Abstract
Bone and cartilage tissue play multiple roles in the organism, including kinematic support, protection of organs, and hematopoiesis. Bone and, above all, cartilaginous tissues present an inherently limited capacity for self-regeneration. The increasing prevalence of disorders affecting these crucial tissues, such as bone fractures, bone metastases, osteoporosis, or osteoarthritis, underscores the urgent imperative to investigate therapeutic strategies capable of effectively addressing the challenges associated with their degeneration and damage. In this context, the emerging field of tissue engineering and regenerative medicine (TERM) has made important contributions through the development of advanced hydrogels. These crosslinked three-dimensional networks can retain substantial amounts of water, thus mimicking the natural extracellular matrix (ECM). Hydrogels exhibit exceptional biocompatibility, customizable mechanical properties, and the ability to encapsulate bioactive molecules and cells. In addition, they can be meticulously tailored to the specific needs of each patient, providing a promising alternative to conventional surgical procedures and reducing the risk of subsequent adverse reactions. However, some issues need to be addressed, such as lack of mechanical strength, inconsistent properties, and low-cell viability. This review describes the structure and regeneration of bone and cartilage tissue. Then, we present an overview of hydrogels, including their classification, synthesis, and biomedical applications. Following this, we review the most relevant and recent advanced hydrogels in TERM for bone and cartilage tissue regeneration.
1. Introduction
The skeleton is one of the largest organs in the human body, and it performs pivotal functions such as providing structural support for the body′s shape and facilitating movement. It also plays a crucial role in protecting vital organs and actively contributes to the overall homeostasis of the entire body by storing calcium and phosphate and harboring the bone marrow [1,2]. Articular cartilage represents a specialized type of connective tissue found in diarthrodial joints covering the surface of bones to allow almost frictionless joint movement and support load transfer, all while protecting the subchondral bone [3]. Bone and cartilage diseases, including bone fractures, tumors, osteoporosis, or osteoarthritis, significantly burden global healthcare systems and the quality of life for affected individuals. These conditions often lead to chronic pain, functional impairment, and reduced mobility, affecting millions of people worldwide [4,5,6]. There are instances in fracture healing where the process of bone regeneration faces challenges, particularly when fractures are too extensive to undergo natural regeneration. For example, up to 13% of tibia fractures are linked to delayed union or, in severe cases, fracture nonunion [7,8]. The conventional approach for treating patients whose bone treatments have been lengthy or unsuccessful is to use bone grafting, which ranks second among the most transplanted tissues in the United States, either as an allograft or an autograft [9]. However, there are issues with bone grafting. A more sustainable, less invasive, long-term healing strategy is consequently required to help treat fractures that have been damaged, and bone graft substitutes are being developed [10]. The following main approaches to bone restoration have been established, depending on the severity of the trauma: synthetic substitutes alone; scaffolds combined with active molecules; nanomedicine; cell-based combination products with different cells from various sources; biomimetic fibrous and nonfibrous substitutes; magnetic field and nano-scaffolds with stem cells; bioactive porous polymer/inorganic composite; and biomaterial-based 3D cell-printing substitutes [11,12,13,14,15,16,17]. The election of the different techniques is based on the healing potential and particular requirements of each case.
Langer and Vacanti defined tissue engineering in the early 1990s as “an interdisciplinary field which applies the principles of engineering and life sciences toward the development of biological substitutes that restore, maintain, or improve tissue function” [18]. In recent decades, there have been remarkable advances in the field of tissue engineering and regenerative medicine (TERM), with particular attention to the development of biomaterials-based strategies to facilitate tissue repair and regeneration [19,20]. Among these biomaterials, hydrogels have emerged as versatile and promising candidates for the promotion of the natural healing processes of bone and cartilage [21,22]. Their unique properties, including high water content, adjustable mechanical properties, and the ability to load bioactive molecules and cells, make hydrogels uniquely suited for TERM applications [23]. Hydrogel-based methods offer less invasive alternatives to conventional surgical techniques, reducing patient discomfort, shortening recovery times, and reducing complications associated with invasive procedures. In addition, these methods can be precisely tailored to the specific needs of each patient [24]. This personalized approach to regenerative therapies has the potential to deliver superior results while minimizing the likelihood of adverse reactions [25,26].
The main objectives of our article are to provide a comprehensive and current overview of advances in advanced hydrogels for bone and cartilage tissue regeneration. The review focuses especially on the recent advances in advanced hydrogels for bone and cartilage regeneration and the novelties of patient-specific treatments. This work arises from the need to address the increasingly prevalent disorders affecting bone and cartilage tissues and aims to bring together the specific contributions of advanced hydrogels in this context, thus contributing to the evolving field of TERM, moving toward personalized medicine. We collect the main knowledge on bone and cartilage structure and regeneration. Below, we present the state of the art of advanced hydrogels in TERM and explore their use in bone and cartilage tissue engineering. Through this review, we aim to illuminate the potentially transformative impact of hydrogel-based therapies in addressing unmet clinical demands associated with bone- and cartilage-related disorders.
2. Bone Biology
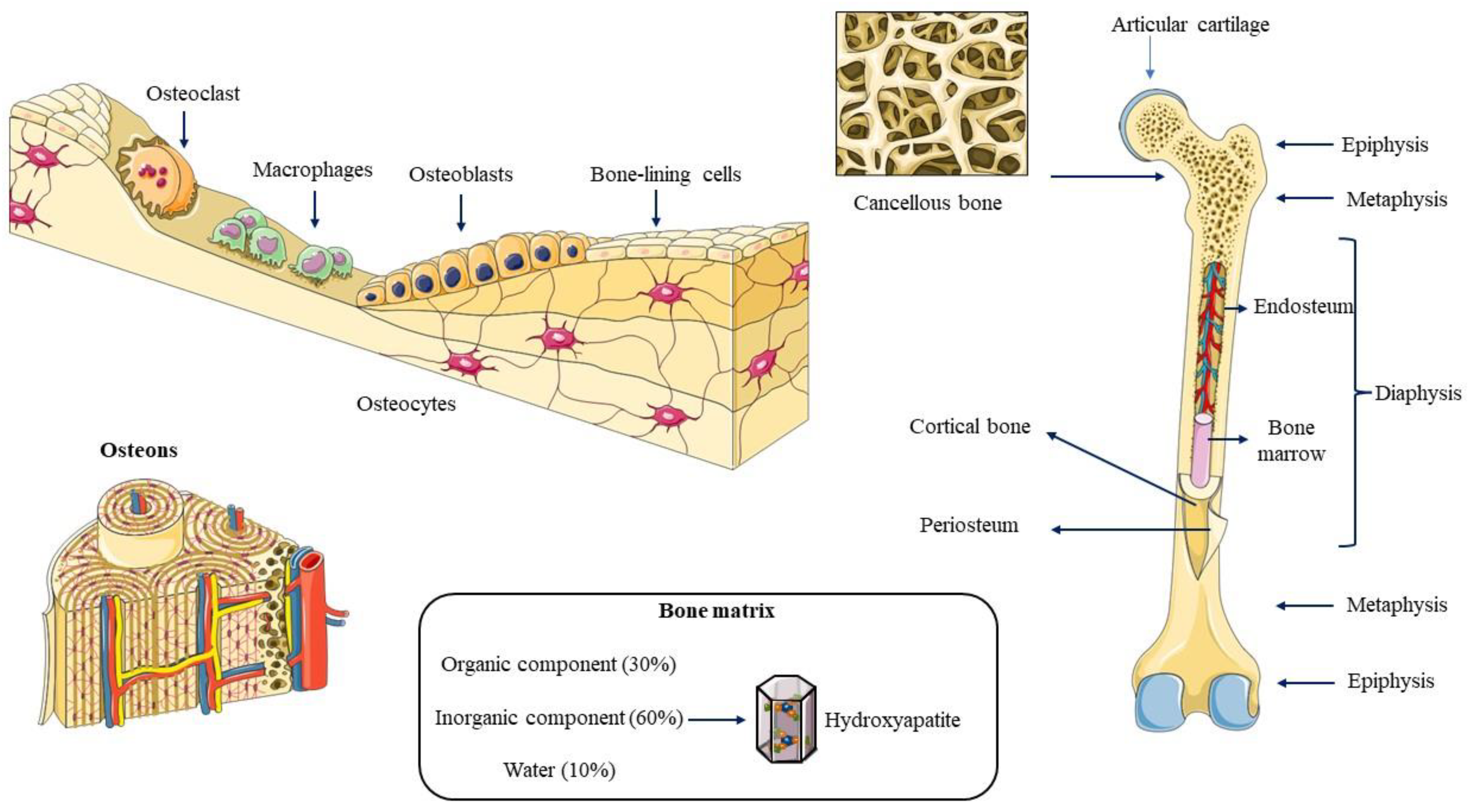
Bone is a robust, multifunctional structure that plays a pivotal role in protecting vital organs, providing crucial kinematic support, regulating hematopoiesis, and preserving mineral balance. This dynamic tissue continuously remodels to maintain bone strength, mass, and the necessary calcium and phosphate mineral homeostasis, and importantly, it is the final step of bone regeneration [27]. It is formed by cells and a mineralized extracellular matrix (ECM) (Figure 1). Bone consists of five major cellular components: osteoprogenitor cells, osteoblasts, osteocytes, osteoclasts, and bone lining cells [2]. Osteoprogenitor cells, derived from mesenchymal stem cells (MSCs), are predominantly located in the bone marrow. These cells can differentiate into osteoblasts and maintain their osteoprogenitor potential in the adult bone system, making them crucial to the repair process [28,29]. Osteoblasts are recognized for their role in the formation of new bone via the secretion of the ECM [30,31]. Osteocytes are the most prevalent cells and are found in lacunae that are enclosed by a mineralized matrix, previously secreted as an osteoblast [32,33]. The osteoclasts are phagocytic multinucleated cells that have undergone terminal differentiation and are derived from the fusion of mononuclear cells of the hematopoietic stem cell (HSC) lineage under the effect of cytokines, such as receptor activator of nuclear factor κΒ ligand (RANKL) and macrophage colony-stimulating factor (M-CSF) [34,35,36]. Finally, the bone lining cells are quiescent flat-shaped osteoblasts that protect the surfaces of bones where neither bone growth nor bone resorption takes place [37].
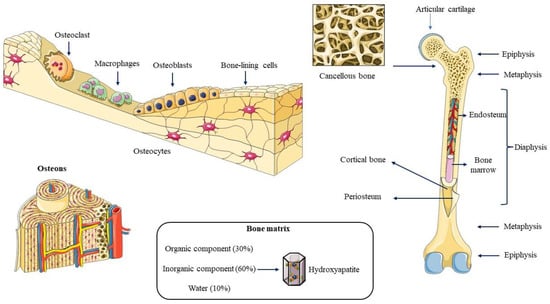
Figure 1.
Bone anatomy and histology. A typical large bone exhibits a distinct structural organization, comprising epiphyses at the extremities housing bone marrow and cancellous bone, a central diaphysis characterized by a robust cortical bone layer, and the transitional metaphysis region. The bone tissue comprises various cell types alongside a mineralized extracellular matrix. The organic component, constituting approximately 30% of bone composition, primarily consists of collagen type I. In contrast, the inorganic component, representing around 60% of the bone’s composition, mainly comprises hydroxyapatite crystals.
The bone matrix is composed of organic compounds (30%), inorganic compounds (60%), and water (10%). The former is mainly composed of collagen type I (90%), and to a lesser extent collagen type V, and more than 30 proteins classified into four groups: proteoglycans, multiadhesive glycoproteins (osteonectin and podoplanin/E11), vitamin K-dependent proteins (osteocalcin and protein S) and growth factors (GFs), and cytokines (CKs) (IGF, TNFα, TGF-β, PDGF, BMP, IL-1, and IL-6) [38,39]. Hydroxyapatite (HA) crystals [Ca10(PO4)6(OH)2] are inorganic compounds, and their deposition is responsible for the mineralization of the bone matrix [40,41]. Research on the roles of bone matrix is essential for the development of hydrogel-based strategies for regenerative medicine.
