Abstract
Neonatal skin care practices are considered crucial for a neonate’s survival and are closely related to healthcare professionals’ (HPs) knowledge and skills in delivering scientifically valid neonatal care interventions. In this descriptive cross-sectional pilot study, conducted in 2022, we aimed to assess HPs’ basic theoretical knowledge of neonatal vernix caseosa, skin microbiota, and bathing as well as knowledge regarding evidence-based clinical practices (referred to as “clinical knowledge”) for preterm neonatal skin care. Eligible participants were neonatologists, pediatricians, obstetricians, midwives and nurses working in the Greek setting. The research instrument was an online questionnaire designed by the research team. Finally, 123 HPs took part in the study. The theoretical, clinical and total knowledge scores were all significantly associated with age, healthcare profession and the sources used for education. Participants’ theoretical and clinical knowledge scores were compared and found not to differ significantly (p = 0.566). A significant and positive correlation was found between theoretical and clinical knowledge scores. Thus, it is concluded that HPs should be updated with the latest evidence-based knowledge and clinical guidelines in order to provide neonatal skin care with high-quality standards.
1. Introduction
The skin is the body’s largest organ with quite an essential role during the neonatal period as it regulates fluid balance, maintains thermoregulation and protects the neonate from infection. More recent evidence supports the skin barrier continuously developing within the first two years of life, and thus optimal skin care is critical from the early neonatal period to toddlerhood [1].
For those neonates born preterm, the skin can be quite immature, especially in the first 2 weeks of life and therefore susceptible to damage. As a consequence, there is an increased risk for invasion by microorganisms and thus morbidity and mortality [2]. During hospitalization, maintenance of skin integrity, the decrease of risk factors and neonatal skin care education for parents/caregivers are key priorities for the multidisciplinary team that takes care of the preterm neonate [3]. That team, mainly consisting of healthcare professionals (HPs) such as pediatricians/neonatologists, midwives and nurses, should be updated with the latest evidence-based knowledge to provide neonatal skin care with high-quality standards. Such knowledge should include assessment of the neonate’s skin condition, identification of high-risk neonates for disruption of normal skin barrier function, recognition of environmental factors and treatment-related agents that may affect neonatal skin integrity as well as interventions to promote optimal skin function and reduce skin trauma [4]. Assurance of high-quality services is provided by the implementation of revised clinical practice guidelines based on the best available evidence.
Previous studies have evaluated knowledge level, experience, practices and beliefs of the nurses working in neonatal units regarding preterm neonatal skin health. Interestingly, the participants in these studies expressed concern about the inadequacy of available evidence and the limited awareness of the subject [5,6]. More specifically, Liversedge et al. [5] reported discrepancies in the participants’ responses, a fact that indicates insufficiency in education and evidence-based clinical practices, while Mohamed et al. [6] demonstrated gaps in participants’ theoretical and practical knowledge of preterm neonatal skin care. In contrast to these studies, we decided to recruit HPs with different employment statuses and working positions in different levels of healthcare instead of neonatal unit staff to investigate knowledge of evidence-based clinical practices for preterm neonatal skin care. We did this because in Greece, a country that has adopted a highly centralized “mixed health system” model [7], the private sector is expanded and plays an important role in the provision of health services, especially in maternal and neonatal care. This means that mothers usually collaborate with private HPs who continuously provide counseling and support during the perinatal period. In the occurrence of an unexpected event, such as a preterm birth, Greek women and their family often consult as a coping mechanism these already known healthcare providers for the care of the preterm neonate. The neonatal unit staff is commonly asked subsequently for advice, as it might take a little more time for them to gain parental confidence, overcome communication gaps, build/maintain relationships, exchange information and share decision-making with parents [8]. Similar behaviors are also observed in women who attend public perinatal care services, as circumstantial evidence implies that informal payments are still common in Greek public hospitals and women usually cooperate with and refer to specific HPs [7]. As a result, we are of the opinion that all perinatal HPs should be updated and in line with the latest guidelines because appropriate neonatal skin care practices are considered crucial for a neonate’s survival and are closely related to HP’s knowledge and skills to deliver scientifically valid neonatal care interventions.
Taking into consideration the Greek healthcare framework and typical Greek behavioral aspects, we aimed to assess HPs’ (a) basic theoretical knowledge of neonatal vernix caseosa, skin microbiota and bathing and (b) knowledge regarding evidence-based clinical practices for preterm neonatal skin care (referred to as “clinical knowledge” for the needs of the present study). We hypothesized that significant and positive correlations between theoretical and clinical knowledge would be found.
2. Materials and Methods
2.1. Study Design and Participants
This is a descriptive cross-sectional study conducted in June 2022. Ethical approval for this study was obtained from the Ethics Committee of the University of West Attica (IRB R.No.: 53752/08-06-2022), which is located in Attica, the capital of Greece.
