Risk and Resilience Variants in the Retinoic Acid Metabolic and Developmental Pathways Associated with Risk of FASD Outcomes
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Whole Exome Sequencing
2.3. Candidate Gene Lists
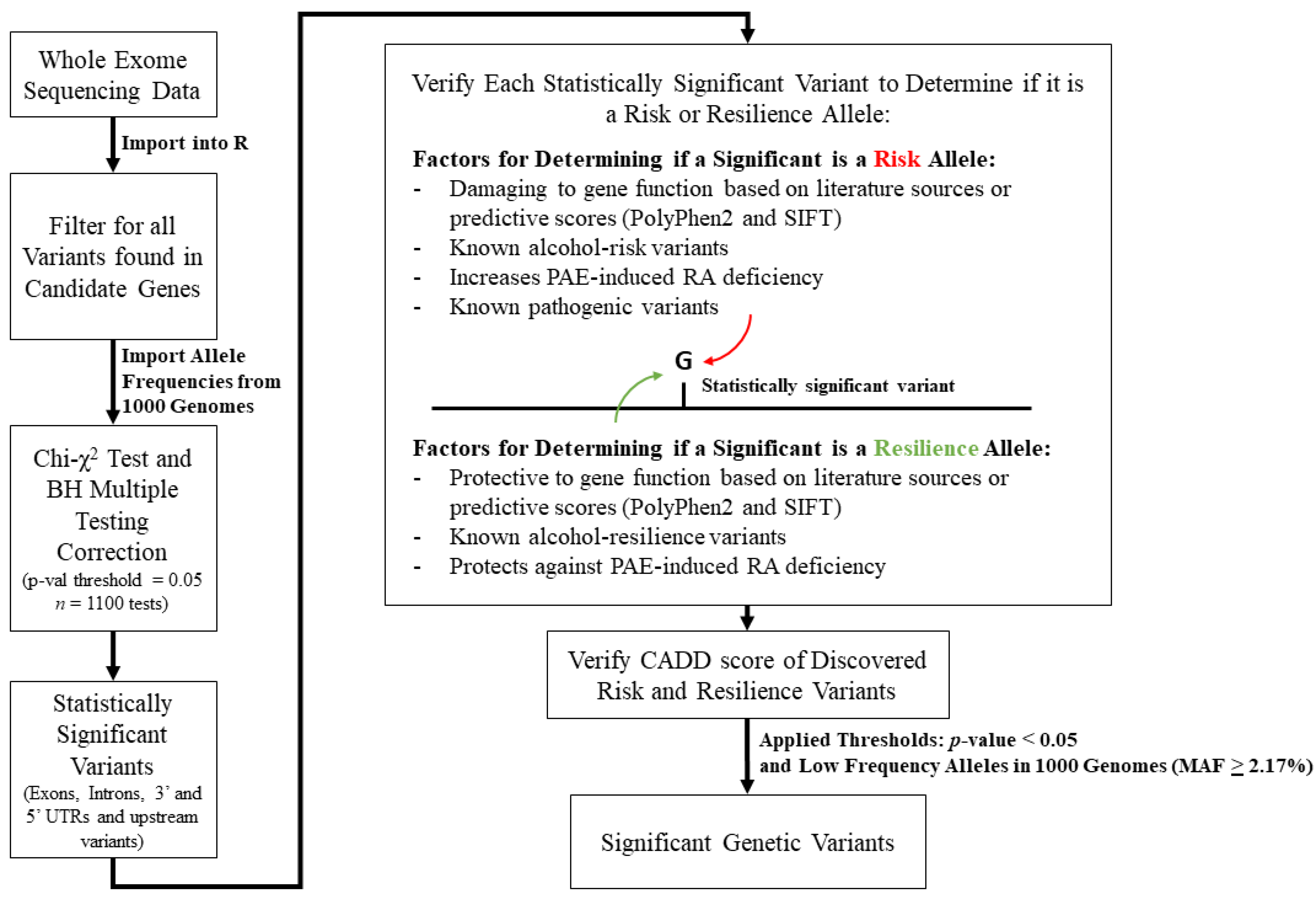
2.4. Variant Analysis of Whole Exome Sequencing Data Using Candidate Gene Approaches
2.5. TaqMan SNP Genotyping Assays
2.6. Determining Differences between FASD Diagnostic Groups and Pathway Analysis
3. Results
3.1. The FASD-Diagnosed Cohort Has Increased Frequencies of RA and Alcohol Metabolism Gene Variants Known to Be Associated with FASD and Alcoholism
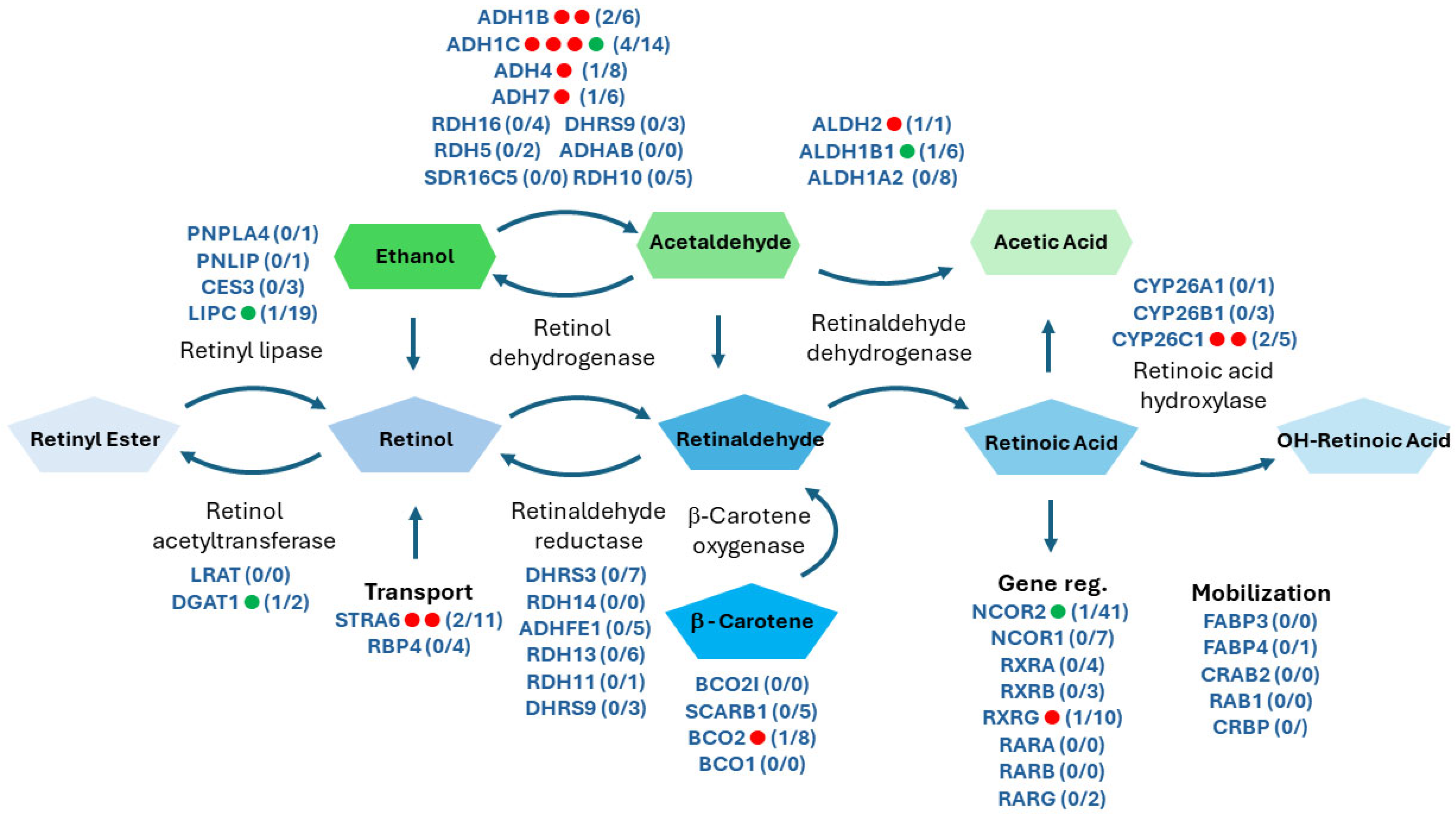
3.2. The FASD Cohort Is Enriched in Both Risk and Resilience Variants in Retinoic Acid-Regulated Developmental Pathways
3.3. The FASD Cohort Is Enriched in Risk Variants in the Causative Genes of Rare Neurodevelopmental Disorders
3.4. Determining Differences between FASD Diagnosis and Pathway Polygenic Risk Score Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Popova, S.; Lange, S.; Poznyak, V.; Chudley, A.E.; Shield, K.D.; Reynolds, J.N.; Murray, M.; Rehm, J. Population-Based Prevalence of Fetal Alcohol Spectrum Disorder in Canada. BMC Public Health 2019, 19, 845. [Google Scholar] [CrossRef] [PubMed]
- Cook, J.L.; Green, C.R.; Lilley, C.M.; Anderson, S.M.; Baldwin, M.E.; Chudley, A.E.; Conry, J.L.; Leblanc, N.; Loock, C.A.; Lutke, J.; et al. Fetal Alcohol Spectrum Disorder: A Guideline for Diagnosis across the Lifespan. Can. Med Assoc. J. 2016, 188, 191–197. [Google Scholar] [CrossRef] [PubMed]
- Chasnoff, I.J.; Wells, A.M.; King, L. Misdiagnosis and Missed Diagnoses in Foster and Adopted Children with Prenatal Alcohol Exposure. Pediatrics 2015, 135, 264–270. [Google Scholar] [CrossRef] [PubMed]
- Bonthius, D.J.; Goodlett, C.R.; West, J.R. Blood Alcohol Concentration and Severity of Microencephaly in Neonatal Rats Depend on the Pattern of Alcohol Administration. Alcohol 1988, 5, 209–214. [Google Scholar] [CrossRef] [PubMed]
- Pierce, D.R.; West, J.R. Alcohol-Induced Microencephaly during the Third Trimester Equivalent: Relationship to Dose and Blood Alcohol Concentration. Alcohol 1986, 3, 185–191. [Google Scholar] [CrossRef] [PubMed]
- Parnell, S.; Holloway, H.T.; O’Leary-Moore, S.K.; Dehart, D.B.; Paniaqua, B.; Oguz, I.; Budin, F.; Styner, M.A.; Johnson, G.A.; Sulik, K.K. Magnetic Resonance Microscopy-Based Analyses of the Neuroanatomical Effects of Gestational Day 9 Ethanol Exposure in Mice. Neurotoxicol. Teratol. 2013, 39, 77–83. [Google Scholar] [CrossRef]
- Godin, E.A.; O’Leary-Moore, S.K.; Khan, A.A.; Parnell, S.E.; Ament, J.J.; Dehart, D.B.; Johnson, B.W.; Allan Johnson, G.; Styner, M.A.; Sulik, K.K. Magnetic Resonance Microscopy Defines Ethanol-Induced Brain Abnormalities in Prenatal Mice: Effects of Acute Insult on Gestational Day 7. Alcohol. Clin. Exp. Res. 2010, 34, 98–111. [Google Scholar] [CrossRef]
- Parnell, S.E.; O’Leary-Moore, S.K.; Godin, E.A.; Dehart, D.B.; Johnson, B.W.; Allan Johnson, G.; Styner, M.A.; Sulik, K.K. Magnetic Resonance Microscopy Defines Ethanol-Induced Brain Abnormalities in Prenatal Mice: Effects of Acute Insult on Gestational Day 8. Alcohol. Clin. Exp. Res. 2009, 33, 1001–1011. [Google Scholar] [CrossRef] [PubMed]
- Anthony, B.; Vinci-Booher, S.; Wetherill, L.; Ward, R.; Goodlett, C.; Zhou, F.C. Alcohol-Induced Facial Dysmorphology in C57BL/6 Mouse Models of Fetal Alcohol Spectrum Disorder. Alcohol 2010, 44, 659–671. [Google Scholar] [CrossRef]
- Kaminen-ahola, N.; Fahey, P.; Cox, T.C.; Kaminen-ahola, N.; Ahola, A.; Maga, M.; Mallitt, K.; Fahey, P.; Cox, T.C. Maternal Ethanol Consumption Alters the Epigenotype and the Phenotype of Offspring in a Mouse Model Maternal Ethanol Consumption Alters the Epigenotype and the Phenotype of Offspring in a Mouse Model. PLoS ONE 2010, 6, e1000811. [Google Scholar] [CrossRef]
