4. Discussion
NcRNAs have been implicated in various hallmarks of cancer. Extensive research on ncRNAs has led to the understanding that lncRNAs as well as miRNAs are able to govern the levels of expression of their corresponding target genes at transcriptomic and translational levels. Gulìa et al. illustrated the effect of ncRNAs on the control of the metastatic, migration, and invasion processes as well as the effect on cell cycle arrest and proliferation of bladder cancer cells [
10]. Moreover, novel treatment pathways are starting to emerge in the clinical practice using targeted inhibition of various ncRNA molecules. This would be of particular importance to women in their fertile years desiring to become pregnant. This is because fertility rates have been found to be about three times lower in women with a history of BC treatment, due to the need to delay conception until treatment is complete and the direct gonadotoxic effects of treatments [
11]. A futuristic yet legitimate outlook to the power of assessing ncRNAs can combine diagnostic, prognostic, and therapeutic parameters to help in generating an ‘epigenetic profile’ of cancer patients and to derive a tailored therapy for cancer patients of different stages and subtypes [
12].
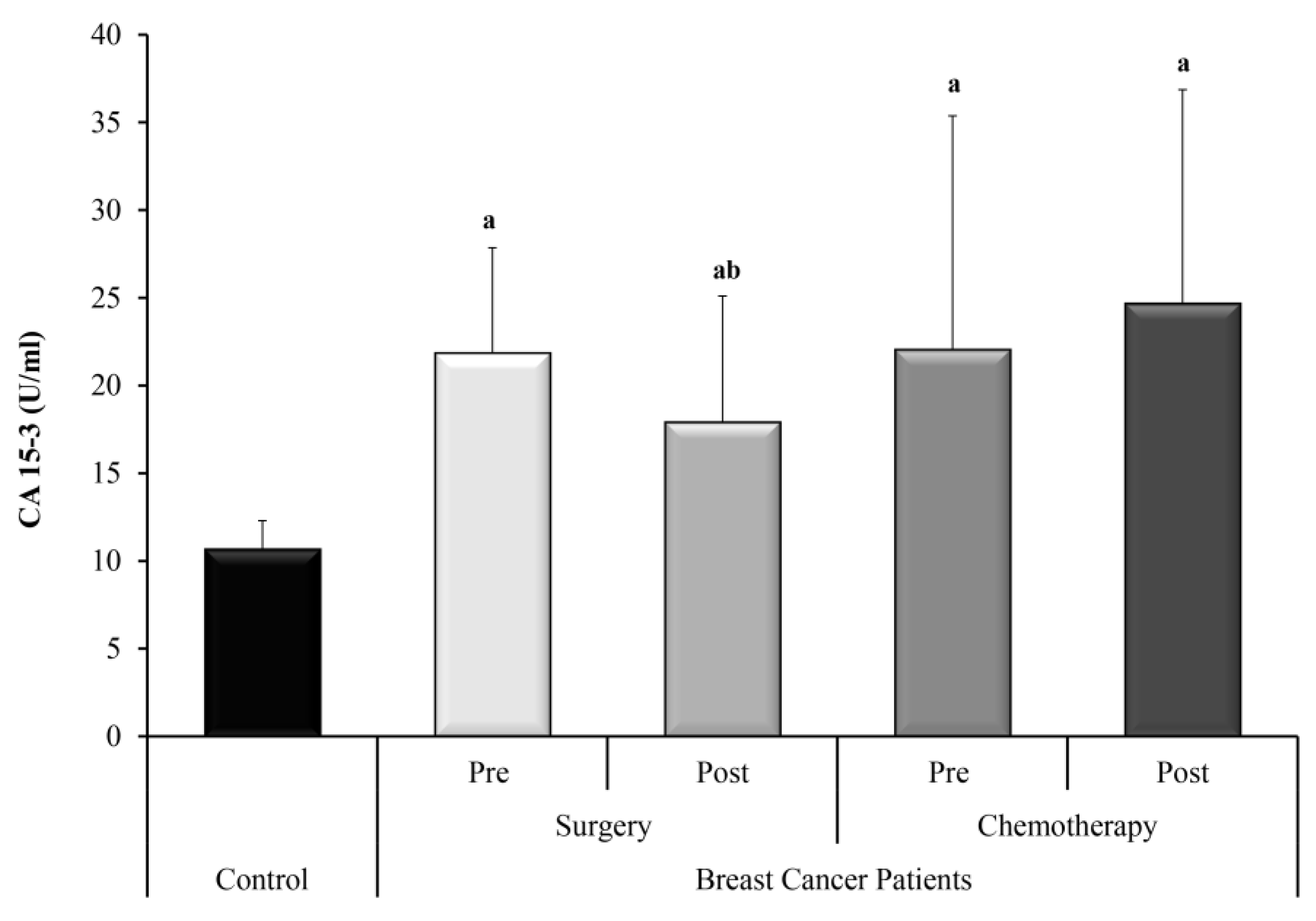
In the present study, CA 15-3 was measured as a conventional circulating tumor marker in breast cancer for comparison of the ncRNAs under investigation. CA 15-3 serum levels were significantly higher in the two groups of BC patients who underwent surgery only and who received adjuvant chemotherapy, compared with the control group. CA 15-3 dropped significantly after surgery yet did not show a significant change after chemotherapy.
H19 is involved in many biological processes including apoptosis, cell proliferation, and invasion in several tumors including BC [
13]. It is implicated in the development of BC and increases G1 to S cell cycle transition when up regulated [
14]. High tumor expressions of H19 were associated with the size of the tumor, nodal status and hormone negativity, having a negative correlation with the prognosis of BC. Unfavorable disease free and overall survival were exhibited in patients with high H19 levels [
15]. Moreover, another study has found that the overexpression of H19 brought about a reversal in the tumor inhibitory effects of Huaier extract, yet its knocking down sensitized BC cells to Huaier extract. This study promoted the idea that the H19/miRNA-675/CBL pathway is responsible for the BC cell proliferation and induction of apoptosis [
7]. In light of these findings, H19 serves as a potential biomarker for the diagnosis of BC as well as a useful tool in the assessment of the response to adjuvant and neoadjuvant chemotherapy in BC. Furthermore, the response to therapy was also correlated to H19, where overly expressed H19 increased BC cell drug resistance to doxorubicin [
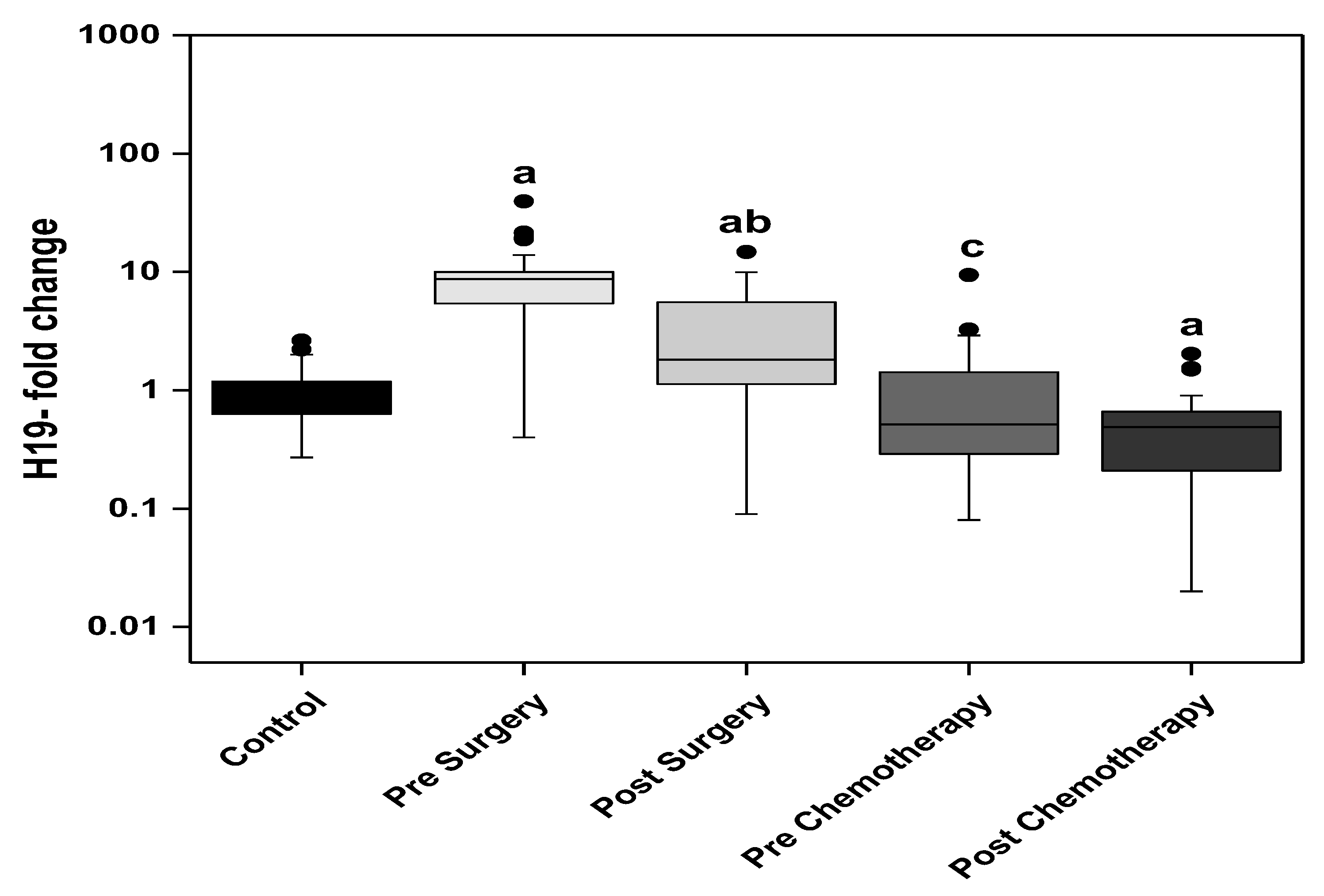
16]. The findings of the present study agree with the emerging evidence identifying H19 as an oncogene. Analysis of the circulating H19 in the present study revealed significantly higher levels in the presurgery BC patients when compared to the control group. The levels significantly dropped after surgery yet were still significantly higher than the control group. A further significant drop in the BC patients about to receive adjuvant chemotherapy was measured with no significant change in circulating H19 upon receiving chemotherapy. Then, the circulating H19 level showed a further significant drop in the prechemotherapy group when compared to the postsurgery BC patients and the chemotherapy did not show further significant change in H19 levels.
