Assessment of Quality of Life after Endovascular and Open Abdominal Aortic Aneurysm Repair: A Retrospective Single-Center Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Assessed Data
2.2. Quality of Life Assessment
2.3. Aortic Access in OR and Routine Follow-Up
2.4. Conduction of EVAR and Routine Follow-Up
2.5. Statistics
3. Results
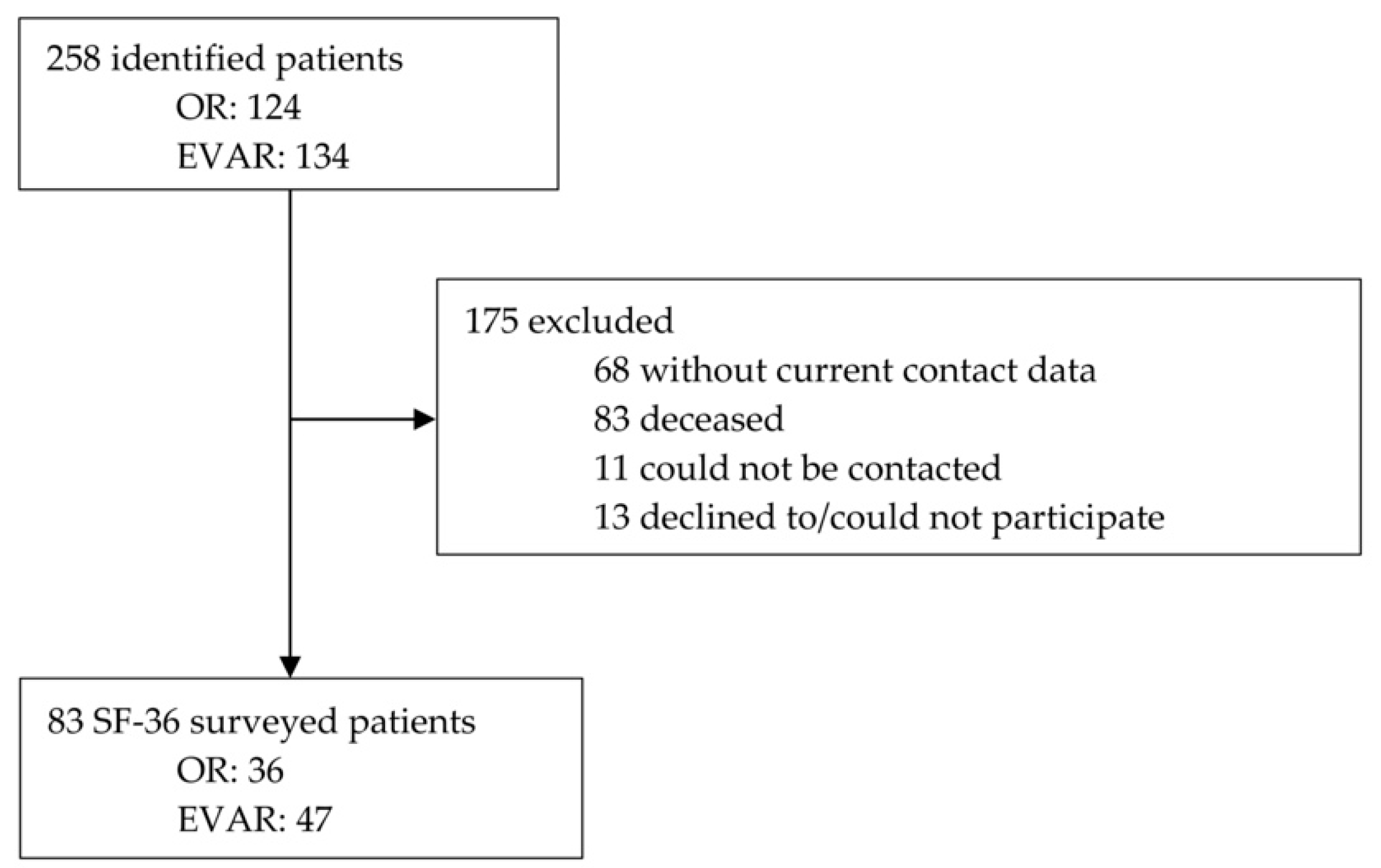
