Adaptation and Validation of the “Support and Control in Birth” (SCIB) Tool in Postpartum Spanish Women
Abstract
1. Introduction
2. Methodology
2.1. Design and Selection
2.2. Information Sources
2.3. Statistical Analysis
3. Results
3.1. Characteristics of Participants
3.2. SCIB Scale Results
3.3. Content Validity
3.4. Psychometric Properties of the SCIB Scale
3.4.1. Factor Construct Validity
3.4.2. Criterion Validity
3.4.3. Internal Consistency
3.4.4. Temporal Stability
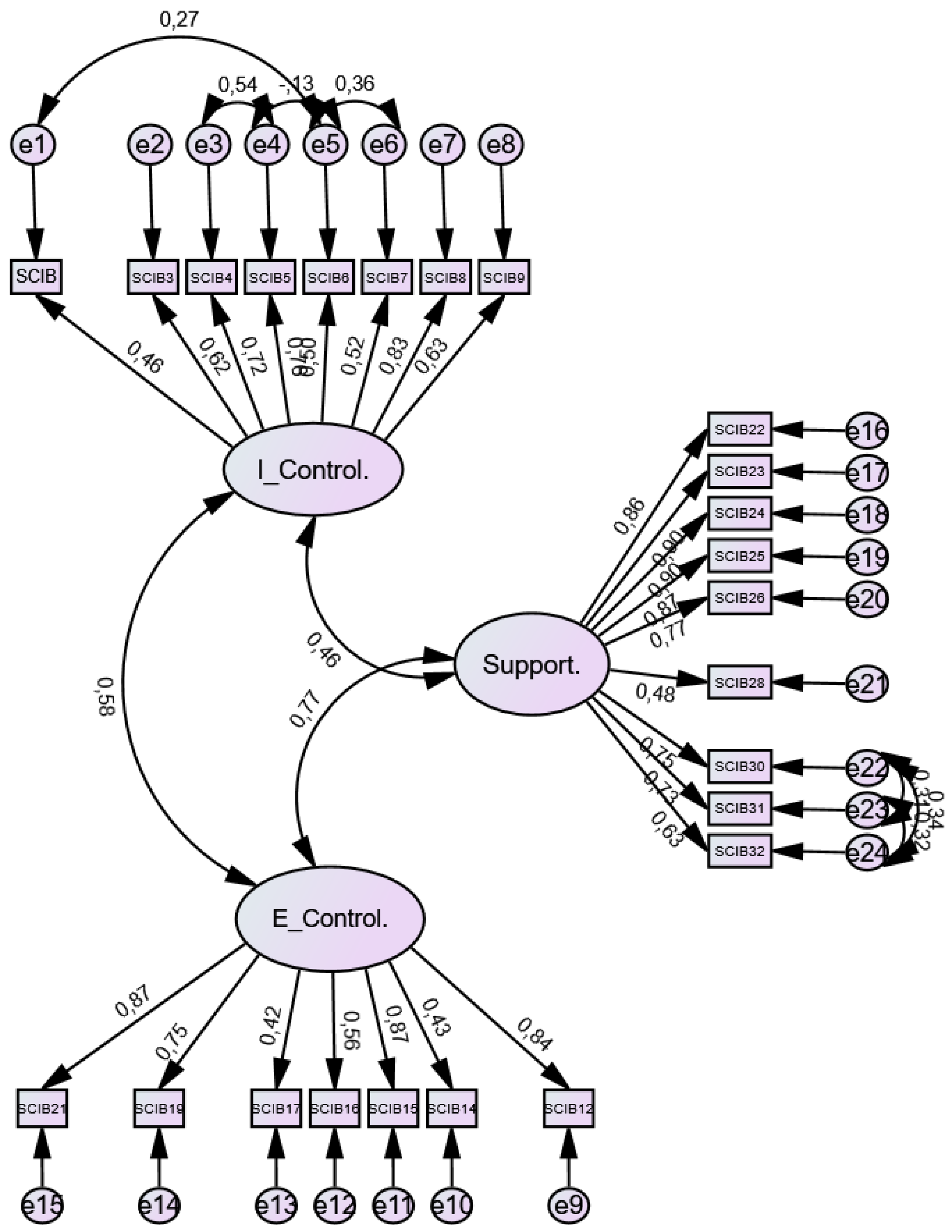
3.4.5. Confirmatory Factor Analysis
3.4.6. Reduced Version SCIB—24 Items
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chabbert, M.; Rozenberg, P.; Wendland, J. Predictors of Negative Childbirth Experiences Among French Women. J. Obstet. Gynecol. Neonatal Nurs. 2021, 50, 450–463. [Google Scholar] [CrossRef]
- Danish, S.; Ambareen, A.; Chaudhry, S.; Sana, M. Determinants of Negative Childbirth Experience and Its Influence on Mode of Delivery Decisions. Cureus 2025, 17, e92825. [Google Scholar] [CrossRef]
- Nahaee, J.; Rezaie, M.; Abdoli, E.; Mirghafourvand, M.; Ghanbari-Homaie, S.; Jafarzadeh, M. Association of childbirth experience with long–term psychological outcomes: A prospective cohort study. Reprod. Health 2024, 21, 71. [Google Scholar] [CrossRef]
- Leinweber, J.; Fontein-Kuipers, Y.; Karlsdottir, S.I.; Ekström-Bergström, A.; Nilsson, C.; Stramrood, C.; Thomson, G. Developing a woman-centered, inclusive definition of positive childbirth experiences: A discussion paper. Birth 2023, 50, 362–383. [Google Scholar] [CrossRef] [PubMed]
- Maung, T.M.; Mon, N.O.; Mehrtash, H.; Bonsaffoh, K.A.; Vogel, J.P.; Aderoba, A.K.; Irinyenikan, T.A.; Balde, M.D.; Pattanittum, P.; Tuncalp, Ö.; et al. Women’s experiences of mistreatment during childbirth and their satisfaction with care: Findings from a multicountry community-based study in four countries. BMJ Glob. Health 2022, 5, e003688. [Google Scholar] [CrossRef]
- McKelvin, G.; Thomson, G.; Downe, S. The childbirth experience: A systematic review of predictors and outcomes. Women Birth 2021, 34, 407–416. [Google Scholar] [CrossRef]
- Volkert, A.; Bach, L.; Hagenbeck, C.; Kössendrup, J.; Oberröhrmann, C.; Okumu, M.-R.; Scholten, N. Obstetric interventions’ effects on the birthing experience. BMC Pregnancy Childbirth 2024, 24, 508. [Google Scholar] [CrossRef] [PubMed]
- Konieczka, J.; Tomczyk, K.; Wilczak, M.; Chmaj-Wierzchowska, K. Factors Affecting Women’s Assessment and Satisfaction with Their Childbirth. Medicina 2024, 60, 86. [Google Scholar] [CrossRef]
- Chen, L.; Pan, W.; Mu, P.; Gau, M. Birth environment interventions and outcomes: A scoping review. Birth 2023, 50, 735–748. [Google Scholar] [CrossRef]
- Haines, H.M.; Hildingsson, I.; Pallant, J.F.; Rubertsson, C. The Role of Women’s Attitudinal Profiles in Satisfaction with the Quality of their Antenatal and Intrapartum Care. J. Obstet. Gynecol. Neonatal Nurs. 2013, 42, 428–441. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.-Y.; Lu, Y.-Y.; Gau, M.-L.; Liu, C.-Y. Psychometric testing of the support and control in birth scale. BMC Pregnancy Childbirth 2020, 20, 293. [Google Scholar] [CrossRef]
- Bell, A.F.; Andersson, E.; Bell, A.F.; Vonderheid, S.C. The birth experience and maternal caregiving attitudes and behavior: A systematic review. Sex. Reprod. Healthc. 2018, 16, 67–77. [Google Scholar] [CrossRef] [PubMed]