With regard to the descendants of H19; miRNA 675-5p and 675-3p, a literature review found that miRNA-675, whether alone or together with H19, plays a role in cellular invasion and migration [
17]. A study of miRNA-675 in paraffin embedded tissues demonstrated that the expression of miRNA-675 was significantly higher in the tissues of patients with BC compared with the control group, where no association was found between expression levels and age, lymph node, stage and receptor status [
18]. In agreement with this data, Matouk et al. demonstrated that miRNA-675 indirectly targets slug leading to increase of cell invasion and in vivo metastasis [
19]. Another study has also identified both H19 and miRNA-675 as key players in the activation of the invasion and migration of BC cells [
17]. These findings contrast with the results of a study carried out on 63 non-metastasized BC patients in University Medical Center Hamburg-Eppendorf, where no deregulation of plasma miRNA-675 was found in the entire BC group [
18]. The discrepancy in the results of miRNA-675 in BC patients may be reasoned by the method of analysis and calculation of data. As there is no consensus concerning the data normalization in the circulation, miRNA-16-5p was chosen as a reference gene in the present study to normalize the lncRNA and microRNAs’ data since miR-16-5p is one of the most frequently used reference gene according to literature [
20]. Meanwhile, in the study of Müller et al. [
18], miR-484 and b-actin were used as references to normalize their miRNA and lncRNA data, respectively.
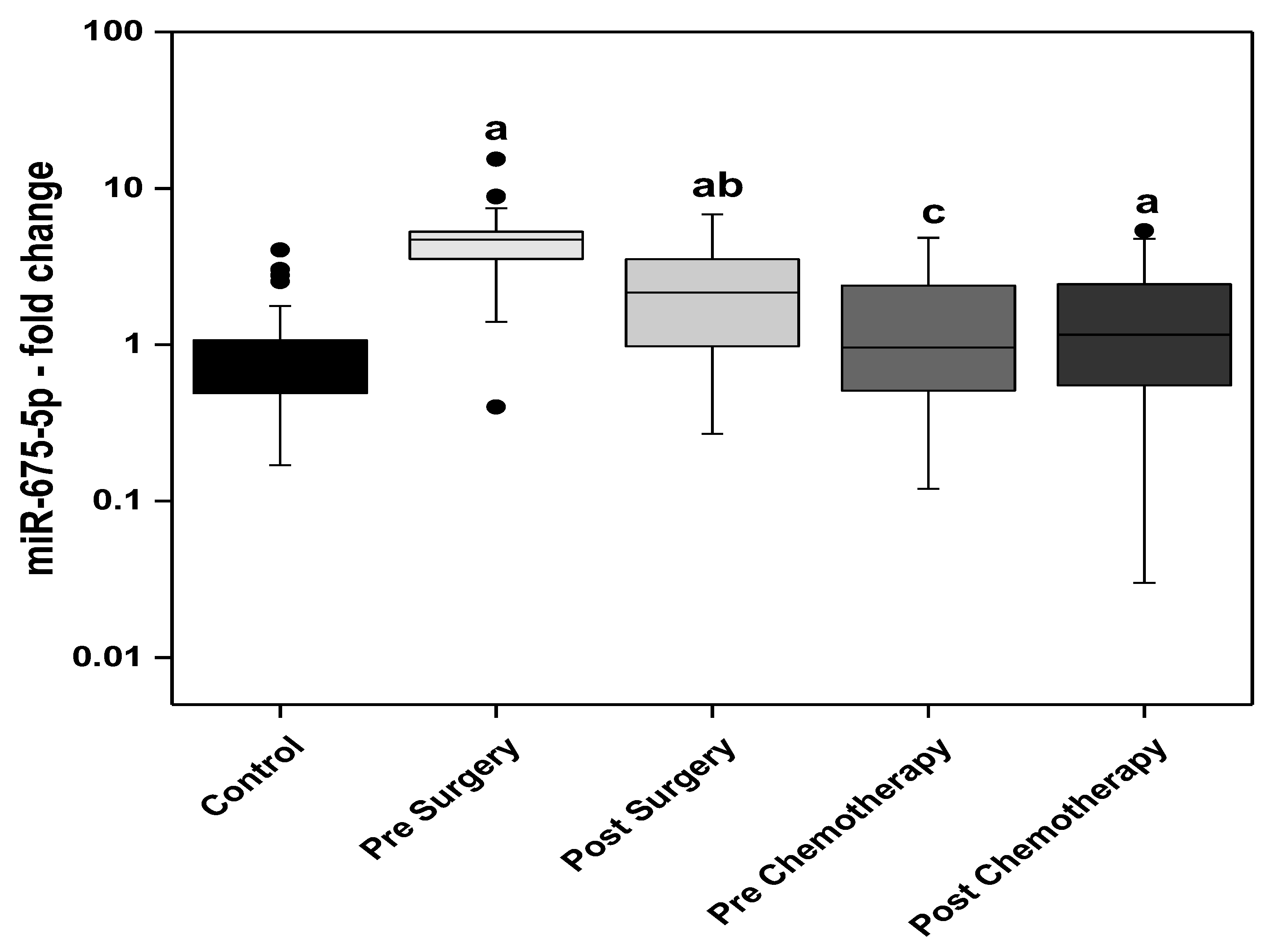
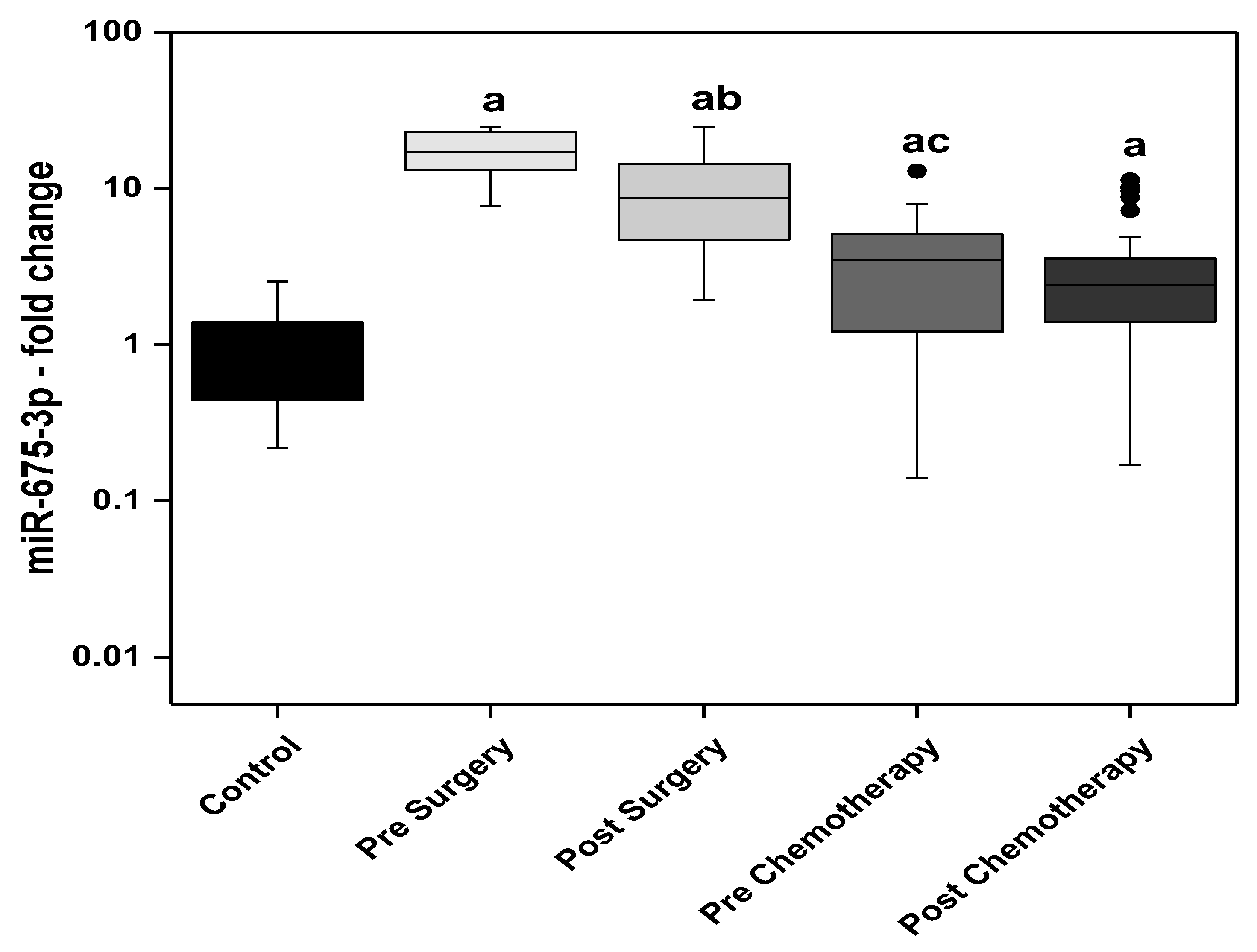
Findings of the present study showed an increase in the levels of miRNA descendants of H19; miR-675-5p and miR-675-3p, in the pre- and post-surgery BC patients when compared to the control group. The post-surgery levels of miR-675-5p showed a significant decline compared with the presurgery level. In the BC patients receiving adjuvant chemotherapy, the prechemotherapy levels of miR-675-5p are not statistically different from the control levels, however significantly lower than the post-surgery group’s levels. The circulating levels of miR-675-3p (passenger strand of miR-675-5p) showed more prominent increase in BC patients compared to miR-675-5p. The highest circulating levels of miR-675-3p were observed in the presurgery patients while the lowest levels were detected in the post-chemotherapy patients. The post-surgery levels were significantly lower than the presurgery. Moreover, the prechemotherapy levels were significantly lower than the post-surgery levels.
