Photobiomodulation—Underlying Mechanism and Clinical Applications
Abstract
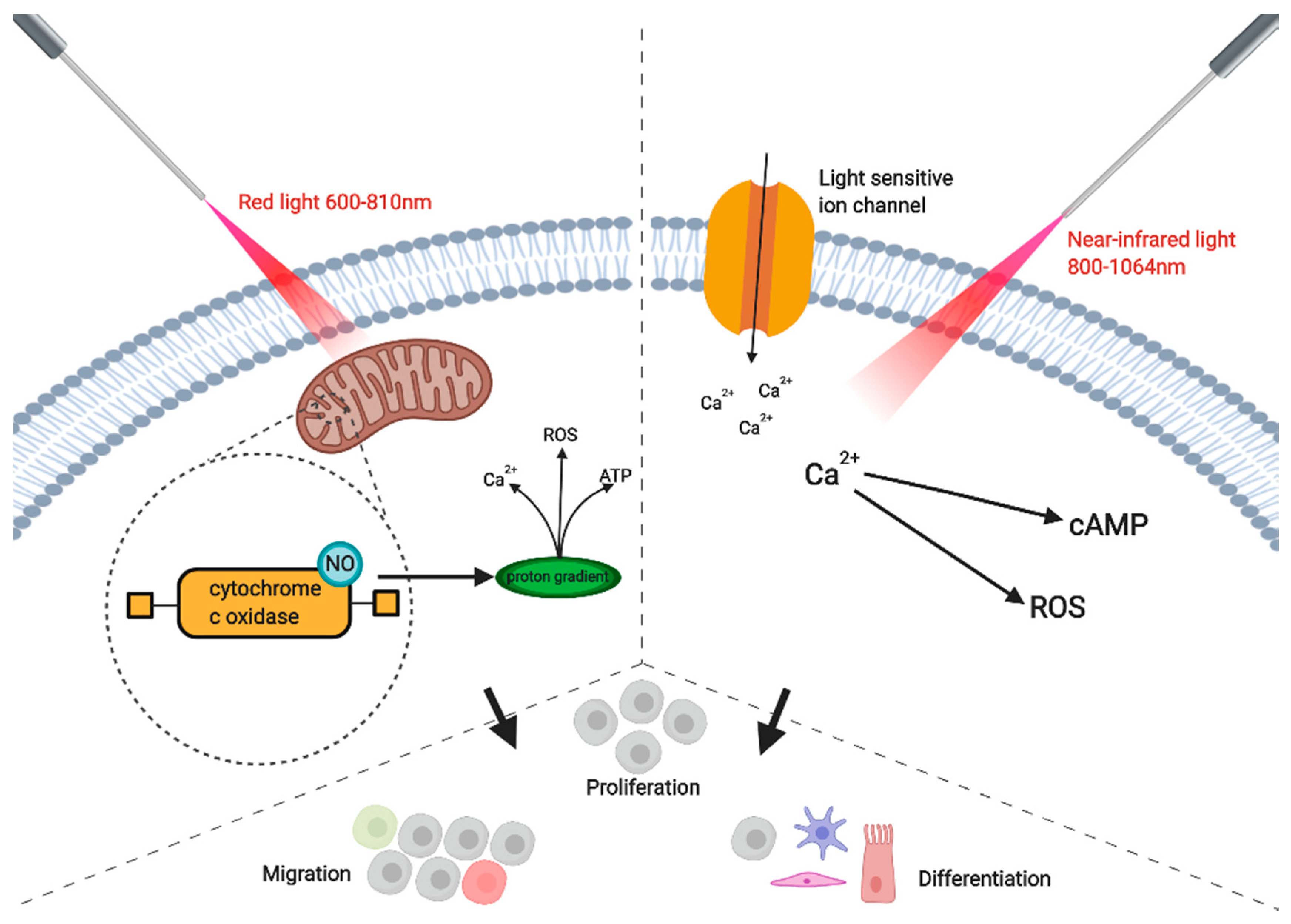
1. Introduction
2. Bio-Modulation of Human Cells and Tissues by Using Lasers
3. Cellular, Sub-Cellular, Morphological and Biochemical Modifications after Laser Treatment
4. Tissue Regeneration after Laser Treatment
5. Types of Lasers and Their Application in Medicine and Dentistry
5.1. PBM in Diabetes Treatments
5.2. PBM Application in Neural Diseases Treatments
5.3. PBM in Dermatology
5.4. PBM in Management of Secondary Complications Following Radiation
5.5. PBM in Dentistry
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- All about High Intensity Laser. BTL High Intensity Laser. Available online: https://www.high-intensity-laser.com/subpage (accessed on 1 June 2020).
- Overman, D. Treating Pain with Low vs. High-Power Lasers: What is the Difference? Rehab Management. 2019. Available online: https://www.rehabpub.com/pain-management/products/treating-pain-low-vs-high-power-lasers-difference/ (accessed on 1 June 2020).
