Abstract
Cancer is a leading cause of mortality and morbidity all over the world and the second major cause of death in Portugal. Dermatological side effects resulting from cancer treatment have a psychosocial impact on patients’ lives, such as quality of life (QoL), body image, cognitive fusion and social inhibition. This systematic review aimed to explore and synthesize the psychosocial impact of dermatological side effects of cancer treatment, answering the following research objectives: (i) Do the dermatological side effects of the cancer treatment present any psychosocial impact for the patients? (ii) How does the psychosocial impact of the dermatological toxicities of the cancer treatment manifest in patients’ lives? Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were followed and guided a systematic search through the PubMed, Cochrane Library and PyscNet databases. The considered studies correlate dermatological side effects of cancer treatments and their psychological/psychosocial outcomes. The studies found were all published in peer-reviewed journals. The results obtained established that cancer treatment causes the most varied skin changes, consequently reducing self-esteem and QoL; disturbing body image; and contributing to cases of stress, depression and anxiety. There is still limited literature that profoundly investigates the experience of living with these skin toxicities. The development of research lines to improve knowledge in this field will allow for significant improvements in healthcare for patients undergoing cancer treatment who need to focus more on the psychosocial implications of skin toxicities. The novelty of this review lies in adding knowledge summarizing the psychosocial implications of dermatological side effects of cancer treatment to support healthcare providers in the development of integrative therapeutic strategies for these patients in their clinical practice.
1. Introduction
Cancer continues to be a leading cause of mortality and morbidity worldwide [1]. Most of the existing oncological diseases are treated based on chemotherapy or radiotherapy alone or in combination with other treatments, with the side effects of these treatments being a clinical limitation of their administration. Health-related side effects induced by the cancer treatment may appear during or a long time after the treatment ends and often rely on the patient’s radiosensitivity [2]. The patient receiving cancer treatment usually has severe side effects such as pain, nausea, diarrhea, cardiotoxicity, depression of the immune system, hair loss, disruption of the cutaneous barrier, and changes in skin color and dryness [3,4,5,6]. This cutaneous toxicity could change the body image of the patient with significant psychosocial impact. Likewise, individuals suffering from skin diseases frequently encounter a situation characterized by physical disfigurement, psychological distress and societal stigma [7]. Dose reduction and discontinuation of treatment are not suitable options to avoid dermatological side effects since they can adversely affect cancer treatment outcomes [8].
The present review aims to synthesize and discuss the evidence from studies examining the psychosocial impact of dermatological effects resulting from cancer treatment and assess whether the psychological and emotional impact is integrated into the therapeutic strategies of the treatment of cancer patients. Thus, this review intends to answer the two following main research questions:
RQ1. Do the dermatological side effects of the cancer treatment present any psychosocial impact on the patients?
RQ2. How does the psychosocial impact of the dermatological toxicities of cancer treatment manifest in patients’ lives?
2. Background
Dermatological toxicity is assumed to be a common side effect caused by cancer treatment [9], which, if not properly managed, can become uncomfortable and disfiguring [6,10,11,12,13,14]. The symptoms usually appear around the second to the third week of cancer treatment [15], and although they are mild at first, they can become severe over time [16]. The impact of cancer on patients is multifaceted and has been documented in some studies [17,18]. The emotional consequences observed in people with cancer are depression, worry, fear, anger and guilt [19,20]. Furthermore, emotional distress is often referred to as the “sixth vital sign” for cancer patients, and healthcare professionals routinely evaluate it in conjunction with other vital signs like pulse, breathing, blood pressure, temperature and pain [21]. Besides the direct impacts, the connections between cancer and psychosocial consequences can also be influenced by the physical symptoms of cancer or the adverse effects of its treatment [22], such as nausea, vomiting and pain. This premise is supported by some studies that show that higher degrees of pain from cancer are related to a decrease in social activities, support and functioning [23]. Simultaneously, fatigue, which is a prevalent symptom among cancer patients, has been identified as a predictor of depression and anxiety [24]. Therefore, the impact of body image change due to the cutaneous toxicity of cancer treatment on the emotional and psychological components of the patient remains to be studied. Accordingly, this review could serve to identify gaps regarding the psychosocial impact of dermatological side effects resulting from cancer treatment and propose future studies and clinical practices to minimize this impact through clinical and psychological therapeutic management strategies. The authors present a discussion of the state of the art and reflections on future research needs.
