Virtual Reality Gait Training to Promote Balance and Gait Among Older People: A Randomized Clinical Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Determination of the Sample Size
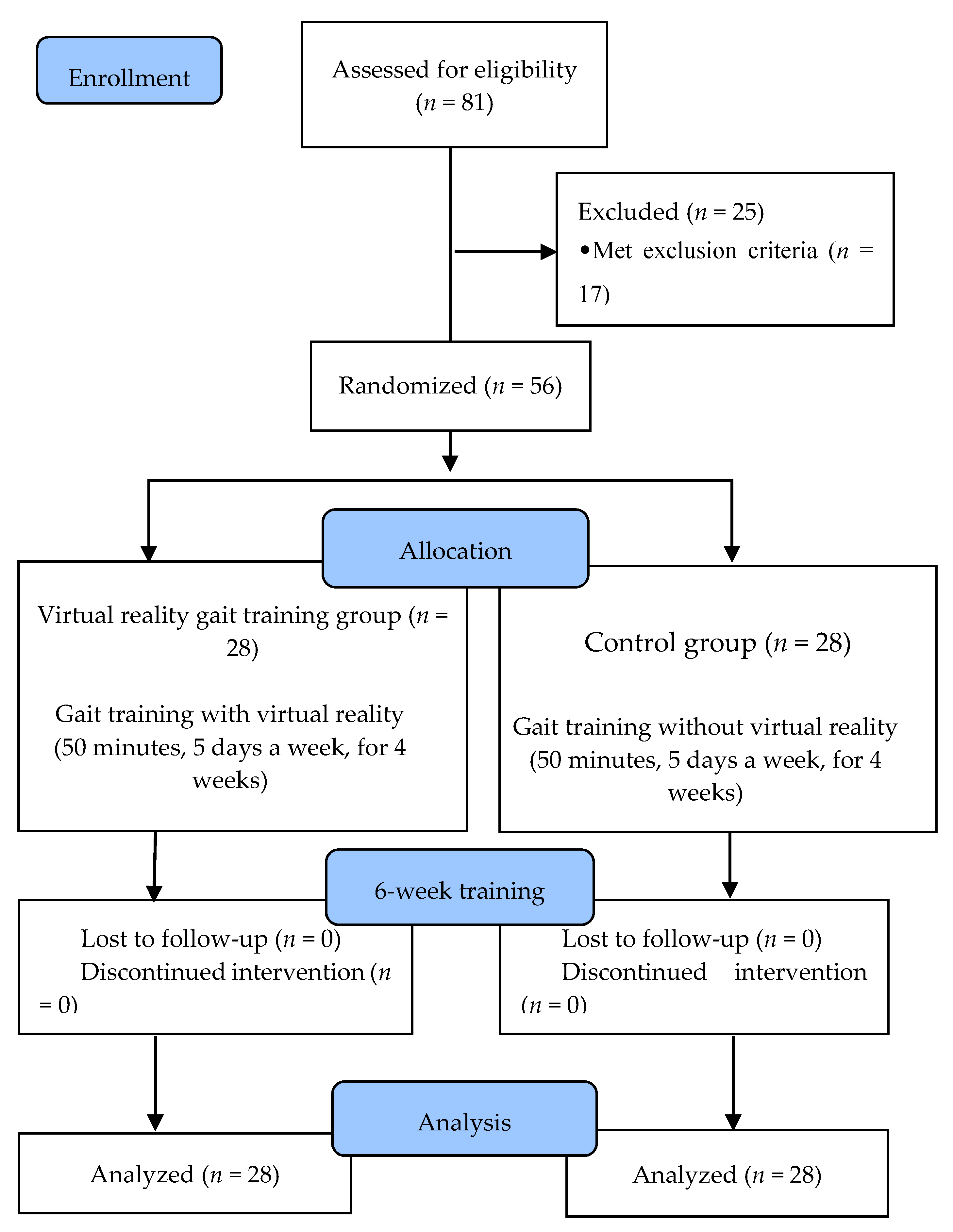
2.3. Procedure
2.4. Virtual Reality Gait Training with Non-Motorized Treadmill
2.5. Virtual Reality Device and Motion Tracking
2.6. Outcome Measurements
2.7. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Bohannon, R.W.; Andrews, A.W.; Thomas, M.W. Walking speed: Reference values and correlates for older adults. J. Orthop. Sports Phys. Ther. 1996, 24, 86–90. [Google Scholar] [CrossRef] [PubMed]
- Morley, J.E. Mobility performance: A high-tech test for geriatricians. J. Gerontol. A Biol. Sci. Med. Sci. 2003, 58, 712–714. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rubenstein, L.Z. Falls in older people: Epidemiology, risk factors and strategies for prevention. Age Ageing 2006, 35 (Suppl. 2), ii37–ii41. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mackenzie, L.; Byles, J.; D’Este, C. Validation of self-reported fall events in intervention studies. Clin. Rehabil. 2006, 20, 331–339. [Google Scholar] [CrossRef]
- Sartini, M.; Cristina, M.L.; Spagnolo, A.M.; Cremonesi, P.; Costaguta, C.; Monacelli, F.; Garau, J.; Odetti, P. The epidemiology of domestic injurious falls in a community dwelling elderly population: An outgrowing economic burden. Eur. J. Public Health 2010, 20, 604–606. [Google Scholar] [CrossRef] [Green Version]
- National Center for Health Statistics. Older Americans 2016: Key Indicators of Well-Being. Federal Interagency Forum on Aging-Related Statistics; US Government Printing Office: Washington, DC, USA, 2016.
