Fungal Infections in the ICU during the COVID-19 Pandemic in Mexico
Abstract
:1. Introduction
2. Materials and Methods
3. Results
3.1. COVID-19-Associated Pulmonary Aspergillosis (CAPA)
3.2. COVID-19-Associated Candidiasis
3.3. COVID-19-Associated Mucormycosis (CAM) and Cryptococcosis (CACr)
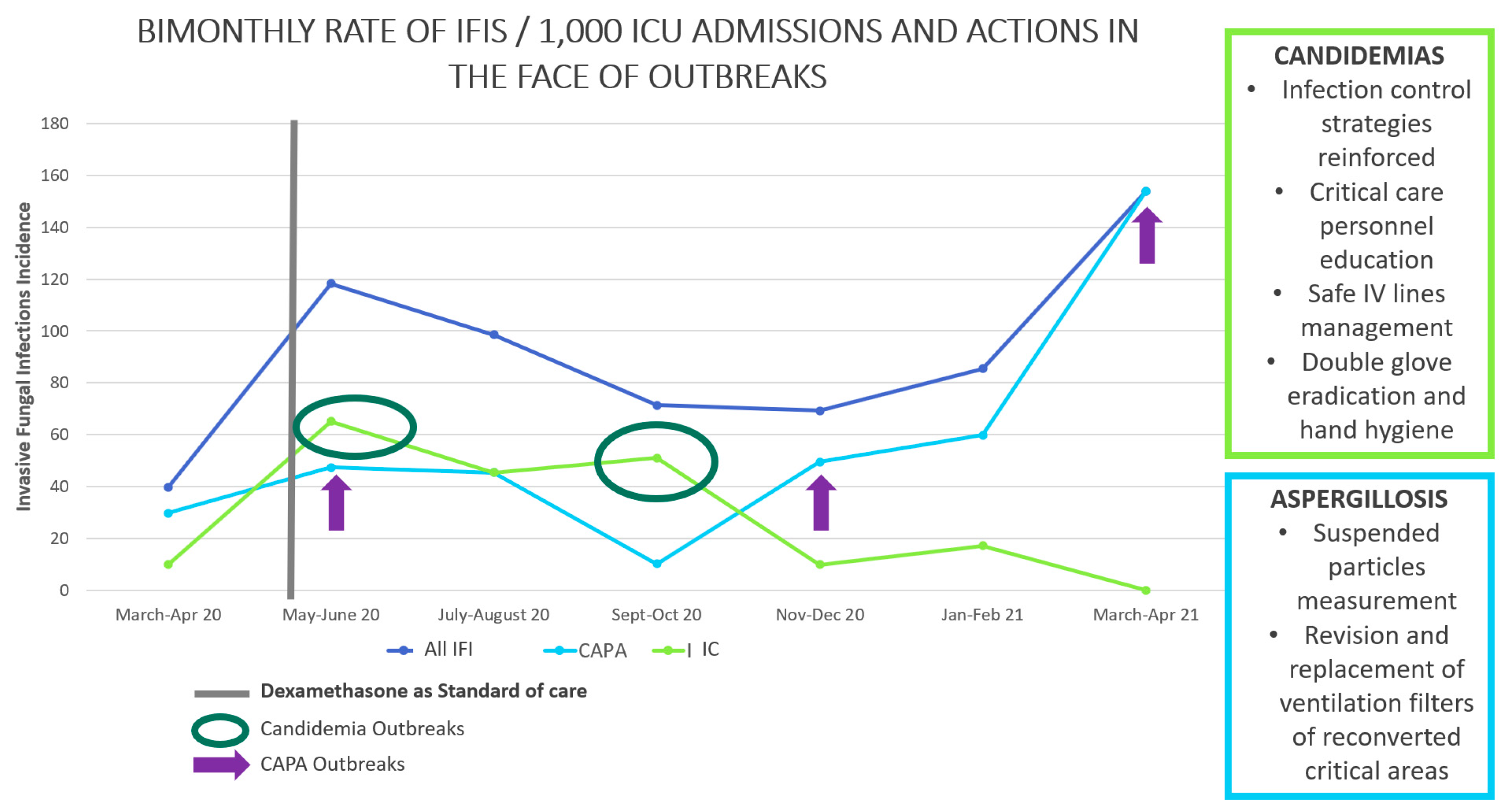
3.4. IFI Cases during the Time of Pandemic
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Arastehfar, A.; Shaban, T.; Zarrinfar, H.; Roudbary, M.; Ghazanfari, M.; Hedayati, M.T.; Sedaghat, A.; Ilkit, M.; Najafzadeh, M.J.; Perlin, D.S. Candidemia among Iranian Patients with Severe COVID-19 Admitted to ICUs. J. Fungi 2021, 7, 280. [Google Scholar] [CrossRef]
- Bartoletti, M.; Pascale, R.; Cricca, M.; Rinaldi, M.; Maccaro, A.; Bussini, L.; Fornaro, G.; Tonetti, T.; Pizzilli, G.; Francalanci, E.; et al. Epidemiology of Invasive Pulmonary Aspergillosis among Intubated Patients with COVID-19: A Prospective Study. Clin. Infect. Dis. 2021, 73, E3606–E3614. [Google Scholar] [CrossRef] [PubMed]
- Hoenigl, M.; Seidel, D.; Carvalho, A.; Rudramurthy, S.M.; Arastehfar, A.; Gangneux, J.P.; Nasir, N.; Bonifaz, A.; Araiza, J.; Klimko, N.; et al. The Emergence of COVID-19 Associated Mucormycosis: A Review of Cases from 18 Countries. Lancet Microbe 2022, 3, e543–e552. [Google Scholar] [CrossRef]
- Casalini, G.; Giacomelli, A.; Ridolfo, A.; Gervasoni, C.; Antinori, S. Invasive Fungal Infections Complicating COVID-19: A Narrative Review. J. Fungi 2021, 7, 921. [Google Scholar] [CrossRef] [PubMed]
- Arastehfar, A.; Carvalho, A.; van de Veerdonk, F.L.; Jenks, J.D.; Koehler, P.; Krause, R.; Cornely, O.A.; Perlin, D.S.; Lass-Flörl, C.; Hoenigl, M. COVID-19 Associated Pulmonary Aspergillosis (CAPA)—From Immunology to Treatment. J. Fungi 2020, 6, 91. [Google Scholar] [CrossRef]
- Chong, W.H.; Neu, K.P. Incidence, Diagnosis and Outcomes of COVID-19-Associated Pulmonary Aspergillosis (CAPA): A Systematic Review. J. Hosp. Infect. 2021, 113, 115–129. [Google Scholar] [CrossRef]
- Kayaaslan, B.; Eser, F.; Kaya Kalem, A.; Bilgic, Z.; Asilturk, D.; Hasanoglu, I.; Ayhan, M.; Tezer Tekce, Y.; Erdem, D.; Turan, S.; et al. Characteristics of Candidemia in COVID-19 Patients; Increased Incidence, Earlier Occurrence and Higher Mortality Rates Compared to Non-COVID-19 Patients. Mycoses 2021, 64, 1083–1091. [Google Scholar] [CrossRef] [PubMed]
- Mastrangelo, A.; Germinario, B.N.; Ferrante, M.; Frangi, C.; Li Voti, R.; Muccini, C.; Ripa, M. Candidemia in Coronavirus Disease 2019 (COVID-19) Patients: Incidence and Characteristics in a Prospective Cohort Compared with Historical Non-COVID-19 Controls. Clin. Infect. Dis. 2021, 73, E2838–E2839. [Google Scholar] [CrossRef]