- Dahlberg, U.; Aune, I. The woman’s birth experience—The effect of interpersonal relationships and continuity of care. Midwifery 2013, 29, 407–415. [Google Scholar] [CrossRef]
- Metwally, S.M.; Shehata, N.S.; El Haleem, S.A.A. Women’s Expectations and Experiences Regarding Nursing Support during Childbirth. Evid.-Based Nurs. Res. 2019, 1, 10. [Google Scholar] [CrossRef]
- Gavine, A.; Shinwell, S.C.; Buchanan, P.; Farre, A.; Wade, A.; Lynn, F.; Marshall, J.; Cumming, S.E.; Dare, S.; McFadden, A. Support for healthy breastfeeding mothers with healthy term babies. Cochrane Database Syst. Rev. 2022, 2022, CD001141. [Google Scholar] [CrossRef]
- Martínez-Vazquez, S.; Rodríguez-Almagro, J.; Hernández-Martínez, A.; Delgado-Rodríguez, M.; Martínez-Galiano, J.M. Long-Term High Risk of Postpartum Post-Traumatic Stress Disorder (PTSD) and Associated Factors. J. Clin. Med. 2021, 10, 488. [Google Scholar] [CrossRef]
- Demirel, G.; Kaya, N.; Evcili, F. The relationship between women’s perception of support and control during childbirth on fear of birth and mother’s satisfaction. J. Obstet. Gynaecol. 2022, 42, 83–90. [Google Scholar] [CrossRef]
- Larkin, P.; Begley, C.M.; Devane, D. Women’s experiences of labour and birth: An evolutionary concept analysis. Midwifery 2009, 25, e49–e59. [Google Scholar] [CrossRef]
- Elmir, R.; Schmied, V.; Wilkes, L.; Jackson, D. Women’s perceptions and experiences of a traumatic birth: A meta-ethnography. J. Adv. Nurs. 2010, 66, 2142–2153. [Google Scholar] [CrossRef] [PubMed]
- Lewkowitz, A.K.; Allen, E.; Sakowicz, A.; Ayala, N.K.; Whelan, A.R.; Battle, C.L.; Miller, E.S. Association between potentially traumatic birthing experience and worsening postpartum depression or anxiety trajectories among participants in perinatal collaborative care model. Am. J. Obstet. Gynecol. MFM 2024, 6, 101418. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Vázquez, S.; Hernández-Martínez, A.; Rodríguez-Almagro, J.; Delgado-Rodríguez, M.; Martínez-Galiano, J.M. Relationship between perceived obstetric violence and the risk of postpartum depression: An observational study. Midwifery 2022, 108, 103297. [Google Scholar] [CrossRef]
- Ogallar, M.A.D.; Vazquez, S.M.; Martínez, A.H.; Molina, R.A.P.; Galiano, J.M.M. Prevalence and associated factors of anxiety in postpartum women. Eur. J. Midwifery 2025, 9, 28. [Google Scholar] [CrossRef]
- Diaz-Ogallar, M.A.; Hernandez-Martinez, A.; Linares-Abad, M.; Martinez-Galiano, J.M. Mother-child bond and its relationship with maternal postpartum depression. J. Reprod. Infant Psychol. 2024, 44, 535–558. [Google Scholar] [CrossRef] [PubMed]
- Wijma, K.; Wijma, B.; Zar, M. Psychometric aspects of the W-DEQ; a new questionnaire for the measurement of fear of childbirth. J. Psychosom. Obstet. Gynecol. 1998, 19, 84–97. [Google Scholar] [CrossRef]
- Hollins Martin, C.J.; Martin, C.R. Development and psychometric properties of the Birth Satisfaction Scale-Revised (BSS-R). Midwifery 2014, 30, 610–619. [Google Scholar] [CrossRef]
- Dencker, A.; Taft, C.; Bergqvist, L.; Lilja, H.; Berg, M. Childbirth experience questionnaire (CEQ): Development and evaluation of a multidimensional instrument. BMC Pregnancy Childbirth 2010, 10, 81. [Google Scholar] [CrossRef]