- Winter, D.A.; Patla, A.E.; Frank, J.S.; Walt, S.E. Biomechanical walking pattern changes in the fit and healthy elderly. Phys. Ther. 1990, 70, 340–347. [Google Scholar] [CrossRef]
- Cromwell, R.; Newton, R.; Grisso, J.; Edwards, W. Relationship between Select Balance Measures and a Gait Stability Ratio in Individuals Who Are Known Fallers; Control of Posture and Gait: Maastricht, The Netherlands, 2001. [Google Scholar]
- Cromwell, R.L.; Newton, R.A.; Forrest, G. Influence of vision on head stabilization strategies in older adults during walking. J. Gerontol. A Biol. Sci. Med. Sci. 2002, 57, M442–M448. [Google Scholar] [CrossRef] [Green Version]
- Alton, F.; Baldey, L.; Caplan, S.; Morrissey, M. A kinematic comparison of overground and treadmill walking. Clin. Biomech. 1998, 13, 434–440. [Google Scholar] [CrossRef]
- Riley, P.O.; Paolini, G.; Della Croce, U.; Paylo, K.W.; Kerrigan, D.C. A kinematic and kinetic comparison of overground and treadmill walking in healthy subjects. Gait Posture 2007, 26, 17–24. [Google Scholar] [CrossRef]
- Pierrynowski, M.R.; Gross, A.; Miles, M.; Galea, V.; McLaughlin, L.; McPhee, C. Reliability of the long-range power-law correlations obtained from the bilateral stride intervals in asymptomatic volunteers whilst treadmill walking. Gait Posture 2005, 22, 46–50. [Google Scholar] [CrossRef]
- Terrier, P.; Deriaz, O. Kinematic variability, fractal dynamics and local dynamic stability of treadmill walking. J. Neuroeng. Rehabil. 2011, 8, 12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mirelman, A.; Rochester, L.; Reelick, M.; Nieuwhof, F.; Pelosin, E.; Abbruzzese, G.; Dockx, K.; Nieuwboer, A.; Hausdorff, J.M. V-time: A treadmill training program augmented by virtual reality to decrease fall risk in older adults: Study design of a randomized controlled trial. BMC Neurol. 2013, 13, 15. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- de Melo, G.E.L.; Kleiner, A.F.R.; Lopes, J.B.P.; Dumont, A.J.L.; Lazzari, R.D.; Galli, M.; Oliveira, C.S. Effect of virtual reality training on walking distance and physical fitness in individuals with parkinson’s disease. NeuroRehabilitation 2018, 42, 473–480. [Google Scholar] [CrossRef] [PubMed]
- Fung, J.; Richards, C.L.; Malouin, F.; McFadyen, B.J.; Lamontagne, A. A treadmill and motion coupled virtual reality system for gait training post-stroke. Cyberpsychol. Behav. 2006, 9, 157–162. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Betances, R.I.; Jimenez-Mixco, V.; Arredondo, M.T.; Cabrera-Umpierrez, M.F. Using virtual reality for cognitive training of the elderly. Am. J. Alzheimer’s Dis. Other Demen. 2015, 30, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Liao, Y.Y.; Chen, I.H.; Lin, Y.J.; Chen, Y.; Hsu, W.C. Effects of virtual reality-based physical and cognitive training on executive function and dual-task gait performance in older adults with mild cognitive impairment: A randomized control trial. Front. Aging Neurosci. 2019, 11, 162. [Google Scholar] [CrossRef] [Green Version]
