-
 Planetary Health Diet Adherence and Medication Use in Older Adults with Chronic Kidney Disease: A Cross-Sectional Study
Planetary Health Diet Adherence and Medication Use in Older Adults with Chronic Kidney Disease: A Cross-Sectional Study -
 Late-Onset Depression in an Aging World: A Multidimensional Perspective on Risks, Mechanisms, and Treatment
Late-Onset Depression in an Aging World: A Multidimensional Perspective on Risks, Mechanisms, and Treatment -
 Effect of Yoga Practices on Postural Stability, Fall Risk, and Psychological Wellbeing in Older Adults
Effect of Yoga Practices on Postural Stability, Fall Risk, and Psychological Wellbeing in Older Adults -
 Assessing Ageist Attitudes: Psychometric Properties of the Fraboni Scale of Ageism in a Population-Based Sample
Assessing Ageist Attitudes: Psychometric Properties of the Fraboni Scale of Ageism in a Population-Based Sample -
 Effects of a Community-Based Multi-Component Intervention on Subjective Well-Being in Older Adults: The Chofu–Digital–Choju Project in Japan
Effects of a Community-Based Multi-Component Intervention on Subjective Well-Being in Older Adults: The Chofu–Digital–Choju Project in Japan
Journal Description
Geriatrics
Geriatrics
is an international, peer-reviewed, scientific open access journal on geriatric medicine published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, and other databases.
- Journal Rank: CiteScore - Q2 (Health (Social Science))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 27.3 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Testimonials: See what our editors and authors say about Geriatrics.
- Journal Cluster of Healthcare Sciences and Services: Geriatrics, Journal of Ageing and Longevity, Healthcare, Hospitals, Hygiene, International Journal of Environmental Research and Public Health and Nursing Reports.
Impact Factor:
2.1 (2024);
5-Year Impact Factor:
2.5 (2024)
Latest Articles
Personalized Hemodialysis Approaches in Frail Older Individuals
Geriatrics 2026, 11(2), 40; https://doi.org/10.3390/geriatrics11020040 - 7 Apr 2026
Abstract
►
Show Figures
The hemodialysis population has progressively aged over the past two decades; in several settings, adults aged ≥75 years represent one of the fastest-growing populations receiving dialysis. Frailty, characterized by reduced physiological reserve and heightened vulnerability to stressors, has emerged as a critical determinant
[...] Read more.
The hemodialysis population has progressively aged over the past two decades; in several settings, adults aged ≥75 years represent one of the fastest-growing populations receiving dialysis. Frailty, characterized by reduced physiological reserve and heightened vulnerability to stressors, has emerged as a critical determinant of outcomes and is commonly assessed using validated instruments such as the Fried Frailty Phenotype or the Clinical Frailty Scale (CFS). Reported frailty prevalence in hemodialysis varies widely (approximately 20% to >80%), largely depending on the assessment instrument and the population studied, with consistently higher prevalence in older cohorts. It is consistently associated with older age, female sex, diabetes, lower serum albumin, cardiovascular disease, longer dialysis vintage, and lower physical activity. Compared with non-frail patients, frail hemodialysis patients have a substantially higher risk of death (approximately two-fold in pooled analyses). Seminal trials and large observational programs that shaped hemodialysis targets underrepresented very old, frail, and highly comorbid patients, limiting generalizability. In frail older adults with limited life expectancy and substantial comorbidity burden, standard thrice-weekly schedules, higher ultrafiltration intensity, and a uniform ‘fistula-first’ approach may increase treatment burden without clear proportional gains in patient-centered outcomes. This review examines evidence supporting individualized hemodialysis strategies in frail older adults. As the dialysis population continues to age, proficiency in goal-concordant, personalized prescribing is increasingly important for nephrologists and dialysis teams.
Full article
Open AccessProject Report
Impact of Comprehensive Geriatric Assessments on Dementia Care
by
Shazia Durrani, Minhal Mussawar and Mariam Alaverdashvili
Geriatrics 2026, 11(2), 39; https://doi.org/10.3390/geriatrics11020039 - 1 Apr 2026
Abstract
Introduction: According to the Alzheimer Society of Canada, over 770,000 people in Canada are living with dementia. This number is expected to rise to nearly 1 million people by 2030. Although the provision of team-based interprofessional assessment in gerontological care is critical for
[...] Read more.
Introduction: According to the Alzheimer Society of Canada, over 770,000 people in Canada are living with dementia. This number is expected to rise to nearly 1 million people by 2030. Although the provision of team-based interprofessional assessment in gerontological care is critical for the early detection and prevention of dementia, its planning and delivery can be a challenge. In Saskatchewan, previous assessments have identified significant gaps between actual and best practices in dealing with this medical condition. The emergence of Geriatric Services Resource Teams (GSRTs), which apply an innovative, team-based model to improve the diagnosis and care of older adults with complex health practices, can be proven beneficial in this regard. The purpose of this study is to compare the efficacy of the care provision process between a GSRT and a traditional medical care channel (i.e., primary health) with respect to dementia patients. Methods: A retrospective patient chart review was conducted by collecting data from a large Primary Care practice (n = 90) and the GSRT in Regina (n = 75). Collected data included information on patient demographics and treatment, and the diagnosis process itself. Results: While demographic characteristics between patient groups were similar, significant differences (p < 0.05) were found in the involvement of pharmacy and other healthcare professionals, prescriptions for memory loss, and in who made the diagnosis. Moreover, although the dementia diagnosis was usually made first in Primary Care, further clarification of the type of dementia, counseling of diagnosis, review of medication, and assessment of functions and social supports were better managed in the GSRT group. Discussion: The use of Geriatric Services Resource Teams is a relatively new concept in Saskatchewan. As these teams are established, initial results show that their role in complex care management has beneficial outcomes for dementia patients.
Full article
Open AccessSystematic Review
The Need for Standardized Data Collection to Improve Harmonization and Pooling of Information About Modifiable Risk Factors for Alzheimer’s Diseases in Italian Clinical Studies: A Systematic Review
by
Patrizio Allegra, Manuela Lodico, Claudia Migliazzo, Domenico Tarantino, Tommaso Piccoli, Nicola Vanacore, Giuseppe Salemi, Laura Maniscalco and Domenica Matranga
Geriatrics 2026, 11(2), 38; https://doi.org/10.3390/geriatrics11020038 - 31 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: At the international level, harmonized networks of dementia clinical studies are available, but Italian participation remains limited. This systematic review aims to define harmonization rules to facilitate the inclusion of Italian clinical studies in existing networks and to propose standardized data collection
[...] Read more.