- Keen, C.; Uriu-Adams, J.Y.; Skalny, A.; Grabeklis, A.; Grabeklis, S.; Green, K.; Yevtushok, L.; Wertelecki, W.W.; Chambers, C.D. The Plausibility of Maternal Nutritional Status Being a Contributing Factor to the Risk for Fetal Alcohol Spectrum Disorders: The Potential Influence of Zinc Status as an Example. Biofactors 2010, 36, 125–135. [Google Scholar] [CrossRef]
- Burd, L.; Blair, J.; Dropps, K. Prenatal Alcohol Exposure, Blood Alcohol Concentrations and Alcohol Elimination Rates for the Mother, Fetus and Newborn. J. Perinatol. 2012, 32, 652–659. [Google Scholar] [CrossRef]
- Alberry, B.; Singh, S.M. Developmental and Behavioral Consequences of Early Life Maternal Separation Stress in a Mouse Model of Fetal Alcohol Spectrum Disorder. Behav. Brain Res. 2016, 308, 94–103. [Google Scholar] [CrossRef]
- Weinberg, J. Prenatal Ethanol Exposure Alters Adrenocortical Development of Offspring. Alcohol. Clin. Exp. Res. 1989, 13, 73–83. [Google Scholar] [CrossRef]
- Smith, S.M.; Garic, A.; Berres, M.E.; Flentke, G.R. Genomic Factors That Shape Craniofacial Outcome and Neural Crest Vulnerability in FASD. Front. Genet. 2014, 5, 224. [Google Scholar] [CrossRef] [PubMed]
- Hemingway, S.J.A.; Bledsoe, J.M.; Davies, J.K.; Brooks, A.; Jirikowic, T.; Olson, E.M.; Thorne, J.C. Twin Study Confirms Virtually Identical Prenatal Alcohol Exposures Can Lead to Markedly Different Fetal Alcohol Spectrum Disorder Outcomes- Fetal Genetics Influences Fetal Vulnerability. Adv. Pediatr. Res. 2018, 5, 23. [Google Scholar] [CrossRef]
- Bandoli, G.; Kable, J.A.; Coles, C.D.; del Campo, M.; Suttie, M.; Chambers, C.D. Trajectories of Prenatal Alcohol Exposure and Behavioral Outcomes: Findings from a Community-Based Sample. Drug Alcohol Depend. 2022, 233, 109351. [Google Scholar] [CrossRef] [PubMed]
- Petrelli, B.; Bendelac, L.; Hicks, G.G.; Fainsod, A. Insights into Retinoic Acid Deficiency and the Induction of Craniofacial Malformations and Microcephaly in Fetal Alcohol Spectrum Disorder. Genesis 2019, 57, e23278. [Google Scholar] [CrossRef] [PubMed]
- Marrs, J.A.; Clendenon, S.G.; Ratcliffe, D.R.; Fielding, S.M.; Liu, Q.; Bosron, W.F. Zebrafish Fetal Alcohol Syndrome Model: Effects of Ethanol Are Rescued by Retinoic Acid Supplement. Alcohol 2010, 44, 707–715. [Google Scholar] [CrossRef]
- McKay, L.; Petrelli, B.; Chudley, A.E.; Hicks, G.G. Genetics of FASD: Confounding Rare Craniofacial and Neurodevelopmental Disorders May Identify Ethanol-Sensitizing Genetic Variants of FASD. In Neuromethods; Chudley, A., Geoffrey, H., Eds.; Humana Press Inc.: Totowa, NJ, USA, 2022; Volume 188, pp. 77–117. [Google Scholar]
- Yelin, R.; Schyr, R.B.H.; Kot, H.; Zins, S.; Frumkin, A.; Pillemer, G.; Fainsod, A. Ethanol Exposure Affects Gene Expression in the Embryonic Organizer and Reduces Retinoic Acid Levels. Dev. Biol. 2005, 279, 193–204. [Google Scholar] [CrossRef]
- Reynolds, J.N.; Weinberg, J.; Clarren, S.; Beaulieu, C.; Rasmussen, C.; Kobor, M.; Dube, M.P.; Goldowitz, D. Fetal Alcohol Spectrum Disorders: Gene-Environment Interactions, Predictive Biomarkers, and the Relationship Between Structural Alterations in the Brain and Functional Outcomes. Semin. Pediatr. Neurol. 2011, 18, 49–55. [Google Scholar] [CrossRef] [PubMed]
- Portales-Casamar, E.; Lussier, A.A.; Jones, M.J.; MacIsaac, J.L.; Edgar, R.D.; Mah, S.M.; Barhdadi, A.; Provost, S.; Lemieux-Perreault, L.P.; Cynader, M.S.; et al. DNA Methylation Signature of Human Fetal Alcohol Spectrum Disorder. Epigenet. Chromatin 2016, 9, 25. [Google Scholar] [CrossRef] [PubMed]
- Homer, N.; Merriman, B.; Nelson, S.F. BFAST: An Alignment Tool for Large Scale Genome Resequencing. PLoS ONE 2009, 4, e7767. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Durbin, R. Fast and Accurate Short Read Alignment with Burrows-Wheeler Transform. Bioinformatics 2009, 25, 1754–1760. [Google Scholar] [CrossRef] [PubMed]
- Broad Institute. Available online: https://gatk.broadinstitute.org/hc/en-us/articles/360046222751-MarkDuplicates-Picard (accessed on 15 January 2021).
