The Management of Asymptomatic Congenital Pulmonary Airway Malformation: Results of a European Delphi Survey
Abstract
:1. Introduction
2. Materials and Methods
Data Analysis
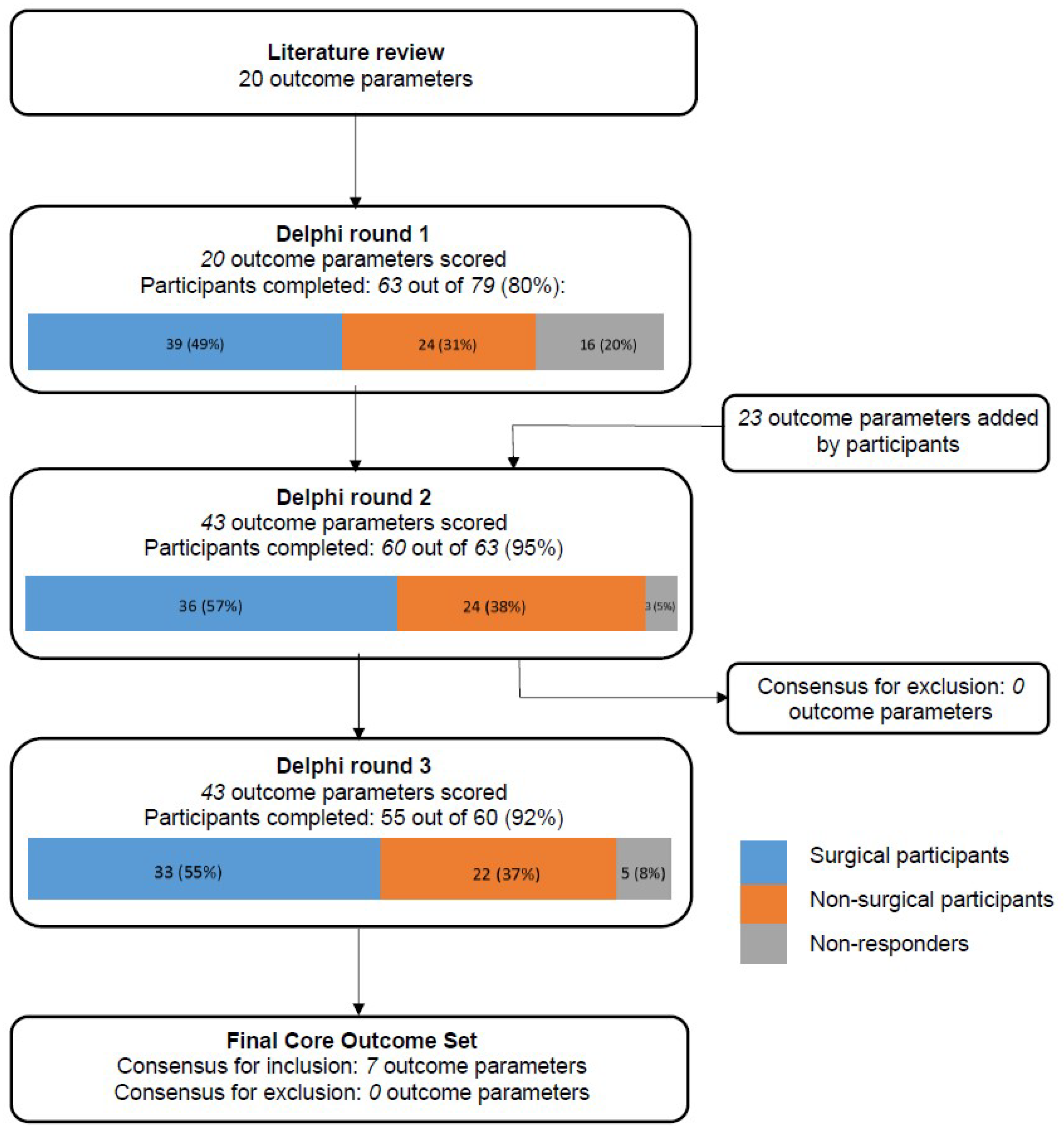
3. Results
3.1. Round 1
3.2. Round 2
3.3. Round 3
3.4. Final Core Outcome Set
3.5. Attrition Rate and Attrition Bias
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Morini, F.; Zani, A.; Conforti, A.; van Heurn, E.; Eaton, S.; Puri, P.; Rintala, R.; Lukac, M.; Kuebler, J.F.; Friedmacher, F.; et al. Current Management of Congenital Pulmonary Airway Malformations: A “European Pediatric Surgeons’ Association” Survey. Eur. J. Pediatr. Surg. 2018, 28, 1–5. [Google Scholar] [CrossRef]
- Stanton, M. The argument for a non-operative approach to asymptomatic lung lesions. Semin. Pediatr. Surg. 2015, 24, 183–186. [Google Scholar] [CrossRef]
- Singh, R.; Davenport, M. The argument for operative approach to asymptomatic lung lesions. Semin. Pediatr. Surg. 2015, 24, 187–195. [Google Scholar] [CrossRef]
- Hermelijn, S.M.; Elders, B.B.L.J.; Ciet, P.; Wijnen, R.M.H.; Tiddens, H.; Schnater, J.M. A clinical guideline for structured assessment of CT-imaging in congenital lung abnormalities. Paediatr. Respir. Rev. 2021, 37, 80–88. [Google Scholar] [CrossRef]
- Stanton, M.; Njere, I.; Ade-Ajayi, N.; Patel, S.; Davenport, M. Systematic review and meta-analysis of the postnatal management of congenital cystic lung lesions. J. Pediatr. Surg. 2009, 44, 1027–1033. [Google Scholar] [CrossRef]
- MacSweeney, F.; Papagiannopoulos, K.; Goldstraw, P.; Sheppard, M.N.; Corrin, B.; Nicholson, A.G. An assessment of the expanded classification of congenital cystic adenomatoid malformations and their relationship to malignant transformation. Am. J. Surg. Pathol. 2003, 27, 1139–1146. [Google Scholar] [CrossRef]
- Baird, R.; Puligandla, P.S.; Laberge, J.M. Congenital lung malformations: Informing best practice. Semin. Pediatr. Surg. 2014, 23, 270–277. [Google Scholar] [CrossRef]
- Kunisaki, S.M.; Lal, D.R.; Saito, J.M.; Fallat, M.E.; St Peter, S.D.; Fox, Z.D.; Heider, A.; Chan, S.S.; Boyd, K.P.; Burns, R.C.; et al. Pleuropulmonary Blastoma in Pediatric Lung Lesions. Pediatrics 2021, 147, e2020028357. [Google Scholar] [CrossRef]
- Hsieh, C.C.; Chao, A.S.; Chang, Y.L.; Kuo, D.M.; Hsieh, T.T.; Hung, H.T. Outcome of congenital cystic adenomatoid malformation of the lung after antenatal diagnosis. Int. J. Gynecol. Obstet. 2005, 89, 99–102. [Google Scholar] [CrossRef]
- Cook, J.; Chitty, L.S.; De Coppi, P.; Ashworth, M.; Wallis, C. The natural history of prenatally diagnosed congenital cystic lung lesions: Long-term follow-up of 119 cases. Arch. Dis Child. 2017, 102, 798–803. [Google Scholar] [CrossRef]