- Nucci, M.; Barreiros, G.; Guimarães, L.F.; Deriquehem, V.A.S.; Castiñeiras, A.C.; Nouér, S.A. Increased Incidence of Candidemia in a Tertiary Care Hospital with the COVID-19 Pandemic. Mycoses 2021, 64, 152–156. [Google Scholar] [CrossRef]
- Riche, C.V.W.; Cassol, R.; Pasqualotto, A.C. Is the Frequency of Candidemia Increasing in COVID-19 Patients Receiving Corticosteroids? J. Fungi 2020, 6, 286. [Google Scholar] [CrossRef]
- Vélez Pintado, M.; Camiro-Zúñiga, A.; Aguilar Soto, M.; Cuenca, D.; Mercado, M.; Crabtree-Ramirez, B. COVID-19-Associated Invasive Pulmonary Aspergillosis in a Tertiary Care Center in Mexico City. Med. Mycol. 2021, 59, 828–833. [Google Scholar] [CrossRef]
- Koehler, P.; Bassetti, M.; Chakrabarti, A.; Chen, S.C.A.; Colombo, A.L.; Hoenigl, M.; Klimko, N.; Lass-Flörl, C.; Oladele, R.O.; Vinh, D.C.; et al. Defining and Managing COVID-19-Associated Pulmonary Aspergillosis: The 2020 ECMM/ISHAM Consensus Criteria for Research and Clinical Guidance. Lancet Infect. Dis. 2021, 21, e149–e162. [Google Scholar] [CrossRef] [PubMed]
- Peter Donnelly, J.; Chen, S.C.; Kauffman, C.A.; Steinbach, W.J.; Baddley, J.W.; Verweij, P.E.; Clancy, C.J.; Wingard, J.R.; Lockhart, S.R.; Groll, A.H.; et al. Revision and Update of the Consensus Definitions of Invasive Fungal Disease from the European Organization for Research and Treatment of Cancer and the Mycoses Study Group Education and Research Consortium. Clin. Infect. Dis. 2020, 71, 1367–1376. [Google Scholar] [CrossRef] [PubMed]
- Gangneux, J.P.; Dannaoui, E.; Fekkar, A.; Luyt, C.E.; Botterel, F.; De Prost, N.; Tadié, J.M.; Reizine, F.; Houzé, S.; Timsit, J.F.; et al. Fungal Infections in Mechanically Ventilated Patients with COVID-19 during the First Wave: The French Multicentre MYCOVID Study. Lancet Respir. Med. 2022, 10, 180–190. [Google Scholar] [CrossRef]
- Grasselli, G.; Zangrillo, A.; Zanella, A.; Antonelli, M.; Cabrini, L.; Castelli, A.; Cereda, D.; Coluccello, A.; Foti, G.; Fumagalli, R.; et al. Baseline Characteristics and Outcomes of 1591 Patients Infected with SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA 2020, 323, 1574–1581. [Google Scholar] [CrossRef]
- Kariyawasam, R.M.; Dingle, T.C.; Kula, B.E.; Vandermeer, B.; Sligl, W.I.; Schwartz, I.S. Defining COVID-19 Associated Pulmonary Aspergillosis: Systematic Review and Meta-Analysis. Clin. Microbiol. Infect. 2022, 28, 920–927. [Google Scholar] [CrossRef]
- Egger, M.; Bussini, L.; Hoenigl, M.; Bartoletti, M. Prevalence of COVID-19-Associated Pulmonary Aspergillosis: Critical Review and Conclusions. J. Fungi 2022, 8, 390. [Google Scholar] [CrossRef]
- Belizario, J.A.; Lopes, L.G.; Pires, R.H. Fungi in the Indoor Air of Critical Hospital Areas: A Review. Aerobiologia 2021, 37, 379–394. [Google Scholar] [CrossRef]