Eligible participants were HPs who worked with neonates, either term or preterm, including neonatologists, pediatricians, obstetricians, midwives and nurses. The HPs needed to speak and understand the Greek language fluently in order to be able to complete the questionnaire of the study. During the recruitment period, numerous HPs all over Greece were invited via email and social media to join the study.
2.2. Procedure of Recruitment
An invitation letter with a link to the survey was posted by the research team on social media platforms for professionals or emailed to the perinatal HPs of Greece, members of professional networks or employees at hospitals/clinics. In the letter, the nature and the purpose of the study was explained, helping to create interest and eagerness to serve as research subjects. Once the participant voluntarily agreed and consented to participate online, the questionnaire was unlocked. Recruitment was in compliance with all ethical principles and participation in the study entailed no direct personal benefits.
The questionnaire was administered online mainly due to COVID-19 restrictions, time constraints and with a view to prevent systematic errors as a result of postal handling procedures. A code was assigned automatically to each participant by the database used so that the de-identification could be preserved.
2.3. Research Instrument
The research instrument was one questionnaire divided into three sections. The first section referred to the demographic and occupational characteristics of gender, age, educational/employment status, healthcare profession, total working experience, geographical area and level of healthcare of current work. The second section consisted of 21 questions that explored theoretical knowledge about neonatal vernix caseosa, skin microbiota and bathing. The third section consisted of 21 questions that assessed the knowledge of HPs regarding evidence-based clinical practices for preterm neonatal skin care. Both theoretical and clinical knowledge were the knowledge derived from the latest available evidence-based, published literature.
The questions for all sections were formulated by the research team following a comprehensive review of the relevant literature. The questionnaire was generated from well-respected sources reporting evidenced-based guidelines or recommending evidence-based practices for optimal neonatal skin care [1,9,10,11,12,13]. Questions were then piloted, redefined and validated by a group of experts that consisted of two neonatologists and two midwives with working experience in a neonatal intensive care unit (NICU) of more than 15 years. The final form of the questionnaire was approved by the research team.
All questions included in the questionnaire were close-ended and were either true/false questions or single-answer multiple choice. Each question needed to be answered within 60 s.
2.4. Statistical Analysis
Quantitative variables were expressed as mean values (standard deviation), while qualitative variables were expressed as absolute and relative frequencies. Student’s t tests and analysis of variance (ANOVA) were computed for the comparison of mean values. Bonferroni correction was used in order to control for type I errors. Pearson correlation coefficients were used to investigate the association of two continuous variables. Paired Student’s t test was used for the comparison between theoretical and clinical knowledge. Multivariate linear regression analyses were conducted in order to identify demographic and occupational characteristics that were independently associated with participants’ knowledge scores. All reported p values are two-tailed. Statistical significance was set at p < 0.05 and analyses were conducted using SPSS statistical software (version 22.0, IBM, Armonk, NY, USA).
3. Results
3.1. Participants’ Demographic and Occupational Characteristics
The final study sample consisted of 123 HPs. Participants’ demographic and occupational characteristics are presented extensively in Table 1. Regarding the HPs’ theoretical knowledge of neonatal vernix caseosa, skin microbiota and bathing, as well as of clinical practices for neonatal skin care, this was mainly derived from professional experience (52.0%) in comparison to other sources (Table 1).

Table 1.
Participants’ demographic and occupational characteristics.
3.2. Participants’ Theoretical Knowledge about Neonatal Vernix Caseosa, Skin Microbiota and Bathing
The questions that assessed HPs’ theoretical knowledge about neonatal vernix caseosa, skin microbiota and bathing, along with their performance, are broadly presented in the table below (Table 2).

Table 2.
Questions and healthcare professionals’ performance regarding theoretical knowledge about neonatal vernix caseosa, skin microbiota and bathing.
The percentages for correct answers ranged from 18.7 to 97.6%. More specifically, few participants answered correctly that ‘the microbial flora of the neonatal skin is more diverse in dry skin areas’ and that ‘neonatal skin microbiota is initially established 3–4 days after birth’. Additionally, the majority of respondents correctly answered that ‘the NICU environment can affect the development of skin microbiota in preterm neonates and that ‘intravenous antibiotics can affect neonatal skin microbiota’.
Participants’ correct answers were then added. This sum was converted into a 0–100 scale. Thus, the theoretical knowledge score could range from 0% to 100%, with higher scores indicating greater knowledge. Total scores varied from 28.57% to 100% with the mean value being 59.47% (SD = 14.8%). None of the participants scored zero (i.e., did not answer any questions correctly) and 1 person (0.8%) scored 100 (i.e., answered all questions correctly).