- Homer, N.; Nelson, S.F. Improved Variant Discovery through Local Re-Alignment of Short-Read next-Generation Sequencing Data Using SRMA. Genome Biol. 2010, 11, R99. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Depristo, M.A.; Banks, E.; Poplin, R.; Garimella, K.V.; Maguire, J.R.; Hartl, C.; Philippakis, A.A.; Del Angel, G.; Rivas, M.A.; Hanna, M.; et al. A Framework for Variation Discovery and Genotyping Using Next-Generation DNA Sequencing Data. Nat. Genet. 2011, 43, 491–501. [Google Scholar] [CrossRef] [PubMed]
- Adzhubei, I.A.; Schmidt, S.; Peshkin, L.; Ramensky, V.E.; Gerasimova, A.; Bork, P.; Kondrashov, A.S.; Sunyaev, S.R. A Method and Server for Predicting Damaging Missense Mutations. Nat. Methods 2010, 7, 248–249. [Google Scholar] [CrossRef]
- Ng, P.C.; Henikoff, S. Predicting Deleterious Amino Acid Substitutions. Genome Res. 2001, 11, 863–874. [Google Scholar] [CrossRef] [PubMed]
- Schubach, M.; Maass, T.; Nazaretyan, L.; Röner, S.; Kircher, M. CADD v1.7: Using Protein Language Models, Regulatory CNNs and Other Nucleotide-Level Scores to Improve Genome-Wide Variant Predictions. Nucleic Acids Res. 2024, 52, D1143–D1154. [Google Scholar] [CrossRef]
- Sambo, D.; Goldman, D. Genetic Influences on Fetal Alcohol Spectrum Disorder. Genes 2023, 14, 195. [Google Scholar] [CrossRef]
- Kot-Leibovich, H.; Fainsod, A. Ethanol Induces Embryonic Malformations by Competing for Retinaldehyde Dehydrogenase Activity during Vertebrate Gastrulation. Dis. Model. Mech. 2009, 2, 295–305. [Google Scholar] [CrossRef] [PubMed]
- Petrelli, B.; Oztürk, A.; Pind, M.; Ayele, H.; Fainsod, A.; Hicks, G.G. Genetically Programmed Retinoic Acid Deficiency during Gastrulation Phenocopies Most Known Developmental Defects Due to Acute Prenatal Alcohol Exposure in FASD. Front. Cell Dev. Biol. 2023, 11, 1208279. [Google Scholar] [CrossRef] [PubMed]
- McCarver, D.G.; Thomasson, H.R.; Martier, S.S.; Sokol, R.J.; Li, T. Alcohol Dehydrogenase-2*3 Allele Protects against Alcohol-Related Birth Defects among African Americans. J. Pharmacol. Exp. Ther. 1997, 283, 1095–1101. [Google Scholar] [PubMed]
- Viljoen, D.L.; Carr, L.G.; Foroud, T.M.; Brook, L.; Ramsay, M.; Li, T.K. Alcohol Dehydrogenase-2*2 Allele Is Associated with Decreased Prevalence of Fetal Alcohol Syndrome in the Mixed-Ancestry Population of the Western Cape Province, South Africa. Alcohol. Clin. Exp. Res. 2001, 25, 1719–1722. [Google Scholar] [CrossRef] [PubMed]
- Cleveland, H.H.; Schlomer, G.L.; Vandenbergh, D.J.; Wolf, P.S.A.; Feinberg, M.E.; Greenberg, M.T.; Spoth, R.L.; Redmond, C. Associations between Alcohol Dehydrogenase Genes and Alcohol Use across Early and Middle Adolescence: Moderation × Preventive Intervention. Dev. Psychopathol. 2018, 30, 297–313. [Google Scholar] [CrossRef] [PubMed]
- Meyers, J.L.; Shmulewitz, D.; Aharonovich, E.; Waxman, R.; Frisch, A.; Weizman, A.; Spivak, B.; Edenberg, H.J.; Gelernter, J.; Hasin, D.S. Alcohol-Metabolizing Genes and Alcohol Phenotypes in an Israeli Household Sample. Alcohol. Clin. Exp. Res. 2013, 37, 1872–1881. [Google Scholar] [CrossRef][Green Version]
- Edenberg, H.J.; Xuei, X.; Chen, H.J.; Tian, H.; Wetherill, L.F.; Dick, D.M.; Almasy, L.; Bierut, L.; Bucholz, K.K.; Goate, A.; et al. Association of Alcohol Dehydrogenase Genes with Alcohol Dependence: A Comprehensive Analysis. Hum. Mol. Genet. 2006, 15, 1539–1549. [Google Scholar] [CrossRef] [PubMed]
- Edenberg, H.J.; McClintick, J.N. Alcohol Dehydrogenases, Aldehyde Dehydrogenases, and Alcohol Use Disorders: A Critical Review. Alcohol. Clin. Exp. Res. 2018, 42, 2281–2297. [Google Scholar] [CrossRef]
- Yu, X.; Song, L.; Zheng, H.; Wei, S.; Wen, X.; Huang, B.; Liu, D. Association between Functional Genetic Variants in Retinoid X Receptor—α/γ and the Risk of Gestational Diabetes Mellitus in a Southern Chinese Population. Biosci. Rep. 2021, 41, BSR20211338. [Google Scholar] [CrossRef]
- Golzio, C.; Martinovic-Bouriel, J.; Thomas, S.; Mougou-Zrelli, S.; Grattagliano-Bessières, B.; Bonnière, M.; Delahaye, S.; Munnich, A.; Encha-Razavi, F.; Lyonnet, S.; et al. Matthew-Wood Syndrome Is Caused by Truncating Mutations in the Retinol-Binding Protein Receptor Gene STRA6. Am. J. Hum. Genet. 2007, 80, 1179–1187. [Google Scholar] [CrossRef]
- Parihar, M.; Bendelac-Kapon, L.; Gur, M.; Abbou, T.; Belorkar, A.; Achanta, S.; Kinberg, K.; Vadigepalli, R.; Fainsod, A. Retinoic Acid Fluctuation Activates an Uneven, Direction-Dependent Network-Wide Robustness Response in Early Embryogenesis. Front. Cell Dev. Biol. 2021, 9, 747969. [Google Scholar] [CrossRef]
- Noroozi, N.; Dastgheib, S.A.; Lookzadeh, M.H.; Mirjalili, S.R.; Noorishadkam, M.; Akbarian-Bafghi, M.J.; Neamatzadeh, H. Association of Axis Inhibition Protein 2 Polymorphisms with Non-Syndromic Cleft Lip with or without Cleft Palate in Iranian Children. Fetal Pediatr. Pathol. 2020, 39, 29–37. [Google Scholar] [CrossRef]
- Calvano, E.; Caio, K.; Bitencourt, L.; Julia, R.; Scariot, R.; Ricardo, P.N.; Olimpio, A.; Mírian, P.; Nakane, A.; Peter, M.; et al. Potential Interactions among Single Nucleotide Polymorphisms in Bone- and Cartilage-Related Genes in Skeletal Malocclusions. Orthod. Craniofacial Res. 2021, 24, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Hao, J.; Gao, R.; Wu, W.; Hua, L.; Chen, Y.; Li, F.; Liu, J. Association between BMP4 Gene Polymorphisms and Cleft Lip with or without Cleft Palate in a Population from South China. Arch. Oral. Biol. 2018, 93, 95–99. [Google Scholar] [CrossRef]
- Rafighdoost, H.; Hashemi, M.; Danesh, H.; Bizhani, F.; Bahari, G.; Taheri, M. Association of Single Nucleotide and IRF6 with Non-Syndromic Cleft Lip with or without Cleft Palate in a Sample of the Southeast Iranian Population. J. Appl. Oral. Sci. 2017, 25, 650–656. [Google Scholar] [CrossRef][Green Version]
- Han, X.; Xiong, X.; Shi, X.; Chen, F.; Li, Y. Targeted Sequencing of NOTCH Signaling Pathway Genes and Association Analysis of Variants Correlated with Mandibular Prognathism. Head Face Med. 2021, 17, 17. [Google Scholar] [CrossRef] [PubMed]
- Carter, T.C.; Molloy, A.M.; Pangilinan, F.; Troendle, J.F.; Kirke, P.N.; Conley, M.R.; Orr, D.J.A.; Earley, M.; Mckiernan, E.; Lynn, E.C.; et al. Testing Reported Associations of Genetic Risk Factors for Oral Clefts in a Large Irish Study Population. Birth Defects Res. (Part A) 2010, 93, 84–93. [Google Scholar] [CrossRef]
- Ma, J.; Lin, K. A Novel Mutation of the PAX3 Gene in a Chinese Family with Waardenburg Syndrome Type I. Mol. Genet. Genom. Med. 2019, 7, e00798. [Google Scholar] [CrossRef] [PubMed]
- Saket, M.; Saliminejad, K.; Kamali, K.; Moghadam, F.A.; Anvar, N.E.; Khorram Khorshid, H.R.; Aghakhani, F.; Esmaeili, N.; Reza, H.; Khorshid, K. BMP2 and BMP4 Variations and Risk of Non-Syndromic Cleft Lip and Palate. Arch. Oral. Biol. 2016, 72, 134–137. [Google Scholar] [CrossRef]
