Implications of Dual Practice on Cataract Surgery Waiting Time and Rescheduling: The Case of Malaysia
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Outcome Measures
2.2.1. Waiting Time for Elective Surgery
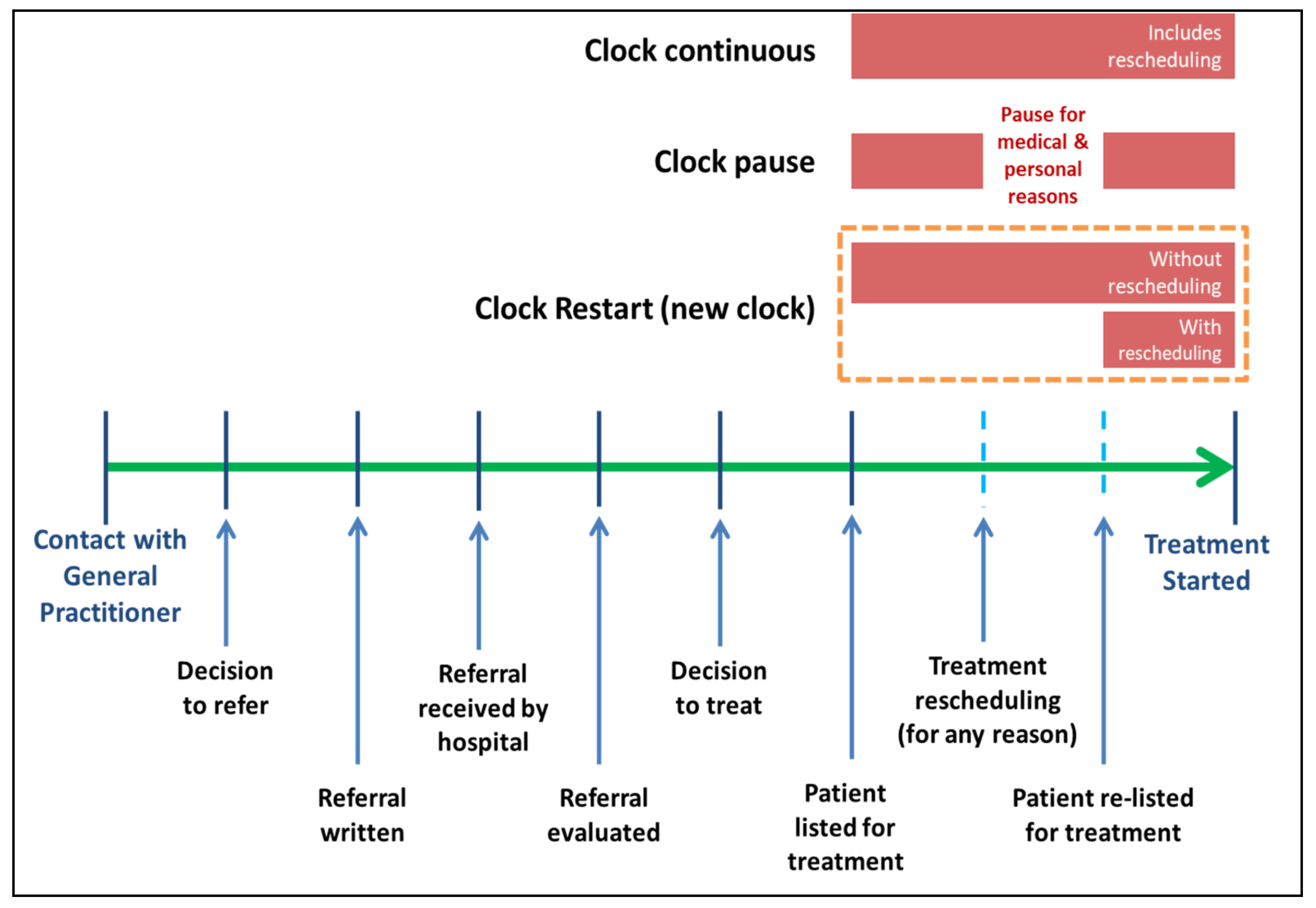
- Clock-continuous scenario: continuous measurement of waiting times in all patients regardless of their reasons for rescheduling [9].
- Clock-pause scenario: discounts the rescheduling period in patients rescheduled due to patient or medical factors [24].
- Clock-restart (“new clock”) scenario: eliminates the previous waiting time and restarts a new clock when there is rescheduling [25].