3. Methods
3.1. Search Strategy
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guided a systematic search through the PubMed, Cochrane Library and PyscNet databases. The keywords used combined: “cancer” with “chemotherapy” or “treatment”, or “dermatological side effects” or “skin side effects” or “alopecia” or “body image” and “quality of life” or “psychosocial impact” or “social inhibition” or “cognitive fusion”. Some additional records were assessed through these articles’ references. The resulting studies were filtered. However, no time limit was imposed. All authors have been actively involved in all the other phases of the review process.
3.2. Inclusion Criteria
The studies’ titles and abstracts were assessed and screened for inclusion following specific criteria: (a) complete studies (no protocols); (b) studies correlating cancer and its psychological and psychosocial outcomes; (c) studies involving specific cancer treatments and their psychological and psychosocial outcomes; (d) studies assessing the psychological and psychosocial consequences of skin toxicities; and (e) studies published in peer-reviewed journals. The articles considered are in the English and French languages.
3.3. Exclusion Criteria
Studies were excluded if they only focused on cancer and its physical outcomes and not on its psychological or psychosocial impacts or if they focused only on the dermatological literature, not establishing an association with psychology. Studies that focused only on the impact of the family/loved ones/caregivers (as their perspective could be biased) were also excluded. Works that only mentioned pharmacological therapies and with a small sample size (<10 participants) were also excluded.
3.4. Screening
The title/abstract of the studies was selected independently by each of the authors, always based on the inclusion and exclusion criteria.