Background/Objectives: At the international level, harmonized networks of dementia clinical studies are available, but Italian participation remains limited. This systematic review aims to define harmonization rules to facilitate the inclusion of Italian clinical studies in existing networks and to propose standardized data collection methods to enable comparison of the study results. Methods: A systematic review was conducted (January 2019–December 2024) to identify Italian clinical studies evaluating Alzheimer’s disease and other dementias as outcomes. Eight modifiable risk factors were extracted: BMI, arterial hypertension, diabetes, dietary patterns, alcohol consumption, smoking habits, depressive symptomatology, and physical activity. WHO definitions and internationally accepted criteria were used as reference standards. Variable harmonization potential was assessed using the DataSHaPER methodology and classified as complete, partial, or impossible, considering information loss across studies. Results: Of 365 records identified, 18 studies met the inclusion criteria. Obesity assessed via BMI showed the highest harmonization potential (44% complete, 33% partial), along with dietary habits measured by food frequency questionnaires (44% complete). Diabetes and physical inactivity followed (33% complete), assessed through fasting glucose or pharmacological treatment and the IPAQ, respectively. Smoking habits classified as current, former, or never smokers were reported in 28% of studies. Depression (assessed by GDS or CES-D) and hypertension (blood pressure measurement or antihypertensive treatment) showed complete harmonization in only 22% of studies. Conclusions: Italian studies show substantial limitations in the harmonization of modifiable risk factor data for Alzheimer’s disease, mainly due to heterogeneous and non-standardized data collection methods, highlighting the need for uniform research protocols.
Full article
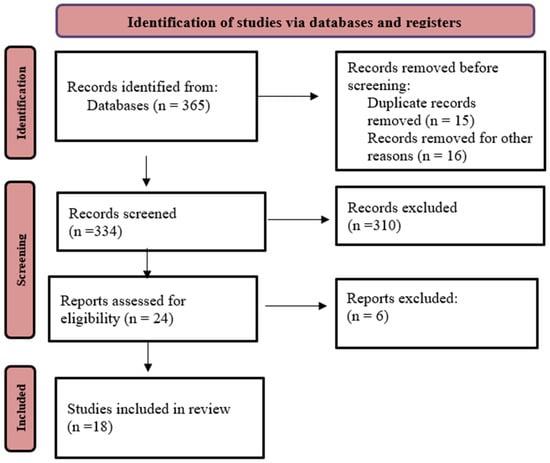
Figure 1
Open AccessCommentary
Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity
by
Adrian Bryła, Jarosław Woroń, Miłosz Miedziaszczyk, Barbara Lorkowska-Zawicka, Beata Bujak-Giżycka, Daniel Orzechowski, Paulina Połetek and Wojciech Pałys
Geriatrics 2026, 11(2), 37; https://doi.org/10.3390/geriatrics11020037 - 31 Mar 2026
Abstract
►▼
Show Figures
The aging of the population and the increasing prevalence of multimorbidity contribute to the widespread use of polypharmacotherapy, which in turn elevates the risk of adverse drug reactions and clinically significant drug–drug interactions. One of the key yet frequently underestimated issues in clinical
[...] Read more.
The aging of the population and the increasing prevalence of multimorbidity contribute to the widespread use of polypharmacotherapy, which in turn elevates the risk of adverse drug reactions and clinically significant drug–drug interactions. One of the key yet frequently underestimated issues in clinical practice is the prescribing cascade, which occurs when an adverse drug reaction is misinterpreted as a new medical condition, leading to the initiation of an additional medication. This phenomenon is particularly relevant in the older population, in whom altered pharmacokinetics and pharmacodynamics, together with reduced organ reserve, increase susceptibility to adverse drug events, including nephrotoxicity (renal impairment is used throughout the review as a clinically relevant example of organ-specific harm resulting from prescribing cascades, rather than as the sole focus of the analysis). This article discusses the mechanisms and clinical consequences of the prescribing cascade—with particular emphasis on renal function deterioration—as well as strategies for its prevention in the geriatric population. Analysis of the literature indicates that prescribing cascades remain insufficiently recognized in clinical practice, despite the availability of pharmacotherapy assessment tools such as The American Geriatrics Society (AGS) Beers Criteria and the STOPP/START criteria. Documented prescribing cascades have been shown to contribute to deterioration in health status and quality of life, an increased frequency of hospitalizations, and a greater burden on healthcare systems. Particularly concerning are cascades involving cardiovascular, neurological, and analgesic medications, which may induce or exacerbate renal injury, ultimately leading to chronic kidney disease and organ failure. Prescribing cascades represent a significant yet frequently underestimated threat to the efficacy and safety of pharmacotherapy in older adults. Their consequences may extend beyond reduced quality of life and increased treatment costs to include serious complications such as the development of renal failure. Enhancing clinicians’ awareness, conducting systematic medication reviews, and employing validated assessment tools are essential for the identification and prevention of prescribing cascades, thereby reducing the risk of renal injury and improving clinical outcomes.
Full article
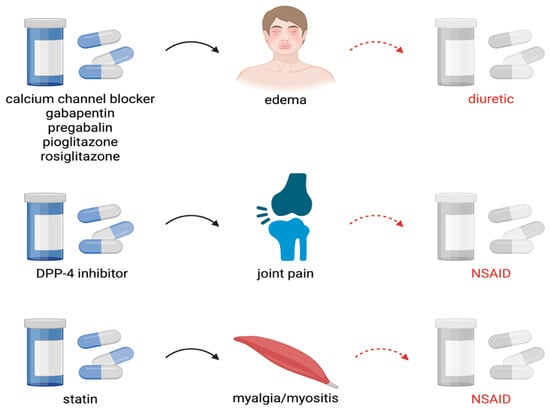
Figure 1
Open AccessArticle
Emergency Ventral Hernia Management in Older Adults: A Retrospective Cohort Study and Structured Review of the Literature
by
Ivan Tomasi, Jeremy Samuel, Eimante Raupelyte, Antonia Elizabeth Loizou, Angela Wang Yihui, Lilian Chioma Ujunwa Nwosu, Sneha Mehrotra, Mariia Druziagina, Kenneth Wing Ngai Law and Magda Sbai
Geriatrics 2026, 11(2), 36; https://doi.org/10.3390/geriatrics11020036 - 27 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: Older adults frequently present with emergency ventral hernias, a situation that carries significant physiological risks and often requires challenging clinical decisions. Despite the prevalence of these cases, there is a lack of robust evidence to inform emergency care in this demographic,
[...] Read more.
