The Evolution of Spinal Endoscopy: Design and Image Analysis of a Single-Use Digital Endoscope Versus Traditional Optic Endoscope
Abstract
:1. Introduction
2. Materials and Methods
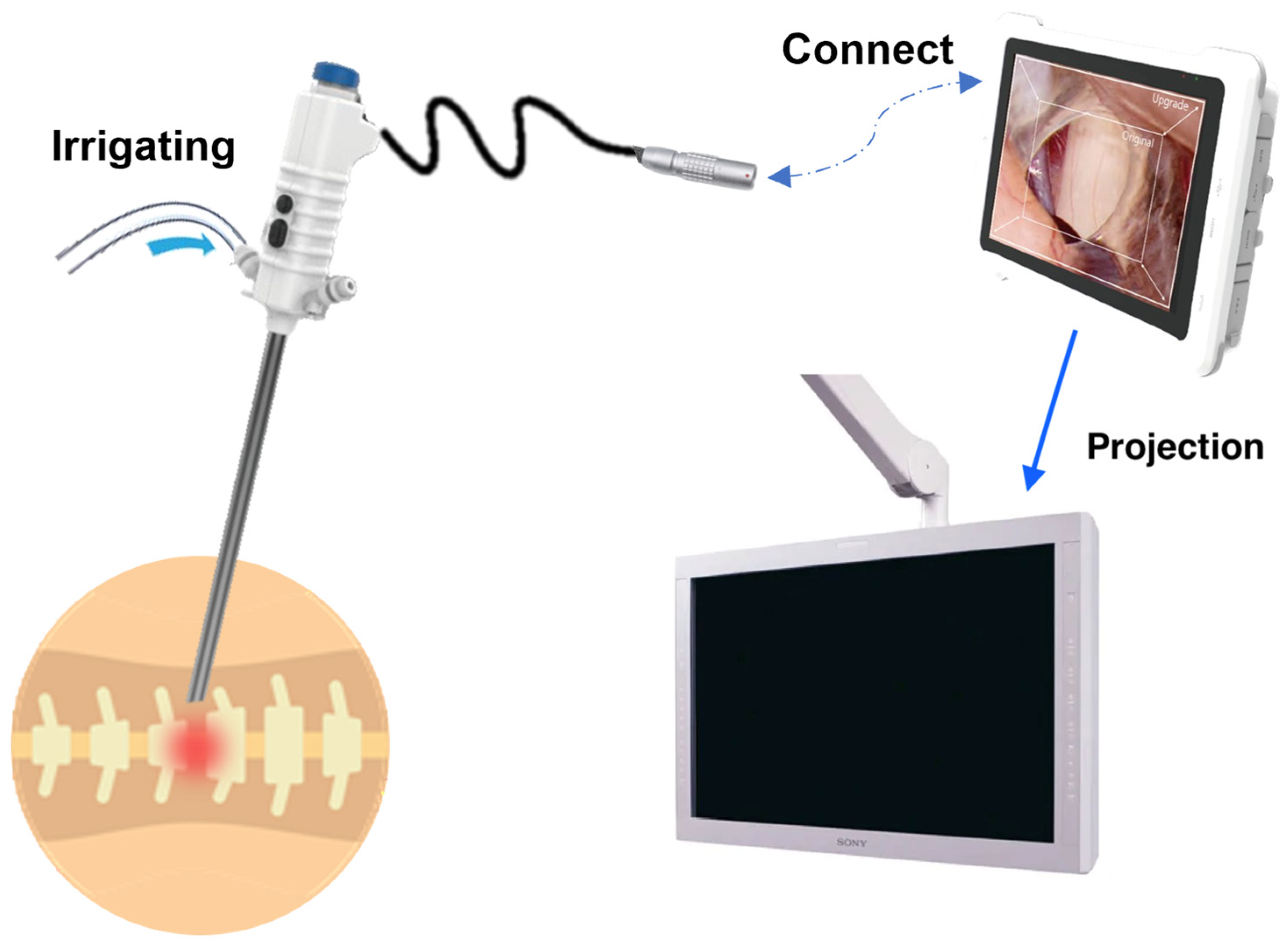
2.1. Design of the Endoscope System
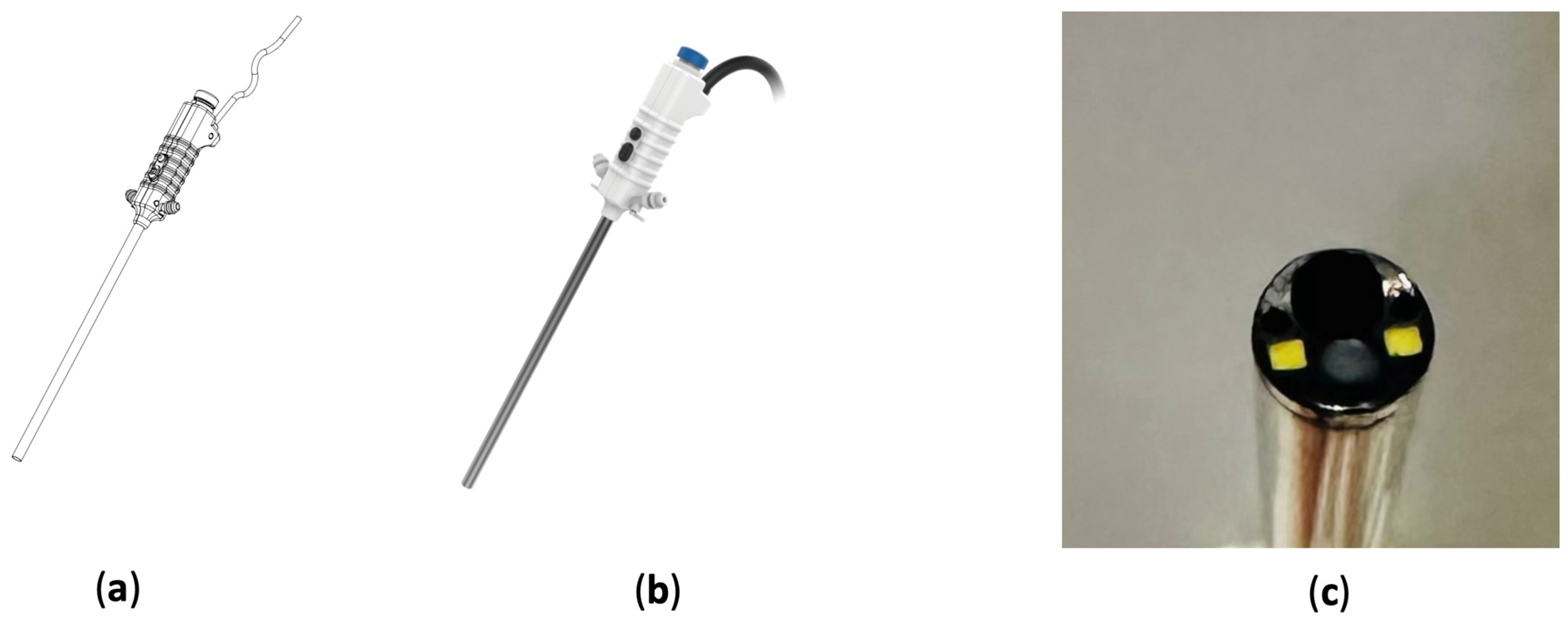
2.2. Design of Endoscope Body and Distal Camera
2.3. Monitor and Endoscope Console
2.4. Image Captures
2.5. Images Analysis and Comparison with a Traditional Optic Endoscope
2.6. Software Analysis Algorithms
2.6.1. Distortion Correction
2.6.2. Modulation Transfer Function
2.6.3. Color Difference
2.6.4. Luminance Uniformity
2.6.5. Gray Scale
2.7. Statistics
3. Results
3.1. Product Dimensions and Specifications
3.2. Field of View
3.3. Grid Ground Test
3.4. Standard for Mobile Imaging Architecture (SMIA) TV Distortion
3.5. Modulation Transfer Function (MTF) and Spatial Frequency Response (SFR) Test
3.6. 1951 United States Air Force (USAF) Resolution Test
3.7. Color Difference
3.8. Luminance
3.9. Grayscale Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Telfeian, A.E.; Veeravagu, A.; Oyelese, A.A.; Gokaslan, Z.L. A brief history of endoscopic spine surgery. Neurosurg. Focus 2016, 40, E2. [Google Scholar] [CrossRef] [PubMed]
- Yeung, A.T. Minimally Invasive Disc Surgery with the Yeung Endoscopic Spine System (YESS). Surg. Technol. Int. 1999, 8, 267–277. [Google Scholar] [PubMed]
- Kim, M.; Kim, H.S.; Oh, S.W.; Adsul, N.M.; Singh, R.; Kashlan, O.N.; Noh, J.H.; Jang, I.T.; Oh, S.H. Evolution of Spinal Endoscopic Surgery. Neurospine 2019, 16, 6–14. [Google Scholar] [CrossRef]
- Jang, J.W.; Lee, D.G.; Park, C.K. Rationale and Advantages of Endoscopic Spine Surgery. Int. J. Spine Surg. 2021, 15, S11–S20. [Google Scholar] [CrossRef]
- Zuo, R.; Jiang, Y.; Ma, M.; Yuan, S.; Li, J.; Liu, C.; Zhang, J. The clinical efficacy of biportal endoscopy is comparable to that of uniportal endoscopy via the interlaminar approach for the treatment of L5/S1 lumbar disc herniation. Front. Surg. 2022, 9, 1014033. [Google Scholar] [CrossRef]