3.5. Quality Assessment
The studies’ methodological quality was assessed by its journal Q Index using Scimago Journal & Country Rank. Out of the seventeen selected articles, nine were in the top impactful 53% (Q1) [25,26,27,28,29,30,31,32,33], seven were in the less impactful 41% (Q2) [34,35,36,37,38,39,40], and one was in the lesser impactful 6% (Q3) [41]. To detail methodological issues and to make future investigation recommendations, studies lower than the ideal Q1 were still included.
4. Results
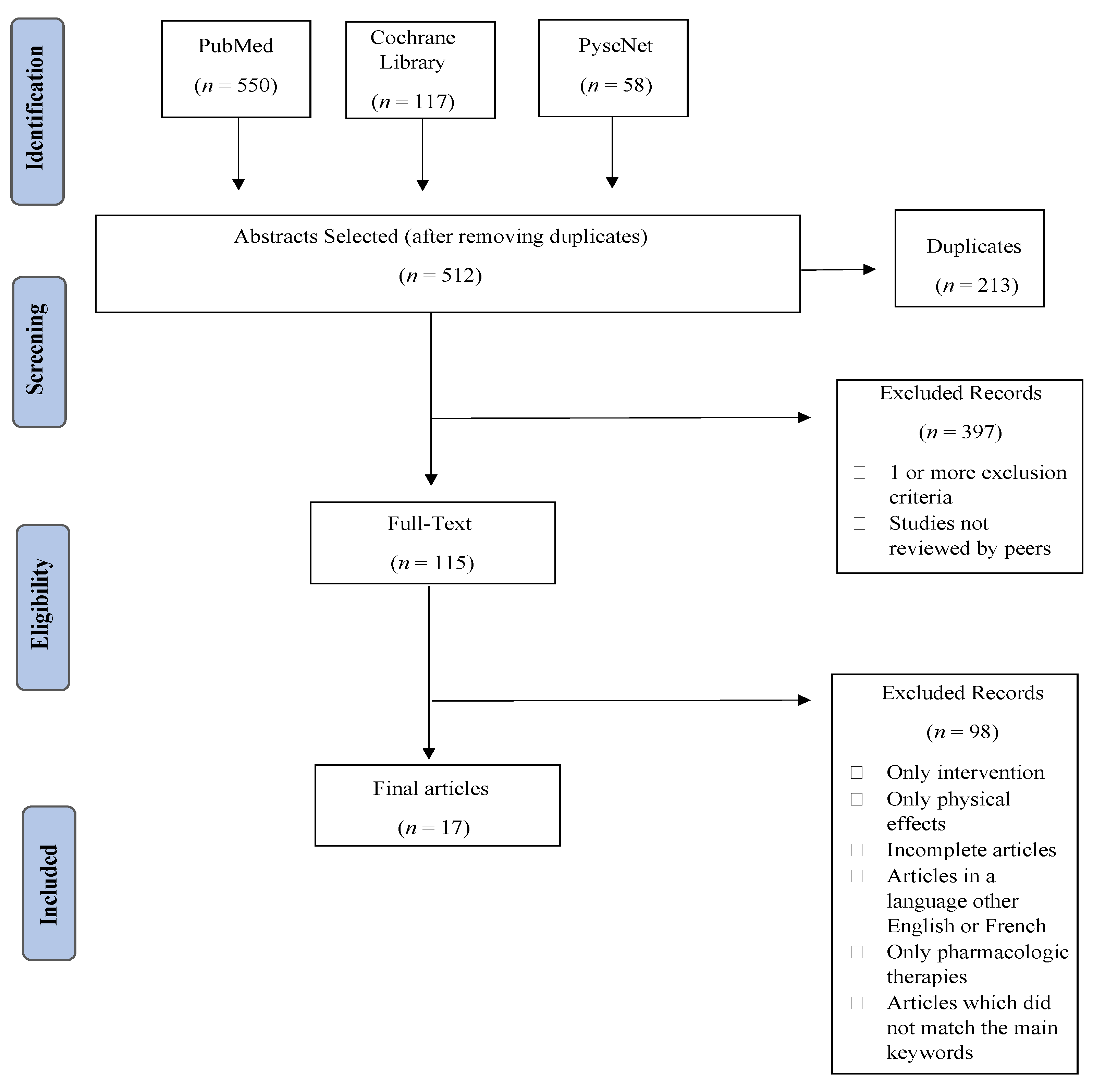
The initial searches through the databases considered resulted in a total of 725 articles, of which 213 (29.38%) were removed because they were duplicates. The abstracts of the remaining 512 (70.62%) studies were screened, and 397 (54.76%) were excluded. From the remaining 115 (15.86%) full-text articles, 98 (13.10%) were ruled out, resulting in 17 (2.76%) articles for review (Figure 1).
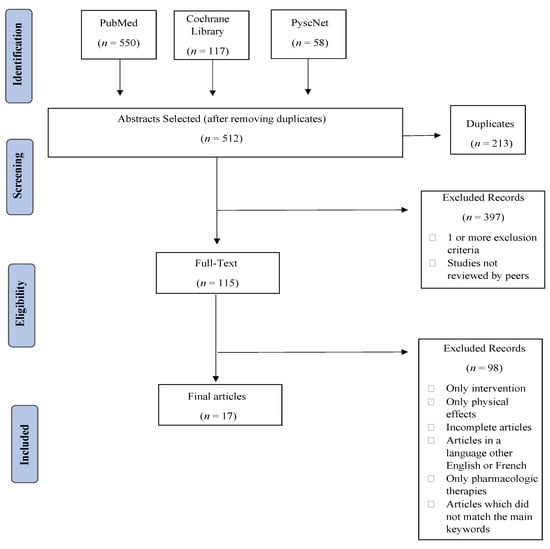
Figure 1.
PRISMA flow diagram comprising the different phases of this systematic review.
4.1. Studies’ Characteristics
The studies’ characteristics (n = 17) are reported in Table 1. One study (6%) includes various types of cancer patients [33], three studies (18%) narrow their samples by recruiting patients with a specific cancer type [26,34,38], nine studies (53%) address the impact of treatments on quality of life [25,26,27,28,32,33,34,37,40] and one study (6%) addresses the role on body image [39]. There are four literature review studies [31,35,39,41], two retrospective studies [25,27], three quantitative studies [29,34,37], one multi-center randomized study [30], one prospective longitudinal study [36] and one prospective study [38].

Table 1.
Resume of the studies reviewed for this literature review.