Furthermore, participants’ theoretical knowledge score was associated with their demographic and occupational characteristics. Results are depicted in Table 3.

Table 3.
Associations among participants’ theoretical knowledge score and demographic and occupational characteristics.
Participants’ theoretical knowledge score was significantly associated with age, healthcare profession, geographical area of current work and the sources used for acquiring knowledge about neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care. More specifically, after the Bonferroni correction it was found that participants aged 20–40 years old and 41–50 years old had significantly lower scores, indicating lower knowledge of the theme compared to those aged 51 and above (p = 0.003 and p = 0.043 respectively). Further analysis showed that participants who had gained the aforementioned knowledge from their undergraduate or postgraduate studies had significantly lower scores in comparison with participants who focused on personal study and research (p = 0.010). Not surprisingly, significantly higher scores, indicating greater knowledge, were observed among doctors and, interestingly, among participants working outside the prefecture of Attica.
3.3. Participants’ Knowledge Regarding Evidence-Based Clinical Practices for Preterm Neonatal Skin Care
Information about participants’ knowledge regarding evidence-based clinical practices for preterm neonatal skin care are presented in the following table (Table 4).

Table 4.
Questions and healthcare professionals’ performance regarding evidence-based clinical practices for preterm neonatal skin care.
The percentages for correct answers ranged from 14.6 to 98.4%. More specifically, a minority of participants answered correctly that ‘to reduce stress in preterm neonates the recommended bathing technique is swaddled immersion bath’ and that ‘in preterm neonates, in order to protect the stratum corneum, the nappy area should be cleaned only with water for the first 4 weeks of life’. Additionally, when participants were asked about ‘the use of inappropriate detergents in the linen and clothing’, most of them answered correctly that in preterm neonates ‘may affect neonatal skin microbiome’. At last, 95.1% of the subjects commented accurately that ‘in preterm neonates, application of protective dressings is suggested when nasal CPAP devices are used’.
Participants’ correct answers were added subsequently. This sum was converted into a 0–100 scale. Total scores ranged from 28.57 to 100% with the mean value being 60.12% (SD = 13.34%). None of the participants scored zero and 2 participants (1.6%) scored 100.
Participants’ clinical knowledge score was then associated with demographic and occupational characteristics (Table 5).

Table 5.
Associations among participants’ clinical knowledge score and demographic and occupational characteristics.
Participants’ clinical knowledge score was significantly associated with age, healthcare profession and the sources used for acquiring knowledge on neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care. More specifically, after the Bonferroni correction it was found that participants aged 20–40 years old had significantly lower scores compared to those who were at least 51 years old (p = 0.015). Moreover, it was observed that participants who learned about neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care from personal study and research had significantly higher scores compared to those who gained knowledge from undergraduate or postgraduate studies (p < 0.001), professional experience (p = 0.006) or seminars/congresses/lectures/courses (p = 0.003). As could be expected, doctors demonstrated significantly higher scores, indicating greater knowledge of the topic.
3.4. Total Knowledge Score
All theoretical and clinical correct answers were added for each participant. The total knowledge score of the participants was found to be between 30.95% and 97.62% with the mean value being 59.79% (SD = 12.63%). None of the participants scored zero or 100. Associations among participants’ total knowledge score and demographic and occupational characteristics are presented in Table 6.

Table 6.
Associations among participants’ total knowledge score and demographic and occupational characteristics.
Participants’ total knowledge score was significantly associated with age, healthcare profession and sources used for acquiring knowledge on neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care. More specifically, after the Bonferroni correction, it was found that participants aged 20–40 years old and 41–50 years old had significantly lower scores compared to those who were at least 51 years old (p = 0.002 and p = 0.024 respectively). In addition, it was found that participants who learned about neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care from personal study and research had significantly higher scores compared to those who had learned about the topic from their undergraduate or postgraduate studies, professional experience and seminars/congresses/lectures/courses or other sources (p < 0.001, p = 0.009 and p = 0.007 respectively). At last, doctors demonstrated significantly higher scores, indicating greater knowledge.
3.5. Demographic and Occupational Characteristics Independently Associated with Participants’ Theoretical, Clinical and Total Knowledge Scores
Multivariate linear regression analysis was conducted in order to identify demographic and occupational characteristics independently associated with participants’ theoretical, clinical and total knowledge scores (Tables S1–S3).
Participants’ age, healthcare profession and sources used for acquiring knowledge on vernix caseosa, skin microbiota, neonatal bathing and clinical practices for neonatal skin care were found to be independently associated with their clinical and total knowledge score, while their theoretical knowledge score was independently associated only with age and healthcare profession.
