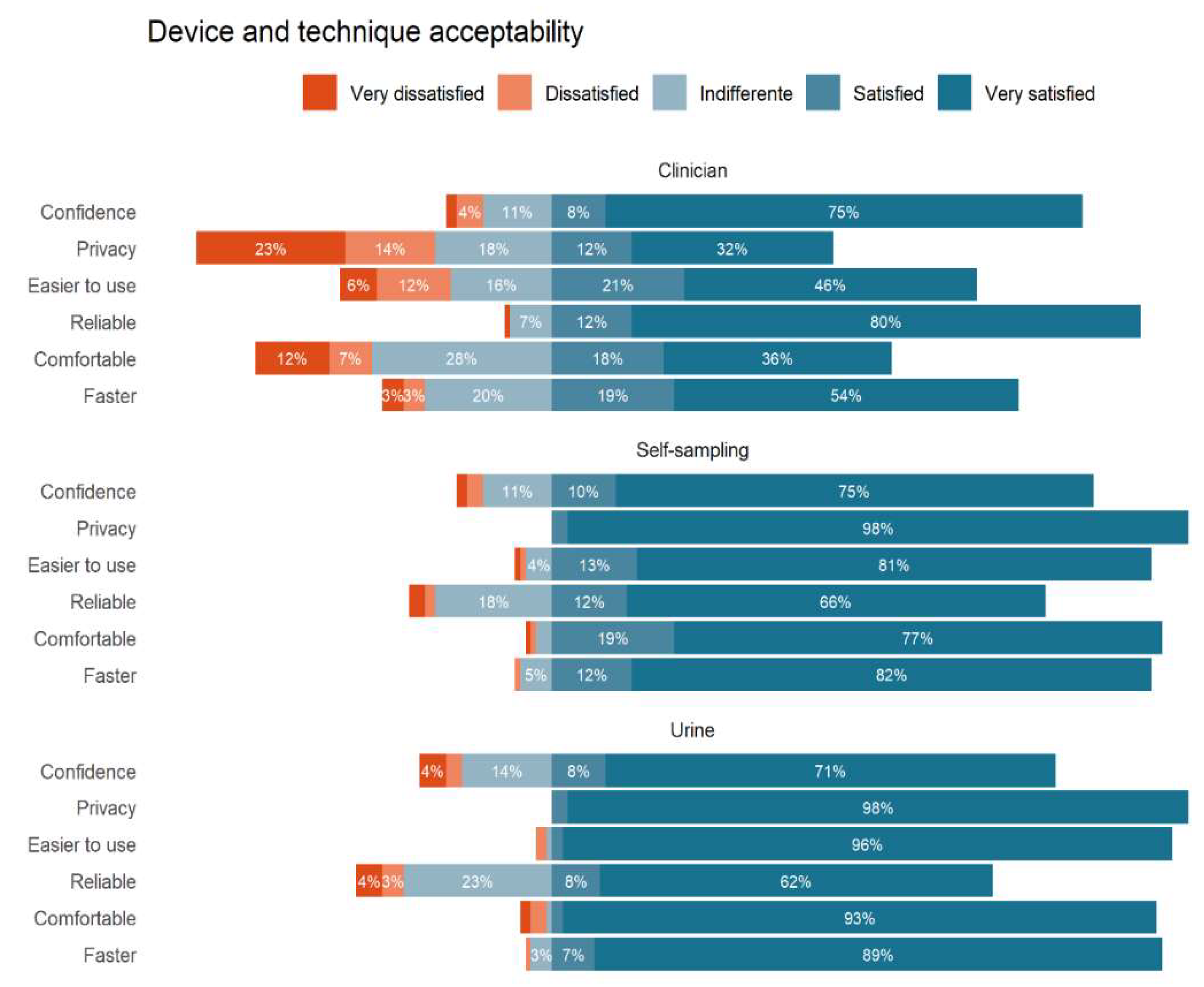
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CC | Cervical cancer |
| CAMIE | (Cáncer Auto Muestreo Igualdad Empoderamiento) Cancer Self Sampling Equity Empowerment |
| DIS | National Directory of Intelligence in Health |
| VIUC | (Dirección de investigación de la Universidad de Cuenca) Vice Rectorate of Research of the University of Cuenca |
| HPV | Human papillomavirus |
| UC-COBIAS | (University de Cuenca Comité de Bioética de las áreas de la Salud) University of Cuenca Comitee of Bioethics of Health Science Areas |
| VLIR-UOS | Vlaamse Interuniversitaire Raad Universitaire Ontwikkelingssamenwerking (Flemish Interuniversities Council University Development Co-Operation) |
| WHO | World Health Organization |
References
- Zhang, S.; Xu, H.; Zhang, L.; Qiao, Y. Cervical cancer: Epidemiology, risk factors and screening. Chin. J. Cancer Res. 2020, 32, 720–728. [Google Scholar] [CrossRef]
- Jit, M.; Prem, K.; Benard, E.; Brisson, M. From cervical cancer elimination to eradication of vaccine-type human papillomavirus: Feasibility, public health strategies and cost-effectiveness. Prev. Med. 2021, 144, 106354. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Strategy to Accelerate the Elimination of Cervical Cancer as a Public Health Problem; World Health Organization: Geneva, Switzerland, 2020; ISBN 978-92-4-001410-7. [Google Scholar]
- Hall, M.T.; Simms, K.T.; Lew, J.-B.; Smith, M.A.; Saville, M.; Canfell, K. Projected future impact of HPV vaccination and primary HPV screening on cervical cancer rates from 2017–2035: Example from Australia. PLoS ONE 2018, 13, e0185332. [Google Scholar] [CrossRef] [PubMed]
- Kang, M.; Ha, S.Y.; Cho, H.Y.; Chung, D.H.; Kim, N.R.; An, J.; Lee, S.; Seok, J.Y.; Jeong, J. Comparison of papanicolaou smear and human papillomavirus (HPV) test as cervical screening tools: Can we rely on HPV test alone as a screening method? An 11-year retrospective experience at a single institution. J. Pathol. Transl. Med. 2020, 54, 112–118. [Google Scholar] [CrossRef] [PubMed]
- Koliopoulos, G.; Nyaga, V.N.; Santesso, N.; Bryant, A.; Martin-Hirsch, P.P.; Mustafa, R.A.; Schünemann, H.; Paraskevaidis, E.; Arbyn, M. Cytology versus HPV testing for cervical cancer screening in the general population. Available online: http//doi.wiley.com/10.1002/14651858.CD008587.pub2 (accessed on 1 March 2019).
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef]
- Canfell, K.; Kim, J.J.; Brisson, M.; Keane, A.; Simms, K.T.; Caruana, M.; Burger, E.A.; Martin, D.; Nguyen, D.T.N.; Bénard, É.; et al. Mortality impact of achieving WHO cervical cancer elimination targets: A comparative modelling analysis in 78 low-income and lower-middle-income countries. Lancet 2020, 395, 591–603. [Google Scholar] [CrossRef]
- Bruni, L.; Albero, G.; Serrano, B.; Mena, M.; Gómez, D.; Muñoz, J.; Bosch, F.X.; de Sanjosé, S. Human Papillomavirus and Related Diseases Report Ecuador; HPV Information Centre: Lyon, France, 2019. [Google Scholar]