- de Almeida, J.N.; Doi, A.M.; Watanabe, M.J.L.; Maluf, M.M.; Calderon, C.L.; Silva, M.; Pasternak, J.; Koga, P.C.M.; Santiago, K.A.S.; Aranha, L.F.C.; et al. COVID-19-Associated Aspergillosis in a Brazilian Referral Centre: Diagnosis, Risk Factors and Outcomes. Mycoses 2022, 65, 449–457. [Google Scholar] [CrossRef] [PubMed]
- Panchabhai, T.S.; Mehta, A.C. Historical Perspectives of Bronchoscopy: Connecting the Dots. Ann. Am. Thorac. Soc. 2015, 12, 631–641. [Google Scholar] [CrossRef]
- Román-Montes, C.M.; Bojorges-Aguilar, S.; Díaz-Lomelí, P.; Cervantes-Sánchez, A.; Rangel-Cordero, A.; Martínez-Gamboa, A.; Sifuentes-Osornio, J.; Ponce-de-León, A.; González-Lara, M.F. Tracheal Aspirate Galactomannan Testing in COVID-19-Associated Pulmonary Aspergillosis. Front. Fungal Biol. 2022, 3, 1–7. [Google Scholar] [CrossRef]
- Leistner, R.; Schroeter, L.; Adam, T.; Poddubnyy, D.; Stegemann, M.; Siegmund, B.; Maechler, F.; Geffers, C.; Schwab, F.; Gastmeier, P.; et al. Corticosteroids as Risk Factor for COVID-19-Associated Pulmonary Aspergillosis in Intensive Care Patients. Crit. Care 2022, 23, 30. [Google Scholar] [CrossRef] [PubMed]
- The RECOVERY Collaborative Group. Dexamethasone in Hospitalized Patients with COVID-19. N. Engl. J. Med. 2021, 384, 693–704. [Google Scholar] [CrossRef] [PubMed]
- Ho, K.S.; Narasimhan, B.; Difabrizio, L.; Rogers, L.; Bose, S.; Li, L.; Chen, R.; Sheehan, J.; El-Halabi, M.A.; Sarosky, K.; et al. Impact of Corticosteroids in Hospitalised COVID-19 Patients. BMJ Open Respir. Res. 2021, 8, e000766. [Google Scholar] [CrossRef]
- Prattes, J.; Wauters, J.; Giacobbe, D.R.; Salmanton-García, J.; Maertens, J.; Bourgeois, M.; Reynders, M.; Rutsaert, L.; Van Regenmortel, N.; Lormans, P.; et al. Risk Factors and Outcome of Pulmonary Aspergillosis in Critically Ill Coronavirus Disease 2019 Patients—A Multinational Observational Study by the European Confederation of Medical Mycology. Clin. Microbiol. Infect. 2022, 28, 580–587. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Verma, N.; Kanaujia, R.; Chakrabarti, A.; Rudramurthy, S.M. Mortality in Critically Ill Patients with Coronavirus Disease 2019-Associated Pulmonary Aspergillosis: A Systematic Review and Meta-Analysis. Mycoses 2021, 64, 1015–1027. [Google Scholar] [CrossRef]
- Chowdhary, A.; Tarai, B.; Singh, A.; Sharma, A. Multidrug-Resistant Candida Auris Infections in Critically Ill Coronavirus Disease Patients, India, April–July 2020. Emerg. Infect. Dis. 2020, 26, 10–12. [Google Scholar] [CrossRef]
- Bonazzetti, C.; Morena, V.; Giacomelli, A.; Oreni, L.; Casalini, G.; Galimberti, L.R.; Bolis, M.; Rimoldi, M.; Ballone, E.; Colombo, R.; et al. Unexpectedly High Frequency of Enterococcal Bloodstream Infections in Coronavirus Disease 2019 Patients Admitted to an Italian ICU: An Observational Study. Crit. Care Med. 2020, 49, E31–E40. [Google Scholar] [CrossRef]