- Kwon, H.; Park, J.Y. The Role and Future of Endoscopic Spine Surgery: A Narrative Review. Neurospine 2023, 20, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Simpson, A.K.; Lightsey, H.M.t.; Xiong, G.X.; Crawford, A.M.; Minamide, A.; Schoenfeld, A.J. Spinal endoscopy: Evidence, techniques, global trends, and future projections. Spine J. 2022, 22, 64–74. [Google Scholar] [CrossRef]
- Jitpakdee, K.; Liu, Y.; Heo, D.H.; Kotheeranurak, V.; Suvithayasiri, S.; Kim, J.S. Minimally invasive endoscopy in spine surgery: Where are we now? Eur. Spine J. 2023, 32, 2755–2768. [Google Scholar] [CrossRef]
- Huang, X.; Liu, X.; Zhu, B.; Hou, X.; Hai, B.; Li, S.; Yu, D.; Zheng, W.; Li, R.; Pan, J.; et al. Evaluation of Augmented Reality Surgical Navigation in Percutaneous Endoscopic Lumbar Discectomy: Clinical Study. Bioengineering 2023, 10, 1297. [Google Scholar] [CrossRef]
- Heo, D.H.; Lee, D.C.; Park, C.K. Comparative analysis of three types of minimally invasive decompressive surgery for lumbar central stenosis: Biportal endoscopy, uniportal endoscopy, and microsurgery. Neurosurg. Focus 2019, 46, E9. [Google Scholar] [CrossRef]
- Goparaju, P.; Rajamani, P.A.; Kulkarni, A.G.; Kumar, P.; Adbalwad, Y.M.; Bhojraj, S.; Nene, A.; Rajasekaran, S.; Acharya, S.; Bhanot, A.; et al. A 2-Year Outcomes and Complications of Various Techniques of Lumbar Discectomy: A Multicentric Prospective Study. Glob. Spine J. 2023, 21925682231220042. [Google Scholar] [CrossRef]
- Luan, H.; Peng, C.; Liu, K.; Song, X. Comparing the efficacy of unilateral biportal endoscopic transforaminal lumbar interbody fusion and minimally invasive transforaminal lumbar interbody fusion in lumbar degenerative diseases: A systematic review and meta-analysis. J. Orthop. Surg. Res. 2023, 18, 888. [Google Scholar] [CrossRef] [PubMed]
- Tieber, F.; Lewandrowski, K.U. Technology advancements in spinal endoscopy for staged management of painful spine conditions. J. Spine Surg. 2020, 6, S19–S28. [Google Scholar] [CrossRef] [PubMed]
- Yuh, W.-T.; Lee, Y.-S.; Jeon, J.-H.; Choi, I. Future of Endoscopic Spine Surgery: Insights from Cutting-Edge Technology in the Industrial Field. Bioengineering 2023, 10, 1363. [Google Scholar] [CrossRef] [PubMed]