Background/Objectives: Older adults frequently present with emergency ventral hernias, a situation that carries significant physiological risks and often requires challenging clinical decisions. Despite the prevalence of these cases, there is a lack of robust evidence to inform emergency care in this demographic, as most existing research centres on short-term mortality rates and operative variables. Key aspects such as the impact of frailty and the course of recovery following surgery are insufficiently addressed in the literature. This study aimed to describe management strategies, frailty burden and postoperative outcomes in older adults presenting with emergency ventral hernias. Methods: This study retrospectively examined patients aged 65 and older who were admitted to a UK tertiary centre with emergency ventral hernias from February 2016 to July 2024. Data, including patient demographics, comorbid conditions, frailty status (as measured by the Clinical Frailty Scale), management approach, healthcare resource use, and clinical outcomes, were analysed descriptively. Additionally, a structured literature review was conducted in accordance with PRISMA guidelines to identify research on emergency ventral hernia treatment outcomes in adults aged 60 years and older. Results: A total of 67 patients met the inclusion criteria for the cohort. High rates of frailty and multiple coexisting health conditions were observed. While surgical intervention was the predominant management strategy, a subset of patients received conservative or palliative care. Greater degrees of frailty correlated with longer hospital stays and an increased need for critical care, even though six-month mortality remained comparatively low. Traditional risk assessment tools tended to overpredict mortality risk and failed to reflect the true postoperative burden or the recovery process. The systematic review yielded 7 studies, most of which documented mortality and complication rates, but few addressed frailty or provided detailed postoperative recovery data. Conclusions: The management of emergency ventral hernias in older adults is highly variable, with a significant postoperative impact that extends beyond mortality statistics. Assessing frailty appears to provide additional information that may support clinical decision-making and help anticipate recovery after surgery. Integrating frailty evaluation into emergency hernia care could enhance multidisciplinary collaboration and help ensure that treatment plans are better tailored to patient vulnerability and individual care goals.
Full article

Graphical abstract
Open AccessReview
Neoplastic Disorders and Cardiovascular Comorbidities in Geriatric Patients: A Simple Association?
by
Andreea Taisia Tiron, Marian-Vlad Lăpădat, Maria Mădălina Georgică, Lavinia Alice Bălăceanu, Ion Daniel Baboi and Ion Dina
Geriatrics 2026, 11(2), 35; https://doi.org/10.3390/geriatrics11020035 - 27 Mar 2026
Abstract
Cardiovascular disease (CVD) and cancer frequently coexist in older patients, posing significant challenges in clinical management due to overlapping risk factors and treatment-related complications. This narrative review summarizes current knowledge on the epidemiology, shared pathophysiological mechanisms and clinical impact of neoplastic comorbidities in
[...] Read more.
Cardiovascular disease (CVD) and cancer frequently coexist in older patients, posing significant challenges in clinical management due to overlapping risk factors and treatment-related complications. This narrative review summarizes current knowledge on the epidemiology, shared pathophysiological mechanisms and clinical impact of neoplastic comorbidities in older adults with cardiovascular diseases. It highlights the increased mortality, morbidity and diminished quality of life resulting from the coexistence of these conditions. The review also discusses personalized management strategies, emphasizing comprehensive geriatric and cardiac assessments, and tailoring oncologic treatments to minimize cardiotoxicity, as well as the role of prevention and rehabilitation programs. As the population ages and cancer survival improves, integrated cardio-oncology care adapted to older adults becomes increasingly essential to optimize outcomes and preserve functional status.
Full article
(This article belongs to the Section Cardiogeriatrics)
Open AccessReview
Integrating a Palliative Approach into Cardiogeriatric Decision-Making for Frail Older Adults with Heart Failure
by
Rémi Esser, Marine Larbaneix, Alejandro Mondragon, Marlène Esteban, Christine Farges, Sophie Nisse Durgeat, Marc Harboun and Olivier Maurou
Geriatrics 2026, 11(2), 34; https://doi.org/10.3390/geriatrics11020034 - 25 Mar 2026
Abstract
Background: Advanced heart failure (HF) in very old patients follows an unpredictable trajectory marked by recurrent decompensations, progressive functional decline, and high mortality. In this population, decision-making regarding goals of care and treatment proportionality is particularly complex due to multimorbidity, frailty, cognitive
[...] Read more.
Background: Advanced heart failure (HF) in very old patients follows an unpredictable trajectory marked by recurrent decompensations, progressive functional decline, and high mortality. In this population, decision-making regarding goals of care and treatment proportionality is particularly complex due to multimorbidity, frailty, cognitive vulnerability, and prognostic uncertainty, and remains insufficiently addressed by conventional disease-centred heart failure pathways. Methods: This narrative review synthesizes current evidence from heart-failure guidelines, geriatric medicine, and palliative care literature to propose a cardiogeriatric framework for end-of-life decision-making in advanced HF. Results: In older adults, functional decline and geriatric vulnerability often progress independently of cardiac parameters, limiting the relevance of prognosis-based thresholds. The palliative turning point should be understood as a multidimensional process resulting from converging cardiological, geriatric, organizational, and patient-reported signals. Therapeutic decisions should be guided by proportionality between expected benefit, treatment burden, and patient priorities. Longitudinal, iterative communication is essential to align care with evolving goals. Conclusions: A cardiogeriatric approach integrating cardiology, geriatrics, and palliative principles supports timely palliative integration, shared decision-making, and coordinated care in very old patients with advanced HF.
Full article
(This article belongs to the Section Cardiogeriatrics)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Reliability and Construct Validity of the Short Physical Performance Battery in Croatian Older Adults
by
Tatjana Njegovan Zvonarević, Ivan Jurak, Mirjana Telebuh, Ana Mojsović Ćuić, Edina Pulić, Ivna Kocijan, Želimir Bertić, Miljenko Franić, Igor Filipčić, Vlatko Brezac, Klara Turković and Lana Feher Turković
Geriatrics 2026, 11(2), 33; https://doi.org/10.3390/geriatrics11020033 - 19 Mar 2026
Abstract
►▼
Show Figures
Background: Population aging represents a major public health challenge, accompanied by an increasing prevalence of chronic diseases and age-related functional decline. Declines in lower-extremity physical function are particularly important, as they are strongly associated with mobility limitations, loss of independence, increased risk
[...] Read more.