- Astori, G.; Vignati, F.; Bardelli, S.; Tubio, M.; Gola, M.; Albertini, V.; Bambi, F.; Scali, G.; Castelli, D.; Rasini, V.; et al. “In vitro” and multicolor phenotypic characterization of cell subpopulations identified in fresh human adipose tissue stromal vascular fraction and in the derived mesenchymal stem cells. J. Transl. Med. 2007, 5, 55. [Google Scholar] [CrossRef]
- Whelan, H.T. The NASA light-emitting diode medical program—progress in space flight and terrestrial applications. In Proceedings of the AIP Conference Proceedings; AIP Publishing: College Park, MD, USA, 2003; Volume 504, pp. 37–43. [Google Scholar]
- Fernandes, A.P.; Junqueira, M.D.A.; Marques, N.C.T.; Machado, M.A.A.M.; Santos, C.F.; Oliveira, T.M.; Sakai, V.T. Effects of low-level laser therapy on stem cells from human exfoliated deciduous teeth. J. Appl. Oral Sci. 2016, 24, 332–337. [Google Scholar] [CrossRef] [PubMed]
- Saito, S.; Shimizu, N. Stimulatory effects of low-power laser irradiation on bone regeneration in midpalatal suture during expansion in the rat. Am. J. Orthod. Dentofac. Orthop. 1997, 111, 525–532. [Google Scholar] [CrossRef]
- Khadra, M.; Lyngstadaas, S.P.; Haanæs, H.R.; Mustafa, K. Effect of laser therapy on attachment, proliferation and differentiation of human osteoblast-like cells cultured on titanium implant material. Biomaterials 2005, 26, 3503–3509. [Google Scholar] [CrossRef] [PubMed]
- De Freitas, L.F.; Hamblin, M.R. Proposed Mechanisms of Photobiomodulation or Low-Level Light Therapy. IEEE J. Sel. Top. Quantum Electron. 2016, 22, 7000417. [Google Scholar] [CrossRef]
- Yadav, A.; Gupta, A. Noninvasive red and near-infrared wavelength-induced photobiomodulation: Promoting impaired cutaneous wound healing. Photodermatol. Photoimmunol. Photomed. 2017, 33, 4–13. [Google Scholar] [CrossRef]
- Chen, A.C.-H.; Arany, P.R.; Huang, Y.-Y.; Tomkinson, E.M.; Sharma, S.K.; Kharkwal, G.B.; Saleem, T.; Mooney, D.; Yull, F.E.; Blackwell, T.S.; et al. Low-Level Laser Therapy Activates NF-kB via Generation of Reactive Oxygen Species in Mouse Embryonic Fibroblasts. PLoS ONE 2011, 6, e22453. [Google Scholar] [CrossRef]
- Zamani, A.R.N.; Saberianpour, S.; Geranmayeh, M.H.; Bani, F.; Haghighi, L.; Rahbarghazi, R. Modulatory effect of photobiomodulation on stem cell epigenetic memory: A highlight on differentiation capacity. Lasers Med. Sci. 2019, 35, 299–306. [Google Scholar] [CrossRef]
- Kujawa, J.; Pasternak, K.; Zavodnik, I.; Irzmański, R.; Wróbel, D.; Bryszewska, M. The effect of near-infrared MLS laser radiation on cell membrane structure and radical generation. Lasers Med. Sci. 2014, 29, 1663–1668. [Google Scholar] [CrossRef]
- Hamblin, M.R. Photobiomodulation for traumatic brain injury and stroke. J. Neurosci. Res. 2018, 96, 731–743. [Google Scholar] [CrossRef]
- Katagiri, W.; Lee, G.; Tanushi, A.; Tsukada, K.; Choi, H.S.; Kashiwagi, S. High-throughput single-cell live imaging of photobiomodulation with multispectral near-infrared lasers in cultured T cells. J. Biomed. Opt. 2020, 25, 036003. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Tian, F.; Soni, S.S.; Gonzalez-Lima, F.; Liu, H. Interplay between up-regulation of cytochrome-c-oxidase and hemoglobin oxygenation induced by near-infrared laser. Sci. Rep. 2016, 6, 30540. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Huang, Y.Y.; Wang, Y.; Lyu, P.; Hamblin, M.R. Photobiomodulation (blue and green light) encourages osteoblastic-differentiation of human adipose-derived stem cells: Role of intracellular calcium and light-gated ion channels. Sci. Rep. 2016, 6, 33719. [Google Scholar] [CrossRef] [PubMed]
- Caruso-Davis, M.K.; Guillot, T.S.; Podichetty, V.K.; Mashtalir, N.; Dhurandhar, N.V.; Dubuisson, O.; Yu, Y.; Greenway, F.L. Efficacy of low-level laser therapy for body contouring and spot fat reduction. Obes. Surg. 2011, 21, 722–729. [Google Scholar] [CrossRef] [PubMed]