- Benjamin, D.R.; Cahill, J.L. Bronchioloalveolar carcinoma of the lung and congenital cystic adenomatoid malformation. Am. J. Clin. Pathol. 1991, 95, 889–892. [Google Scholar] [CrossRef] [Green Version]
- Papagiannopoulos, K.A.; Sheppard, M.; Bush, A.P.; Goldstraw, P. Pleuropulmonary blastoma: Is prophylactic resection of congenital lung cysts effective? Ann. Thorac. Surg. 2001, 72, 604–605. [Google Scholar] [CrossRef]
- Peters, R.T.; Burge, D.M.; Marven, S.S. Congenital lung malformations: An ongoing controversy. Ann. R. Coll. Surg. Engl. 2013, 95, 144–147. [Google Scholar] [CrossRef] [Green Version]
- Eber, E. Antenatal diagnosis of congenital thoracic malformations: Early surgery, late surgery, or no surgery? Semin. Respir. Crit. Care Med. 2007, 28, 355–366. [Google Scholar] [CrossRef]
- David, M.; Lamas-Pinheiro, R.; Henriques-Coelho, T. Prenatal and Postnatal Management of Congenital Pulmonary Airway Malformation. Neonatology 2016, 110, 101–115. [Google Scholar] [CrossRef]
- Kantor, N.; Wayne, C.; Nasr, A. Symptom development in originally asymptomatic CPAM diagnosed prenatally: A systematic review. Pediatr. Surg. Int. 2018, 34, 613–620. [Google Scholar] [CrossRef]
- Criss, C.N.; Musili, N.; Matusko, N.; Baker, S.; Geiger, J.D.; Kunisaki, S.M. Asymptomatic congenital lung malformations: Is nonoperative management a viable alternative? J. Pediatr. Surg. 2018, 53, 1092–1097. [Google Scholar] [CrossRef]
- Kapralik, J.; Wayne, C.; Chan, E.; Nasr, A. Surgical versus conservative management of congenital pulmonary airway malformation in children: A systematic review and meta-analysis. J. Pediatr. Surg. 2016, 51, 508–512. [Google Scholar] [CrossRef]
- Tocchioni, F.; Lombardi, E.; Ghionzoli, M.; Ciardini, E.; Noccioli, B.; Messineo, A. Long-term lung function in children following lobectomy for congenital lung malformation. J. Pediatr. Surg. 2017, 52, 1891–1897. [Google Scholar] [CrossRef]
- Spoel, M.; van de Ven, K.P.; Tiddens, H.A.W.M.; Hop, W.C.J.; Wijnen, R.M.H.; Tibboel, D.; Ijsselstijn, H. Lung function of infants with congenital lung lesions in the first year of life. Neonatology 2013, 103, 60–66. [Google Scholar] [CrossRef] [Green Version]
- Hijkoop, A.; van Schoonhoven, M.M.; van Rosmalen, J.; Tibboel, D.; van der Cammen-van Zijp, M.H.M.; Pijnenburg, M.W.; Cohen-Overbeek, T.E.; Schnater, J.M.; IJsselstijn, H. Lung function, exercise tolerance, and physical growth of children with congenital lung malformations at 8 years of age. Pediatr. Pulmonol. 2019, 54, 1326–1334. [Google Scholar] [CrossRef] [Green Version]
- Naito, Y.; Beres, A.; Lapidus-Krol, E.; Ratjen, F.; Langer, J.C. Does earlier lobectomy result in better long-term pulmonary function in children with congenital lung anomalies? A prospective study. J. Pediatr. Surg. 2012, 47, 852–856. [Google Scholar] [CrossRef]