Literature regarding miR-let 7 in BC has been controversial. On one hand, let-7a is well characterized as a tumor suppressor, with downregulated levels in several solid organ cancers [
21]. It has also been linked to the chemosensitivity of cancer in vitro cell lines, where miR-let 7 has been found to be an important predictor for the clinical response to the anthracycline drug epirubicin. Hence, it has been suggested to be a therapeutic target to regulate resistance from epirubicin-based chemotherapy [
22]. Research findings indicate that lower expression of let-7a miRNA can induce chemoresistance in breast cancer by enhancing cellular apoptosis and suggest that let-7a may be used as a therapeutic target to modulate epirubicin-based chemotherapy resistance [
22]. This phenomenon, although proven in cell lines, has not yet been proven in clinical breast tumors. On the other hand, miR-let 7 levels were unexpectedly almost 11.2-fold increased in BC patients when compared with the control group. After tumor resection, levels significantly dropped to levels comparable to that of the control group [
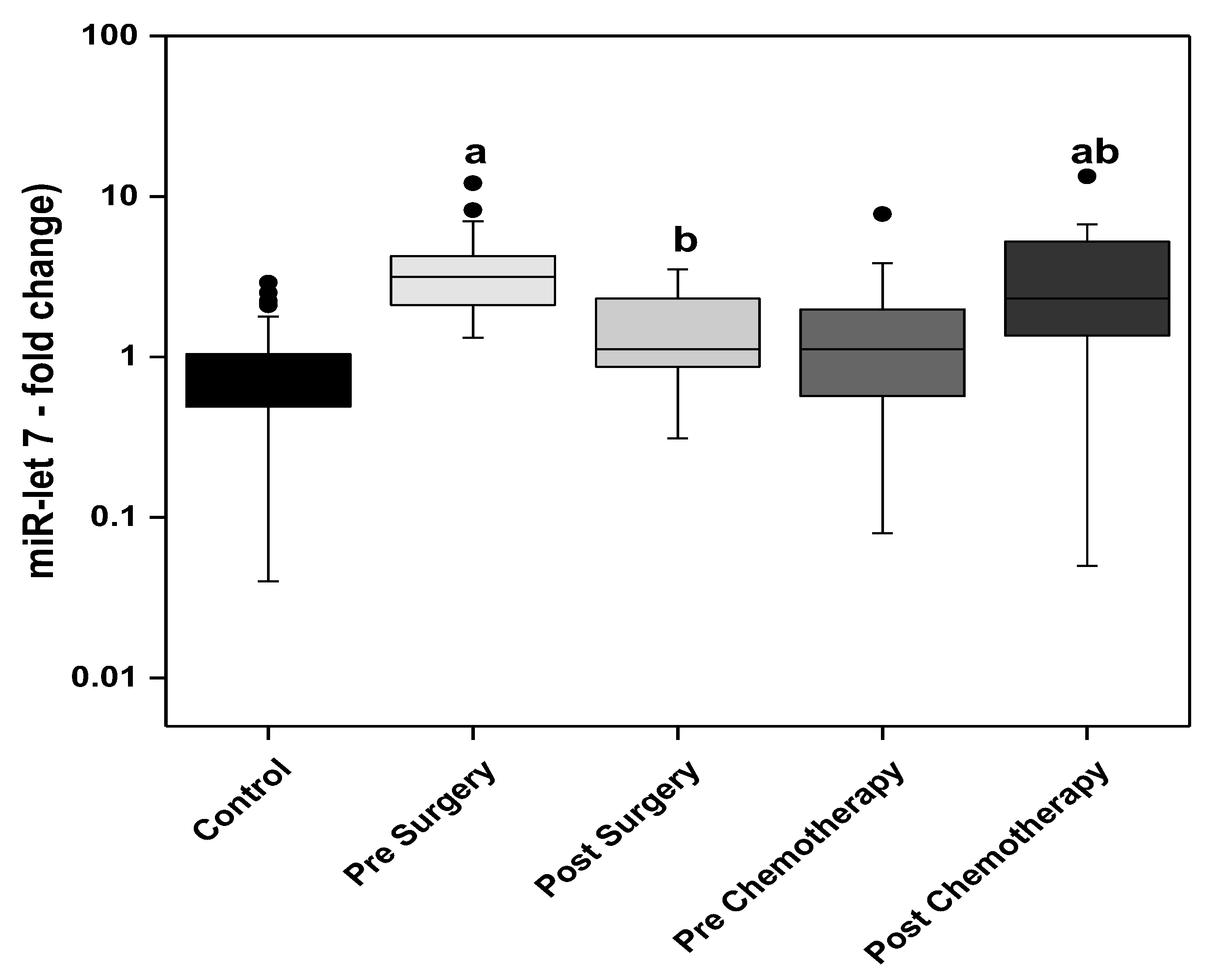
23]. These findings were in line with the results of the present study which show significantly increased levels of circulating miR-let 7 in the presurgery and post-chemotherapy BC patients when compared to the control group. Although initially high in the BC patients, surgery brought upon a significant reduction. In contrast, chemotherapy brought about a significant increase in the levels of miR-let 7 in the BC group receiving adjuvant chemotherapy.
The finding that miR-let 7 was greatly increased in the blood of BC patients raises an interesting question concerning the origin of the circulating miRNAs. The mechanism of delivery of tumor associated ncRNAs into the bloodstream remains unknown. Two hypotheses were raised by Slack et al. in a report. Primarily, tumor cell lyses and death releases ncRNAs into the circulation. A second hypothesis is that tumor cells expel ncRNAs across new blood vessels and pour into the circulation of the microenvironment of the tumor [
24]. The upregulation after chemotherapy could indicate that the patients in this study showed a hypothetically good response to chemotherapy and could possess a good prognosis for their treatment, yet the upregulation in the non-intervened BC patients could be a feedback mechanism for the cells in response to the elevated H19 levels.
