Role of CGRP in Neuroimmune Interaction via NF-κB Signaling Genes in Glial Cells of Trigeminal Ganglia
Abstract
:1. Introduction
2. Results
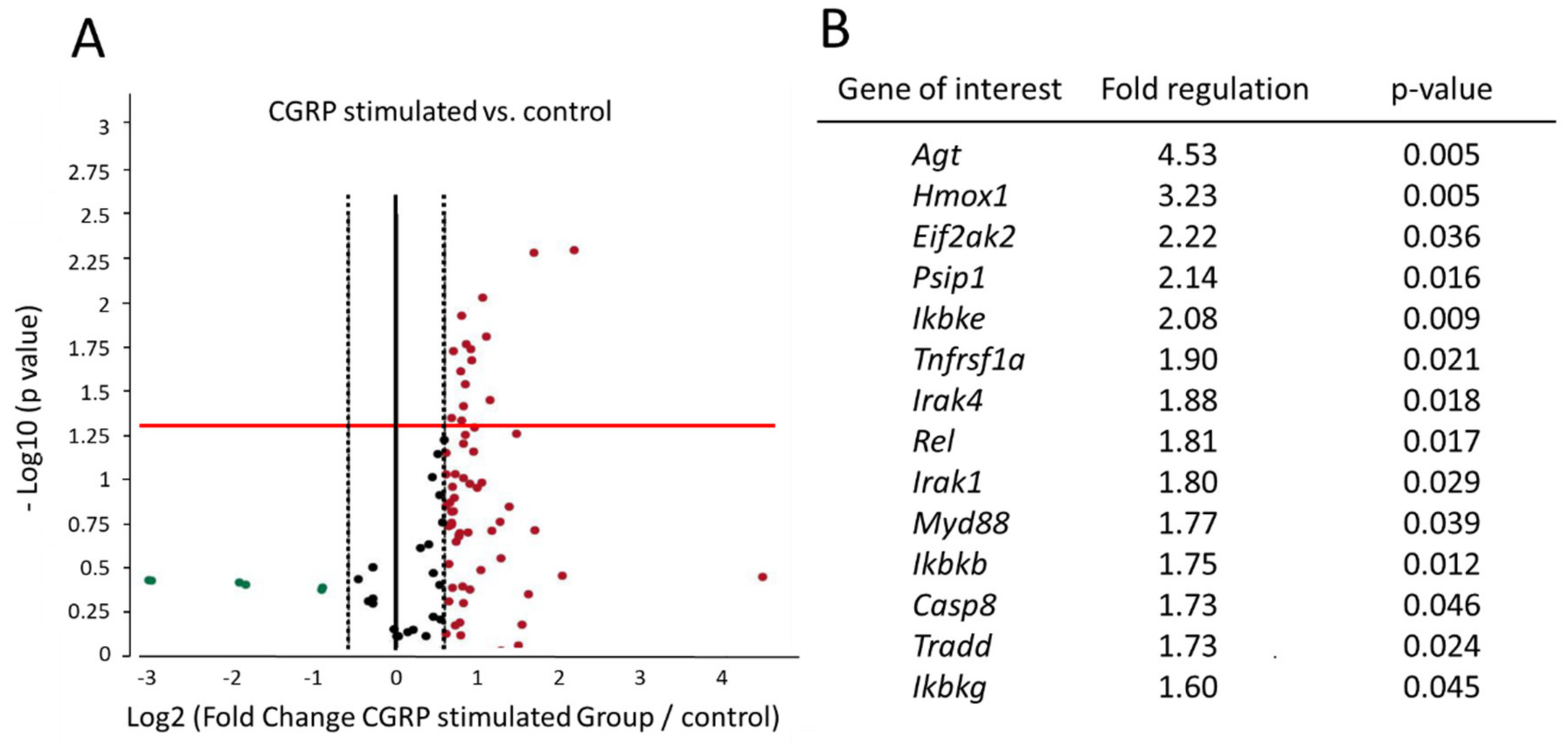
2.1. CGRP Induces Differential Regulation of Several Genes in Glial Cells of TG Involved in NF-κB Signaling Pathway
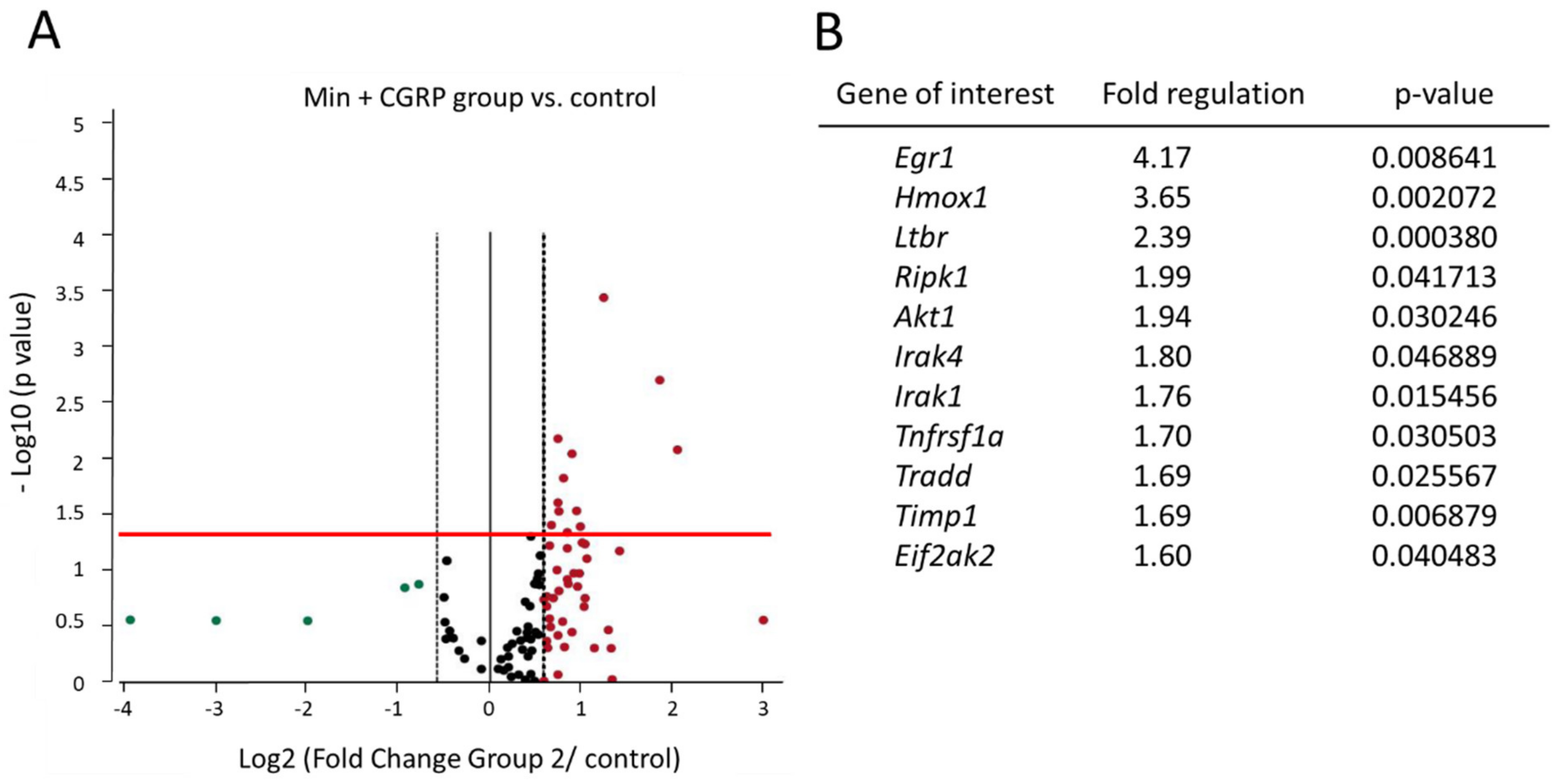
2.2. Effect of Minocycline Treatment for 30 Min Followed by CGRP Stimulation on NF-κB Pathway’s Signaling Genes
2.3. Effect of IG CGRP Administration and Minocycline Treatment Followed by CGRP Stimulation on the Gene Expression of Myd88, Egr1 and Akt1
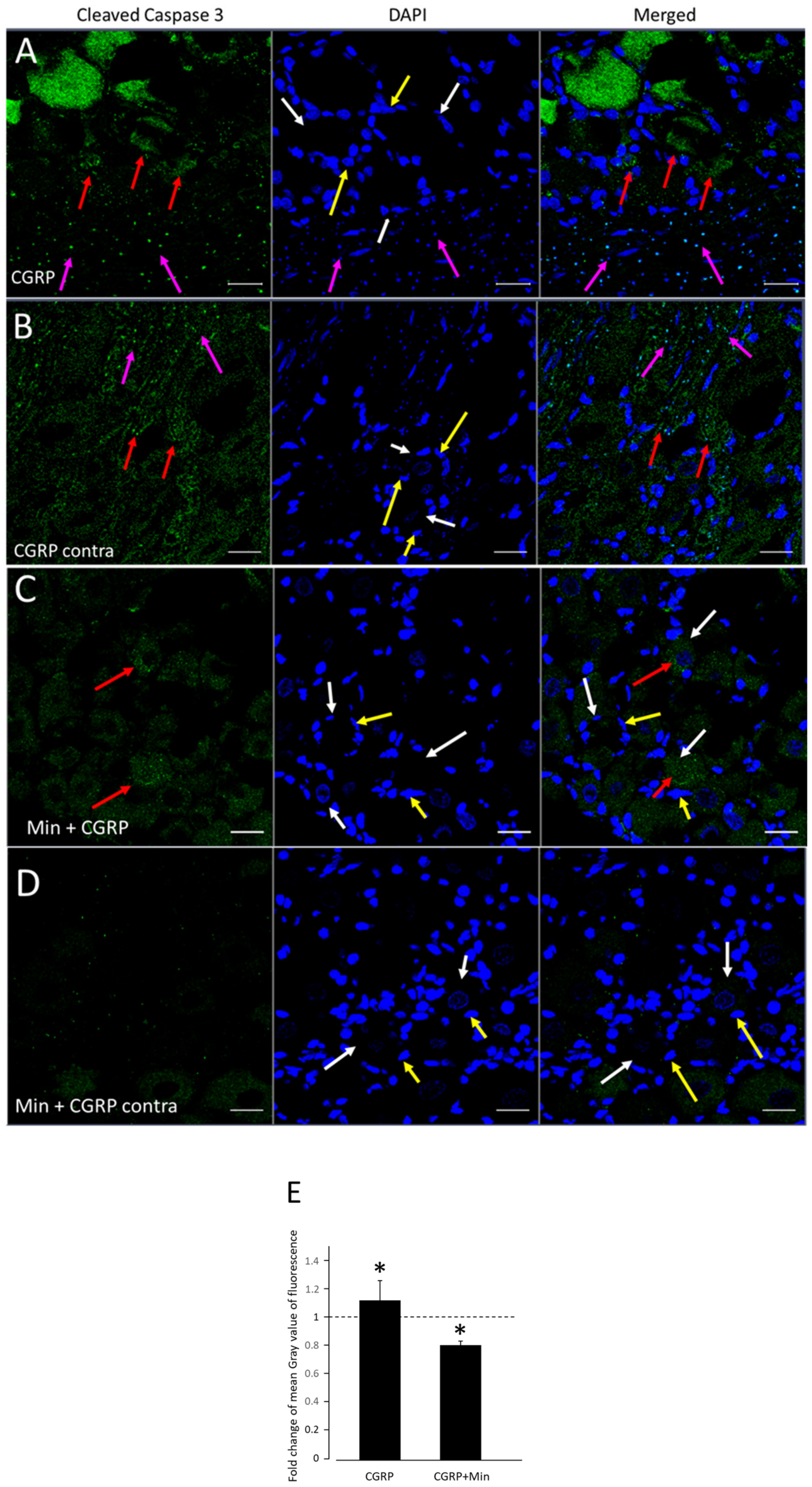
2.4. Effect of CGRP Stimulation on Cleaved Caspase-3 (Cleav Casp3) Protein Expression of TG
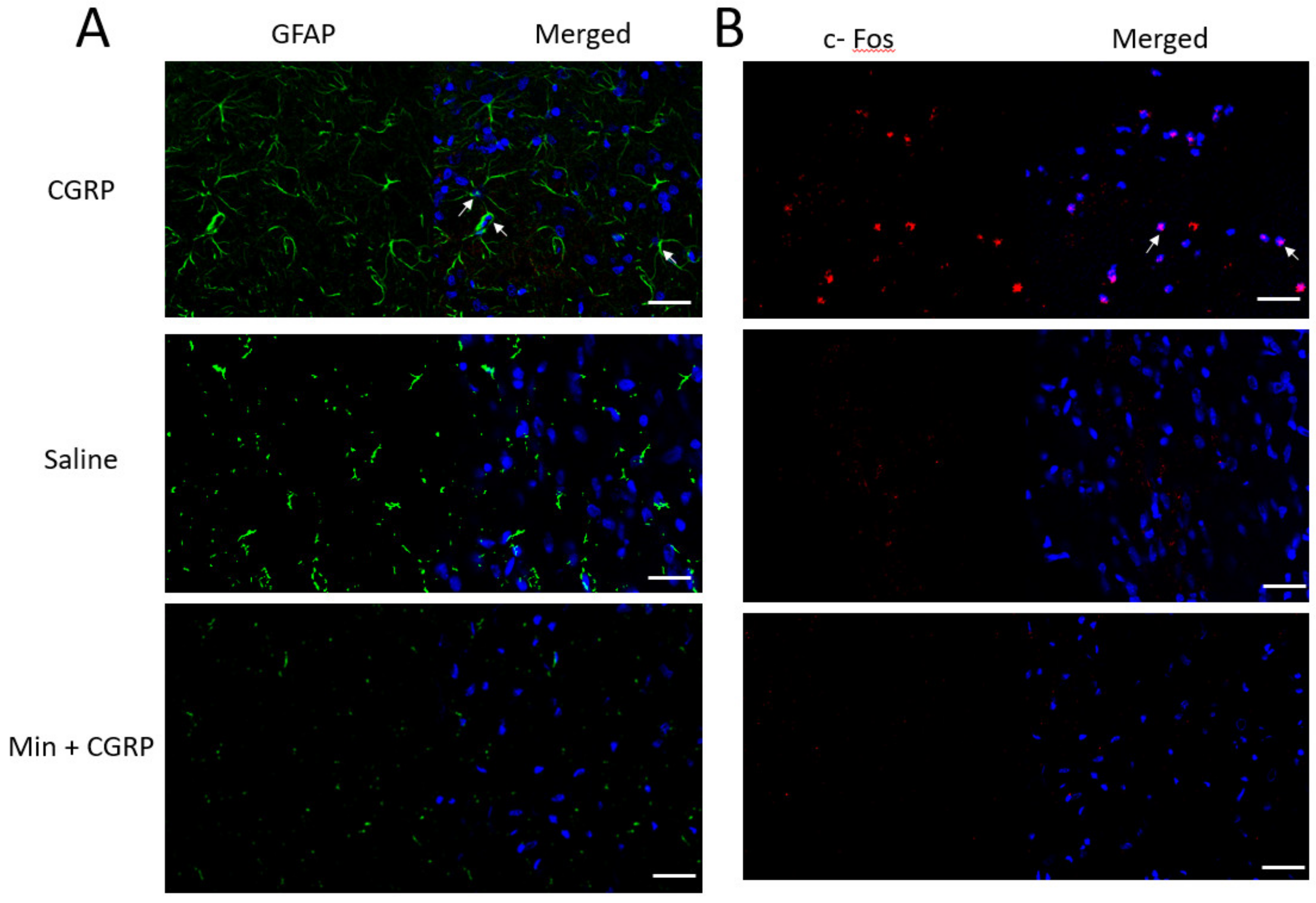
2.5. Effect of IG CGRP Administration on the Spinal Trigeminal Nucleus Caudalis Glial and Neuronal Activation—A Qualitative Assessment
3. Discussion
4. Materials and Methods
4.1. Animals
4.2. Glial Rich Culture
4.3. NF-κB Signaling Pathway RT2 Profiler PCR Array
4.4. Intraganglionar Drug Administration
4.5. Quantitative Real-Time Polymerase Chain Reaction (qRT-PCR)
4.6. Immunohistochemistry
4.7. Measurement of Staining Intensity for Cleav Casp3 Expression
4.8. Statistical Analysis
Author Contributions
Funding
Conflicts of Interest
References
- McMahon, S.B.; Cafferty, W.B.; Marchand, F. Immune and glial cell factors as pain mediators and modulators. Exp. Neurol. 2005, 192, 444–462. [Google Scholar] [CrossRef]
- Perkins, N.M.; Tracey, D.J. Hyperalgesia due to nerve injury: Role of neutrophils. Neuroscience 2000, 101, 745–757. [Google Scholar] [CrossRef]
- Iwasa, T.; Afroz, S.; Inoue, M.; Arakaki, R.; Oshima, M.; Raju, R.; Waskitho, A.; Inoue, M.; Baba, O.; Matsuka, Y. IL-10 and CXCL2 in trigeminal ganglia in neuropathic pain. Neurosci. Lett. 2019, 703, 132–138. [Google Scholar] [CrossRef]
- Matsuka, Y.; Afroz, S.; Dalanon, J.C.; Iwasa, T.; Waskitho, A.; Oshima, M. The role of chemical transmitters in neuron-glia interaction and pain in sensory ganglion. Neurosci. Biobehav. Rev. 2020, 108, 393–399. [Google Scholar] [CrossRef]
- Ma, W.; Bisby, M.A. Increased activation of nuclear factor kappa B in rat lumbar dorsal root ganglion neurons following partial sciatic nerve injuries. Brain Res. 1998, 797, 243–254. [Google Scholar] [CrossRef]
- Kaltschmidt, B.; Widera, D.; Kaltschmidt, C. Signaling via NF-kappaB in the nervous system. Biochim. Biophys. Acta 2005, 1745, 287–299. [Google Scholar] [CrossRef] [Green Version]
- Fu, E.S.; Zhang, Y.P.; Sagen, J.; Candiotti, K.A.; Morton, P.D.; Liebl, D.J.; Bethea, J.R.; Brambilla, R. Transgenic inhibition of glial NF-kappa B reduces pain behavior and inflammation after peripheral nerve injury. Pain 2010, 148, 509–518. [Google Scholar] [CrossRef] [Green Version]
- Cady, R.J.; Glenn, J.R.; Smith, K.M.; Durham, P.L. Calcitonin gene-related peptide promotes cellular changes in trigeminal neurons and glia implicated in peripheral and central sensitization. Mol. Pain 2011, 7, 94. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Benemei, S.; Nicoletti, P.; Capone, J.G.; Geppetti, P. CGRP receptors in the control of pain and inflammation. Curr. Opin. Pharmacol. 2009, 9, 9–14. [Google Scholar] [CrossRef] [PubMed]
- De Felice, M.; Ossipov, M.H.; Wang, R.; Lai, J.; Chichorro, J.; Meng, I.; Dodick, D.W.; Vanderah, T.W.; Dussor, G.; Porreca, F. Triptan-induced latent sensitization: A possible basis for medication overuse headache. Ann. Neurol. 2010, 67, 325–337. [Google Scholar] [CrossRef] [PubMed]
- Assas, B.M.; Pennock, J.I.; Miyan, J.A. Calcitonin gene-related peptide is a key neurotransmitter in the neuro-immune axis. Front. Neurosci. 2014, 8, 23. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Z.; Ma, W.; Chabot, J.G.; Quirion, R. Calcitonin gene-related peptide as a regulator of neuronal CaMKII-CREB, microglial p38-NFκB and astroglial ERK-Stat1/3 cascades mediating the development of tolerance to morphine-induced analgesia. Pain 2010, 151, 194–205. [Google Scholar] [CrossRef] [PubMed]