- Dincel, A.; Yilmaz Yegit, C.; Ergenekon, A.P.; Erdem Eralp, E.; Gokdemir, Y.; Kiyan, G.; Karadag, B. Long-term respiratory outcomes of post-op congenital lung malformations. Pediatr. Int. 2020, 63, 704–709. [Google Scholar] [CrossRef]
- Calzolari, F.; Braguglia, A.; Valfrè, L.; Dotta, A.; Bagolan, P.; Morini, F. Outcome of infants operated on for congenital pulmonary malformations. Pediatr. Pulmonol. 2016, 51, 1367–1372. [Google Scholar] [CrossRef]
- Pinter, A.; Kalman, A.; Karsza, L.; Verebely, T.; Szemledy, F. Long-term outcome of congenital cystic adenomatoid malformation. Pediatr. Surg. Int. 1999, 15, 332–335. [Google Scholar] [CrossRef]
- Williamson, P.R.; Altman, D.G.; Bagley, H.; Barnes, K.L.; Blazeby, J.M.; Brookes, S.T.; Clarke, M.; Gargon, E.; Gorst, S.; Harman, N.; et al. The COMET Handbook: Version 1.0. Trials 2017, 18, 280. [Google Scholar] [CrossRef] [Green Version]
- Knaapen, M.; Hall, N.J.; van der Lee, J.H.; Butcher, N.J.; Offringa, M.; Van Heurn, E.W.E.; Bakx, R.; Gorter, R.R. Establishing a core outcome set for treatment of uncomplicated appendicitis in children: Study protocol for an international Delphi survey. BMJ Open 2019, 9, e028861. [Google Scholar] [CrossRef] [Green Version]
- Sherratt, F.C.; Eaton, S.; Walker, E.; Beasant, L.; Blazeby, J.M.; Young, B.; Crawley, E.; Wood, W.W.; Hall, N.J. Development of a core outcome set to determine the overall treatment success of acute uncomplicated appendicitis in children: A study protocol. BMJ Paediatr Open 2017, 1, e000151. [Google Scholar] [CrossRef] [Green Version]
- Blackwood, B.; Ringrow, S.; Clarke, M.; Marshall, J.C.; Connolly, B.; Rose, L.; McAuley, D.F. A Core Outcome Set for Critical Care Ventilation Trials. Crit. Care Med. 2019, 47, 1324–1331. [Google Scholar] [CrossRef]
- Hermelijn, S.; Kersten, C.; Mullassery, D.; Muthialu, N.; Cobanoglu, N.; Gartner, S.; Bagolan, P.; Mesas Burgos, C.; Sgro, A.; Heyman, S.; et al. Development of a core outcome set for congenital pulmonary airway malformations: Study protocol of an international Delphi survey. BMJ Open 2021, 11, e044544. [Google Scholar] [CrossRef]
- Eyes, D. Welphi-Home. Available online: https://www.welphi.com/en/Home.html (accessed on 16 February 2021).
- de Magalhães, S.T. The European Union’s General Data Protection Regulation (GDPR). Available online: https://www.semanticscholar.org/paper/The-European-Union%E2%80%99s-General-Data-Protection-(GDPR)-Magalhaes/6e9933ee4eb634ba691903ccbc83c9abd871747b (accessed on 16 February 2021).