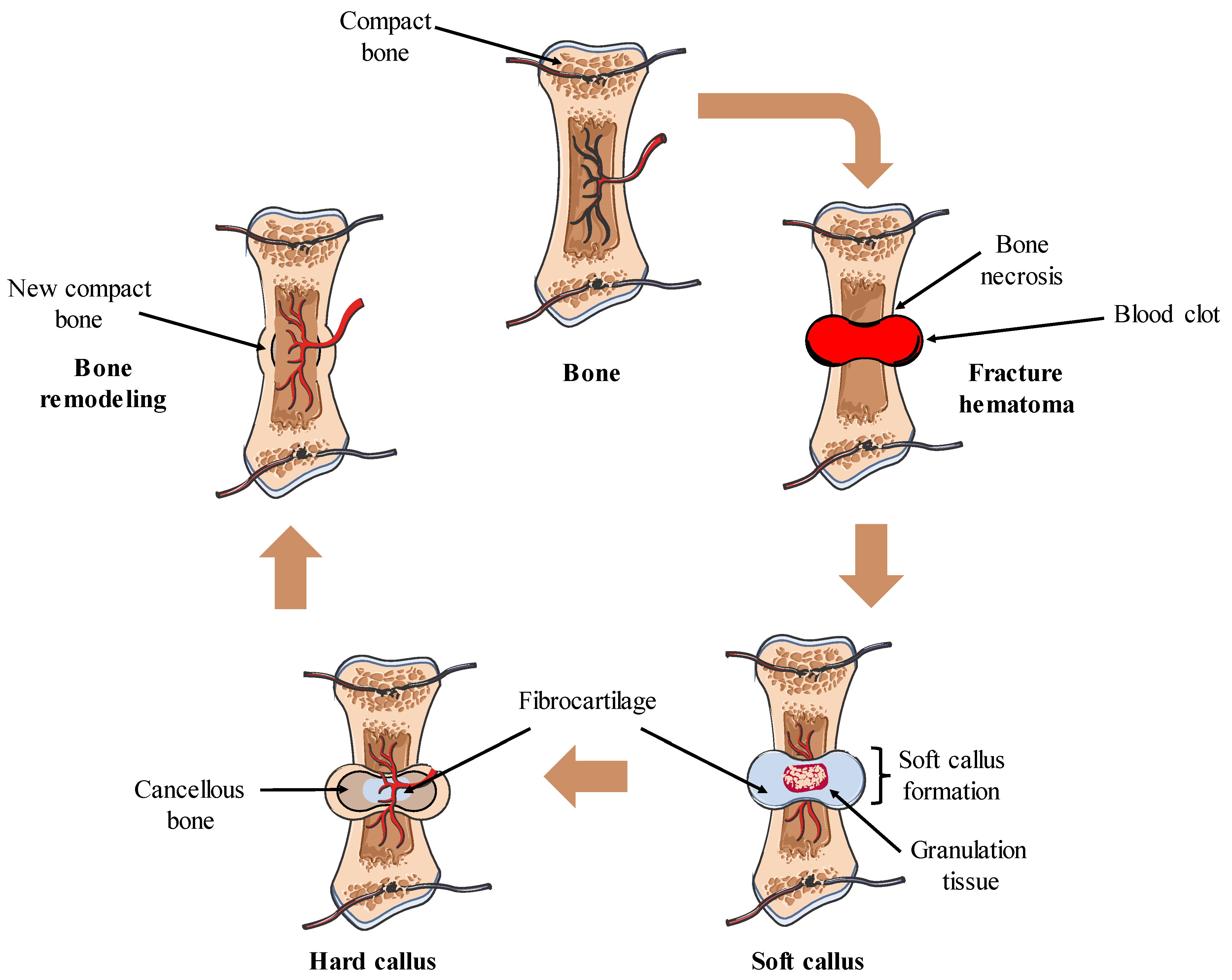
Bone regeneration is composed of a well-orchestrated sequence of biological events of bone induction and conduction that involve a variety of types of cells and intracellular and extracellular molecular-signaling pathways [42]. Contrary to other tissues, the majority of skeletal injuries, such as fractures, heal without the development of scar tissue. Instead, bone regenerates, with many of its pre-existing qualities restored, and finally becomes identical to the nearby uninjured bone [43,44]. The process of bone regeneration encompasses three sequential steps: the acute inflammatory response, bone repair, and remodeling (described in Figure 2) [45,46,47,48,49]. Surgical and non-surgical procedures play a crucial role in facilitating and expediting the bone-repair process by immobilizing the bones and bridging the gap between the two fractured ends [50,51]. With a greater understanding of bone biology at the molecular level, numerous new treatment approaches have been developed, and it is projected that there will be many more (or advancements to existing ones) in the years to come.
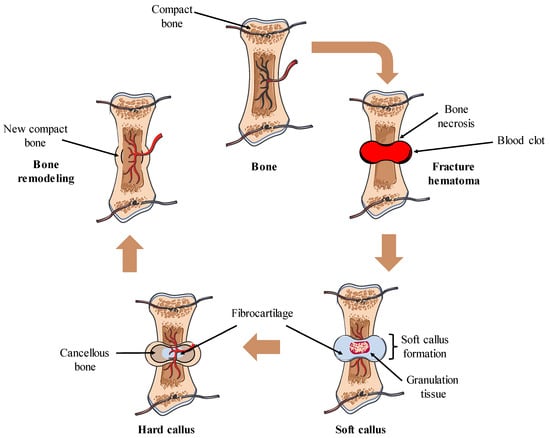
Figure 2.
Bone healing process. The bone healing process comprises different phases. It begins with the formation of a hematoma and coagulation at the fracture site, followed by the recruitment of neutrophils and macrophages, together with the proliferation of fibroblasts and endothelial cells, leading to the formation of granulation tissue. Subsequently, a soft callus, characterized by a fibrocartilaginous matrix, connects the fractured bone ends. Osteoprogenitor cells of the periosteum differentiate into osteoblasts, initiating the formation of new bone around the soft callus. As fibrocartilage calcification occurs, new bone is deposited, culminating in the formation of a hard callus. Finally, bone remodeling occurs, restoring normal bone structure.
3. Cartilage Biology
Cartilage is an avascular, aneural, a-lymphatic connective tissue that is also present in the growth plates of children and adolescents. Humans have three different forms of cartilage: hyaline, fibrous, and elastic [52]. The chondrocytes, which produce and secrete the main elements of the extracellular matrix (EMC), are present in low density in all three types. The cartilage ECM has a special family of proteoglycans interwoven within a highly hydrated collagen fibrillar network to carry out the biomechanical responsibilities of giving structural support and resistance to deformation [53]. This matrix is produced and assembled by chondrocytes with the help of a large number of other non-collagenous proteins, proteoglycans, and glycoproteins. Each of the three forms of cartilage has varied abundance, distribution, and types of collagen and proteoglycans, which results in variations in appearance and biomechanical capabilities. The most prevalent type of cartilage in the human body is hyaline cartilage, which has a glassy appearance. It is located in the growth plates, ribs, nose, trachea, bronchi, and articulating surfaces of bones in synovial joints [54]. Articular cartilage is very similar to hyaline cartilage, except for the absence of perichondrium. It contains cartilage-specific collagen molecules that are crosslinked together in a copolymeric network, as well as proteoglycans and multiadhesive glycoproteins [55]. The limited regenerative capacity is due to the stability of cartilage-specific collagen molecules and the low activity of metalloproteinases.
Cartilage damage should ideally recover without leaving a scar. The smooth surface of the joint would be hampered by scar tissues inside the joint, and they would also have bad mechanical qualities [56]. Catabolic and anabolic damage responses in cartilage can be distinguished. The synthesis of agreement can degrade enzyme disintegrant and metalloproteinase with thrombospondin motifs 5 (ADAMTS-5), and the collagen matrix metalloproteinase 13 (MMP-13), which exclusively destroys type II collagen, is the catabolic activity that is most relevant to cartilage [57]. In reaction to injury, ADAMTS-5 is released quickly, but MMP-13 expression has a delayed response [58]. Instead, the anabolic activity involves the induction of chondroprotective genes like the transforming growth factor beta (TFG-β) family member activin A, hyaluronan-binding anti-inflammatory molecule, and tumor necrosis factor-inducible gene 6 protein (TSG-6). Uncertain factors may have contributed to the failure of cartilage regrowth [59,60]. Additional hints have been offered from the study of cartilage engineering: for instance, it is uncommon to see neocartilage integrating laterally with neighboring cartilage.
4. Hydrogels: Concept, Synthesis, and Biomedical Applications
Hydrogels are three-dimensional (3D) networks that are created by crosslinked polymers and can swell in aqueous solutions. These hydrogels possess unique properties such as biocompatibility, low toxicity, wide availability, viscoelasticity, and biodegradability, making them suitable for numerous biomedical applications [61,62,63,64]. These include TERM (reviewed in this paper), wound dressing, contact lenses, 3D cell cultures, drug delivery, antimicrobial resistance treatment, and biosensing.
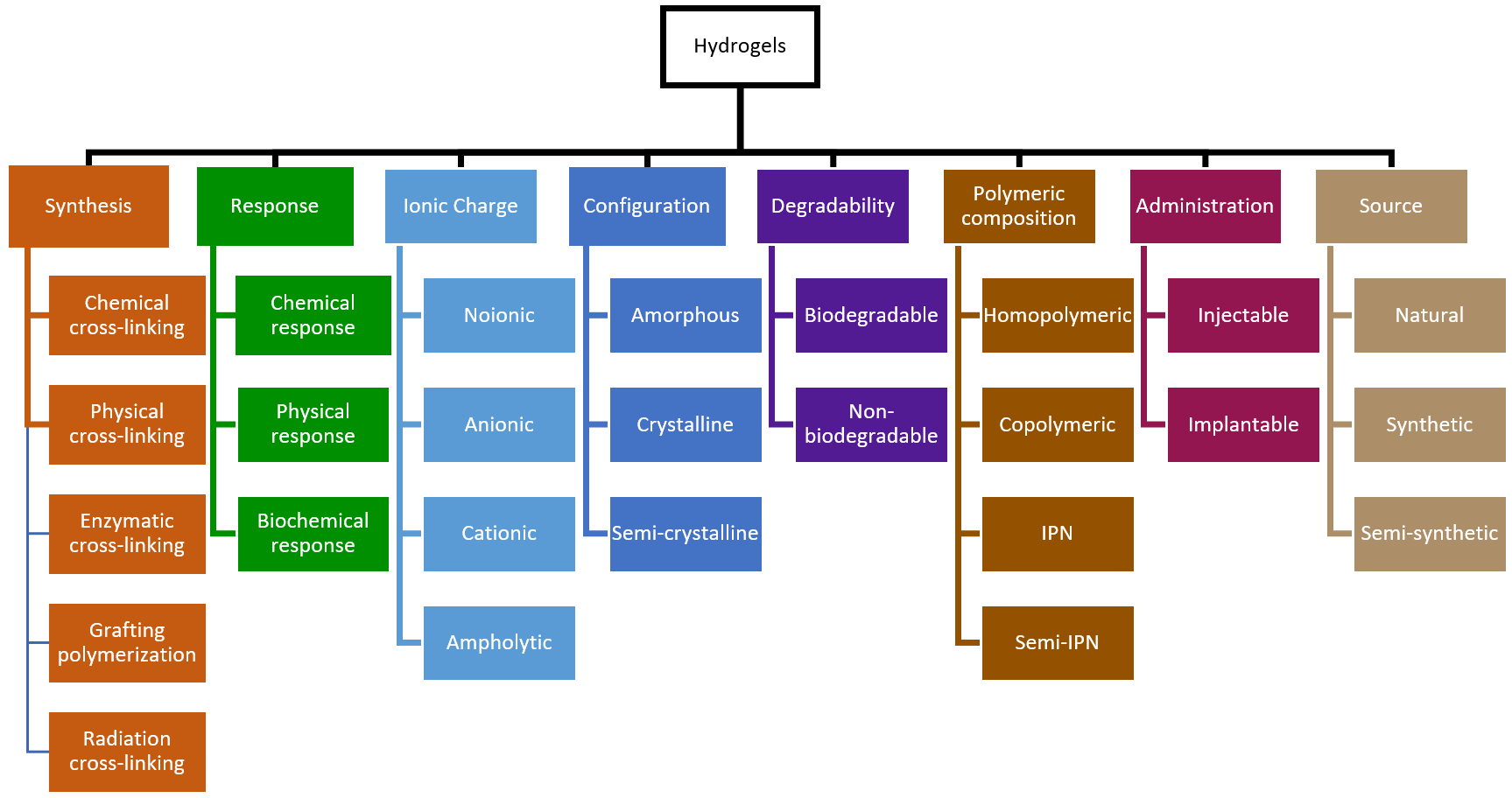
Hydrogels can be classified according to different criteria (Figure 3), such as their source/composition, crosslinking, ionic charge, configuration, preparation, degradability, administration, and sensitivity to external stimuli [65]. Their diverse composition comprises natural polymers, synthetic polymers, or hybrid combinations of both. Natural polymers, from various biological origins, offer remarkable advantages, such as excellent biocompatibility, biodegradability, and non-toxicity [66,67,68]. Examples of natural polymers are chitosan, hyaluronic acid (HA), gelatin, alginate, and cellulose. In contrast, synthetic hydrogels contain synthetic polymers, making them ideal for tailoring and optimizing mechanical properties [69,70]. Some synthetic examples are polycaprolactone, poly (vinylpyrrolidone) (PVP), poly (lactic acid) (PLA), poly (ethylene glycol) (PEG), and poly (vinyl alcohol) (PVA).
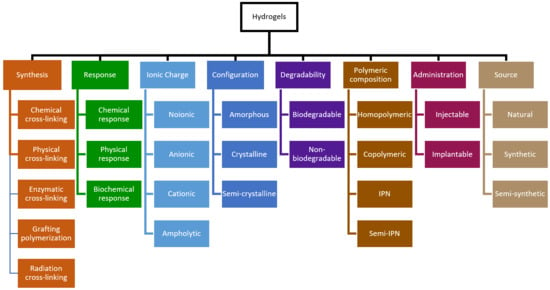
Figure 3.
Classification of hydrogels according to different criteria.
Hydrogels are prepared through different procedures—chemical crosslinking, physical crosslinking, enzymatic crosslinking, grafting polymerization, and radiation crosslinking—which facilitate a broad spectrum of applications and fine-tuning of their characteristics to align with specific therapeutic and biomedical requirements [62,71,72]. Chemical crosslinking involves the establishment of covalent bonds that ensure long-term stability and durability [73,74]. For this purpose, crosslinking agents or the grafting of monomers onto the polymer backbone are used, and various chemical reactions can be employed, such as Schiff base reactions, photoelectric crosslinking, and crosslinking by chemical reactions of complementary groups [75,76,77]. In contrast, physical crosslinking relies on reversible interactions that provide flexibility and responsiveness to external stimuli [78]. These interactions include hydrogen bonding, the formation of amphiphilic grafting, crystallization, ionic interactions, maturation (heat-induced aggregation), and hydrophobic interactions, all of which contribute to the remarkable adaptability and multifunctionality of hydrogels in the biomedical field. These types of hydrogels are known for their ease of synthesis and lack of a crosslinking agent, which may have an impact on the reliability of loaded materials because of their toxicity [79,80]. Stress or changes in the physical environment can disrupt these interactions, allowing the hydrogel to revert to its polymer chains. Enzymatic crosslinking is a method in which an enzyme, such as tyrosinase, lysyl oxidase, or peroxidase, catalyzes the crosslinking within polymer chains [81,82,83]. They create in situ hydrogels characterized by exceptional biocompatibility. Grafting consists of the covalent attachment of a monomer to a polymeric host molecule or the polymerization of a monomer into a prefabricated polymeric skeleton [84,85,86,87]. This can be achieved using chemical or radiation-based methods, leading to the formation of functional hydrogels with specific properties. Radiation crosslinking uses sources such as electron beams, gamma radiation, or X-rays to generate free radicals in the polymer, resulting in crosslinking [88,89]. This method is preferred because of its ability to modify biopolymers without the need for chemical additives while ensuring biocompatibility and cost-effectiveness [90,91,92].