In particular, participants who were at least 51 years old when compared to participants aged 20–40 years old were found to demonstrate significantly higher scores in theoretical, clinical and total knowledge by 10.85, 11.12 and 10.99 units, respectively. Moreover, doctors when compared to midwives and nurses were found to have significantly higher scores in theoretical, clinical and total knowledge by 11.85, 11.42 and 11.64 units, respectively. Finally, participants who had learned about neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care from personal study and research had significantly higher scores in clinical and total knowledge by 11.74 and 9.88 units, respectively, compared to those who had learned about the topic from their undergraduate or postgraduate studies.
3.6. Comparison between Theoretical and Clinical Knowledge Scores
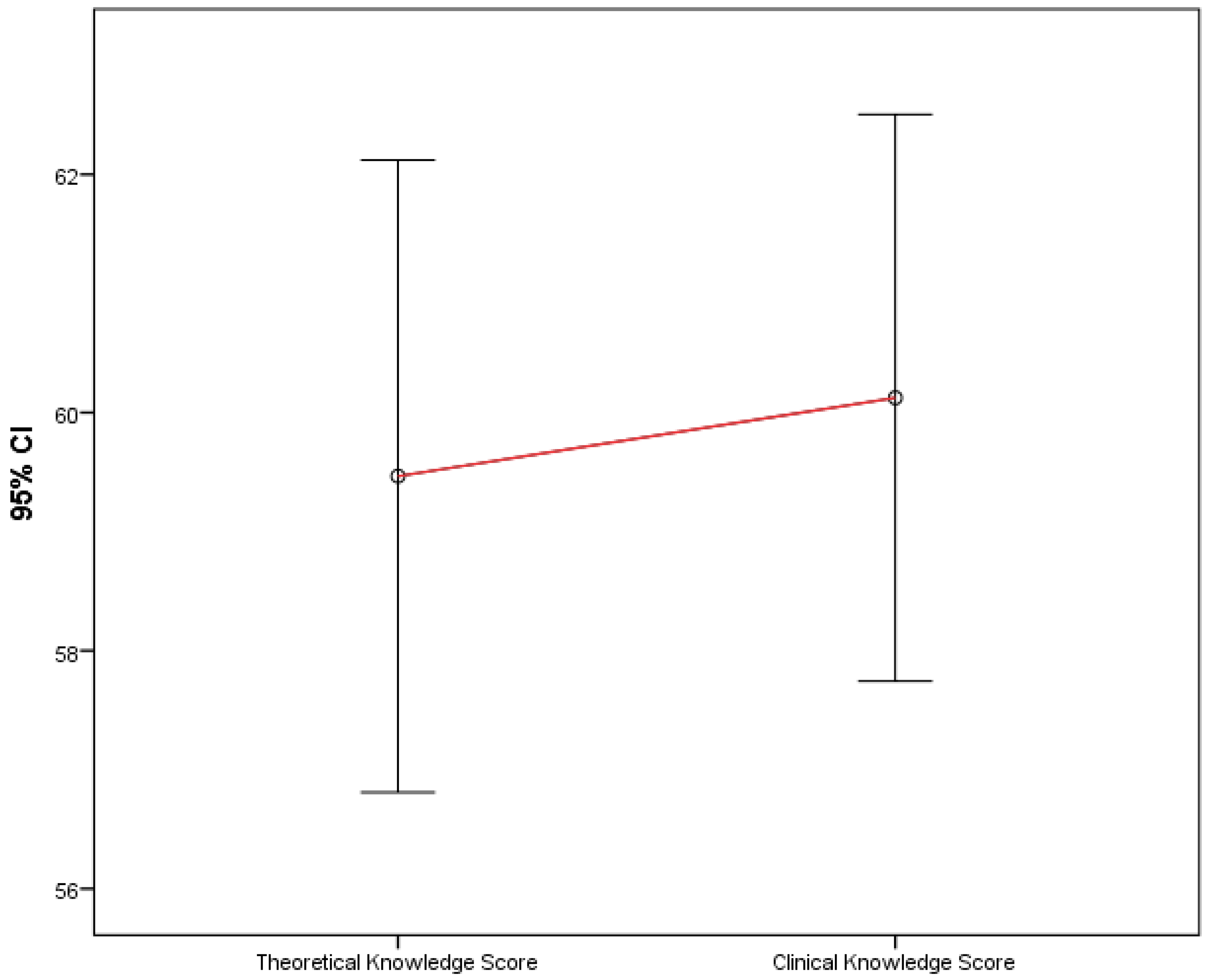
Participants’ theoretical and clinical knowledge scores were compared and found not to differ significantly (p = 0.566), as shown in Figure 1.