- Crauciuc, G.A.; Iancu, M.; Olah, P.; Tripon, F.; Anciuc, M.; Gozar, L.; Togănel, R.; Bănescu, C. Significant Associations between AXIN1 Rs1805105, Rs12921862, Rs370681 Haplotypes and Variant Genotypes of AXIN2 Rs2240308 with Risk of Congenital Heart Defects. Int. J. Environ. Res. Public Health 2020, 17, 7671. [Google Scholar] [CrossRef]
- Lin, H.; Sinner, M.F.; Brody, J.A.; Arking, D.E.; Lunetta, K.L.; Rienstra, M.; Lubitz, S.A.; Magnani, J.W.; Sotoodehnia, N.; Mcknight, B.; et al. Targeted Sequencing in Candidate Genes for Atrial Fibrillation: The Cohorts for Heart and Aging Research in Genomic Epidemiology (CHARGE) Targeted Sequencing Study. Heart Rhythm. 2014, 11, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Milting, H.; Lukas, N.; Osterziel, K.; Peters, S.; Thieleczek, R.; Varsa, M. Composite Polymorphisms in the Ryanodine Receptor 2 Gene Associated with Arrhythmogenic Right Ventricular Cardiomyopathy. Cardiovasc. Res. 2006, 71, 496–505. [Google Scholar] [CrossRef] [PubMed]
- Hu, D.; Xiao, L.; Li, S.; Hu, S.; Sun, Y.; Wang, Y. Prediction of HF-Related Mortality Risk Using Genetic Risk Score Alone and in Combination With Traditional Risk Factors. Front. Cardiovasc. Med. 2021, 8, 634966. [Google Scholar] [CrossRef] [PubMed]
- Guan, W.; Zhang, J.; Chen, J. Connection of GLI1 Variants to Congenital Heart Disease Susceptibility. Medicine 2020, 99, e19868. [Google Scholar] [CrossRef] [PubMed]
- Yan, L.; Gao, R.; Liu, Y.; He, B.; Lv, S.; Hao, D. The Pathogenesis of Ossification of the Posterior Longitudinal Ligament. Aging Dis. 2017, 8, 570–582. [Google Scholar] [CrossRef] [PubMed]
- Zmuda, J.M.; Yerges, L.M.; Kammerer, C.M.; Cauley, J.A.; Wang, X.; Nestlerode, C.S.; Wheeler, V.W.; Patrick, A.L.; Bunker, C.H.; Moffett, S.P.; et al. Association Analysis of WNT10B With Bone Mass and Structure Among Individuals of African Ancestry. J. Bone Miner. Res. 2009, 24, 437–447. [Google Scholar] [CrossRef]
- Zheng, H.; Tobias, J.H.; Duncan, E.; Evans, D.M.; Eriksson, J.; Bergstro, U.; Paternoster, L.; Yerges-armstrong, L.M.; Lehtima, T.; Goltzman, D.; et al. WNT16 Influences Bone Mineral Density, Cortical Bone, Bone Strength, and Osteoporotic Fracture Risk. PLoS ONE 2012, 8, e1002745. [Google Scholar] [CrossRef] [PubMed]
- Zhou, H.; Mori, S.; Ishizaki, T.; Takahashi, A.; Matsuda, K.; Koretsune, Y. Bone Reports Genetic Risk Score Based on the Prevalence of Vertebral Fracture in Japanese Women with Osteoporosis. Bone Rep. 2016, 5, 168–172. [Google Scholar] [CrossRef] [PubMed]
- David, D.; Marques, B.; Ferreira, C.; Vieira, P.; Corona-Rivera, A.; Ferreira, J.C.; Van Bokhoven, H. Characterization of Two Ectrodactyly-Associated Breakpoints Separated by 2.5Mb on chromosome 2q14.1–Q14.2. Eur. J. Hum. Genet. 2009, 17, 1024–1033. [Google Scholar] [CrossRef]
- Ma, W.; Li, Y.; Wang, M.; Li, H.; Su, T.; Li, Y.; Wang, S. Associations of Polymorphisms in WNT9B and PBX1 with Mayer-Rokitansky-Küster- Hauser Syndrome in Chinese Han. PLoS ONE 2015, 10, e0130202. [Google Scholar] [CrossRef][Green Version]
- Vlachakis, D.; Tsaniras, S.C.; Ioannidou, K.; Papageorgiou, L.; Baumann, M.; Kossida, S. A Series of Notch3 Mutations in CADASIL.; Insights from 3D Molecular Modelling and Evolutionary Analyses. J. Mol. Biochem. 2019, 3, 134. [Google Scholar]
- Toomey, S.; Madden, S.F.; Furney, S.J.; Fan, Y.; Mccormack, M.; Stapleton, C.; Cremona, M.; Cavalleri, G.L.; Milewska, M.; Elster, N.; et al. The Impact of ERBB-Family Germline Single Nucleotide Polymorphisms on Survival Response to Adjuvant Trastuzumab Treatment in HER2-Positive Breast Cancer. Oncotarget 2016, 7, 75518–75525. [Google Scholar] [CrossRef]
- Martin, L.J.; Smith, S.B.; Khoutorsky, A.; Magnussen, C.A.; Samoshkin, A.; Sorge, R.E.; Cho, C.; Yosefpour, N.; Sivaselvachandran, S.; Tohyama, S.; et al. Epiregulin and EGFR Interactions Are Involved in Pain Processing. J. Clin. Investig. 2017, 127, 3353–3366. [Google Scholar] [CrossRef] [PubMed]
- Matsushita, M.; Kitoh, H.; Kaneko, H.; Mishima, K.; Kadono, I.; Ishiguro, N.; Nishimura, G. A Novel SOX9 H169Q Mutation in a Family With Overlapping Phenotype of Mild Campomelic Dysplasia and Small Patella Syndrome. Am. J. Med. Genet. Part A 2013, 161, 2528–2534. [Google Scholar] [CrossRef]
- Munshi, A.; Khetarpal, P.; Das, S. Apert’s Syndrome: Study by Whole Exome Sequencing. Genes. Dis. 2018, 5, 119–122. [Google Scholar] [CrossRef] [PubMed]
- Nowaczyk, M.; Wassif, C. Smith-Lemli-Opitz Syndrome; Adam, M., Ardinger, H., Pagon, R.A., Eds.; GeneReviews: Seattle, WA, USA, 2024. [Google Scholar]
- Barboza-Cerda, M.C.; Barboza-Quintana, O.; Martínez-Aldape, G.; Garza-Guajardo, R.; Déctor, M.A. Phenotypic Severity in a Family with MEND Syndrome Is Directly Associated with the Accumulation of Potentially Functional Variants of Cholesterol Homeostasis Genes. Mol. Genet. Genomic Med. 2019, 7, e931. [Google Scholar] [CrossRef] [PubMed]
- Irving, M.; Holder-Espinasse, M. Three M Syndrome; Adam, M., Feldman, J., Mirzaa, G., Eds.; GeneReviews: Seattle, WA, USA, 2019. [Google Scholar]
- Park, J.E.; Lee, T.; Ha, K.; Ki, C.S. Carrier Frequency and Incidence Estimation of Smith—Lemli—Opitz Syndrome in East Asian Populations by Genome Aggregation Database (GnomAD) Based Analysis. Orphanet. J. Rare Dis. 2021, 16, 166. [Google Scholar] [CrossRef] [PubMed]
- Kranzler, H.R.; Zhou, H.; Kember, R.L.; Smith, R.V.; Justice, A.C.; Damrauer, S.; Tsao, P.S.; Klarin, D.; Baras, A.; Reid, J.; et al. Genome-Wide Association Study of Alcohol Consumption and Use Disorder in 274,424 Individuals from Multiple Populations. Nat. Commun. 2019, 10, 1499. [Google Scholar] [CrossRef] [PubMed]
- Gelernter, J.; Kranzler, H.R.; Sherva, R.; Almasy, L.; Koesterer, R.; Smith, A.H.; Anton, R.; Preuss, U.W.; Ridinger, M.; Rujescu, D. Genome-Wide Association Study of Alcohol Dependence: Significant Findings in African- and European-Americans Including Novel Risk Loci. Mol. Psychiatry 2014, 19, 41–49. [Google Scholar] [CrossRef]
- Luo, X.; Kranzler, H.R.; Zuo, L.; Wang, S.; Schork, N.J.; Gelernter, J. Multiple ADH Genes Modulate Risk for Drug Dependence in Both African- and European-Americans. Hum. Mol. Genet. 2007, 16, 380–390. [Google Scholar] [CrossRef]
- Bjerregaard, P.; Mikkelsen, S.S.; Becker, U.; Hansen, T.; Tolstrup, J.S. Genetic Variation in Alcohol Metabolizing Enzymes among Inuit and Its Relation to Drinking Patterns. Drug Alcohol Depend. 2014, 144, 239–244. [Google Scholar] [CrossRef] [PubMed]
- Shabtai, Y.; Bendelac, L.; Jubran, H.; Hirschberg, J.; Fainsod, A. Acetaldehyde Inhibits Retinoic Acid Biosynthesis to Mediate Alcohol Teratogenicity. Sci. Rep. 2018, 8, 347. [Google Scholar] [CrossRef] [PubMed]
- Shabtai, Y.; Fainsod, A. Competition between Ethanol Clearance and Retinoic Acid Biosynthesis in the Induction of Fetal Alcohol Syndrome. Biochem. Cell Biol. 2018, 96, 148–160. [Google Scholar] [CrossRef] [PubMed]
- Ribes, V.; Wang, Z.; Dollé, P.; Niederreither, K. Retinaldehyde Dehydrogenase 2 (RALDH2)-Mediated Retinoic Acid Synthesis Regulates Early Mouse Embryonic Forebrain Development by Controlling FGF and Sonic Hedgehog Signaling. Development 2006, 133, 351–361. [Google Scholar] [CrossRef] [PubMed]