Background: Population aging represents a major public health challenge, accompanied by an increasing prevalence of chronic diseases and age-related functional decline. Declines in lower-extremity physical function are particularly important, as they are strongly associated with mobility limitations, loss of independence, increased risk of falls, hospitalization, and mortality in older adults. Reliable and valid tools to assess physical performance are therefore essential in both clinical and research settings. The Short Physical Performance Battery (SPPB) is a widely used instrument for assessing lower-extremity physical performance in older adults and is recommended within the diagnostic algorithm of the European Working Group on Sarcopenia in Older People (EWGSOP2) for evaluating physical performance severity. However, the SPPB has not yet been psychometrically validated in the Croatian older population. This study aimed to evaluate the reliability and validity of the SPPB in Croatian older adults. Methods: This study examined the metric properties of the SPPB in a sample of 153 older adults recruited from nursing homes and community settings. Results: The SPPB demonstrated acceptable internal consistency (Cronbach’s alpha = 0.74) and good test–retest reliability (ICC = 0.893) for the total score. Convergent and construct validity were supported by significant associations with established measures of functional mobility and muscle strength. Conclusions: The Croatian version of the SPPB is a reliable and valid instrument for assessing lower-extremity physical performance in older adults. Its use is supported in clinical practice and research settings in Croatia. Further studies should examine responsiveness and predictive validity in nationally representative samples.
Full article

Figure 1
Open AccessArticle
Dose–Response Relationship Between Sleep Regularity Index and Stage-Specific Alzheimer’s Disease: Cross-Sectional Evidence from Japanese Adults
by
Yue Cao, Jaehee Lee, Jaehoon Seol, Kenji Tsunoda, Kyohei Shibuya, Jieun Yoon, Tetsuaki Arai and Tomohiro Okura
Geriatrics 2026, 11(2), 32; https://doi.org/10.3390/geriatrics11020032 - 18 Mar 2026
Abstract
Background/Objectives: Daily sleep patterns are associated with cognitive health and Alzheimer’s disease (AD). However, it remains unclear how suboptimal irregular sleep manifests in AD from the preclinical stage to dementia. This study aimed to establish the dose–response association between sleep irregularity and
[...] Read more.
Background/Objectives: Daily sleep patterns are associated with cognitive health and Alzheimer’s disease (AD). However, it remains unclear how suboptimal irregular sleep manifests in AD from the preclinical stage to dementia. This study aimed to establish the dose–response association between sleep irregularity and psychometrically defined stage-specific AD as well as executive dysfunction, among adults with subjective cognitive and sleep issues. Methods: Cross-sectional data were obtained from 532 Japanese adults (mean age = 63.9 years) between March 2023 and April 2024. Sleep irregularity was quantified using the Sleep Regularity Index (SRI) with 24/7 accelerometer data. A modified Poisson regression with cubic splines was performed to establish the dose–response association. Results: This study identified novel non-linear associations. The prevalence ratios of cognitive impairment, defined as being in the preclinical and more advanced stages of AD, significantly declined beyond a median SRI of 60. Participants within this SRI range also showed significantly lower prevalence ratios of poorer Trail Making Test B performance. All results were independent of age, sleep duration, and risk of depression. Conclusions: Maintaining balanced-to-regular daily sleep patterns might be optimal for AD progress from its preclinical stages, with a potential benchmark at SRI of 60, especially for those individuals at risk for cognitive decline and sleep disorders. Further research is needed to replicate this benchmark in diverse populations and to evaluate the effect of rigid sleep regularity on cognitive health.
Full article
(This article belongs to the Section Healthy Aging)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Effects of a Proactive Driving Transition Class on Extending Safe Driving and Preparing for Life After Driving Cessation Among Older Drivers
by
Tsutomu Sasaki, Kyohei Yamada, Takeshi Yamakita, Naoto Sakuta, Hajime Yoshida and Takeshi Tominaga
Geriatrics 2026, 11(2), 31; https://doi.org/10.3390/geriatrics11020031 - 16 Mar 2026
Abstract
Background/Objectives: Driving cessation is associated with adverse health outcomes. Proactive support that extends safe driving while preparing for life after driving cessation has been emphasized, but empirical evidence remains limited. This study examined the effects of a proactive class for older drivers on
[...] Read more.
Background/Objectives: Driving cessation is associated with adverse health outcomes. Proactive support that extends safe driving while preparing for life after driving cessation has been emphasized, but empirical evidence remains limited. This study examined the effects of a proactive class for older drivers on awareness and behavior related to driving and mobility (Study 1) and on longitudinal changes in on-road driving behavior (Study 2). Methods: The proactive class was implemented as a municipal program, including information provision, training activities, group discussions, and optional on-road driving evaluations. Study 1 included 71 older drivers who attended the class at least five times annually and completed an anonymous questionnaire assessing perceived changes in awareness and behavior. Study 2 included 29 participants who completed standardized on-road driving evaluations at baseline and at a 1-year follow-up. Paired t-tests or Wilcoxon signed-rank tests with effect sizes were applied. Results: In Study 1, participants reported increased awareness of safe driving, greater confidence in continuing to drive, heightened risk perception, initiation of health-related behaviors, trial use of public transportation, and increased healthcare utilization, particularly ophthalmology visits. In Study 2, total scores on the on-road driving skill test improved significantly at follow-up (Cohen’s dz = 0.805). No significant changes were observed in individual on-road driving skill subitems, physical function, cognitive function, or daily functioning after correction for multiple comparisons, except for a reduction in driving simulator accidents. Conclusions: Participation in a proactive, continuous driving transition support class was associated with multidimensional behavioral changes and improved on-road driving performance among older drivers, potentially contributing to safer mobility and healthier aging.
Full article
(This article belongs to the Section Healthy Aging)
►▼
Show Figures

Figure 1
Open AccessArticle
The Use of Direct Oral Anticoagulants (DOACs) in Older Adults Receiving Multidose Drug Dispensing; Interactions, Anticholinergic and Fall-Risk Increasing Drugs
by
Anette Vik Josendal, Ole Martin Sobakk, Anne Gerd Granas and Anne Katrine Eek
Geriatrics 2026, 11(2), 30; https://doi.org/10.3390/geriatrics11020030 - 6 Mar 2026
Abstract
►▼
Show Figures
Objectives: To examine the prescribing of non-vitamin K-dependent oral anticoagulants (DOACs) among multidose drug dispensing (MDD) users aged ≥65 years, and to describe associated drug–drug interactions (DDIs), concomitant use of fall-risk increasing drugs (FRIDs) and anticholinergic drugs (AC). Methods: Cross-sectional analysis of
[...] Read more.