- Vale, D.B.; Teixeira, J.C.; Bragança, J.F.; Derchain, S.; Sarian, L.O.; Zeferino, L.C. Elimination of cervical cancer in low- and middle-income countries: Inequality of access and fragile healthcare systems. Int. J. Gynecol. Obstet. 2021, 152, 7–11. [Google Scholar] [CrossRef]
- Instituto Nacional de Estadísticas y Censos. Encuesta Nacional de Salud y Nutrición 2018; INEC: Quito, Ecudor, 2018. [Google Scholar]
- Agurto, I.; Bishop, A.; Sánchez, G.; Betancourt, Z.; Robles, S. Perceived barriers and benefits to cervical cancer screening in Latin America. Prev. Med. 2004, 39, 91–98. [Google Scholar] [CrossRef]
- Austad, K.; Chary, A.; Xocop, S.M.; Messmer, S.; King, N.; Carlson, L.; Rohloff, P. Barriers to Cervical Cancer Screening and the Cervical Cancer Care Continuum in Rural Guatemala: A Mixed-Method Analysis. J. Glob. Oncol. 2018, 4, 1–10. [Google Scholar] [CrossRef]
- Godoy, Y.; Godoy, C.; Reyes, J. Social Representations of Gynecologic Cancer Screening Assessment a Qualitative research on Ecuadorian women. Rev. Esc. Enferm. USP 2016, 50, 68–73. [Google Scholar] [CrossRef] [Green Version]
- Black, E.; Hyslop, F.; Richmond, R. Barriers and facilitators to uptake of cervical cancer screening among women in Uganda: A systematic review. BMC Womens Health 2019, 19, 108. [Google Scholar] [CrossRef] [PubMed]
- Rohner, E.; McGuire, F.H.; Liu, Y.; Li, Q.; Miele, K.; Desai, S.A.; Schmitt, J.W.; Knittel, A.; Nelson, J.A.E.; Edelman, C.; et al. Racial and Ethnic Differences in Acceptability of Urine and Cervico-Vaginal Sample Self-Collection for HPV-Based Cervical Cancer Screening. J. Womens Health 2020, 29, 971–979. [Google Scholar] [CrossRef] [PubMed]
- Shin, H.Y.; Lee, B.; Hwang, S.-H.; Lee, D.O.; Sung, N.Y.; Park, J.Y.; Jun, J.K. Evaluation of satisfaction with three different cervical cancer screening modalities: Clinician-collected Pap test vs. HPV test by self-sampling vs. HPV test by urine sampling. J. Gynecol. Oncol. 2019, 30, e76. [Google Scholar] [CrossRef] [PubMed]
- Nelson, E.J.; Maynard, B.R.; Loux, T.; Fatla, J.; Gordon, R.; Arnold, L.D. The acceptability of self-sampled screening for HPV DNA: A systematic review and meta-analysis. Sex. Transm. Infect. 2017, 93, 56–61. [Google Scholar] [CrossRef]
- Schaafsma, M.; van den Helder, R.; Bleeker, M.C.G.; Rosier-van Dunné, F.; van der Avoort, I.A.M.; Steenbergen, R.D.M.; van Trommel, N.E. Experiences and preferences towards collecting a urine and cervicovaginal self-sample among women attending a colposcopy clinic. Prev. Med. Rep. 2022, 26, 101749. [Google Scholar] [CrossRef]
- Vega Crespo, B.; Neira, V.A.; Ortíz Segarra, J.; Rengel, R.M.; López, D.; Orellana, M.P.; Gómez, A.; Vicuña, M.J.; Mejía, J.; Benoy, I.; et al. Role of Self-Sampling for Cervical Cancer Screening: Diagnostic Test Properties of Three Tests for the Diagnosis of HPV in Rural Communities of Cuenca, Ecuador. Int. J. Environ. Res. Public. Health 2022, 19, 4619. [Google Scholar] [CrossRef]
- Wang, R.; Lee, K.; Gaydos, C.A.; Anderson, J.; Keller, J.; Coleman, J. Performance and acceptability of self-collected human papillomavirus testing among women living with HIV. Int. J. Infect. Dis. 2020, 99, 452–457. [Google Scholar] [CrossRef]