Hydrogels can also be classified into four main categories based on their polymeric composition: homopolymers, copolymers, interpenetrating polymer networks (IPNs), and semi-IPNs [62]. Homopolymer hydrogels are formed from a single monomer species, while copolymer hydrogels are derived from two or more monomer species and can be arranged as block, alternating, or random configurations along the chain of the polymer network [93,94]. Both present the same type of polymer. In contrast, semi-IPN hydrogels involve a polymeric network embedded within linear polymeric chains without crosslinking agents, whereas IPN hydrogels result from multiple polymeric networks crosslinked together using a crosslinking agent [95,96,97]. Semi-IPN and IPN hydrogels exhibit superior mechanical strength and swelling properties compared to homopolymeric and copolymeric hydrogels [98].
5. Hydrogels for TERM of Bone and Cartilage
Tissue engineering and regenerative medicine (TERM) is an emerging field that aims to achieve complete restoration of damaged tissues or organs. On the one hand, tissue engineering integrates the interplay of cells, scaffolds, and bioactive molecules to fabricate functional tissues. On the other hand, regenerative medicine encompasses a broader spectrum by synergizing tissue engineering with complementary strategies, such as cell therapy, gene therapy, and immunomodulation, all working in concert to promote tissue and organ regeneration [99]. In recent years, there have been significant advances in TERM, especially in the field of bone and articular cartilage regeneration [100,101].
In the field of TERM, hydrogels present ideal properties that make them suitable for bone regeneration and cartilage repair. Their ability to retain and release these therapeutic agents in a controlled manner facilitates tissue regeneration processes [102]. Moreover, the hydrophilic groups that retain water and the chemical crosslinker can also interact with the cells and molecules of the damaged tissue [103]. In addition, hydrogels offer the advantage of being customizable, allowing their physical and mechanical properties to be adjusted to those of the target tissue [102]. This fine tuning enhances their versatility and applicability in the field of tissue engineering and regenerative medicine (TERM). For example, hydrogels can be carefully designed to reproduce the characteristic stiffness and elasticity of specific tissues, facilitating seamless integration and optimal functionality in regenerative applications. In the following sections, we will provide an overview of some of the most prominent hydrogels used in TERM for bone and cartilage applications.
Hydrogels have diverse applications in the TERM of bone and cartilage defects. They play a crucial role in fracture healing by releasing bioactive molecules to accelerate the bone healing process and as bone graft substitutes that fill bone defects, eliminating the need for traditional bone grafting procedures [104,105,106,107]. Hydrogels act as supporting scaffolds, encapsulating cells, and growth factors to facilitate the formation of new bone tissue. In the treatment of osteoporosis, hydrogels are used to release drugs in a sustained manner and increase bone density [108,109,110,111,112]. In addition, they serve as lubricants in joints, offering relief to patients with joint diseases such as osteoarthritis [113,114,115,116,117]. In minimally invasive surgeries, injectable hydrogels conform to the irregular shapes of defects, providing structural support for bone and cartilage problems [118,119]. Finally, hydrogels are useful for local drug delivery, as they precisely target foci of bone infection with antibiotics, silver nanoparticles, or bacteriophages [120,121,122,123]. This variety of applications underscores the versatility and importance of hydrogels in meeting diverse clinical needs related to bone and cartilage regeneration.
In the context of the TERM of bone and cartilage, physically crosslinked hydrogels are formed through reversible non-covalent interactions, offering high biocompatibility and suitability for applications requiring temporary support, flexibility, and rapid degradation [124,125]. Chemically crosslinked hydrogels, on the other hand, are created by covalent bonds, providing permanent and robust networks with increased mechanical strength. They are suitable for load-bearing applications due to their non-reversible nature and slower degradation rate, although concerns regarding residual chemicals must be taken into account [126,127]. The choice between these hydrogels in bone regeneration depends on specific clinical requirements, with physically crosslinked hydrogels being ideal for temporary and sensitive solutions and chemically crosslinked hydrogels being suitable for long-term stability and load-bearing applications [128].
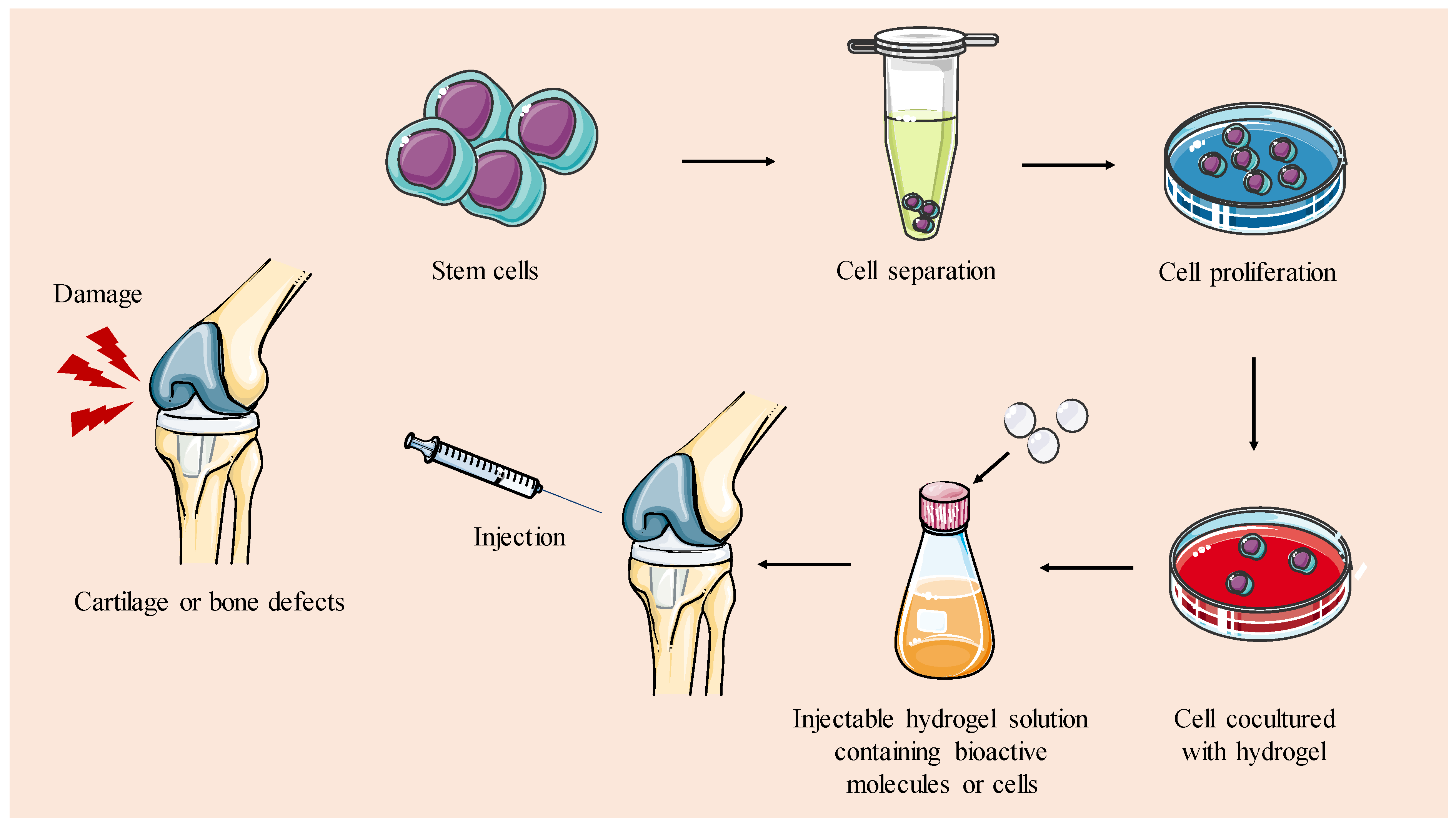
Injectable hydrogels are a type of biomaterial that can be administered in liquid or gel form and then solidify or gel in situ at the desired site in the body [118,119]. Injectable scaffolds can be molded to fit bone/cartilage defects of any shape, which makes them a versatile option for various defect types and sizes and the most widely investigated technology in the field [129]. Injectable scaffolds also have the advantage of adhering well to the surrounding tissue, which promotes tissue integration. In addition, they minimize the need for aggressive surgical interventions, making them a more comfortable option for the patient [130]. These hydrogels are easily handled and can be loaded with cells, creating an environment conducive to cell survival and growth. This cell support facilitates specific cellular responses and guides the formation of new tissue (Figure 4). Lastly, they are suitable for drug delivery, allowing controlled release of bioactive molecules to enhance the regenerative process [131].
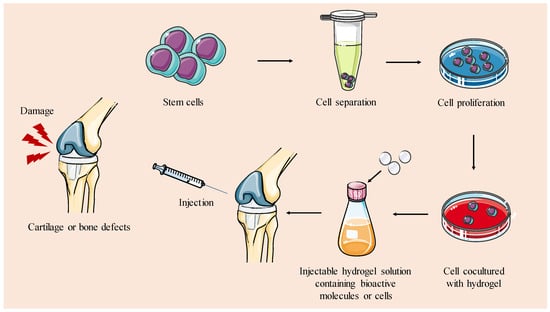
Figure 4.
Schematic representation of strategies for creating injectable hydrogels intended for TERM applications in cartilage and bone. Injectable hydrogels are designed to solidify in situ via chemical reactions or the induction of physical factors to repair bone or cartilage defects.
In the field of 3D bioprinting, bioinks based on naturally occurring hydrogels, such as (HA), gelatin, and fibrin, have demonstrated their ability to preserve crucial quality attributes of MSCs [132,133,134]. This preservation is attributed to the minimization of shear stress imparted by these bioinks, which not only provide structural support for cell proliferation but also facilitate osteogenic differentiation. Regarding cartilage tissue engineering, the main advantage of 3D bioprinting lies in its ability to hierarchically and spatially distribute 3D bioprinted cells, hydrogels, and active substances according to specific 3D requirements [135,136]. This approach generates an interconnected pore structure with substantial surface area, which facilitates cell adhesion, growth, intercellular communication, and gas and nutrient exchange [137]. These advantages represent a significant advance in promoting cartilage tissue regeneration compared to conventional solvent hydrogels. Bioinks are composed of conventional synthetic materials such as PVA, PAA, or nylon, charged with cells to construct allogeneic tissues and organs to avoid surgical invasive procedures, i.e., bone autografting [138]. Four-dimensional bioprinting goes beyond traditional three-dimensional bioprinting by incorporating the dimension of time as a critical factor in the printing process. In 4D bioprinting, hydrogels can respond to environmental stimuli, such as changes in temperature, pH, or the presence of specific molecules in a predetermined and programmable manner over time [139]. In the context of bone and cartilage TERM, shape memory implants adapt to evolving tissue needs, while stimuli-responsive scaffolds allow controlled cell differentiation through the release of growth factors [140]. These constructs mimic the behavior of natural tissue by altering its mechanical properties in response to mechanical loading. In addition, 4D-printed implants offer dynamic drug delivery to enhance regeneration and osteogenic maturation properties that promote osteoblast development [141]. Cartilage constructs adapt to changing joint conditions, promoting cartilage repair and joint function. Customized solutions can be achieved for each patient, ensuring that the regenerated tissue is precisely tailored to the anatomy and requirements of the patient.
5.1. Hydrogels in Bone Tissue Regeneration
In bone tissue engineering (BTE), hydrogels need specific fundamental attributes: tissue and cell compatibility, along with osteoinductive and osteoconductive properties. Osteoinduction denotes the ability to stimulate osteogenesis, while osteoconduction refers to the capacity to facilitate bone growth on a surface or scaffold [142]. These essential attributes collectively contribute to the efficacy of the hydrogel in promoting bone regeneration and healing. The composition of hydrogels in bone tissue engineering (BTE) involves a hydrogel-inspired scaffold designed to reproduce the mechanical properties of the extracellular matrix (ECM) and facilitate bone remodeling [143]. Within this scaffold, cells with osteogenic potential, including several varieties of stem cells, are included along with bioactive molecules, mainly growth factors, and cytokines, aimed at recruiting immune and osteoprogenitor cells to the injured site [106]. This multifaceted structure is intended to recreate an environment conducive to bone regeneration [144]. The various techniques used to prepare hydrogels give rise to a wide range of options in terms of their structure. In the context of bone regeneration, the most commonly used forms are microbeads, nanogels, and hydrogel fibers [106].
In the field of bone regeneration, there have been significant advances in hydrogel research in recent years, accompanied by the emergence of numerous innovative strategies. In particular, drug delivery systems, especially bioactive molecules, and cell-loaded hydrogels, have shown promising results. Moreover, advanced hydrogels show multifunctional properties that improve the outcomes of bone tissue regeneration. Examples of hydrogels employed in the TERM of bone tissue are reported in Table 1.