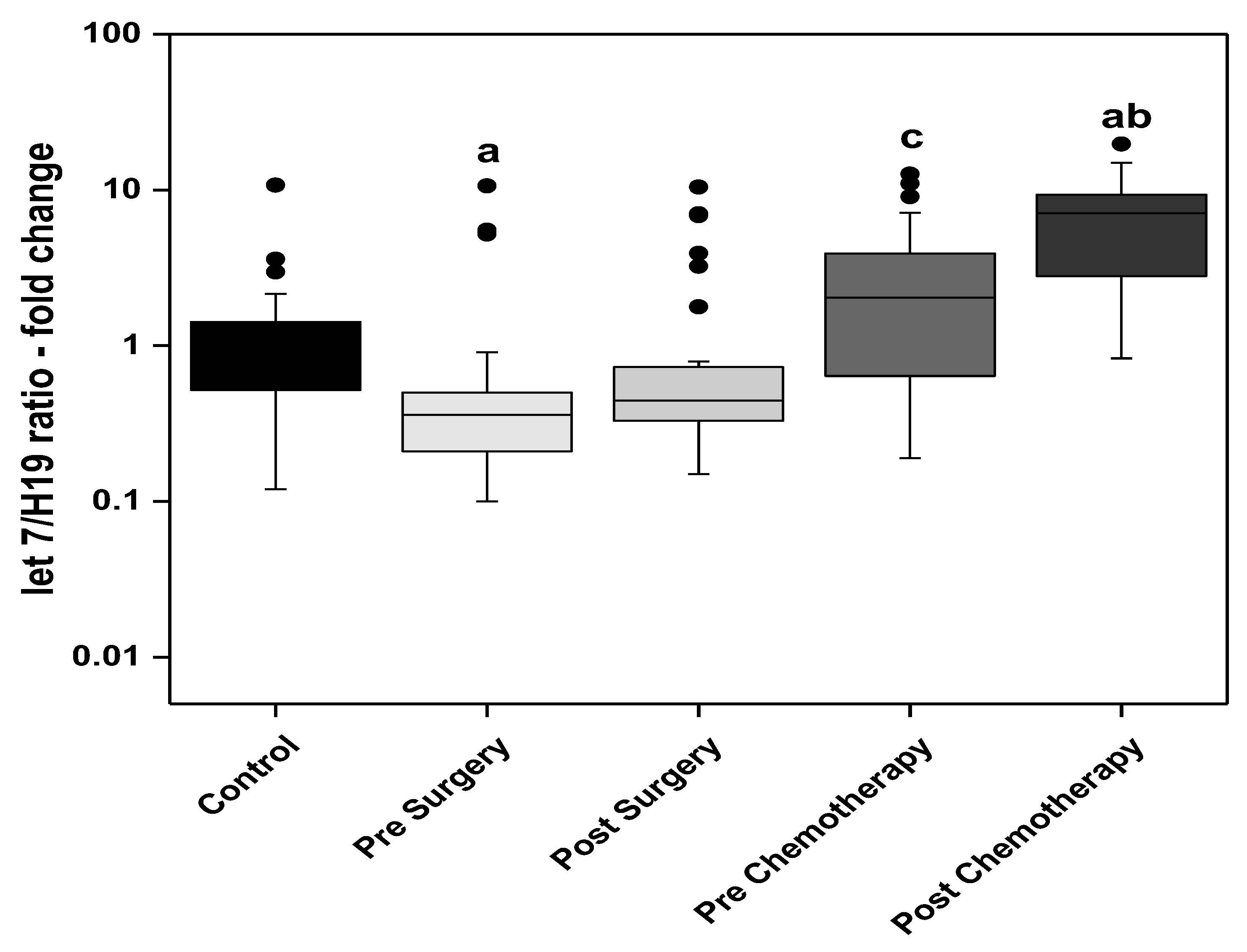
From the assumption above, a consequent ratio was derived from the present work of miR-let 7 to H19 demonstrating a theoretical tumor suppressor to oncogene level analysis. Statistical analysis of this ratio revealed that the presurgery group had a significantly lower ratio when compared with the control group. This ratio increased significantly in the prechemotherapy group when compared to the post-surgery group and showed a further statistically significant increased after receiving chemotherapy, also becoming significantly higher than the control group in the post-chemotherapy group.
The results of the present study, in terms of the effect of surgery on the levels of the ncRNAs, revealed a significant decrease in the levels of CA 15-3, H19, miR-675-5p, miR-675-3p, and miR-let 7. The ratio of miR-let 7 to H19 showed no statistical difference after surgery. Chemotherapy on the other hand, showed no statistically significant difference between the prechemotherapy and post-chemotherapy levels of H19, miR-675-5p and miR-675-3p. MiR-let 7 levels as well as let 7 to H19 ratio showed a statistically significant rise in the post-chemotherapy group when compared with the prechemotherapy group.