Objectives: To examine the prescribing of non-vitamin K-dependent oral anticoagulants (DOACs) among multidose drug dispensing (MDD) users aged ≥65 years, and to describe associated drug–drug interactions (DDIs), concomitant use of fall-risk increasing drugs (FRIDs) and anticholinergic drugs (AC). Methods: Cross-sectional analysis of anonymized MDD medication lists from 87,519 patients in 2018. DDIs were identified using The Norwegian Medical Products Agency interaction tool, FRIDs were defined using the Swedish National Board of Health and Welfare list, and the CRIDECO Anticholinergic Load Scale assessed anticholinergic burden. Results: Among the 13,215 patients aged 65 and older the mean number of prescribed medications was 10.3. At least one DDI involving the prescribed DOACs was present in 26.8% of patients, whereas severe DDIs were rare (0.2%). Almost all (96.7%) used at least one FRID, and nearly half (46.8%) had an anticholinergic score ≥ 3. Conclusions: DOACs are frequently prescribed together with medications that increase the risk of falls and bleeding. These findings highlight the need for individualized risk–benefit evaluations and deprescribing or substituting high impact FRIDS and ACs when clinically appropriate.
Full article

Figure 1
Open AccessArticle
Development of a Prediction Model for Community-Dwelling Older Adults at Risk of Long-Term Care with Dementia
by
Kana Kazawa, Ken Sugimoto, Yoko Aihara and Michiko Moriyama
Geriatrics 2026, 11(2), 29; https://doi.org/10.3390/geriatrics11020029 - 5 Mar 2026
Abstract
Background: Early detection of modifiable risk factors for long-term care certification with dementia is essential. This study aimed to develop a risk-scoring tool using data from the Kihon Checklist and Questionnaire for the Late-Stage Elderly over a 2-year period to predict long-term care
[...] Read more.
Background: Early detection of modifiable risk factors for long-term care certification with dementia is essential. This study aimed to develop a risk-scoring tool using data from the Kihon Checklist and Questionnaire for the Late-Stage Elderly over a 2-year period to predict long-term care certification with dementia under Japan’s Long-Term Care Insurance system. Methods: Participants included 2041 functionally independent, community-dwelling older adults in Kure City, Japan, as of March 2021. A retrospective cohort study was conducted. Associations between KCL and LSEQ domains and certification for long-term care with dementia were examined using logistic regression. To improve practical use, a score chart was developed to predict certification for long-term care with dementia. Results: Two years after completing the Kihon Checklist and Questionnaire, 143 participants (7.0%) were certified for long-term care with dementia. Factors independently associated with certification for long-term care with to dementia included age, homebound status, cognitive decline, and locomotor decline. The prediction model, developed using these variables, showed excellent discriminatory ability, with an area under the curve of 0.790 (95% confidence interval: 0.754–0.827). Conclusions: We developed an effective predictive model for future long-term care certification with dementia using routinely collected administrative data. This tool may help healthcare providers and health planners identify older adults at increased risk of long-term care certification with dementia.
Full article
(This article belongs to the Special Issue Care, Connection and Equity: Advancing the Science of Caregiving in Aging)
►▼
Show Figures

Figure 1
Open AccessArticle
Aging Redefined: Cognitive and Physical Improvement with Positive Age Beliefs
by
Becca R. Levy and Martin D. Slade
Geriatrics 2026, 11(2), 28; https://doi.org/10.3390/geriatrics11020028 - 4 Mar 2026
Abstract
Background/Objectives: A widespread assumption exists among scientists, health care providers, and the public that later life is a time of inevitable and universal cognitive and physical decline. This assumption is likely due to considering older persons who improve to be exceptions, and
[...] Read more.
Background/Objectives: A widespread assumption exists among scientists, health care providers, and the public that later life is a time of inevitable and universal cognitive and physical decline. This assumption is likely due to considering older persons who improve to be exceptions, and the reliance on aging-health measures that do not allow for improvement. In contrast, we utilized a measure that allowed for an upward trajectory to occur. Our objective was to examine whether a meaningful number of older persons improve with this measure and, if so, to examine whether a promising modifiable culture-based variable, positive age beliefs, contributes to this improvement. Methods: Individuals 65 years and older, who participated in a nationally representative longitudinal study, had their physical health assessed by walking speed and their cognitive health assessed by a global performance measure. We calculated the percentage of the sample that showed improvement in each domain from baseline to the last measurement up to 12 years later. We also examined whether a positive-age-belief measure predicted this improvement in regression models. Results: It was found that 45.15% of persons improved in cognitive and/or physical function over this period, and positive age beliefs predicted these two types of improvement, both with and without adjusting for relevant covariates. Conclusions: Our findings underscore the need to instill or magnify the positivity of age beliefs and to redefine aging so that it includes the possibility of improvement.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
►▼
Show Figures

Figure 1
Open AccessArticle
Effects of a Community-Based Multi-Component Intervention on Subjective Well-Being in Older Adults: The Chofu–Digital–Choju Project in Japan
by
Tsubasa Nakada, Kayo Kurotani, Satoshi Seino, Takako Kozawa, Shinichi Murota, Miki Eto, Junko Shimasawa, Yumiko Shimizu, Shinobu Tsurugano, Fuminori Katsukawa, Kazunori Sakamoto, Hironori Washizaki, Yo Ishigaki, Maki Sakamoto, Keiki Takadama, Keiji Yanai, Osamu Matsuo, Chiyoko Kameue, Hitomi Suzuki and Kazunori Ohkawara
Geriatrics 2026, 11(2), 27; https://doi.org/10.3390/geriatrics11020027 - 3 Mar 2026
Abstract
►▼
Show Figures
Background: Subjective well-being (SWB) is an essential indicator of successful aging. Although social connections enhance SWB among older adults, few interventions have integrated community-based approaches with information and communication technology (ICT). This study evaluated the Chofu–Digital–Choju (CDC) project, a multi-component community intervention fostering
[...] Read more.