- Komarova, S.V.; Ataullakhanov, F.I.; Globus, R.K. Bioenergetics and mitochondrial transmembrane potential during differentiation of cultured osteoblasts. Am. J. Physiol. Cell Physiol. 2000, 279, C1220–C1229. [Google Scholar] [CrossRef]
- Kim, J.E.; Woo, Y.J.; Sohn, K.M.; Jeong, K.H.; Kang, H. Wnt/β-catenin and ERK pathway activation: A possible mechanism of photobiomodulation therapy with light-emitting diodes that regulate the proliferation of human outer root sheath cells. Lasers Surg. Med. 2017, 49, 940–947. [Google Scholar] [CrossRef]
- Pires Marques, E.C.; Piccolo Lopes, F.; Nascimento, I.C.; Morelli, J.; Pereira, M.V.; Machado Meiken, V.M.; Pinheiro, S.L. Photobiomodulation and photodynamic therapy for the treatment of oral mucositis in patients with cancer. Photodiagn. Photodyn. Ther. 2020, 29, 101621. [Google Scholar] [CrossRef]
- Arany, P. Photobiomodulation therapy—Easy to do, but difficult to get right. Laser Focus World 2019, 55, 22–24. [Google Scholar]
- Dos Santos, S.A.; Serra, A.J.; Stancker, T.G.; Simões, M.C.B.; Dos Santos Vieira, M.A.; Leal-Junior, E.C.; Prokic, M.; Vasconsuelo, A.; Santos, S.S.; De Carvalho, P.D.T.C. Effects of Photobiomodulation Therapy on Oxidative Stress in Muscle Injury Animal Models: A Systematic Review. Oxid. Med. Cell. Longev. 2017, 2017, 5273403. [Google Scholar] [CrossRef]
- Migliario, M.; Pittarella, P.; Fanuli, M.; Rizzi, M.; Renò, F. Laser-induced osteoblast proliferation is mediated by ROS production. Lasers Med. Sci. 2014, 29, 1463–1467. [Google Scholar] [CrossRef]
- Wang, Y.; Huang, Y.Y.; Wang, Y.; Lyu, P.; Hamblin, M.R. Photobiomodulation of human adipose-derived stem cells using 810 nm and 980 nm lasers operates via different mechanisms of action. Biochim. Biophys. Acta Gen. Subj. 2017, 1861, 441–449. [Google Scholar] [CrossRef] [PubMed]
- Mvula, B.; Abrahamse, H. Low intensity laser irradiation and growth factors influence differentiation of adipose derived stem cells into smooth muscle cells in a coculture environment over a period of 72 hours. Int. J. Photoenergy 2014, 2014, 598793. [Google Scholar] [CrossRef]
- Kim, H.; Choi, K.; Kweon, O.K.; Kim, W.H. Enhanced wound healing effect of canine adipose-derived mesenchymal stem cells with low-level laser therapy in athymic mice. J. Dermatol. Sci. 2012, 68, 149–156. [Google Scholar] [CrossRef]
- Soleimani, M.; Abbasnia, E.; Fathi, M.; Sahraei, H.; Fathi, Y.; Kaka, G. The effects of low-level laser irradiation on differentiation and proliferation of human bone marrow mesenchymal stem cells into neurons and osteoblasts-an in vitro study. Lasers Med. Sci. 2012, 27, 423–430. [Google Scholar] [CrossRef]
- Son, J.H.; Park, B.S.; Kim, I.R.; Sung, I.Y.; Cho, Y.C.; Kim, J.S.; Kim, Y.D. A novel combination treatment to stimulate bone healing and regeneration under hypoxic conditions: Photobiomodulation and melatonin. Lasers Med. Sci. 2017, 32, 533–541. [Google Scholar] [CrossRef]
- Son, J.-H.; Cho, Y.-C.; Sung, I.-Y.; Kim, I.-R.; Park, B.-S.; Kim, Y.-D. Melatonin promotes osteoblast differentiation and mineralization of MC3T3-E1 cells under hypoxic conditions through activation of PKD/p38 pathways. J. Pineal Res. 2014, 57, 385–392. [Google Scholar] [CrossRef] [PubMed]
- Ho-Shui-Ling, A.; Bolander, J.; Rustom, L.E.; Johnson, A.W.; Luyten, F.P.; Picart, C. Bone regeneration strategies: Engineered scaffolds, bioactive molecules and stem cells current stage and future perspectives. Biomaterials 2018, 180, 143–162. [Google Scholar] [CrossRef] [PubMed]
- Abramovitch-Gottlib, L.; Gross, T.; Naveh, D.; Geresh, S.; Rosenwaks, S.; Bar, I.; Vago, R. Low level laser irradiation stimulates osteogenic phenotype of mesenchymal stem cells seeded on a three-dimensional biomatrix. Lasers Med. Sci. 2005, 20, 138–146. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Yeung, K.W.K. Bone grafts and biomaterials substitutes for bone defect repair: A review. Bioact. Mater. 2017, 2, 224–247. [Google Scholar] [CrossRef]