3.1. Patient Characteristics
3.2. Complications after EVAR and OR
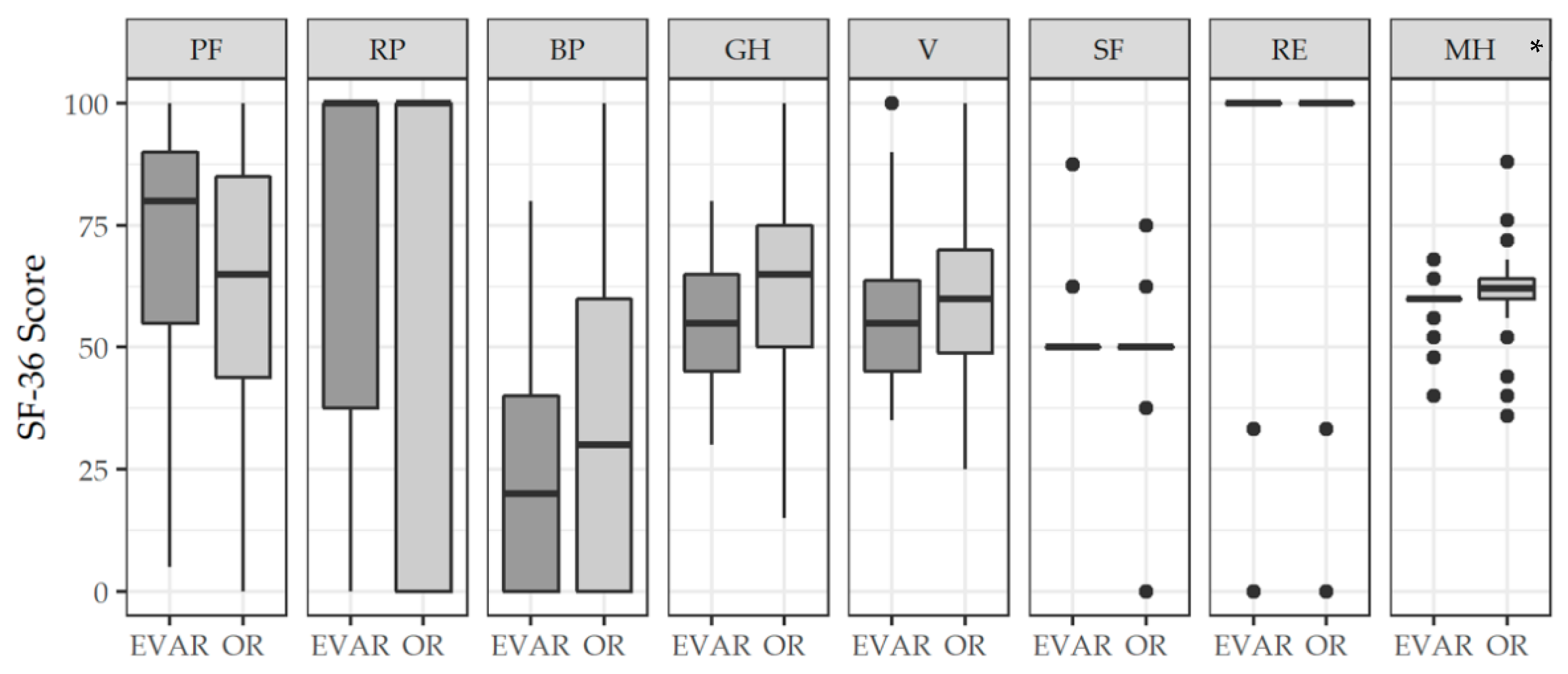
3.3. HRQoL after EVAR and OR
3.4. Effects of IH on HRQoL after OR
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. The Top 10 Causes of Death. Available online: https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death/ (accessed on 20 November 2021).