- Esber, A. Feasibility, validity and acceptability of self-collected samples for human papillomavirus (HPV) testing in rural Malawi. Malawi Med. J. 2018, 30, 61. [Google Scholar] [CrossRef]
- Kuriakose, S.; Sabeena, S.; Binesh, D.; Abdulmajeed, J.; Ravishankar, N.; Ramachandran, A.; Vijaykumar, B.; Ameen, N. Diagnostic accuracy of self-collected vaginal samples for HPV DNA detection in women from South India. Int. J. Gynecol. Obstet. 2020, 149, 219–224. [Google Scholar] [CrossRef]
- Cómbita, A.L.; Gheit, T.; González, P.; Puerto, D.; Murillo, R.H.; Montoya, L.; Vorsters, A.; Van Keer, S.; Van Damme, P.; Tommasino, M.; et al. Comparison between Urine and Cervical Samples for HPV DNA Detection and Typing in Young Women in Colombia. Cancer Prev. Res. 2016, 9, 766–771. [Google Scholar] [CrossRef] [Green Version]
- Madzima, T.R.; Vahabi, M.; Lofters, A. Emerging role of HPV self-sampling in cervical cancer screening for hard-to-reach women. Can. Fam. Physician 2017, 63, 597–601. [Google Scholar]
- Burton-Jeangros, C.; Fargnoli, V.; Petignat, P. To what extent will women accept HPV self-sampling for cervical cancer screening? A qualitative study conducted in Switzerland. Int. J. Womens Health 2015, 7, 883. [Google Scholar] [CrossRef]
- Pourette, D.; Cripps, A.; Guerrien, M.; Desprès, C.; Opigez, E.; Bardou, M.; Dumont, A. Assessing the Acceptability of Home-Based HPV Self-Sampling: A Qualitative Study on Cervical Cancer Screening Conducted in Reunion Island Prior to the RESISTE Trial. Cancers 2022, 14, 1380. [Google Scholar] [CrossRef]
- Sullivan, G.M.; Artino, A.R. Analyzing and Interpreting Data From Likert-Type Scales. J. Grad. Med. Educ. 2013, 5, 541–542. [Google Scholar] [CrossRef]
- Sultana, F.; Mullins, R.; English, D.R.; Simpson, J.A.; Drennan, K.T.; Heley, S.; Wrede, C.D.; Brotherton, J.M.L.; Saville, M.; Gertig, D.M. Women’s experience with home-based self-sampling for human papillomavirus testing. BMC Cancer 2015, 15, 849. [Google Scholar] [CrossRef]
- Cadman, L.; Reuter, C.; Jitlal, M.; Kleeman, M.; Austin, J.; Hollingworth, T.; Parberry, A.L.; Ashdown-Barr, L.; Patel, D.; Nedjai, B.; et al. A Randomized Comparison of Different Vaginal Self-sampling Devices and Urine for Human Papillomavirus Testing—Predictors 5.1. Cancer Epidemiol. Biomark. Prev. 2021, 30, 661–668. [Google Scholar] [CrossRef]
- Drysdale, H.; Marlow, L.A.; Lim, A.; Sasieni, P.; Waller, J. Self-sampling for cervical screening offered at the point of invitation: A cross-sectional study of preferences in England. J. Med. Screen. 2022, 29, 096914132210922. [Google Scholar] [CrossRef]
- Tchounwou, P. Environmental Research and Public Health. Int. J. Environ. Res. Public Health 2004, 1, 1–2. [Google Scholar] [CrossRef]
- Le, D.; Coriolan Ciceron, A.; Jeon, M.J.; Gonzalez, L.I.; Jordan, J.A.; Bordon, J.; Long, B. Cervical Cancer Prevention and High-Risk HPV Self-Sampling Awareness and Acceptability among Women Living with HIV: A Qualitative Investigation from the Patients’ and Providers’ Perspectives. Curr. Oncol. 2022, 29, 516–533. [Google Scholar] [CrossRef]