- Leonida, A.; Paiusco, A.; Rossi, G.; Carini, F.; Baldoni, M.; Caccianiga, G. Effects of low-level laser irradiation on proliferation and osteoblastic differentiation of human mesenchymal stem cells seeded on a three-dimensional biomatrix: In vitro pilot study. Lasers Med. Sci. 2013, 28, 125–132. [Google Scholar] [CrossRef]
- Robinson, N.G. Beyond the Laboratory, into the Clinic: What Dogs with Disk Disease Have Taught Us about Photobiomodulation for Spinal Cord Injury. Photomed. Laser Surg. 2017, 35, 589–594. [Google Scholar] [CrossRef] [PubMed]
- Bennaim, M.; Porato, M.; Jarleton, A.; Hamon, M.; Carroll, J.D.; Gommeren, K.; Balligand, M. Preliminary evaluation of the effects of photobiomodulation therapy and physical rehabilitation on early postoperative recovery of dogs undergoing hemilaminectomy for treatment of thoracolumbar intervertebral disk disease. Am. J. Vet. Res. 2017, 78, 195–206. [Google Scholar] [CrossRef] [PubMed]
- De Witte, T.-M.; Fratila-Apachitei, L.E.; Zadpoor, A.A.; Peppas, N.A. Bone tissue engineering via growth factor delivery: From scaffolds to complex matrices. Regen. Biomater. 2018, 5, 197–211. [Google Scholar] [CrossRef] [PubMed]
- Kocherova, I.; Bryja, A.; Mozdziak, P.; Angelova Volponi, A.; Dyszkiewicz-Konwińska, M.; Piotrowska-Kempisty, H.; Antosik, P.; Bukowska, D.; Bruska, M.; Iżycki, D.; et al. Human Umbilical Vein Endothelial Cells (HUVECs) Co-Culture with Osteogenic Cells: From Molecular Communication to Engineering Prevascularised Bone Grafts. J. Clin. Med. 2019, 8, 1602. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Zhu, L.X.; Wang, Z.; Lou, A.J.; Yang, Y.X.; Guo, Y.; Liu, S.; Zhang, C.; Zhang, Z.; Hu, H.S.; et al. Development of a centrally vascularized tissue engineering bone graft with the unique core-shell composite structure for large femoral bone defect treatment. Biomaterials 2018, 175, 44–60. [Google Scholar] [CrossRef]
- Sobol, E.; Baum, O.; Shekhter, A.; Wachsmann-Hogiu, S.; Shnirelman, A.; Alexandrovskaya, Y.; Sadovskyy, I.; Vinokur, V. Laser-induced micropore formation and modification of cartilage structure in osteoarthritis healing. J. Biomed. Opt. 2017, 22, 091515. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Xue, T.; He, F.; Liu, Z.; Ouyang, S.; Cao, D.; Wu, J. A time-resolved proteomic analysis of transcription factors regulating adipogenesis of human adipose derived stem cells. Biochem. Biophys. Res. Commun. 2019, 511, 855–861. [Google Scholar] [CrossRef]
- Baum, O.I.; Zheltov, G.I.; Omelchenko, A.I.; Romanov, G.S.; Romanov, O.G.; Sobol, E.N. Thermomechanical effect of pulse-periodic laser radiation on cartilaginous and eye tissues. Laser Phys. 2013, 23, 085602. [Google Scholar] [CrossRef]
- Oron, U.; Maltz, L.; Tuby, H.; Sorin, V.; Czerniak, A. Enhanced Liver Regeneration Following Acute Hepatectomy by Low-Level Laser Therapy. Photomed. Laser Surg. 2010, 28, 675–678. [Google Scholar] [CrossRef]
- Rathnakar, B.; Rao, B.S.S.; Prabhu, V.; Chandra, S.; Rai, S.; Rao, A.C.K.; Sharma, M.; Gupta, P.K.; Mahato, K.K. Photo-biomodulatory response of low-power laser irradiation on burn tissue repair in mice. Lasers Med. Sci. 2016, 31, 1741–1750. [Google Scholar] [CrossRef]
- Matys, J.; Świder, K.; Flieger, R. Laser instant implant impression method: A case presentation. Dent. Med. Probl. 2017, 54, 101–106. [Google Scholar] [CrossRef]
- Milonni, P.W.; Eberly, J.H. Laser Physics; John Wiley & Sons: Hoboken, NJ, USA, 2010; ISBN 9780470387719. [Google Scholar]
- Matys, J.; Flieger, R.; Dominiak, M. Effect of diode lasers with wavelength of 445 and 980 nm on a temperature rise when uncovering implants for second stage surgery: An ex-vivo study in pigs. Adv. Clin. Exp. Med. 2017, 26, 687–693. [Google Scholar] [CrossRef] [PubMed]