- Debus, E.S.; Behrendt, C.-A.; Gross-Fengels, W.; Kölbel, T. Aneurysmen der infrarenalen Aorta: Klinik, Diagnostik einschließlich Screening und Therapieindikationen. In Operative und Interventionelle Gefäßmedizin; Debus, E.S., Gross-Fengels, W., Eds.; Springer Reference Medizin; Springer: Berlin/Heidelberg, Germany, 2020; pp. 673–689. ISBN 978-3-662-53378-9. [Google Scholar]
- Debus, E.S.; Gross-Fengels, W.; Mahlmann, A.; Muhl, E.; Pfister, K.; Roth, S.; Stroszczynski, C.; Weiss, N.; Wilhelmi, M.; Grundmann, R.T. S3-Leitlinie zu Screening, Diagnostik, Therapie und Nachsorge des Bauchaortenaneurysmas. Gefässchirurgie 2018, 23, 402–403. [Google Scholar] [CrossRef] [Green Version]
- Debono, S.; Nash, J.; Tambyraja, A.L.; Newby, D.E.; Forsythe, R.O. Endovascular Repair for Abdominal Aortic Aneurysms. Heart 2021, 107, 1783–1789. [Google Scholar] [CrossRef]
- Antoniou, G.A.; Georgiadis, G.S.; Antoniou, S.A.; Granderath, F.A.; Giannoukas, A.D.; Lazarides, M.K. Abdominal Aortic Aneurysm and Abdominal Wall Hernia as Manifestations of a Connective Tissue Disorder. J. Vasc. Surg. 2011, 54, 1175–1181. [Google Scholar] [CrossRef] [Green Version]
- Musella, M.; Milone, F.; Chello, M.; Angelini, P.; Jovino, R. Magnetic Resonance Imaging and Abdominal Wall Hernias in Aortic Surgery. J. Am. Coll. Surg. 2001, 193, 392–395. [Google Scholar] [CrossRef]
- Takagi, H.; Sugimoto, M.; Kato, T.; Matsuno, Y.; Umemoto, T. Postoperative Incision Hernia in Patients with Abdominal Aortic Aneurysm and Aortoiliac Occlusive Disease: A Systematic Review. J. Vasc. Surg. 2007, 33, 177–181. [Google Scholar] [CrossRef] [Green Version]
- Alnassar, S.; Bawahab, M.; Abdoh, A.; Guzman, R.; Al Tuwaijiri, T.; Louridas, G. Incisional Hernia Postrepair of Abdominal Aortic Occlusive and Aneurysmal Disease: Five-Year Incidence. Vascular 2012, 20, 273–277. [Google Scholar] [CrossRef]
- Den Hartog, D.; Dur, A.H.M.; Kamphuis, A.G.A.; Tuinebreijer, W.E.; Kreis, R.W. Comparison of Ultrasonography with Computed Tomography in the Diagnosis of Incisional Hernias. Hernia 2009, 13, 45–48. [Google Scholar] [CrossRef] [Green Version]
- Nieuwenhuizen, J.; Eker, H.H.; Timmermans, L.; Hop, W.C.; Kleinrensink, G.-J.; Jeekel, J.; Lange, J.F.; PRIMA Trialist Group. A Double Blind Randomized Controlled Trial Comparing Primary Suture Closure with Mesh Augmented Closure to Reduce Incisional Hernia Incidence. BMC Surg. 2013, 13, 48. [Google Scholar] [CrossRef] [Green Version]
- Hidalgo, M.P.; Ferrero, E.H.; Ortiz, M.A.; Castillo, J.M.F.; Hidalgo, A.G. Incisional Hernia in Patients at Risk: Can It Be Prevented? Hernia 2011, 15, 371–375. [Google Scholar] [CrossRef]
- Horowitz, M.I.; Leitman, I.M. Risk Factors for the Development of Incisional Hernia Following Roux-En-Y Gastric Bypass Surgery. Open Surg. J. 2008, 2, 15–17. [Google Scholar]
- Hesselink, V.J.; Luijendijk, R.W.; de Wilt, J.H.; Heide, R.; Jeekel, J. An Evaluation of Risk Factors in Incisional Hernia Recurrence. Surg. Gynecol. Obstet. 1993, 176, 228–234. [Google Scholar]
- Wanhainen, A. European Society for Vascular Surgery (ESVS) 2019 Clinical Practice Guidelines on the Management of Abdominal Aorto-Iliac Artery Aneurysms. Eur. J. Vasc. Endovasc. Surg. 2019, 57, 8–93. [Google Scholar] [CrossRef] [Green Version]
- National Institute for Health and Care Excellence. Abdominal Aortic Aneurysm: Diagnosis and Management. NICE Guideline NG156. 2020. Available online: https://www.nice.org.uk/guidance/NG156 (accessed on 20 November 2021).