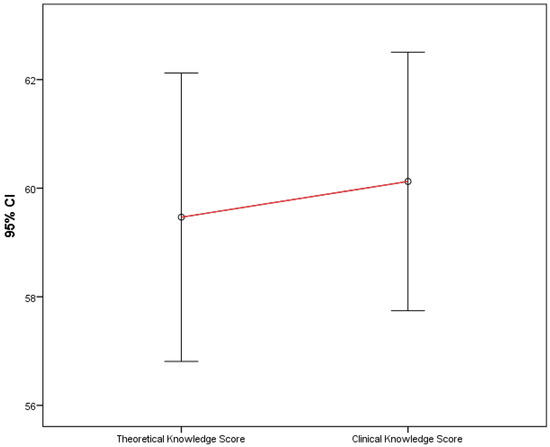
Figure 1.
Comparison of theoretical and clinical knowledge scores.
3.7. Correlation between Theoretical and Clinical Knowledge Scores
Pearson’s correlation coefficient (r) between theoretical and clinical knowledge scores is presented in Table 7.

Table 7.
Correlation between theoretical and clinical knowledge scores.
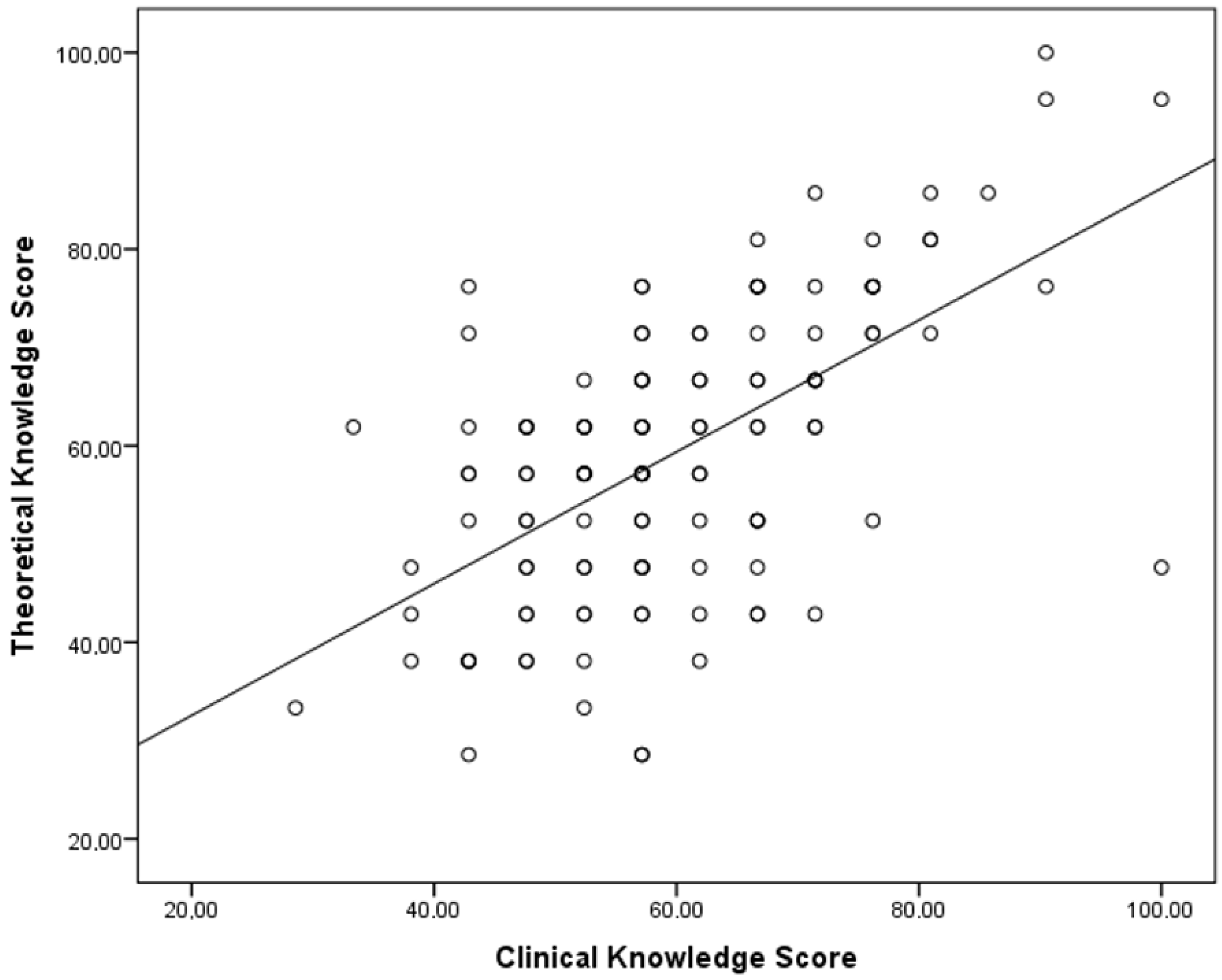
A significant and positive correlation was found between theoretical and clinical knowledge scores. Thus, greater theoretical knowledge was significantly associated with greater clinical knowledge (Figure 2).

