Contemporary and Emerging Modalities of Kidney Assistance Therapy for Patients with Kidney Dysfunction Requiring Dialysis
A special issue of Toxins (ISSN 2072-6651). This special issue belongs to the section "Uremic Toxins".
Deadline for manuscript submissions: 30 June 2026 | Viewed by 13066
Special Issue Editors
Interests: extracorporeal kidney assistance therapy; individualized dialysis; individualized vascular access
2. Medical Services, Ralph H. Johnson VA Medical Center, Charleston, SC 29401, USA
Interests: dialysis; CRRT; electrolytes; transplant
Special Issues, Collections and Topics in MDPI journals
Special Issue Information
Dear Colleagues,
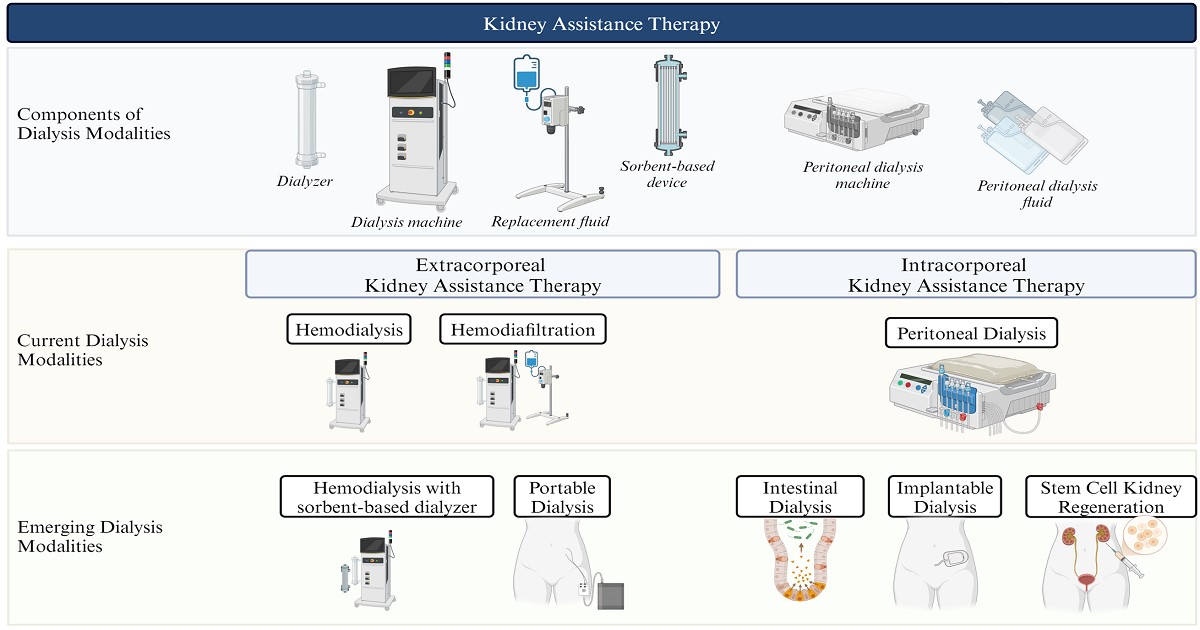
Kidney assistance therapy is the cornerstone of treatment for kidney dysfunction requiring dialysis (KDRD) and focuses on uremic toxin removal and fluid regulation. Broadly, kidney assistance therapy can be divided into two categories: extracorporeal and intracorporeal.
Extracorporeal therapy is the most prevalent form of kidney assistance with core components consisting of a dialyzer and dialysis machine. Adjunctive elements like replacement fluids or sorbent technologies may modulate its functionality. Based on the configuration of these components, extracorporeal therapy can be classified into two main modalities: hemodialysis and hemodiafiltration. Each modality provides varying levels of uremic toxin clearance and employs distinct fluid management strategies. Hemodialysis primarily relies on diffusion for solute removal, targeting small and medium-sized toxins. Hemodiafiltration combines diffusion and convection, enhancing the clearance of larger molecular weight toxins while improving fluid balance. Adjunctive technologies, such as sorbent-based devices, are tools that can optimize uremic toxin removal.
Intracorporeal therapy, currently represented by peritoneal dialysis, involves the utilization of the patient’s peritoneal membrane as a natural filter. Core components include a peritoneal dialysis machine and dialysate. The effectiveness of this modality hinges on individual peritoneal membrane characteristics, which influence solute clearance and fluid removal.
In addition to the established extracorporeal and intracorporeal kidney assistance therapies, innovations hold promise for transforming the management of kidney dysfunction by improving portability, accessibility, and patient outcomes. These innovations include portable extracorporeal kidney assistance devices, implantable intracorporeal artificial kidneys, and intestinal dialysis.
In this Toxins Special Issue, we welcome manuscripts focusing on the core and adjunctive components of extracorporeal and intracorporeal kidney assistance therapies utilized for the chronic treatment of patients with KDRD. They will explore how kidney assistance technologies differ in their ability to address uremic toxin levels and fluid imbalances, providing insights into selecting appropriate techniques for individualized care. Additionally, papers will cover emerging innovations in kidney assistance, including portable devices, intestinal dialysis, and implantable therapies, offering a glimpse into future possibilities. The goal of this Special Issue is to empower clinicians with a deeper understanding of current and emerging technologies in kidney assistance therapy, enabling them to tailor treatments that evolve alongside patients’ biological and clinical conditions.
Dr. Mariana Murea
Prof. Dr. Tibor Fülöp
Guest Editors
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the special issue website. Research articles, review articles as well as short communications are invited. For planned papers, a title and short abstract (about 250 words) can be sent to the Editorial Office for assessment.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a double-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Toxins is an international peer-reviewed open access monthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2700 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Keywords
- uremic toxin
- dialysis
- dialyzer
- filtration
- intestinal
- implantable
- portable
- sorbent
Benefits of Publishing in a Special Issue
- Ease of navigation: Grouping papers by topic helps scholars navigate broad scope journals more efficiently.
- Greater discoverability: Special Issues support the reach and impact of scientific research. Articles in Special Issues are more discoverable and cited more frequently.
- Expansion of research network: Special Issues facilitate connections among authors, fostering scientific collaborations.
- External promotion: Articles in Special Issues are often promoted through the journal's social media, increasing their visibility.
- Reprint: MDPI Books provides the opportunity to republish successful Special Issues in book format, both online and in print.
Further information on MDPI's Special Issue policies can be found here.