- Sinha, I.P.; Smyth, R.L.; Williamson, P.R. Using the Delphi technique to determine which outcomes to measure in clinical trials: Recommendations for the future based on a systematic review of existing studies. PLoS Med. 2011, 8, e1000393. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sauvat, F.; Michel, J.L.; Benachi, A.; Emond, S.; Revillon, Y. Management of asymptomatic neonatal cystic adenomatoid malformations. J. Pediatr. Surg. 2003, 38, 548–552. [Google Scholar] [CrossRef] [PubMed]
- Davenport, M.; Warne, S.A.; Cacciaguerra, S.; Patel, S.; Greenough, A.; Nicolaides, K. Current outcome of antenally diagnosed cystic lung disease. J. Pediatr. Surg. 2004, 39, 549–556. [Google Scholar] [CrossRef]
- Miller, J.A.; Corteville, J.E.; Langer, J.C. Congenital cystic adenomatoid malformation in the fetus: Natural history and predictors of outcome. J. Pediatr. Surg. 1996, 31, 805–808. [Google Scholar] [CrossRef]
- Bunduki, V.; Ruano, R.; da Silva, M.M.; Miguelez, J.; Miyadahira, S.; Maksoud, J.G.; Zugaib, M. Prognostic factors associated with congenital cystic adenomatoid malformation of the lung. Prenat. Diagn. 2000, 20, 459–464. [Google Scholar] [CrossRef]
- Mallmann, M.R.; Graham, V.; Rösing, B.; Gottschalk, I.; Müller, A.; Gembruch, U.; Geipel, A.; Berg, C. Thoracoamniotic Shunting for Fetal Hydrothorax: Predictors of Intrauterine Course and Postnatal Outcome. Fetal Diagn. Ther. 2017, 41, 58–65. [Google Scholar] [CrossRef]
- Shulman, R.; Sparks, T.N.; Gosnell, K.; Blat, C.; Norton, M.E.; Lee, H.; Gonzalez-Velez, J.; Goldstein, R.B. Fetal Congenital Pulmonary Airway Malformation: The Role of an Objective Measurement of Cardiomediastinal Shift. Am. J. Perinatol. 2019, 36, 225–232. [Google Scholar]
- Aziz, D.; Langer, J.C.; Tuuha, S.E.; Ryan, G.; Ein, S.H.; Kim, P.C. Perinatally diagnosed asymptomatic congenital cystic adenomatoid malformation: To resect or not? J. Pediatr. Surg. 2004, 39, 329–334. [Google Scholar] [CrossRef]
- Hermelijn, S.M.; Dragt, O.V.; Bosch, J.J.; Hijkoop, A.; Riera, L.; Ciet, P.; Wijnen, R.M.H.; Schnater, J.M.; Tiddens, H. Congenital lung abnormality quantification by computed tomography: The CLAQ method. Pediatr. Pulmonol. 2020, 55, 3152–3161. [Google Scholar] [CrossRef]
- Ryu, J.H.; Tian, X.; Baqir, M.; Xu, K. Diffuse cystic lung diseases. Front. Med. 2013, 7, 316–327. [Google Scholar] [CrossRef]
- Priest, J.R.; Williams, G.M.; Hill, D.A.; Dehner, L.P.; Jaffé, A. Pulmonary cysts in early childhood and the risk of malignancy. Pediatr. Pulmonol. 2009, 44, 14–30. [Google Scholar] [CrossRef]
- Nasr, A.; Himidan, S.; Pastor, A.C.; Taylor, G.; Kim, P.C. Is congenital cystic adenomatoid malformation a premalignant lesion for pleuropulmonary blastoma? J. Pediatr. Surg. 2010, 45, 1086–1089. [Google Scholar] [CrossRef]