4.2. Studies’ Results Summary
The analysis of Table 1, Table 2 and Table 3 allows for the understanding that while the methodology and instruments may differ (Table 2 and Table 3), most studies are highly qualified in terms of metrics (Table 1), mostly Q1 and Q2, which demonstrate how valued studies on this topic are. The most studied variables were sociodemographic and clinical characteristics, such as age, sex, type of cancer and treatment (Table 2). QoL is clearly the focus of most articles, underlining aspects related to the psychological well-being or social interactions of the patients. The side effects of cancer treatment and medication are extensively addressed in the reviewed studies, demonstrating the importance given to this specific factor in the well-being of patients. Treatment with EGFRI seems to result in significant physical and psychosocial discomfort of patients and was associated with more dermatological side effects, therefore highlighting the need to further invest in the well-being of patients during the treatment phase. The sense of hope and despair during the illness has been described in some studies, once more within the contest of QoL. While dealing with chemotherapy, there is a perceived need to move away from the disease symptoms and focus on the QoL. These connections need to be better explored, tailored to each patient beyond the improved aspects of health and also specifically address the psychological aspects involved in the QoL.

Table 2.
Variables, analysis and statistical methods used in the studies reviewed for this literature review.

Table 3.
Instruments used in the studies reviewed for this review.
Thus, skin changes are frequently perceived as secondary issues in the context of cancer, often overshadowed by more evident symptoms of the disease. Nevertheless, these dermatological changes can exert a substantial and sometimes underestimated impact on a patient’s QoL, primarily due to their unpredictable nature. It is well established that healthcare practitioners frequently possess limited knowledge regarding these dermatological effects, thereby impeding their ability to provide comprehensive support not only to patients but also to their families. Consequently, it becomes imperative for healthcare professionals to proactively engage in self-education concerning the potential side effects of cancer treatments, particularly those related to changes in physical appearance that may evolve gradually over time. Furthermore, healthcare providers should endeavor to facilitate the holistic management of patients, addressing both the physical and psychological repercussions of these dermatological side effects. This not only empowers patients with a deeper understanding of what they might encounter during their cancer journey but also equips healthcare professionals with the necessary tools to offer more comprehensive and empathetic care. In doing so, the aim is to enhance the overall well-being and QoL of cancer patients and their families, acknowledging the significant role that skin changes can play in their cancer experience.
Clearly, through this systematic review, the two research questions being addressed in this study were answered: The dermatological side effects of the cancer treatment result in psychosocially impacting the patients (RQ1). The psychosocial impact of the dermatological toxicities of the cancer treatment manifest in patients’ lives is demonstrated in the reviewed studies (RQ2).
Table 3 details the instruments used in the analyzed studies.
5. Discussion and Conclusions
Patients with the most varied types of cancer survive longer and mention an improvement in the level of QoL as a consequence of new cancer therapies. Dermatological changes are a common side effect of this treatment [12,42]. They can range from mild to severe and can affect a patient’s physical appearance, comfort and QoL. Some of the most common skin alterations in cancer patients include dryness, itching, rashes, changes in skin color, hair loss or nail changes. These skin effects can be caused by a variety of factors, including chemotherapy, radiation therapy, immunotherapy and surgery. The severity of skin changes can vary depending on the type of cancer treatment, the patient’s individual response to treatment and the patient’s skin type. In some cases, skin changes can be temporary and improve after treatment is finished [43,44]. However, in other cases, these cutaneous alterations can be permanent. It is important for cancer patients to be aware of the potential skin changes that can occur during treatment and the effect they may have on their QoL. Skin toxicities are often understood as minor concerns when compared to cancer symptoms, but they can seriously affect patients’ QoL due to their unforeseen nature. They can impact a patient’s self-esteem, body image and sense of well-being. Skin changes can also make it difficult for patients to perform everyday activities, such as bathing, dressing and sleeping [25,26]. Few studies have addressed the psychosocial impact of the side effects of cancer treatment, as demonstrated in this review. However, the psychological and social impact of dermatoses is well documented, and so it is expected that this impact will be high, similar to what happens with these diseases [45,46,47,48]. Health professionals often have limited knowledge about these effects, which limits their ability to effectively support not only patients but also their families. Therefore, this impact is not considered in therapeutic strategies, and if it were, it would greatly benefit the patient [49]. It is important for healthcare providers to be aware of the potential skin alterations that can occur in cancer patients. They should also be able to provide patients with information and support to help them manage these effects. It is important that these professionals educate themselves and the patients about the possible side effects of cancer treatment, such as modifications in the appearance that may manifest over time, and also seek to help the management of patients’ physical and psychological dimensions.