Figure 2.
Correlation between theoretical and clinical knowledge scores.
4. Discussion
The present study, as far as we know, is the first to identify HPs’ knowledge of evidence-based clinical practices for preterm neonatal skin care in the Greek setting. Previous research from the UK [5] demonstrated the beliefs and practices of nurses working in neonatal units in which participants stated that formal skin care training was severely lacking, and instead, bedside training was offered from the more experienced colleagues to the junior staff. This finding is in agreement with our own observation, where 52% of the participants reported that basic theoretical knowledge about neonatal skin and its care is mainly derived from professional experience in comparison to other sources of education. However, the present study was conducted in the midst of the COVID-19 pandemic, so it cannot be ruled out that it had a strong impact on teaching and learning in health professional education [14], including the non-occurrence of educational courses. The development and presence of continuing educational programs in neonatal units and operational frameworks for primary healthcare maintain current practice, translate knowledge into clinical implementation, connect newly acquired knowledge and skills to what is already known or experienced and thus sustain an HP’s career [15,16].
In our study, participants’ total scores in theoretical knowledge about neonatal vernix caseosa, skin microbiota and bathing varied from 28.57% to 100%. Such an observation can be explained by the main differences in the study sample (age, specialty, sources of education). Nevertheless, the highest scores indicating greater knowledge were observed in questions relating to NICU environment and intravenous antibiotics use, showing that HPs were aware of key factors that affect mainly preterm neonates and neonatal skin microbiota. Primary caregivers in a NICU setting and during the neonatal period should be updated to the best available research to apply clinical practices that protect neonatal skin microbiome as its development is critical, having long-term impacts [17].
As far as HPs’ clinical and total knowledge are concerned, these were significantly associated with age and profession specialty but also with sources of education. Participants who educated themselves on the topic by personal study and research had significantly higher scores compared to other sources of education. This finding highlights the fact that for HPs it is very important to develop independence in determining their learning needs as well as to ascertain when and how these needs can be addressed. Healthcare professionals are continuous learners, and self-study skills are distinguishing traits of practitioners who want to be professionally competent [18].
Furthermore, participants’ theoretical and clinical knowledge scores were found not to differ significantly and a positive correlation between theoretical and clinical knowledge scores was confirmed. These results demonstrate the absence of a knowledge gap between theoretical and clinical knowledge concerning neonatal skin care, especially the preterm, possibly due to the fact that a large percentage had acquired an MSc or PhD degree (67.5%) and 36.6% had more than 10 years of experience. Several studies, though [6,19,20], have found barriers that utilize theoretical knowledge in clinical settings, such as disbelief in clinical competence, deficiencies in the teaching and learning process and differences between simulation-based learning and real-life clinical situations.
This pilot study has gone some way towards enhancing our understanding of the HPs’ knowledge of evidence-based clinical practices for preterm neonatal skin care, especially in the Greek setting. We are aware, though, that our research had some strengths and limitations. A major strength was that participants came from health facilities of different levels of care, which belonged to either the public or the private sector, and were located both in the capital and the provinces, indicating a more representative sample in terms of knowledge. We acknowledge, though, that these are preliminary findings of a pilot study and as a consequence their generalization in the whole Greek context is restricted. Another strength of our study was that our questionnaire was based on the latest available evidence-based research [1,9,10,11,12,13] and exploring whether HPs are in line with it. Furthermore, because the present study was conducted online via email and social media invitation, a main limitation is that the response rate cannot be calculated. Moreover, the questionnaire’s section which assessed HPs’ theoretical knowledge of ‘neonatal vernix caseosa, skin microbiota, bathing and clinical practices for neonatal skin care’, included questions both for term and preterm neonates, creating a difficulty in strictly investigating knowledge about preterm neonatal skin care. Lastly, participants in our study had different specialties and it was not mandatory to belong to neonatal units’ staff, making our results difficult to compare with other studies which recruited only experienced neonatal staff.
The lessons learned from this pilot study will undoubtedly improve the research design of further inquiries. Future researchers should consider expanding resources and develop enough evidence for subsequent studies. We recommend that further research should recruit a larger number of HPs so as to achieve a representative sample. A flexible recruitment plan which allows modifications when unexpected barriers appear should be developed as well. Procedures of data collection should be well defined to demonstrate validity and reliability [21].