- Oliveira, C.; Himidan, S.; Pastor, A.C.; Nasr, A.; Manson, D.; Taylor, G.; Yanchar, N.L.; Brisseau, G.; Kim, P.C. Discriminating preoperative features of pleuropulmonary blastomas (PPB) from congenital cystic adenomatoid malformations (CCAM): A retrospective, age-matched study. Eur. J. Pediatr. Surg. 2011, 21, 2–7. [Google Scholar] [CrossRef] [PubMed]
- Leblanc, C.; Baron, M.; Desselas, E.; Phan, M.H.; Rybak, A.; Thouvenin, G.; Lauby, C.; Irtan, S. Congenital pulmonary airway malformations: State-of-the-art review for pediatrician′s use. Eur. J. Pediatr. 2017, 176, 1559–1571. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.; Davies, A.; Young, A.E. Systematic review of international Delphi surveys for core outcome set development: Representation of international patients. BMJ Open 2020, 10, e040223. [Google Scholar] [CrossRef]
| Outcome Category | Outcome Parameter | Age at Measurement | Median Scoring during Round 3 | ||||
|---|---|---|---|---|---|---|---|
| Surgical Group | Non-Surgical Group | p-Value | |||||
| Respiratory Symptoms | Wheezing defined as ≥3 episodes per year | All follow-up visits | 4 | 9 | <0.000 | † | |
| Respiratory insufficiency * | All follow-up visits | 9 | 7.5 | 0.006 | |||
| Liverpool Respiratory Symptom Questionnaire (LRSQ) | All follow-up visits | 6 | 5 | 0.22 | |||
| Respiratory rate | All follow-up visits | ‡ | 6 | 6 | 0.039 | ||
| Reduced breath sounds on chest auscultation | All follow-up visits | ‡ | 6 | 6.5 | 0.037 | ||
| Infection | Infection at lesion site § | All follow-up visits | 9 | 5 | <0.001 | ||
| Parent reported hospital admission with IV antibiotics due to LRTI | All follow-up visits | 7 | 5.5 | <0.001 | |||
| Parent reported oral antibiotics due to LRTI | All follow-up visits | 6 | 5.5 | 0.2 | |||
| Chronic inflammation in resected specimens | Not applicable | ‡ | 6 | 5 | 0.569 | ||
| Parental Anxiety | Amsterdam Preoperative Anxiety and Information Scale (APAIS) | All follow-up visits | 5 | 7 | <0.001 | ||
| Visual Analog Scale (VAS) scoring | All follow-up visits | 5 | 7 | <0.001 | |||
| Quality of Life | Pediatric Quality of Life Inventory (PedsQL) | All follow-up visits | 6 | 6 | 0.747 | ||
| Anthropometric Measurements | Height for age measurements (WHO standards) | All follow-up visits | 5 | 6 | 0.004 | † | |
| Weight for height measurements (WHO standards) | All follow-up visits | 5 | 6 | 0.025 | † | ||
| Lesion Characteristics | Lesion size on first postnatal chest X-ray | <1month | 6 | 6 | 0.401 | ||
| Lesion location on CT-scan | 3–9 months | ‡ | 6 | 5 | 0.458 | ||
| Mass effect/mediastinal shift on chest x-ray | <1 month | ‡ | 8 | 8 | 0.757 | ||
| Mass effect/mediastinal shift on CT-scan | 3–9 months | ‡ | 7 | 7 | 0.844 | ||
| Mass effect/mediastinal shift on CT-scan | 2.5 years | ‡ | 7 | 7 | 0.933 | ||