- de Freitas, P.M.; Simoes, A. Lasers in Dentistry: Guide for Clinical Practice; John Wiley & Sons: Hoboken, NJ, USA, 2015; ISBN 9781118275023. [Google Scholar]
- Matys, J.; Grzech-Leśniak, K.; Flieger, R.; Dominiak, M. Assessment of an impact of a diode laser mode with wavelength of 980 nm on a temperature rise measured by means of k-02 thermocouple: Preliminary results. Dent. Med. Probl. 2016, 53, 345–351. [Google Scholar] [CrossRef]
- Gomes, F.V.; Mayer, L.; Massotti, F.P.; Baraldi, C.E.; Ponzoni, D.; Webber, J.B.B.; de Oliveira, M.G. Low-level laser therapy improves peri-implant bone formation: Resonance frequency, electron microscopy, and stereology findings in a rabbit model. Int. J. Oral Maxillofac. Surg. 2015, 44, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Mohammed, I.F.R.; Kaka, L.N.; Kaka, L.N. Promotion of Regenerative Processes in Injured Peripheral Nerve Induced by Low-Level Laser Therapy. Photomed. Laser Surg. 2007, 25, 107–111. [Google Scholar] [CrossRef]
- Grzech-Lesniak, K.; Matys, J.; Jurczyszyn, K.; Ziółkowski, P.; Dominiak, M.; Brugnera Junior, A.; Romeo, U. Histological and thermometric examination of soft tissue de-epithelialization using digitally controlled Er:YAG laser handpiece: An ex vivo study. Photomed. Laser Surg. 2018, 36, 313–319. [Google Scholar] [CrossRef]
- Matys, J.; Flieger, R.; Tenore, G.; Grzech-Leśniak, K.; Romeo, U.; Dominiak, M. Er:YAG laser, piezosurgery, and surgical drill for bone decortication during orthodontic mini-implant insertion: Primary stability analysis—An animal study. Lasers Med. Sci. 2018, 33, 489–495. [Google Scholar] [CrossRef]
- Patel, C.K.N. Continuous-Wave Laser Action on Vibrational-Rotational Transitions of CO2. Phys. Rev. 1964, 136, A1187–A1193. [Google Scholar] [CrossRef]
- Grzech-Leśniak, K.; Nowicka, J.; Pajączkowska, M.; Matys, J.; Szymonowicz, M.; Kuropka, P.; Rybak, Z.; Dobrzyński, M.; Dominiak, M. Effects of Nd:YAG laser irradiation on the growth of Candida albicans and Streptococcus mutans: In vitro study. Lasers Med. Sci. 2018, 34, 129–137. [Google Scholar] [CrossRef]
- Matys, J.; Flieger, R.; Dominiak, M. Assessment of Temperature Rise and Time of Alveolar Ridge Splitting by Means of Er:YAG Laser, Piezosurgery, and Surgical Saw: An Ex Vivo Study. Biomed. Res. Int. 2016, 2016, 9654975. [Google Scholar] [CrossRef]
- Khadra, M.; Ronold, H.J.; Lyngstadaas, S.P.; Ellingsen, J.E.; Haanaes, H.R. Low-level laser therapy stimulates bone-implant interaction: An experimental study in rabbits. Clin. Oral Implants Res. 2004, 15, 325–332. [Google Scholar] [CrossRef] [PubMed]
- Matys, J.; Świder, K.; Grzech-Leśniak, K.; Dominiak, M.; Romeo, U. Photobiomodulation by a 635 nm Diode Laser on Peri-Implant Bone: Primary and Secondary Stability and Bone Density Analysis—A Randomized Clinical Trial. Biomed. Res. Int. 2019, 2019, 2785302. [Google Scholar] [CrossRef] [PubMed]
- AlGhamdi, K.M.; Kumar, A.; Moussa, N.A. Low-level laser therapy: A useful technique for enhancing the proliferation of various cultured cells. Lasers Med. Sci. 2012, 27, 237–249. [Google Scholar] [CrossRef] [PubMed]
- Schindl, A.; Schindl, M.; Pernerstorfer-Schön, H.; Schindl, L. Low-intensity laser therapy: A review. J. Investig. Med. 2000, 48, 312–326. [Google Scholar] [PubMed]
- Pires Oliveira, D.A.A.; de Oliveira, R.F.; Zangaro, R.A.; Soares, C.P. Evaluation of Low-Level Laser Therapy of Osteoblastic Cells. Photomed. Laser Surg. 2008, 26, 401–404. [Google Scholar] [CrossRef]
- Amid, R.; Kadkhodazadeh, M.; Ahsaie, M.G.; Hakakzadeh, A. Effect of low level laser therapy on proliferation and differentiation of the cells contributing in bone regeneration. J. Lasers Med. Sci. 2014, 5, 163–170. [Google Scholar] [PubMed]