- Afroz, S.; Arakaki, R.; Iwasa, T.; Oshima, M.; Hosoki, M.; Inoue, M.; Baba, O.; Okayama, Y.; Matsuka, Y. CGRP Induces Differential Regulation of Cytokines from Satellite Glial Cells in Trigeminal Ganglia and Orofacial Nociception. Int. J. Mol. Sci. 2019, 20, 711. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vause, C.V.; Durham, P.L. Calcitonin gene-related peptide differentially regulates gene and protein expression in trigeminal glia cells: Findings from array analysis. Neurosci. Lett. 2010, 473, 163–167. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Thalakoti, S.; Patil, V.V.; Damodaram, S.; Vause, C.V.; Langford, L.E.; Freeman, S.E.; Durham, P.L. Neuron-glia signaling in trigeminal ganglion: Implications for migraine pathology. Headache 2007, 47, 1008–1025. [Google Scholar] [CrossRef] [Green Version]
- Ceruti, S.; Villa, G.; Fumagalli, M.; Colombo, L.; Magni, G.; Zanardelli, M.; Fabbretti, E.; Verderio, C.; van den Maagdenberg, A.M.; Nistri, A.; et al. Calcitonin gene-related peptide-mediated enhancement of purinergic neuron/glia communication by the algogenic factor bradykinin in mouse trigeminal ganglia from wild-type and R192Q Cav2.1 Knock-in mice: Implications for basic mechanisms of migraine pain. J. Neurosci. Off. J. Soc. Neurosci. 2011, 31, 3638–3649. [Google Scholar] [CrossRef] [Green Version]
- Chan, C.F.; Sun, W.Z.; Lin, J.K.; Lin-Shiau, S.Y. Activation of transcription factors of nuclear factor kappa B, activator protein-1 and octamer factors in hyperalgesia. Eur. J. Pharmacol. 2000, 402, 61–68. [Google Scholar] [CrossRef]
- Ahmed, A.S.; Berg, S.; Alkass, K.; Druid, H.; Hart, D.A.; Svensson, C.I.; Kosek, E. NF-κB-Associated Pain-Related Neuropeptide Expression in Patients with Degenerative Disc Disease. Int. J. Mol. Sci. 2019, 20, 658. [Google Scholar] [CrossRef] [Green Version]
- Zhongyi, S.; Sai, Z.; Chao, L.; Jiwei, T. Effects of nuclear factor kappa B signaling pathway in human intervertebral disc degeneration. Spine 2015, 40, 224–232. [Google Scholar] [CrossRef]
- Sun, L.; Xu, Q.; Zhang, W.; Jiao, C.; Wu, H.; Chen, X. The involvement of spinal annexin A10/NF-κB/MMP-9 pathway in the development of neuropathic pain in rats. BMC Neurosci. 2019, 20, 28. [Google Scholar] [CrossRef] [Green Version]
- Fusco, R.; Scuto, M.; Cordaro, M.; D’Amico, R.; Gugliandolo, E.; Siracusa, R.; Peritore, A.F.; Crupi, R.; Impellizzeri, D.; Cuzzocrea, S.; et al. N-Palmitoylethanolamide-Oxazoline Protects against Middle Cerebral Artery Occlusion Injury in Diabetic Rats by Regulating the SIRT1 Pathway. Int. J. Mol. Sci. 2019, 20, 4845. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bettoni, I.; Comelli, F.; Rossini, C.; Granucci, F.; Giagnoni, G.; Peri, F.; Costa, B. Glial TLR4 receptor as new target to treat neuropathic pain: Efficacy of a new receptor antagonist in a model of peripheral nerve injury in mice. Glia 2008, 56, 1312–1319. [Google Scholar] [CrossRef] [PubMed]
- Xu, L.; Liu, Y.; Sun, Y.; Li, H.; Mi, W.; Jiang, Y. Analgesic effects of TLR4/NF-κB signaling pathway inhibition on chronic neuropathic pain in rats following chronic constriction injury of the sciatic nerve. Biomed. Pharmacother. Biomed. Pharmacother. 2018, 107, 526–533. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Zhang, H.; Zhang, H.; Kosturakis, A.K.; Jawad, A.B.; Dougherty, P.M. Toll-like receptor 4 signaling contributes to Paclitaxel-induced peripheral neuropathy. J. Pain Off. J. Am. Pain Soc. 2014, 15, 712–725. [Google Scholar] [CrossRef] [Green Version]
- Liu, F.; Wang, Z.; Qiu, Y.; Wei, M.; Li, C.; Xie, Y.; Shen, L.; Huang, Y.; Ma, C. Suppression of MyD88-dependent signaling alleviates neuropathic pain induced by peripheral nerve injury in the rat. J. Neuroinflamm. 2017, 14, 70. [Google Scholar] [CrossRef] [Green Version]