5.1.1. Bioactive Molecules-Loaded Hydrogels
Shekaran et al., designed a protease-degradable PEG synthetic hydrogel with a triple helical, α2β1 integrin-specific peptide (GFOGER) as a BMP-2 delivery vehicle [145]. This hydrogel showed susceptibility to matrix metalloproteinase (MMP) activity, resulting in a controlled and sustained release of BMP-2 at low doses in vivo. Consequently, it facilitated bone fracture regeneration by recruiting osteoprogenitor cells and bridging fracture sites in mice. Another example is SDF-1α/chitosan/carboxymeymethy-chitosan nanoparticles (NPs), which were prepared and added to thermosensitive chitosan/glycerol phosphate hydrogels [146]. These were injected into calvarial defects induced in rats. Bone regeneration was induced by the sustained release of SDF-1α in situ, which signals for the homing of host MSCs. Zhang et al., constructed an alginate hydrogel loaded with peptide nanofibers made of two ultrashort peptides for the self-assembly and the stimulation of the M2 phenotype [147]. Following this, the hydrogel was applied to treat bone defects in mice, and upon ultrasound stimulation, the nanofibers were released from the hydrogel. The M2 phenotype was induced in macrophages through the STAT6/PPAR-γ/SOCS3 signaling axis, leading to the inhibition of the production of reactive oxygen species (ROS) and secretion of BMP-2 and IGF-I that promote the osteogenic differentiation of bone marrow mesenchymal stem cells (BMSCs). Collectively, all this contributes to the bone regeneration of rats. Atsttrin is a derivative of progranulin, a secreted glycoprotein that binds to TNFα receptors and is involved in anti-inflammation, tissue repair, wound healing, and cartilage development [148]. Moradi et al., synthesized a chitosan/graphene oxide/hydroxyethyl cellulose/β-glycerol phosphate hydrogel loaded with Atsttrin [149]. Enhanced bone regeneration was observed using the injectable hydrogel, which facilitated the sustained release of Atsttrin, thereby promoting the establishment of a well-defined callus structure in a murine diabetic model. Wang and colleagues engineered a dynamic hydrogel mimicking the gel-like nature of a hematoma, crucially involved in the initial stages of bone repair, as we have reviewed above [150]. The gel was formulated by taking advantage of the reversible interaction between vancomycin and D-Ala-D-Ala dipeptide, effectively trapping and killing bacteria within the hematoma-like environment. In addition, the incorporation of an osteogenic peptide facilitated bone healing. This approach holds great promise for preventing infections in vulnerable bone fractures or cases of osteomyelitis. Lastly, hydrogels can also include plasmids. Cheng et al., loaded a glycol-based dendronized chitosan with G protein-coupled receptor kinase 2 interacting protein 1 (GIT1) plasmid [151]. MSCs were effectively transfected in vivo, which promotes bone repair and neovascularization around bone defects via the Notch signaling pathway. Calcium phosphate (CaP)-based products, including hydrogels, are very useful for bone tissue engineering [152,153]. Fatimi and colleagues developed an innovative cellulose-derived pH-sensitive hydrogel combined with biphasic calcium phosphate to create an injectable formulation aimed at enhancing bone regeneration. This injectable bone substitute exhibits osteoconductive characteristics and has demonstrated its ability to stimulate the formation of new bone tissue [154,155]. The addition of beta-tricalcium phosphate (β-TCP) particles in hydrogels significantly broadens the range of hydrogel stiffness and promotes osteogenic differentiation of human mesenchymal stem cells (hMSCs), with lower-stiffness composites showing the highest expression of alkaline phosphatase and gene markers associated with osteogenesis [156]. Svarca et al., added strontium ranelate and CaP nanoparticles to HA-based hydrogels for local osteoporosis treatment as a drug delivery system [157]. The incorporation of these components significantly affected hydrogel properties, such as swelling behavior, gel fraction, rheological properties, and microstructure, while strontium ranelate demonstrates a positive impact on cell viability, particularly within the concentration range of 0.05–0.2 μg/mL.
5.1.2. Cells-Loaded Hydrogels
Stem cells from different sources are the most employed cells in hydrogel therapies due to their potential for proliferation and differentiation to regenerate the tissues. The treatment of osteoporosis with BMSCs in preclinical studies is effective [158]. Furthermore, hydrogels loaded with BMSCs have been used extensively in animal models of osteoporosis, with favorable results. A hydrogel composed of poloxamer 407 and HA was fortified with MnO2 to protect administered BMSCs from reactive oxygen species (ROS) accumulation in osteoporosis, thus effectively promoting bone regeneration [159]. In particular, this hydrogel induced an M2 phenotype of macrophages while reducing the expression of proinflammatory cytokines and the secretion of osteogenic factors such as TGF-β and PDGF. Human tonsil-derived mesenchymal stem cells (TMSCs) loaded on gelatin-hydroxyphenyl propionic acid hydrogel were delivered subcutaneously to the dorsal of ovariectomized mice [160]. It demonstrated a recovery of the femoral heads and serum osteocalcin and alkaline phosphatase. Interestingly, the mice also showed a reduction in visceral fat.
Therefore, it can be deduced that in the development of hydrogels, attention must extend beyond just the degradation timeline. It is essential to take into account both the process of osteogenesis and osteodegradation and to carry out a thorough evaluation of constituents, their ratios, and fillers, which may prove invaluable in future research.

Table 1.
Recent research on advanced hydrogels incorporating bioactive molecules and cells for bone tissue regeneration: composition, preparation, and the process of application and evaluation.
Table 1.
Recent research on advanced hydrogels incorporating bioactive molecules and cells for bone tissue regeneration: composition, preparation, and the process of application and evaluation.
| Polymer | Biological Factor | Mechanism of Gelation | Application | Year | References |
|---|---|---|---|---|---|
| PEG | BMP-2 | Chemical crosslinking | Murine non-healing radial bone defect | 2014 | [145] |
| Chitosan/β-glycerol phosphate disodium salt | SDF-1α | Chemical crosslinking | Critical-sized calvarial defects in rats | 2017 | [146] |
| Calcium alginate | Ultrashort peptide nanofibers | Physical crosslinking | Rebuild osteogenic immune microenvironments | 2024 | [147] |
| Chitosan/graphene oxide/hydroxyethyl cellulose/β-glycerol phosphate | Atsttrin | Physical crosslinking | Bone regeneration in diabetic mice model | 2023 | [149] |
| Vancomycin/D-Ala-D-Ala/acrylamide | OGP | Physical crosslinking | Infected bone fracture | 2023 | [150] |
| Glycol-based dendronized chitosan | GIT1 plasmids | Physical crosslinking | Bone defects | 2023 | [151] |
| Hydroxypropylmethylcellulose | Biphasic calcium phosphate | Chemical crosslinking | New bone formation | 2009/12 | [154,155] |
| Agarose and agarose–collagen | β-TCP | Chemical crosslinking | Osteogenic differentiation of hMSCs | 2018 | [156] |
| HA | CaP NPs and strontium ranelate | Chemical crosslinking | Osteoporosis | 2022 | [157] |
| Poloxamer 407/HA | BMSCs | Chemical crosslinking | Osteoporosis | 2023 | [159] |
| Gelatin-hydroxyphenyl propionic acid | TMSCs | Chemical crosslinking | Postmenopausal osteoporosis | 2018 | [160] |
5.2. Hydrogels in Cartilage Regeneration
TERM also takes advantage of the advantageous properties of hydrogels for articular cartilage regeneration, mainly their less invasive and easy application. These hydrogels, being swollen with water, offer a convenient means of effectively filling cartilage defects [60]. For these reasons, the most employed are injectable hydrogels, which homogenously distribute any shape before gelation. Within this, some common natural biomaterials are chitosan, collagen/gelatin, alginate, fibrin, elastin, heparin, chondroitin sulfate, and HA, while synthetic polymers include PEG, poly(L-glutamic acid), poly(vinyl alcohol), poly(propylene fumarate), α,β-poly-(N-hydroxyethyl)-DL-aspartamide, PEG-poly(N-isopropyl acrylamide), methoxy polyethylene glycol, and methoxy polyethylene glycol–poly(ε-caprolactone) [118]. The most common approaches found in the literature divide cell-free and cell-loaded hydrogels. Examples of hydrogels employed in TERM of cartilage tissue are reported in Table 2.
5.2.1. Cell-Free Hydrogels
Chitosan–gelatin hydrogels exhibit both durability and the ability to be finely adjusted in terms of their porosity and degradation rates [161]. In vitro, cell culture with cartilage cells of the human thyroid displays excellent adhesion, proliferation, and secretion of ECM. Lei et al., developed rapamycin-liposome-incorporating HA-based hydrogel microspheres to enhance joint lubrication, maintain cellular homeostasis, and mitigate the progression of osteoarthritis [162]. These microspheres formed self-renewable hydration layers, improved lubrication through a smooth rolling mechanism, and released rapamycin (autophagy activator) to target cartilage, ultimately offering effective lubrication and potential relief for friction-related conditions like osteoarthritis. Han et al., introduced injectable hydrogel microspheres (GelMA@DMA-MPCs) with enhanced lubrication and sustained drug release for the treatment of osteoarthritis (OA) [163]. These microspheres effectively improved lubrication, released diclofenac sodium (DS) for anti-inflammatory action, and demonstrated significant therapeutic effects in an OA rat model, offering a promising approach to the treatment of OA. Injectable marine collagen-based hydrogel effectively preserved the differentiated state of chondrocytes during in vitro culturing, a significant challenge in cartilage regeneration [164]. This biocompatible hydrogel formulation, capable of retaining cells without cytotoxic effects, allows for stiffness modulation and promotes chondrogenic gene expression (namely Sox9, Col2A1, and Acan).
In other studies, an injectable double crosslinked hydrogel modified was developed with sodium alginate and gelatin, loaded with kartogenin (KGN) and TGF-β3 [165]. This cell-free hydrogel system attracted endogenous MSCs, induced chondrogenesis, and showed promise for cartilage repair in a one-step procedure. The study demonstrated the potential of the combination of KGN and TGF-β3 to promote MSC chondrogenesis for cartilage regeneration. Indeed, 4-aminobiphenyl (4-ABP) enzymatically derived from KGN significantly enhanced cartilage repair in a murine model of osteoarthritis. This improvement was achieved through the activation of the PI3K-Akt pathway, which in turn stimulates mesenchymal stem cell (MSC) proliferation and facilitates chondrogenic differentiation [166]. Similarly, Zhu et al., aimed to evaluate the efficacy of an integrated scaffold of 3D-printed decellularized cartilage extracellular matrix (ECM) and PEG diacrylate (PEGDA), in combination with the natural compound honokiol (Hon), to regenerate osteochondral defects [167]. Hon is a polyphenol extracted from Magnolia officinalis with pleiotropic properties, including anti-inflammation and anti-oxidant properties [168]. The research employed a controlled laboratory design using a rat model with cylindrical osteochondral defect in the trochlear groove of the femur. The results indicated that the PEGDA/ECM/Hon scaffold effectively reduced the release of proinflammatory cytokines from LPS-stimulated macrophages in vitro. In addition, the PEGDA/ECM/Hon group demonstrated superior results in terms of International Cartilage Repair Society (ICRS) score, micro-CT evaluation, and histological analysis, suggesting its potential as a promising hydrogel for the repair of osteochondral defects.

Table 2.
Recent research on advanced hydrogels incorporating bioactive molecules and cells for cartilage regeneration: composition, preparation, and the process of application and evaluation.
Table 2.
Recent research on advanced hydrogels incorporating bioactive molecules and cells for cartilage regeneration: composition, preparation, and the process of application and evaluation.
| Hydrogel | Core Material | Preparation | Application | Year | References |
|---|---|---|---|---|---|
| HA | Rapamycin-liposome microspheres | Physical crosslinking | Osteoarthritis | 2022 | [162] |
| Methacrylate gelatin hydrogel microspheres | Diclofenac sodium | Physical crosslinking | Osteoarthritis | 2021 | [163] |
| Marine collagen | Enzymatic crosslinking | Cartilage regeneration | 2020 | [164] | |
| Sodium alginate and gelatin | KGN/TGF-β3 | Double crosslinking | Cartilage regeneration | 2020 | [165,166] |
| PEGDA/ECM | Honokiol | Physical crosslinking | Osteochondral defect repair | 2020 | [167] |
| PEG-GelMA-HA | DPSCs | Physical crosslinking | Chondrogenic differentiation of DPSCs | 2014 | [169] |
| Carrageenan | MSCs | Physical crosslinking | 3D bioprinting | 2016 | [170] |
| Chitosan glycerol phosphate/starch | ASCs | Physical crosslinking | Cartilage tissue engineering | 2010 | [171,172] |
| HSMSSA | Chondrocytes | Di-self-crosslinking | Cartilage repair fille | 2020 | [173] |
5.2.2. Cell-Loaded Hydrogels
Hydrogels provide a proper environment for loading cells, especially SCs. These protect the cells from high shear forces and improve the therapy. Nemeth et al., utilized ultraviolet-assisted capillary force lithography to create nanostructured scaffolds of composite PEG-GelMA-HA hydrogels, promoting the chondrogenic differentiation of dental pulp stem cells (DPSCs) [169]. DPSCs cultured on these nanopatterned scaffolds exhibited upregulation of chondrogenic gene markers and increased collagen type II deposition, indicating that nanotopography and HA cues are crucial for enhancing DPSC chondrogenesis. Thakur et al., developed 2D nanosilicate-reinforced κ-carrageenan hydrogels with shear-thinning properties, enhanced mechanical stiffness, and physiological stability for MSCs delivery [170]. Sa-Lima et al., investigated the development of injectable thermosensitive hydrogels based on chitosan glycerol phosphate (CGP) and starch for cartilage tissue engineering. These hydrogels showed minimal changes in transition temperature with increasing starch concentrations, making them suitable for minimally invasive applications [171]. The addition of starch improved the viscoelastic properties and degradation profile of the hydrogels. In a subsequent phase, the potential of the hydrogels to induce chondrocyte differentiation and cartilage matrix accumulation was evaluated, in particular with encapsulated adipose-derived stromal cells (ADSCs) [172]. The results indicated that chitosan-β-glycerophosphate-starch hydrogels, especially novel CST constructs, were promising for chondrogenic differentiation of ADSCs in cartilage tissue engineering using minimally invasive techniques. Yao et al., developed an injectable thiolated hyaluronic acid (HA-SH) and maleimided hyaluronic acid (HA-Mal) (HSMSSA) hydrogel, formed using thiol oxidation reactions and thiol/maleimide click chemistry, showed physicochemical properties affected by molecular weight and precursor concentration [173]. Although a single HSMSSA gel demonstrated moderate injectivity and promoted cartilage tissue formation, it lacked adhesion sites for efficient cell-cluster connections. Combining HSMSSA with bioactive collagen I in a self-crosslinking blend hydrogel improved degradation resistance, chondrocyte adhesion, and proliferation, together with an upregulation of gene expression levels associated with hyaline cartilage formation and proteoglycan secretion (collagen I, II and X, Sox 9, and aggrecan), making it a potential strategy for clinical cartilage repair fillers with expanded autologous chondrocytes. Overall, there is growing evidence supporting the potential usefulness of hydrogels for treating conditions affecting articular cartilage, such as osteoarthritis or rheumatoid arthritis.