- Giacobbe, D.R.; Battaglini, D.; Ball, L.; Brunetti, I.; Bruzzone, B.; Codda, G.; Crea, F.; De Maria, A.; Dentone, C.; Di Biagio, A.; et al. Bloodstream Infections in Critically Ill Patients with COVID-19. Eur. J. Clin. Investig. 2020, 50, 1–8. [Google Scholar] [CrossRef]
- Macauley, P.; Epelbaum, O. Epidemiology and mycology of candidaemia in non-oncological medical intensive care unit patients in a tertiary center in the United States: Overall analysis and comparison between non-COVID-19 and COVID-19 cases. Mycoses 2021, 64, 634–640. [Google Scholar] [CrossRef] [PubMed]
- Koukaki, E.; Rovina, N.; Tzannis, K.; Sotiropoulou, Z.; Loverdos, K.; Koutsoukou, A.; Dimopoulos, G. Fungal Infections in the ICU during the COVID-19 Era: Descriptive and Comparative Analysis of 178 Patients. J. Fungi 2022, 8, 881. [Google Scholar] [CrossRef] [PubMed]
- Blaize, M.; Raoelina, A.; Kornblum, D.; Kamus, L.; Lampros, A.; Berger, M.; Demeret, S.; Constantin, J.M.; Monsel, A.; Mayaux, J.; et al. Occurrence of Candidemia in Patients with COVID-19 Admitted to Five ICUs in France. J. Fungi 2022, 8, 678. [Google Scholar] [CrossRef] [PubMed]
- Prestel, C.; Anderson, E.; Forsberg, K.; Lyman, M.; de Perio, M.A.; Kuhar, D.; Edwards, K.; Rivera, M.; Shugart, A.; Walters, M.; et al. Candida auris Outbreak in a COVID-19 Specialty Care Unit—Florida, July–August 2020. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 56–57. [Google Scholar] [CrossRef] [PubMed]
- Altinkaya Çavuş, M.; Sav, H. Opportunistic Candida Infections in Critical COVID-19 Patients. Polish J. Microbiol. 2022, 71, 411–419. [Google Scholar] [CrossRef] [PubMed]
- Machado, M.; Estévez, A.; Sánchez-Carrillo, C.; Guinea, J.; Escribano, P.; Alonso, R.; Valerio, M.; Padilla, B.; Bouza, E.; Muñoz, P. Incidence of Candidemia Is Higher in COVID-19 versus Non-COVID-19 Patients, but Not Driven by Intrahospital Transmission. J. Fungi 2022, 8, 305. [Google Scholar] [CrossRef]
- Seagle, E.E.; Jackson, B.R.; Lockhart, S.R.; Georgacopoulos, O.; Nunnally, N.S.; Roland, J.; Barter, D.M.; Johnston, H.L.; Czaja, C.A.; Kayalioglu, H.; et al. The Landscape of Candidemia During the Coronavirus Disease 2019 (COVID-19) Pandemic. Clin. Infect. Dis. 2022, 74, 802–811. [Google Scholar] [CrossRef] [PubMed]
- Hanson, B.M.; Dinh, A.Q.; Tran, T.T.; Arenas, S.; Pronty, D.; Gershengorn, H.B.; Ferreira, T.; Arias, C.A.; Shukla, B.S. Candida Auris Invasive Infections during a COVID-19 Case Surge. Antimicrob. Agents Chemother. 2021, 65, 1–6. [Google Scholar] [CrossRef]
- Allaw, F.; Haddad, S.F.; Habib, N.; Moukarzel, P.; Naji, N.S.; Kanafani, Z.A.; Ibrahim, A.; Zahreddine, N.K.; Spernovasilis, N.; Poulakou, G.; et al. COVID-19 and C. Auris: A Case-Control Study from a Tertiary Care Center in Lebanon. Microorganisms 2022, 10, 1011. [Google Scholar] [CrossRef]