- Reuter, U.; Bolay, H.; Jansen-Olesen, I.; Chiarugi, A.; Sanchez del Rio, M.; Letourneau, R.; Theoharides, T.C.; Waeber, C.; Moskowitz, M.A. Delayed inflammation in rat meninges: Implications for migraine pathophysiology. Brain J. Neurol. 2001, 124 Pt 12, 2490–2502. [Google Scholar] [CrossRef]
- Croston, G.E.; Cao, Z.; Goeddel, D.V. NF-kappa B activation by interleukin-1 (IL-1) requires an IL-1 receptor-associated protein kinase activity. J. Biol. Chem. 1995, 270, 16514–16517. [Google Scholar] [CrossRef] [Green Version]
- Atlas of Genetics and Cytogenetics in Oncology. Available online: http://atlasgeneticsoncology.org/Deep/NFΚBID20033.html (accessed on 16 March 2020).
- Eftekhari, S.; Salvatore, C.A.; Calamari, A.; Kane, S.A.; Tajti, J.; Edvinsson, L. Differential distribution of calcitonin gene-related peptide and its receptor components in the human trigeminal ganglion. Neuroscience 2010, 169, 683–696. [Google Scholar] [CrossRef] [Green Version]
- Miller, S.; Liu, H.; Warfvinge, K.; Shi, L.; Dovlatyan, M.; Xu, C.; Edvinsson, L. Immunohistochemical localization of the calcitonin gene-related peptide binding site in the primate trigeminovascular system using functional antagonist antibodies. Neuroscience 2016, 328, 165–183. [Google Scholar] [CrossRef]
- Lennerz, J.K.; Rühle, V.; Ceppa, E.P.; Neuhuber, W.L.; Bunnett, N.W.; Grady, E.F.; Messlinger, K. Calcitonin receptor-like receptor (CLR), receptor activity-modifying protein 1 (RAMP1), and calcitonin gene-related peptide (CGRP) immunoreactivity in the rat trigeminovascular system: Differences between peripheral and central CGRP receptor distribution. J. Comp. Neurol. 2008, 507, 1277–1299. [Google Scholar] [CrossRef]
- Mitterreiter, J.G.; Ouwendijk, W.; van Velzen, M.; van Nierop, G.P.; Osterhaus, A.; Verjans, G. Satellite glial cells in human trigeminal ganglia have a broad expression of functional Toll-like receptors. Eur. J. Immunol. 2017, 47, 1181–1187. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Parameswaran, N.; Disa, J.; Spielman, W.S.; Brooks, D.P.; Nambi, P.; Aiyar, N. Activation of multiple mitogen-activated protein kinases by recombinant calcitonin gene-related peptide receptor. Eur. J. Pharmacol. 2000, 389, 125–130. [Google Scholar] [CrossRef]
- Vause, C.V.; Durham, P.L. CGRP stimulation of iNOS and NO release from trigeminal ganglion glial cells involves mitogen-activated protein kinase pathways. J. Neurochem. 2009, 110, 811–821. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brettschneider, J.; Hartmann, N.; Lehmensiek, V.; Mogel, H.; Ludolph, A.C.; Tumani, H. Cerebrospinal fluid markers of idiopathic intracranial hypertension: Is the renin-angiotensinogen system involved? Cephalalgia Int. J. Headache 2011, 31, 116–121. [Google Scholar] [CrossRef] [PubMed]
- Paul, M.; Poyan Mehr, A.; Kreutz, R. Physiology of local renin-angiotensin systems. Physiol. Rev. 2006, 86, 747–803. [Google Scholar] [CrossRef] [PubMed]
- Bäckryd, E.; Ghafouri, B.; Carlsson, A.K.; Olausson, P.; Gerdle, B. Multivariate proteomic analysis of the cerebrospinal fluid of patients with peripheral neuropathic pain and healthy controls—A hypothesis-generating pilot study. J. Pain Res. 2015, 8, 321–333. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bhat, S.A.; Goel, R.; Shukla, R.; Hanif, K. Angiotensin Receptor Blockade Modulates NFκB and STAT3 Signaling and Inhibits Glial Activation and Neuroinflammation Better than Angiotensin-Converting Enzyme Inhibition. Mol. Neurobiol. 2016, 53, 6950–6967. [Google Scholar] [CrossRef]
- Gil, J.; García, M.A.; Esteban, M. Caspase 9 activation by the dsRNA-dependent protein kinase, PKR: Molecular mechanism and relevance. FEBS Lett. 2002, 529, 249–255. [Google Scholar] [CrossRef] [Green Version]
- Von Roretz, C.; Gallouzi, I.E. Protein kinase RNA/FADD/caspase-8 pathway mediates the proapoptotic activity of the RNA-binding protein human antigen R (HuR). J. Biol. Chem. 2010, 285, 16806–16813. [Google Scholar] [CrossRef] [Green Version]