2.2.2. Rescheduling of Surgery
2.3. Sample Size Calculation
2.4. Data Collection
2.5. Data Analysis
3. Results
3.1. Socio-Demographic Characteristics
3.2. Waiting Time to Operation
3.3. Surgery Rescheduling
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chua, H.T.; Cheah, J.C.H. Financing Universal Coverage in Malaysia: A case study. BMC Public Health 2012, 12, S7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rannan-Eliya, R.P.; Anuranga, C.; Manual, A.; Sararaks, S.; Jailani, A.S.; Hamid, A.J.; Razif, I.M.; Tan, E.H.; Darzi, A. Improving Health Care Coverage, Equity, And Financial Protection Through A Hybrid System: Malaysia’s Experience. Health Aff. 2016, 35, 838–846. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chan, C.K. The state and healthcare in Malaysia: Provider, regulator, investor. In Proceedings of the Health & Health Systems in Southeast Asia, Cambridge, MA, USA, 25–26 June 2019; Volume 296/297, pp. 34–37. [Google Scholar]
- Socha, K.Z.; Bech, M. Physician dual practice: A review of literature. Health Policy 2011, 102, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Hipgrave, D.B.; Hort, K. Will current health reforms in South and East Asia improve equity? Med. J. Aust. 2014, 200, 514–516. [Google Scholar] [CrossRef] [PubMed]
- Moghri, J.; Arab, M.; Rashidian, A.; Akbari Sari, A. Physician Dual Practice: A Descriptive Mapping Review of Literature. Iran. J. Public Health 2016, 45, 278–288. [Google Scholar]
- Private Wards in Public Hospitals: What Are the Policy and Governance Implications? A Case Study of Tygerberg Academic Hospital. Available online: https://www.who.int/alliance-hpsr/projects/alliancehpsr_gehwadeegilson.pdf (accessed on 10 May 2021).
- Pillay, D.I.; Ghazali, R.J.; Manaf, N.H.; Abdullah, A.H.; Bakar, A.A.; Salikin, F.; Umapathy, M.; Ali, R.; Bidin, N.; Ismail, W.I. Hospital waiting time: The forgotten premise of healthcare service delivery? Int. J. Health Care Qual. Assur. 2011, 24, 506–522. [Google Scholar] [CrossRef]
- Siciliani, L.; Moran, V.; Borowitz, M. Measuring and comparing health care waiting times in OECD countries. Health Policy 2014, 118, 292–303. [Google Scholar] [CrossRef] [Green Version]
- Harrison, A.; Appleby, J. Reducing waiting times for hospital treatment: Lessons from the English NHS. J. Health Serv. Res. Policy 2009, 14, 168–173. [Google Scholar] [CrossRef]
- Boudreau, S.A.; Gibson, M.J. Surgical cancellations: A review of elective surgery cancellations in a tertiary care pediatric institution. J. Perianesthesia Nurs. 2011, 26, 315–322. [Google Scholar] [CrossRef]
- Haana, V.; Sethuraman, K.; Stephens, L.; Rosen, H.; Meara, J.G. Case cancellations on the day of surgery: An investigation in an Australian paediatric hospital. ANZ J. Surg. 2009, 79, 636–640. [Google Scholar] [CrossRef]
- Perroca, M.G.; Jerico Mde, C.; Facundin, S.D. Surgery cancelling at a teaching hospital: Implications for cost management. Rev. Lat. Am. Enferm. 2007, 15, 1018–1024. [Google Scholar] [CrossRef] [Green Version]
- Al Talalwah, N.; McIltrot, K.H.; Al Ghamdi, A. Elective Surgical Cancellations in a Tertiary Hospital in the Middle East: Quality Improvement Process. J. Perianesthesia Nurs. 2019, 34, 310–321. [Google Scholar] [CrossRef]
- Pratap, J.N.; Varughese, A.M.; Mercurio, P.; Lynch, T.; Lonnemann, T.; Ellis, A.; Rugg, J.; Stone, W.R.; Bedinghaus, C. Reducing Cancellations on the Day of Scheduled Surgery at a Children’s Hospital. Pediatrics 2015, 135, e1292–e1299. [Google Scholar] [CrossRef] [Green Version]
- Botazini, N.O.; de Carvalho, R. Cancellation of surgeries: An integrative literature review. Rev. SOBECC 2017, 22, 230–244. [Google Scholar] [CrossRef] [Green Version]