- Ford, E.; Ayers, S.; Wright, D.B. Measurement of Maternal Perceptions of Support and Control in Birth (SCIB). J. Womens Health 2009, 18, 245–252. [Google Scholar] [CrossRef] [PubMed]
- Inci, F.; Gokce Isbir, G.; Tanhan, F. The Turkish version of perceived support and control in birth scale. J. Psychosom. Obstet. Gynecol. 2015, 36, 103–113. [Google Scholar] [CrossRef]
- Ghanbari-Homaie, S.; Mohammad-Alizadeh-Charandabi, S.; Asghari-Jafarabadi, M.; Meedya, S.; Mohammadi, E.; Mirghafourvand, M. Persian version of the support and control in birth questionnaire among Iranian women. J. Educ. Health Promot. 2023, 12, 191. [Google Scholar] [CrossRef]
- Molgora, S.; Bonazza, F.; Carones, M.B.; Ferrazzi, E.M.; Ford, E. Measuring woman’s perception of support and control during childbirth: Psychometric proprieties of the SCIB scale in an Italian sample. Eur. J. Obstet. Gynecol. Reprod. Biol. X 2025, 27, 100424. [Google Scholar] [CrossRef] [PubMed]
- Ramada-Rodilla, J.M.; Serra-Pujadas, C.; Delclós-Clanchet, G.L. Cross-cultural adaptation and health questionnaires validation: Revision and methodological recommendations. Salud Publica Mex. 2013, 55, 57–66. [Google Scholar] [CrossRef]
- de Vet, H.C.W.; Adèr, H.J.; Terwee, C.B.; Pouwer, F. Are factor analytical techniques used appropriately in the validation of health status questionnaires? A systematic review on the quality of factor analysis of the SF-36. Qual. Life Res. 2005, 14, 1203–1218. [Google Scholar] [CrossRef]
- Soto-Balbuena, C.; Rodríguez-Muñoz, M.F.; Le, H.N. Validación de la Escala de Cribado del Trastorno de Ansiedad Generalizado (GAD-7) en mujeres embarazadas españolas. Psicothema 2021, 33, 164–170. [Google Scholar] [CrossRef] [PubMed]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A Brief Measure for Assessing Generalized Anxiety Disorder. Arch. Intern. Med. 2006, 166, 1092. [Google Scholar] [CrossRef] [PubMed]
- Romero-Gonzalez, B.; Peralta-Ramirez, M.I.; Caparros-Gonzalez, R.A.; Cambil-Ledesma, A.; Martin, C.J.H.; Martin, C.R. Spanish validation and factor structure of the Birth Satisfaction Scale-Revised (BSS-R). Midwifery 2019, 70, 31–37. [Google Scholar] [CrossRef]
- Ford, E.; Ayers, S. Stressful events and support during birth: The effect on anxiety, mood and perceived control. J. Anxiety Disord. 2009, 23, 260–268. [Google Scholar] [CrossRef]
- Lawshe, C.H. A quantitative approach to content validity. Pers. Psychol. 1975, 28, 563–575. [Google Scholar] [CrossRef]
- Davis, L.L. Instrument review: Getting the most from a panel of experts. Appl. Nurs. Res. 1992, 5, 194–197. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 6th ed.; Pearson Education Limited: Harlow, UK, 2013. [Google Scholar]
- Streiner, D.; Norman, G.R.; Cairney, J. Health Measurement Scales. In A Practical Development and Use, 5th ed.; Oxford University Press: Oxford, UK, 2015. [Google Scholar]
- Hu, L.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Koo, T.K.; Li, M.Y. A Guideline of Selecting and Reporting Intraclass Correlation Coefficients for Reliability Research. J. Chiropr. Med. 2016, 15, 155–163. [Google Scholar] [CrossRef]
- Brand, R.J.; Gartland, C.A.; Koo, G.; McMahon, J.E.; Hicks, J.M.; Al-Khayyat, R.; Jaatinen, M.M. Perceived autonomy during childbirth predicts mothers’ parental self-efficacy: A prospective cohort study. J. Health Psychol. 2025, 30, 2001–2012. [Google Scholar] [CrossRef]