- Khandelwal, P.J.; Herman, A.M.; Moussa, C.E. Inflammation in the early stages of neurodegenerative pathology. J. Neuroimmunol. 2011, 238, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Bonnet, M.C.; Weil, R.; Dam, E.; Hovanessian, A.G.; Meurs, E.F. PKR stimulates NF-kappaB irrespective of its kinase function by interacting with the IkappaB kinase complex. Mol. Cell. Biol. 2000, 20, 4532–4542. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tronel, C.; Page, G.; Bodard, S.; Chalon, S.; Antier, D. The specific PKR inhibitor C16 prevents apoptosis and IL-1β production in an acute excitotoxic rat model with a neuroinflammatory component. Neurochem. Int. 2014, 64, 73–83. [Google Scholar] [CrossRef] [PubMed]
- Schipper, H.M.; Song, W. A heme oxygenase-1 transducer model of degenerative and developmental brain disorders. Int. J. Mol. Sci. 2015, 16, 5400–5419. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, K.; Gunter, K.; Maines, M.D. Neurons overexpressing heme oxygenase-1 resist oxidative stress-mediated cell death. J. Neurochem. 2000, 75, 304–313. [Google Scholar] [CrossRef]
- Schipper, H.M.; Song, W.; Zukor, H.; Hascalovici, J.R.; Zeligman, D. Heme oxygenase-1 and neurodegeneration: Expanding frontiers of engagement. J. Neurochem. 2009, 110, 469–485. [Google Scholar] [CrossRef]
- Yama, K.; Sato, K.; Murao, Y.; Tatsunami, R.; Tampo, Y. Epalrestat Upregulates Heme Oxygenase-1, Superoxide Dismutase, and Catalase in Cells of the Nervous System. Biol. Pharm. Bull. 2016, 39, 1523–1530. [Google Scholar] [CrossRef] [Green Version]
- Hirata, K.; He, J.W.; Kuraoka, A.; Omata, Y.; Hirata, M.; Islam, A.T.; Noguchi, M.; Kawabuchi, M. Heme oxygenase1 (HSP-32) is induced in myelin-phagocytosing Schwann cells of injured sciatic nerves in the rat. Eur. J. Neurosci. 2000, 12, 4147–4152. [Google Scholar] [CrossRef]
- Kim, M.; Kim, H.; Kim, D.; Kim, D.; Huh, Y.; Park, C.; Chung, H.J.; Jung, J.; Jeong, N.Y. Heme Oxygenase 1 in Schwann Cells Regulates Peripheral Nerve Degeneration against Oxidative Stress. ASN Neuro 2019, 11, 1759091419838949. [Google Scholar] [CrossRef] [Green Version]
- Lee, T.S.; Tsai, H.L.; Chau, L.Y. Induction of heme oxygenase-1 expression in murine macrophages is essential for the anti-inflammatory effect of low dose 15-deoxy-Delta 12,14-prostaglandin J2. J. Biol. Chem. 2003, 278, 19325–19330. [Google Scholar] [CrossRef] [Green Version]
- Chen, M.; Ona, V.O.; Li, M.; Ferrante, R.J.; Fink, K.B.; Zhu, S.; Bian, J.; Guo, L.; Farrell, L.A.; Hersch, S.M.; et al. Minocycline inhibits caspase-1 and caspase-3 expression and delays mortality in a transgenic mouse model of Huntington disease. Nat. Med. 2000, 6, 797–801. [Google Scholar] [CrossRef]
- Tikka, T.; Fiebich, B.L.; Goldsteins, G.; Keinanen, R.; Koistinaho, J. Minocycline, a tetracycline derivative, is neuroprotective against excitotoxicity by inhibiting activation and proliferation of microglia. J. Neurosci. Off. J. Soc. Neurosci. 2001, 21, 2580–2588. [Google Scholar] [CrossRef]
- Zhu, S.; Stavrovskaya, I.G.; Drozda, M.; Kim, B.Y.; Ona, V.; Li, M.; Sarang, S.; Liu, A.S.; Hartley, D.M.; Wu, D.C.; et al. Minocycline inhibits cytochrome c release and delays progression of amyotrophic lateral sclerosis in mice. Nature 2002, 417, 74–78. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.; Zhang, Y.; Dodel, R.; Farlow, M.R.; Paul, S.M.; Du, Y. Minocycline blocks nitric oxide-induced neurotoxicity by inhibition p38 MAP kinase in rat cerebellar granule neurons. Neurosci. Lett. 2001, 315, 61–64. [Google Scholar] [CrossRef]
- Liévens, J.C.; Iché, M.; Laval, M.; Faivre-Sarrailh, C.; Birman, S. AKT-sensitive or insensitive pathways of toxicity in glial cells and neurons in Drosophila models of Huntington’s disease. Hum. Mol. Genet. 2008, 17, 882–894. [Google Scholar] [CrossRef] [Green Version]