- Bailey, B.A.; Sokol, R.J. Preterm Delivery, and Sudden Infant Death Syndrome. Alcohol Res. Health 2011, 34, 86–91. [Google Scholar] [PubMed]
- Kietzman, H.W.; Everson, J.L.; Sulik, K.K.; Lipinski, R.J. The Teratogenic Effects of Prenatal Ethanol Exposure Are Exacerbated by Sonic Hedgehog or Gli2 Haploinsufficiency in the Mouse. PLoS ONE 2014, 9, e89448. [Google Scholar] [CrossRef] [PubMed]
- Sambo, D.; Gohel, C.; Yuan, Q.; Sukumar, G.; Alba, C.; Dalgard, C.L.; Goldman, D. Cell Type-Specific Changes in Wnt Signaling and Neuronal Differentiation in the Developing Mouse Cortex after Prenatal Alcohol Exposure during Neurogenesis. Front. Cell Dev. Biol. 2022, 10, 1011974. [Google Scholar] [CrossRef] [PubMed]
- Niederreither, K.; Dollé, P. Retinoic Acid in Development: Towards an Integrated View. Nat. Rev. Genet. 2008, 9, 541–553. [Google Scholar] [CrossRef] [PubMed]
- Edenberg, H.J. The Genetics of Alcohol Metabolism: Role of Alcohol Dehydrogenase and Aldehyde Dehydrogenase Variants. Alcohol Res. Health 2007, 30, 5–13. [Google Scholar]
- Bierut, L.J.; Goate, A.M.; Breslau, N.; Johnson, E.O.; Bertelsen, S.; Fox, L.; Agrawal, A.; Bucholz, K.K.; Grucza, R.; Hesselbrock, V.; et al. ADH1B Is Associated with Alcohol Dependence and Alcohol Consumption in Populations of European and African Ancestry. Mol. Psychiatry 2012, 5, 445–450. [Google Scholar] [CrossRef]
- Warren, K.R.; Li, T.K. Genetic Polymorphisms: Impact on the Risk of Fetal Alcohol Spectrum Disorders. Birth Defects Res. A Clin. Mol. Teratol. 2005, 73, 195–203. [Google Scholar] [CrossRef]
- Hoang, Y.T.T.; Nguyen, Y.T.; Nguyen, H.D.; Le, A.T.P.; Bui, H.T.T.; Vu, N.P.; Nguyen, H.H. Single Nucleotide Polymorphisms of ADH1B, ADH1C and ALDH2 Genes in 235 People Living in Thai Nguyen Province of Vietnam. Asian Pac. J. Cancer Prev. 2022, 23, 4243–4251. [Google Scholar] [CrossRef] [PubMed]
- Luo, X.; Kranzler, H.R.; Zuo, L.; Yang, B.; Lappalainen, J.; Gelernter, J. ADH4 Gene Variation Is Associated with Alcohol and Drug Dependence: Results from Family Controlled and Population-Structured Association Studies. Pharmacogenet. Genom. 2005, 15, 755–768. [Google Scholar] [CrossRef]
- Luo, X.; Kranzler, H.R.; Zuo, L.; Wang, S.; Gelernter, J. Personality Traits of Agreeableness and Extraversion Are Associated with ADH4 Variation. Biol. Psychiatry 2007, 61, 599–608. [Google Scholar] [CrossRef]
- Pavan, M.; Ruiz, V.F.; Silva, F.A.; Sobreira, T.J.; Cravo, R.M.; Vasconcelos, M.; Marques, L.P.; Mesquita, S.M.F.; Krieger, J.E.; Lopes, A.A.B.; et al. ALDH1A2 (RALDH2) Genetic Variation in Human Congenital Heart Disease. BMC Med. Genet. 2009, 10, 113. [Google Scholar] [CrossRef] [PubMed]
- Deak, K.L.; Dickerson, M.E.; Linney, E.; Enterline, D.S.; George, T.M.; Melvin, E.C.; Graham, F.L.; Siegel, D.G.; Hammock, P.; Mehltretter, L.; et al. Analysis of ALDH1A2, CYP26A1, CYP26B1, CRABP1, and CRABP2 in Human Neural Tube Defects Suggests a Possible Association with Alleles in ALDH1A2. Birth Defects Res. A Clin. Mol. Teratol. 2005, 73, 868–875. [Google Scholar] [CrossRef] [PubMed]
- Li, K.; Zhong, Y.; Peng, Y.; Zhou, B.; Wang, Y.; Li, Q.; Zhang, Y.; Song, H.; Rao, L. Association Between AXIN1 Gene Polymorphisms and Dilated Cardiomyopathy in a Chinese Han Population. DNA Cell Biol. 2019, 38, 436–442. [Google Scholar] [CrossRef] [PubMed]
- Zhou, B.; Tang, T.; Chen, P.; Pu, Y.; Ma, M.; Zhang, D.; Li, L.; Zhang, P.; Song, Y.; Zhang, L. The Variations in the AXIN1 Gene and Susceptibility to Cryptorchidism. J. Pediatr. Urol. 2015, 11, 132.e1–132.e5. [Google Scholar] [CrossRef] [PubMed]
- Styrkarsdottir, U.; Thorleifsson, G.; Gudjonsson, S.A.; Sigurdsson, A.; Center, J.R.; Lee, S.H.; Nguyen, T.V.; Kwok, T.C.Y.; Lee, J.S.W.; Ho, S.C.; et al. Sequence Variants in the PTCH1 Gene Associate with Spine Bone Mineral Density and Osteoporotic Fractures. Nat. Commun. 2016, 7, 10129. [Google Scholar] [CrossRef]
- Callahan, N.; Modesto, A.; Meira, R.; Seymen, F.; Patir, A.; Vieira, A.R. Axis Inhibition Protein 2 (AXIN2) Polymorphisms and Tooth Agenesis. Arch. Oral. Biol. 2009, 54, 45–49. [Google Scholar] [CrossRef]
- Tian, T.; Lei, Y.; Chen, Y.; Karki, M.; Jin, L.; Finnell, R.H.; Wang, L.; Ren, A. Somatic Mutations in Planar Cell Polarity Genes in Neural Tissue from Human Fetuses with Neural Tube Defects. Hum. Genet. 2020, 139, 1299–1314. [Google Scholar] [CrossRef] [PubMed]
- Parmalee, N.L.; Schubert, C.; Merriam, J.E.; Allikmets, K.; Bird, A.C.; Gillies, M.C.; Peto, T.; Figueroa, M.; Friedlander, M.; Fruttiger, M.; et al. Analysis of Candidate Genes for Macular Telangiectasia Type 2. Mol. Vis. 2010, 16, 2718–2726. [Google Scholar] [PubMed]
- Lasabova, Z.; Stanclova, A.; Grendar, M.; Mikolajcikova, S.; Calkovska, A.; Lenhartova, N.; Ziak, P.; Matasova, K.; Caprnda, M.; Kruzliak, P.; et al. Genetic Association of Single Nucleotide Polymorphisms of FZD4 and BDNF Genes with Retinopathy of Prematurity. Ophthalmic Genet. 2018, 39, 332–337. [Google Scholar] [CrossRef] [PubMed]
- Magic, M.; Zeljic, K.; Jovandic, S.; Stepic, J.; Pejovic, M.; Colic, S.; Magic, Z.; Supic, G. Hedgehog Signaling Pathway and Vitamin D Receptor Gene Variants as Potential Risk Factors in Odontogenic Cystic Lesions. Clin. Oral. Investig. 2018, 23, 2675–2684. [Google Scholar] [CrossRef] [PubMed]
- Chang, J.; Wang, S.; Zheng, Z. Etiology of Hypospadias: A Comparative Review of Genetic Factors and Developmental Processes between Human and Animal Models. Res. Rep. Urol. 2020, 12, 673–686. [Google Scholar] [CrossRef] [PubMed]
- Renard, E.; Chéry, C.; Oussalah, A.; Josse, T.; Perrin, P.; Tramoy, D.; Voirin, J.; Klein, O.; Leheup, B.; Feillet, F.; et al. Exome Sequencing of Cases with Neural Tube Defects Identifies Candidate Genes Involved in One—Carbon/Vitamin B12 Metabolisms and Sonic Hedgehog Pathway. Hum. Genet. 2019, 138, 703–713. [Google Scholar] [CrossRef] [PubMed]
- Deneault, E.; Faheem, M.; White, S.H.; Rodrigues, D.C.; Sun, S.; Wei, W.; Piekna, A.; Thompson, T.; Howe, J.L.; Chalil, L.; et al. CNTN5-/+or EHMT2-/+human IPSC-Derived Neurons from Individuals with Autism Develop Hyperactive Neuronal Networks. Elife 2019, 8, e40092. [Google Scholar] [CrossRef] [PubMed]
- Pinard, A.; Eudes, N.; Mitchell, J.; Bajolle, F.; Grelet, M.; Okoronkwo, J.; Bonnet, D.; Collod, G.; Stéphane, B. Analysis of HOXB1 Gene in a Cohort of Patients with Sporadic Ventricular Septal Defect. Mol. Biol. Rep. 2018, 45, 1507–1513. [Google Scholar] [CrossRef] [PubMed]
- Dargis, N.; Lamontagne, M.; Gaudreault, N.; Sbarra, L.; Henry, C.; Pibarot, P.; Mathieu, P.; Bossé, Y. Identification of Gender-Specific Genetic Variants in Patients With Bicuspid Aortic Valve. Am. J. Cardiol. 2016, 117, 420–426. [Google Scholar] [CrossRef]
- Girdauskas, E.; Kaemmerer, H.; Kodolitsch, Y. Von Unravelling the Pathogenetic Mechanisms in Congenital Aortopathies: Need for an Integrative Translational Approach. J. Clin. Med. 2020, 9, 204. [Google Scholar] [CrossRef]