- Corcione, S.; Montrucchio, G.; Shbaklo, N.; De Benedetto, I.; Sales, G.; Cedrone, M.; Vita, D.; Costa, C.; Zozzoli, S.; Zaccaria, T.; et al. First Cases of Candida Auris in a Referral Intensive Care Unit in Piedmont Region, Italy. Microorganisms 2022, 10, 1521. [Google Scholar] [CrossRef]
- Vaseghi, N.; Sharifisooraki, J.; Khodadadi, H.; Nami, S.; Safari, F.; Ahangarkani, F.; Meis, J.F.; Badali, H.; Morovati, H. Global Prevalence and Subgroup Analyses of Coronavirus Disease (COVID-19) Associated Candida Auris Infections (CACa): A Systematic Review and Meta-Analysis. Mycoses 2022, 65, 683–703. [Google Scholar] [CrossRef] [PubMed]
- Vinayagamoorthy, K.; Pentapati, K.C.; Prakash, H. Prevalence, Risk Factors, Treatment and Outcome of Multidrug Resistance Candida Auris Infections in Coronavirus Disease (COVID-19) Patients: A Systematic Review. Mycoses 2022, 65, 613–624. [Google Scholar] [CrossRef] [PubMed]
- Villanueva-Lozano, H.; Treviño-Rangel, R.d.J.; González, G.M.; Ramírez-Elizondo, M.T.; Lara-Medrano, R.; Aleman-Bocanegra, M.C.; Guajardo-Lara, C.E.; Gaona-Chávez, N.; Castilleja-Leal, F.; Torre-Amione, G.; et al. Outbreak of Candida Auris Infection in a COVID-19 Hospital in Mexico. Clin. Microbiol. Infect. 2021, 27, 813–816. [Google Scholar] [CrossRef] [PubMed]
- Corzo-Leon, D.E.; Alvarado-Matute, T.; Colombo, A.L.; Cornejo-Juarez, P.; Cortes, J.; Echevarria, J.I.; Guzman-Blanco, M.; Macias, A.E.; Nucci, M.; Ostrosky-Zeichner, L.; et al. Surveillance of Candida Spp Bloodstream Infections: Epidemiological Trends and Risk Factors of Death in Two Mexican Tertiary Care Hospitals. PLoS ONE 2014, 9, 1–6. [Google Scholar] [CrossRef]
- Horn, D.L.; Neofytos, D.; Anaissie, E.J.; Fishman, J.A.; Steinbach, W.J.; Olyaei, A.J.; Marr, K.A.; Pfaller, M.A.; Chang, C.H.; Webster, K.M. Epidemiology and Outcomes of Candidemia in 2019 Patients: Data from the Prospective Antifungal Therapy Alliance Registry. Clin. Infect. Dis. 2009, 48, 1695–1703. [Google Scholar] [CrossRef] [PubMed]
- Kutlu, M.; Sayın-Kutlu, S.; Alp-Çavuş, S.; Öztürk, Ş.B.; Taşbakan, M.; Özhak, B.; Kaya, O.; Kutsoylu, O.E.; Şenol-Akar, Ş.; Turhan, Ö.; et al. Mortality-Associated Factors of Candidemia: A Multi-Center Prospective Cohort in Turkey. Eur. J. Clin. Microbiol. Infect. Dis. 2022, 41, 597–607. [Google Scholar] [CrossRef]
- Corzo-Leon, D.E.; Peacock, M.; Rodriguez-Zulueta, P.; Salazar-Tamayo, G.J.; MacCallum, D.M. General Hospital Outbreak of Invasive Candidiasis Due to Azole-Resistant Candida Parapsilosis Associated with an Erg11 Y132F Mutation. Med. Mycol. 2021, 59, 664–671. [Google Scholar] [CrossRef]