- Tarassishin, L.; Suh, H.S.; Lee, S.C. Interferon regulatory factor 3 plays an anti-inflammatory role in microglia by activating the PI3K/Akt pathway. J. Neuroinflamm. 2011, 8, 187. [Google Scholar] [CrossRef] [Green Version]
- Marte, B.M.; Downward, J. PKB/Akt: Connecting phosphoinositide 3-kinase to cell survival and beyond. Trends Biochem. Sci. 1997, 22, 355–358. [Google Scholar] [CrossRef]
- Pi, R.; Li, W.; Lee, N.T.; Chan, H.H.; Pu, Y.; Chan, L.N.; Sucher, N.J.; Chang, D.C.; Li, M.; Han, Y. Minocycline prevents glutamate-induced apoptosis of cerebellar granule neurons by differential regulation of p38 and Akt pathways. J. Neurochem. 2004, 91, 1219–1230. [Google Scholar] [CrossRef]
- Kawasaki, Y.; Xu, Z.Z.; Wang, X.; Park, J.Y.; Zhuang, Z.Y.; Tan, P.H.; Gao, Y.J.; Roy, K.; Corfas, G.; Lo, E.H.; et al. Distinct roles of matrix metalloproteases in the early- and late-phase development of neuropathic pain. Nat. Med. 2008, 14, 331–336. [Google Scholar] [CrossRef]
- Ali, S.; Driscoll, H.E.; Newton, V.L.; Gardiner, N.J. Matrix metalloproteinase-2 is downregulated in sciatic nerve by streptozotocin induced diabetes and/or treatment with minocycline: Implications for nerve regeneration. Exp. Neurol. 2014, 261, 654–665. [Google Scholar] [CrossRef]
- Bozon, B.; Davis, S.; Laroche, S. A requirement for the immediate early gene zif268 in reconsolidation of recognition memory after retrieval. Neuron 2003, 40, 695–701. [Google Scholar] [CrossRef] [Green Version]
- Jiang, Y.; Liu, Y.; Zhu, C.; Ma, X.; Ma, L.; Zhou, L.; Huang, Q.; Cen, L.; Pi, R.; Chen, X. Minocycline enhances hippocampal memory, neuroplasticity and synapse-associated proteins in aged C57 BL/6 mice. Neurobiol. Learn. Mem. 2015, 121, 20–29. [Google Scholar] [CrossRef] [PubMed]
- Rygh, L.J.; Suzuki, R.; Rahman, W.; Wong, Y.; Vonsy, J.L.; Sandhu, H.; Webber, M.; Hunt, S.; Dickenson, A.H. Local and descending circuits regulate long-term potentiation and zif268 expression in spinal neurons. Eur. J. Neurosci. 2006, 24, 761–772. [Google Scholar] [CrossRef] [PubMed]
- Ko, S.W.; Vadakkan, K.I.; Ao, H.; Gallitano-Mendel, A.; Wei, F.; Milbrandt, J.; Zhuo, M. Selective contribution of Egr1 (zif/268) to persistent inflammatory pain. J. Pain Off. J. Am. Pain Soc. 2005, 6, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Dolan, S.; Hastie, P.; Crossan, C.; Nolan, A.M. Co-induction of cyclooxygenase-2 [correction of cyclooxyenase-2] and early growth response gene (Egr-1) in spinal cord in a clinical model of persistent inflammation and hyperalgesia. Mol. Pain 2011, 7, 91. [Google Scholar] [CrossRef] [Green Version]
- Plant, S.R.; Iocca, H.A.; Wang, Y.; Thrash, J.C.; O’Connor, B.P.; Arnett, H.A.; Fu, Y.X.; Carson, M.J.; Ting, J.P. Lymphotoxin beta receptor (Lt betaR): Dual roles in demyelination and remyelination and successful therapeutic intervention using Lt betaR-Ig protein. J. Neurosci. Off. J. Soc. Neurosci. 2007, 27, 7429–7437. [Google Scholar] [CrossRef]
- Xiao, X.; Putatunda, R.; Zhang, Y.; Soni, P.V.; Li, F.; Zhang, T.; Xin, M.; Luo, J.J.; Bethea, J.R.; Cheng, Y.; et al. Lymphotoxin β receptor-mediated NFκB signaling promotes glial lineage differentiation and inhibits neuronal lineage differentiation in mouse brain neural stem/progenitor cells. J. Neuroinflamm. 2018, 15, 49. [Google Scholar] [CrossRef]
- Arnoux, I.; Hoshiko, M.; Sanz Diez, A.; Audinat, E. Paradoxical effects of minocycline in the developing mouse somatosensory cortex. Glia 2014, 62, 399–410. [Google Scholar] [CrossRef]
- Diguet, E.; Fernagut, P.O.; Wei, X.; Du, Y.; Rouland, R.; Gross, C.; Bezard, E.; Tison, F. Deleterious effects of minocycline in animal models of Parkinson’s disease and Huntington’s disease. Eur. J. Neurosci. 2004, 19, 3266–3276. [Google Scholar] [CrossRef]
- Tsuji, M.; Wilson, M.A.; Lange, M.S.; Johnston, M.V. Minocycline worsens hypoxic-ischemic brain injury in a neonatal mouse model. Exp. Neurol. 2004, 189, 58–65. [Google Scholar] [CrossRef]