- Maluf, A.P.; Maluf, R.P.; Da Rocha Brito, C.; França, F.M.G.; De Brito, R.B. Mechanical evaluation of the influence of low-level laser therapy in secondary stability of implants in mice shinbones. Lasers Med. Sci. 2010, 25, 693–698. [Google Scholar] [CrossRef]
- Stein, A.; Benayahu, D.; Maltz, L.; Oron, U. Low-Level Laser Irradiation Promotes Proliferation and Differentiation of Human Osteoblasts in Vitro. Photomed. Laser Surg. 2005, 23, 161–166. [Google Scholar] [CrossRef]
- Kreisler, M.; Christoffers, A.B.; Al-Haj, H.; Willershausen, B.; d’Hoedt, B. Low level 809-nm diode laser-induced in vitro stimulation of the proliferation of human gingival fibroblasts. Lasers Surg. Med. 2002, 30, 365–369. [Google Scholar] [CrossRef]
- Khadra, M.; Kasem, N.; Lyngstadaas, S.P.; Haanaes, H.R.; Mustafa, K. Laser therapy accelerates initial attachment and subsequent behaviour of human oral fibroblasts cultured on titanium implant material. A scanning electron microscopic and histomorphometric analysis. Clin. Oral Implants Res. 2005, 16, 168–175. [Google Scholar] [CrossRef]
- Almeida-Lopes, L.; Rigau, J.; Amaro Zângaro, R.; Guidugli-Neto, J.; Marques Jaeger, M.M. Comparison of the low level laser therapy effects on cultured human gingival fibroblasts proliferation using different irradiance and same fluence. Lasers Surg. Med. 2001, 29, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Rani, P.K.; Raman, R.; Agarwal, S.; Paul, P.G.; Uthra, S.; Margabandhu, G.; Senthilkumar, D.; Kumaramanickavel, G.; Sharma, T. Diabetic retinopathy screening model for rural population: Awareness and screening methodology. Rural Remote Health 2005, 5, 350. [Google Scholar] [PubMed]
- Grzech-Leśniak, K.; Sculean, A.; Gašpirc, B. Laser reduction of specific microorganisms in the periodontal pocket using Er:YAG and Nd:YAG lasers: A randomized controlled clinical study. Lasers Med. Sci. 2018, 33, 1461–1470. [Google Scholar] [CrossRef] [PubMed]
- Grzech-Leśniak, K.; Gaspirc, B.; Sculean, A. Clinical and microbiological effects of multiple applications of antibacterial photodynamic therapy in periodontal maintenance patients. A randomized controlled clinical study. Photodiagn. Photodyn. Ther. 2019, 27, 44–50. [Google Scholar] [CrossRef]
- Grzech-Leśniak, K.; Matys, J.; Dominiak, M. Comparison of the clinical and microbiological effects of antibiotic therapy in periodontal pockets following laser treatment: An in vivo study. Adv. Clin. Exp. Med. 2018, 27, 1263–1270. [Google Scholar] [CrossRef]
- Shibli, J.A. Is Laser the Best Choice for the Treatment of Peri-Implantitis? Photomed. Laser Surg. 2018, 36, 569–570. [Google Scholar] [CrossRef]
- Makela, A. Why the Same Laser Protocols can have Different Clinical Results in the Treatment of Diabetes. Lasers Med. Sci. 2007, 23, 71–116. [Google Scholar]
- Bodnar, P.M.; Peshko, A.O.; Prystupiuk, O.M.; Voronko, A.A.; Kyriienko, D.V.; Mykhal’chyshyn, H.P.; Naumova, M.I. Laser therapy in diabetes mellitus. Likars’ka Sprav. 1999, 6, 125–128. [Google Scholar]
- Zhang, J.; Xing, D.; Gao, X. Low-power laser irradiation activates Src tyrosine kinase through reactive oxygen species-mediated signaling pathway. J. Cell. Physiol. 2008, 217, 518–528. [Google Scholar] [CrossRef]
- Azbel’, D.I.; Egorushkina, N.V.; Kuznetsova, I.I.; Ratushniak, A.S.; Shergin, S.M.; Shurgaia, A.M.; Shtark, M.B. The effect of the blood serum from patients subjected to intravenous laser therapy on the parameters of synaptic transmission. Biull. Eksp. Biol. Med. 1993, 116, 149–151. [Google Scholar]
- Naeser, M.A.; Zafonte, R.; Krengel, M.H.; Martin, P.I.; Frazier, J.; Hamblin, M.R.; Knight, J.A.; Meehan, W.P.; Baker, E.H. Significant Improvements in Cognitive Performance Post-Transcranial, Red/Near-Infrared Light-Emitting Diode Treatments in Chronic, Mild Traumatic Brain Injury: Open-Protocol Study. J. Neurotrauma 2014, 31, 1008–1017. [Google Scholar] [CrossRef]