- Kaddoum, R.; Fadlallah, R.; Hitti, E.; El-Jardali, F.; El Eid, G. Causes of cancellations on the day of surgery at a Tertiary Teaching Hospital. BMC Health Serv. Res. 2016, 16, 259. [Google Scholar] [CrossRef] [Green Version]
- Dhafar, K.O.; Ulmalki, M.A.; Felemban, M.A.; Mahfouz, M.E.; Baljoon, M.J.; Gazzaz, Z.J.; Baig, M.; Hamish, N.M.; AlThobaiti, S.A.; Al-Hothali, F.T. Cancellation of operations in Saudi Arabian hospitals: Frequency, reasons and suggestions for improvements. Pak. J. Med. Sci. 2015, 31, 1027–1032. [Google Scholar] [CrossRef]
- Kumar, R.; Gandhi, R. Reasons for cancellation of operation on the day of intended surgery in a multidisciplinary 500 bedded hospital. J. Anaesthesiol. Clin. Pharmacol. 2012, 28, 66–69. [Google Scholar] [CrossRef]
- Yu, K.; Xie, X.; Luo, L.; Gong, R. Contributing factors of elective surgical case cancellation: A retrospective cross-sectional study at a single-site hospital. BMC Surg. 2017, 17, 100. [Google Scholar] [CrossRef]
- Lankoandé, M.; Bonkoungou, P.; K Ki, B.; Flavien, R.; Kaboré, A.; Ouangré, E.; Savadogo, Y.; Thw Bougouma, C.; Sanou, J.; Ouedraogo, N.; et al. Economic and psychological burden of scheduled surgery cancellation in a sub-Saharan country (Burkina Faso). S. Afr. J. Anaesth. Analg. 2017, 23, 145–151. [Google Scholar] [CrossRef]
- Dimitriadis, P.A.; Iyer, S.; Evgeniou, E. The challenge of cancellations on the day of surgery. Int. J. Surg. 2013, 11, 1126–1130. [Google Scholar] [CrossRef] [Green Version]
- Ministry of Health Malaysia. Guidelines for Implementation Fee Order (Medical) (Full Paying Patient). 2007; Ministry of Health Malaysia: Putrajaya, Malaysia, 2015.
- Australian Institute of Health and Welfare (AIHW). National Definitions for Elective Surgery Urgency Categories: Proposal for the Standing Council on Health; Australian Institute of Health and Welfare (AIHW), Royal Australasian College of Surgeons: Canberra, Australia, 2013.
- NHS Clinical Services Team. Referral to Treatment Consultant-Led Waiting Times. Rules Suite; October 2015; Department of Health England: Leeds, UK, 2015.
- Viberg, N.; Forsberg, B.C.; Borowitz, M.; Molin, R. International comparisons of waiting times in health care—Limitations and prospects. Health Policy 2013, 112, 53–61. [Google Scholar] [CrossRef] [Green Version]
- NHS Modernisation Agency. Theatre Programme. In Step Guide to Improving Operating Theatre Performance; NHS Modernisation Agency: London, UK, 2002. [Google Scholar]
- Sullivan, L.M. Essentials of Biostatistics in Public Health; Jones & Bartlett Publishers: Burlington, MA, USA, 2011. [Google Scholar]
- Valente, R.; Testi, A.; Tanfani, E.; Fato, M.; Porro, I.; Santo, M.; Santori, G.; Torre, G.; Ansaldo, G. A model to prioritize access to elective surgery on the basis of clinical urgency and waiting time. BMC Health Serv. Res. 2009, 9, 1. [Google Scholar] [CrossRef] [Green Version]
- World Health Organization. International Statistical Classification of Diseases and Related Health Problems 10th Revision (English version). Available online: https://icd.who.int/browse10/2010/en (accessed on 30 April 2021).
- Cole, E.; Hopman, W.; Kawakami, J. High resolution analysis of wait times and factors affecting surgical expediency. Can. Urol. Assoc. J. 2011, 5, 13–17. [Google Scholar] [CrossRef] [Green Version]
- Kawakami, J.; Hopman, W.M.; Smith-Tryon, R.; Siemens, D.R. Measurement of surgical wait times in a universal health care system. Can. Urol. Assoc. J. 2008, 2, 597–603. [Google Scholar] [CrossRef] [Green Version]
- National Health Service (NHS) England. Recording and Reporting Referral to Treatment (RTT) Waiting Times for Consultant-Led Elective Care; National Health Services (NHS) England: London, UK, 2015.