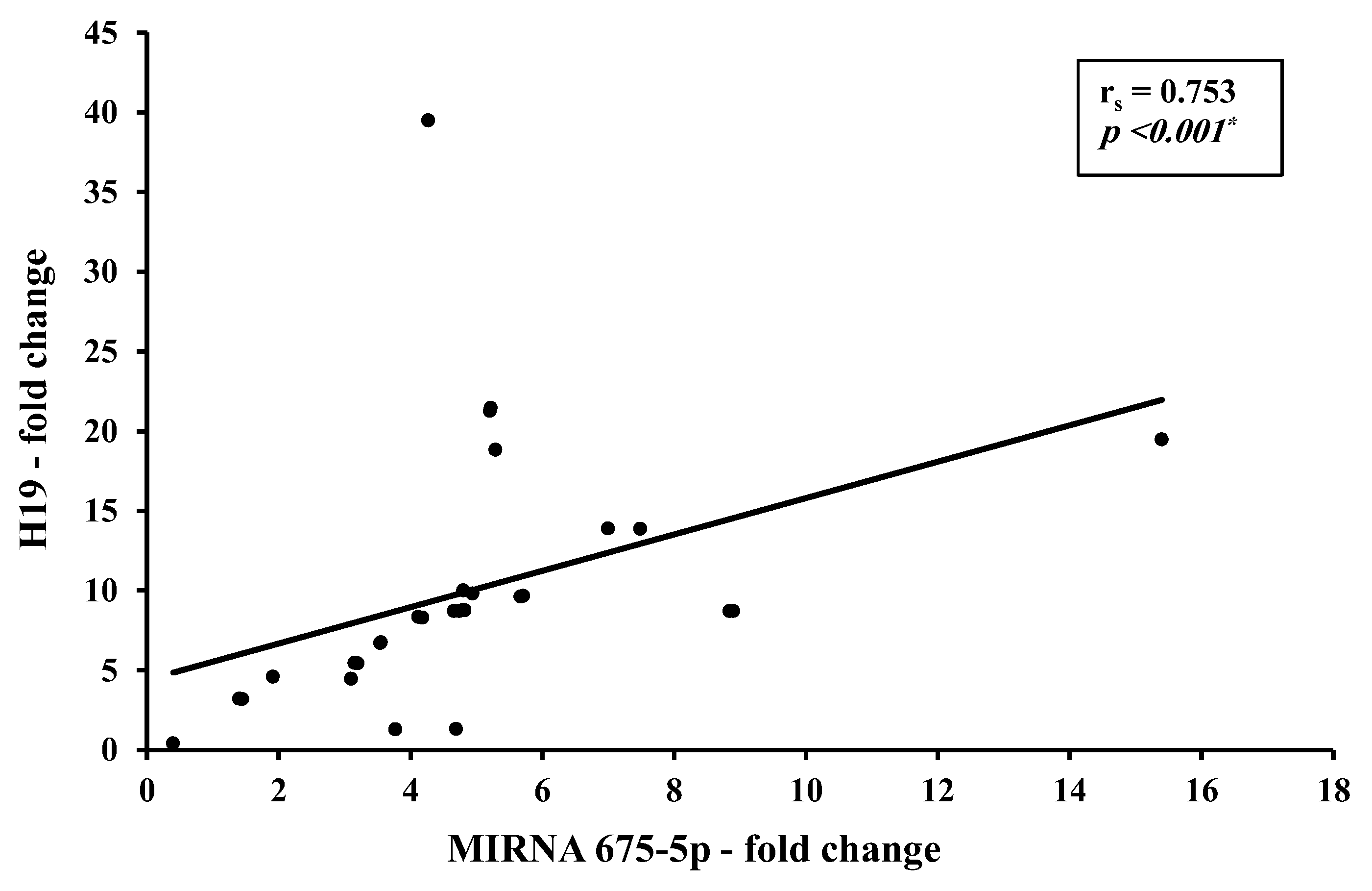
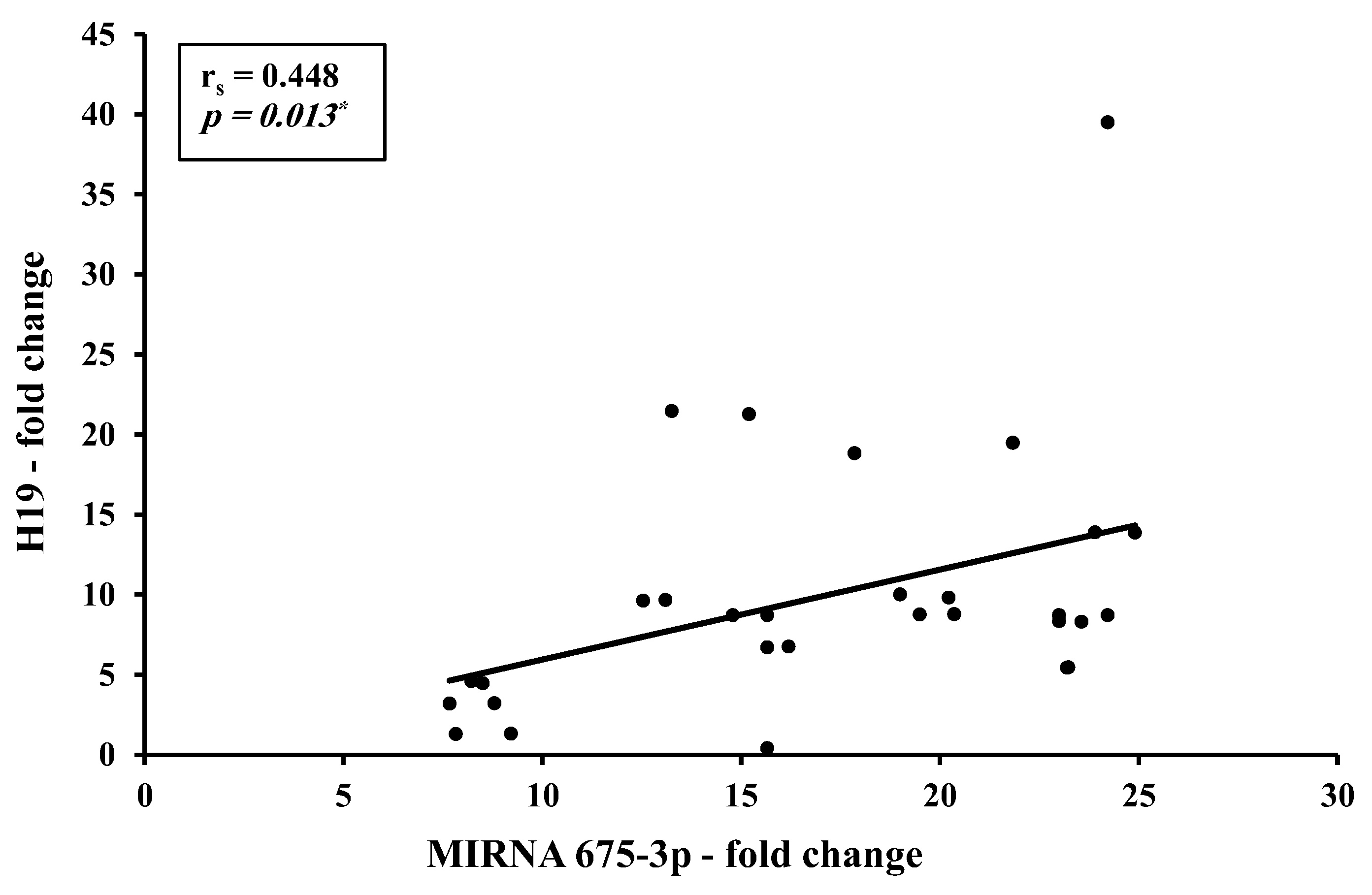
Correlation studies from the present work identified a direct strong correlation between H19 and miR-675-5p (r = 0.753,
p < 0.001) and a direct moderate correlation between H19 and miR-675-3p (r = 0.448,
p < 0.05). This could be explained as an increase in precursor H19 results in a consequent increase in its descendants miR-675-5p and -3p. Although this finding agrees with most of the studies assessing the H19/ miR-675 in BC patients, a striking finding was found where opposite levels were reported with an increase in H19 accompanied by a decrease in miRNA-675 in the HER2-positive BC subgroup [
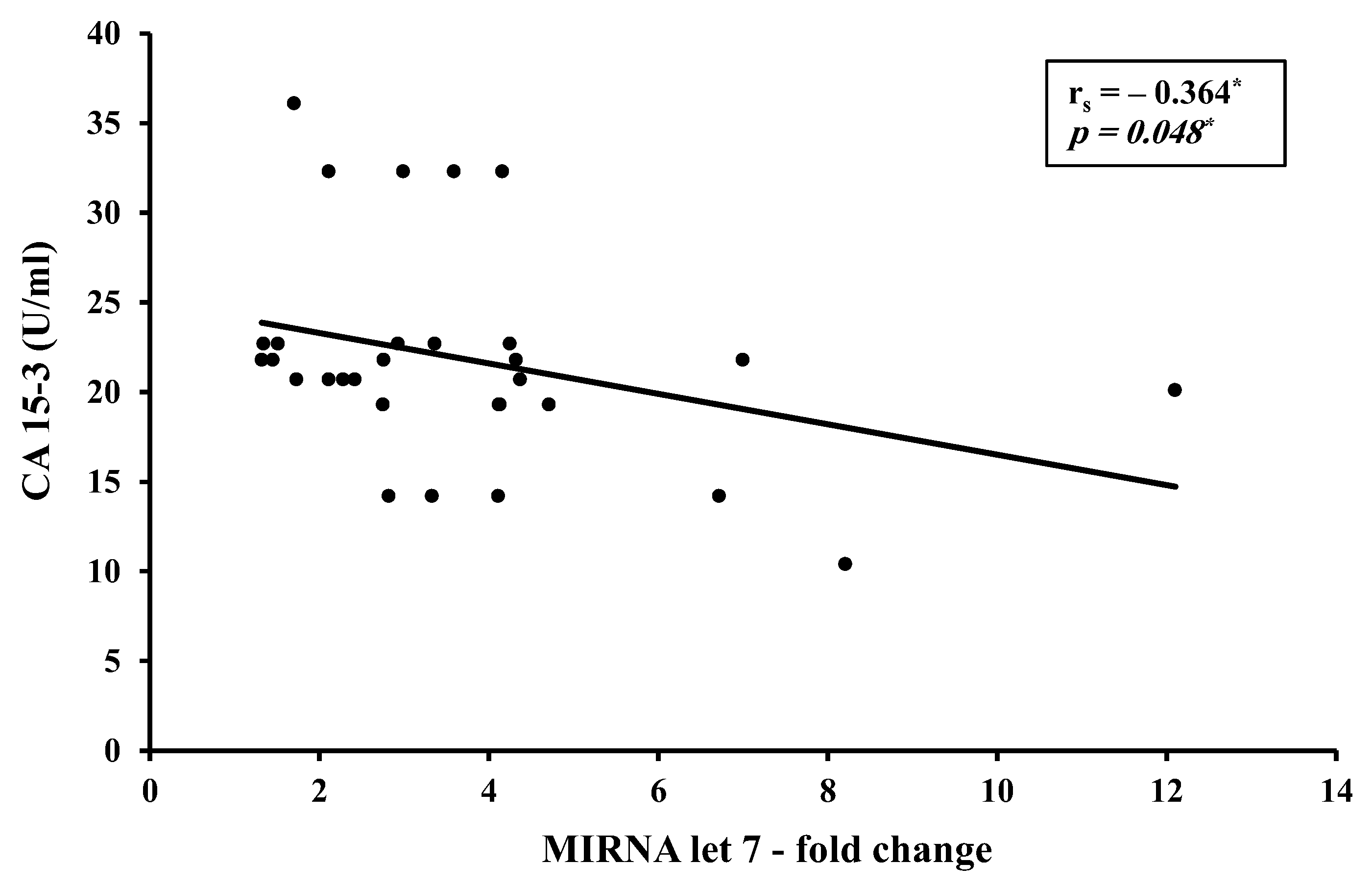
15]. No correlation was found between H19 and let7 levels in the BC in the present study, yet an inverse moderate correlation between CA 15-3 and miR-let 7 level was found (r = −0.0364,
p < 0.05). This goes in alignment with literature identifying CA 15-3 as a tumor invasion promoter and miR-let 7 as a tumor suppressor.