- Gordon, P.H.; Moore, D.H.; Miller, R.G.; Florence, J.M.; Verheijde, J.L.; Doorish, C.; Hilton, J.F.; Spitalny, G.M.; MacArthur, R.B.; Mitsumoto, H.; et al. Efficacy of minocycline in patients with amyotrophic lateral sclerosis: A phase III randomised trial. Lancet Neurol. 2007, 6, 1045–1053. [Google Scholar] [CrossRef]
- Li, J.; Vause, C.V.; Durham, P.L. Calcitonin gene-related peptide stimulation of nitric oxide synthesis and release from trigeminal ganglion glial cells. Brain Res. 2008, 1196, 22–32. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reuter, U.; Chiarugi, A.; Bolay, H.; Moskowitz, M.A. Nuclear factor-kappaB as a molecular target for migraine therapy. Ann. Neurol. 2002, 51, 507–516. [Google Scholar] [CrossRef] [PubMed]
- Matsuka, Y.; Edmonds, B.; Mitrirattanakul, S.; Schweizer, F.E.; Spigelman, I. Two types of neurotransmitter release patterns in isolectin B4-positive and negative trigeminal ganglion neurons. Neuroscience 2007, 144, 665–674. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Neubert, J.K.; Mannes, A.J.; Keller, J.; Wexel, M.; Iadarola, M.J.; Caudle, R.M. Peripheral targeting of the trigeminal ganglion via the infraorbital foramen as a therapeutic strategy. Brain Res. Brain Res. Protoc. 2005, 15, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Shen, G.Y.; Ren, H.; Huang, J.J.; Zhang, Z.D.; Zhao, W.H.; Yu, X.; Shang, Q.; Qiu, T.; Zhang, Y.Z.; Tang, J.J.; et al. Plastrum Testudinis Extracts Promote BMSC Proliferation and Osteogenic Differentiation by Regulating Let-7f-5p and the TNFR2/PI3K/AKT Signaling Pathway. Cell. Physiol. Biochem. Int. J. Exp. Cell. Physiol. Biochem. Pharmacol. 2018, 47, 2307–2318. [Google Scholar] [CrossRef] [PubMed]
- Guan, M.; Li, W.; Xu, L.; Zeng, Y.; Wang, D.; Zheng, Z.; Lyv, F.; Xue, Y. Metformin Improves Epithelial-to-Mesenchymal Transition Induced by TGF-β1 in Renal Tubular Epithelial NRK-52E Cells via Inhibiting Egr-1. J. Diabetes Res. 2018, 2018, 1031367. [Google Scholar] [CrossRef]
- Sun, Q.; Dai, Y.; Zhang, X.; Hu, Y.C.; Zhang, D.; Li, W.; Zhang, X.S.; Zhu, J.H.; Zhou, M.L.; Hang, C.H. Expression and cell distribution of myeloid differentiation primary response protein 88 in the cerebral cortex following experimental subarachnoid hemorrhage in rats: A pilot study. Brain Res. 2013, 1520, 134–144. [Google Scholar] [CrossRef]
- Wang, Y.; Shan, Q.; Meng, Y.; Pan, J.; Yi, S. Mrpl10 and Tbp Are Suitable Reference Genes for Peripheral Nerve Crush Injury. Int. J. Mol. Sci. 2017, 18, 263. [Google Scholar] [CrossRef] [Green Version]

| Gene Symbol | CGRP vs. Control | Min + CGRP vs. Control | CGRP vs. Min + CGRP | |||
|---|---|---|---|---|---|---|
| Fold Regulation | p-Value | Fold Regulation | p-Value | Fold Regulation | p-Value | |
| Angiotensinogen (Agt) | 4.53 | 0.00507 | 1.68 | 0.3879 | 2.7 | 0.028231 |
| Heme oxygenase (decycling) 1 (Hmox1) | 3.23 | 0.00524 | 3.65 | 0.00207 | −1.13 | 0.353707 |
| Inhibitor of kappa light polypeptide gene enhancer in B-cells, kinase epsilon (Ikbke) | 2.08 | 0.00939 | 1.42 | 0.13566 | 1.47 | 0.032139 |
| Inhibitor of kappa light polypeptide gene enhancer in B-cells, kinase beta (Ikbkb) | 1.75 | 0.01188 | 1.45 | 0.10942 | 1.21 | 0.303584 |
| PC4 and SFRS1 interacting protein 1 (Psip1) | 2.14 | 0.01558 | 1.46 | 0.13784 | 1.47 | 0.010853 |
| V-rel avian reticuloendotheliosis viral oncogene homolog (Rel) | 1.81 | 0.01719 | 1.23 | 0.35578 | 1.47 | 0.007833 |
| Interleukin-1 receptor-associated kinase 4 (Irak4) | 1.88 | 0.01835 | 1.8 | 0.04689 | 1.05 | 0.842815 |
| Tumor necrosis factor receptor superfamily, member 1a (Tnfrsf1a) | 1.9 | 0.02122 | 1.7 | 0.0305 | 1.12 | 0.419134 |
| TNFRSF1A-associated via death domain (Tradd) | 1.73 | 0.02449 | 1.69 | 0.02557 | 1.03 | 0.841517 |
| Interleukin-1 receptor-associated kinase 1 (Irak1) | 1.8 | 0.02899 | 1.76 | 0.01546 | 1.02 | 0.806749 |
| Eukaryotic translation initiation factor 2-alpha kinase 2 (Eif2ak2) | 2.22 | 0.03561 | 1.6 | 0.04048 | 1.39 | 0.079264 |