Background: Subjective well-being (SWB) is an essential indicator of successful aging. Although social connections enhance SWB among older adults, few interventions have integrated community-based approaches with information and communication technology (ICT). This study evaluated the Chofu–Digital–Choju (CDC) project, a multi-component community intervention fostering in-person and online social connections among community-dwelling older adults in urban Japan. Methods: This quasi-experimental study (January 2022 to March 2024) included community-dwelling older adults aged 65–84 years in Chofu City, Tokyo, Japan. The intervention consisted of online classes, community hubs as local third places, and community events. Baseline and follow-up data were collected using self-administered questionnaires. Propensity score matching (1:1) was used to reduce selection bias, and generalized estimating equations were applied to evaluate the intervention effects. The primary outcome was SWB (Cantril Ladder). The secondary outcomes included social isolation, neighborhood relationships, social participation, health literacy, psychological health, physical activity, and ICT use. Results: Among the 1599 participants who completed both surveys, 209 (13.1%) participated in at least one CDC intervention component. After propensity score matching, 195 pairs were analyzed. No significant interaction effect was observed for SWB (β = 0.08, 95% confidence interval [CI]: −0.20, 0.37; p = 0.565). However, a significant interaction effect favored the intervention group for Internet usage frequency (odds ratio = 1.53, 95% CI: 1.08, 2.16; p = 0.016). A significant borderline interaction was also observed in health literacy (β = 0.13, 95% CI: −0.00, 0.26; p = 0.056), which reached significance in covariate-adjusted sensitivity analysis (p = 0.044). Subgroup analyses revealed that community hub participants showed significant interaction effects in health literacy (p = 0.021) and a trend toward reduced depressive symptoms (p = 0.084). Conclusions: The CDC intervention did not improve SWB over 2 years but enhanced Internet use and supported health literacy and depressive symptoms, particularly among hub participants. Community-based, multi-component interventions that integrate online and in-person activities may foster digital inclusion and specific health behaviors. Although SWB did not change in this study, these proximal gains may serve as foundational steps for long-term improvement. The study protocol was preregistered in the UMIN Clinical Trials Registry (UMIN000051393; Registered on 21 June 2023).
Full article

Figure 1
Open AccessArticle
Aging Successfully Despite Limitations? Meanings and Perceptions of Aging Well Among Older Adults Living in Long-Term Care Institutions
by
Feliciano Villar, Nuria Ramón and Juan José Zacarés
Geriatrics 2026, 11(2), 26; https://doi.org/10.3390/geriatrics11020026 - 28 Feb 2026
Abstract
Background/Objectives: Dominant models of successful aging emphasize health, autonomy, and active engagement, often excluding older adults belonging to vulnerable groups, such as those living in long-term care facilities (LTCFs). This study aims to address this limitation by exploring how LTCF residents define
[...] Read more.
Background/Objectives: Dominant models of successful aging emphasize health, autonomy, and active engagement, often excluding older adults belonging to vulnerable groups, such as those living in long-term care facilities (LTCFs). This study aims to address this limitation by exploring how LTCF residents define “aging well” and by examining whether they perceive themselves as aging well according to their own criteria. Methods: A qualitative design was employed using semi-structured interviews with 30 residents aged 67–95 living in three long-term care facilities located in Barcelona, Spain. Interview transcripts were analyzed using inductive thematic analysis. Results: Five core themes emerged in the participants’ definitions of aging well: health, attitude, social ties, security, and activities. Health was the most frequently mentioned domain but was conceptualized in undemanding terms, focusing on basic autonomy and cognitive functioning. Psychological attitudes and meaningful social relationships were also key, alongside contextual factors, such as security and access to activities. Two-thirds of the participants perceived themselves as aging well, with justifications closely aligned with their personal definitions; negative self-perceptions were mainly associated with poor health, loss of autonomy, or loneliness. Conclusions: The findings suggest that, in contrast with academic definitions, LTCF residents define aging well in a broader, more context-sensitive manner, which allows them to view themselves positively despite their limitations. Person-centered care environments may play a crucial role in supporting aging well in institutional settings.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Tablet Acceptability in Older Outpatients Undergoing Cancer Chemotherapy
by
Eri Hikita, Mami Oosaki, Ayano Suzuki, Maiko Anzai, Nanako Yoshioka, Yoshiyasu Terayama and Takeo Yasu
Geriatrics 2026, 11(2), 25; https://doi.org/10.3390/geriatrics11020025 - 26 Feb 2026
Abstract
Background/Objectives: Patient acceptability of oral anticancer drugs is a critical factor that influences treatment in older outpatients receiving cancer chemotherapy and plays a central role in enhancing adherence and treatment effectiveness. Identifying older outpatients receiving cancer chemotherapy who exhibit poor tablet acceptability before
[...] Read more.
Background/Objectives: Patient acceptability of oral anticancer drugs is a critical factor that influences treatment in older outpatients receiving cancer chemotherapy and plays a central role in enhancing adherence and treatment effectiveness. Identifying older outpatients receiving cancer chemotherapy who exhibit poor tablet acceptability before initiating oral anticancer therapy and offering alternative treatment options are beneficial. Therefore, we investigated the characteristics of patients with poor tablet acceptability by focusing on the tablet size, geriatric assessment, and polypharmacy. Methods: A questionnaire survey on experiences with tablet medication was conducted among patients who received chemotherapy at the Outpatient Treatment Center of Tokyo Metropolitan Bokutoh Hospital from September 2024 to September 2025. The median values of the long diameter (12 mm) and the combined length, width, and thickness (26 mm) of the tablets reported as acceptable in the questionnaire described in Method 1 were used as cutoff values. Patients whose reported acceptable tablet dimensions were below these median values were classified as “poor tablet acceptability,” whereas those with values above the median were classified as “good tablet acceptability”. Univariate and multivariate logistic regression analysis was performed to identify characteristic factors associated with poor tablet acceptability in older outpatients receiving cancer chemotherapy, with poor tablet acceptability as the dependent variable and patient sex, body mass index, Geriatric 8 score, each item of the Oral Frailty 5-item Checklist, and polypharmacy as explanatory variables. Results: 90 patients completed the questionnaire survey. Female sex and polypharmacy were independent factors associated with poor tablet acceptability in older outpatients receiving cancer chemotherapy. In addition, subjective difficulty in chewing tended to be associated with poor tablet acceptability. Conclusions: This study suggests that assessing polypharmacy and oral function, along with early multidisciplinary intervention before and during oral anticancer therapy, particularly in females, patients taking multiple medications, and those reporting difficulty in chewing, may help maintain tablet acceptability and improve adherence.