Relation studies were evaluated in the presurgery group assessing the effect of family history, menopause, grade, lymph invasion, tumor size, and stage. No relation was found in the levels of the ncRNAs in the present study with regards to the menopausal state, grade and stage. No relation was also found in nodal status subgroups, in agreement with a previous study performed on BC tissue of patients finding no differences between nodal status subgroups [
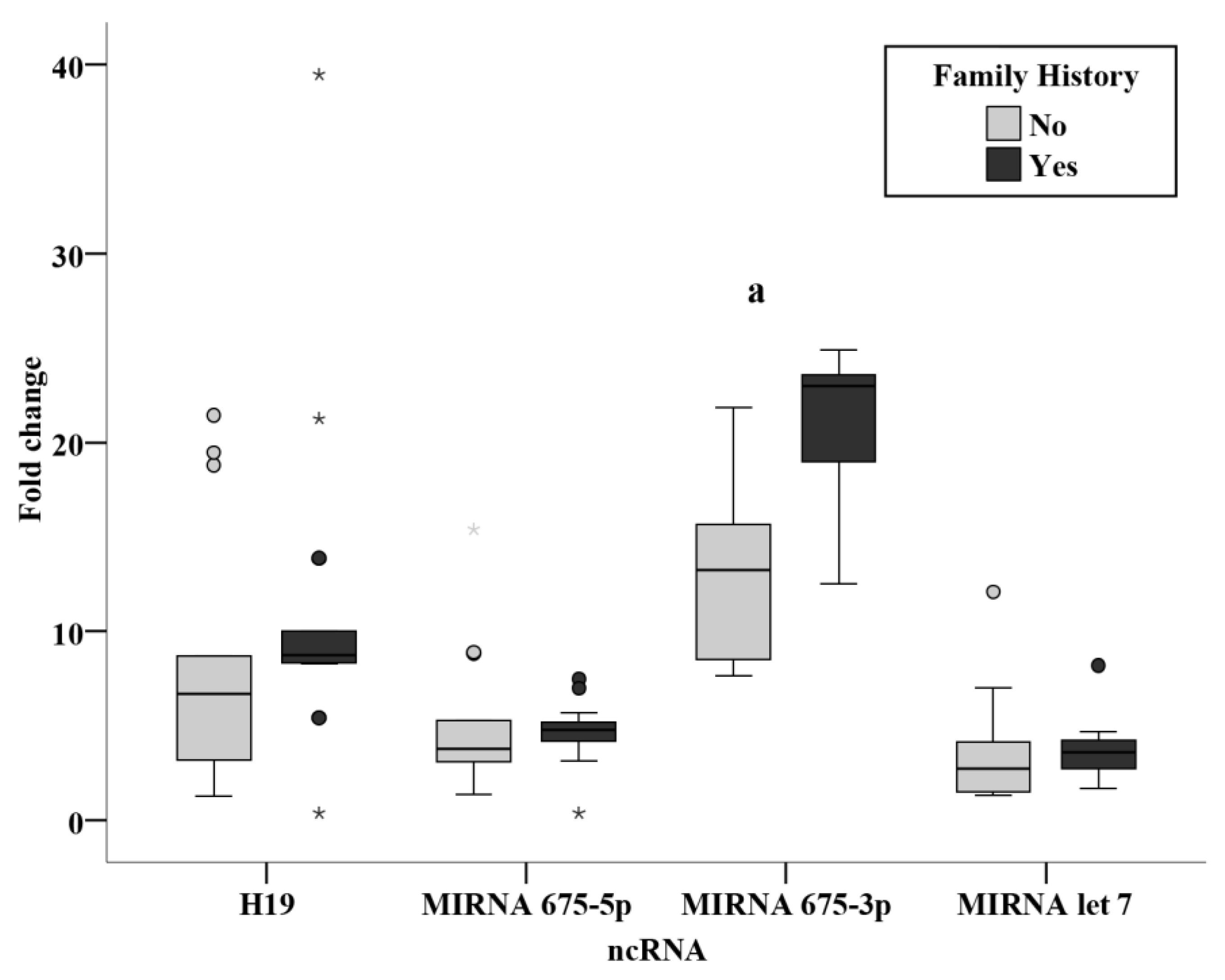
15]. The results revealed a significantly increased miR-675-3p level in patients with a positive family history of breast cancer (
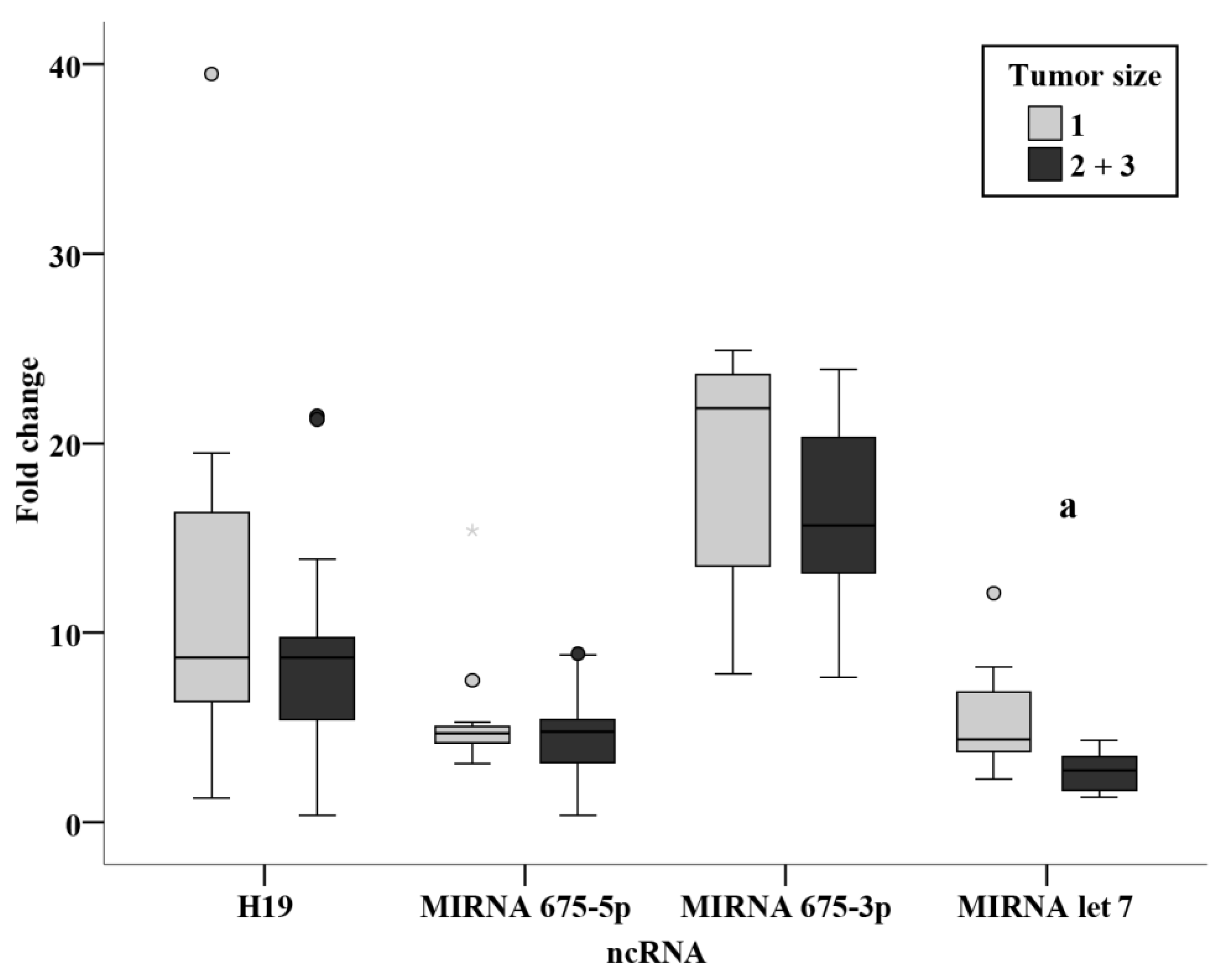
p < 0.001). From this finding, we could derive a non-invasive method for the surveillance of circulating miR-675-3p in individuals with a positive family history of BC. An inverse relation was also identified from the current study between tumor size and miR-let 7, where a significantly lower level in tumor sizes of more than 2 cm as compared with tumors of less than 2cm (