Following the PRISMA guidelines, this article aimed to address the psychosocial impacts of cancer treatment-related dermatological side effects and how they can be synthesized through a systematic review. While there is a recognition of the adverse impact of dermatological side effects caused by cancer treatments on patients, there remains a dearth of understanding regarding how coping with these effects influences the psychological and social dimensions of cancer patients’ daily lives. This review highlights that the majority of the studies developed have focused on the physical aspects of cancer, and no additional relevance was given to the dermatological aspects associated with the side effects of the treatment. Additionally, research studies concentrating on the consequences of dermatological alterations as their primary focus did not establish a direct connection to cancer itself. This review aimed to contribute to further clarification in relation to the aspects contributing to clarify the key points in the treatment of skin cancer diseases, adding knowledge in this respect. The development of further research studies that are able to assess the psychosocial impact of the dermatological side effects of cancer treatment and psychological interventions to minimize this impact will allow a significant improvement in healthcare for patients undergoing cancer treatment.
Author Contributions
All authors have been involved in all the phases of the review process. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
All data used are included in the study.
Acknowledgments
This work was supported by CESPU—Cooperativa de Ensino Superior Universitário under the Grant “PSYONCODERM_PI_3RL_IINFACTS-2021”.
Conflicts of Interest
The authors declare no conflict of interest.
References
- McDaniel, J.T.; Nuhu, K.; Ruiz, J.; Alorbi, G. Social determinants of cancer incidence and mortality around the world: An ecological study. Glob. Health Promot. 2019, 26, 41–49. [Google Scholar] [CrossRef] [PubMed]
- Drobin, K.; Marczyk, M.; Halle, M.; Danielsson, D.; Papiez, A.; Sangsuwan, T.; Bendes, A.; Hong, M.-G.; Qundos, U.; Harms-Ringdahl, M.; et al. Molecular profiling for predictors of radiosensitivity in patients with breast or head-and-neck cancer. Cancers 2020, 12, 753. [Google Scholar] [CrossRef] [PubMed]
- Sereno, M.; Brunello, A.; Chiappori, A.; Barriuso, J.; Casado, E.; Belda, C.; de Castro, J.; Feliu, J.; González-Barón, M. Cardiac toxicity: Old and new issues in anti-cancer drugs. Clin. Transl. Oncol. 2008, 10, 35–46. [Google Scholar] [CrossRef] [PubMed]
- Ky, B.; Vejpongsa, P.; Yeh, E.T.H.; Force, T.; Moslehi, J.J. Emerging paradigms in cardiomyopathies associated with cancer therapies. Circ. Res. 2013, 113, 754–764. [Google Scholar] [CrossRef] [PubMed]
- Metri, K.G.; Bhargav, H.; Chowdhury, P.; Koka, P.S. Ayurveda for chemo-radiotherapy induced side effects in cancer patients. J. Stem Cells 2013, 8, 115–129. [Google Scholar]
- Lacouture, M.E. Mechanisms of cutaneous toxicities to EGFR inhibitors. Nat. Rev. Cancer 2006, 6, 803–812. [Google Scholar] [CrossRef]
- Zhang, X.J.; Wang, A.P.; Shi, T.Y.; Zhang, J.; Xu, H.; Wang, D.Q.; Feng, L. The psychosocial adaptation of patients with skin disease: A scoping review. BMC Public Health 2019, 19, 1404. [Google Scholar] [CrossRef]