- Dencker, A.; Bergqvist, L.; Berg, M.; Greenbrook, J.T.V.; Nilsson, C.; Lundgren, I. Measuring women’s experiences of decision-making and aspects of midwifery support: A confirmatory factor analysis of the revised Childbirth Experience Questionnaire. BMC Pregnancy Childbirth 2020, 20, 199. [Google Scholar] [CrossRef]
- Weng, M.-H.; Chou, H.-C.; Liaw, J.-J. Women’s sense of control during labour and birth with epidural analgesia: A qualitative descriptive study. Midwifery 2023, 116, 103496. [Google Scholar] [CrossRef] [PubMed]
- Fair, C.D.; Morrison, T.E. The relationship between prenatal control, expectations, experienced control, and birth satisfaction among primiparous women. Midwifery 2012, 28, 39–44. [Google Scholar] [CrossRef] [PubMed]
- O’Hare, J.; Fallon, A. Women’s experience of control in labour and childbirth. Br. J. Midwifery 2011, 19, 164–169. [Google Scholar] [CrossRef]
- Cook, K.; Loomis, C. The Impact of Choice and Control on Women’s Childbirth Experiences. J. Perinat. Educ. 2012, 21, 158–168. [Google Scholar] [CrossRef]
- Di Gesto, C.; Spinoni, M.; Grano, C. Measuring childbirth-related posttraumatic stress disorder: Psychometric properties of the Italian version of the City Birth Trauma Scale (City BiTS). Psychol. Trauma Theory Res. Pract. Policy 2025, 17, 341–352. [Google Scholar] [CrossRef]
- Chabbert, M.; Panagiotou, D.; Wendland, J. Predictive factors of women’s subjective perception of childbirth experience: A systematic review of the literature. J. Reprod. Infant. Psychol. 2021, 39, 43–66. [Google Scholar] [CrossRef]
- World Health Organization. WHO Recommendations: Intrapartum Care for a Positive Childbirth Experience; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Christiaens, W.; Bracke, P. Assessment of social psychological determinants of satisfaction with childbirth in a cross-national perspective. BMC Pregnancy Childbirth 2007, 7, 26. [Google Scholar] [CrossRef]
- Hidalgo-Lopezosa, P.; Rodríguez-Borrego, M.A.; Muñoz-Villanueva, M.C. Are Birth Plans Associated with Improved Maternal or Neonatal Outcomes? MCN Am. J. Matern. Child. Nurs. 2013, 38, 150–156. [Google Scholar] [CrossRef]

| Variable | Total | Variable | Total |
|---|---|---|---|
| (n) % | (n) % | ||
| Maternal age | Number of pregnancy visits | ||
| Mean (SD) | 35.2 (4.18) | <7 | 95 (31.5) |
| SCIB Scale | 7–10 | 138 (45.7) | |
| Mean (SD) | 113.86 (27.91) | >10 | 69 (22.8) |
| Internal control | 34.18 (8.68) | Satisfaction degree with pregnancy follow-up | |
| External control | 35.31 (11.82) | Not at all | 5 (1.7) |
| Support | 44.37 (12.27) | Low satisfaction | 31 (10.3) |
| Marital Status | Satisfied | 85 (28.1) | |
| Single | 53 (17.5) | Quite satisfied | 77 (25.5) |
| Married | 199 (65.9) | Highly satisfied | 104 (34.4) |
| Unmarried partner | 46 (15.2) | Worked during last pregnancy | |
| Divorced | 3 (1.0) | No | 50 (16.6) |
| Widowed | 1 (0.3) | Yes | 252 (83.4) |
| Nationality | Health issues during last pregnancy | ||
| Spanish | 292 (96.7) | No | 183 (60.6) |
| Other | 10 (3.3) | Yes | 119 (39.4) |
| Belongs to a religion | Setting where pregnancy was followed up | ||
| No | 148 (49.0) | Public | 132 (43.7) |