- Huang, S.-F.; Tsai, Y.-A.; Wu, S.-B.; Wei, Y.-H.; Tsai, P.-Y.; Chuang, T.-Y. Effects of Intravascular Laser Irradiation of Blood in Mitochondria Dysfunction and Oxidative Stress in Adults with Chronic Spinal Cord Injury. Photomed. Laser Surg. 2012, 30, 579–586. [Google Scholar] [CrossRef] [PubMed]
- Yamany, A.A.; Sayed, H.M. Effect of low level laser therapy on neurovascular function of diabetic peripheral neuropathy. J. Adv. Res. 2012, 3, 21–28. [Google Scholar] [CrossRef]
- Barolet, D.; Roberge, C.J.; Auger, F.A.; Boucher, A.; Germain, L. Regulation of Skin Collagen Metabolism In Vitro Using a Pulsed 660nm LED Light Source: Clinical Correlation with a Single-Blinded Study. J. Invest. Dermatol. 2009, 129, 2751–2759. [Google Scholar] [CrossRef] [PubMed]
- Wikramanayake, T.C.; Rodriguez, R.; Choudhary, S.; Mauro, L.M.; Nouri, K.; Schachner, L.A.; Jimenez, J.J. Effects of the Lexington LaserComb on hair regrowth in the C3H/HeJ mouse model of alopecia areata. Lasers Med. Sci. 2012, 27, 431–436. [Google Scholar] [CrossRef]
- Feber, T. Management of mucositis in oral irradiation. Clin. Oncol. R. Coll. Radiol. 1996, 8, 106–111. [Google Scholar] [CrossRef]
- Ciais, G.; Namer, M.; Schneider, M.; Demard, F.; Pourreau-Schneider, N.; Martin, P.M.; Soudry, M.; Franquin, J.C.; Zattara, H. Laser therapy in the prevention and treatment of mucositis caused by anticancer chemotherapy. Bull. Cancer 1992, 79, 183–191. [Google Scholar]
- Cowen, D.; Tardieu, C.; Schubert, M.; Peterson, D.; Resbeut, M.; Faucher, C.; Franquin, J.C. Low energy Helium-Neon laser in the prevention of oral mucositis in patients undergoing bone marrow transplant: Results of a double blind randomized trial. Int. J. Radiat. Oncol. Biol. Phys. 1997, 38, 697–703. [Google Scholar] [CrossRef]
- Lalla, R.V.; Bowen, J.; Barasch, A.; Elting, L.; Epstein, J.; Keefe, D.M.; McGuire, D.B.; Migliorati, C.; Nicolatou-Galitis, O.; Peterson, D.E.; et al. MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Cancer 2014, 120, 1453–1461. [Google Scholar] [CrossRef]
- Artés-Ribas, M.; Arnabat-Dominguez, J.; Puigdollers, A. Analgesic effect of a low-level laser therapy (830 nm) in early orthodontic treatment. Lasers Med. Sci. 2013, 28, 335–341. [Google Scholar] [CrossRef]
- Genc, G.; Kocadereli, İ.; Tasar, F.; Kilinc, K.; El, S.; Sarkarati, B. Effect of low-level laser therapy (LLLT) on orthodontic tooth movement. Lasers Med. Sci. 2013, 28, 41–47. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.-J.; Kang, Y.-G.; Park, J.-H.; Kim, E.-C.; Park, Y.-G. Effects of low-intensity laser therapy on periodontal tissue remodeling during relapse and retention of orthodontically moved teeth. Lasers Med. Sci. 2013, 28, 325–333. [Google Scholar] [CrossRef] [PubMed]
- Aras, M.H.; Güngörmüş, M. The Effect of Low-Level Laser Therapy on Trismus and Facial Swelling Following Surgical Extraction of a Lower Third Molar. Photomed. Laser Surg. 2009, 27, 21–24. [Google Scholar] [CrossRef] [PubMed]
- Faria Amorim, J.C.; De Sousa, G.R.; Silveira, L.D.B.; Prates, R.A.; Pinotti, M.; Ribeiro, M.S. Clinical Study of the Gingiva Healing after Gingivectomy and Low-Level Laser Therapy. Photomed. Laser Surg. 2006, 24, 588–594. [Google Scholar] [CrossRef] [PubMed]
- Han, M.; Fang, H.; Li, Q.-L.; Cao, Y.; Xia, R.; Zhang, Z.-H. Effectiveness of Laser Therapy in the Management of Recurrent Aphthous Stomatitis: A Systematic Review. Scientifica (Cairo) 2016, 2016, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Jijin, M.J.; Rakaraddi, M.; Pai, J.; Jaishankar, H.P.; Krupashankar, R.; Kavitha, A.P.; Anjana, R.; Shobha, R. Low-level laser therapy versus 5% amlexanox: A comparison of treatment effects in a cohort of patients with minor aphthous ulcers. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2016, 121, 269–273. [Google Scholar] [CrossRef]