- Yang, S.; Hwang, W.H.; Tsai, Y.C.; Liu, F.K.; Hsieh, L.F.; Chern, J.S. Improving balance skills in patients who had stroke through virtual reality treadmill training. Am. J. Phys. Med. Rehabil. 2011, 90, 969–978. [Google Scholar] [CrossRef]
- Cho, K.H.; Lee, W.H. Effect of treadmill training based real-world video recording on balance and gait in chronic stroke patients: A randomized controlled trial. Gait Posture 2014, 39, 523–528. [Google Scholar] [CrossRef]
- Lee, J.; Lee, K.; Song, C. Speed-interactive treadmill training using smartphone-based motion tracking technology improves gait in stroke patients. J. Motor Behav. 2017, 49, 675–685. [Google Scholar] [CrossRef]
- Cho, C.; Hwang, W.; Hwang, S.; Chung, Y. Treadmill training with virtual reality improves gait, balance, and muscle strength in children with cerebral palsy. Tohoku J. Exp. Med. 2016, 238, 213–218. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- de Rooij, I.J.; van de Port, I.G.; Meijer, J.G. Effect of virtual reality training on balance and gait ability in patients with stroke: Systematic review and meta-analysis. Phys. Ther. 2016, 96, 1905–1918. [Google Scholar] [CrossRef] [PubMed]
- Darter, B.J.; Wilken, J.M. Gait training with virtual reality-based real-time feedback: Improving gait performance following transfemoral amputation. Phys. Ther. 2011, 91, 1385–1394. [Google Scholar] [CrossRef] [PubMed]
- De Rooij, I.J.M.; van de Port, I.G.L.; Visser-Meily, J.M.A.; Meijer, J.G. Virtual reality gait training versus non-virtual reality gait training for improving participation in subacute stroke survivors: Study protocol of the virtas randomized controlled trial. Trials 2019, 20, 89. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Franks, K.A.; Brown, L.E.; Coburn, J.W.; Kersey, R.D.; Bottaro, M. Effects of motorized vs non-motorized treadmill training on hamstring/quadriceps strength ratios. J. Sports Sci. Med. 2012, 11, 71–76. [Google Scholar]
- Smoliga, J.M.; Hegedus, E.J.; Ford, K.R. Increased physiologic intensity during walking and running on a non-motorized, curved treadmill. Phys. Ther. Sport 2015, 16, 262–267. [Google Scholar] [CrossRef] [PubMed]
- Highton, J.M.; Lamb, K.L.; Twist, C.; Nicholas, C. The reliability and validity of short-distance sprint performance assessed on a nonmotorized treadmill. J. Strength Cond. Res. 2012, 26, 458–465. [Google Scholar] [CrossRef] [Green Version]
- Berg, K.O.; Wood-Dauphinee, S.L.; Williams, J.I.; Maki, B. Measuring balance in the elderly: Validation of an instrument. Can. J. Public Health 1992, 83 (Suppl. 2), S7–S11. [Google Scholar]
- Duncan, P.W.; Weiner, D.K.; Chandler, J.; Studenski, S. Functional reach: A new clinical measure of balance. J. Gerontol. 1990, 45, M192–M197. [Google Scholar] [CrossRef]
- Mathias, S.; Nayak, U.S.; Isaacs, B. Balance in elderly patients: The “get-up and go” test. Arch. Phys. Med. Rehabil. 1986, 67, 387–389. [Google Scholar]
- Wilson, P.N.; Foreman, N.; Stanton, D. Virtual reality, disability and rehabilitation. Disabil. Rehabil. 1997, 19, 213–220. [Google Scholar] [CrossRef]