- Rutala, W.A.; Weber, D.J. Disinfection of endoscopes: Review of new chemical sterilants used for high-level disinfection. Infect. Control Hosp. Epidemiol. 1999, 20, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Skogas, J.; Marvik, R. Measures taken to reduce damage and repair costs of rigid endoscopes during their handling and processing in surgical practice. Minim. Invasive Ther. Allied Technol. 2003, 12, 76–81. [Google Scholar] [CrossRef]
- Ofstead, C.L.; Heymann, O.L.; Quick, M.R.; Eiland, J.E.; Wetzler, H.P. Residual moisture and waterborne pathogens inside flexible endoscopes: Evidence from a multisite study of endoscope drying effectiveness. Am. J. Infect. Control 2018, 46, 689–696. [Google Scholar] [CrossRef]
- Snyder, G.M.; Wright, S.B.; Smithey, A.; Mizrahi, M.; Sheppard, M.; Hirsch, E.B.; Chuttani, R.; Heroux, R.; Yassa, D.S.; Olafsdottir, L.B.; et al. Randomized Comparison of 3 High-Level Disinfection and Sterilization Procedures for Duodenoscopes. Gastroenterology 2017, 153, 1018–1025. [Google Scholar] [CrossRef]
- Alfa, M.J.; Singh, H. Impact of wet storage and other factors on biofilm formation and contamination of patient-ready endoscopes: A narrative review. Gastrointest. Endosc. 2020, 91, 236–247. [Google Scholar] [CrossRef]
- Hasan, S.; Hartl, R.; Hofstetter, C.P. The benefit zone of full-endoscopic spine surgery. J. Spine Surg. 2019, 5, S41–S56. [Google Scholar] [CrossRef]
- Hoogland, T.; Schubert, M.; Miklitz, B.; Ramirez, A. Transforaminal posterolateral endoscopic discectomy with or without the combination of a low-dose chymopapain: A prospective randomized study in 280 consecutive cases. Spine 2006, 31, E890–E897. [Google Scholar] [CrossRef] [PubMed]
- Mahan, M.A.; Prasse, T.; Kim, R.B.; Sivakanthan, S.; Kelly, K.A.; Kashlan, O.N.; Bredow, J.; Eysel, P.; Wagner, R.; Bajaj, A.; et al. Full-endoscopic spine surgery diminishes surgical site infections—A propensity score-matched analysis. Spine J. 2023, 23, 695–702. [Google Scholar] [CrossRef] [PubMed]
- Choi, K.B.; Lee, C.D.; Lee, S.H. Pyogenic spondylodiscitis after percutaneous endoscopic lumbar discectomy. J. Korean Neurosurg. Soc. 2010, 48, 455–460. [Google Scholar] [CrossRef] [PubMed]
- Kenters, N.; Huijskens, E.G.; Meier, C.; Voss, A. Infectious diseases linked to cross-contamination of flexible endoscopes. Endosc. Int. Open 2015, 3, E259–E265. [Google Scholar] [CrossRef] [PubMed]