The feasibility of assessing HPs’ knowledge, in relation to preterm neonatal skin care, according to the level of healthcare facility they work or their specialty/subspecialty, should be examined, also taking into account how much time during the day the HP works with preterm neonates. Additionally, the measurement tool was relatively new, so this pilot study provided direction for its refinement [22], mainly regarding the second section which investigated theoretical knowledge. It is proposed that future work should focus on NICU staff as preterm neonates are more likely to require prolonged hospitalization and therefore be in need of supportive care that may increase the risk of skin injury. By gaining a wider perspective on whether knowledge gaps in preterm infants’ skin care exist among NICU staff, it will bring to light the necessity or not of developing clinical evidence based guidelines on preterm infant skin care in a national level so as to promote consistency in practice within the contexts of NICUs.
Finally, future studies need to investigate the applicability of reported evidence-based research to the clinical setting and their potential effect on care outcomes, by ensuring that guidelines are efficiently disseminated and implemented [23]. This will provide direction for incorporating educational intervention and continuing professional support with the goal to optimize preterm neonatal skin care.
5. Conclusions
Our work has led us to conclude that knowledge of evidence-based clinical practices for preterm neonatal skin care is an under-reported problem. Further research is needed to evaluate if HPs work along with evidence-based guidelines in their daily clinical practice. Implementing clinical practice guidelines demands a systematic planning process with a focus on institutional and social context, barriers and facilitators that arise from the introduction of innovations or changes of proven value in specific environments and finally, assessment of intervention strategies for the implementation to be efficient, effective, safe and patient-centered.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/children9081235/s1: Table S1: Demographic and occupational characteristics independently associated with participants’ theoretical knowledge score; Table S2: Demographic and occupational characteristics independently associated with participants’ clinical knowledge score; Table S3: Demographic and occupational characteristics independently associated with participants’ total knowledge score; Figure S1: Participants’ total knowledge score.
Author Contributions
Conceptualization, D.M. and K.L.; methodology, D.M., C.N. and K.L.; software, D.M. and G.K.; validation, D.M., C.N. and K.L.; formal analysis, D.M.; investigation, D.M. and P.T.; resources, D.M and C.N.; data curation, D.M. and P.T.; writing—original draft preparation, D.M. and P.T.; writing—review and editing, C.N. and K.L.; visualization, D.M and G.K..; supervision, K.L.; project administration, C.N. and K.L.; funding acquisition, C.N. and K.L. All authors have read and agreed to the published version of the manuscript.
Funding
The APC was partially funded by the “Special Account for Research Grants” through University of West Attica and the Master of Science Program “Advanced and Evidence Based Midwifery Care”.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of UNIVERSITY OF WEST ATTICA (53752/08-06-2022).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
References
- New, K. Evidence-based guidelines for infant bathing. Res. Rev. 2019, 1–4. Available online: https://www.researchreview.co.nz/getmedia/0a9e5190-b8ac-419f-8f44-43b8e5ba8c4b/Educational-Series-Evidence-based-guidelines-for-infant-bathing.pdf.aspx?ext=.pdf (accessed on 15 June 2022).
- Visscher, M.O.; Adam, R.; Brink, S.; Odio, M. Newborn infant skin: Physiology, development, and care. Clin. Dermatol. 2015, 33, 271–280. [Google Scholar] [CrossRef]
- Hockenberry, M.J.; Rodgers, C.C.; Wilson, D. Wong’s Essentials of Pediatric Nursing, 11th ed.; Elsevier/Mosby: St. Louis, MO, USA, 2022; pp. 477–510. [Google Scholar]
- Lead Nurse Neonatal and Paediatric Services, Skin Care Guidelines for Neonates Including Care of Nappy Rash, Northern Devon Healthcare. 2019. Available online: https://www.northdevonhealth.nhs.uk (accessed on 15 June 2022).
- Liversedge, H.L.; Bader, D.L.; Schoonhoven, L.; Worsley, P.R. Survey of neonatal nurses’ practices and beliefs in relation to skin health. J. Neonatal Nurs. 2018, 24, 86–93. [Google Scholar] [CrossRef]
- Mohamed, Z.; Newton, J.M.; Lau, R. Malaysian nurses’ skin care practices of preterm infants: Experience vs. knowledge. Int. J. Nurs. Pract. 2014, 20, 187–193. [Google Scholar] [CrossRef]
- OECD/European Observatory on Health Systems and Policies. State of Health in the EU Greece Country Health Profile 2021, OECD Publishing, Paris/European Observatory on Health Systems and Policies, Brussels. 2021. Available online: https://eurohealthobservatory.who.int/ (accessed on 15 June 2022).