6. Conclusions and Future Trends
In summary, advanced hydrogels hold great promise in the field of tissue engineering and regenerative medicine, especially for the regeneration of bone and cartilage tissues. Their exceptional physical and chemical characteristics, such as mechanical strength, water-retaining capacity, and ability to transport and deliver bioactive agents and cells, make them well suited to treat a variety of bone and cartilage defects. This is especially important for cartilage, whose natural regenerative capacity is limited. However, further research is crucial to optimize the efficacy of these hydrogels and accelerate their integration into clinical practices, where they can be used to treat a variety of conditions, such as bone fractures, infections, metastases, osteoporosis, or osteoarthritis.
Looking ahead, there are several critical findings and future trends to consider. Personalized therapies, facilitated by advances in 3D and 4D bioprinting, are expected to improve the precision of treatments. Stimuli-responsive hydrogels that react to physiological signals and combination therapies with hydrogels, growth factors, stem cells, and gene therapy could offer even more effective solutions. Regulatory approval, long-term safety and efficacy studies, and efforts to bridge the gap between research and commercialization will be essential steps. Patient education and global accessibility efforts will ensure that these cutting-edge hydrogel-based treatments reach a wide range of people in need, ultimately improving their quality of life.
Author Contributions
Conceptualization, D.D.L.-O., D.L.B. and M.A.O.; methodology, D.D.L.-O., D.L.B. and M.A.O.; software, D.D.L.-O., D.L.B. and M.A.O.; validation, B.d.l.T. and M.A.O.; formal analysis, D.D.L.-O., D.L.B., R.E.P.-E., O.F.-M. and C.G.-M.; investigation, D.D.L.-O., D.L.B., R.E.P.-E., O.F.-M., C.G.-M., R.D., J.B., N.G.-H., L.L.-G., M.Á.-M., J.V.S., B.d.l.T. and M.A.O.; resources, M.A.O.; data curation, D.D.L.-O., D.L.B., R.E.P.-E., O.F.-M. and C.G.-M.; writing—original draft preparation, D.D.L.-O., D.L.B., R.E.P.-E., O.F.-M., C.G.-M., R.D., J.B., N.G.-H., L.L.-G., M.Á.-M., J.V.S., B.d.l.T. and M.A.O.; writing—review and editing, D.D.L.-O., D.L.B., R.E.P.-E., O.F.-M., C.G.-M., R.D., J.B., N.G.-H., L.L.-G., M.Á.-M., J.V.S., B.d.l.T. and M.A.O.; supervision, B.d.l.T. and M.A.O.; project administration, M.A.O.; funding acquisition, M.Á.-M. and M.A.O. All authors have read and agreed to the published version of the manuscript.
Funding
The study was supported by SECOT and the European Development Regional Fund “A way to achieve Europe”, as well as P2022/BMD-7321 (Comunidad de Madrid) and ProACapital, Halekulani S.L., and MJR.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Su, N.; Yang, J.; Xie, Y.; Du, X.; Chen, H.; Hong, Z.; Chen, L. Bone function, dysfunction and its role in diseases including critical illness. Int. J. Biol. Sci. 2019, 15, 776–787. [Google Scholar] [CrossRef] [PubMed]
- Florencio-Silva, R.; da Silva Sasso, G.R.; Sasso-Cerri, E.; Simões, M.J.; Cerri, P.S. Biology of Bone Tissue: Structure, Function, and Factors That Influence Bone Cells. BioMed. Res. Int. 2015, 2015, 421746. [Google Scholar] [CrossRef]
- Sophia Fox, A.J.; Bedi, A.; Rodeo, S.A. The Basic Science of Articular Cartilage: Structure, Composition, and Function. Sports Health 2009, 1, 461–468. [Google Scholar] [CrossRef] [PubMed]
- Clynes, M.A.; Harvey, N.C.; Curtis, E.M.; Fuggle, N.R.; Dennison, E.M.; Cooper, C. The epidemiology of osteoporosis. Br. Med. Bull. 2020, 133, 105–117. [Google Scholar] [CrossRef] [PubMed]
- Wu, A.-M.; Bisignano, C.; James, S.L.; Abady, G.G.; Abedi, A.; Abu-Gharbieh, E.; Alhassan, R.K.; Alipour, V.; Arabloo, J.; Asaad, M.; et al. Global, regional, and national burden of bone fractures in 204 countries and territories, 1990–2019: A systematic analysis from the Global Burden of Disease Study 2019. Lancet Health Longev. 2021, 2, e580–e592. [Google Scholar] [CrossRef] [PubMed]
- Litwic, A.; Edwards, M.H.; Dennison, E.M.; Cooper, C. Epidemiology and burden of osteoarthritis. Br. Med. Bull. 2013, 105, 185–199. [Google Scholar] [CrossRef]
- Audigé, L.; Griffin, D.; Bhandari, M.; Kellam, J.; Rüedi, T.P. Path Analysis of Factors for Delayed Healing and Nonunion in 416 Operatively Treated Tibial Shaft Fractures. Clin. Orthop. Relat. Res. 2005, 438, 221–232. [Google Scholar] [CrossRef] [PubMed]
- Tian, R.; Zheng, F.; Zhao, W.; Zhang, Y.; Yuan, J.; Zhang, B.; Li, L. Prevalence and influencing factors of nonunion in patients with tibial fracture: Systematic review and meta-analysis. J. Orthop. Surg. Res. 2020, 15, 377. [Google Scholar] [CrossRef]
- Baldwin, P.; Li, D.J.; Auston, D.A.; Mir, H.S.; Yoon, R.S.; Koval, K.J. Autograft, Allograft, and Bone Graft Substitutes: Clinical Evidence and Indications for Use in the Setting of Orthopaedic Trauma Surgery. J. Orthop. Trauma 2019, 33, 203–213. [Google Scholar] [CrossRef] [PubMed]
- Ansari, M. Bone tissue regeneration: Biology, strategies and interface studies. Prog. Biomater. 2019, 8, 223–237. [Google Scholar] [CrossRef]
- Fernandez De Grado, G.; Keller, L.; Idoux-Gillet, Y.; Wagner, Q.; Musset, A.-M.; Benkirane-Jessel, N.; Bornert, F.; Offner, D. Bone substitutes: A review of their characteristics, clinical use, and perspectives for large bone defects management. J. Tissue Eng. 2018, 9, 2041731418776819. [Google Scholar] [CrossRef]
- Ho-Shui-Ling, A.; Bolander, J.; Rustom, L.E.; Johnson, A.W.; Luyten, F.P.; Picart, C. Bone regeneration strategies: Engineered scaffolds, bioactive molecules and stem cells current stage and future perspectives. Biomaterials 2018, 180, 143–162. [Google Scholar] [CrossRef] [PubMed]
- Fathi-Achachelouei, M.; Knopf-Marques, H.; da Silva, C.E.R.; Barthès, J.; Bat, E.; Tezcaner, A.; Vrana, N.E. Use of Nanoparticles in Tissue Engineering and Regenerative Medicine. Front. Bioeng. Biotechnol. 2019, 7, 113. [Google Scholar] [CrossRef]
- Perez, J.R.; Kouroupis, D.; Li, D.J.; Best, T.M.; Kaplan, L.; Correa, D. Tissue Engineering and Cell-Based Therapies for Fractures and Bone Defects. Front. Bioeng. Biotechnol. 2018, 6, 105. [Google Scholar] [CrossRef]
- Teng, S.; Lee, E.; Wang, P.; Shin, D.; Kim, H. Three-layered membranes of collagen/hydroxyapatite and chitosan for guided bone regeneration. J. Biomed. Mater. Res. Part B Appl. Biomater. 2008, 87B, 132–138. [Google Scholar] [CrossRef]
- Hu, S.; Zhou, Y.; Zhao, Y.; Xu, Y.; Zhang, F.; Gu, N.; Ma, J.; Reynolds, M.A.; Xia, Y.; Xu, H.H. Enhanced bone regeneration and visual monitoring via superparamagnetic iron oxide nanoparticle scaffold in rats. J. Tissue Eng. Regen. Med. 2018, 12, e2085–e2098. [Google Scholar] [CrossRef] [PubMed]
- Ke, Y.; Zhang, X.; Ramakrishna, S.; He, L.; Wu, G. Reactive blends based on polyhydroxyalkanoates: Preparation and biomedical application. Mater. Sci. Eng. C 2017, 70, 1107–1119. [Google Scholar] [CrossRef]
- Langer, R.; Vacanti, J.P. Tissue Engineering. Science 1993, 260, 920–926. [Google Scholar] [CrossRef]
- Cao, D.; Ding, J. Recent advances in regenerative biomaterials. Regen. Biomater. 2022, 9, rbac098. [Google Scholar] [CrossRef]
- Fraile-Martínez, O.; García-Montero, C.; Coca, A.; Álvarez-Mon, M.A.; Monserrat, J.; Gómez-Lahoz, A.M.; Coca, S.; Álvarez-Mon, M.; Acero, J.; Bujan, J.; et al. Applications of Polymeric Composites in Bone Tissue Engineering and Jawbone Regeneration. Polymers 2021, 13, 3429. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Téllez, D.A.; Téllez-Jurado, L.; Rodríguez-Lorenzo, L.M. Hydrogels for Cartilage Regeneration, from Polysaccharides to Hybrids. Polymers 2017, 9, 671. [Google Scholar] [CrossRef] [PubMed]
- Yue, S.; He, H.; Li, B.; Hou, T. Hydrogel as a Biomaterial for Bone Tissue Engineering: A Review. Nanomaterials 2020, 10, 1511. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Hsu, S.-H. Synthesis and Biomedical Applications of Self-healing Hydrogels. Front. Chem. 2018, 6, 449. [Google Scholar] [CrossRef]
- Tayler, I.M.; Stowers, R.S. Engineering hydrogels for personalized disease modeling and regenerative medicine. Acta Biomater. 2021, 132, 4–22. [Google Scholar] [CrossRef]
- Galán-Olleros, M.; Marco, J.; Oteo, D.; Cristóbal-Bilbao, R.; Manrique, E.; García-Maroto, R.; Marco, F.; Cebrián-Parra, J.L. Orthopedic Surgical Treatment and Perioperative Complications in Multiple Myeloma Bone Disease: Analysis of a Series (2009–2018). Ann. Surg. Oncol. 2021, 28, 1158–1166. [Google Scholar] [CrossRef] [PubMed]
- Tetteh, E.S.; Bajaj, S.; Ghodadra, N.S.; Cole, B.J. The Basic Science and Surgical Treatment Options for Articular Cartilage Injuries of the Knee. J. Orthop. Sports Phys. Ther. 2012, 42, 243–253. [Google Scholar] [CrossRef] [PubMed]
- Karsenty, G.; Ferron, M. The contribution of bone to whole-organism physiology. Nature 2012, 481, 314–320. [Google Scholar] [CrossRef] [PubMed]
- Nahian, A.; Davis, D.D. Histology, Osteoprogenitor Cells. In StatPearls—NCBI Bookshelf; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Weng, Y.; Wang, H.; Wu, D.; Xu, S.; Chen, X.; Huang, J.; Feng, Y.; Li, L.; Wang, Z. A novel lineage of osteoprogenitor cells with dual epithelial and mesenchymal properties govern maxillofacial bone homeostasis and regeneration after MSFL. Cell Res. 2022, 32, 814–830. [Google Scholar] [CrossRef]
- Capulli, M.; Paone, R.; Rucci, N. Osteoblast and osteocyte: Games without frontiers. Arch. Biochem. Biophys. 2014, 561, 3–12. [Google Scholar] [CrossRef] [PubMed]
- Long, F. Building strong bones: Molecular regulation of the osteoblast lineage. Nat. Rev. Mol. Cell. Biol. 2012, 13, 27–38. [Google Scholar] [CrossRef]
- Rochefort, G.Y.; Pallu, S.; Benhamou, C.L. Osteocyte: The unrecognized side of bone tissue. Osteoporos. Int. 2010, 21, 1457–1469. [Google Scholar] [CrossRef] [PubMed]
- Franz-Odendaal, T.A.; Hall, B.K.; Witten, P.E. Buried alive: How osteoblasts become osteocytes. Dev. Dyn. 2006, 235, 176–190. [Google Scholar] [CrossRef] [PubMed]
- Tsukasaki, M.; Takayanagi, H. Osteoclast biology in the single-cell era. Inflamm. Regen. 2022, 42, 27. [Google Scholar] [CrossRef] [PubMed]
- Jacome-Galarza, C.E.; Percin, G.I.; Muller, J.T.; Mass, E.; Lazarov, T.; Eitler, J.; Rauner, M.; Yadav, V.K.; Crozet, L.; Bohm, M.; et al. Developmental origin, functional maintenance and genetic rescue of osteoclasts. Nature 2019, 568, 541–545. [Google Scholar] [CrossRef]
- De Leon-Oliva, D.; Barrena-Blázquez, S.; Jiménez-Álvarez, L.; Fraile-Martinez, O.; García-Montero, C.; López-González, L.; Torres-Carranza, D.; García-Puente, L.M.; Carranza, S.T.; Álvarez-Mon, M.Á.; et al. The RANK–RANKL–OPG System: A Multifaceted Regulator of Homeostasis, Immunity, and Cancer. Medicina 2023, 59, 1752. [Google Scholar] [CrossRef]
