- Review
Gut–Sinus Axis and the Role of the Microbiome in the Pathogenesis of Chronic Rhinosinusitis: A Literature Review
- Vivekanand Ashok,
- Mikash Mohan and
- Anna Juline
- + 3 authors
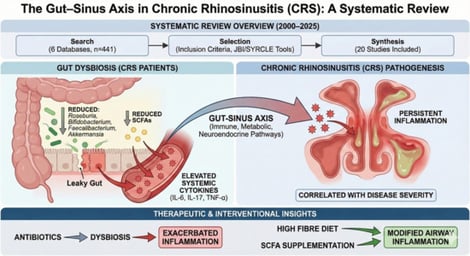
Chronic rhinosinusitis (CRS) is a persistent inflammatory disorder of the nasal and paranasal mucosa, typically attributed to local infection or anatomical obstruction. However, recent evidence suggests that CRS may also reflect systemic inflammatory dysregulation influenced by the gut microbiome, establishing a potential ‘gut–sinus axis’. This systematic review aims to synthesise current evidence linking gut microbiome alterations to the pathogenesis and clinical course of CRS and to explore emerging therapeutic strategies targeting this axis. Five databases were comprehensively searched for studies published between January 2000 and October 2025. Data were extracted and evaluated for quality using the JBI and SYRCLE tools. A total of 441 records were retrieved, of which 20 studies met the inclusion criteria. Human studies consistently showed gut dysbiosis in CRS, characterised by reductions in Roseburia, Bifidobacterium, Faecalibacterium and Akkermansia species. These microbial shifts correlated with increased levels of systemic cytokines, such as interleukin-6, interleukin-17 and tumour necrosis factor-α, and disease severity. Animal and interventional studies confirmed that high-fibre diets and short-chain fatty acid (SCFA) supplementation modified airway inflammation, whereas antibiotic-induced dysbiosis exacerbated it. Current evidence substantiates a gut–sinus axis mediated by immune, metabolic and neuroendocrine pathways. Dysbiosis-driven reductions in SCFA-producing bacteria appear central to systemic pro-inflammatory signalling implicated in CRS.
12 March 2026