- Zhu, C.; Wang, Y.; Zeng, Q.; Qian, Y.; Li, H.; Yang, Z. Combined Effects of Age and Polymorphisms in Notch3 in the Pathogenesis of Cerebral Infarction Disease. Metab. Brain Dis. 2016, 31, 1157–1164. [Google Scholar] [CrossRef] [PubMed]
- Sowers, L.P.; Loo, L.; Wu, Y.; Campbell, E.; Ulrich, J.D.; Wu, S.; Paemka, L.; Wassink, T.; Meyer, K.; Bing, X.; et al. Disruption of the Non-Canonical Wnt Gene PRICKLE2 Leads to Autism-like Behaviors with Evidence for Hippocampal Synaptic Dysfunction. Mol. Psychiatry 2013, 18, 1077–1089. [Google Scholar] [CrossRef]
- Koop, A.; Goldmann, P.; Chen, S.R.W.; Thieleczek, R.; Varsa, M. ARVC-Related Mutations in Divergent Region 3 Alter Functional Properties of the Cardiac Ryanodine Receptor. Biophys. J. 2008, 94, 4668–4677. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Martin, P.; Yang, X.; Robin, N.; Lam, E.; Rabinowitz, J.S.; Erdman, C.A.; Quinn, J.; Weiss, L.A.; Hamilton, S.P.; Kwok, P.; et al. A Rare WNT1 Missense Variant Overrepresented in ASD Leads to Increased Wnt Signal Pathway Activation. Transl. Psychiatry 2013, 3, e301. [Google Scholar] [CrossRef]
- Christodoulides, C.; Scarda, A.; Granzotto, M.; Milan, G.; Dalla Nora, E.; Keogh, J.; De Pergola, G.; Stirling, H.; Pannacciulli, N.; Sethi, J.; et al. WNT10B Mutations in Human Obesity. Diabetologia 2006, 49, 678–684. [Google Scholar] [CrossRef]
- Mues, G.; Bonds, J.; Xiang, L.; Vieira, A.R.; Seymen, F.; Klein, O.; Souza, R.N.D. The WNT10A Gene in Ectodermal Dysplasias and Selective Tooth Agenesis. Am. J. Med. Genet. A 2014, 164, 2455–2460. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Jiang, L.; Yang, H.; Wu, L.; Xu, N.; Zhou, X.; Li, J. Variations of Wnt/Β-catenin Pathway-related Genes in Susceptibility to Knee Osteoarthritis: A Three-centre Case-control Study. J. Cell Mol. Med. 2019, 23, 8246–8257. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Liu, H.; Dong, Y. Significance of Neurexin and Neuroligin Polymorphisms in Regulating Risk of Hirschsprung’s Disease. J. Investig. Med. 2018, 66, 944–951. [Google Scholar] [CrossRef]
- Corsten-Janssen, N.; Saitta, S.C.; Hoefsloot, L.H.; McDonal-McGinn, D.M.; Driscoll, D.A.; Derks, R.; Dickinson, K.A.; Kerstjens-Frederiske, W.S.; Emanuel, B.S.; Zackai, E.H.; et al. More Clinical Overlap between 22q11 . 2 Deletion Syndrome and CHARGE Syndrome than Often Anticipated. Mol. Syndromol. 2013, 4, 235–245. [Google Scholar] [CrossRef]
- Cuola, D.; Li, Y.; Yuanyuan, C.; Jianghua, L.; Shuguang, W. Association Study of Catechol-o-Methyltransferase and Alpha-1-Adrenergic Receptor Gene Polymorphisms with Multiple Phenotypes of Heroin Use Disorder. Neurosci. Lett. 2021, 748, 135677. [Google Scholar] [CrossRef]
- Bender, H.-U.; Almashanu, S.; Steel, G.; Hu, C.-A.; Lin, W.-W.; Willis, A.; Pulver, A.; Valle, D. Functional Consequences of PRODH Missense Mutations. Am. J. Hum. Genet. 2005, 76, 409–420. [Google Scholar] [CrossRef]
- Clelland, C.L.; Drouet, V.; Rilett, K.C.; Smeed, J.A.; Nadrich, R.H.; Rajparia, A.; Read, L.L.; Clelland, J.D. Evidence That COMT Genotype and Proline Interact on Negative-Symptom Outcomes in Schizophrenia and Bipolar Disorder. Transl. Psychiatry 2016, 6, e891. [Google Scholar] [CrossRef] [PubMed]
- Mozzi, A.; Guerini, F.R.; Forni, D.; Costa, A.S.; Nemni, R.; Baglio, F.; Cabinio, M.; Riva, S.; Pontremoli, C.; Clerici, M.; et al. REST, a Master Regulator of Neurogenesis, Evolved under Strong Positive Selection in Humans and in Non Human Primates. Sci. Rep. 2017, 7, 9530. [Google Scholar] [CrossRef]
- Ravizza, T.; Onat, F.Y.; Brooks-Kayal, A.R.; Depaulis, A.; Galanopoulou, A.S.; Mazarati, A.; Numis, A.L.; Sankar, R.; Friedman, A. WONOEP Appraisal: Biomarkers of Epilepsy-Associated Comorbidities. Epilepsia 2017, 58, 331–342. [Google Scholar] [CrossRef]
- Xu, Y.; Wang, J.; Xu, R.; Zhao, P.; Wang, X.; Sun, H.; Bao, L.; Shen, J. Detecting 22q11.2 Deletion in Chinese Children with Conotruncal Heart Defects and Single Nucleotide Polymorphisms in the Haploid TBX1 Locus. BMC Med. Genet. 2011, 12, 169. [Google Scholar] [CrossRef] [PubMed]
- Akiyama, K.; Saito, A.; Saito, S.; Ozeki, Y.; Watanabe, T. Association of Genetic Variants at 22q11.2 Chromosomal Region with Cognitive Performance in Japanese Patients with Schizophrenia. Schizophr. Res. Cogn. 2019, 17, 100134. [Google Scholar] [CrossRef]
- Caputo, V.; Strafella, C.; Termine, A.; Campione, E. RNAseq-Based Prioritization Revealed COL6A5, COL8A1, COL10A1 and MIR146A as Common and Differential Susceptibility Biomarkers for Psoriasis and Psoriatic Arthritis: Confirmation from Genotyping Analysis of 1417 Italian Subjects. Int. J. Mol. Sci. 2020, 21, 2740. [Google Scholar] [CrossRef] [PubMed]
- Den Hollander, W.; Pulyakhina, I.; Boer, C.; Bomer, N.; Van Der Breggen, R.; Arindrarto, W.; De Almeida, R.C.; Lakenberg, N.; Sentner, T.; Laros, J.F.J.; et al. Annotating Transcriptional Effects of Genetic Variants in Disease-Relevant Tissue: Transcriptome-Wide Allelic Imbalance in Osteoarthritic Cartilage. Arthritis Rheumatol. 2019, 71, 561–570. [Google Scholar] [CrossRef] [PubMed]
- Trefilova, V.V.; Shnayder, N.A.; Petrova, M.M.; Kaskaeva, D.S.; Tutynina, O.V.; Petrov, K.V.; Popova, T.E.; Balberova, O.V.; Medvedev, G.V.; Nasyrova, R.F. The Role of Polymorphisms in Collagen-Encoding Genes in Intervertebral Disc Degeneration. Biomolecules 2021, 11, 1279. [Google Scholar] [CrossRef]
- Jamieson, S.E.; De Roubaix, L.; Cortina-borja, M.; Tan, H.K.; Mui, E.J.; Cordell, H.J.; Kirisits, M.J.; Miller, E.N.; Peacock, C.S.; Hargrave, A.C.; et al. Genetic and Epigenetic Factors at COL2A1 and ABCA4 Influence Clinical Outcome in Congenital Toxoplasmosis. Investig. Ophthalmol. Vis. Sci. 2008, 3, e2285. [Google Scholar] [CrossRef]
- Tang, Y.; Epstein, M.P.; Anderson, G.M.; Zabetian, C.P.; Cubells, J.F. Genotypic and Haplotypic Associations of the DBH Gene with Plasma Dopamine b -Hydroxylase Activity in African Americans. Eur. J. Hum. Genet. 2007, 15, 878–883. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Lopez, E.; Kawasawa-imamura, Y.; Zhang, L.; Huang, X.; Koltun, W.A.; Coates, M.D.; Vrana, K.E. A Single Nucleotide Polymorphism in Dopamine Beta Hydroxylase (Rs6271 (C > T)) Is over-Represented in Inflammatory Bowel Disease Patients and Reduces Circulating Enzyme. PLoS ONE 2019, 14, e0210175. [Google Scholar] [CrossRef] [PubMed]
- Punchaichira, T.J.; Dey, S.K.; Mukhopadhyay, A. Characterization of SNPs in the Dopamine-β-Hydroxylase Gene Providing New Insights into Its Structure-Function Relationship. Neurogenetics 2017, 18, 155–168. [Google Scholar] [CrossRef] [PubMed]
- Ates, O.; Cam, F.; Erdogan, S.; Sezer, S.; Karakus, N. Association between 1603C > T Polymorphism of DBH Gene and Bipolar Disorder in a Turkish Population. Gene 2013, 519, 356–359. [Google Scholar] [CrossRef] [PubMed]