- De Pauw, H.; Donders, G.; Weyers, S.; De Sutter, P.; Doyen, J.; Tjalma, W.A.A.; Vanden Broeck, D.; Peeters, E.; Van Keer, S.; Vorsters, A.; et al. Cervical cancer screening using HPV tests on self-samples: Attitudes and preferences of women participating in the VALHUDES study. Arch. Public Health 2021, 79, 155. [Google Scholar] [CrossRef]
- Rawat, A.; Sanders, C.; Mithani, N.; Amuge, C.; Pedersen, H.; Namugosa, R.; Payne, B.; Mitchell-Foster, S.; Orem, J.; Ogilvie, G.; et al. Acceptability and preferences for self-collected screening for cervical cancer within health systems in rural Uganda: A mixed-methods approach. Int. J. Gynecol. Obstet. 2021, 152, 103–111. [Google Scholar] [CrossRef] [PubMed]
- Miller, M.J.; Xu, L.; Qin, J.; Hahn, E.E.; Ngo-Metzger, Q.; Mittman, B.; Tewari, D.; Hodeib, M.; Wride, P.; Saraiya, M.; et al. Impact of COVID-19 on Cervical Cancer Screening Rates Among Women Aged 21–65 Years in a Large Integrated Health Care System—Southern California, January 1–September 30, 2019, and January 1–September 30, 2020. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 109–113. [Google Scholar] [CrossRef] [PubMed]
- Lim, A.W.W. Will COVID-19 Be the Tipping Point for Primary HPV Self-sampling? Cancer Epidemiol. Biomark. Prev. 2021, 30, 245–247. [Google Scholar] [CrossRef] [PubMed]


| Variable | N (%) | |
|---|---|---|
| Age | Age median: 35; mode: 24; and SD ± 11.23 | |
| <35 years | 60 (50%) | |
| >35 years | 60 (50%) | |
| Level of instruction | ||
| None or primary | 65 (54.17%) | |
| Secondary or superior | 55 (45.83%) | |
| Civil status | ||
| Married or stable union | 77 (64.17%) | |
| Divorced, widow | 18 (15%) | |
| Single | 25 (20.83%) | |
| Familyincome per month | ||
| <USD 100 | 22 (18.33%) | |
| USD 101 to 200 | 44 (36.67%) | |
| USD 201 to 400 | 19 (15.83%) | |
| >USD 400 | 35 (29.17%) | |
| Occupation | ||
| Housewife | 69 (57.5%) | |
| Merchant | 13 (10.83%) | |
| Employed | 27 (22.5%) | |
| Others | 11 (9.17%) | |
| Currently working | ||
| Yes | 45 (37.5%) | |
| No | 75 (62.5%) | |
| Number of Pap tests during lifetime | Median: 5.24; mode: 3; minimum: 0; maximum: 3; and SD ± 11.23 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vega Crespo, B.; Neira, V.A.; Ortíz S, J.; Maldonado-Rengel, R.; López, D.; Gómez, A.; Vicuña, M.J.; Mejía, J.; Benoy, I.; Carreño, T.P.; et al. Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador. Healthcare 2022, 10, 1614. https://doi.org/10.3390/healthcare10091614
Vega Crespo B, Neira VA, Ortíz S J, Maldonado-Rengel R, López D, Gómez A, Vicuña MJ, Mejía J, Benoy I, Carreño TP, et al. Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador. Healthcare. 2022; 10(9):1614. https://doi.org/10.3390/healthcare10091614
Chicago/Turabian StyleVega Crespo, Bernardo, Vivian Alejandra Neira, José Ortíz S, Ruth Maldonado-Rengel, Diana López, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, and et al. 2022. "Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador" Healthcare 10, no. 9: 1614. https://doi.org/10.3390/healthcare10091614