Full article
(This article belongs to the Section Geriatric Oncology)
►▼
Show Figures

Figure 1
Open AccessArticle
Comparisons of Functional, Physical, and Mental Health Outcomes Among Young and Old Stroke Survivors
by
Molly M. Jacobs and Charles Ellis, Jr.
Geriatrics 2026, 11(2), 24; https://doi.org/10.3390/geriatrics11020024 - 26 Feb 2026
Abstract
Objective: The objective of this study was to examine how functional, mental, and physical health outcomes differ between younger (<age 50) and older (≥age 50) stroke survivors. Methods: Data from adult stroke survivors examined health-related outcomes (physical and mental health) over the past
[...] Read more.
Objective: The objective of this study was to examine how functional, mental, and physical health outcomes differ between younger (<age 50) and older (≥age 50) stroke survivors. Methods: Data from adult stroke survivors examined health-related outcomes (physical and mental health) over the past 30 days. Logistic regression models were used for binary functional outcomes, and Poisson regression models were used to estimate count outcomes for poor mental and physical health days. Results: Compared with older adults, younger stroke survivors were more likely to report difficulty concentrating or remembering (41.1% vs. 23.2%, p < 0.0001) and difficulty doing errands alone (27.11% vs. 23.67%, p = 0.00), but less likely to report difficulty walking or climbing stairs (34.3% vs. 47.6%, p < 0.0001). Additionally, younger adults with stroke reported significantly more poor mental health days (10.81 vs. 5.76, p < 0.0001) than older adults. In adjusted models, being out of work or out of the labor force was consistently associated with greater odds of functional limitations (e.g., OR for activity difficulty = 2.07, 95% CI: 1.56–2.75) and higher counts of poor mental and physical health days. Younger stroke survivors who were out of the labor force had significantly greater odds of difficulty concentrating (OR = 2.02, 95% CI: 1.17–3.48) and increased days of poor mental (IRR = 1.27, 95% CI: 1.19–1.70) and physical health (IRR = 1.26, 95% CI: 1.19–1.53). Conclusions: These findings highlight the intersection of age and employment on stroke outcomes. Younger stroke survivors face unique and disproportionate challenges in functional and mental health.
Full article
(This article belongs to the Section Geriatric Neurology)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Risk Stratification for In-Hospital Mortality in Alzheimer’s Disease Using Interpretable Regression and Explainable AI
by
Tursun Alkam, Ebrahim Tarshizi and Andrew H. Van Benschoten
Geriatrics 2026, 11(2), 23; https://doi.org/10.3390/geriatrics11020023 - 24 Feb 2026
Abstract
Background: Older adults with Alzheimer’s disease (AD) face a heightened risk of adverse hospital outcomes, including mortality. However, early identification of high-risk patients remains a challenge. While regression models provide interpretable associations, they may miss non-linear interactions that machine learning can uncover. Objective:
[...] Read more.
Background: Older adults with Alzheimer’s disease (AD) face a heightened risk of adverse hospital outcomes, including mortality. However, early identification of high-risk patients remains a challenge. While regression models provide interpretable associations, they may miss non-linear interactions that machine learning can uncover. Objective: To identify key predictors of in-hospital mortality among AD patients using both survey-weighted logistic regression and explainable machine learning. Methods: We analyzed hospitalizations among AD patients aged ≥60 in the 2017 Nationwide Inpatient Sample (NIS). The outcome was in-hospital death. Predictors included demographics, hospital variables, and 15 comorbidities. Logistic regression used survey weighting to generate nationally representative inference; XGBoost incorporated NIS discharge weights as sample weights during 5-fold hospital-grouped cross-validation and used the same weights in performance evaluation. Missing-value imputation and feature scaling were performed within the cross-validation pipelines to prevent data leakage. Model performance was assessed using AUROC, AUPRC, Brier score, and log loss. Feature importance was assessed using adjusted odds ratios and SHapley Additive exPlanations (SHAP). A sensitivity analysis excluded palliative care and DNR status and was re-evaluated under the same grouped cross-validation. Results: In the full model, logistic regression achieved AUROC 0.879 and AUPRC 0.310, while XGBoost achieved AUROC 0.887 and AUPRC 0.324. Palliative care (aOR 6.19), acute respiratory failure (aOR 5.15), DNR status (aOR 2.20), and sepsis (aOR 2.26) were the strongest logistic predictors. SHAP analysis corroborated these findings and additionally emphasized dysphagia, malnutrition, and pressure ulcers. In sensitivity analysis excluding palliative care and DNR status, logistic regression performance declined (AUROC 0.806; AUPRC 0.206), while XGBoost performed similarly (AUROC 0.811; AUPRC 0.206). SHAP corroborated the dominant signals from end-of-life documentation and acute organ failure in the full model; in the restricted model (excluding DNR and palliative care), SHAP highlighted physiologic and frailty-related features (e.g., dysphagia, malnutrition, aspiration risk) that may be more actionable when end-of-life documentation is absent. Conclusions: Combining regression with explainable machine learning enables robust mortality risk stratification in hospitalized AD patients. Restricted models excluding end-of-life indicators provide actionable risk signals when such documentation is absent, while the full model may better support resource allocation and goals-of-care workflows.
Full article
(This article belongs to the Section Geriatric Neurology)
►▼
Show Figures

Figure 1
Open AccessReview
Interdisciplinary Strategies for Improving Oral Health in Older Adults: A Comprehensive Review
by
Joanna Cheuk Yan Hui, Lindsey Lingxi Hu, Alice Kit Ying Chan and Chun Hung Chu
Geriatrics 2026, 11(1), 22; https://doi.org/10.3390/geriatrics11010022 - 19 Feb 2026
Abstract
Oral health in older adults is a critical component of overall well-being requiring integrated, interdisciplinary approaches to address its complex interplay of medical, functional, and psychosocial challenges. The aim of this is to examine strategies to enhance interdisciplinary collaboration among dental professionals, physicians,
[...] Read more.