- Routsi, C.; Meletiadis, J.; Charitidou, E.; Gkoufa, A.; Kokkoris, S.; Karageorgiou, S.; Giannopoulos, C.; Koulenti, D.; Andrikogiannopoulos, P.; Perivolioti, E.; et al. Epidemiology of Candidemia and Fluconazole Resistance in an ICU before and during the COVID-19 Pandemic Era. Antibiotics 2022, 11, 771. [Google Scholar] [CrossRef]
- Trevijano-Contador, N.; Torres-Cano, A.; Carballo-González, C.; Puig-Asensio, M.; Martín-Gómez, M.T.; Jiménez-Martínez, E.; Romero, D.; Nuvials, F.X.; Olmos-Arenas, R.; Moretó-Castellsagué, M.C.; et al. Global Emergence of Resistance to Fluconazole and Voriconazole in Candida Parapsilosis in Tertiary Hospitals in Spain During the COVID-19 Pandemic. Open Forum Infect. Dis. 2022, 9, ofac605. [Google Scholar] [CrossRef]
- Sacks, D.; Baxter, B.; Campbell, B.C.V.; Carpenter, J.S.; Cognard, C.; Dippel, D.; Eesa, M.; Fischer, U.; Hausegger, K.; Hirsch, J.A.; et al. Multisociety Consensus Quality Improvement Revised Consensus Statement for Endovascular Therapy of Acute Ischemic Stroke. Int. J. Stroke 2018, 13, 612–632. [Google Scholar] [CrossRef]
- Krishna, V.; Bansal, N.; Morjaria, J.; Kaul, S. COVID-19-Associated Pulmonary Mucormycosis. J. Fungi 2022, 8, 711. [Google Scholar] [CrossRef]
- Regalla, D.; VanNatta, M.; Alam, M.; Malek, A.E. COVID-19-Associated Cryptococcus Infection (CACI): A Review of Literature and Clinical Pearls. Infection 2022, 50, 1007–1012. [Google Scholar] [CrossRef] [PubMed]
- Kanamori, H.; Rutala, W.A.; Sickbert-Bennett, E.E.; Weber, D.J. Review of fungal outbreaks and infection prevention in healthcare settings during construction and renovation. Clin. Infect. Dis. 2015, 61, 433–444. [Google Scholar] [CrossRef] [PubMed]
- Hoenigl, M.; Seidel, D.; Sprute, R.; Cunha, C.; Oliverio, M.; Goldman, G.H.; Ibrahim, A.S.; Carvalho, A. COVID-19-Associated Fungal Infections. Nat. Microbiol. 2022, 7, 1127–1140. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | General n = 156 (%) | IFI n = 78 (%) | Controls n = 78 (%) | Bivariate p |
|---|---|---|---|---|
| Age, mean (SD) | 56.6 (14.1) | 56.5 (14.2) | 57.8 (14.1) | 0.9 |
| Male Sex | 112 (72) | 56 (72) | 56 (72) | 1.0 |
| Comorbidities | ||||
| Obesity | 81 (52) | 42 (54) | 39 (50) | 0.63 |
| Overweight | 56 (36) | 28 (36) | 28 (36) | 0.95 |
| Arterial hypertension | 53 (34) | 27 (35) | 26 (33) | 0.86 |
| Type 2 diabetes mellitus | 49 (32) | 23 (29.5) | 26 (38) | 0.56 |
| Immunosuppression | 7 (4.5) | 7 (9) | 0 | 0.01 |
| Pulmonary disease | 7 (4.5) | 5 (6) | 2 (2.5) | 0.44 |
| Smoking | 23 (15) | 13 (17) | 10 (13) | 0.49 |
| Charlson ≥ 4 | 22 (14) | 12 (15) | 10 (13) | 0.65 |
| Severity scores | ||||
| APACHE II Score ≥ 10 | 73 (47) | 38 (49) | 35 (45) | 0.63 |
| SOFA score > 2 | 126 (81) | 72 (92) | 54 (69) | <0.01 |
| Lymphopenia * | 107 (69) | 49 (63) | 58 (74) | 0.12 |