- Kukshal, P.; Chowdari, V.; Srivastava, V.; Wood, J.; Mcclain, L.; Bhatia, T.; Bhagwat, A.M.; Neelkanth, S.; Laxmikant, V.; Thelma, B.K. Dopaminergic Gene Polymorphisms and Cognitive Function in a North Indian Schizophrenia Cohort. J. Psychiatr. Res. 2013, 47, 1615–1622. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yeung, E.W.; Craggs, J.G.; Gizer, I.R. Comorbidity of Alcohol Use Disorder and Chronic Pain: Genetic Influences on Brain Reward and Stress Systems. Alcohol. Clin. Exp. Res. 2017, 41, 1831–1848. [Google Scholar] [CrossRef] [PubMed]
- Meyers, J.L.; Nyman, E.; Loukola, A.; Rose, R.J.; Kaprio, J.; Dick, D.M. The Association between DRD2/ANKK1 and Genetically Informed Measures of Alcohol Use and Problems. Addict. Biol. 2013, 18, 523–536. [Google Scholar] [CrossRef] [PubMed]
- Franco, G.B.; Mara, F.; Bertoli, D.P.; De Souza, J.F.; Scariot, R. Dopamine Receptor D2 and Ankyrin Repeat Domain Containing One in Temporomandibular Disorder of Adolescents. Int. J. Paediatr. Dent. 2019, 29, 748–755. [Google Scholar] [CrossRef]
- Popescu, A.; Marian, M.; Drăgoi, A.N.A.M.; Costea, R.V. Understanding the Genetics and Neurobiological Pathways behind Addiction (Review). Exp. Ther. Med. 2021, 21, 544. [Google Scholar] [CrossRef]
- Lundwall, R.A.; Guo, D.; Dannemiller, J.L. Exogenous Visual Orienting Is Associated with Specific Neurotransmitter Genetic Markers: A Population-Based Genetic Association Study. PLoS ONE 2012, 7, e30731. [Google Scholar] [CrossRef]
- Kirley, A.; Lowe, N.; Mullins, C.; Mccarron, M.; Daly, G.; Waldman, I.; Fitzgerald, M.; Gill, M.; Hawi, Z. Phenotype Studies of the DRD4 Gene Polymorphisms in ADHD: Association With Oppositional Defiant Disorder and Positive Family History Analysis of Association With. Am. J. Med. Genet. Part B 2004, 131, 38–42. [Google Scholar] [CrossRef] [PubMed]
- Nemoda, Z.; Szekely, A.; Sasvari-szekely, M. Neuroscience and Biobehavioral Reviews Psychopathological Aspects of Dopaminergic Gene Polymorphisms in Adolescence and Young Adulthood. Neurosci. Biobehav. Rev. 2011, 35, 1665–1686. [Google Scholar] [CrossRef] [PubMed]
- Nakajima, M.; Hattori, E.; Yamada, K.; Iwayama, Y.; Toyota, T.; Iwata, Y.; Tsuchiya, K.; Sugihara, G.; Hashimoto, K.; Watanabe, H.; et al. Association and Synergistic Interaction between Promoter Variants of the DRD4 Gene in Japanese Schizophrenics. J. Hum. Genet. 2007, 52, 86–91. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wang, S.; Chen, Y.; Lee, C.; Cheng, C. Opioid Addiction, Genetic Susceptibility, and Medical Treatments: A Review. Int. J. Mol. Sci. 2019, 20, 4294. [Google Scholar] [CrossRef]
- Haenisch, B.; Linsel, K.; Br, M.; Gilsbach, R.; Propping, P.; Markus, M.N.; Rietschel, M.; Fimmers, R.; Maier, W.; Zobel, A.; et al. Association of Major Depression With Rare Functional Variants in Norepinephrine Transporter and Serotonin 1A Receptor Genes. Am. J. Med. Genet. Part B 2008, 150, 1013–1016. [Google Scholar] [CrossRef] [PubMed]
- Brüss, M.; Kostanian, A.; Bönisch, H.; Göthert, M. The Naturally Occurring Arg 219 Leu Variant of the Human 5-HT 1A Receptor: Impairment of Signal Transduction. Pharmacog. Genom. 2005, 15, 257–264. [Google Scholar] [CrossRef]
- Fanous, A.H.; Chen, X.; Wang, X.; Amdur, R.; O’Neill, A.; Walsh, D.; Kendler, K. Genetic Variation in the Serotonin 2A Receptor and Suicidal Ideation in a Sample of 270 Irish High-Density Schizophrenia Families. Am. J. Med. Genet. B Neuropsychiatr. Genet. 2009, 150, 411–417. [Google Scholar] [CrossRef]
- Tavares, G.A.; Torres, A.; Souza, J.A. De Early Life Stress and the Onset of Obesity: Proof of MicroRNAs ’ Involvement Through Modulation of Serotonin and Dopamine Systems’ Homeostasis. Front. Physiol. 2020, 11, 925. [Google Scholar] [CrossRef]
- Mccaffery, J.M.; Duan, Q.L.; Frasure-Smith, N.; Lespérance, F.; Théroux, P.; Rouleau, G.A.; Dubé, M.-P. Genetic Predictors of Depressive Symptoms in Cardiac Patients. Am. J. Med. Genet. B Neuropsychiatr. Genet. 2009, 150, 381–388. [Google Scholar] [CrossRef]
- Jakubczyk, A.; Klimkiewicz, A.; Kopera, M.; Krasowska, A.; Wrzosek, M.; Matsumoto, H.; Burmeister, M.; Brower, K.J.; Wojnar, M. The CC Genotype in the T102C HTR2A Polymorphism Predicts Relapse in Individuals after Alcohol Treatment. J. Psychiatr. Res. 2013, 47, 527–533. [Google Scholar] [CrossRef][Green Version]
- Jakubczyk, A.; Wrzosek, M.; Łukaszkiewicz, J.; Sadowska-Mazuryk, J.; Matsumoto, H.; Śliwerska, E.; Glass, J.; Burmeister, M.; Browser, K.J.; Wojnar, M. The CC Genotype in HTR2A T102C Polymorphism Is Associated with Behavioral Impulsivity in Alcohol-Dependent Patients. J. Psychiatr. Res. 2012, 46, 44–49. [Google Scholar] [CrossRef][Green Version]
- Cao, J.; Liu, X.; Han, S.; Zhang, C.K.; Liu, Z.; Li, D. Association of the HTR2A Gene with Alcohol and Heroin Abuse. Hum. Genet. 2014, 133, 357–365. [Google Scholar] [CrossRef]
- Sinopoli, V.M.; Burton, C.L.; Arnold, P.D. Neuroscience and Biobehavioral Reviews Review Article A Review of the Role of Serotonin System Genes in Obsessive-Compulsive Disorder. Neurosci. Biobehav. Rev. 2017, 80, 372–381. [Google Scholar] [CrossRef] [PubMed]
- Cheah, S.-Y.; Lawford, B.R.; Young, R.M.; Morris, C.P.; Voisey, J. MRNA Expression and DNA Methylation Analysis of Serotonin Receptor 2A (HTR2A) in the Human Schizophrenic Brain. Genes 2017, 8, 14. [Google Scholar] [CrossRef] [PubMed]
- Rappold, G.; Walstab, J.; Hammer, C.; Bo, H. Naturally Occurring Variants in the HTR3B Gene Significantly Alter Properties of Human Heteromeric 5-Hydroxytryptamine-3A/B Receptors. Pharmacog. Genom. 2008, 18, 793–802. [Google Scholar] [CrossRef]
- Yosifova, A.; Mushiroda, T.; Stoianov, D.; Vazharova, R.; Dimova, I.; Karachanak, S.; Zaharieva, I.; Milanova, V.; Madjirova, N.; Gerdjikov, I.; et al. Case-Control Association Study of 65 Candidate Genes Revealed a Possible Association of a SNP of HTR5A to Be a Factor Susceptible to Bipolar Disease in Bulgarian Population. J. Affect. Disord. 2009, 117, 87–97. [Google Scholar] [CrossRef] [PubMed]
- Stoychev, K.; Dilkov, D.; Naghavi, E.; Kamburova, Z. Genetic Basis of Dual Diagnosis: A Review of Genome-Wide Association Studies (GWAS) Focusing on Patients with Mood or Anxiety Disorders and Co-Occurring Alcohol-Use Disorders. Diagnostics 2021, 11, 1055. [Google Scholar] [CrossRef]
- Birkett, J.T.; Arranz, M.J.; Munro, J.; Osbourn, S.; Kerwin, R.W.; Collier, D.A. Association Analysis of the 5-HT5A Gene in Depression, Psychosis and Antipsychotic Response. Neuroreport 2000, 11, 2017–2020. [Google Scholar] [CrossRef]

| rsID | Gene | Type of Mutation | Risk Allele | Biological Impact of Variant | FASD Risk Allele Frequency | 1000 Gen. Risk Allele Frequency | p-Value |
|---|---|---|---|---|---|---|---|
| Known Alcohol Protective Alleles | |||||||
| rs1229984 * | ADH1B | Missense | C | More alcohol consumption | 0.96 | 0.82 | 1.70 × 10−2 |
| rs1614972 * | ADH1C | Intron | C | T variant is associated with reduced alcohol dependence | 0.93 | 0.48 | 5.61 × 10−9 |
| rs2066702 * | ADH1B | Missense | G | A variant oxidizes ethanol fast | 1.00 | 0.95 | 5.00 × 10−3 |