- McCafferty, C.E.; Aghajani, M.J.; Abi-Hanna, D.; Gosbell, I.B.; Jensen, S.O. An update on gastrointestinal endoscopy-associated infections and their contributing factors. Ann. Clin. Microbiol. Antimicrob. 2018, 17, 36. [Google Scholar] [CrossRef] [PubMed]
- Harlow, C.; Sivananthan, A.; Ayaru, L.; Patel, K.; Darzi, A.; Patel, N. Endoscopic submucosal dissection: An update on tools and accessories. Ther. Adv. Gastrointest. Endosc. 2020, 13, 2631774520957220. [Google Scholar] [CrossRef] [PubMed]
- Herve, R.; Keevil, C.W. Current limitations about the cleaning of luminal endoscopes. J. Hosp. Infect. 2013, 83, 22–29. [Google Scholar] [CrossRef]
- Urban, J.P.; Smith, S.; Fairbank, J.C. Nutrition of the intervertebral disc. Spine 2004, 29, 2700–2709. [Google Scholar] [CrossRef]
- Little, R.M.; Deal, A.M.; Zanation, A.M.; McKinney, K.; Senior, B.A.; Ebert, C.S., Jr. Occupational hazards of endoscopic surgery. Int. Forum Allergy Rhinol. 2012, 2, 212–216. [Google Scholar] [CrossRef]
- Lawrentschuk, N.; Fleshner, N.E.; Bolton, D.M. Laparoscopic lens fogging: A review of etiology and methods to maintain a clear visual field. J. Endourol. 2010, 24, 905–913. [Google Scholar] [CrossRef]
- Arianpour, A.; Tremblay, E.J.; Stamenov, I.; Ford, J.E.; Schanzlin, D.J.; Lo, Y. An optomechanical model eye for ophthalmological refractive studies. J. Refract. Surg. 2013, 29, 126–132. [Google Scholar] [CrossRef] [PubMed]
- Bayrakceken, K.; Hondur, A.M.; Atalay, H.T.; Aribas, Y.K. Real-life comparison of the viewing angle and the image quality of two commonly used viewing systems for vitreoretinal surgery. Turk. J. Med. Sci. 2020, 50, 689–696. [Google Scholar] [CrossRef] [PubMed]
- Minaker, S.A.; Mason, R.H.; Chow, D.R. Optimizing Color Performance of the Ngenuity 3-Dimensional Visualization System. Ophthalmol. Sci. 2021, 1, 100054. [Google Scholar] [CrossRef] [PubMed]
- Duarte, R.M.; Vaccaro, A.R. Spinal infection: State of the art and management algorithm. Eur. Spine J. 2013, 22, 2787–2799. [Google Scholar] [CrossRef] [PubMed]
- Ofstead, C.L.; Hopkins, K.M.; Buro, B.L.; Eiland, J.E.; Wetzler, H.P. Challenges in achieving effective high-level disinfection in endoscope reprocessing. Am. J. Infect. Control 2020, 48, 309–315. [Google Scholar] [CrossRef] [PubMed]