- Chaikof, E.L.; Dalman, R.L.; Eskandari, M.K.; Jackson, B.M.; Lee, W.A.; Mansour, M.A.; Mastracci, T.M.; Mell, M.; Murad, M.H.; Nguyen, L.L.; et al. The Society for Vascular Surgery practice guidelines on the care of patients with an abdominal aortic aneurysm. J. Vasc. Surg. 2018, 67, 2–77.e2. [Google Scholar] [CrossRef] [Green Version]
- Coughlin, P.A.; Jackson, D.; White, A.D.; Bailey, M.A.; Farrow, C.; Scott, D.J.A.; Howell, S.J. Meta-Analysis of Prospective Trials Determining the Short- and Mid-Term Effect of Elective Open and Endovascular Repair of Abdominal Aortic Aneurysms on Quality of Life. Br. J. Surg. 2013, 100, 448–455. [Google Scholar] [CrossRef]
- De Bruin, J.L.; Groenwold, R.H.H.; Baas, A.F.; Brownrigg, J.R.; Prinssen, M.; Grobbee, D.E.; Blankensteijn, J.D.; for the DREAM Study Group. Quality of Life from a Randomized Trial of Open and Endovascular Repair for Abdominal Aortic Aneurysm: Quality of Life after Aortic Aneurysm Repair. Br. J. Surg. 2016, 103, 995–1002. [Google Scholar] [CrossRef]
- Shan, L.; Saxena, A.; Goh, D.; Robinson, D. A Systematic Review on the Quality of Life and Functional Status after Abdominal Aortic Aneurysm Repair in Elderly Patients with an Average Age Older than 75 Years. J. Vasc. Surg. 2019, 69, 1268–1281. [Google Scholar] [CrossRef]
- Ellert, U.; Kurth, B.-M. Methodische Betrachtungen zu den Summenscores des SF-36 anhand der erwachsenen bundesdeutschen Bevölkerung. Bundesgesundheitsblatt Gesundh. Gesundh. 2004, 47, 1027–1032. [Google Scholar] [CrossRef]
- R Development Core Team (Ed.) R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2008; ISBN 3-900051-07-0. [Google Scholar]
- Patrick, D.L.; Erickson, P. Health Status and Health Policy: Quality of Life in Health Care Evaluation and Resource Allocation; Oxford University Press: New York, NY, USA, 1993. [Google Scholar]
- Kovács, L.; Kipke, R.; Lutz, R. (Eds.) Lebensqualität in der Medizin; Springer VS: Wiesbaden, Germany, 2016; ISBN 978-3-658-10678-2. [Google Scholar]
- Akbulut, M.; Aksoy, E.; Kara, İ.; Cekmecelioglu, D.; Koksal, C. Quality of Life After Open Surgical versus Endovascular Repair of Abdominal Aortic Aneurysms. Braz. J. Cardiovasc. Surg. 2018, 33, 265–270. [Google Scholar] [CrossRef]
- Ellert, U.; Kurth, B.M. Gesundheitsbezogene Lebensqualität bei Erwachsenen in Deutschland: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt Gesundh. Gesundh. 2013, 56, 643–649. [Google Scholar] [CrossRef]
- Ferguson, R.J.; Robinson, A.B.; Splaine, M. Use of the Reliable Change Index to Evaluate Clinical Significance in SF-36 Outcomes. Qual. Life Res. 2002, 11, 509–516. [Google Scholar] [CrossRef]
- Scoggins, J.F.; Patrick, D.L. The Use of Patient-Reported Outcomes Instruments in Registered Clinical Trials: Evidence from ClinicalTrials.Gov. Contemporary 2009, 30, 289–292. [Google Scholar] [CrossRef] [Green Version]