- Boone, S.L.; Rademaker, A.; Liu, D.; Pfeiffer, C.; Mauro, D.J.; Lacouture, M.E. Impact and management of skin toxicity associated with anti-epidermal growth factor receptor therapy: Survey results. Oncology 2008, 72, 152–159. [Google Scholar] [CrossRef]
- Hackbarth, M.; Haas, N.; Fotopoulou, C.; Lichtenegger, W.; Sehouli, J. Chemotherapy-induced dermatological toxicity: Frequencies and impact on quality of life in women’s cancers. Results of a prospective study. Support. Care Cancer 2008, 16, 267–273. [Google Scholar] [CrossRef]
- Jacot, W.; Bessis, D.; Jorda, E.; Ychou, M.; Fabbro, M.; Pujol, J.-L.; Guillot, B. Acneiform eruption induced by epidermal growth factor receptor inhibitors in patients with solid tumours. Br. J. Dermatol. 2004, 151, 238–241. [Google Scholar] [CrossRef]
- Bonner, J.A.; Harari, P.M.; Giralt, J.; Azarnia, N.; Shin, D.M.; Cohen, R.B.; Jones, C.U.; Sur, R.; Raben, D.; Jassem, J.; et al. Radiotherapy plus Cetuximab for Squamous—Cell Carcinoma of the Head and Neck. N. Engl. J. Med. 2006, 354, 567–578. [Google Scholar] [CrossRef] [PubMed]
- Segaert, S.; Van Cutsem, E. Clinical signs, pathophysiology and management of skin toxicity during therapy with epidermal growth factor receptor inhibitors. Ann. Oncol. 2005, 16, 1425–1433. [Google Scholar] [CrossRef] [PubMed]
- Segaert, S.; Chiritescu, G.; Lemmens, L.; Dumon, K.; Van Cutsem, E.; Tejpar, S. Skin toxicities of targeted therapies. Eur. J. Cancer 2009, 45, 295–308. [Google Scholar] [CrossRef] [PubMed]
- Robert, C.; Sibaud, V.; Mateus, C.; Verschoore, M.; Charles, C.; Lanoy, E.; Baran, R. Nail toxicities induced by systemic anticancer treatments. Lancet Oncol. 2015, 16, 181–189. [Google Scholar] [CrossRef] [PubMed]
- Mateus, C.; Robert, C. Effets cutanés des nouvelles molécules utilisées en cancérologie. Rev. Med. Interne 2009, 30, 401–410. [Google Scholar] [CrossRef]
- Lynch, T.J.; Kim, E.S.; Eaby, B.; Garey, J.; West, D.P.; Lacouture, M.E. Epidermal Growth Factor Receptor Inhibitor—Associated Cutaneous Toxicities: An Evolving Paradigm in Clinical Management. Oncologist 2007, 12, 610–621. [Google Scholar] [CrossRef]
- Duijts, S.F.A.; Van Egmond, M.P.; Spelten, E.; Van Muijen, P.; Anema, J.R.; Van Der Beek, A.J. Physical and psychosocial problems in cancer survivors beyond return to work: A systematic review. Psychooncology 2014, 23, 481–492. [Google Scholar] [CrossRef]
- Kent, E.E.; Rowland, J.H.; Northouse, L.; Litzelman, K.; Chou, W.-Y.S.; Shelburne, N.; Timura, C.; O’Mara, A.; Huss, K. Caring for caregivers and patients: Research and clinical priorities for informal cancer caregiving. Cancer 2016, 122, 1987–1995. [Google Scholar] [CrossRef]
- Holland, J.C. History of psycho-oncology: Overcoming attitudinal and conceptual barriers. Psychosom. Med. 2002, 64, 206–221. [Google Scholar] [CrossRef]
- Larouche, S.; Edgar, L. The measure of distress. Contin. CARE Courses Dir. 2004, 3, 34–39. [Google Scholar]
- Bultz, B.D.; Holland, J.C. Emotional distress in patients with cancer: The sixth vital sign. Community Oncol. 2006, 3, 311–314. [Google Scholar] [CrossRef]
- Costa, D.S.J.; Mercieca-Bebber, R.; Rutherford, C.; Gabb, L.; King, M.T. The Impact of Cancer on Psychological and Social Outcomes. Aust. Psychol. 2016, 51, 89–99. [Google Scholar] [CrossRef]