| Yes, but not practising | 104 (34.4) | Private | 17 (5.6) |
| Yes, and practising | 50 (16.6) | Mixed (Public mainly) | 94 (31.1) |
| Current illness | Mixed (Private mainly) | 28 (9.3) | |
| No | 241 (79.8) | Mixed (Equally) | 31 (10.3) |
| Yes | 61 (20.2) | Birth plan | |
| Type of birth | No | 157 (52.0) | |
| Vaginal | 181 (59.9) | Yes, respected | 107 (35.4) |
| Instrumental | 55 (18.2) | Yes, but not respected | 38 (12.6) |
| Elective C/S | 15 (5.0) | Epidural | |
| Emergency C/S | 51 (16.9) | No, maternal choice | 31 (10.3) |
| Current medical treatment | No, medical reason | 4 (1.3) | |
| No | 242 (80.1) | No, other reasons | 18 (6.0) |
| Yes | 60 (19.9) | Yes | 249 (82.5) |
| Family history of suicide | Non-pharmacological analgesia | ||
| No | 248 (82.1) | No | 197 (65.2) |
| Yes | 54 (17.9) | Yes | 105 (34.8) |
| Stressful event during last year | Satisfaction degree with postpartum care | ||
| No | 189 (62.6) | Not at all | 7 (2.3) |
| Yes | 113 (37.4) | Low satisfaction | 28 (9.3) |
| Any previous mental health treatment | Satisfied | 54 (17.9) | |
| No | 125 (41.4) | Quite satisfied | 80 (26.5) |
| Yes | 177 (58.6) | Highly satisfied | 133 (44.0) |
| Admission to a mental health unit | Postpartum complications | ||
| No | 298 (98.7) | No | 241 (79.8) |
| Yes | 4 (1.3) | Yes | 53 (17.5) |
| Number of pregnancies (including current) | Unsure | 8 (2.6) | |
| 1 | 157 (52.0) | Planned pregnancy | |
| 2 | 90 (29.8) | No | 29 (9.6) |
| 3 | 37 (12.3) | Yes | 273 (90.4) |
| 4 | 8 (2.6) | Pregnancy Risk | |
| 5 | 7 (2.3) | Low risk | 227 (75.2) |
| 6 | 1 (0.3) | High risk | 75 (24.8) |
| 7 | 2 (0.7) | Perineal tear | |
| Active participation during birth | No | 122 (40.4) | |
| No, by choice | 9 (3.0) | Episiotomy | 49 (16.2) |
| No, not possible | 67 (22.2) | Spontaneous tear (any degree) | 130 (43.0) |
| Yes | 226 (74.8) | Episiotomy + tear | 1 (0.3) |
| Items | Support | External Control | Internal Control |
|---|---|---|---|
| 1. The pain was too great for me to gain control over it. | 0.704 | ||
| 2. I was overcome by the pain. | 0.757 | ||
| 3. I was able to control my reactions to the pain. | 0.612 | ||
| 4. I was mentally calm. | 0.647 | ||
| 5. I was in control of my emotions. | 0.663 | ||
| 6. I felt my body was on a mission that I could not control. | 0.661 | ||
| 7. Negative feelings overwhelmed me. | 0.599 | ||
| 8. I gained control by working with my body. | 0.694 | ||
| 9. I could control the sounds I was making. | 0.577 | ||
| 10. I behaved in a way not like myself. | 0.604 | ||
| 11. I had control over when procedures happened. | 0.658 | ||
| 12. I could influence which procedures were carried out. | 0.762 | ||
| 13. I decided whether procedures were carried out or not. | 0.788 | ||
| 14. The people in the room took control. | 0.495 | ||
| 15. I had control over the decisions that were made. | 0.799 | ||
| 16. I could get up and move around as much as I wanted. | 0.461 | ||
| 17. People coming in and out of the room were beyond my control. | 0.316 | ||
| 18. I chose whether I was given information or not. | 0.634 | ||
| 19. I could decide when I received information. | 0.724 | ||
| 20. I had control over what information I was given. | 0.727 | ||
| 21. I felt I had control over the way my baby was finally born. | 0.700 | ||