- Bullinger, M.; Kirchberger, I.; Ware, J. Der deutsche SF-36 Health Survey: Übersetzung und psychometrische Testung eines krankheitstübergreifenden Instruments zur Erfassung der gesundheitsbezogenen Lebensqualität. Z. Gesundh. 1995, 3, 21–36. [Google Scholar] [CrossRef]
- Beattie, D.K.; Golledge, J.; Greenhalgh, R.M.; Davies, A.H. Quality of Life Assessment in Vascular Disease: Towards a Consensus. Eur. J. Vasc. Endovasc. Surg. 1997, 13, 9–13. [Google Scholar] [CrossRef] [Green Version]
- Prinssen, M.; Cuypers, P.W.M.; Buskens, E. A Randomized Trial Comparing Conventional and Endovascular Repair of Abdominal Aortic Aneurysms. N. Engl. J. Med. 2004, 351, 1607–1618. [Google Scholar] [CrossRef] [Green Version]
- Greenhalgh, R.M.; Brown, L.C.; Epstein, D.; Kwong, G.P.S.; Powell, J.T.; Sculpher, M.J.; Thompson, S.G.; EVAR trial participants. Endovascular Aneurysm Repair versus Open Repair in Patients with Abdominal Aortic Aneurysm (EVAR Trial 1): Randomised Controlled Trial. Lancet 2005, 365, 2179–2186. [Google Scholar] [CrossRef]
- Schanzer, A.; Greenberg, R.K.; Hevelone, N.; Robinson, W.P.; Eslami, M.H.; Goldberg, R.J. Predictors of abdominal aortic aneurysm sac enlargement after endovascular repair. Circulation 2011, 123, 2848–2855. [Google Scholar] [CrossRef]
- Kontopodis, N.; Papadopoulos, G.; Galanakis, N.; Tsetis, D.; Ioannou, C.V. Improvement of patient eligibility with the use of new generation endografts for the treatment of abdominal aortic aneurysms. A comparison study among currently used endografts and literature review. Expert Rev. Med. Devices 2017, 14, 245–250. [Google Scholar] [CrossRef]
- Zavatta, M.; Squizzato, F.; Balestriero, G.; Bonvini, S.; Perkmann, R.; Milite, D.; Veraldi, G.F.; Antonello, M.; Triveneto Incraft Registry Collaborators. Early and midterm outcomes of endovascular aneurysm repair with an ultra-low-profile endograft from the Triveneto Incraft Registry. J. Vasc. Surg. 2021, 73, 1950–1957.e2. [Google Scholar] [CrossRef]
- De Donato, G.; Pasqui, E.; Nano, G.; Lenti, M.; Mangialardi, N.; Speziale, F.; Ferrari, M.; Michelagnoli, S.; Tozzi, M.; Palasciano, G.; et al. Long-Term results of treatment of infrarenal aortic aneurysms with low-profile stent grafts in a multicenter registry. J. Vasc. Surg. 2022, 75, 1242–1252.e2. [Google Scholar] [CrossRef]
- Hajibandeh, S.; Hajibandeh, S.; Antoniou, S.A.; Child, E.; Torella, F.; Antoniou, G.A. Percutaneous access for endovascular aortic aneurysm repair: A systematic review and meta-analysis. Vascular 2016, 24, 638–648. [Google Scholar] [CrossRef]
- Cao, Z.; Wu, W.; Zhao, K.; Zhao, J.; Yang, Y.; Jiang, C.; Zhu, R. Safety and Efficacy of Totally Percutaneous Access Compared with Open Femoral Exposure for Endovascular Aneurysm Repair: A Meta-Analysis. J. Endovasc. Ther. 2017, 24, 246–253. [Google Scholar] [CrossRef]