Oral health in older adults is a critical component of overall well-being requiring integrated, interdisciplinary approaches to address its complex interplay of medical, functional, and psychosocial challenges. The aim of this is to examine strategies to enhance interdisciplinary collaboration among dental professionals, physicians, nurses, nutritionists, and caregivers to improve oral health outcomes in aging populations. Older adults commonly face dental problems such as periodontal disease which can be exacerbated by polypharmacy, systemic diseases, and barriers to accessing care. These multifaceted needs necessitate coordinated efforts across dentistry, geriatric medicine, nursing, and social support systems. Strategies of effective interdisciplinary care include: (1) Medical-dental integration, enabling physicians to screen for oral health issues during routine assessments; (2) Nursing and caregiver engagement in daily oral hygiene support and early problem identification; (3) Nutritional interventions tailored to address chewing difficulties and prevent malnutrition; (4) Social support systems to improve access to affordable care; and (5) Technology-driven solutions such as tele-dentistry to enhance communication, early detection, and care coordination. Despite these opportunities, systemic barriers persist, including fragmented healthcare systems, financial constraints, workforce shortages, cultural biases, and technological gaps. Progress requires commitment from policymakers, healthcare institutions, and health care professionals to prioritize geriatric oral health as a public health imperative. In conclusion, interdisciplinary collaboration enhances older adults’ oral-systemic health via cross-sector policies and healthcare workforce education. Implementing these strategies can mitigate oral health disparities, reduce the burden of chronic diseases, and improve quality of life for aging populations through holistic, patient-centered care.
Full article
(This article belongs to the Special Issue Oral Health Care in Older Adults)
►▼
Show Figures

Figure 1
Open AccessArticle
Temporal Prognostic Factors in Elderly Patients with Acute Heart Failure: A Cohort Study from a Spanish Emergency Department
by
Itziar Ostolaza Tazón, Héctor Alonso Valle and Pedro Muñoz Cacho
Geriatrics 2026, 11(1), 21; https://doi.org/10.3390/geriatrics11010021 - 18 Feb 2026
Abstract
Background/Objectives: Acute heart failure (AHF) is a common cause of hospitalization in older adults, associated with high morbidity and mortality. In this population, frailty, comorbidity, and functional variability significantly influence prognosis. This study evaluated short-term (30-day) and long-term (1-year) mortality predictors in elderly
[...] Read more.
Background/Objectives: Acute heart failure (AHF) is a common cause of hospitalization in older adults, associated with high morbidity and mortality. In this population, frailty, comorbidity, and functional variability significantly influence prognosis. This study evaluated short-term (30-day) and long-term (1-year) mortality predictors in elderly patients with AHF treated in the emergency department (HED), considering clinical variables, comorbidities, and precipitating factors (PFs). Materials and Methods: An observational cohort study was conducted based on a secondary analysis of older patients with AHF included in the Epidemiology of Acute Heart Failure in Emergency Departments (EAHFE) registry, treated at Hospital Universitario Marqués de Valdecilla (HUMV) between 2007 and 2022. Clinical, laboratory, and PF-related variables were collected. The primary outcome was all-cause mortality at 30 days and 1 year. Univariate and multivariate logistic regression analyses were performed. Results: A total of 548 patients were included (mean age: 80.7 years), of whom 78.6% required hospitalization, mainly in the Internal Medicine department. Mortality was 11.1% at 30 days and 29.9% at 1 year. Age, valvular heart disease, dementia, and elevated creatinine levels were independently associated with higher mortality. Hypoxemia and low-output symptoms were linked to short-term mortality, while NYHA class III and anemia were associated with long-term mortality. Among PFs, acute coronary syndrome (ACS) was related to worse short-term outcomes, whereas rapid atrial fibrillation (AF) was inversely associated with long-term mortality. Conclusions: The prognostic relevance of risk factors differs between short- and long-term outcomes in older patients with AHF. Incorporating clinical characteristics and PFs into risk stratification models may support individualized management and guide follow-up strategies tailored to the geriatric profile. This multidimensional approach is essential to improve clinical decision-making and outcomes in a highly vulnerable population.
Full article
(This article belongs to the Section Cardiogeriatrics)
►▼
Show Figures

Figure 1

Journal Menu
► ▼ Journal Menu-
- Geriatrics Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
- 10th Anniversary
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
IJERPH, Medicina, Hospitals, Healthcare, Safety, Geriatrics
The Imperative of Patient Safety and Safety Culture in Contemporary Healthcare
Topic Editors: Hana Brborović, Ognjen Brborovic, Reinhard StrametzDeadline: 8 July 2026
Topic in
Geriatrics, IJMS, Life, Sports, Neurology International, Obesities
Exercise and Human Aging: Physiological and Psychological Functions
Topic Editors: Samuel Da Silva Aguiar, Ismael Perez-SuarezDeadline: 20 September 2026
Topic in
IJMS, Cells, Biomolecules, Geriatrics, Immuno
Inflammaging: The Immunology of Aging, 2nd Edition
Topic Editors: Brianna Cyr, Juan Pablo de Rivero VaccariDeadline: 15 February 2027
Topic in
Behavioral Sciences, Brain Sciences, Geriatrics
Psychopathology and Developmental Trajectories
Topic Editors: Donatella Rita Petretto, Carmelo Masala, Stefan BogaertsDeadline: 31 March 2027

Conferences
Special Issues
Special Issue in
Geriatrics
Comprehensive Geriatric Assessment of Older Surgical Patients
Guest Editors: David Shipway, Frances RickardDeadline: 20 April 2026
Special Issue in
Geriatrics
Neurodegenerative Diseases, Physical Fitness, and Exercise Interventions in Aging
Guest Editors: José Daniel Jiménez García, Antonio Martinez-AmatDeadline: 30 April 2026
Special Issue in
Geriatrics
Healthy Ageing and Lifestyle Medicine: Current Knowledge and Future Direction (2nd Edition)
Guest Editors: Alice Masini, Massimiliano PanellaDeadline: 10 May 2026
Special Issue in
Geriatrics
Oral Health Care in Older Adults
Guest Editor: Alice Kit Ying ChanDeadline: 20 May 2026
Topical Collections
Topical Collection in
Geriatrics
Joint Arthroplasty in the Oldest People
Collection Editors: Juan F. Blanco, Carmen da Casa
Topical Collection in
Geriatrics
Ageism, the Black Sheep of the Decade of Healthy Ageing
Collection Editor: Lydia Gimenez Llort
Topical Collection in
Geriatrics
Responding to the Pandemic: Geriatric Care Models
Collection Editor: James Powers