- Persad, C.C.; Cook, S.; Giordani, B. Assessing falls in the elderly: Should we use simple screening tests or a comprehensive fall risk evaluation? Eur. J. Phys. Rehabil. Med. 2010, 46, 249–259. [Google Scholar] [PubMed]
- Jonsson, E.; Seiger, A.; Hirschfeld, H. One-leg stance in healthy young and elderly adults: A measure of postural steadiness? Clin. Biomech. (Bristol Avon) 2004, 19, 688–694. [Google Scholar] [CrossRef] [PubMed]
- Bohannon, R.W.; Larkin, P.A.; Cook, A.C.; Gear, J.; Singer, J. Decrease in timed balance test scores with aging. Phys. Ther. 1984, 64, 1067–1070. [Google Scholar] [CrossRef] [PubMed]
- Perry, J.; Burnfield, J. Gait Analysis: Normal and Pathological Function, 2nd ed.; Slack Incorporated: Thorofare, NJ, USA, 2010. [Google Scholar]
- Bischoff, H.A.; Stahelin, H.B.; Monsch, A.U.; Iversen, M.D.; Weyh, A.; von Dechend, M.; Akos, R.; Conzelmann, M.; Dick, W.; Theiler, R. Identifying a cut-off point for normal mobility: A comparison of the timed ‘up and go’ test in community-dwelling and institutionalised elderly women. Age Ageing 2003, 32, 315–320. [Google Scholar] [CrossRef] [Green Version]
- Callisaya, M.L.; Blizzard, L.; McGinley, J.L.; Srikanth, V.K. Risk of falls in older people during fast-walking—The tascog study. Gait Posture 2012, 36, 510–515. [Google Scholar] [CrossRef]
- Hausdorff, J.M.; Rios, D.A.; Edelberg, H.K. Gait variability and fall risk in community-living older adults: A 1-year prospective study. Arch. Phys. Med. Rehabil. 2001, 82, 1050–1056. [Google Scholar] [CrossRef]
- Mirelman, A.; Rochester, L.; Maidan, I.; Del Din, S.; Alcock, L.; Nieuwhof, F.; Rikkert, M.O.; Bloem, B.R.; Pelosin, E.; Avanzino, L.; et al. Addition of a non-immersive virtual reality component to treadmill training to reduce fall risk in older adults (v-time): A randomised controlled trial. Lancet 2016, 388, 1170–1182. [Google Scholar] [CrossRef] [Green Version]
- Thaler-Kall, K.; Peters, A.; Thorand, B.; Grill, E.; Autenrieth, C.S.; Horsch, A.; Meisinger, C. Description of spatio-temporal gait parameters in elderly people and their association with history of falls: Results of the population-based cross-sectional kora-age study. BMC Geriatr. 2015, 15, 32. [Google Scholar] [CrossRef] [Green Version]
| Variables | VRGT Group (n = 28) | Control Group (n = 28) | χ2/t | p |
|---|---|---|---|---|
| Age (year) | 81.01 ± 6.89 | 79.47 ± 6.15 | 0.879 | 0.383 |
| Height (cm) | 166.36 ± 6.42 | 164.21 ± 8.58 | 1.058 | 0.295 |
| Weight (kg) | 63.12 ± 6.53 | 61.52 ± 8.62 | 0.782 | 0.438 |
| BMI (point) | 22.81 ± 2.14 | 22.83 ± 2.76 | 0.024 | 0.981 |
| MMSE-K | 25.86 ± 1.38 | 25.64 ± 0.91 | 0.686 | 0.496 |
| Gender (male/female) | 16/12 | 15/13 | 0.788 | 0.072 |
| Variables | VRGT Group (n = 28) | Control Group (n = 28) | χ2/t | p | |
|---|---|---|---|---|---|
| OLS (sec) | Pre | 28.82 ± 6.32 | 27.76 ± 7.01 | 0.594 | 0.555 |
| Post | 37.64 ± 9.29 | 29.45 ± 7.40 | |||
| Change Score | 8.82 ± 3.58 | 1.69 ± 4.87 | 6.240 | 0.000 | |
| t | 13.026 | 1.837 | |||
| p | 0.000 | 0.078 | |||
| BBS (point) | Pre | 46.18 ± 3.86 | 44.89 ± 4.59 | 1.135 | 0.262 |