- Ah-kee, E.Y.; Kallachil, T.; O’Dwyer, P.J. Patient Awareness and Symptoms from an Incisional Hernia. Int. Surg. 2014, 99, 241–246. [Google Scholar] [CrossRef] [Green Version]
- Van Ramshorst, G.H.; Eker, H.H.; Hop, W.C.J.; Jeekel, J.; Lange, J.F. Impact of Incisional Hernia on Health-Related Quality of Life and Body Image: A Prospective Cohort Study. Am. J. Surg. 2012, 204, 144–150. [Google Scholar] [CrossRef]
- O’Hare, J.L.; Ward, J.; Earnshaw, J.J. Late Results of Mesh Wound Closure after Elective Open Aortic Aneurysm Repair. Eur. J. Vasc. Endovasc. Surg. 2007, 33, 412–413. [Google Scholar] [CrossRef] [Green Version]
- Caglià, P.; Tracia, A.; Borzì, L.; Amodeo, L.; Tracia, L.; Veroux, M.; Amodeo, C. Incisional Hernia in the Elderly: Risk Factors and Clinical Considerations. Int. J. Surg. 2014, 12, S164–S169. [Google Scholar] [CrossRef] [Green Version]
- Yahchouchy-Chouillard, E.; Aura, T.; Picone, O.; Etienne, J.-C.; Fingerhut, A. Incisional Hernias. Dig. Surg. 2003, 20, 3–9. [Google Scholar] [CrossRef]
- Jairam, A.P.; Timmermans, L.; Eker, H.H.; Pierik, R.E.G.J.M.; van Klaveren, D.; Steyerberg, E.W.; Timman, R.; van der Ham, A.C.; Dawson, I.; Charbon, J.A.; et al. Prevention of Incisional Hernia with Prophylactic Onlay and Sublay Mesh Reinforcement versus Primary Suture Only in Midline Laparotomies (PRIMA): 2-Year Follow-up of a Multicentre, Double-Blind, Randomised Controlled Trial. Lancet 2017, 390, 567–576. [Google Scholar] [CrossRef]
- Lederle, F.A.; Matsumura, J.S.; Kougias, P.; Cikrit, D.F. Long-Term Comparison of Endovascular and Open Repair of Abdominal Aortic Aneurysm. N. Engl. J. Med. 2012, 367, 1988–1997. [Google Scholar] [CrossRef] [Green Version]
- Höer, J.; Lawong, G.; Klinge, U.; Schumpelick, V. Einflussfaktoren der Narbenhernienentstehung: Retrospektive Untersuchung an 2.983 laparotomierten Patienten über einen Zeitraum von 10 Jahren. Chirurg 2002, 73, 474–480. [Google Scholar] [CrossRef]
- Depuydt, M.; Allaeys, M.; de Carvalho, L.A.; Vanlander, A.; Berrevoet, F. Prophylactic Mesh after Midline Laparotomy: Evidence Is out There, but Why Do Surgeons Hesitate? World J. Surg. 2021, 45, 1349–1361. [Google Scholar] [CrossRef]
- Itani, K.M.F.; Neumayer, L.; Reda, D.; Kim, L.; Anthony, T. Repair of Ventral Incisional Hernia: The Design of a Randomized Trial to Compare Open and Laparoscopic Surgical Techniques. Am. J. Surg. 2004, 188, 22–29. [Google Scholar] [CrossRef]
- Muysoms, F.E.; Detry, O.; Vierendeels, T.; Huyghe, M.; Miserez, M.; Ruppert, M.; Tollens, T.; Defraigne, J.-O.; Berrevoet, F. Prevention of Incisional Hernias by Prophylactic Mesh-Augmented Reinforcement of Midline Laparotomies for Abdominal Aortic Aneurysm Treatment: A Randomized Controlled Trial. Ann. Surg. 2016, 263, 638–645. [Google Scholar] [CrossRef]