| (Myeloid differentiation primary response gene 88) Myd88 | 1.77 | 0.03856 | 1.36 | 0.21353 | 1.3 | 0.080385 |
| Inhibitor of kappa light polypeptide gene enhancer in B-cells, kinase gamma (Ikbkg) | 1.6 | 0.04495 | 1.41 | 0.13474 | 1.13 | 0.599914 |
| Caspase 8 (Casp8) | 1.73 | 0.04646 | 1.81 | 0.06508 | −1.04 | 0.721599 |
| V-rel reticuloendotheliosis viral oncogene homolog A (avian) (Rela) | 1.94 | 0.05081 | 1.63 | 0.18091 | 1.19 | 0.470757 |
| Epidermal growth factor receptor (Egfr) | 2.77 | 0.05516 | 2.06 | 0.18127 | 1.35 | 0.336574 |
| V-raf-leukemia viral oncogene 1 (Raf1) | 1.79 | 0.05592 | 1.67 | 0.10164 | 1.08 | 0.732804 |
| TIMP metallopeptidase inhibitor 1 (Timp1) | 1.5 | 0.05971 | 1.69 | 0.00688 | −1.12 | 0.266271 |
| CREB binding protein (Crebbp) | 1.76 | 0.06267 | 1.8 | 0.12331 | −1.02 | 0.782512 |
| Receptor (TNFRSF)-interacting serine-threonine kinase 1 (Ripk1) | 1.92 | 0.06956 | 1.99 | 0.04171 | −1.03 | 0.84311 |
| Tnf receptor-associated factor 6 (Traf6) | 1.52 | 0.07076 | 1.57 | 0.06166 | −1.03 | 0.772281 |
| Jun oncogene (Jun) | 1.66 | 0.09329 | 1.98 | 0.10892 | −1.2 | 0.407036 |
| Mitogen activated protein kinase 3 (Mapk3) | 1.53 | 0.09343 | 1.47 | 0.07564 | 1.04 | 0.771937 |
| Toll-like receptor 4 (Tlr4) | 1.77 | 0.09811 | 1.42 | 0.36215 | 1.25 | 0.53273 |
| Interleukin 1 receptor, type I (Il1r1) | 2.07 | 0.1041 | 1.58 | 0.3264 | 1.31 | 0.200475 |
| Activating transcription factor 1 (Atf1) | 1.87 | 0.10581 | 2.07 | 0.05969 | −1.11 | 0.50731 |
| Tnf receptor-associated factor 3 (Traf3) | 1.61 | 0.11009 | 1.26 | 0.43188 | 1.27 | 0.063863 |
| Tumor necrosis factor receptor superfamily, member 1b (Tnfrsf1b) | 1.99 | 0.11131 | 1.57 | 0.27579 | 1.27 | 0.062087 |
| Fas (TNFRSF6)-associated via death domain (Fadd) | 1.45 | 0.12247 | 1.07 | 0.771 | 1.35 | 0.178473 |
| Mitogen activated protein kinase kinase kinase 1 (Map3k1) | 1.63 | 0.12685 | 1.33 | 0.36626 | 1.23 | 0.198982 |
| Signal transducer and activator of transcription 1 (Stat1) | 1.57 | 0.13515 | 1.19 | 0.4605 | 1.32 | 0.189901 |
| Mitogen activated protein kinase kinase 3 (Map2k3) | 1.53 | 0.1407 | 1.43 | 0.12152 | 1.07 | 0.760551 |
| Toll-like receptor 3 (Tlr3) | 2.61 | 0.14249 | 1.77 | 0.49273 | 1.48 | 0.021363 |
| Nuclear factor of kappa light polypeptide gene enhancer in B-cells 1 (Nfkb1) | 1.62 | 0.1512 | 1.51 | 0.18631 | 1.07 | 0.608812 |
| Colony stimulating factor 1 (macrophage) (Csf1) | 1.6 | 0.15174 | 1.15 | 0.7453 | 1.39 | 0.034653 |
| Toll interacting protein (Tollip) | 2.42 | 0.17346 | 1.89 | 0.1088 | 1.28 | 0.408384 |
| Lymphotoxin alpha (TNF superfamily, member 1) (Ltbr) | 1.48 | 0.17467 | 2.39 | 0.00038 | −1.62 | 0.042208 |
| CASP8 and FADD-like apoptosis regulator (Cflar) | 1.6 | 0.17536 | 1.33 | 0.40881 | 1.2 | 0.183055 |
| Tumor necrosis factor receptor superfamily, member 10b (Tnfrsf10b) | 1.6 | 0.18011 | 2.1 | 0.08054 | −1.31 | 0.235267 |
| Conserved helix-loop-helix ubiquitous kinase (Chuk) | 1.56 | 0.18368 | 1.55 | 0.17499 | 1.01 | 0.970965 |
| B-cell CLL/lymphoma 3 (Bcl3) | 3.25 | 0.19355 | 2.21 | 0.50387 | 1.47 | 0.062677 |
| FBJ osteosarcoma oncogene (Fos) | 2.24 | 0.19478 | 2.69 | 0.06886 | −1.2 | 0.459281 |
| Interferon regulatory factor 1 (Irf1) | 1.83 | 0.19915 | 1.34 | 0.59688 | 1.37 | 0.085414 |
| SMAD family member 4 (Smad4) | 1.71 | 0.20071 | 1.69 | 0.1561 | 1.01 | 0.952726 |
| TANK-binding kinase 1 (Tbk1) | 1.71 | 0.20588 | 1.28 | 0.51904 | 1.33 | 0.146051 |
| Receptor-interacting serine-threonine kinase 2 (Ripk2) | 1.7 | 0.20951 | 1.81 | 0.13488 | −1.07 | 0.604089 |
| P300/CBP-associated factor (Kat2b) | 1.66 | 0.22458 | 1.54 | 0.21379 | 1.08 | 0.519346 |
| Tnf receptor-associated factor 2 (Traf2) | 1.32 | 0.23271 | 1.31 | 0.19467 | 1 | 0.993216 |
| V-akt murine thymoma viral oncogene homolog 1 (Akt1) | 1.23 | 0.24355 | 1.94 | 0.03025 | −1.57 | 0.071343 |