- Zaza, C.; Baine, N. Cancer pain and psychosocial factors: A critical review of the literature. J. Pain. Symptom Manag. 2002, 24, 526–542. [Google Scholar] [CrossRef]
- Brown, L.F.; Kroenke, K. Cancer-Related Fatigue and Its Associations with Depression and Anxiety: A Systematic Review. Psychosomatics 2009, 50, 440–447. [Google Scholar] [CrossRef] [PubMed]
- Joshi, S.S.; Ortiz, S.; Witherspoon, J.N.; Rademaker, A.; West, D.P.; Anderson, R.; Rosenbaum, S.E.; Lacouture, M.E. Effects of epidermal growth factor receptor inhibitor-induced dermatologic toxicities on quality of life. Cancer 2010, 116, 3916–3923. [Google Scholar] [CrossRef]
- Ocvirk, J.; Cencelj, S. Management of cutaneous side-effects of cetuximab therapy in patients with metastatic colorectal cancer. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 453–459. [Google Scholar] [CrossRef]
- Osio, A.; Mateus, C.; Soria, J.-C.; Massard, C.; Malka, D.; Boige, V.; Besse, B.; Robert, C. Cutaneous side-effects in patients on long-term treatment with epidermal growth factor receptor inhibitors. Br. J. Dermatol. 2009, 161, 515–521. [Google Scholar] [CrossRef]
- De Boer-Dennert, M.; de Wit, R.; Schmitz, P.; Djontono, J.; Beurden, V.V.; Stoter, G.; Verweij, J. Patient perceptions of the side-effects of chemotherapy: The influence of 5HT3 antagonists. Br. J. Cancer 1997, 76, 1055–1061. [Google Scholar] [CrossRef]
- Griffin, A.M.; Butow, P.N.; Coates, A.S.; Childs, A.M.; Ellis, P.M.; Dunn, S.M.; Tattersall, M.H.N. On the receiving end V: Patient perceptions of the side effects of cancer chemotherapy in 1993. Ann. Oncol. 1996, 7, 189–195. [Google Scholar] [CrossRef]
- Kiebert, G.M.; de Haes, J.H.C.J.M.; Kievit, J.; van de Velde, C.J.H. Effect of peri-operative chemotherapy on the quality of life of patients with early breast cancer. Eur. J. Cancer Clin. Oncol. 1990, 26, 1038–1042. [Google Scholar] [CrossRef]
- Agero, A.L.C.; Dusza, S.W.; Benvenuto-Andrade, C.; Busam, K.J.; Myskowski, P.; Halpern, A.C. Dermatologic side effects associated with the epidermal growth factor receptor inhibitors. J. Am. Acad. Dermatol. 2006, 55, 657–670. [Google Scholar] [CrossRef] [PubMed]
- Freites-Martinez, A.; Chan, D.; Sibaud, V.; Shapiro, J.; Fabbrocini, G.; Tosti, A.; Cho, J.; Goldfarb, S.; Modi, S.; Gajria, D.; et al. Assessment of Quality of Life and Treatment Outcomes of Patients With Persistent Postchemotherapy Alopecia. JAMA Dermatol. 2019, 155, 724–728. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Lim, J.; Park, J.S.; Kim, M.; Kim, T.Y.; Kim, T.M.; Lee, K.H.; Keam, B.; Han, S.W.; Mun, J.H.; et al. The Impact of Skin Problems on the Quality of Life in Patients Treated with Anticancer Agents: A Cross-Sectional Study. Cancer Res. Treat. 2018, 50, 1186–1193. [Google Scholar] [CrossRef] [PubMed]
- Romito, F.; Giuliani, F.; Cormio, C.; Tulipani, C.; Mattioli, V.; Colucci, G. Psychological effects of cetuximab-induced cutaneous rash in advanced colorectal cancer patients. Support. Care Cancer 2010, 18, 329–334. [Google Scholar] [CrossRef]
- Hesketh, P.J.; Batchelor, D.; Golant, M.; Lyman, G.H.; Rhodes, N.; Yardley, D. Chemotherapy-induced alopecia: Psychosocial impact and therapeutic approaches. Support. Care Cancer 2004, 12, 543–549. [Google Scholar] [CrossRef]