- Diener, H.; Eckstein, H.H.; Wenk, H.; Gahlen, J.; Kellersmann, R.; Grommes, J.; Verhoeven, E.; Daum, H.; Hupp, T.; Debus, S. Prevention of Incisional Hernia after Abdominal Aortic Aneurysm Repair (AIDA Study). Eur. J. Vasc. Endovasc. Surg. 2016, 52, 412–413. [Google Scholar] [CrossRef]
- Henriksen, N.A.; Helgstrand, F.; Vogt, K.C.; Jorgensen, L.N.; Bisgaard, T. Risk Factors for Incisional Hernia Repair after Aortic Reconstructive Surgery in a Nationwide Study. J. Vasc. Surg. 2013, 57, 1524–1530.e3. [Google Scholar] [CrossRef] [Green Version]
- Cobb, W.S.; Warren, J.A.; Ewing, J.A.; Burnikel, A.; Merchant, M.; Carbonell, A.M. Open Retromuscular Mesh Repair of Complex Incisional Hernia: Predictors of Wound Events and Recurrence. J. Am. Coll. Surg. 2015, 220, 606–613. [Google Scholar] [CrossRef]
- Brown, R.H.; Subramanian, A.; Hwang, C.S.; Chang, S.; Awad, S.S. Comparison of Infectious Complications with Synthetic Mesh in Ventral Hernia Repair. Am. J. Surg. 2013, 205, 182–187. [Google Scholar] [CrossRef]
- Van den Dop, M.L.; Sneiders, D.; Kleinrensink, G.-J.; Jeekel, H.J.; Lange, J.F.; Timmermans, L. Infectious Complication in Relation to the Prophylactic Mesh Position: The PRIMA Trial Revisited. J. Am. Coll. Surg. 2021, 232, 738–745. [Google Scholar] [CrossRef]

| OR n = 36 | EVAR n = 47 | |||
|---|---|---|---|---|
| n | % | n | % | |
| Age | 64 ± 8.8 | 70.2 ± 6.9 * | ||
| Male | 32 | 88.9 | 45 | 95.7 |
| Female | 4 | 11.1 | 2 | 4.3 |
| CAD | 14 | 38.9 | 19 | 40.4 |
| Arterial hypertension | 33 | 91.7 | 34 | 72.3 * |
| HLP | 18 | 50.0 | 16 | 34.0 |
| Smoking | 10 | 27.8 | 9 | 19.1 * |
| Diabetes | 11 | 30.5 | 5 | 10.6 * |
| COPD | 6 | 16.7 | 6 | 12.8 |
| BMI | 28.01 ± 3.62 | 29.29 ± 3.05 | ||
| Elective intervention | 30 | 83.3 | 46 | 97.9 * |
| Emergent intervention | 6 | 16.6 | 1 | 2.1 * |
| Follow-up (years) | 7.8 ± 2.7 | 6.6 ± 1.9 | ||
| Min. follow-up (years) | 3.6 | 3.6 | ||
| Max. follow-up (years) | 12.1 | 12.4 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gruel, J.; Grambow, E.; Weinrich, M.; Heller, T.; Groß, J.; Leuchter, M.; Philipp, M. Assessment of Quality of Life after Endovascular and Open Abdominal Aortic Aneurysm Repair: A Retrospective Single-Center Study. J. Clin. Med. 2022, 11, 3017. https://doi.org/10.3390/jcm11113017
Gruel J, Grambow E, Weinrich M, Heller T, Groß J, Leuchter M, Philipp M. Assessment of Quality of Life after Endovascular and Open Abdominal Aortic Aneurysm Repair: A Retrospective Single-Center Study. Journal of Clinical Medicine. 2022; 11(11):3017. https://doi.org/10.3390/jcm11113017
Chicago/Turabian StyleGruel, Johanna, Eberhard Grambow, Malte Weinrich, Thomas Heller, Justus Groß, Matthias Leuchter, and Mark Philipp. 2022. "Assessment of Quality of Life after Endovascular and Open Abdominal Aortic Aneurysm Repair: A Retrospective Single-Center Study" Journal of Clinical Medicine 11, no. 11: 3017. https://doi.org/10.3390/jcm11113017