| 22. The staff helped me find the energy to continue when I wanted to give up. | 0.782 | ||
| 23. The staff seemed to know instinctively what I wanted or needed. | 0.804 | ||
| 24. The staff went out of their way to try to keep me comfortable. | 0.832 | ||
| 25. The staff encouraged me to try new ways of coping. | 0.838 | ||
| 26. The staff realised the pain I was in. | 0.809 | ||
| 27. The staff encouraged me not to fight against what my body was doing. | 0.733 | ||
| 28. I felt the staff had their own agenda. | 0.499 | ||
| 29. I felt like the staff tried to move things along for their own convenience. | 0.569 | ||
| 30. I was given time to ask questions. | 0.659 | ||
| 31. The staff helped me to try different positions. | 0.603 | ||
| 32. The staff stopped doing something if I asked them to stop. | 0.530 | ||
| 33. The staff dismissed things I said to them. | 0.378 | ||
| Eigenvalues | 7.12 | 6.36 | 5.15 |
| Rotated variance (%) | 21.60 | 19.28 | 15.61 |
| Unrotated variance (%) | 40.62 | 10.35 | 5.51 |
| Cumulative variance (%) | 56.49 | ||
| Cronbach’s alpha | 0.88 | 0.92 | 0.93 |
| Cronbach’s alpha SCIB | 0.951 | ||
| Items | Internal Control | External Control | Support | SCIB | ||||
|---|---|---|---|---|---|---|---|---|
| Mean (SD) | p Value | Mean (SD) | p Value | Mean (SD) | p Value | Mean (SD) | p Value | |
| Parity | 0.855 | 0.040 | 0.509 | 0.224 | ||||
| Primiparous | 34.12 (8.97) | 34.40 (11.90) | 44.07 (12.45) | 112.59 (28.01) | ||||
| Multiparous | 34.32 (8.01) | 37.46 (11.43) | 45.09 (11.89) | 116.87 (27.61) | ||||
| Wanted pregnancy | 0.016 | 0.117 | 0.002 | 0.006 | ||||
| No | 30.48 (10.25) | 32.03 (13.18) | 37.79 (15.05) | 100.31 (36.12) | ||||
| Yes | 34.58 (8.42) | 35.66 (11.65) | 45.07 (11.76) | 115.30 (26.57) | ||||
| Stressful event last year | 0.027 | 0.010 | 0.131 | 0.014 | ||||
| No | 35.03 (8.55) | 36.66 (11.59) | 45.19 (11.46) | 116.90 (26.69) | ||||
| Yes | 32.75 (8.73) | 33.04 (11.91) | 42.99 (13.45) | 108.79 (29.27) | ||||
| Current illness | 0.691 | 0.952 | 0.776 | 0.981 | ||||
| No | 34.28 (8.86) | 35.33 (11.83) | 44.26 (12.17) | 113.88 (87.84) | ||||
| Yes | 33.78 (7.95) | 35.23 (11.91) | 44.77 (12.73) | 113.78 (28.40) | ||||
| Previous mental health treatment | 0.312 | 0.029 | 0.466 | 0.119 | ||||
| No | 34.78 (8.68) | 37.08 (11.27) | 44.98 (11.31) | 116.84 (26.30) | ||||
| Yes | 33.76 (8.68) | 34.06 (12.07) | 43.93 (12.92) | 111.75 (28.88) | ||||
| Pregnancy risk | 0.002 | <0.001 | 0.006 | <0.001 | ||||
| Low risk | 35.06 (8.15) | 36.79 (11.33) | 45.48 (11.48) | 117.32 (25.79) | ||||
| High risk | 31.53 (9.70) | 30.84 (12.25) | 41.03 (13.96) | 103.40 (31.48) | ||||
| Antenatal classes | 0.966 | 0.772 | 0.876 | 0.859 | ||||
| No | 34.14 (8.62) | 35.67 (12.69) | 44.57 (11.90) | 114.39 (28.43) | ||||
| Yes | 34.19 (8.72) | 35.20 (11.58) | 44.31 (12.41) | 113.71 (27.81) | ||||
| Onset of last labour | <0.001 | <0.001 | <0.001 | <0.001 | ||||
| Spontaneous | 36.27 (7.96) | 39.73 (10.47) | 47.85 (10.27) | 123.84 (23.67) | ||||
| Induced | 32.70 (8.86) | 32.84 (11.54) | 42.58 (13.03) | 108.11 (28.56) | ||||
| Elective C/S | 33.17 (9.34) | 24.58 (8.55) | 33.00 (10.49) | 90.75 (28.89) | ||||
| Urgent C/S | 27.40 (8.19) | 21.70 (9.02) | 34.90 (11.53) | 84.00 (22.11) | ||||
| Type of birth | <0.001 | <0.001 | <0.001 | <0.001 | ||||