- Epstein, L.; Hunter, J.C.; Arwady, M.A.; Tsai, V.; Stein, L.; Gribogiannis, M.; Frias, M.; Guh, A.Y.; Laufer, A.S.; Black, S.; et al. New Delhi metallo-beta-lactamase-producing carbapenem-resistant Escherichia coli associated with exposure to duodenoscopes. JAMA 2014, 312, 1447–1455. [Google Scholar] [CrossRef]
- Bajolet, O.; Ciocan, D.; Vallet, C.; de Champs, C.; Vernet-Garnier, V.; Guillard, T.; Brasme, L.; Thiefin, G.; Cadiot, G.; Bureau-Chalot, F. Gastroscopy-associated transmission of extended-spectrum beta-lactamase-producing Pseudomonas aeruginosa. J. Hosp. Infect. 2013, 83, 341–343. [Google Scholar] [CrossRef]
- Ofstead, C.L.; Wetzler, H.P.; Eiland, J.E.; Heymann, O.L.; Held, S.B.; Shaw, M.J. Assessing residual contamination and damage inside flexible endoscopes over time. Am. J. Infect. Control 2016, 44, 1675–1677. [Google Scholar] [CrossRef]
- Ofstead, C.L.; Wetzler, H.P.; Snyder, A.K.; Horton, R.A. Endoscope reprocessing methods: A prospective study on the impact of human factors and automation. Gastroenterol. Nurs. 2010, 33, 304–311. [Google Scholar] [CrossRef]
- Chua, T.; Halim, N.; Reicher, S. Recent Advances in Endoscope Disinfection: Where Do We Stand in the COVID era? Tech. Innov. Gastrointest. Endosc. 2021, 23, 190–198. [Google Scholar] [CrossRef]
- Ciocirlan, M. Low-cost disposable endoscope: Pros and cons. Endosc. Int. Open 2019, 7, E1184–E1186. [Google Scholar] [CrossRef] [PubMed]
- Rutala, W.A.; Kanamori, H.; Sickbert-Bennett, E.E.; Weber, D.J. What’s new in reprocessing endoscopes: Are we going to ensure “the needs of the patient come first” by shifting from disinfection to sterilization? Am. J. Infect. Control 2019, 47S, A62–A66. [Google Scholar] [CrossRef] [PubMed]
- Ryu, K.; Jang, S. Single Use (Disposable) Duodenoscope: Recent Development and Future. Clin. Endosc. 2022, 55, 191–196. [Google Scholar] [CrossRef] [PubMed]
- FDA Recommends Health Care Facilities and Manufacturers Begin Transitioning to Duodenoscopes with Disposable Components to Reduce Risk of Patient Infection. Available online: https://www.fda.gov/news-events/press-announcements/fda-recommends-health-care-facilities-and-manufacturers-begin-transitioning-duodenoscopes-disposable (accessed on 29 August 2019).