- Münstedt, K.; Manthey, N.; Sachsse, S.; Vahrson, H. Changes in self-concept and body image during alopecia induced cancer chemotherapy. Support. Care Cancer 1997, 5, 139–143. [Google Scholar] [CrossRef]
- Charles, C.; Razavi, D.; Bungener, C.; Mateus, C.; Lanoy, E.; Verschoore, M.; Dauchy, S.; Robert, C. Impact of Skin Toxicities Associated with Targeted Cancer Therapies on Body Image: A Prospective Study. Clin. Drug Investig. 2016, 36, 235–242. [Google Scholar] [CrossRef]
- De Sanctis, V.; Agolli, L.; Visco, V.; Monaco, F.; Muni, R.; Spagnoli, A.; Campanella, B.; Valeriani, M.; Minniti, G.; Osti, M.F.; et al. Cytokines, fatigue, and cutaneous erythema in early stage breast cancer patients receiving adjuvant radiation therapy. BioMed Res. Int. 2014, 2014, 523568. [Google Scholar] [CrossRef]
- Helms, R.L.; O’Hea, E.L.; Corso, M. Body image issues in women with breast cancer. Psychol. Health Med. 2008, 13, 313–325. [Google Scholar] [CrossRef]
- Abd EL-rafea, S.A.K.; Abd Allah, E.S.; Elsayed Ahmed, N.M. Effect of skin reactions on quality of life for elderly women with breast cancer receiving chemotherapy. Zagazig Nurs. J. 2021, 17, 42–55. [Google Scholar]
- Silva, D.; Gomes, A.; Ms Lobo, J.; Almeida, V.; Almeida, I.F. Management of skin adverse reactions in oncology. J. Oncol. Pharm. Pract. 2020, 26, 1703–1714. [Google Scholar] [CrossRef] [PubMed]
- Robert, C.; Soria, J.-C.; Spatz, A.; Le Cesne, A.; Malka, D.; Pautier, P.; Wechsler, J.; Lhomme, C.; Escudier, B.; Boige, V.; et al. Cutaneous side-effects of kinase inhibitors and blocking antibodies. Lancet Oncol. 2005, 6, 491–500. [Google Scholar] [CrossRef] [PubMed]
- Rosman, I.S.; Anadkat, M.J. Tufted hair folliculitis in a woman treated with trastuzumab. Target. Oncol. 2010, 5, 295–296. [Google Scholar] [CrossRef] [PubMed]
- Duffour, J.; Thézenas, S.; Dereure, O.; Garcin, A.; Caron, J.; Samalin, E.; Portales, F.; Fiess, C.; Chalbos, P.; Gestin-Boyer, C.; et al. Inter-observer agreement between dermatologists and oncologists in assessing dermatological toxicities in patients with metastatic colorectal cancer treated by cetuximab-based chemotherapies: A pilot comparative study. Eur. J. Cancer 2010, 46, 3169–3174. [Google Scholar] [CrossRef]
- Mian, M.; Silfvast-Kaiser, A.; Paek, S.; Kivelevitch, D.; Menter, A. A review of the most common dermatologic conditions and their debilitating psychosocial impacts. Int. Arch. Int. Med. 2019, 3, 18. [Google Scholar] [CrossRef]
- Lukaviciute, L.; Ganceviciene, R.; Navickas, P.; Navickas, A.; Grigaitiene, J.; Zouboulis, C.C. Anxiety, depression, and suicidal ideation amongst patients with facial dermatoses (acne, rosacea, perioral dermatitis, and folliculitis) in Lithuania. Dermatology 2020, 236, 314–322. [Google Scholar] [CrossRef]
- Ozcan, Y.; Sungur, M.A.; Ozcan, B.Y.; Eyup, Y.; Ozlu, E. The Psychosocial Impact of Chronic Facial Dermatoses in Adults. Dermatol. Pract. Concept. 2023, 13, e2023029. [Google Scholar] [CrossRef]
- Kelly, K.A.; Balogh, E.A.; Kaplan, S.G.; Feldman, S.R. Skin disease in children: Effects on quality of life, stigmatization, bullying, and suicide risk in pediatric acne, atopic dermatitis, and psoriasis patients. Children 2021, 8, 1057. [Google Scholar] [CrossRef]
- Picardi, A.; Lega, I.; Tarolla, E. Suicide risk in skin disorders. Clin. Dermatol. 2013, 31, 47–56. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).