- Wein, M.N. Bone Lining Cells: Normal Physiology and Role in Response to Anabolic Osteoporosis Treatments. Curr. Mol. Biol. Rep. 2017, 3, 79–84. [Google Scholar] [CrossRef]
- Sroga, G.E.; Vashishth, D. Effects of Bone Matrix Proteins on Fracture and Fragility in Osteoporosis. Curr. Osteoporos. Rep. 2012, 10, 141–150. [Google Scholar] [CrossRef] [PubMed]
- Ma, C.; Du, T.; Niu, X.; Fan, Y. Biomechanics and mechanobiology of the bone matrix. Bone Res. 2022, 10, 59. [Google Scholar] [CrossRef]
- Feng, X. Chemical and Biochemical Basis of Cell-Bone Matrix Interaction in Health and Disease. Curr. Chem. Biol. 2009, 3, 189–196. [Google Scholar] [CrossRef] [PubMed]
- Lin, X.; Patil, S.; Gao, Y.-G.; Qian, A. The Bone Extracellular Matrix in Bone Formation and Regeneration. Front. Pharmacol. 2020, 11, 757. [Google Scholar] [CrossRef]
- Huang, S.; Jin, M.; Su, N.; Chen, L. New insights on the reparative cells in bone regeneration and repair. Biol. Rev. 2021, 96, 357–375. [Google Scholar] [CrossRef] [PubMed]
- Löffler, J.; Noom, A.; Ellinghaus, A.; Dienelt, A.; Kempa, S.; Duda, G.N. A comprehensive molecular profiling approach reveals metabolic alterations that steer bone tissue regeneration. Commun. Biol. 2023, 6, 327. [Google Scholar] [CrossRef] [PubMed]
- Dimitriou, R.; Jones, E.; McGonagle, D.; Giannoudis, P.V. Bone regeneration: Current concepts and future directions. BMC Med. 2011, 9, 66. [Google Scholar] [CrossRef]
- Siddiqui, J.A.; Partridge, N.C. Physiological Bone Remodeling: Systemic Regulation and Growth Factor Involvement. Physiology 2016, 31, 233–245. [Google Scholar] [CrossRef] [PubMed]
- Dallas, S.L.; Prideaux, M.; Bonewald, L.F. The Osteocyte: An Endocrine Cell … and More. Endocr. Rev. 2013, 34, 658–690. [Google Scholar] [CrossRef] [PubMed]
- Kenkre, J.S.; Bassett, J.H.D. The bone remodelling cycle. Ann. Clin. Biochem. 2018, 55, 308–327. [Google Scholar] [CrossRef] [PubMed]
- Duda, G.N.; Geissler, S.; Checa, S.; Tsitsilonis, S.; Petersen, A.; Schmidt-Bleek, K. The decisive early phase of bone regeneration. Nat. Rev. Rheumatol. 2023, 19, 78–95. [Google Scholar] [CrossRef] [PubMed]
- Salhotra, A.; Shah, H.N.; Levi, B.; Longaker, M.T. Mechanisms of bone development and repair. Nat. Rev. Mol. Cell Biol. 2020, 21, 696–711. [Google Scholar] [CrossRef] [PubMed]
- Einhorn, T.A.; Gerstenfeld, L.C. Fracture healing: Mechanisms and interventions. Nat. Rev. Rheumatol. 2015, 11, 45–54. [Google Scholar] [CrossRef]
- Perez, R.A.; Seo, S.-J.; Won, J.-E.; Lee, E.-J.; Jang, J.-H.; Knowles, J.C.; Kim, H.-W. Therapeutically relevant aspects in bone repair and regeneration. Mater. Today 2015, 18, 573–589. [Google Scholar] [CrossRef]
- Wachsmuth, L.; Söder, S.; Fan, Z.; Finger, F.; Aigner, T. Immunolocalization of matrix proteins in different human cartilage subtypes. Histol. Histopathol. 2006, 21, 477–485. [Google Scholar] [CrossRef]
- Vincent, T.L.; McClurg, O.; Troeberg, L. The Extracellular Matrix of Articular Cartilage Controls the Bioavailability of Pericellular Matrix-Bound Growth Factors to Drive Tissue Homeostasis and Repair. Int. J. Mol. Sci. 2022, 23, 6003. [Google Scholar] [CrossRef]
- Krishnan, Y.; Grodzinsky, A.J. Cartilage Diseases. Matrix Biol. 2018, 71–72, 51–69. [Google Scholar] [CrossRef] [PubMed]
- Rikkers, M.; Korpershoek, J.V.; Levato, R.; Malda, J.; Vonk, L.A. The clinical potential of articular cartilage-derived progenitor cells: A systematic review. npj Regen. Med. 2022, 7, 2. [Google Scholar] [CrossRef] [PubMed]
- Degen, K.E.; Gourdie, R.G. Embryonic wound healing: A primer for engineering novel therapies for tissue repair. Birth Defects Res. Part C Embryo Today Rev. 2012, 96, 258–270. [Google Scholar] [CrossRef] [PubMed]
- Roseti, L.; Desando, G.; Cavallo, C.; Petretta, M.; Grigolo, B. Articular Cartilage Regeneration in Osteoarthritis. Cells 2019, 8, 1305. [Google Scholar] [CrossRef]
- Burleigh, A.; Chanalaris, A.; Gardiner, M.D.; Driscoll, C.; Boruc, O.; Saklatvala, J.; Vincent, T.L. Joint immobilization prevents murine osteoarthritis and reveals the highly mechanosensitive nature of protease expression in vivo. Arthritis Rheum. 2012, 64, 2278–2288. [Google Scholar] [CrossRef] [PubMed]
- Huey, D.J.; Hu, J.C.; Athanasiou, K.A. Unlike Bone, Cartilage Regeneration Remains Elusive. Science 2012, 338, 917–921. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Shah, K.M.; Luo, J. Strategies for Articular Cartilage Repair and Regeneration. Front. Bioeng. Biotechnol. 2021, 9, 770655. [Google Scholar] [CrossRef] [PubMed]
- Bashir, S.; Hina, M.; Iqbal, J.; Rajpar, A.H.; Mujtaba, M.A.; Alghamdi, N.A.; Wageh, S.; Ramesh, K.; Ramesh, S. Fundamental Concepts of Hydrogels: Synthesis, Properties, and Their Applications. Polymers 2020, 12, 2702. [Google Scholar] [CrossRef] [PubMed]
- Ho, T.-C.; Chang, C.-C.; Chan, H.-P.; Chung, T.-W.; Shu, C.-W.; Chuang, K.-P.; Duh, T.-H.; Yang, M.-H.; Tyan, Y.-C. Hydrogels: Properties and Applications in Biomedicine. Molecules 2022, 27, 2902. [Google Scholar] [CrossRef] [PubMed]
- Ortega, M.A.; De Leon-Oliva, D.; Boaru, D.L.; Fraile-Martinez, O.; García-Montero, C.; Diaz, R.; Coca, S.; Barrena-Blázquez, S.; Bujan, J.; García-Honduvilla, N.; et al. Unraveling the New Perspectives on Antimicrobial Hydrogels: State-of-the-Art and Translational Applications. Gels 2023, 9, 617. [Google Scholar] [CrossRef] [PubMed]
- Cao, H.; Duan, L.; Zhang, Y.; Cao, J.; Zhang, K. Current hydrogel advances in physicochemical and biological response-driven biomedical application diversity. Signal Transduct. Target. Ther. 2021, 6, 426. [Google Scholar] [CrossRef] [PubMed]
- Varaprasad, K.; Raghavendra, G.M.; Jayaramudu, T.; Yallapu, M.M.; Sadiku, R. A mini review on hydrogels classification and recent developments in miscellaneous applications. Mater. Sci. Eng. C 2017, 79, 958–971. [Google Scholar] [CrossRef]
- Catoira, M.C.; Fusaro, L.; Di Francesco, D.; Ramella, M.; Boccafoschi, F. Overview of natural hydrogels for regenerative medicine applications. J. Mater. Sci. Mater. Med. 2019, 30, 115. [Google Scholar] [CrossRef] [PubMed]
- Kapusta, O.; Jarosz, A.; Stadnik, K.; Giannakoudakis, D.A.; Barczyński, B.; Barczak, M. Antimicrobial Natural Hydrogels in Biomedicine: Properties, Applications, and Challenges—A Concise Review. Int. J. Mol. Sci. 2023, 24, 2191. [Google Scholar] [CrossRef]
- Cifuentes, A.; Gómez-Gil, V.; Ortega, M.A.; Asúnsolo, Á.; Coca, S.; Román, J.S.; Álvarez-Mon, M.; Buján, J.; García-Honduvilla, N. Chitosan hydrogels functionalized with either unfractionated heparin or bemiparin improve diabetic wound healing. Biomed. Pharmacother. 2020, 129, 110498. [Google Scholar] [CrossRef]
- Teodorescu, M.; Bercea, M.; Morariu, S. Biomaterials of PVA and PVP in medical and pharmaceutical applications: Perspectives and challenges. Biotechnol. Adv. 2019, 37, 109–131. [Google Scholar] [CrossRef] [PubMed]
- Madduma-Bandarage, U.S.K.; Madihally, S.V. Synthetic hydrogels: Synthesis, novel trends, and applications. J. Appl. Polym. Sci. 2021, 138, 50376. [Google Scholar] [CrossRef]
- Ahmad, Z.; Salman, S.; Khan, S.A.; Amin, A.; Rahman, Z.U.; Al-Ghamdi, Y.O.; Akhtar, K.; Bakhsh, E.M.; Khan, S.B. Versatility of Hydrogels: From Synthetic Strategies, Classification, and Properties to Biomedical Applications. Gels 2022, 8, 167. [Google Scholar] [CrossRef] [PubMed]
- Singhal, R.; Gupta, K. A Review: Tailor-made Hydrogel Structures (Classifications and Synthesis Parameters). Polym.-Plast. Technol. Eng. 2016, 55, 54–70. [Google Scholar] [CrossRef]
- Rebers, L.; Reichsöllner, R.; Regett, S.; Tovar, G.E.M.; Borchers, K.; Baudis, S.; Southan, A. Differentiation of physical and chemical cross-linking in gelatin methacryloyl hydrogels. Sci. Rep. 2021, 11, 3256. [Google Scholar] [CrossRef] [PubMed]
- Parhi, R. Cross-Linked Hydrogel for Pharmaceutical Applications: A Review. Adv. Pharm. Bull. 2017, 7, 515–530. [Google Scholar] [CrossRef] [PubMed]
- Gadhave, R.V.; Mahanwar, P.A.; Gadekar, P.T. Effect of glutaraldehyde on thermal and mechanical properties of starch and polyvinyl alcohol blends. Des. Monomers Polym. 2019, 22, 164–170. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Zhu, K.; Jiao, T.; Xing, R.; Hong, W.; Zhang, L.; Zhang, Q.; Peng, Q. Preparation of graphene oxide-polymer composite hydrogels via thiol-ene photopolymerization as efficient dye adsorbents for wastewater treatment. Colloids Surf. A Physicochem. Eng. Asp. 2017, 529, 668–676. [Google Scholar] [CrossRef]
- Smith, L.J.; Taimoory, S.M.; Tam, R.Y.; Baker, A.E.G.; Mohammad, N.B.; Trant, J.F.; Shoichet, M.S. Diels–Alder Click-Cross-Linked Hydrogels with Increased Reactivity Enable 3D Cell Encapsulation. Biomacromolecules 2018, 19, 926–935. [Google Scholar] [CrossRef]
- Maitra, J.; Shukla, V.K. Cross-linking in Hydrogels—A Review. Am. J. Polym. Sci. 2014, 4, 25–31. [Google Scholar]
- Elsayed, M.M. Hydrogel Preparation Technologies: Relevance Kinetics, Thermodynamics and Scaling up Aspects. J. Polym. Environ. 2019, 27, 871–891. [Google Scholar] [CrossRef]
- Nasution, H.; Harahap, H.; Dalimunthe, N.F.; Ginting, M.H.S.; Jaafar, M.; Tan, O.O.H.; Aruan, H.K.; Herfananda, A.L. Hydrogel and Effects of Crosslinking Agent on Cellulose-Based Hydrogels: A Review. Gels 2022, 8, 568. [Google Scholar] [CrossRef] [PubMed]
- Naranjo-Alcazar, R.; Bendix, S.; Groth, T.; Ferrer, G.G. Research Progress in Enzymatically Cross-Linked Hydrogels as Injectable Systems for Bioprinting and Tissue Engineering. Gels 2023, 9, 230. [Google Scholar] [CrossRef]
- Badali, E.; Hosseini, M.; Mohajer, M.; Hassanzadeh, S.; Saghati, S.; Hilborn, J.; Khanmohammadi, M. Enzymatic Crosslinked Hydrogels for Biomedical Application. Polym. Sci. Ser. A 2021, 63, S1–S22. [Google Scholar] [CrossRef]
- Song, W.; Ko, J.; Choi, Y.H.; Hwang, N.S. Recent advancements in enzyme-mediated crosslinkable hydrogels: In vivo-mimicking strategies. APL Bioeng. 2021, 5, 021502. [Google Scholar] [CrossRef] [PubMed]
- Barbosa, M.; Martins, M.C.L.; Gomes, P. Grafting Techniques towards Production of Peptide-Tethered Hydrogels, a Novel Class of Materials with Biomedical Interest. Gels 2015, 1, 194–218. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, A.G.; Sayed, A.Z.; El-Wahab, H.A.; Sayah, M.M. Synthesis of a hydrogel by grafting of acrylamide-co-sodium methacrylate onto chitosan for effective adsorption of Fuchsin basic dye. Int. J. Biol. Macromol. 2020, 159, 422–432. [Google Scholar] [CrossRef]
- Chung, Y.-C.; Bae, J.C.; Choi, J.W.; Chun, B.C. The preparation of hydrogel-like polyurethane using the graft polymerization of N,N-dimethylaminoethyl methacrylate and acrylic acid. Polym. Bull. 2019, 76, 6371–6386. [Google Scholar] [CrossRef]