- Willcox, S.; Seddon, M.; Dunn, S.; Edwards, R.T.; Pearse, J.; Tu, J.V. Measuring and reducing waiting times: A cross-national comparison of strategies. Health Aff. 2007, 26, 1078–1087. [Google Scholar] [CrossRef] [Green Version]
- Australian Institute of Health and Welfare (AIHW). Admitted Patient Care 2016–17: Australian Hospital Statistics; AIHW: Canberra, Austrilia, 2018.
- Viberg, N. Swedish Waiting Times for Health Care in an International Perspective; Swedish Association of Local Authorities and Regions (SALAR): Stockholm, Sweden, 2011. [Google Scholar]
- Canadian Institute for Health Information. Wait Times for Priority Procedures in Canada; CIHI: Ottawa, ON, Canada, 2016. [Google Scholar]
- Ministry of Health Malaysia. Key Performance Indicators (KPI) for Clinical Departments: Ophthalmology 2008; Section on Quality in Medical Care, Medical Development Division, Ministry of Health Malaysia: Putrajaya, Malaysia, 2007.
- Hovlid, E.; Bukve, O.; Haug, K.; Aslaksen, A.B.; von Plessen, C. A new pathway for elective surgery to reduce cancellation rates. BMC Health Serv. Res. 2012, 12, 154. [Google Scholar] [CrossRef] [Green Version]
- Knox, M.; Myers, E.; Hurley, M. The impact of pre-operative assessment clinics on elective surgical case cancellations. Surgeon 2009, 7, 76–78. [Google Scholar] [CrossRef]
- Ezike, H.; Ajuzieogu, V.; Amucheazi, A. Reasons for elective surgery cancellation in a referral hospital. Ann. Med. Health Sci. Res. 2011, 1, 197–202. [Google Scholar] [PubMed]
- Kenis, P. Waiting lists in Dutch health care: An analysis from an organization theoretical perspective. J. Health Organ. Manag. 2006, 20, 294–308. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Finn, C.; Hardiman, N. Creating Two Levels of Healthcare; University College Dublin Geary Institute: Dublin, Ireland, 2007. [Google Scholar]
- McPake, B.; Nakamba, P.; Hanson, K.; McLoughlin, B. Private Wards in Public Hospitals: Two-Tier Charging and the Allocation of Resources in Tertiary Hospitals in Zambia; Health Economics and Financing Programme: Lusaka, Zambia, 2004. [Google Scholar]
- Cooper, Z.N.; McGuire, A.; Jones, S.; Le Grand, J. Equity, waiting times, and NHS reforms: Retrospective study. BMJ 2009, 339, b3264. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Derrett, S.; Bevin, T.H.; Herbison, P.; Paul, C. Access to elective surgery in New Zealand: Considering equity and the private and public mix. Int. J. Health Plan. Manag. 2009, 24, 147. [Google Scholar] [CrossRef]
- Parliament of Malaysia. Private Healthcare Facilities and Services and Other Private Healthcare FAcilities) (Amendment) Order 2013. In P.U.(A) 358; Chambers, A.G.S., Ed.; Parliament of Malaysia: Kuala Lumpur, Malaysia, 2013. [Google Scholar]
- Parliament of Malaysia. Fees (Medical) (Full Paying Patient) Order 2007. In Order (PU (A) 252/2007 ed., Gazette, 16; Chambers, A.G.S., Ed.; Parliament of Malaysia: Kuala Lumpur, Malaysia, 2007. [Google Scholar]
- Ministry of Health Malaysia. DG of Health Circular: Implementation of Elective Surgery on Saturday at Identified Government Hopsital (Malay). Available online: https://www.moh.gov.my/index.php/database_stores/store_view_page/10/160 (accessed on 26 April 2021).