| rs3762894 * | ADH4 | Upstream | T | T allele is associated with less alcohol consumption | 0.91 | 0.68 | 4.00 × 10−3 |
| rs671 * | ALDH2 | Missense | G | G allele is associated with reduced alcohol consump. | 1.00 | 0.96 | 8.10 × 10−4 |
| Known Alcohol Sensitizing Alleles | |||||||
| rs2241894 | ADH1C | Silent | C | C allele is associated with alcohol dependence | 0.09 | 0.47 | 1.23 × 10−6 |
| rs698 * | ADH1C | Missense | C | C variant is 1.5 to 2-fold less kinetically active | 0.54 | 0.21 | 2.66 × 10−6 |
| rs1612735 | ADH1C | Intron | C | C allele is associated with alcohol dependence | 0.52 | 0.21 | 1.77 × 10−6 |
| rs971074 | ADH7 | Silent | T | T allele is associated with heroin addiction | 0.22 | 0.12 | 3.00 × 10−2 |
| rs2073478 | ALDH1B1 | Missense | G | TT genotype is protective against drinking | 0.41 | 0.61 | 3.00 × 10−2 |
| New Retinoic Acid Metabolizing Risk and Resilience Variants | |||||||
| rs2298753 * | ADH1C | 3′ UTR | C | VUS | 0.72 | 0.94 | 7.28 × 10−10 |
| rs10891338 | BCO2 | Missense | C | C allele probably has a damaging PolyPhen score | 1.00 | 0.97 | 2.20 × 10−4 |
| rs12263200 * | CYP26C1 | Intron | G | T allele has a damaging SIFT prediction | 0.80 | 0.88 | 1.00 × 10−3 |
| rs58993699 | CYP26C1 | Intron | C | T allele has a damaging SIFT prediction | 0.02 | 0.03 | 1.00 × 10−3 |
| rs55962377 | DGAT1 | Missense | T | T allele has a damaging PolyPhen score | 0.02 | 0.04 | 2.00 × 10−3 |
| rs3829462 | LIPC | Missense | A | A allele has a damaging PolyPhen score | 0.65 | 0.94 | 3.30 × 10−15 |
| rs2227277 | NCOR2 | Missense | C | T allele has damaging PolyPhen and SIFT scores | 0.07 | 0.06 | 3.00 × 10−2 |
| rs2134095 * | RXRG | Silent | A | A allele affects splicing: lower cholesterol and gest. diabetes | 0.72 | 0.48 | 2.80 × 10−3 |
| Variants in RA Metabolism Genes Associated with Congenital Malformations/Syndromes | |||||||
| rs971756 * | STRA6 | Missense | T | T variant damaging SIFT; Matthew–Wood syndrome | 0.13 | 0.05 | 2.00 × 10−3 |
| rs11857410 * | STRA6 | Silent | A | A allele in microphthalmia; Matthew–Wood syndrome | 0.13 | 0.06 | 5.00 × 10−3 |
| rsID | Gene | Type of Mutation | Risk Allele | Biological Impact of Variant | FASD Risk Allele Frequency | 1000 Gen. Risk Allele Frequency | p-Value | Risk or Resilience |
|---|---|---|---|---|---|---|---|---|
| Variants Found in Genes Regulated Directly by Retinoic Acid Signaling | ||||||||
| rs2240308 | AXIN2 (3) | Missense | A | Cryptorchidism and congenital heart disease | 0.65 | 0.34 | 3.64 × 10−5 | Risk |
| rs1049007 | BMP2 (2) | Silent | A | Ossification defects (ligament) | 0.47 | 0.25 | 1.70 × 10−3 | Risk |
| rs45498702 | CAV1 | 3′ UTR | T | T variant nominally associated with arterial fibrillation | 0.07 | 0.04 | 4.00 × 10−3 | Risk |
| rs1140475 | EGFR | Silent | C | C variant assoc. with temporomandibular disorder | 0.80 | 0.92 | 2.00 × 10−3 | Resilience |
| rs2592595 | GLI2 | Silent | A | A variant found in a study of ectrodactyly patients | 1.00 | 0.83 | 4.00 × 10−3 | Risk |
| rs1044006 | NOTCH3 | Silent | C | C variant: cerebral infarction, mandibular prognathism | 0.71 | 0.87 | 2.00 × 10−3 | Resilience |
| rs2066836 | PTCH1 | Silent | A | A variant: non-syndromic cleft lip and palate | 0.33 | 0.09 | 4.80 × 10−8 | Risk |
| rs139884 | SOX10 | Silent | G | G variant: Waardenburg Type I and II syndromes | 0.46 | 0.71 | 5.10 × 10−4 | Resilience |
| rs1051886 | WNT10B | Silent | A | A variant: hip bone mineral density | 0.52 | 0.31 | 7.00 × 10−3 | Risk |
| Variants Found in Genes Downstream of Retinoic Acid-Controlled Pathways | ||||||||
| rs8940 | CAV2 | Missense | G | G Variant has damaging PolyPhen and SIFT scores | 0.33 | 0.14 | 5.50 × 10−4 | Risk |
| rs1638630 | PTCHD3 | Missense | C | C Variant has damaging PolyPhen score | 0.04 | 0.03 | 7.31 × 10−5 | Resilience |
| rsID | Gene | Type of Mutation | Risk Allele | Syndrome and Comorbidity | FASD Risk Allele Frequency | 1000 Gen. Risk Allele Frequency | p-Value | Risk or Resilience |
|---|---|---|---|---|---|---|---|---|
| rs55975541 | CDC42BPG * | Missense | A | Aarskog | 0.11 | 0.03 | 3.66 × 10−6 | Risk |
| rs75659311 | FGD1 † | Missense | A | Aarskog | 0.04 | 0.02 | 4.48 × 10−5 | Risk |
| rs1047057 | FGFR2 * | Silent | G | Apert | 0.65 | 0.41 | 5.00 × 10−3 | Risk |
| rs2229989 | SOX9 * | Silent | T | Campomelic Dysplasia | 0.24 | 0.14 | 4.00 × 10−2 | Risk |
| rs80068543 | ARVCF * | Missense | T | 22q11.2 Deletion | 0.02 | 0.04 | 2.00 × 10−3 | Resilience |
| rs712952 | CLTCL1 † (2) | Missense | A | 22q11.2 Deletion | 0.11 | 0.05 | 3.30 × 10−3 | Risk |
| rs4819756 | PRODH | Missense | A | 22q11.2 Deletion | 0.54 | 0.22 | 5.20 × 10−7 | Risk |
| rs2277838 | P2RX6 | Missense | A | 22q11.2 Deletion | 0.13 | 0.08 | 3.50 × 10−2 | Resilience |
| rs2227902 | REST * | Missense | T | 22q11.2 Deletion | 0.09 | 0.07 | 3.60 × 10−2 | Risk |
| rs874100 | SCARF2 (3) | Missense | C | 22q11.2 Deletion | 0.04 | 0.24 | 5.00 × 10−3 | Resilience |
| rs5746826 | TBX1 * (2) | 3′ UTR | T | 22q11.2 Deletion | 0.30 | 0.59 | 4.00 × 10−4 | Risk |
| rs3747052 | TSSK2 | Missense | G | 22q11.2 Deletion | 0.02 | 0.04 | 2.90 × 10−3 | Resilience |
| rs2871053 | ZDHHC8 | Upstream | C | 22q11.2 Deletion | 0.07 | 0.05 | 1.40 × 10−2 | Risk |
| rs2230808 | ABCA1 | Missense | T | Smith–Lemli–Opitz | 0.76 | 0.58 | 1.00 × 10−2 | Risk |
| rs10932816 | OBSL1 | Silent | G | Smith–Lemli–Opitz | 1.00 | 0.96 | 8.90 × 10−4 | Risk |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
McKay, L.; Petrelli, B.; Pind, M.; Reynolds, J.N.; Wintle, R.F.; Chudley, A.E.; Drögemöller, B.; Fainsod, A.; Scherer, S.W.; Hanlon-Dearman, A.; et al. Risk and Resilience Variants in the Retinoic Acid Metabolic and Developmental Pathways Associated with Risk of FASD Outcomes. Biomolecules 2024, 14, 569. https://doi.org/10.3390/biom14050569
McKay L, Petrelli B, Pind M, Reynolds JN, Wintle RF, Chudley AE, Drögemöller B, Fainsod A, Scherer SW, Hanlon-Dearman A, et al. Risk and Resilience Variants in the Retinoic Acid Metabolic and Developmental Pathways Associated with Risk of FASD Outcomes. Biomolecules. 2024; 14(5):569. https://doi.org/10.3390/biom14050569
Chicago/Turabian StyleMcKay, Leo, Berardino Petrelli, Molly Pind, James N. Reynolds, Richard F. Wintle, Albert E. Chudley, Britt Drögemöller, Abraham Fainsod, Stephen W. Scherer, Ana Hanlon-Dearman, and et al. 2024. "Risk and Resilience Variants in the Retinoic Acid Metabolic and Developmental Pathways Associated with Risk of FASD Outcomes" Biomolecules 14, no. 5: 569. https://doi.org/10.3390/biom14050569
APA StyleMcKay, L., Petrelli, B., Pind, M., Reynolds, J. N., Wintle, R. F., Chudley, A. E., Drögemöller, B., Fainsod, A., Scherer, S. W., Hanlon-Dearman, A., & Hicks, G. G. (2024). Risk and Resilience Variants in the Retinoic Acid Metabolic and Developmental Pathways Associated with Risk of FASD Outcomes. Biomolecules, 14(5), 569. https://doi.org/10.3390/biom14050569