| SARS-CoV-2 PCR Ct < 24 | 52 (33) | 27 (35) | 25 (32) | 0.73 |
| COVID-19 treatment | ||||
| Tocilizumab | 10 (27) | 7 (37) | 3 (17) | 0.16 |
| Remdesivir | 4 (11) | 2 (10.5) | 2 (10.5) | 0.95 |
| Empiric antibiotic | 99 (63.5) | 72 (92) | 27 (35) | <0.01 |
| Dexamethasone | 103 (66) | 47 (60) | 56 (72) | 0.12 |
| Hospital stay, mdn (IQR) | 26 (17–41.5) | 34.5 (23–51) | 21 (12–29) | <0.01 |
| ICU stay, mdn (IQR) | 18 (11–28) | 22 (16–41) | 13 (7–24) | <0.01 |
| IMV duration, mdn (IQR) | 15.5 (9.5–25.5) | 20 (14–31) | 11 (7–22) | <0.01 |
| Prolonged IMV (>21 days) | 56 (36) | 35 (45) | 21 (27) | 0.02 |
| Prone position | 115 (74) | 61 (78) | 54 (69) | 0.20 |
| Vasopressors | 124 (79.5) | 70 (90) | 54 (69) | 0.002 |
| Hemodialysis | 12 (8) | 9 (11.5) | 3 (4) | 0.07 |
| Myocardial injury | 24 (15) | 17 (22) | 7 (9) | 0.03 |
| Pulmonary Venous thrombosis | 21 (13.5) | 12 (15) | 9 (11.5) | 0.48 |
| Bacterial co-infection $ | 92 (59) | 49 (63) | 43 (55) | 0.33 |
| VAP | 77 (87.5) | 38 (84) | 39 (91) | 0.37 |
| In-hospital mortality | 72 (46) | 38 (49) | 34 (44) | 0.52 |
| Variables | Multivariate Analysis |
|---|---|
| SOFA score > 2 | aOR 5.1, 95% CI 1.5–16.8, p = 0.007 |
| Empiric antibiotic | aOR 30, 95% CI 10.2–87.6, p = <0.01 |
| Prolonged IVM | aOR 2.3, 95% 0.9–6.2, p = 0.09 |
| Dexamethasone | aOR 0.81, 95% CI 0.31–2.1, p = 0.68 |
| Lymphopenia | aOR 0.56, 95% CI 0.20–1.5, p = 0.27 |
| Characteristics | All CAPA Cases n = 47 (%) | Probable CAPA n = 15 (%) | Possible CAPA n = 32 (%) | p Bivariate |
|---|---|---|---|---|
| Male sex | 34 (72) | 14 (93) | 20 (62.5) | 0.02 |
| Age, mean (SD) | 57.3 (14.3) | 53.3 (15.9) | 59.2 (13.4) | 0.18 |
| Obesity | 23 (49) | 6 (40) | 17 (53) | 0.40 |
| Immunosuppression | 6 (13) | 3 (20) | 3 (9) | 0.30 |
| Severity scores | ||||
| APACHE II Score ≥ 10 | 23 (49) | 3 (20) | 20 (62.5) | 0.007 |
| SOFA score > 2 | 45 (96) | 15 (100) | 30 (94) | 0.32 |
| Lymphopenia | 31 (66) | 8 (53) | 23 (72) | 0.21 |
| Empiric antibiotic previous ICU | 42 (89) | 14 (83) | 28 (87.5) | 0.54 |
| Dexamethasone | 30 (64) | 10 (67) | 20 (62.5) | 0.78 |
| CAPA diagnosis | ||||
| Persistent Fever | 14 (30) | 7 (47) | 7 (22) | 0.08 |
| Recurrent Fever | 32 (68) | 9 (60) | 23 (72) | 0.41 |
| Worsening ventilatory parameters | 36 (77) | 12 (80) | 24 (75) | 0.70 |
| Chest CT for diagnosis | 31 (66) | 11 (73) | 20 (62.5) | 0.46 |
| Antifungal treatment | 40 (85) | 15 (100) | 25 (78) | 0.05 |
| Death | 27 (57.5) | 7 (47) | 20 (62.5) | 0.30 |
| Characteristic/Patient | CAM Patient 1 | CAM Patient 2 | CAM Patient 3 | CACr Patient 1 | CACr Patient 2 | CACr Patient 3 |
|---|---|---|---|---|---|---|
| Sex | Male | Male | Male | Male | Male | Male |
| Age | 62 | 68 | 51 | 51 | 86 | 70 |