- Tezel, A.; Kara, C.; Balkaya, V.; Orbak, R. An Evaluation of Different Treatments for Recurrent Aphthous Stomatitis and Patient Perceptions: Nd:YAG Laser versus Medication. Photomed. Laser Surg. 2009, 27, 101–106. [Google Scholar] [CrossRef]
- Stona, P.; da Silva Viana, E.; dos Santos Pires, L.; Blessmann Weber, J.B.; Floriani Kramer, P. Recurrent Labial Herpes Simplex in Pediatric Dentistry: Low-level Laser Therapy as a Treatment Option. Int. J. Clin. Pediatr. Dent. 2014, 7, 140–143. [Google Scholar] [CrossRef]
- Bello-Silva, M.S.; de Freitas, P.M.; Aranha, A.C.C.; Lage-Marques, J.L.; Simões, A.; de Paula Eduardo, C. Low- and High-Intensity Lasers in the Treatment of Herpes Simplex Virus 1 Infection. Photomed. Laser Surg. 2010, 28, 135–139. [Google Scholar] [CrossRef]
- Merigo, E.; Rocca, J.-P.; Pinheiro, A.L.B.; Fornaini, C. Photobiomodulation Therapy in Oral Medicine: A Guide for the Practitioner with Focus on New Possible Protocols. Photobiomodul. Photomed. Laser Surg. 2019, 37, 669–680. [Google Scholar] [CrossRef]
- Gobbo, M.; Verzegnassi, F.; Ronfani, L.; Zanon, D.; Melchionda, F.; Bagattoni, S.; Majorana, A.; Bardellini, E.; Mura, R.; Piras, A.; et al. Multicenter randomized, double-blind controlled trial to evaluate the efficacy of laser therapy for the treatment of severe oral mucositis induced by chemotherapy in children: laMPO RCT. Pediatr. Blood Cancer 2018, 65, e27098. [Google Scholar] [CrossRef] [PubMed]
- Cafaro, A.; Arduino, P.G.; Massolini, G.; Romagnoli, E.; Broccoletti, R. Clinical evaluation of the efficiency of low-level laser therapy for oral lichen planus: A prospective case series. Lasers Med. Sci. 2014, 29, 185–190. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Grzech-Leśniak, K. Making Use of Lasers in Periodontal Treatment: A New Gold Standard? Photomed. Laser Surg. 2017, 35, 513–514. [Google Scholar] [CrossRef]
- Świder, K.; Dominiak, M.; Grzech-Leśniak, K.; Matys, J. Effect of Different Laser Wavelengths on Periodontopathogens in Peri-Implantitis: A Review of In Vivo Studies. Microorganisms 2019, 7, 189. [Google Scholar] [CrossRef]
- Sulka, A.; Mierzwa-Dudek, D.; Dominiak, M. 13 Years of Own Experience with the Use of Laser Biostimulation in Oral Surgery. Dent. Med. Probl. 2007, 44, 37–44. [Google Scholar]


| Culture Group | Energy Density (J/cm2) | Enhanced Proliferation and Differentiation Induced Cell Type |
|---|---|---|
| 1 | 2 | Osteoblast |
| 2 | 3 | Neural |
| 3 | 4 | Osteoblast |
| 4 | 6 | Neural |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dompe, C.; Moncrieff, L.; Matys, J.; Grzech-Leśniak, K.; Kocherova, I.; Bryja, A.; Bruska, M.; Dominiak, M.; Mozdziak, P.; Skiba, T.H.I.; et al. Photobiomodulation—Underlying Mechanism and Clinical Applications. J. Clin. Med. 2020, 9, 1724. https://doi.org/10.3390/jcm9061724
Dompe C, Moncrieff L, Matys J, Grzech-Leśniak K, Kocherova I, Bryja A, Bruska M, Dominiak M, Mozdziak P, Skiba THI, et al. Photobiomodulation—Underlying Mechanism and Clinical Applications. Journal of Clinical Medicine. 2020; 9(6):1724. https://doi.org/10.3390/jcm9061724
Chicago/Turabian StyleDompe, Claudia, Lisa Moncrieff, Jacek Matys, Kinga Grzech-Leśniak, Ievgeniia Kocherova, Artur Bryja, Małgorzata Bruska, Marzena Dominiak, Paul Mozdziak, Tarcio Hiroshi Ishimine Skiba, and et al. 2020. "Photobiomodulation—Underlying Mechanism and Clinical Applications" Journal of Clinical Medicine 9, no. 6: 1724. https://doi.org/10.3390/jcm9061724
APA StyleDompe, C., Moncrieff, L., Matys, J., Grzech-Leśniak, K., Kocherova, I., Bryja, A., Bruska, M., Dominiak, M., Mozdziak, P., Skiba, T. H. I., Shibli, J. A., Angelova Volponi, A., Kempisty, B., & Dyszkiewicz-Konwińska, M. (2020). Photobiomodulation—Underlying Mechanism and Clinical Applications. Journal of Clinical Medicine, 9(6), 1724. https://doi.org/10.3390/jcm9061724