| CPAM type as seen on CT | 3–9 months | ‡ | 7 | 7 | 0.607 | ||
| Systemic blood supply on CT-scan | 3–9 months | ‡ | 7 | 7 | 0.227 | ||
| Multifocal disease on CT scan | 3–9 months | ‡ | 7 | 7 | 0.805 | ||
| Multifocal disease on CT scan | 2.5 years | ‡ | 7 | 7 | 0.576 | ||
| Quantitative lung volume measurement of first CT-scan | 3–9 months | 6 | 5 | 0.017 | |||
| Quantitative lung volume measurement of follow-up CT-scan | 2.5 years | 6 | 5 | 0.004 | |||
| Spirometry | FEV1 | 5 years | 5 | 7 | <0.001 | ||
| FEV1 | 10 years | ‡ | 5 | 6 | 0.868 | ||
| FEF25–75 | 5 years | 5 | 9 | <0.001 | |||
| FEF25–75 | 10 years | ‡ | 5 | 4.5 | 0.246 | ||
| FVC | 5 years | 5 | 7 | <0.001 | |||
| FVC | 10 years | ‡ | 5 | 6 | 0.273 | ||
| Lung clearance index | 5 years | ‡ | 4 | 4 | 0.327 | ||
| FRC | 5 years | ‡ | 4 | 4 | 0.576 | ||
| Exercise Tolerance | Bruce treadmill test | 5 years | 6 | 6 | 0.157 | ||
| VO2 max measurements | 8 years | ‡ | 5 | 5 | 0.771 | ||
| VO2 max measurements | 10 years | ‡ | 5 | 5 | 0.804 | ||
| Surgical Complications | Surgical complications ¶ | Not applicable | 7 | 9 | 0.018 | ||
| Malignancy | Proven malignancy on histology by experienced pathologist | Not applicable | 9 | 6 | <0.001 | ||
| Skeletal Deformity | Physical examination | All follow-up visits | ‡ | 6 | 6 | 0.205 | |
| Chest/Spine X-ray | 2.5 years | ‡ | 5 | 6 | 0.222 | ||
| Chest/Spine X-ray | 5 years | ‡ | 6 | 6 | 0.544 | ||
| CT-imaging | 2.5 years | ‡ | 5 | 6 | 0.299 | ||
| CT-imaging | 5 years | ‡ | 5 | 6 | 0.392 | ||
| Outcome Category | Outcome Parameter | Age at Measurement | Percentage Scoring during Round 3 | |
|---|---|---|---|---|
| 7–9 “Critical” | 1–3 “Not Important” | |||
| Respiratory Symptoms | Respiratory insufficiency * | All follow-up visits | 98 | 0 |
| Surgical Complications | Surgical complications ¶ | Not applicable | 95 | 2 |
| Lesion Characteristics | Mass effect/mediastinal shift ‡ | <1 month | 91 | 3 |
| 3–9 months | 89 | 0 | ||
| 2.5 years | 89 | 2 | ||
| Multifocal disease on CT scan | 3–9 months | 73 | 2 | |
| 2.5 years | 71 | 4 | ||
| Consensus | Outcome Category | Outcome Parameter | Age at Measurement | Percentage Scoring 7–9 “Critical” during Round 3 | |
|---|---|---|---|---|---|
| Surgical Group | Non-Surgical Group | ||||
| Both Stakeholder Groups | Respiratory symptoms | Respiratory insufficiency * | All follow-up visits | 97 | 100 |
| Surgical | Surgical complications ¶ | Not applicable | 91 | 100 | |
| Lesion characteristics | Mass effect/mediastinal shift ‡ | <1 month | 94 | 86 | |
| 3–9 months | 91 | 86 | |||
| 2.5 years | 91 | 86 | |||
| Multifocal disease on CT scan | 3–9 months | 70 | 77 | ||
| 2.5 years | 70 | 73 | |||