| Normal | 35.93 (8.14) | 40.19 (9.76) | 48.54 (9.92) | 124.66 (22.83) | ||||
| Instrumental | 31.33 (9.16) | 28.35 (10.84) | 38.89 (13.33) | 98.56 (27.92) | ||||
| Elective C/S | 34.00 (8.66) | 25.87 (8.72) | 34.93 (11.04) | 94.80 (22.45) | ||||
| Urgent C/S | 31.12 (8.61) | 28.27 (11.56) | 38.27 (12.87) | 97.67 (27.84) | ||||
| Birth plan | 0.004 | <0.001 | <0.001 | <0.001 | ||||
| No | 34.17 (8.75) | 35.81 (11.45) | 45.08 (11.42) | 115.06 (26.74) | ||||
| Yes, and respected | 35.64 (8.21) | 38.71 (9.74) | 48.67 (8.04) | 123.02 (20.04) | ||||
| Yes, but not respected | 30.16 (8.60) | 23.68 (11.84) | 29.32 (14.20) | 83.16 (30.94) | ||||
| Active participation in the last birth | <0.001 | <0.001 | <0.001 | <0.001 | ||||
| No, by choice | 34.00 (10.09) | 33.56 (16.19) | 43.78 (13.54) | 111.33 (34.42) | ||||
| No, not possible | 28.63 (8.69) | 22.37 (8.45) | 33.06 (13.22) | 84.06 (23.36) | ||||
| Yes | 35.84 (7.94) | 39.22 (9.57) | 47.75 (9.70) | 122.80 (22.25) | ||||
| Satisfaction degree with last pregnancy care | 0.031 | 0.004 | <0.001 | <0.001 | ||||
| Not at all | 28.40 (11.78) | 26.00 (17.10) | 31.20 (20.68) | 85.60 (47.70) | ||||
| Little satisfied | 32.03 (8.39) | 32.48 (12.52) | 41.26 (12.71) | 105.77 (29.12) | ||||
| Satisfied | 32.87 (8.76) | 32.53 (11.77) | 41.26 (13.18) | 106.66 (29.06) | ||||
| Quite satisfied | 36.21 (8.22) | 36.91 (10.37) | 45.12 (9.57) | 118.23 (22.31) | ||||
| Very satisfied | 34.67 (8.61) | 37.69 (11.78) | 47.92 (11.61) | 120.29 (26.99) | ||||
| Satisfaction degree with last birth care | <0.001 | <0.001 | <0.001 | <0.001 | ||||
| Not at all | 27.71 (14.69) | 14.29 (2.36) | 15.14 (3.18) | 57.14 (18.00) | ||||
| Little satisfied | 25.96 (7.12) | 18.64 (6.66) | 24.64 (8.79) | 69.25 (18.84) | ||||
| Satisfied | 31.44 (7.74) | 31.15 (9.86) | 40.28 (9.76) | 102.87 (21.10) | ||||
| Quite satisfied | 33.88 (8.15) | 35.11 (8.71) | 45.86 (8.15) | 114.85 (19.24) | ||||
| Very satisfied | 37.55 (7.53) | 41.74 (9.70) | 50.83 (8.43) | 130.11 (19.50) | ||||
| Epidural in last birth | 0.028 | <0.001 | 0.118 | 0.003 | ||||
| No, maternal choice | 38.23 (8.22) | 42.87 (9.28) | 48.65 (10.44) | 129.74 (21.78) | ||||
| No, medical indication | 38.00 (7.79) | 44.75 (5.85) | 50.75 (7.80) | 133.50 (12.01) | ||||
| No, other reasons | 32.17 (7.02) | 32.89 (11.25) | 45.56 (9.59) | 110.81 (21.78) | ||||
| Yes | 33.76 (8.74) | 34.39 (11.83) | 43.65 (12.61) | 111.80 (28.48) | ||||
| Issues during last pregnancy | 0.036 | 0.203 | 0.443 | 0.126 | ||||
| No | 35.03 (8.35) | 36.01 (11.45) | 44.81 (11.49) | 115.85 (26.49) | ||||
| Yes | 32.88 (9.04) | 34.24 (12.36) | 43.70 (13.41) | 110.82 (29.83) | ||||
| In utero health problem | 0.139 | <0.001 | 0.031 | 0.005 | ||||
| No | 34.40 (8.70) | 35.99 (11.68) | 44.83 (11.99) | 115.22 (27.53) | ||||
| Yes | 31.72 (8.18) | 27.80 (11.06) | 39.32 (14.41) | 98.84 (28.33) | ||||
| Postpartum complications | 0.007 | 0.001 | 0.002 | <0.001 | ||||
| No | 34.80 (8.54) | 36.36 (11.50) | 45.37 (11.85) | 116.53 (26.44) | ||||
| Yes | 31.26 (8.84) | 30.40 (12.19) | 39.68 (13.22) | 101.34 (31.35) | ||||
| Neonatal admission to any care unit | 0.001 | 0.021 | 0.033 | 0.003 | ||||
| No | 34.80 (8.57) | 35.92 (11.72) | 44.95 (12.05) | 115.67 (27.40) | ||||
| Yes | 30.03 (8.38) | 31.23 (11.89) | 40.46 (13.18) | 101.72 (28.66) | ||||