- Xu, J.; Abetz, V. Synthesis of a Degradable Hydrogel Based on a Graft Copolymer with Unexpected Thermoresponsiveness. Macromol. Chem. Phys. 2022, 223, 2200058. [Google Scholar] [CrossRef]
- Yang, J.; Rao, L.; Wang, Y.; Zhao, Y.; Liu, D.; Wang, Z.; Fu, L.; Wang, Y.; Yang, X.; Li, Y.; et al. Recent Advances in Smart Hydrogels Prepared by Ionizing Radiation Technology for Biomedical Applications. Polymers 2022, 14, 4377. [Google Scholar] [CrossRef] [PubMed]
- Raza, M.A.; Jeong, J.-O.; Park, S.H. State-of-the-Art Irradiation Technology for Polymeric Hydrogel Fabrication and Application in Drug Release System. Front. Mater. 2021, 8, 769436. [Google Scholar] [CrossRef]
- Călina, I.; Demeter, M.; Scărișoreanu, A.; Sătulu, V.; Mitu, B. One Step e-Beam Radiation Cross-Linking of Quaternary Hydrogels Dressings Based on Chitosan-Poly(Vinyl-Pyrrolidone)-Poly(Ethylene Glycol)-Poly(Acrylic Acid). Int. J. Mol. Sci. 2020, 21, 9236. [Google Scholar] [CrossRef]
- Rahaman, M.S.; Hasnine, S.M.M.; Ahmed, T.; Sultana, S.; Bhuiyan, M.A.Q.; Manir, M.S.; Ullah, N.; Sen, S.K.; Hossain, M.N.; Hossain, M.S.; et al. Radiation crosslinked polyvinyl alcohol/polyvinyl pyrrolidone/acrylic acid hydrogels: Swelling, crosslinking and dye adsorption study. Iran. Polym. J. 2021, 30, 1101–1116. [Google Scholar] [CrossRef]
- Jeong, J.-O.; Park, J.-S.; Kim, E.J.; Jeong, S.-I.; Lee, J.Y.; Lim, Y.-M. Preparation of Radiation Cross-Linked Poly(Acrylic Acid) Hydrogel Containing Metronidazole with Enhanced Antibacterial Activity. Int. J. Mol. Sci. 2020, 21, 187. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, E.M. Hydrogel: Preparation, characterization, and applications: A review. J. Adv. Res. 2015, 6, 105–121. [Google Scholar] [CrossRef] [PubMed]
- Kumar Singh, S.; Dhyani, A.; Juyal, D. Hydrogel: Preparation, Characterization and Applications. Pharma Innov. J. 2017, 6, 25–32. [Google Scholar]
- Dragan, E.S. Design and applications of interpenetrating polymer network hydrogels. A review. Chem. Eng. J. 2014, 243, 572–590. [Google Scholar] [CrossRef]
- Crosby, C.O.; Stern, B.; Kalkunte, N.; Pedahzur, S.; Ramesh, S.; Zoldan, J. Interpenetrating polymer network hydrogels as bioactive scaffolds for tissue engineering. Rev. Chem. Eng. 2022, 38, 347–361. [Google Scholar] [CrossRef] [PubMed]
- Gugoasa, A.I.; Racovita, S.; Vasiliu, S.; Popa, M. Semi-Interpenetrating Polymer Networks Based on Hydroxy-Ethyl Methacrylate and Poly(4-vinylpyridine)/Polybetaines, as Supports for Sorption and Release of Tetracycline. Polymers 2023, 15, 490. [Google Scholar] [CrossRef]
- Dhand, A.P.; Galarraga, J.H.; Burdick, J.A. Enhancing Biopolymer Hydrogel Functionality through Interpenetrating Networks. Trends Biotechnol. 2021, 39, 519–538. [Google Scholar] [CrossRef]
- Han, F.; Wang, J.; Ding, L.; Hu, Y.; Li, W.; Yuan, Z.; Guo, Q.; Zhu, C.; Yu, L.; Wang, H.; et al. Tissue Engineering and Regenerative Medicine: Achievements, Future, and Sustainability in Asia. Front. Bioeng. Biotechnol. 2020, 8, 83. [Google Scholar] [CrossRef] [PubMed]
- Henkel, J.; Woodruff, M.A.; Epari, D.R.; Steck, R.; Glatt, V.; Dickinson, I.C.; Choong, P.F.M.; Schuetz, M.A.; Hutmacher, D.W. Bone Regeneration Based on Tissue Engineering Conceptions—A 21st Century Perspective. Bone Res. 2013, 1, 216–248. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Hu, J.; Athanasiou, K.A. The Role of Tissue Engineering in Articular Cartilage Repair and Regeneration. Crit. Rev. Biomed. Eng. 2009, 37, 1–57. [Google Scholar] [CrossRef]
- Li, X.; Sun, Q.; Li, Q.; Kawazoe, N.; Chen, G. Functional Hydrogels with Tunable Structures and Properties for Tissue Engineering Applications. Front. Chem. 2018, 6, 499. [Google Scholar] [CrossRef]
- Nie, J.; Pei, B.; Wang, Z.; Hu, Q. Construction of ordered structure in polysaccharide hydrogel: A review. Carbohydr. Polym. 2019, 205, 225–235. [Google Scholar] [CrossRef]
- Gibbs, D.M.R.; Black, C.R.M.; Dawson, J.I.; Oreffo, R.O.C. A review of hydrogel use in fracture healing and bone regeneration. J. Tissue Eng. Regen. Med. 2014, 10, 187–198. [Google Scholar] [CrossRef] [PubMed]
- Kolambkar, Y.M.; Dupont, K.M.; Boerckel, J.D.; Huebsch, N.; Mooney, D.J.; Hutmacher, D.W.; Guldberg, R.E. An alginate-based hybrid system for growth factor delivery in the functional repair of large bone defects. Biomaterials 2011, 32, 65–74. [Google Scholar] [CrossRef] [PubMed]
- Bai, X.; Gao, M.; Syed, S.; Zhuang, J.; Xu, X.; Zhang, X.-Q. Bioactive hydrogels for bone regeneration. Bioact. Mater. 2018, 3, 401–417. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Yu, C.; Xiong, Y.; Chen, K.; Liu, P.; Panayi, A.C.; Xiao, X.; Feng, Q.; Mi, B.; Liu, G. Multifunctional hydrogel enhances bone regeneration through sustained release of Stromal Cell-Derived Factor-1α and exosomes. Bioact. Mater. 2023, 25, 460–471. [Google Scholar] [CrossRef]
- Li, D.; Zhou, J.; Zhang, M.; Ma, Y.; Yang, Y.; Han, X.; Wang, X. Long-term delivery of alendronate through an injectable tetra-PEG hydrogel to promote osteoporosis therapy. Biomater. Sci. 2020, 8, 3138–3146. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Z.; Li, G.; Ruan, H.; Chen, K.; Cai, Z.; Lu, G.; Li, R.; Deng, L.; Cai, M.; Cui, W. Capturing Magnesium Ions via Microfluidic Hydrogel Microspheres for Promoting Cancellous Bone Regeneration. ACS Nano 2021, 15, 13041–13054. [Google Scholar] [CrossRef]
- Gong, Y.; Bu, Y.; Li, Y.; Hao, D.; He, B.; Kong, L.; Huang, W.; Gao, X.; Zhang, B.; Qu, Z.; et al. Hydrogel-based delivery system applied in the local anti-osteoporotic bone defects. Front. Bioeng. Biotechnol. 2022, 10, 1058300. [Google Scholar] [CrossRef]
- Bai, H.; Zhao, Y.; Wang, C.; Wang, Z.; Wang, J.; Liu, H.; Feng, Y.; Lin, Q.; Li, Z.; Liu, H. Enhanced osseointegration of three-dimensional supramolecular bioactive interface through osteoporotic microenvironment regulation. Theranostics 2020, 10, 4779–4794. [Google Scholar] [CrossRef]
- Ding, W.; Zhou, Q.; Lu, Y.; Wei, Q.; Tang, H.; Zhang, D.; Liu, Z.; Wang, G.; Wu, D. ROS-scavenging hydrogel as protective carrier to regulate stem cells activity and promote osteointegration of 3D printed porous titanium prosthesis in osteoporosis. Front. Bioeng. Biotechnol. 2023, 11, 1103611. [Google Scholar] [CrossRef] [PubMed]
- Seo, B.-B.; Kwon, Y.; Kim, J.; Hong, K.H.; Kim, S.-E.; Song, H.-R.; Kim, Y.-M.; Song, S.-C. Injectable polymeric nanoparticle hydrogel system for long-term anti-inflammatory effect to treat osteoarthritis. Bioact. Mater. 2022, 7, 14–25. [Google Scholar] [CrossRef] [PubMed]
- Vinikoor, T.; Dzidotor, G.K.; Le, T.T.; Liu, Y.; Kan, H.-M.; Barui, S.; Chorsi, M.T.; Curry, E.J.; Reinhardt, E.; Wang, H.; et al. Injectable and biodegradable piezoelectric hydrogel for osteoarthritis treatment. Nat. Commun. 2023, 14, 6257. [Google Scholar] [CrossRef] [PubMed]
- Duan, W.-L.; Zhang, L.-N.; Bohara, R.; Martin-Saldaña, S.; Yang, F.; Zhao, Y.-Y.; Xie, Y.; Bu, Y.-Z.; Pandit, A. Adhesive hydrogels in osteoarthritis: From design to application. Mil. Med. Res. 2023, 10, 4. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Qiu, Y.; Qu, L.; Wang, Q.; Zhou, Q. Hydrogels for Treatment of Different Degrees of Osteoarthritis. Front. Bioeng. Biotechnol. 2022, 10, 858656. [Google Scholar] [CrossRef]
- Wei, Z.; Zhang, G.; Cao, Q.; Zhao, T.; Bian, Y.; Zhu, W.; Weng, X. Recent Developments and Current Applications of Organic Nanomaterials in Cartilage Repair. Bioengineering 2022, 9, 390. [Google Scholar] [CrossRef]
- Liu, M.; Zeng, X.; Ma, C.; Yi, H.; Ali, Z.; Mou, X.; Li, S.; Deng, Y.; He, N. Injectable hydrogels for cartilage and bone tissue engineering. Bone Res. 2017, 5, 17014. [Google Scholar] [CrossRef]
- Ghandforoushan, P.; Alehosseini, M.; Golafshan, N.; Castilho, M.; Dolatshahi-Pirouz, A.; Hanaee, J.; Davaran, S.; Orive, G. Injectable hydrogels for cartilage and bone tissue regeneration: A review. Int. J. Biol. Macromol. 2023, 246, 125674. [Google Scholar] [CrossRef]
- Jung, S.W.; Oh, S.H.; Lee, I.S.; Byun, J.-H.; Lee, J.H. In Situ Gelling Hydrogel with Anti-Bacterial Activity and Bone Healing Property for Treatment of Osteomyelitis. Tissue Eng. Regen. Med. 2019, 16, 479–490. [Google Scholar] [CrossRef]
- Xie, X.; Wei, J.; Zhang, B.; Xiong, W.; He, Z.; Zhang, Y.; Gao, C.; Zhao, Y.; Liu, B. A self-assembled bilayer polypeptide-engineered hydrogel for spatiotemporal modulation of bactericidal and anti-inflammation process in osteomyelitis treatment. J. Nanobiotechnol. 2022, 20, 416. [Google Scholar] [CrossRef]
- Xin, W.; Gao, Y.; Yue, B. Recent Advances in Multifunctional Hydrogels for the Treatment of Osteomyelitis. Front. Bioeng. Biotechnol. 2022, 10, 865250. [Google Scholar] [CrossRef] [PubMed]
- Kuo, C.-Y.; Lin, T.-Y.; Yeh, Y.-C. Hydrogel-Based Strategies for the Management of Osteomyelitis. ACS Biomater. Sci. Eng. 2023, 9, 1843–1861. [Google Scholar] [CrossRef] [PubMed]
- Vega, S.L.; Kwon, M.Y.; Burdick, J.A. Recent advances in hydrogels for cartilage tissue engineering. Eur. Cells Mater. 2017, 33, 59–75. [Google Scholar] [CrossRef] [PubMed]
- Escalante, S.; Rico, G.; Becerra, J.; Román, J.S.; Vázquez-Lasa, B.; Aguilar, M.R.; Durán, I.; García-Fernández, L. Chemically crosslinked hyaluronic acid-chitosan hydrogel for application on cartilage regeneration. Front. Bioeng. Biotechnol. 2022, 10, 1058355. [Google Scholar] [CrossRef]
- Spiller, K.L.; Maher, S.A.; Lowman, A.M. Hydrogels for the Repair of Articular Cartilage Defects. Tissue Eng. Part B Rev. 2011, 17, 281–299. [Google Scholar] [CrossRef] [PubMed]
- Ding, Q.; Zhang, S.; Liu, X.; Zhao, Y.; Yang, J.; Chai, G.; Wang, N.; Ma, S.; Liu, W.; Ding, C. Hydrogel Tissue Bioengineered Scaffolds in Bone Repair: A Review. Molecules 2023, 28, 7039. [Google Scholar] [CrossRef] [PubMed]
- Xue, X.; Hu, Y.; Wang, S.; Chen, X.; Jiang, Y.; Su, J. Fabrication of physical and chemical crosslinked hydrogels for bone tissue engineering. Bioact. Mater. 2022, 12, 327–339. [Google Scholar] [CrossRef]
- Sun, Y.; Nan, D.; Jin, H.; Qu, X. Recent advances of injectable hydrogels for drug delivery and tissue engineering applications. Polym. Test. 2020, 81, 106283. [Google Scholar] [CrossRef]
- Almawash, S.; Osman, S.K.; Mustafa, G.; El Hamd, M.A. Current and Future Prospective of Injectable Hydrogels—Design Challenges and Limitations. Pharmaceuticals 2022, 15, 371. [Google Scholar] [CrossRef]
- Olov, N.; Bagheri-Khoulenjani, S.; Mirzadeh, H. Injectable hydrogels for bone and cartilage tissue engineering: A review. Prog. Biomater. 2022, 11, 113–135. [Google Scholar] [CrossRef] [PubMed]