- Courdier, S.; Garbin, O.; Hummel, M.; Thoma, V.; Ball, E.; Favre, R.; Wattiez, A. Equipment failure: Causes and consequences in endoscopic gynecologic surgery. J. Minim. Invasive Gynecol. 2009, 16, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Paracchini, S.; Bustos, B.; Aviles, R.; Bourdel, N.; Canis, M.; Rabischong, B.; Slim, K.; Botchorishvili, R. Equipment failures in laparoscopic surgery: Causes and consequences. J. Visc. Surg. 2021, 158, 476–480. [Google Scholar] [CrossRef] [PubMed]
- Lewandrowski, K.U.; Tieber, F.; Hellinger, S.; Teixeira de Carvalho, P.S.; Freitas Ramos, M.R.; Xifeng, Z.; Calderaro, A.L.; Santos, T.S.D.; Ramirez Leon, J.F.; de Lima, E.S.M.S.; et al. Durability of Endoscopes Used During Routine Lumbar Endoscopy: An Analysis of Use Patterns, Common Failure Modes, Impact on Patient Care, and Contingency Plans. Int. J. Spine Surg. 2021, 15, 1147–1160. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Khanicheh, A.; Leiner, D.; Shafer, D.; Zobel, J. Endoscope field of view measurement. Biomed. Opt. Express 2017, 8, 1441–1454. [Google Scholar] [CrossRef]
- Choi, H.; Seo, J.G.; Park, D.H.; Kang, E.S. Chapter 35—Precision distortion correction technique based on FOV model for wide-angle cameras in automotive sector. In Emerging Trends in Image Processing, Computer Vision and Pattern Recognition; Deligiannidis, L., Arabnia, H.R., Eds.; Morgan Kaufmann: Boston, MA, USA, 2015; pp. 533–549. [Google Scholar]
- Ju, C.I.; Lee, S.M. Complications and Management of Endoscopic Spinal Surgery. Neurospine 2023, 20, 56–77. [Google Scholar] [CrossRef]
- Reeve, L.; Baldrick, P. Biocompatibility assessments for medical devices—Evolving regulatory considerations. Expert. Rev. Med. Devices 2017, 14, 161–167. [Google Scholar] [CrossRef]
- Jagadeeswaran, I.; Chandran, S. ISO 11135: Sterilization of Health-Care Products—Ethylene Oxide, Requirements for Development, Validation and Routine Control of a Sterilization Process for Medical Devices. In Medical Device Guidelines and Regulations Handbook; Springer: Berlin/Heidelberg, Germany, 2022; pp. 145–153. [Google Scholar]
- ISO 11737; Wasowska, A. Microbiological Tests Performed According to the PN-EN ISO 11737 Polish Norm. ISO: Geneva, Switzerland, 2018.
- IEC 62304; Jordan, P. Medical Device Software-Software Lifecycle Processes. ISO: Geneva, Switzerland, 2006.