- Muhammad Nur Amir, A.; Sharifa Ezat, W. Physician’s intention to leave from malaysia government hospitals with existing retention strategy. J. Public Health Policy Plan. 2020, 4, 5–7. [Google Scholar]

| Characteristic | Cataract (ICD10 H26–28) | p-Value | |
|---|---|---|---|
| Private | Public | ||
| Age (year) [Mean (SD)] | 58.66 (14.41) | 50.44 (22.56) | 0.166 a |
| Gender (%) | 0.625 b | ||
| Male | 30 (56.6) | 78 (52.7) | |
| Female | 23 (43.4) | 70 (47.3) | |
| Nationality (%) | 0.001 *,c | ||
| Malaysian | 48 (90.6) | 148 (100) | |
| Non-Malaysian | 5 (9.4) | 0 (0) | |
| Ethnicity (%) | <0.001 *,c | ||
| Malay | 13 (24.5) | 80 (54.1) | |
| Chinese | 17 (32.1) | 41 (27.7) | |
| Indian | 18 (34.0) | 24 (16.2) | |
| Others d | 5 (9.4) | 3 (2.0) | |
| Comorbidities e (%) | 0.015 *,b | ||
| Yes | 32 (60.4) | 115 (77.7) | |
| No | 21 (39.6) | 33 (22.3) | |
| Surgery Performed Time (%) | <0.001 *,c | ||
| Office hour | 0 (0) | 117 (79.0) | |
| After hours on weekdays/weekends | 53 (100.0) | 29 (19.6) | |
| Unknown | 0 | 2 (1.4) | |
| Waiting Time to Cataract Procedure Approaches (Days) | Private (n = 53) | Public (n = 148) | Public: Private Ratio a | |
|---|---|---|---|---|
| Clock continuous | Median (Q1, Q3) | 7 (2.00, 14.00) | 48.00 (16.00, 94.00) | 6.9 * |
| Mean (SD) | 15.26 (27.28) | 70.57 (82.50) | ||
| Clock pause | Median (Q1, Q3) | 7 (2.00, 14.00) | 41.5 (15.50, 89.50) | 5.9 * |
| Mean (SD) | 15.26 (27.28) | 60.48 (59.69) | ||
| Clock restart (new clock) | Median (Q1, Q3) | 7 (2.00, 14.00) | 38.5 (13.00, 83.00) | 5.5 * |
| Mean (SD) | 15.26 (27.28) | 57.41 (66.14) | ||
| Private | Public | |
|---|---|---|
| Scheduling status a,*(%) | ||
| Scheduled | 53 (100) | 126 (85.1) |
| Rescheduled | 0 | 22 (14.9) |
| Number and reason for rescheduling (%) | ||
| One time | 0 (0) | 19 (86.4) |
| Medical | 14 (73.7) | |
| Patient | 3 (15.8) | |
| Resource | 2 (10.5) | |
| Two times | 0 (0) | 3 (13.6) |
| Medical | 2 (66.7) | |
| Medical and Patient | 1 (33.3) |
| Reason * | Count | % |
|---|---|---|
| Medical Factor | ||
| Uncontrolled blood pressure | 8 | 38.1 |
| Upper Respiratory Tract Infection | 5 | 23.8 |
| Cardiac condition | 1 | 4.8 |
| Uncontrolled diabetes | 3 | 14.3 |
| Other medical factors | 3 | 14.3 |
| Additional investigation required | 1 | 4.8 |
| Total | 21 | 100.0 |
| Patient Factor | ||
| Patient’s request or due to other personal reasons | 4 | 100.0 |
| Total | 4 | 100.0 |
| Resource Factor | ||
| Operation theatre chiller not functioning | 1 | 50.0 |
| To try new phacoemulsification machine | 1 | 50.0 |
| Total | 2 | 100.0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fun, W.H.; Tan, E.H.; Sararaks, S.; Md. Sharif, S.; Ab Rahim, I.; Jawahir, S.; Eow, V.H.Y.; Sibert, R.M.Y.; Fadzil, M.M.; Mahmud, S.H. Implications of Dual Practice on Cataract Surgery Waiting Time and Rescheduling: The Case of Malaysia. Healthcare 2021, 9, 653. https://doi.org/10.3390/healthcare9060653
Fun WH, Tan EH, Sararaks S, Md. Sharif S, Ab Rahim I, Jawahir S, Eow VHY, Sibert RMY, Fadzil MM, Mahmud SH. Implications of Dual Practice on Cataract Surgery Waiting Time and Rescheduling: The Case of Malaysia. Healthcare. 2021; 9(6):653. https://doi.org/10.3390/healthcare9060653
Chicago/Turabian StyleFun, Weng Hong, Ee Hong Tan, Sondi Sararaks, Shakirah Md. Sharif, Iqbal Ab Rahim, Suhana Jawahir, Vivien Han Ying Eow, Raoul Muhammad Yusof Sibert, Malindawati Mohd Fadzil, and Siti Haniza Mahmud. 2021. "Implications of Dual Practice on Cataract Surgery Waiting Time and Rescheduling: The Case of Malaysia" Healthcare 9, no. 6: 653. https://doi.org/10.3390/healthcare9060653