- Martorell, L.; López-Fernández, A.; García-Lizarribar, A.; Sabata, R.; Gálvez-Martín, P.; Samitier, J.; Vives, J. Preservation of critical quality attributes of mesenchymal stromal cells in 3D bioprinted structures by using natural hydrogel scaffolds. Biotechnol. Bioeng. 2023, 120, 2717–2724. [Google Scholar] [CrossRef]
- Fatimi, A.; Okoro, O.V.; Podstawczyk, D.; Siminska-Stanny, J.; Shavandi, A. Natural Hydrogel-Based Bio-Inks for 3D Bioprinting in Tissue Engineering: A Review. Gels 2022, 8, 179. [Google Scholar] [CrossRef] [PubMed]
- Chyzy, A.; Plonska-Brzezinska, M.E. Hydrogel Properties and Their Impact on Regenerative Medicine and Tissue Engineering. Molecules 2020, 25, 5795. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.; Xiong, J.; Wang, D.; Zhang, J.; Yang, L.; Sun, S.; Liang, Y. 3D Bioprinting of Hydrogels for Cartilage Tissue Engineering. Gels 2021, 7, 144. [Google Scholar] [CrossRef]
- Yang, X.; Li, S.; Ren, Y.; Qiang, L.; Liu, Y.; Wang, J.; Dai, K. 3D printed hydrogel for articular cartilage regeneration. Compos. Part B Eng. 2022, 237, 109863. [Google Scholar] [CrossRef]
- Yang, Z.; Yi, P.; Liu, Z.; Zhang, W.; Mei, L.; Feng, C.; Tu, C.; Li, Z. Stem Cell-Laden Hydrogel-Based 3D Bioprinting for Bone and Cartilage Tissue Engineering. Front. Bioeng. Biotechnol. 2022, 10, 865770. [Google Scholar] [CrossRef] [PubMed]
- Zhai, X.; Ma, Y.; Hou, C.; Gao, F.; Zhang, Y.; Ruan, C.; Pan, H.; Lu, W.W.; Liu, W. 3D-Printed High Strength Bioactive Supramolecular Polymer/Clay Nanocomposite Hydrogel Scaffold for Bone Regeneration. ACS Biomater. Sci. Eng. 2017, 3, 1109–1118. [Google Scholar] [CrossRef]
- Kang, X.; Zhang, X.-B.; Gao, X.-D.; Hao, D.-J.; Li, T.; Xu, Z.-W. Bioprinting for bone tissue engineering. Front. Bioeng. Biotechnol. 2022, 10, 1036375. [Google Scholar] [CrossRef]
- Zhang, X.; Yang, Y.; Yang, Z.; Ma, R.; Aimaijiang, M.; Xu, J.; Zhang, Y.; Zhou, Y. Four-Dimensional Printing and Shape Memory Materials in Bone Tissue Engineering. Int. J. Mol. Sci. 2023, 24, 814. [Google Scholar] [CrossRef]
- Wan, Z.; Zhang, P.; Liu, Y.; Lv, L.; Zhou, Y. Four-dimensional bioprinting: Current developments and applications in bone tissue engineering. Acta Biomater. 2020, 101, 26–42. [Google Scholar] [CrossRef] [PubMed]
- Albrektsson, T.; Johansson, C. Osteoinduction, osteoconduction and osseointegration. Eur. Spine J. 2001, 10, S96–S101. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Yang, L.; Liu, K.; Gao, F. Hydrogel scaffolds in bone regeneration: Their promising roles in angiogenesis. Front. Pharmacol. 2023, 14, 1050954. [Google Scholar] [CrossRef] [PubMed]
- Short, A.R.; Koralla, D.; Deshmukh, A.; Wissel, B.; Stocker, B.; Calhoun, M.; Dean, D.; Winter, J.O. Hydrogels that allow and facilitate bone repair, remodeling, and regeneration. J. Mater. Chem. B 2015, 3, 7818–7830. [Google Scholar] [CrossRef] [PubMed]
- Shekaran, A.; García, J.R.; Clark, A.Y.; Kavanaugh, T.E.; Lin, A.S.; Guldberg, R.E.; García, A.J. Bone regeneration using an alpha 2 beta 1 integrin-specific hydrogel as a BMP-2 delivery vehicle. Biomaterials 2014, 35, 5453–5461. [Google Scholar] [CrossRef] [PubMed]
- Mi, L.; Liu, H.; Gao, Y.; Miao, H.; Ruan, J. Injectable nanoparticles/hydrogels composite as sustained release system with stromal cell-derived factor-1α for calvarial bone regeneration. Int. J. Biol. Macromol. 2017, 101, 341–347. [Google Scholar] [CrossRef]
- Zhang, F.; Lv, M.; Wang, S.; Li, M.; Wang, Y.; Hu, C.; Hu, W.; Wang, X.; Wang, X.; Liu, Z.; et al. Ultrasound-triggered biomimetic ultrashort peptide nanofiber hydrogels promote bone regeneration by modulating macrophage and the osteogenic immune microenvironment. Bioact. Mater. 2024, 31, 231–246. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.-L.; Fu, W.; Ding, Y.-J.; Hettinghouse, A.; Lendhey, M.; Schwarzkopf, R.; Kennedy, O.D.; Liu, C.-J. Progranulin derivative Atsttrin protects against early osteoarthritis in mouse and rat models. Arthritis Res. Ther. 2017, 19, 280. [Google Scholar] [CrossRef]
- Moradi, L.; Witek, L.; Nayak, V.V.; Pereira, A.C.; Kim, E.; Good, J.; Liu, C.-J. Injectable hydrogel for sustained delivery of progranulin derivative Atsttrin in treating diabetic fracture healing. Biomaterials 2023, 301, 122289. [Google Scholar] [CrossRef]
- Wang, S.; He, W.; Wang, H.; Liu, D.; Wang, M.; Yang, H.; Pan, G.; Li, B. Hematoma-like dynamic hydrogelation through natural glycopeptide molecular recognition for infected bone fracture repair. Bioact. Mater. 2023, 30, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Cheng, L.; Zhou, Z.; Li, Q.; Li, W.; Li, X.; Li, G.; Fan, J.; Yu, L.; Yin, G. Dendronized chitosan hydrogel with GIT1 to accelerate bone defect repair through increasing local neovascular amount. Bone Rep. 2023, 19, 101712. [Google Scholar] [CrossRef]
- Moussi, H.; Weiss, P.; Le Bideau, J.; Gautier, H.; Charbonnier, B. Injectable macromolecule-based calcium phosphate bone substitutes. Mater. Adv. 2022, 3, 6125–6141. [Google Scholar] [CrossRef]
- Fatimi, A.; Tassin, J.-F.; Axelos, M.A.V.; Weiss, P. The stability mechanisms of an injectable calcium phosphate ceramic suspension. J. Mater. Sci. Mater. Med. 2010, 21, 1799–1809. [Google Scholar] [CrossRef] [PubMed]
- Fatimi, A.; Tassin, J.-F.; Turczyn, R.; Axelos, M.A.; Weiss, P. Gelation studies of a cellulose-based biohydrogel: The influence of pH, temperature and sterilization. Acta Biomater. 2009, 5, 3423–3432. [Google Scholar] [CrossRef] [PubMed]
- Fatimi, A.; Tassin, J.-F.; Bosco, J.; Deterre, R.; Axelos, M.A.V.; Weiss, P. Injection of calcium phosphate pastes: Prediction of injection force and comparison with experiments. J. Mater. Sci. Mater. Med. 2012, 23, 1593–1603. [Google Scholar] [CrossRef] [PubMed]
- Sen, K.S.; Campos, D.F.D.; Köpf, M.; Blaeser, A.; Fischer, H. The Effect of Addition of Calcium Phosphate Particles to Hydrogel-Based Composite Materials on Stiffness and Differentiation of Mesenchymal Stromal Cells toward Osteogenesis. Adv. Health Mater. 2018, 7, e1800343. [Google Scholar] [CrossRef]
- Svarca, A.; Grava, A.; Dubnika, A.; Ramata-Stunda, A.; Narnickis, R.; Aunina, K.; Rieksta, E.; Boroduskis, M.; Jurgelane, I.; Locs, J.; et al. Calcium Phosphate/Hyaluronic Acid Composite Hydrogels for Local Antiosteoporotic Drug Delivery. Front. Bioeng. Biotechnol. 2022, 10, 917765. [Google Scholar] [CrossRef] [PubMed]
- Soliman, T.; Ali, Z.; Zayed, M.; Sabry, D.; AbuBakr, N. Assessing the bone-healing potential of bone marrow mesenchymal stem cells in jawbone osteoporosis in albino rats. Dent. Med. Probl. 2022, 59, 75–83. [Google Scholar] [CrossRef] [PubMed]
- Ye, Y.; Zhong, H.; Huang, S.; Lai, W.; Huang, Y.; Sun, C.; Zhang, Y.; Zheng, S. Reactive Oxygen Species Scavenging Hydrogel Regulates Stem Cell Behavior and Promotes Bone Healing in Osteoporosis. Tissue Eng. Regen. Med. 2023, 20, 981–992. [Google Scholar] [CrossRef]
- Kim, G.; Park, Y.S.; Lee, Y.; Jin, Y.M.; Choi, D.H.; Ryu, K.-H.; Park, Y.J.; Park, K.D.; Jo, I. Tonsil-derived mesenchymal stem cell-embedded in situ crosslinkable gelatin hydrogel therapy recovers postmenopausal osteoporosis through bone regeneration. PLoS ONE 2018, 13, e0200111. [Google Scholar] [CrossRef] [PubMed]
- Shen, Z.-S.; Cui, X.; Hou, R.-X.; Li, Q.; Deng, H.-X.; Fu, J. Tough biodegradable chitosan–gelatin hydrogels via in situ precipitation for potential cartilage tissue engineering. RSC Adv. 2015, 5, 55640–55647. [Google Scholar] [CrossRef]
- Lei, Y.; Wang, Y.; Shen, J.; Cai, Z.; Zhao, C.; Chen, H.; Luo, X.; Hu, N.; Cui, W.; Huang, W. Injectable hydrogel microspheres with self-renewable hydration layers alleviate osteoarthritis. Sci. Adv. 2022, 8, eabl6449. [Google Scholar] [CrossRef] [PubMed]
- Han, Y.; Yang, J.; Zhao, W.; Wang, H.; Sun, Y.; Chen, Y.; Luo, J.; Deng, L.; Xu, X.; Cui, W.; et al. Biomimetic injectable hydrogel microspheres with enhanced lubrication and controllable drug release for the treatment of osteoarthritis. Bioact. Mater. 2021, 6, 3596–3607. [Google Scholar] [CrossRef] [PubMed]
- Rigogliuso, S.; Salamone, M.; Barbarino, E.; Barbarino, M.; Nicosia, A.; Ghersi, G. Production of Injectable Marine Collagen-Based Hydrogel for the Maintenance of Differentiated Chondrocytes in Tissue Engineering Applications. Int. J. Mol. Sci. 2020, 21, 5798. [Google Scholar] [CrossRef] [PubMed]
- Fan, W.; Yuan, L.; Li, J.; Wang, Z.; Chen, J.; Guo, C.; Mo, X.; Yan, Z. Injectable double-crosslinked hydrogels with kartogenin-conjugated polyurethane nano-particles and transforming growth factor β3 for in-situ cartilage regeneration. Mater. Sci. Eng. C 2020, 110, 110705. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Hu, P.; Liu, T.; Li, Z.; Huang, Y.; Liao, J.; Hamid, M.R.; Wen, L.; Wang, T.; Mo, C.; et al. Kartogenin hydrolysis product 4-aminobiphenyl distributes to cartilage and mediates cartilage regeneration. Theranostics 2019, 9, 7108–7121. [Google Scholar] [CrossRef] [PubMed]
- Zhu, S.; Chen, P.; Chen, Y.; Li, M.; Chen, C.; Lu, H. 3D-Printed Extracellular Matrix/Polyethylene Glycol Diacrylate Hydrogel Incorporating the Anti-inflammatory Phytomolecule Honokiol for Regeneration of Osteochondral Defects. Am. J. Sports Med. 2020, 48, 2808–2818. [Google Scholar] [CrossRef]
- Rauf, A.; Olatunde, A.; Imran, M.; Alhumaydhi, F.A.; Aljohani, A.S.M.; Khan, S.A.; Uddin, M.S.; Mitra, S.; Bin Emran, T.; Khayrullin, M.; et al. Honokiol: A review of its pharmacological potential and therapeutic insights. Phytomedicine 2021, 90, 153647. [Google Scholar] [CrossRef]
- Nemeth, C.L.; Janebodin, K.; Yuan, A.E.; Dennis, J.E.; Reyes, M.; Kim, D.-H. Enhanced Chondrogenic Differentiation of Dental Pulp Stem Cells Using Nanopatterned PEG-GelMA-HA Hydrogels. Tissue Eng. Part A 2014, 20, 2817–2829. [Google Scholar] [CrossRef]
- Thakur, A.; Jaiswal, M.K.; Peak, C.W.; Carrow, J.K.; Gentry, J.; Dolatshahi-Pirouz, A.; Gaharwar, A.K. Injectable shear-thinning nanoengineered hydrogels for stem cell delivery. Nanoscale 2016, 8, 12362–12372. [Google Scholar] [CrossRef] [PubMed]
- Sá-Lima, H.; Caridade, S.G.; Mano, J.F.; Reis, R.L. Stimuli-responsive chitosan-starch injectable hydrogels combined with encapsulated adipose-derived stromal cells for articular cartilage regeneration. Soft Matter 2010, 6, 5184–5195. [Google Scholar] [CrossRef]
- Hafezi, M.; Khorasani, S.N.; Zare, M.; Neisiany, R.E.; Davoodi, P. Advanced Hydrogels for Cartilage Tissue Engineering: Recent Progress and Future Directions. Polymers 2021, 13, 4199. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Wang, P.; Li, X.; Xu, Y.; Lu, G.; Jiang, Q.; Sun, Y.; Fan, Y.; Zhang, X. A di-self-crosslinking hyaluronan-based hydrogel combined with type I collagen to construct a biomimetic injectable cartilage-filling scaffold. Acta Biomater. 2020, 111, 197–207. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).