| Stillbirth | 0.959 | 0.784 | 0.212 | 0.496 | ||||
| No | 34.19 (8.70) | 35.34 (11.85) | 44.50 (12.19) | 114.02 (106.17) | ||||
| Yes | 34.00 (8.63) | 34.00 (11.24) | 38.17 (15.85) | 106.17 (33.69) | ||||
| Variable | BSS-R | GAD-7 | p-Value |
|---|---|---|---|
| Internal control | 0.62 | −0.32 | <0.001 |
| External control | 0.73 | −0.28 | <0.001 |
| Support | 0.73 | −0.19 | <0.001 |
| SCIB Total | 0.82 | −0.30 | <0.001 |
| Indicators | Reference Criteria | Original Model Estimated Values | Estimated Values After Correlating Errors |
|---|---|---|---|
| Absolute fit indices | |||
| Chi-squared | >0.05 | <0.05 | <0.05 |
| Chi-Squared/df | <3 | 4.62 | 2.36 |
| Root mean squared error of approximation (RMSEA) | <0.08 | 0.11 | 0.07 |
| Incremental fit indices | |||
| Tucker–Lewis Index (TLI) | >0.90 | 0.75 | 0.91 |
| Comparative fit index (CFI) | >0.90 | 0.77 | 0.92 |
| Normed Fit Index (NFI) | >0.90 | 0.72 | 0.86 |
| Parsimonious fit indices | |||
| Parsimony ratio (PRATIO) | >0.90 | 0.93 | 0.90 |
| Comparative Fixed Parsimony Index (PCFI) | >0.80 | 0.71 | 0.83 |
| Parsimony Normed fit Index (PNFI) | >0.80 | 0.67 | 0.78 |
| Akaike Information Criterion (AIC) | Minor value | 2413.718 | 1294.281 |
| Indicators | Reference Criteria | Original Model Estimated Values | Estimated Values After Correlating Errors |
|---|---|---|---|
| Absolute fit indices | |||
| Chi-squared | >0.05 | <0.05 | <0.05 |
| Chi-squared/df | <3 | 4.62 | 2.40 |
| Root mean squared error of approximation (RMSEA) | <0.08 | 0.11 | 0.07 |
| Incremental fit indices | |||
| Tucker–Lewis Index (TLI) | >0.90 | 0.75 | 0.92 |
| Comparative fit index (CFI) | >0.90 | 0.77 | 0.93 |
| Normed Fit Index (NFI) | >0.90 | 0.72 | 0.88 |
| Parsimonious fit indices | |||
| Parsimony ratio (PRATIO) | >0.90 | 0.93 | 0.88 |
| Comparative Fixed Parsimony Index (PCFI) | >0.80 | 0.71 | 0.81 |
| Parsimony Normed fit Index (PNFI) | >0.80 | 0.67 | 0.77 |
| Akaike Information Criterion (AIC) | Minor value | 2413.718 | 697.040 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Martínez-Vázquez, S.; Peinado-Molina, R.A.; Molina-García, L.; Hernández-Martínez, A.; Martínez-Galiano, J.M. Adaptation and Validation of the “Support and Control in Birth” (SCIB) Tool in Postpartum Spanish Women. J. Clin. Med. 2026, 15, 2495. https://doi.org/10.3390/jcm15072495
Martínez-Vázquez S, Peinado-Molina RA, Molina-García L, Hernández-Martínez A, Martínez-Galiano JM. Adaptation and Validation of the “Support and Control in Birth” (SCIB) Tool in Postpartum Spanish Women. Journal of Clinical Medicine. 2026; 15(7):2495. https://doi.org/10.3390/jcm15072495
Chicago/Turabian StyleMartínez-Vázquez, Sergio, Rocío Adriana Peinado-Molina, Leticia Molina-García, Antonio Hernández-Martínez, and Juan Miguel Martínez-Galiano. 2026. "Adaptation and Validation of the “Support and Control in Birth” (SCIB) Tool in Postpartum Spanish Women" Journal of Clinical Medicine 15, no. 7: 2495. https://doi.org/10.3390/jcm15072495
APA StyleMartínez-Vázquez, S., Peinado-Molina, R. A., Molina-García, L., Hernández-Martínez, A., & Martínez-Galiano, J. M. (2026). Adaptation and Validation of the “Support and Control in Birth” (SCIB) Tool in Postpartum Spanish Women. Journal of Clinical Medicine, 15(7), 2495. https://doi.org/10.3390/jcm15072495