p < 0.001). This could potentially provide a more accurate estimate of tumor size before surgery, being of substantial value in neoadjuvant therapy, where tumor size could be monitored easily and directly using circulating miR-let 7 levels.
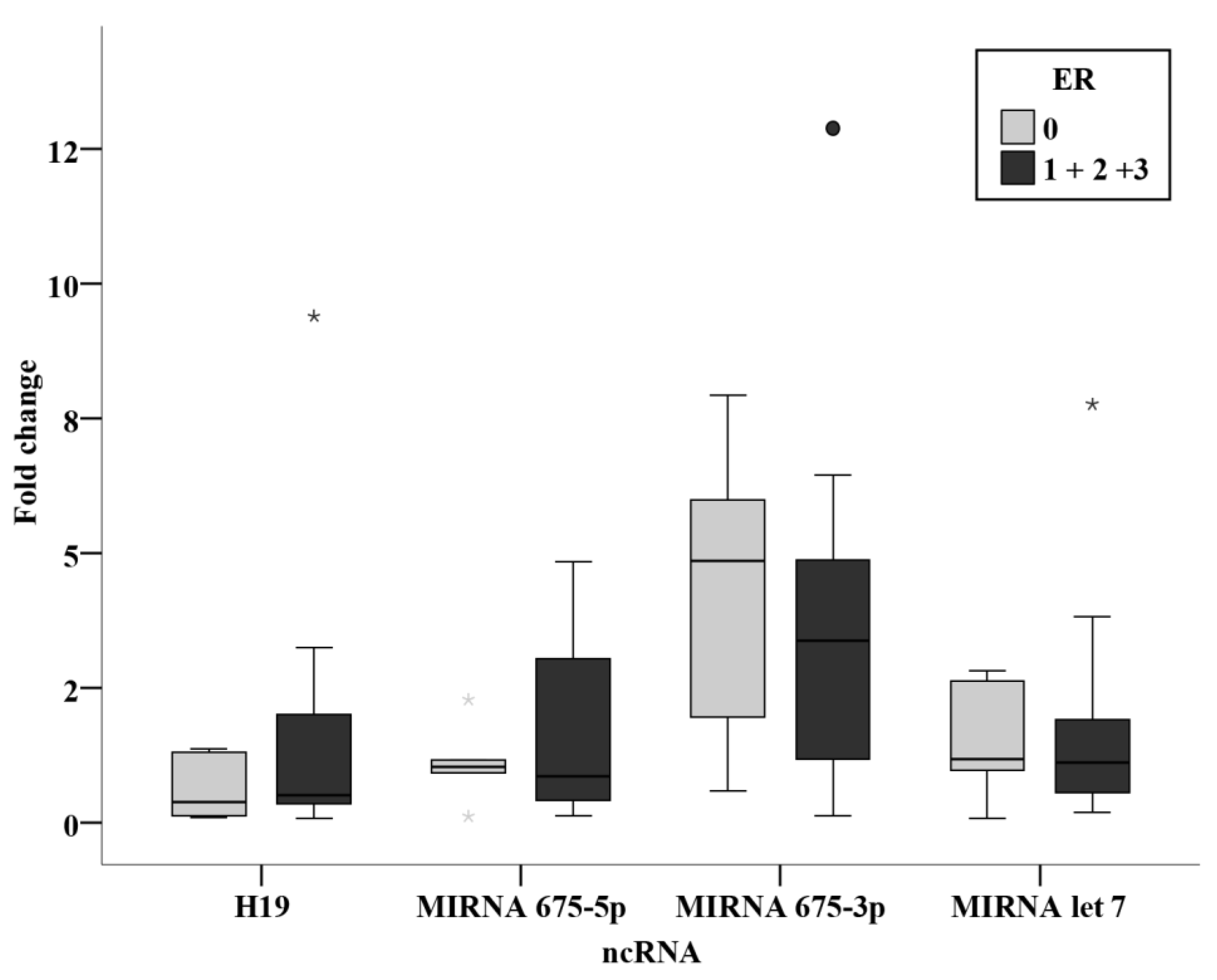
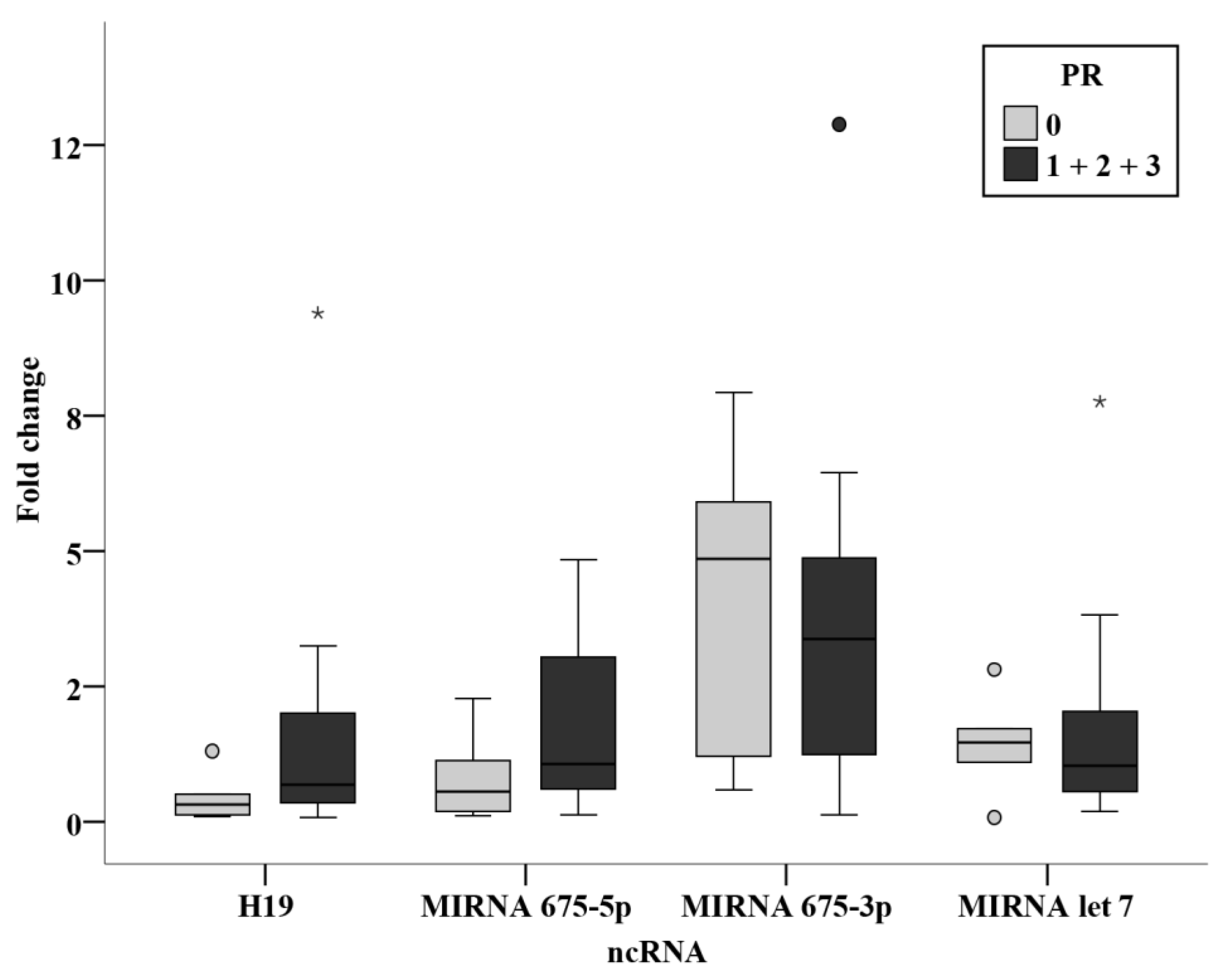
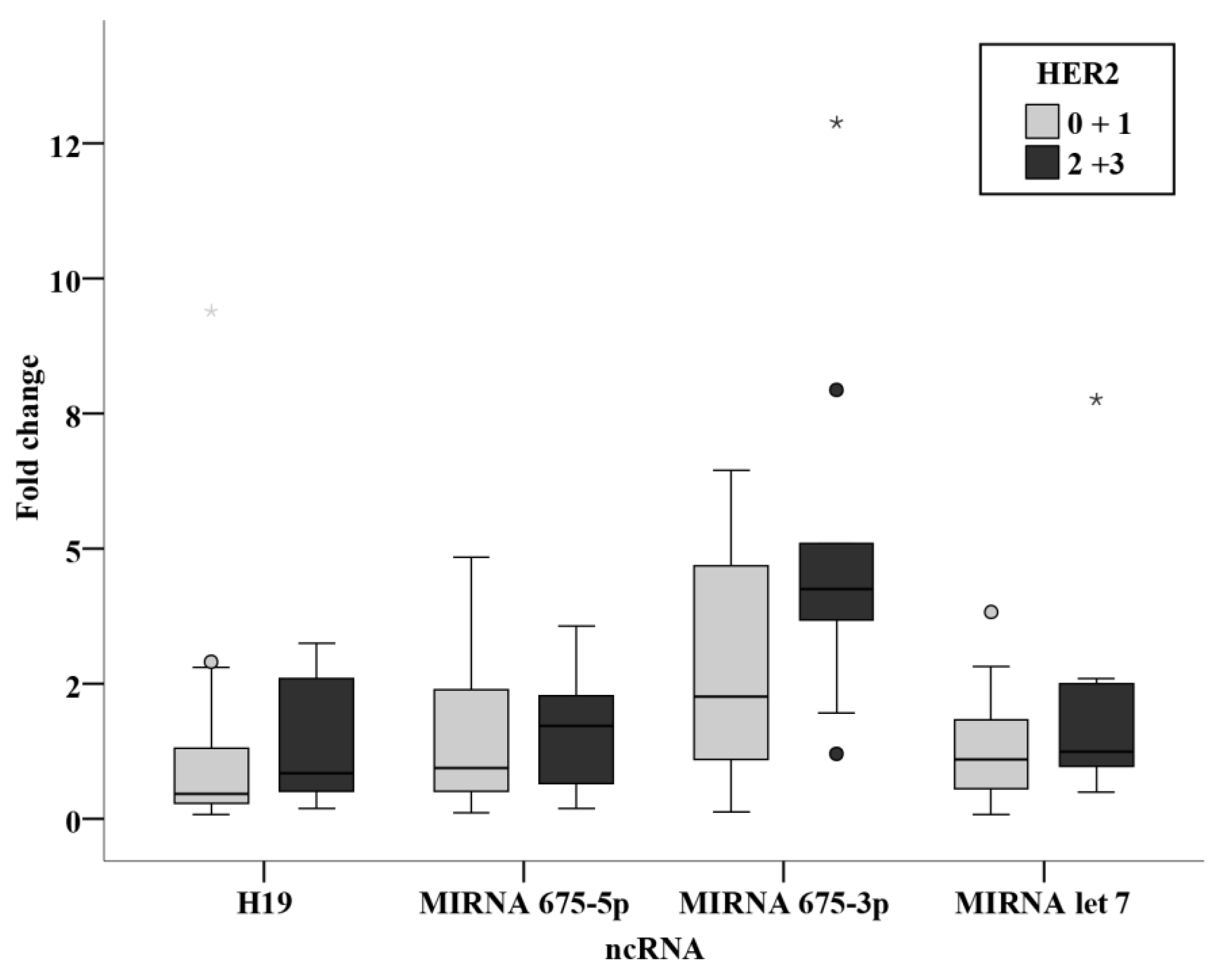
Among the chemotherapy group, relation studies relating receptor status, ER, PR, and HER2 were analyzed together with their intrinsic subtyping classification and the triple negativity. Although no statistically significant results were concluded, miR-675-3p levels were notably higher in the HER2 positive group when compared with the negative group with a significance of 0.077. This shows similar findings to the study by Müller et al. [
15], where an association was found between circulating H19 and HER2 overexpression [
15]. They were also remarkably higher in the luminal B group when compared to the luminal A group. These difference although have not proven significance in the present study, indicate that levels of miR-675-3p are higher in subgroups with worse prognosis. More conclusive results could be attained by performing the study on a larger sample size of BC patients.