| Post | 46.39 ± 4.34 | 45.25 ± 4.64 | |||
| Change Score | 0.21 ± 1.10 | 0.36 ± 1.13 | 0.479 | 0.634 | |
| t | 1.030 | 1.676 | |||
| p | 0.312 | 0.106 | |||
| FRT (cm) | Pre | 25.19 ± 5.31 | 25.45 ± 4.26 | 0.202 | 0.841 |
| Post | 23.80 ± 5.38 | 25.39 ± 3.58 | |||
| Change Score | −1.39 ± 7.17 | −0.06 ± 5.73 | 0.764 | 0.448 | |
| t | 1.024 | 0.057 | |||
| p | 0.315 | 0.955 | |||
| TUG (sec) | Pre | 13.24 ± 5.91 | 12.55 ± 4.48 | 0.486 | 0.629 |
| Post | 11.92 ± 5.42 | 12.33 ± 4.86 | |||
| Change Score | −1.31 ± 1.51 | −0.22 ± 0.83 | 3.339 | 0.002 | |
| t | 4.600 | 1.431 | |||
| p | 0.000 | 0.164 |
| Variables | VRGT Group (n = 28) | Control Group (n = 28) | χ2/t | p | |
|---|---|---|---|---|---|
| Velocity (m/s) | Pre | 1.02 ± 0.04 | 1.06 ± 0.14 | 1.529 | 0.132 |
| Post | 1.05 ± 0.04 | 1.08 ± 0.09 | |||
| Change Score | 0.03 ± 0.04 | 0.02 ± 0.13 | 0.245 | 0.807 | |
| t | 3.452 | 0.816 | |||
| p | 0.002 | 0.422 | |||
| Cadence (step/min) | Pre | 113.29 ± 20.77 | 121.63 ± 23.86 | 1.395 | 0.169 |
| Post | 109.98 ± 12.95 | 119.65 ± 23.47 | |||
| Change Score | −3.32 ± 9.24 | −1.98 ± 9.24 | 0.541 | 0.591 | |
| t | 1.900 | 1.137 | |||
| p | 0.068 | 0.266 | |||
| Stride time (sec) | Pre | 1.09 ± 0.17 | 1.02 ± 0.19 | 1.366 | 0.178 |
| Post | 1.11 ± 0.13 | 1.04 ± 0.18 | |||
| Change Score | 0.02 ± 0.06 | 0.01 ± 0.06 | 0.154 | 0.878 | |
| t | 1.423 | 1.176 | |||
| p | 0.166 | 0.250 | |||
| Step time (sec) | Pre | 0.54 ± 0.09 | 0.51 ± 0.10 | 1.366 | 0.178 |
| Post | 0.55 ± 0.06 | 0.52 ± 0.09 | |||
| Change Score | 0.01 ± 0.03 | 0.01 ± 0.03 | 0.154 | 0.878 | |
| t | 1.423 | 1.176 | |||
| p | 0.166 | 0.250 |
| Variables | VRGT Group (n = 28) | Control Group (n = 28) | χ2/t | p | |
|---|---|---|---|---|---|
| Stride length (cm) | Pre | 110.99 ± 16.29 | 109.17 ± 13.13 | 0.462 | 0.646 |
| Post | 115.61 ± 12.06 | 111.29 ± 15.02 | |||
| Change Score | 4.61 ± 5.01 | 2.12 ± 3.60 | 2.136 | 0.037 | |
| t | 4.875 | 3.134 | |||
| p | 0.000 | 0.004 | |||
| Step length (cm) | Pre | 55.50 ± 8.14 | 54.58 ± 6.56 | 0.462 | 0.646 |
| Post | 57.80 ± 6.03 | 55.65 ± 7.51 | |||
| Change Score | 2.31 ± 2.50 | 1.06 ± 1.80 | 2.136 | 0.037 | |
| t | 4.875 | 3.134 | |||
| p | 0.000 | 0.004 | |||
| Step width (cm) | Pre | 9.95 ± 2.34 | 10.13 ± 1.84 | 0.327 | 0.745 |
| Post | 9.15 ± 2.25 | 10.47 ± 2.11 | |||
| Change Score | −0.80 ± 0.40 | 0.34 ± 2.52 | 2.364 | 0.022 | |
| t | 10.713 | 0.709 | |||
| p | 0.000 | 0.485 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, K. Virtual Reality Gait Training to Promote Balance and Gait Among Older People: A Randomized Clinical Trial. Geriatrics 2021, 6, 1. https://doi.org/10.3390/geriatrics6010001
Lee K. Virtual Reality Gait Training to Promote Balance and Gait Among Older People: A Randomized Clinical Trial. Geriatrics. 2021; 6(1):1. https://doi.org/10.3390/geriatrics6010001
Chicago/Turabian StyleLee, Kyeongjin. 2021. "Virtual Reality Gait Training to Promote Balance and Gait Among Older People: A Randomized Clinical Trial" Geriatrics 6, no. 1: 1. https://doi.org/10.3390/geriatrics6010001