- Lorié, E.S.; Wreesmann, W.W.; van Veenendaal, N.R.; van Kempen, A.A.M.W.; Labrie, N.H.M. Parents’ needs and perceived gaps in communication with healthcare professionals in the neonatal (intensive) care unit: A qualitative interview study. Patient Educ. Couns. 2021, 104, 1518–1525. [Google Scholar] [CrossRef] [PubMed]
- Northern Devon District Hospital. Skin Care Guidelines for Neonates Including Care of Nappy Rash. Available online: https://www.northdevonhealth.nhs.uk/wp-content/uploads/2019/06/Skin-care-for-Neonates-guidelines-May-19.pdf (accessed on 28 June 2022).
- Thames Valley Neonatal ODN Quality Care Group. Guideline Framework for Skin Integrity. Available online: https://southodns.nhs.uk/wp-content/uploads/2019/12/Skin-Integrity-Guideline-Dec-2019-Final.pdf (accessed on 28 June 2022).
- Nishijima, K.; Yoneda, M.; Hirai, T.; Takakuwa, K.; Enomoto, T. Biology of the vernix caseosa: A review. J. Obstet. Gynaecol. Res. 2019, 45, 2145–2149. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO recommendations on newborn health: Guidelines approved by the WHO Guidelines Review Committee. World Health Organization 2017. Available online: https://apps.who.int/iris/handle/10665/259269 (accessed on 28 June 2022).
- Blume-Peytavi, U.; Lavender, T.; Jenerowicz, D.; Ryumina, I.; Stalder, J.F.; Torrelo, A.; Cork, M.J. Recommendations from a European Roundtable Meeting on Best Practice Healthy Infant Skin Care. Pediatr. Dermatol. 2016, 33, 311–321. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.; Sarkar, M.; Davis, E.; Morphet, L.; Maloney, S.; Ilic, D.; Palermo, C. Impact of the COVID-19 pandemic on teaching and learning in health professional education: A mixed methods study protocol. BMC Med. Educ. 2021, 21, 439. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine (US) Committee on Planning a Continuing Health Professional Education Institute. Continuing Professional Development: Building and Sustaining a Quality Workforce. In Redesigning Continuing Education in the Health Professions; National Academies Press: Washington, DC, USA, 2010; Volume 1. Available online: https://www.ncbi.nlm.nih.gov/books/NBK219809/ (accessed on 15 June 2022).
- Norman, M.K.; Lotrecchiano, G.R. Translating the learning sciences into practice: A primer for clinical and translational educators. J. Clin. Transl. Sci. 2021, 5, e173. [Google Scholar] [CrossRef] [PubMed]
- Luna, P.C. Skin Microbiome as Years Go By. Am. J. Clin. Dermatol. 2020, 21, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Woods, J.C. Self-Study: A Method for Continuous Professional Learning and A Methodology for Knowledge Transfer. QANE AFI 2021, 7, 7. [Google Scholar] [CrossRef]
- Hashemiparast, M.; Negarandeh, R.; Theofanidis, D. Exploring the barriers of utilizing theoretical knowledge in clinical settings: A qualitative study. Int. J. Nurs. Sci. 2019, 6, 399–405. [Google Scholar] [CrossRef] [PubMed]
- Saifan, A.; Devadas, B.; Daradkeh, F.; Hadya, A.F.; Mohannad, A.; Lintu, M.M. Solutions to bridge the theory-practice gap in nursing education in the UAE: A qualitative study. BMC Med. Educ. 2021, 21, 490. [Google Scholar] [CrossRef] [PubMed]
- Danesh, V.; Zuñiga, J.A.; Timmerman, G.M.; Radhakrishnan, K.; Cuevas, H.E.; Young, C.C.; Henneghan, A.M.; Morrison, J.; Kim, M.T. Lessons learned from eight teams: The value of pilot and feasibility studies in self-management science. Appl. Nurs. Res. 2021, 57, 151345. [Google Scholar] [CrossRef] [PubMed]
- Beebe, L.H. What can we learn from pilot studies? Perspect Psychiatr. Care 2007, 43, 213–218. [Google Scholar] [CrossRef] [PubMed]
- Panteli, D.; Legido-Quigley, H.; Reichebner, C.; Ollenschläger, G.; Schäfer, C.; Busse, R. Clinical Practice Guidelines as a quality strategy. In Improving Healthcare Quality in Europe: Characteristics, Effectiveness and Implementation of Different Strategies; Busse, R., Klazinga, N., Panteli, D., Quentin, W., Eds.; European Observatory on Health Systems and Policies: Copenhagen, Denmark, 2019. Available online: https://www.ncbi.nlm.nih.gov/books/NBK549283/ (accessed on 22 July 2022).
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).