| Comorbidity | Obesity | Talcum pulmonary silicosis | Uncontrolled Diabetes | Uncontrolled Diabetes | Health previously | Health previously |
| Risk Factor | None | Lymphopenia | Lymphopenia | Lymphopenia | None | None |
| Dexamethasone for COVID-19 | Yes | Yes | Yes | Yes | Yes | Yes |
| Site of infection | Pulmonary/ Sinusitis | Pulmonary | Pulmonary/ Sinusitis | Pulmonary/ meningeal | Pulmonary | Pulmonary/ Pleural |
| Clinic | Fever, anosmia, dysgeusia, cyanosis without dyspnea | Dry cough, sore throat, fever, dyspnea | Cephalea, dry cough, arthralgia, myalgia, dyspnea | Fever (38.5 °C), dry cough, dyspnea | Dyspnea, backache, cephalea | General discomfort, diarrhea, dyspnea |
| CT finding | Thorax: progression of pneumonia, crazy paving, consolidation Paranasal: Pansinusitis | Thorax: progression of pneumonia, micronodular Paranasal: none | Thorax: progression of pneumonia, ground glass opacities, consolidation CT paranasal: Pansinusitis | Thorax: progression of pneumonia, ground glass opacities Brain MRI: bilateral frontotemporal pachymeningitis | Thorax: progression of pneumonia, ground glass opacities, and apical nodule | Thorax: pulmonary embolism, ground glass opacities, subpleural cyst, pneumatocele, hydro-pneumothorax |
| Mycologic | Rhizopus spp. in TA | Rhizopus oryzae in TA | Lichteimia corymbifera TA | Cryptococcus neoformans in TA Negative antigen LF in CSF | Cryptococcus neoformans in TA | Cryptococcus neoformans in pleural effusion |
| Treatment | Posaconazole | Isavuconazole | Isavuconazole | Amphotericin B + Fluconazole | Non-treatment (post-mortem diagnosis) | Fluconazole |
| Outcome | Dead | Alive | Dead | Alive | Dead | Dead |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Roman-Montes, C.M.; Bojorges-Aguilar, S.; Corral-Herrera, E.A.; Rangel-Cordero, A.; Díaz-Lomelí, P.; Cervantes-Sanchez, A.; Martinez-Guerra, B.A.; Rajme-López, S.; Tamez-Torres, K.M.; Martínez-Gamboa, R.A.; et al. Fungal Infections in the ICU during the COVID-19 Pandemic in Mexico. J. Fungi 2023, 9, 583. https://doi.org/10.3390/jof9050583
Roman-Montes CM, Bojorges-Aguilar S, Corral-Herrera EA, Rangel-Cordero A, Díaz-Lomelí P, Cervantes-Sanchez A, Martinez-Guerra BA, Rajme-López S, Tamez-Torres KM, Martínez-Gamboa RA, et al. Fungal Infections in the ICU during the COVID-19 Pandemic in Mexico. Journal of Fungi. 2023; 9(5):583. https://doi.org/10.3390/jof9050583
Chicago/Turabian StyleRoman-Montes, Carla M., Saul Bojorges-Aguilar, Ever Arturo Corral-Herrera, Andrea Rangel-Cordero, Paulette Díaz-Lomelí, Axel Cervantes-Sanchez, Bernardo A. Martinez-Guerra, Sandra Rajme-López, Karla María Tamez-Torres, Rosa Areli Martínez-Gamboa, and et al. 2023. "Fungal Infections in the ICU during the COVID-19 Pandemic in Mexico" Journal of Fungi 9, no. 5: 583. https://doi.org/10.3390/jof9050583