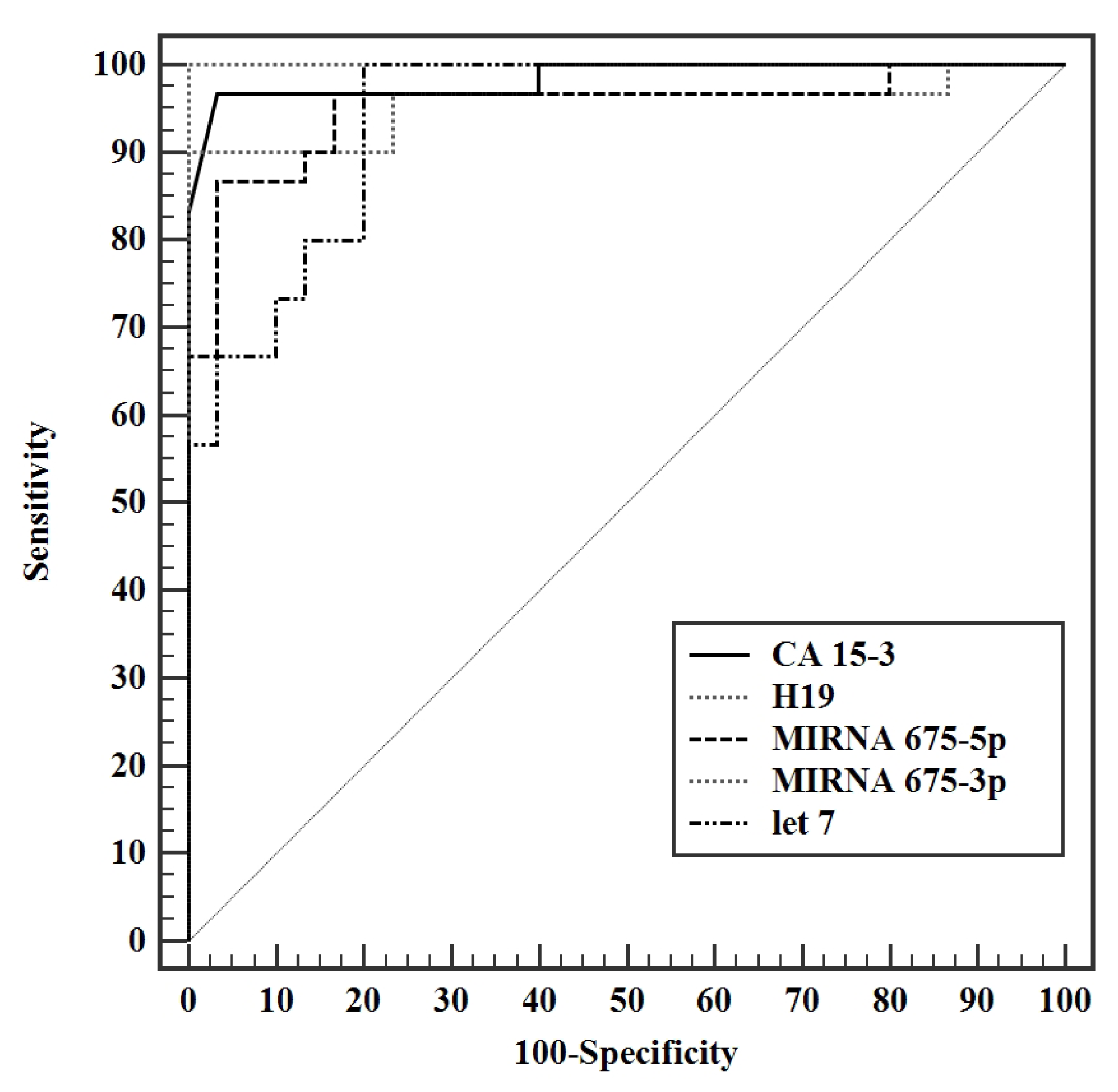
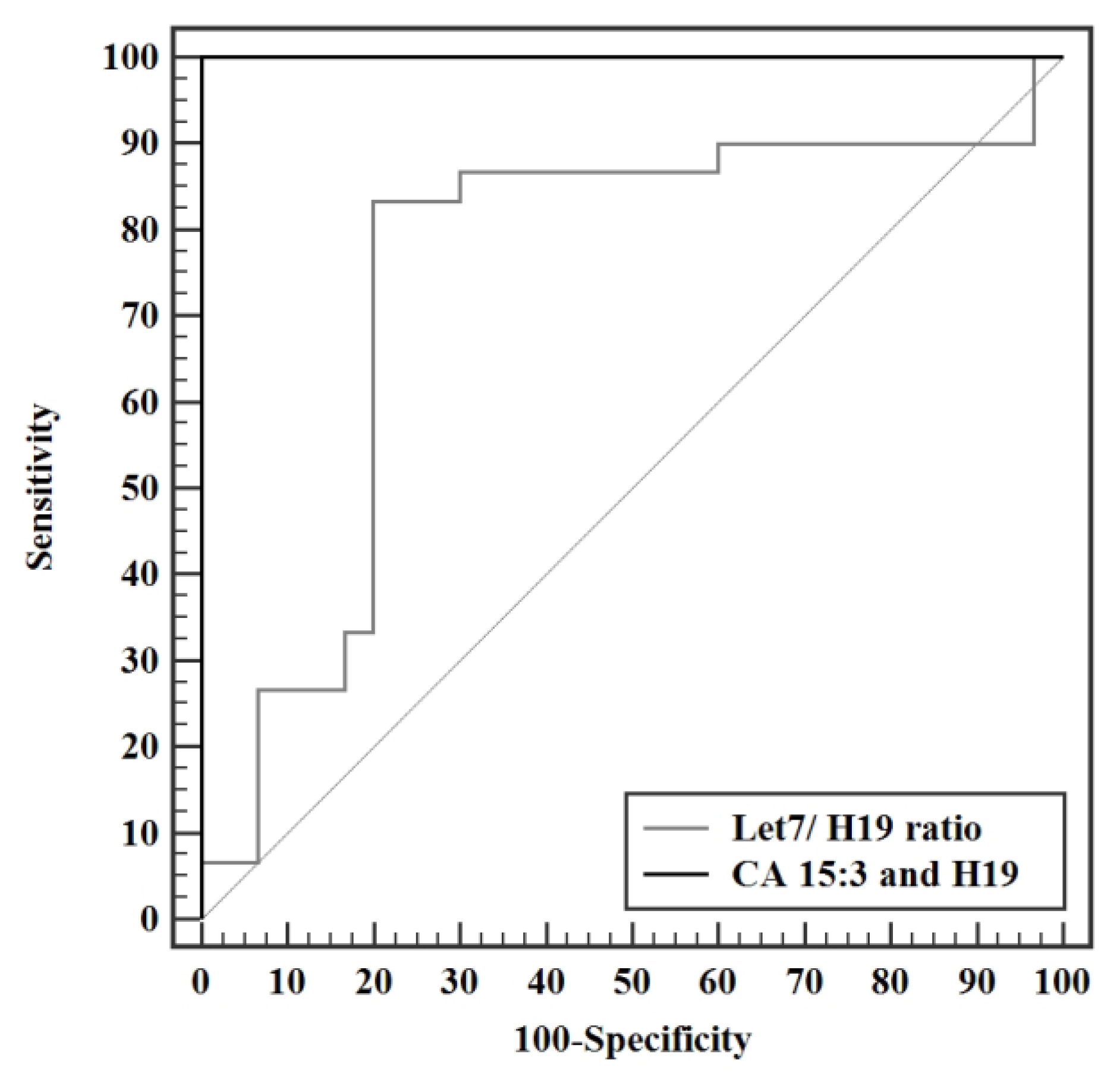
Validity analysis of the parameters measured in this study displayed a maximal AUC for miR-675-3p at a cut off value of >2.53, with an AUC of 1.000 and 100% sensitivity, specificity, PPV, and NPV. CA 15-3 produced an AUC of 0.984 (95% CI: 0.957—1.012) with a cut of value >13.1 U/mL, having a sensitivity and specificity of 96.7% and 93.3% respectively. Although exhibiting an excellent sensitivity and specificity in this study, a cut off value of 13.1 U/mL is not a reflection of the acceptable reference level used by the laboratory standards. Analysis of H19 shortly followed with an AUC of 0.956 (95% CI: 0.895—1.016) with a cutoff value of >1.65 and a sensitivity and specificity of 90.0 and 86.67 respectively, making it a very strong diagnostic tool for BC. MiR-675-5p produced an AUC of 0.951 (95% CI 0.893—1.009) with a cut off value of >1.45, a sensitivity of 90%, and specificity of 83.3%. Let 7 exhibited an AUC of 0.941 (95% CI: 0.887—0.995) at a cut off value > 1.32 with a sensitivity and specificity of 96.67% and 80%, respectively. The let 7/ H19 index yielded a weaker diagnostic power with an AUC of 0.749 (95% CI: 0.613—0.885) with a cut off value of ≤0.51, sensitivity of 83.3% and specificity of 80%. The combination of the conventional CA 15-3 with the H19 in the present study further enhanced the discriminative power of this test, producing a viable complement to current BC detection strategies, yielding an AUC of 1.000 with 100% sensitivity, specificity, PPV, and NPV. In conclusion, the entire panel of ncRNAs in this study can potentially act as novel biomarkers whether alone or combined in the diagnosis of BC. Surgery results in a significant drop in the levels of all H19, miR-675-5p, miR-675-3p, and miR-let 7. Adjuvant chemotherapy did not result in a profound effect on the levels of ncRNAs in this study, yet it resulted in a statistically significant increase in the level of miR-let 7. Significantly increased miR-675-3p was associated with a positive family history of BC, making it a potential tool for assessing the onset of disease in females with a family history of BC. Elevated miR-let 7 levels were associated with smaller tumor sizes and, if validated, could provide a non-invasive method for tumor size surveillance.
The present study was not free from limitations. Results could be further validated and verified by adopting a larger sample size to obtain a more representative significance that is true to value, measuring the levels of ncRNAs in another group of subjects with benign tumors, following through with the same non-intervened BC patients, collecting blood before and after surgery, as well as before and after chemotherapy for the same patients, and assessing the levels of the studied panel of ncRNAs in patients receiving neoadjuvant chemotherapy followed by surgery.