| Nuclear factor of kappa light polypeptide gene enhancer in B-cells inhibitor, alpha (Nfkbia) | 2.44 | 0.27856 | 1.4 | 0.98802 | 1.74 | 0.002189 |
| Intercellular adhesion molecule 1 (Icam1) | 1.57 | 0.30001 | 1.44 | 0.38205 | 1.08 | 0.716784 |
| Activating transcription factor 2 (Atf2) | 2.05 | 0.32496 | 1.87 | 0.36302 | 1.1 | 0.525649 |
| Toll-like receptor 6 (Tlr6) | 1.36 | 0.33783 | 1.11 | 0.79499 | 1.23 | 0.301466 |
| CD40 molecule, TNF receptor superfamily member 5 (Cd40) | 4.09 | 0.34993 | 2.55 | 0.95769 | 1.61 | 0.060072 |
| Fas ligand (TNF superfamily, member 6) (Faslg) | −8.17 | 0.37086 | −4 | 0.28782 | −2.04 | 0.346818 |
| Interleukin 1 alpha (Il1α) | −7.98 | 0.37275 | −15.36 | 0.28247 | 1.93 | 0.223631 |
| Similar to Tnf receptor-associated factor 1 (LOC687813) | 1.75 | 0.40218 | 1.56 | 0.50132 | 1.13 | 0.594782 |
| Interleukin-1 receptor-associated kinase 2 (Irak2) | 1.61 | 0.40882 | 1.18 | 0.90517 | 1.37 | 0.2152 |
| Toll-like receptor 9 (Tlr9) | −1.27 | 0.48708 | −1.9 | 0.14612 | 1.5 | 0.296125 |
| B-cell CLL/lymphoma 10 (Bcl10) | 1.76 | 0.49896 | 2.05 | 0.21512 | −1.16 | 0.352739 |
| Caspase recruitment domain family, member 10 (Card10) | 1.37 | 0.59587 | 2.02 | 0.05805 | −1.47 | 0.015496 |
| Bcl2-like 1 (Bcl2l1) | 1.46 | 0.61736 | 1.96 | 0.14253 | −1.34 | 0.059029 |
| Toll-like receptor 2 (Tlr2) | 1.71 | 0.64305 | 1.25 | 0.87114 | 1.37 | 0.24527 |
| Early growth response 1 (Egr1) | 1.65 | 0.6683 | 4.17 | 0.00864 | −2.53 | 0.007471 |
| Coagulation factor II (thrombin) receptor (F2r) | 1.15 | 0.70587 | −1.21 | 0.62531 | 1.39 | 0.324815 |
| Tumor necrosis factor (TNF superfamily, member 2) (Tnf) | 1.1 | 0.72791 | 1.37 | 0.85781 | −1.24 | 0.518336 |
| B-cell leukemia/lymphoma 2 related protein A1d (Bcl2a1) | 1.53 | 0.74497 | 1.15 | 0.49908 | 1.33 | 0.446459 |
| Caspase 1 (Casp1) | 1.72 | 0.75883 | 1.31 | 0.96179 | 1.31 | 0.469404 |
| Nuclear factor of kappa light polypeptide gene enhancer in B-cells 2, p49/p100 (Nfkb2) | 1.28 | 0.76734 | 1.74 | 0.29266 | −1.36 | 0.323335 |
| Interleukin 1 beta (Il1β) | 2.81 | 0.86644 | 1.55 | 0.43662 | 1.82 | 0.288445 |
| Chemokine (C-C motif) ligand 2 (Ccl2) | 2.42 | 0.92611 | −1.07 | 0.43466 | 2.59 | 0.011511 |
| Toll-like receptor 1 (Tlr1) | 1.45 | 0.94286 | 1.09 | 0.63331 | 1.33 | 0.266362 |
| Baculoviral IAP repeat-containing 3 (Birc3) | 1.56 | 0.99554 | 1.52 | 0.98963 | 1.03 | 0.983089 |
| ID | Sequence (5’-3’) |
|---|---|
| Akt F | CTTTATTGGCTACAAGGAACGG |
| Akt R | CAGTCTGAATGGCGGTGGT |
| Egr1 F | CCAGTGCCCACCTCTTACTC |
| Egr1 R | TGCAGACTGGAAGGTGCTG |
| Myd88 F | TTCTCCAACGCTGTCCTGTC |
| Myd88 R | AACTGAGATGTGTGCCCAGG |
| Tbp F | TGGGATTGTACCACAGCTCCA |
| Tbp R | CTCATGATGACTGCAGCAAACC |
| Antibody Name | Company | Dilution |
|---|---|---|
| Cleaved Caspase-3 | Cell-signalling technology (9664) | 1:800 |
| C-Fos | Enzolife (ALX-210-130-C100) | 1:20 |
| GFAP | Abcam (ab53554) | 1:500 |
| Alexa Fluor 488 | Abcam (ab150129) | 1:200 |
| Alexa Fluor 555 | Abcam (ab150074) | 1:200 |
| Alexa Fluor 488 | Thermo Fisher Scientific (A11008) | 1:200 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Afroz, S.; Arakaki, R.; Iwasa, T.; Waskitho, A.; Oshima, M.; Matsuka, Y. Role of CGRP in Neuroimmune Interaction via NF-κB Signaling Genes in Glial Cells of Trigeminal Ganglia. Int. J. Mol. Sci. 2020, 21, 6005. https://doi.org/10.3390/ijms21176005
Afroz S, Arakaki R, Iwasa T, Waskitho A, Oshima M, Matsuka Y. Role of CGRP in Neuroimmune Interaction via NF-κB Signaling Genes in Glial Cells of Trigeminal Ganglia. International Journal of Molecular Sciences. 2020; 21(17):6005. https://doi.org/10.3390/ijms21176005
Chicago/Turabian StyleAfroz, Shaista, Rieko Arakaki, Takuma Iwasa, Arief Waskitho, Masamitsu Oshima, and Yoshizo Matsuka. 2020. "Role of CGRP in Neuroimmune Interaction via NF-κB Signaling Genes in Glial Cells of Trigeminal Ganglia" International Journal of Molecular Sciences 21, no. 17: 6005. https://doi.org/10.3390/ijms21176005