| Surgical Stakeholder Group only | Malignancy | Proven malignancy on histology by experienced pathologist | Not applicable | 97 | 14 |
| Infection | Infection at lesion site § | All follow-up visits | 94 | 0 | |
| Parent reported hospital admission with IV antibiotics due to LRTI | All follow-up visits | 82 | 27 | ||
| Non-Surgical Stakeholder Group only | Respiratory symptoms | Wheezing, defined as ≥3 episodes per year | All follow-up visits | 9 | 100 |
| Spirometry | FVC | 5 years | 21 | 100 | |
| FEF25–75 | 5 years | 21 | 91 | ||
| FEV1 | 5 years | 21 | 82 | ||
| Lesion characteristics | Systemic blood supply on CT-scan | 3–9 months | 64 | 77 | |
| Outcome Category | Outcome Parameter | Percentage Scored | |
|---|---|---|---|
| Total | |||
| Respiratory Symptoms | Respiratory insufficiency * | 6 | |
| Infection | LRTI | 16 | 32 |
| Infection at lesion site § | 8 | ||
| Frequency of antibiotics usage due to LRTI | 6 | ||
| Recurrent infection ¶ | 2 | ||
| Quality of Life | Quality of life | 4 | |
| Lesion Characteristics | CT-scan evaluation, dimensions of lesion | 16 | 30 |
| Mass effect/mediastinal shift on CT-scan | 8 | ||
| Radiological imaging | 2 | ||
| Evaluation with expert radiologist of first CT-scan | 2 | ||
| Change in lesion size over time | 2 | ||
| Spirometry | Lung function | 2 | 4 |
| FEV1 | 2 | ||
| Exercise Tolerance | Symptoms or mediastinal shift on CT/x ray at 6 months of age | 2 | |
| Malignancy | Malignancy risk/suspicion | 6 | 14 |
| Malignancy histologically proven | 4 | ||
| Malignancy | 4 | ||
| Other | Age | 2 | 6 |
| History | 2 | ||
| Oxygen supply | 2 | ||
| Combinations | Symptoms or mediastinal shift on CT/x ray at 6 months of age | 2 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kersten, C.M.; Hermelijn, S.M.; Mullassery, D.; Muthialu, N.; Cobanoglu, N.; Gartner, S.; Bagolan, P.; Mesas Burgos, C.; Sgrò, A.; Heyman, S.; et al. The Management of Asymptomatic Congenital Pulmonary Airway Malformation: Results of a European Delphi Survey. Children 2022, 9, 1153. https://doi.org/10.3390/children9081153
Kersten CM, Hermelijn SM, Mullassery D, Muthialu N, Cobanoglu N, Gartner S, Bagolan P, Mesas Burgos C, Sgrò A, Heyman S, et al. The Management of Asymptomatic Congenital Pulmonary Airway Malformation: Results of a European Delphi Survey. Children. 2022; 9(8):1153. https://doi.org/10.3390/children9081153
Chicago/Turabian StyleKersten, Casper M., Sergei M. Hermelijn, Dhanya Mullassery, Nagarajan Muthialu, Nazan Cobanoglu, Silvia Gartner, Pietro Bagolan, Carmen Mesas Burgos, Alberto Sgrò, Stijn Heyman, and et al. 2022. "The Management of Asymptomatic Congenital Pulmonary Airway Malformation: Results of a European Delphi Survey" Children 9, no. 8: 1153. https://doi.org/10.3390/children9081153