- Grob, A.; Biersach, B.; Peck, J. Risk Management And IEC 60601-1: Assessing Compliance. Biomed. Instrum. Technol. 2015, 49, 55–59. [Google Scholar] [CrossRef]
- Ferlito, S.; La Mantia, I.; Caruso, S.; Cammaroto, G.; Chiesa-Estomba, C.M.; Iannella, G.; Nocera, F.; Ingrassia, A.; Cocuzza, S.; Vicini, C.; et al. High Definition Three-Dimensional Exoscope (VITOM 3D) in E.N.T. Surgery: A Systematic Review of Current Experience. J. Clin. Med. 2022, 11, 3639. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Health; Care Research Global Health Research Unit on Global Surgery. Reducing the environmental impact of surgery on a global scale: Systematic review and co-prioritization with healthcare workers in 132 countries. Br. J. Surg. 2023, 110, 804–817. [Google Scholar] [CrossRef] [PubMed]







| Medium | Distance | Optic Endoscope (Mean ± SD) | Digital Endoscope (Mean ± SD) | p Value |
|---|---|---|---|---|
| Air | 10 mm | 6.8 ± 0.13 | 8.2 ± 0.14 | <0.001 |
| Air | 20 mm | 13.2 ± 0.16 | 16.0 ± 0.19 | <0.001 |
| Air | 30 mm | 20.1 ± 0.19 | 23.8 ± 0.21 | <0.001 |
| Water | 10 mm | 4.3 ± 0.10 | 5.2 ± 0.10 | <0.001 |
| Water | 20 mm | 8.2 ± 0.12 | 9.5 ± 0.14 | <0.001 |
| Water | 30 mm | 11.3 ± 0.15 | 14.0 ± 0.13 | <0.001 |
| Distance | Optic Endoscope | Digital Endoscope |
|---|---|---|
| 3 mm | 3–4 (11.30 lp/mm) | 4–4 (22.62 lp/mm) |
| 5 mm | 3–6 (14.3 lp/mm) | 4–2 (17.95 lp/mm) |
| 10 mm | 3–5 (12.7 lp/mm) | 3–5 (12.7 lp/mm) |
| 15 mm | 3–2 (8.98 lp/mm) | 3–3 (10.10 lp/mm) |
| 20 mm | 3–1 (8 lp/mm) | 3–1 (8 lp/mm) |
| Digital Endoscope | Optic Endoscope | |
|---|---|---|
| Weight | Lighter (39 g) | Heavier (214 g) |
| Endoscope characteristics | Single-use | Repetitive use |
| Field of view | Larger (100–131°) | Smaller (89°) |
| Shape of visual field | Square | Circle |
| Distortion | Smaller (−16.0%) | Larger (−17.6%) |
| Resolution | Better at close distances | Better at longer distances |
| Color difference | Larger (ΔC: 17.7, ΔE: 25.3) | Smaller (ΔC: 13.1, ΔE: 24.4) |
| Grey scale | 20 levels | 17 levels |
| Luminance | Even | Central |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cheng, S.-H.; Lin, Y.-T.; Lu, H.-T.; Tsuei, Y.-C.; Chu, W.; Chu, W.-C. The Evolution of Spinal Endoscopy: Design and Image Analysis of a Single-Use Digital Endoscope Versus Traditional Optic Endoscope. Bioengineering 2024, 11, 99. https://doi.org/10.3390/bioengineering11010099
Cheng S-H, Lin Y-T, Lu H-T, Tsuei Y-C, Chu W, Chu W-C. The Evolution of Spinal Endoscopy: Design and Image Analysis of a Single-Use Digital Endoscope Versus Traditional Optic Endoscope. Bioengineering. 2024; 11(1):99. https://doi.org/10.3390/bioengineering11010099
Chicago/Turabian StyleCheng, Shih-Hao, Yen-Tsung Lin, Hsin-Tzu Lu, Yu-Chuan Tsuei, William Chu, and Woei-Chyn Chu. 2024. "The Evolution of Spinal Endoscopy: Design and Image Analysis of a Single-Use Digital Endoscope Versus Traditional Optic Endoscope" Bioengineering 11, no. 1: 99. https://doi.org/10.3390/bioengineering11010099
APA StyleCheng, S.-H., Lin, Y.-T., Lu, H.-T., Tsuei, Y.-C., Chu, W., & Chu, W.-C. (2024). The Evolution of Spinal Endoscopy: Design and Image Analysis of a Single-Use Digital Endoscope Versus Traditional Optic Endoscope. Bioengineering, 11(1), 99. https://doi.org/10.3390/bioengineering11010099






